Physicians as Stakeholders in Health Care: PQRI Is An Opportunity to Participate
Physicians as Stakeholders in Health Care: PQRI Is An Opportunity to Participate
Authors: K. Gabrielle Gaspar, MD, MPH, Executive Director, Gage Healthcare Consulting, Sacramento, CA; Sherellen Gerhart, MD, MPH, President, Gage Healthcare Consulting, Sacramento, CA; and Paul L. Weygandt, MD, JD, MPH, MBA, Vice President Physician Services, J.A. Thomas & Associates, Smyrna, GA
Peer Reviewer: Neil R. West, MD, Millennium Medicine, Tucson, AZ.
The Physician Quality Reporting Initiative (PQRI) is a program by the Centers for Medicare and Medicaid Services (CMS) that affects physicians and other health care providers who participate in Medicare. Clinicians in practically all medical specialties can participate in this voluntary reporting initiative and earn a bonus for satisfactory reporting. Originally launched in July 2007, the program enters the second reporting period on January 1, 2008, and continues through December 31, 2008. It is expected to continue in 2009. Eligible providers include allopathic and osteopathic physicians; doctors of podiatry, optometry, oral surgery, dental medicine, and chiropractic medicine; midlevel practitioners; physical and occupational therapists; social workers; nutrition specialists and other medical professionals who hold a National Provider Identifier. Participation involves selecting at least three quality measures applicable to one's practice from a list of 119 quality measures and submitting information for each qualified patient concurrently with Medicare claims during the entire reporting period. Successful reporting earns the provider a bonus payment on their Part B Medicare billings for the reporting period.1
As the PQRI is currently voluntary, many providers are considering whether to take part now or wait until participation is mandated. Careful weighing of factors on both sides of the issue allows for a more informed decision. Obstacles to participation include learning new vocabulary, codes, and rules of the program. Capturing data may involve changes in clinic work flow processes, education of staff, and extra documentation. There is also controversy regarding Medicare's transition into pay-for-performance and whether physician involvement in the PQRI benefits or harms the profession. In an increasingly demanding and competitive health care environment, all of these concerns merit attention. Potential benefits of participation include the bonus payment, receiving feedback on quality measures of interest, improving quality and documentation of patient care, and preparing for future quality improvement and pay-for-performance programs. As physicians face increasing accountability to patients and payers alike, successful participation in the PQRI early on may provide value beyond the immediate program incentives.
This article describes the PQRI in the context of the current health care environment. Relevant concerns include rising medical costs, demand for increasing physician accountability, and the trend toward performance incentive programs for clinicians. Specific guidelines for program participation and strategies for success are discussed.
The Editor
Background: What is PQRI?
PQRI is in its second iteration, yet a number of health care providers have heard little or nothing about this Medicare reporting program. Since starting in July 2007, the initiative has escaped the attention of many clinicians, yet they are the people who most need to know about the program, understand its impact on the delivery of health care, and appreciate the implications of participation for both themselves and the patients they treat.
PQRI is a program by the Centers for Medicare and Medicaid Services (CMS) that allows physicians and other clinical professionals to submit data on specified quality measures for eligible Medicare patients. It is voluntary, provider driven, evidence based, and designed to capture quality data at the claims level. The program currently focuses on the reporting of measures rather than the achievement of clinical outcomes and is linked to a monetary bonus that can be earned by any provider who meets the reporting requirements.
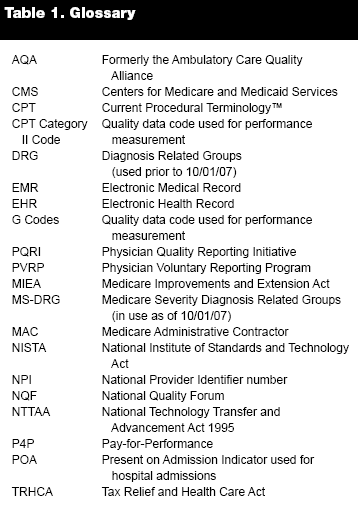
From a policy perspective, PQRI is part of Medicare's transition into an active purchaser of quality health care. The concept of value-based purchasing (VBP) has been in the government's sights for decades and has been gaining increased attention from legislators and program administrators.2 In 2001, the Department of Health and Human Services announced the Quality Initiative, an effort "to assure quality health care for all Americans through accountability and public disclosure."3 In its move toward a purchaser model of health care in which value is defined, measured and rewarded, several CMS programs have already been implemented. These include the Nursing Home Quality Initiative (2002), the Home Health Quality Initiative (2003), the Hospital Quality Initiative (2004), the Physician Focused Quality Initiativepredecessor to PQRI(2004), the End Stage Renal Disease Quality Project (2005), and the Physician Voluntary Reporting Program (2006). More recently, the Hospital Acquired Conditions and Present on Admission program was launched in late 2007. PQRI, which also began in 2007, has its statutory basis in the Tax Relief and Health Care Act of 2006 (TRHCA).4 (See Table 1 for a glossary of acronyms and terms.)
 |
Unlike the previous programs, PQRI focuses on data capture for individual clinicians of most specialties and is being launched on a national level. Any physician or other eligible Medicare provider with a National Provider Identifier (NPI) can participate. Providers submit data on selected quality measures with Medicare claims for services during the reporting period. While this may eventually provide useful, comprehensive data on the kind of care providers deliver to their patients, the program raises concerns regarding the difficulty of measure selection and design, the need for acuity adjustments, accurate physician profiling, and whether such measures can ever meaningfully be translated into information about patient care. Skeptics also worry about a lack of transparency in the development of program specifics, the challenges of obtaining program information in a timely manner, and the impression that providers are being asked to do more work while being subjected to diminishing reimbursement.
These concerns deserve consideration, but PQRI should not be dismissed. Rather, the initiative is a unique opportunity for individual providers to participate in shaping the delivery and funding of medical care in the future. Whether fair or unfair, elegant or burdensome, quality-driven or cost-motivated, temporary or permanent, PQRI allows clinical professionals to weigh in on the important issues of health care delivery, best practices, reimbursement, outcomes measurement, and resource use. By participating, individuals can meaningfully contribute to this giant experiment in national health care data collection. They do so by choosing measures that are relevant to their practices and patients, making a good faith effort to report on those measures, providing feedback to CMS and related parties on the design and utility of the measures, and publicly commenting on the value of the provider reports and bonus awards. While all of this may require significant effort, it provides clinicians the opportunity to gain experience in quality data reporting and to offer feedback on an emerging program.
Trends in Pay for Performance (P4P): What is Pay for Performance?
P4P is "a tsunami building offshore in a sea of stakeholder unrest, threatening those who are not prepared."5
In the context of rising U.S. health care costs and unsatisfactory health indicators, efforts to improve delivery of medical care are becoming common. The Institute of Medicine's (IOM) pivotal 2001 report, Crossing the Quality Chasm: A New Health System for the 21st Century, notes that health care "harms patients too frequently and routinely fails to deliver its potential benefits."6 It also asserts that payment for services is an important factor influencing the behavior of providers and patients alike. While policy makers and industry experts weigh various strategies to improve quality, P4P is one approach that is increasingly familiar to health care professionals and the public. There is no set definition of the term or rules governing its implementation, but P4P invariably involves linking remuneration to measurements of "quality" at the organizational or individual level. In the private sector, many insurers have incentive programs that assign bonuses based on patient satisfaction surveys, laboratory values suggestive of effective disease management, and other proxy measures of clinician performance. Use of electronic health records and other technology is frequently included. Health Maintenance Organizations (HMO) and large health plans have been increasingly using performance incentives in their contracts with hospitals and individual providers. In 2006, Hill Physicians Medical Group paid $32 million in performance compensation to its participating physicians, up from $7.5 million in 2002 and $13.5 million in 2003.7 This HMO health care network also reports quality improvement and patient satisfaction results on its web site. Similarly, Blue Cross of California announced a distribution of $69 million in physician bonus incentives in August 2007, the most awarded since initiating its P4P program in 2001.8 Their performance assessment includes quality measures in chronic disease management and adherence to screening guidelines as well as patient satisfaction surveys, clinical measures, waiting times for appointments, number of complaints and grievances, and review of medical group functions.
The Agency for Healthcare Research and Quality (AHRQ) reported that more than half of HMOs in the United States included P4P in their contracts for individual physicians as well as hospitals in 2005.9 Other reports suggest that 90% of the nation's HMOs were using some sort of P4P to compensate physicians in 2005.10 In 2007 there were 155 health care P4P programs in the commercial sector compared to 39 in 2003.11 Also noteworthy is the emergence of nonprofit organizations aimed at promoting excellence and accountability in the delivery of health care. One example is Bridges to Excellence, which partners with the Leapfrog Group to develop and implement physician rewards programs.12 In California, the Integrated Healthcare Association is a statewide leadership group that promotes quality improvement, accountability, and affordability in the industry. Its five year old California Pay for Performance Program promotes the use of P4P in quality improvement through a collaboration between numerous stakeholders including professional associations, government agencies, private vendors and payors, nonprofit foundations, and consensus bodies.13
The interest in P4P is growing in the public sector as well. In 2005, the Medicare Payment Advisory Commission (MedPAC) recommended that Congress establish a quality payment program for Medicare physicians.14 MedPAC Executive Director Mark Miller testified to the U.S. Senate Committee on Finance, "Providers are not all created equalthere's abundant evidence that some providers do a better job than others. To continue to pay them as if they're all performing equally well is a tragic situation."15
By any measure, the trend toward pay-for-performance in the medical industry is not a transient phenomenon. Indeed, the AHRQ within the Department of Health and Human Services devotes a section of its web site to research and resources on pay-for-performance incentives.9 A recent report by the Commonwealth Fund cites increased transparency in the quality and price of health care as key mechanisms to reduce medical spending and improve performance of the system overall.16 The paper notes that public reporting of clinical processes, outcomes, and patient experience of care are essential factors in stimulating providers to improve quality and efficiency through benchmarking and financially rewarding performance. In 2007, the American Medical Group Association issued a policy statement addressing the need to pursue improved quality through the "measuring, reporting, and application of findings using evidence-based clinical and service quality measures and tools such as benchmarking, best practices, and peer review."17
CMS has been increasing its efforts to identify delivery of quality medical care and reward those providing it. As our nation's medical system increases in bulk and cost, the federal government has inched its way into the P4P arena at the organizational and individual levels. On the premise that there is an effective way to identify and pay for only quality medical care, Congress and the Executive Branch have set into law several statutes for value based purchasing. These require CMS to measure quality in health care and attach financial incentives to high quality performance. Examples of these programs are mentioned above.
According to a Congressional Budget Office report released November 13, 2007, health care spending in the United States will increase to 50% of the nation's gross domestic product in 75 years if left unchecked.18 CBO Director Peter Orszag commented that "in their efforts to stem the growth of health care costs, Congress and federal policymakers need to promote cost effectiveness and 'evidence-based' medicine."19 The report further suggests assigning to hospitals and physicians "modest bonuses for practicing effective care or modest cuts in their payments for using less effective treatments."18
Along these lines, two initiatives effecting both hospitals and physicians have been implemented. The first major revision of the Diagnosis Related Group (DRG) system since 1983 was implemented on October 1, 2007, only 90 days after the launch of PQRI. This was not a matter of coincidence but rather reflects the government's multi-faceted approach to profiling and payment for quality. A principal justifying reason for instituting the new Modified Severity-DRGS (MSDRG) was to provide more accurate severity data for measuring quality and inpatient outcomes.20 Also mandated by Congress was the implementation of the Present on Admission (POA) initiative for hospital care. Eight initial conditions have been selected as meeting the criteria of being high cost or high volume, assigned to a higher paying DRG when present as secondary diagnosis, and reasonably preventable through the application of evidence-based guidelines.21 In essence, the use of POA indicators ensures that if any of the conditions develop during hospital stay and are not documented as being present upon admission to the hospital, neither the hospital nor the treating physician are credited for the care provided or severity assigned. It is evident that financial incentives for performance are becoming more prominent in CMS' quality improvement efforts. The Department of Health and Human Services' recent report to Congress on its plan for a Hospital Value-Based Purchasing Program notes that public reporting and financial incentives are both important tools to drive improvements in clinical quality, patient-centeredness, and efficiency.22 While CMS has focused its early reporting and P4P efforts on the hospital setting, it is steadily expanding the trend to individual professionals. The PQRI is CMS' entree into P4P at the provider level.
CMS has launched PQRI as a national voluntary reporting program that allows providers to choose quality measures and submit data directly with their claims information. Participation only requires that providers have an NPI and can identify measures that fit their patient population and scope of practice. Reporting on selected measures uses codes that indicate performance of certain clinical tasks or administration of therapies premised on evidence-based medicine. There are also mechanisms for clinicians to report without penalty when a clinical action has not been completed or documented.
In this way, PQRI is more accurately a "pay-for-reporting" than pay-for-performance program. With regard to the bonus, providers are measured on their level of reporting rather than their actions directed toward patient care, even though data on the latter are being captured. Presumably, this design allows for program revisions before actually attempting to measure and reward "performance" or "quality." That CMS is making the effort to refine the reporting process before attaching incentives to high clinical performance can be seen as a strong point in its movement toward active purchasing of quality care. The value of PQRI is that it provides an opportunity to find strengths and weaknesses in the data reporting and analysis process. This should lead to the development of a manageable reporting process that captures useful data truly reflective of the clinician's efforts at the practice level.
Outcomes, Metrics and Quality: How Is Quality Measured?
In order to reward excellence in medical care delivery, quality must be appropriately defined and accurately measured. Developing ways to collect meaningful quality-of-care data remains a challenge and may become the bane of pay-for-performance efforts.23 Many physicians are doubtful that the measures used in PQRI and other performance incentive programs have any relationship to quality health care, but rather primarily address cost containment and use of resources. Such factors will inevitably be part of the final analysis, but a genuine effort to use best evidence and include input from medical specialty groups and other professional organizations has been made. In fact, TRHCA requires that the measures included in 2008 PQRI be endorsed or adopted by a consensus organization.3 The National Quality Forum and the AQA Alliance have been identified as organizations that can develop measures through a defined consensus process or endorse measures submitted by medical specialty organizations. The AQA was formed in September 2004 as a consortium of representatives from the American Academy of Family Practitioners (AAFP), American College of Physicians (ACP), American Health Insurance Plans (AHIP), and AHRQ. Its goal was to facilitate efficient and effective methods for quality data aggregation and reporting as they pertain to the ambulatory care setting.24 Since its inception, the AQA has expanded its original mission into all settings of physician clinical practice. The National Quality Forum (NQF) is a private not-for-profit organization focused on the advancement of sound quality measurement efforts to facilitate health care system improvement.25 This organization has developed and trademarked standards for quality measurement in the U.S. health care system. CMS looks to NQF for the foundation of consensus formation processes regarding PQRI measures. As mentioned earlier, most PQRI measures relate directly to clinical care, but statute requires the inclusion of structural measures for 2008, such as the adoption and use of health information technology. More details about the formal process of measure development can be found in the Medicare Physician Fee Schedule Final Rule.3
The role of specialty organizations such as the AAFP and the ACP in the development of quality measures should not be overlooked. As members of the AQA and through their involvement in quality measurement efforts, the AAFP and ACP demonstrate implicit support for quality reporting. Each offers its members information on performance measurement, P4P, and PQRI. The AAFP summarizes PQRI information and provides CMS links on its web page.26 The ACP has identified seven PQRI measures as being particularly relevant to internal medicine and has created a tool to assist with data collection.27
Implications for Patients and Physicians: Do Pay for Performance Programs Improve Quality of Care and Benefit Patients?
Given the cost and burden of implementing health care performance incentive programs, it is important to know whether such efforts positively impact the quality of health care. The use of P4P programs as a means for improving quality assumes that if providers, hospitals, and other medical facilities are subject to measurements of quality, especially when associated with financial implications, then patients will receive better care. This is not well supported in the literature.28 Research has shown that incentive programs can have positive, neutral, or even negative effects on quality measures and patient experiences. While performance-based programs with positive results may increase preventative care or other services, unintended effects can include decreased access for severely ill patients.29 Substantial data on the impact of P4P and other reporting programs on the quality of health care are lacking. A report by the Health Research Institute found that major private payers fail to rigorously evaluate their P4P programs.30 Only one in 10 of the nation's largest commercial health plans has a statistically valid process for evaluating results of its physician incentive program. Yet these plans cover 39 million patients and incur significant administrative costs scoring physicians on measures of quality. As the trend in P4P advances, tools for assessing the impact of physician rating programs on health care cost and quality will need to be standardized and readily available to organizations using such programs. Notably, The Leapfrog Group web site provides the ROI Estimator, an open source tool for calculating the benefits and savings from P4P programs.31
How Does Pay for Performance Impact Providers?
In the context of health care incentive programs including PQRI, the value of data depends ultimately on its translation into meaningful changes in the practice setting. Inherent in this process is the capture of appropriate data and its accurate interpretation, followed by the development and implementation of viable policies. Assuming that the measures for PQRI 2008 address a fair sampling of clinical issues and corresponding appropriate clinical actions, there remains the question of how the data will be used. This is perhaps one of the greatest obstacles to provider participation in the program while participation is still optional. The data obtained may have a negative impact on physicians as an artifact of program structure, or it may be used to discourage clinical resource use. Providers also worry that measures may fail to account for patient acuity, effectively penalizing those who take care of more ill and complicated patients. While acuity is addressed in other CMS programs such as with the new MS-DRGs, it is not a factor in current assignments of the bonus in PQRI, and it remains unclear how the issue will be addressed in later iterations of the initiative. Concerns about physician profiling, however, are both immediate and substantiated. It is important for practitioners to realize that physician profiling exists in many forms, and public sector programs are not immune. The PQRI feedback reports will be provided directly to the practitioner in a confidential manner for the 2007 and 2008 reporting periods, but it is expected that data in later years will be public domain. The reports may be valuable for physician quality improvement efforts, but only if physicians use the data to assess and improve their performance. Studies show that this does not routinely happen.32 Further, physicians are typically reluctant to share data publicly, and they are seldom involved in quality improvement redesign activities.
With the growing awareness of public reporting in health care, the profession cannot continue its pattern of noninvolvement. Physician profiling may seem inconsequential in the current environment, but the trend is toward increased emphasis by payers and awareness of it by consumers. Consumers of health care, including the public and third-party payers, are accessing multiple and rapidly proliferating sources for ranking of hospitals and individual providers. Data from future CMS and quality initiatives will inevitably provide models for large scale reporting as well as competitive rankings for physicians and other practitioners. As a profession, our failure to participate in an objective and critical manner may leave us with misleading statistics and inaccurate and potentially damaging clinician profiling.
Thomson Healthcare's Sixth Consumer Insight Report released in September of 2007 characterizes the quality-driven medical consumer as more likely to research information on doctors and hospitals. So while "for 58% of the adult population, good physicians and the best treatment options drive opinions on quality health care," there is a 20% segment that is more likely to switch to another practitioner or hospital if unfavorable reports are encountered.33 The latter group tends to be highly educated, higher earning and preferentially trusts quality-rating organizations and web sites for their health care information. Twenty percent may seem like a relatively small portion of the health care market, but the number of consumers actively seeking information can be expected to grow as rankings become more accessible. "One of the things we were trying to illustrate is that there is a highly segmented market out there, and that there is already a meaningful segment of the market that is inclined to think about quality as a way of making a decision around health care," states Kaveh Safavi (Chief Medical Officer of Thomson Healthcare), one of the report's authors.34 Consumers only need visit internet sites such as www.hospitalcompare.hhs.gov, www.leapfroggroup.org or www.ahrq.gov to obtain a vast range of quality information that stems from years of quality–rating proxy databases. This trend will accelerate with the growing use of electronic health and medical records.
While ranking systems may not be the most accurate way of presenting quality data, we can expect them to remain part of the health care landscape. Achievement of clinical benchmarks is perhaps a more appropriate way of judging quality in health care delivery, but our competitive culture gravitates toward comparisons. It is likely that as health care providers we will continue to encounter these systems in our professional lives, and we must take an active role guiding their evolution. The more physicians participate in reporting and quality initiatives early on, the more likely we are to have a voice in how the data are gathered, interpreted and used. If such systems are going to exist, we should fully participate in their development and actively scrutinize the data produced and how it is applied.
We will undoubtedly see more physician rating systems made public, and there is no guarantee that they will be fair or accurate. Some may be used for educational purposes, showing physicians how they practice in comparison to their peers and practice standards. Others may be used to penalize resource use through denial of staff privileges or elimination from preferred provider lists. There are already numerous controversies surrounding the use of physician performance data, including lawsuits against third party payers. A notable example is the suit last year filed in November 2006 by physicians and the Washington State Medical Association against Regence BlueShield for dropping more than 500 providers from their preferred network in that state due to poor ratings in the "quality and efficiency of their practices."35 This policy allegedly affected more than 8000 patients and their physicians. The AMA joined the case, and when Regence dropped its use of a Select Network the following month, it was noted to be "a good first step toward eliminating arbitrary measures that do not accurately reflect physician quality."35 More recently, New York State Attorney General Andrew Cuomo reached an agreement with CIGNA Healthcare, a leading national insurer, to create a physician ranking system that emphasizes accuracy, disclosure, transparency, and fairness. CIGNA, whose program reaches 28 states, has agreed to use measures endorsed by NQF or other nationally recognized standards, account for risk adjustment and valid sampling, disclose to physicians and consumers how rankings are designed, and allow for appeals and complaints from all parties.36
Physician profiles are only useful if they are reliable and accurate, yet there is little research that demonstrates that existing programs are either. This is largely due to a lack of standardization in quality data measurements. Few studies have been done that have the necessary adjustments for risk and large enough numbers of participating providers to produce useful data. The literature has yet to show that outcomes for patients can be consistently linked to measurements of physician actions in the clinical setting. This does not stop profilers from producing and disseminating data.
In April 2007, Blue Cross and Blue Shield of Texas launched a web site that rates more than 40,000 physicians in its network and is open to members and nonmembers alike.37 Initially created in December 2006 and criticized by the Texas Medical Association for deficient data collection and reporting procedures, the online program assigns quality and affordability ratings based on physician scores.38
Consumers and practitioners can be led astray by rankings that reflect subtleties of data-gathering techniques or alternative agendas behind the reporting systems. By participating in PQRI in its early phases and providing feedback to CMS, providers can advocate for the use of standardized performance criteria that benefit patients rather than arbitrary rating systems that may penalize good practitioners.
Physicians as Stakeholders in Health Care: Should I Participate in PQRI?
Currently PQRI offers providers 1.5% bonus on their total Part B Medicare billings if successful reporting is achieved. Commercial insurance plans report incentive payments ranging from 1% to 8% of total base physician reimbursement, while some executives suggest that inducing changes in physician clinical behavior would require bonuses up to 10%.28 Some estimates speculate that up to 30% of physician compensation may be outcomes driven within the next few years.
Participation in PQRI can earn a primary care practitioner a few thousand dollars, but it will also require significant effort. It is difficult to counter the argument that Congress has legislated a cut in Medicare reimbursements to providers for the last several years and now is offering a small payment for extra work. Nonetheless, PQRI is here, and the early iterations of the program will likely shape how CMS approaches provider-based performance incentives and reimbursement in the coming years. Further, physicians need to understand that P4P has been intentionally devised to create incentives to improve the quality of patient care, an issue that is not going away. "Pay for performance isn't about pay, it's about performance. And if (doctors) think that ignoring accountability on performance, independent of any level of pay, is realistic then they don't understand." comments Dr. Safavi.34 Whether or not financial incentives are attached, clinical professionals will be held increasingly accountable for the care we provide. Ultimately we need to participate in efforts to improve health care delivery. Indeed, the Medical Group Management Association (MGMA) advances in the their position statement on pay for performance that for "any pay for performance program to be effective, participating physicians must fully understand and support the measures used and the operation of the program. That 'buy-in' can best be achieved by having practicing physicians and physician organizations actively involved in program design."39
So what is the cost of not participating? Should we ignore the program and hope it goes away due to lack of physician input? That is not likely to happen, since doctors did not ask for the program in the first place. By taking an unconditional stance against PQRI or pay-for-performance efforts, the harm may reach beyond the loss of data gathering opportunities. In the public's view, physicians resisting quality reporting efforts based on small financial incentives may appear to be against improving health care delivery in general. To come out ahead in our patients' perception and to advance our professional interests, medical providers need to engage constructively in this dialogue. Failing to do so, we may suffer the suspicion of patients who doubt our commitment to providing excellent care. We can also expect bureaucrats with no clinical experience to create a cumbersome reporting system of little use that we will be forced to adopt. On the other hand, participating in quality improvement efforts affords physicians the opportunity for input on how the programs will look going forward while gaining the respect of the public. Input on PQRI can be transmitted through several mechanisms. CMS provides National PQRI Provider telephone conferences, communication through regional officers, and provision of public comment periods for proposed rule changes. Further, recommendations and comments on specific measures can be directed to the "owners" of the measures including the AMA, AQA, and other organizations.1
PQRI Program Specifics
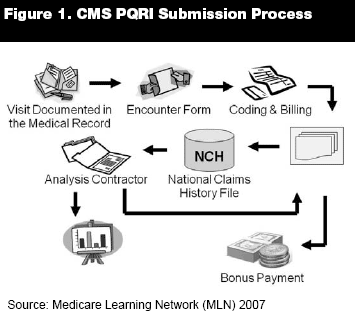
How Does it Work? Participation in PQRI is voluntary and there is no formal enrollment process. Any eligible provider with an NPI can begin reporting by simply including the proper codes on their paper or electronic claims. The 2007 reporting period was six months long and ran from July 1, 2007 through December 31, 2007. All data for 2007 must be submitted by February 29, 2008 to count toward bonus eligibility. Reporting for 2008 begins January 1, 2008, and ends on December 31, 2008. The exact deadline for final submission of 2008 data has not been announced. At the end of the reporting period, data will be analyzed for each participating professional and bonus checks will be awarded to those who reported successfully.4 Confidential feedback reports will also be issued. (See Figure 1.)
 |
Who Can Participate? Any practitioner who accepts Medicare part B payment and holds an active NPI can take part in the program This includes non-physician providers such as physical therapists, registered dietitians, social workers, and other licensed practitioners. The complete list of eligible reporters can be found on the CMS web site. At this time, physicians that practice at Federally Qualified Clinics (FQC) and do not bill under individual NPIs cannot participate.
Selecting Measures. To participate, a practitioner selects at least three measures that apply to his or her practice situation. Measures are not specific to specialties per se, but they may lend themselves to particular scopes of practice. The 119 measures for 2008 include 59 measures from the 2007 program, plus additional clinical and structural measures that were approved through consensus process. (Note that not all of the original 74 measures used in 2007 are included for 2008 because they did not meet consensus standards.)4 In general, the measures address management of chronic conditions, procedure related actions, acute episodes of care, resource utilization, prevention, and care coordination. New for 2008 are measures pertaining to the use of health information technology and electronic prescribing.
It is entirely up to the provider to choose which measures to use, and there is no upper limit to the number on which one can report. Some measures are designed to be reported only once during the entire period while others require reporting with each patient contact.
How to Report. Proper reporting consists of documenting measure-specific information in the medical record and submitting the appropriate quality data code(s) with the billing information. To report, providers submit data on paper-based CMS 1500 claims or via electronic 837-P claims at the time of billing. The PQRI reporting format uses numeric codes to relate whether or not a clinical action was completed. CMS, in conjunction with the AMA and other "owners" of the quality measures, have assigned special CPT Category II and G codes to quality measures. These are known as quality data codes, and they correspond to the 119 quality measures to be used in the 2008 program. To correctly report, claims forms need to include CPT Category I codes, ICD-9 codes, and the corresponding quality data codes pertaining to that visit. Again, quality data codes must be submitted at the time of billing and will not be accepted if submitted after a billing has occurred for a given PQRI eligible service. A practitioner's NPI must also appear on the billing information submitted to the Medicare Administrative Contractor (MAC). It is important to ensure that the MAC recognizes the NPI and maintains a link between it and the billing/claims data. Confidential feedback reports will be based on NPI and made available directly to the providers. The reports are to include information about the level of reporting as well as clinical performance as related to quality measures. A participant can earn a bonus of 1.5% of all Medicare Part B billings for successful reporting.
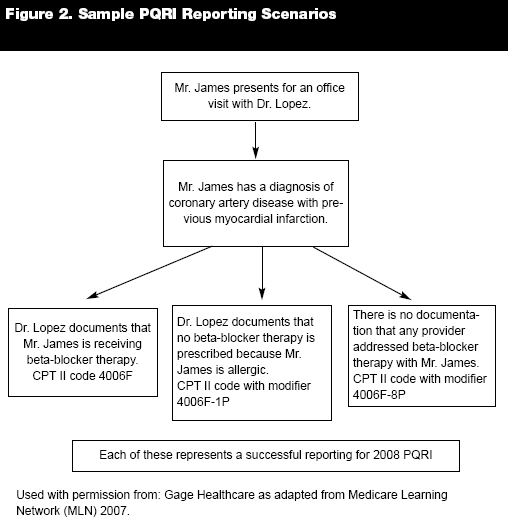
Reporting Measures Correctly. Successful participation involves reporting on 80% of eligible cases for at least three measures during the reporting period. Again, as the measures are not ascribed to specific specialties, practitioners may choose any three or more measures on which they wish to report. Once the measures have been selected, the participant submits data by use of the CPT Category II or G codes corresponding to each measure. When clinical actions are not done, reporting involves use of modifier codes along with the CPT Category II or G codes. Modifiers include 1P, 2P, 3P, and 8P. For example, a physician may determine that a patient meets eligibility for reporting on a measure but cannot receive the therapeutic intervention recommended by the quality indicator due to one of four reasons; (1P) patient reason (refusal); (2P) medical reason (adverse reaction to therapy or contraindication); (3P) system reason (intervention not available or inaccessible); or (8P) reason not specified. The physician submits the quality data code and appropriate modifier and is credited for reporting regardless of whether or not the clinical action was completed. (See Figure 2.) Note that some measures require more than on CPT Category II or G code as well as the appropriate modifiers.40 All required quality data codes must be included when reporting. Further, there must be appropriate documentation within the patient medical record to support all PQRI reporting.
 |
What Happens Next? Providers that meet program requirements by the end of the reporting period, December 31, 2008, will qualify for a one-time reimbursement check from CMS for a sum equal to 1.5% of their eligible professional services under the Physician Fee Schedule. It should be noted that the bonus calculation is based on all Medicare professional billings linked to the practitioner's NPI for the reporting period and is not limited to the fees specific to PQRI contact. The bonus will be issued to the holder of the Tax ID Number (TIN). There is no penalty assessed for reporting below the threshold level.
The Fine Print. There are some caveats. The measure list has been expanded in 2008, but there will be some specialists and practitioners who may find that only one or two measures fit with their scope of their practice. This would limit their eligible cases and decrease the denominator for reporting. Providers reporting on less than three measures or small numbers of cases may be subject to validation. Note that the cap provision from the 2007 program has been discontinued for 2008. More detailed information can be obtained from the CMS PQRI web site.1 Also, unlike current CMS reimbursement processes, PQRI incentive bonuses are not subject to appeals or judicial review. If CMS deems a practitioner ineligible to receive the bonus reimbursement, it will not be paid. An informal inquiry process is being developed.
Tips for Success in PQRI: How Do I Participate?
First, know the basics of the program. You must report on at least 80% of eligible cases per measure to qualify for the incentive payment. Providers are expected to report on at least three measures unless there are fewer than three that apply to their scope of practice. Reporting occurs at the time of claim for service for eligible cases. (See Table 2.)
 |
 |
You do not need to know all the measures and their corresponding quality data codes. Pick three measures that fit with your scope of practice and patient population. If you are in a practice with multiple providers, each participant selects his or her own measures for reporting. It does not matter if providers report on the same or different measures than their colleagues. It will be important for billing and coding staff to know which measures are being reported by each provider. Be familiar with the measures that apply to your practice and don't worry about the rest. Review the ICD-9-CM and CPT I codes that qualify claims for reporting on those measures. Refer to the CMS Coding for Quality Handbook and the PQRI Measure Finder Tool for more information.40
Determine your goals for participating. It is important to consider your goals for participating in the PQRI program. Are you most interested in quality improvement information, earning the bonus, preparing for future incentive programs, improved public profiling, or other benefits of participation? Some measures may be easier to report while others may provide useful outcomes data. Prioritizing your goals at the beginning will help you in selecting measures that facilitate success.
Also, it is important to choose measures that have meaning to your practice. Consider looking at your current practice demographics as well as anticipated growth or transition. If there are clinical conditions or processes that you would like to improve, look for measures in those areas. While choosing measures to assist you in meeting goals for quality improvement with a specific diagnosis or population, consider the number of patients within the category, ease of reporting on a particular measure and how the data or act of reporting will assist you adjusting practice habits to improve outcomes.
It can be helpful to use a team approach when implementing PQRI. Teach office, billing, and clinical staff about the program, reasons for participating, the concept of quality reporting, and any changes in their responsibilities that will be required. Allowing staff to participate in setting quality improvement goals and defining their role in the PQRI effort may increase their investment in the program.
There is no substitute for knowing your measures and coding well. After selecting the measures, learn the corresponding quality data codes (either CPT II or G codes). Review the modifiers that can be used with each quality data code. Create a "cheat sheet" or use the many tool kits available to demystify PQRI (CMS resources or commercially available tools).41 Be familiar with age, sex, or other demographic requirements for the measures. Know the reporting frequency and time frames that apply to your measures.
Before starting to report, analyze your practice processes. You can expect to make at least minor adjustments to prepare for PQRI. Examine clinic flow, staff responsibilities, office processes, methods of documentation, and billing system. Determine the best mechanism within your office to "flag" eligible patients. Be sure office staff are educated about the program and have the tools needed for reference. If you use an electronic practice management system or electronic medical record (EMR), find out if it can accommodate PQRI data collection. If your EMR system is linked to a billing system, find out if the data can be transferred directly or must be manually uploaded.
As always in patient care, it is essential to document thoroughly. Support your reporting of quality measures by documenting clinical actions, laboratory values, other study results, and pertinent medical history or other information in the patient's medical record. You can include the PQRI Data Collection Worksheets in the chart to support documentation of the quality measure.
Additionally, the sooner you begin reporting the better. Some measures need only be reported once during the reporting period, so submitting data with early encounters increases opportunities for success. Early participation will also allow you to modify processes for reporting as needed.
And lastly, report quality data codes with claims submissions. Remember that if you fail to report the measure at the time of initial bill submission, you will not be able to resubmit the claim for purposes of adding quality data codes.
References
1. PQRI Program Summary and Educational Resources, Centers for Medicare and Medicaid Services. Available at: http://www.cms.hhs.gov/PQRI. Accessed 11-21-07.
2. Meyer JA, Rybowski LS, Eichler R. Theory and Reality of Value Based Purchasing: Lessons from the Pioneers. AHCPR Publication No.98-0004, November 1997. Agency for Health Care Policy and Research, Rockville, MD. Available at http://www.ahrq.gov/qual/meyerrpt.htm. Accessed 11-11-07.
3. Quality Initiatives General Information, Centers for Medicare and Medicaid Services. Available at: http://www.cms.hhs.gov/QualityInitiativesGenInfo. Accessed 11-26-07.
4. MEIA-TRHCA final rule on PQRI 2008. Available at: http://www.cms.hhs.gov/physicianfeesched/downloads/CMS-1385-FC.pdf. Accessed 11-14-07.
5. American Medical Association Issues Report to Member Physicians on Pay for Performance. California Healthline. December 10, 2004. Available at: http://www.californiahealthline.org/articles/2004/12/10/American-Medical-Association-Issues-Report-to-Member-Physicians-on-Pay-for-Performance.aspx?topicID=37. Accessed 11-14-07.
6. Report Brief. Crossing the Quality Chasm: A New Health System for the 21st Century March 2001. Available at: http://iom.edu/CMS/8089/5432/27184.aspx. Accessed 9-25-07.
7. Way beyond Vitals. Hills Physician Medical Group 2006 Annual Report. Available at: https://www.hillphysicians.com/About_Us/Annual_Report.aspx. Accessed 11-21-07.
8. Blue Cross of California Pays Out Over $69 Million in Physician Bonus Incentives. August 24, 2007. Blue Cross web site Press Room. Available at: http://www.bluecrossca.com. Released on July 2, 2004. Accessed 11-21-07
9. AHRQ Resources on Pay for Performance (P4P). Available at: http://www.ahrq.gov/qual/pay4per.htm. Accessed 11-22-07.
10. Pay-for-Performance Incentives for Physicians are Common (Evidence of Practice). AORN Journal April 1, 2007. Available at: http://www.highbeam.com/doc/1G1-162360763.html. Accessed 11-21-07.
11. Pay for Performance Programs for Providers Now Total 150 published August 29, 2007. Available at: http://www.leapfroggroup.org/media/file/MV-Leapfrog_P4P_Press_Release.pdf. Accessed 9-10-07.
12. Measuring Provider Efficiency 1.0, a collaborative multistakeholder effort. Available at: http://www.bridgestoexcellence.org/Documents/Measuring_Provider_Efficiency_Version1_12-31-20041.pdf. Accessed 9-10-07
13. Integrated Healthcare Association web site. Advancing Quality Through Collaboration: The California Pay for Performance Program. February 2006. Available at http://iha.org/wp020606.pdf. Accessed 1-17-2008.
14. Strategies to Improve Care: Pay for Performance and Information Technology Med Pac Publication. Available at: http://www.medpac.gov/publications/congressional_reports/Mar05_Ch04.pdf. Accessed 11-28-07.
15. Miller ME. Pay for Performance in Medicare, Testimony to the U.S. Senate Committee on Finance, July 27, 2005. Available at: http://www.medpac.gov/publications/congressional_testimony/Testimony_P4P.pdf. Accessed 11-28-07.
16. Shea KK, Shih A, Davis K. Health Care Opinion Leaders' Views on the Transparency of Health Care Quality and Price Information in the United States, The Commonwealth Fund, November 2007.
17. Roman G H. AMGA Public Policy Statement. Group Practice Journal 2007;56(6).
18. Long-Term Outlook for Health Care Spending. Congressional Office Budget Report. Available at: www.cbo.gov. Accessed on 11-12-07.
19. CBO Testimony. Peter R. Orszag, June 21, 2007. Available at http://www.cbo.gov/ftpdoc.cfm?index=8255. Accessed 11-14-07.
20. Federal Register Vol. 72, No. 147 Wednesday, August 1, 2007. http://www.access.gpo.gov/su_docs/fedreg/a070801c.html. Accessed 11-14-07.
21. MLN Matters Number MM5499 Revised. Available at: http://www.cms.hhs.gov/MLNMattersArticles/downloads/MM5499.pdf. Accessed 11-14-07.
22. The Medicare Hospital Value Based Purchasing Plan. Available at: http://www.cms.hhs.gov/AcuteInpatientPPS/downloads/hospital_VBP_plan_issues_paper.pdf. Accessed 11-28-07.
23. Landon BE, Normand SLT, Blumenthal D, et al. Physician clinical performance assessment: Prospects and barriers. JAMA 2007;290:1183-1189.
24. AQA Alliance web site. www.aqaalliance.org. Accessed 1-17-2008.
25. Standardizing Ambulatory Care Performance Measures 2004. National Quality Forum web site. Available at:http://www.qualityforum.org/projects/ongoing/ambulatory/index.asp. Accessed 11/21/2007.
26. American Academy of Family Physicians web site. Performance Measurement and Pay-for-Performance. http://www.aafp.org/online/en/home/practicemgt/quality/qitools/perfmeasure.html. Accessed 1-17-2008
27. American College of Physicians web site. Medicare Pay for Report Program: Physicians Quality Reporting Initiative (PQRI) Resources for 2008. http://www.acponline.org/pmc/pqri.htm. Accessed 1-17-2008.
28. Grol R. Improving the quality of medical care: Building bridges among professional pride, payer profit, and patient satisfaction. JAMA 2007;286: 2578-2585.
29. Petersen L, Woodward L, Urech T, et al. Does Pay-for-performance improve the quality of health care? Ann Int Med 2006;145:265-272.
30. Keeping Score* A Comparison of Pay-for-Performance Programs Among Commercial Insures. PricewaterhouseCoopers' Health Research Institute, 2007.
31. Leapfrog Hospital Rewards Program™ ROI Estimator Available at: http://www.roiestimator.com. Accessed 11-27-08.
32. Audet AJ, Doty MM, Shamsadin J, et al. Measure, learn, and improve: Physicians' involvement in quality improvement. Health Affairs 2005;24:843-853.
33. MacCracken L, Pickens G, Ray L, et al. Sixth Consumer Insight Report from Thomson Healthcare, September 2007.
34. Kaveh Safavi, CMO Thomson Healthcare. (Personal Communication). 11-26-07.
35. Regence calls off flawed physician profiling. Statement attributed to: William G. Plested, MD, AMA President. Available at: www.ama-assn.org/ama/pub/category/17128.html. Accessed 11-14-07
36. Press Release. Attorney General Cuomo Announces Agreement with CIGNA Creating a New Model for Doctor Ranking Programs. New York, NY. October 29, 2007.
37. Goodman J. "Blue Cross Physician Rating Tools Go Live." Dallas Business Journal. May 18, 2007. Available at: http://www.bizjournals.com/dallas/stories/2007/05/21/story6.html?b=1179720000^1464779. Accessed 1-17-2008.
38. Press Release. Dec. 14, 2006. Faulty Doctor Rating System to be Suspended. Texas Medical Association web site. Available at: http://www.texmed.org/Template.aspx?id=5413. Accessed 11-24-07.
39. Principles for Pay-for-Performance Programs and Recommendations for Medical Group Practices. Medical Group Management Association. Available at: www.mgma.com/WorkArea/showcontent.aspx?id=1454.
40. Coding for Quality, A Handbook for PQRI Participation, June 18, 2007, CMS. Accessed at http://www.cms.hhs.gov/PQRI/Downloads/PQRI_Coding_for_Quality_Handbook.pdf. June 24, 2007. Accessed 1-17-2008.
41. Centers for Medicare and Medicaid Services web site. 2007 PQRI Tool Kit. Available at: http://www.cms.hhs.gov/PQRI/31_PQRIToolKit.asp#TOP. Accessed 7-1-07.
The Physician Quality Reporting Initiative (PQRI) is a program by the Centers for Medicare and Medicaid Services (CMS) that affects physicians and other health care providers who participate in Medicare. Clinicians in practically all medical specialties can participate in this voluntary reporting initiative and earn a bonus for satisfactory reporting.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
