Sleeve Gastrectomy: Mother of All Bariatric Procedures?
Sleeve Gastrectomy: Mother of All Bariatric Procedures?
Abstract & Commentary
By Amir Mehran, MD, FACS, Assistant Clinical Professor of Surgery; Director, Bariatric Surgery, Section for Minimally Invasive and Bariatric Surgery, Department of Surgery, UCLA. Dr. Mehran reports no financial relationships relevant to this field of study.
Synopsis: The Magenstrasse and Mill procedure is the simplest and most physiological gastroplasty yet described.
Source: Johnston D, et al. The Magenstrasse and Mill operation for morbid obesity. Obes Surg. 2003;13:10-16.
Laparoscopic Sleeve Gastrectomy (LSG) has attracted widespread attention in the bariatric surgery community. Originally advocated as part of a staged approach to high-risk patients, some now tout it as a one-shot operation of choice. LSG's origin dates back to the mid-1990's.
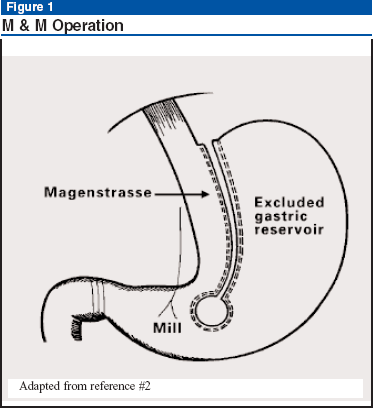
In 2003, Johnston and colleagues published their 6-year, 130-patient experience with what they coined the "Magenstrasse & Mill" (M&M) operation for morbid obesity.1 The Magenstrasse, or "street of the stomach," is a long narrow tube fashioned from the lesser curvature, which conveys food from the esophagus to the antral "mill." Normal antral grinding of solid food and antro-pyloroduodenal regulation of gastric emptying and secretion are preserved (see Figure 1). No anastomoses are created, and common complications, such as strictures, internal hernias, and nutritional deficiencies can therefore be avoided. The mean excess weight loss in this group was 60%. With the exception of gastroesophageal reflux disease in 28% of the patients, the complication profile was otherwise very favorable.
 |
Since then, several papers have been published about both the M&M operation, as well as its more commonly accepted variation, the sleeve gastrectomy. In 2003, Regan and colleagues first described their early favorable experience with LSG as part of a 2-stage operation in high-risk, super obese patients.3 One of the largest and most widely referenced papers is published by Cottam and colleagues.4 Over 4 years, 126 consecutive LSGs were performed at the University of Pittsburg under an IRB protocol. The patients were typically older, male, with a high BMI, and several severe co-morbidities. They reported only one late death, a 14% major complication rate, and a 46% excess weight loss at one year. In the vast majority of patients, co-morbidities had either improved or were completely resolved. With their American Society of Anesthesiology risk classification levels down-staged dramatically, 30% of the patients subsequently underwent a gastric bypass.
Laparoscopic sleeve gastrectomy has also been compared to other popular restrictive procedures: the BioEnterics intragastric balloon (BIB) and the adjustable gastric band (AGB). Gagner and colleagues matched 20 LSG patients with 57 historical controls from 2 other BIB series.5 At 6 months, 7% of the balloons had to be removed, and the excess weight loss results were 50% lower than the LSG patients. The LSG group had sustained no complications, leading Gagner et al to conclude that it was a superior first-stage procedure for the super obese compared to the BIB. In a randomized, prospective study, the only one of its kind published about the LSG, Himpens and colleagues compared the sleeve gastrectomy with the AGB.6 With only 40 patients in each arm, the LSG group demonstrated higher excess weight loss results (66% vs 48%) and better hunger control (47% vs 3%) at 3 years. Even though complications with the AGB were more frequent, LSG's complications tended to be more severe.
All of the above papers can be criticized on the basis of improper design, inadequate power, or short-term follow-up. To date, no large, prospective, randomized studies have been published comparing LSG to other weight loss procedures. This problem, however, has not stopped the bariatric surgical community from offering it, or from the patient population demanding it. Free of insurance and other regulatory issues, for example, surgeons in Mexico have been aggressively marketing LSG on their web sites, which are geared towards Americans. Patients, themselves, have been driving much of the increased demand, including perceived excellent weight loss results, yet safer' than the Roux-en-Y gastric bypass (RYGB) or the duodenal switch (DS), and devoid of the hassles of maintaining the adjustable band.
Similar to the perennial and never-ending AGB vs RYGB vs DS arguments, LSG has indeed been the topic of hot discussion at various conferences around the country. On March 16th, 2007, Ethicon Endo-Surgery held one such symposium at its corporate headquarters in Cincinnati, Ohio. The course was moderated by Drs. Philip Schauer and Samuel Szomstein from the Cleveland Clinic of Ohio and Florida, respectively, and included a live telesurgery from the latter location. The various surgical techniques and pearls, indications, complications, patient selection criteria, insurance reimbursement hurdles, etc., were all fully discussed. A diverse group of bariatric surgeons from around the country were in attendance. Even though most had successfully performed this operation, there were a few dissenting voices who were appropriately concerned about subjecting patients to 2 operations and 2 separate sets of risks. By the end of the session, however, there was uniform agreement that the laparoscopic sleeve gastrectomy should not be offered as a one-stage operation, except in unusual circumstances, such as inflammatory bowel disease, extensive intra-abdominal adhesions, and the like, where intestinal surgery can be fraught with numerous complications.
As its current president, Dr. Schauer discussed the American Society for Bariatric Surgery's goal to provide a position statement about the sleeve gastrectomy at its next meeting in June 2007. Until then, as he put it, the jury is not yet out. It is a relatively easy operation with very good short-term results. However, until more long-term data are published, bariatric surgeons should limit its use to high-risk patients as part of a staged approach. In the current environment, where bariatric surgery is under a thick microscope, any potentially negative publicity about LSG outcomes or complications would be detrimental to our community.
References
1) Johnston D, et al. The Magenstrasse and Mill operation for morbid obesity. Obes Surg. 2003;13:10-16.
2) Carmichael AR, et al. Effects of the Magenstrasse and Mill operation for obesity on plasma plasminogen activator inhibitor type 1, tissue plasminogen activator, fibrinogen and insulin. Pathophysiol Haemost Thromb. 2002;32:40-43.
3) Regan JP, et al. Early experience with two-stage laparoscopic Roux-en-Y gastric bypass as an alternative in the super-super obese patient. Obes Surg. 2003:13:861-864.
4) Cottam D, et al. Laparoscopic sleeve gastrectomy as an initial weight-loss procedure for high-risk patients with morbid obesity. Surg Endosc. 2006:20:859-863.
5) Milone L, et al. Laparoscopic sleeve gastrectomy is superior to endoscopic balloon as a first stage procedure for super-obese patients. Obes Surg. 2005;15:612-617.
6) Himpens J, et al. A prospective randomized study between laparoscopic gastric banding and laparoscopic isolated sleeve gastrectomy: Results after 1 and 3 years. Obes Surg. 2006;16:1450-1456.
The Magenstrasse and Mill procedure is the simplest and most physiological gastroplasty yet described.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
