Keeping an an "Eye" on the Patient: Pediatric Eye Trauma
Keeping an "Eye" on the Patient: Pediatric Eye Trauma
Authors: Catherine A. Marco, MD, FACEP, Clinical Professor, Surgery, Medical University of Ohio, Attending Physician, St. Vincent Mercy Medical Center, Toledo, OH; and Jeffrey Salisbury, MD, St. Vincent Mercy Medical Center, Toledo, OH.
Peer reviewer: Melanie Kazlas, MD, Acting Director, Pediatric Ophthalmology and Strabismus, Massachusetts Eye and Ear Infirmary, Harvard Medical School.
Eye trauma is a common chief complaint among emergency department (ED) pediatric patients. Although many eye injuries can be prevented by appropriate supervision of children's activities and the appropriate use of protective eye wear, eye injuries remain an important cause of visual loss. Specific attention to the physical examination is mandatory in the evaluation of pediatric eye trauma, and although challenging should include visual acuity, pupillary reactions, external examination, ocular motility, visual field testing, slit-lamp examination, fluorescein staining, intraocular pressure, and funduscopic examination. Certain "tricks of the trade" are presented here to aid the clinician in obtaining this critical information.
Following complete evaluation, many patients with eye injuries can be managed as outpatients with appropriate medical management and ophthalmologic follow-up. Certain eye injuries warrant ophthalmologic consultation, including hyphema, penetrating globe injury, suspected or known open globe injury, retrobulbar hematoma, or any eye injury resulting in significant visual loss. The authors present a complete review of the evaluation and management of the patient with a potential eye injury.
— The Editor
Introduction
Eye trauma is a common chief complaint among ED patients. It is estimated that 2.4 million eye injuries occur annually in the United States, accounting for 0.2% of ED visits; approximately one-third of eye injuries occur in pediatrics.1,2 The majority of injuries occur in the home, followed by public places, such as schools or athletic facilities.3 The most common injuries include corneal abrasion, blunt trauma, and corneal foreign body.4,5 Ocular trauma is one of the most significant causes of visual loss in pediatric patients. Many eye injuries can be prevented by appropriate supervision of children's activities and the appropriate use of protective eye wear during sports.
Eye injuries often are isolated injuries and may be managed as outpatients; Approximately 2-3% of patients require inpatient hospital admission.6 It is important to note, however, that eye injuries also may be associated with major trauma, particularly in patients with facial fractures, facial contusions, or basilar skull fractures; patients require a comprehensive evaluation to exclude concomitant injuries.7,8
Examination of the Injured Eye in the Pediatric Patient
Examining the injured eye of a pediatric patient may pose a significant challenge. Most patients older than age 3 can be successfully examined using interactive distracting techniques and parental assistance; rarely, a papoose board or sedation may be required to complete an adequate examination. Topical anesthesia may give the patient comfort during the eye examination. After collecting a comprehensive history, the physical examination of the eye should include these elements: visual acuity, pupillary reactions, external examination, ocular motility, visual field testing, slit-lamp examination, fluorescein staining, intraocular pressure, and funduscopic examination.9 However, certain areas of a thorough eye examination are age specific, other areas are independent of age, and most depend on patient cooperation. Remember to perform the more uncomfortable portions of the examination last.
Visual acuity is the vital sign of the eye, and is absolutely essential in the evaluation of eye trauma. An adhesive eye patch should be used for the assessment of vision in children. Inadvertent peeking around a parent's hand or wand occluder can lead to a false determination of vision in the traumatized eye. Visual acuity should never be excluded and the only time that it should be postponed is when a patient presents with a chemical exposure to the eye requiring immediate irrigation. Visual acuity in the neonate, infant, and toddlers is performed by assessing pupillary reaction to light. A light source should be used 1-3 feet away; the ability to track and fixate on light determines adequate visual acuity. Steady fixation is considered roughly equivalent to 20/40, unsteady fixation is equivalent to 20/100, and inability to fixate is equivalent to 20/400. By the age of 2-3 years, normal development places visual acuity at 20/20; therefore, a child should be able to participate in formal acuity testing by this age.
Formal visual acuity testing is performed using a Snellen chart, Allen figures (pictures), or rotating "E" chart at 20 feet. Testing should always be done with correction (if possible) or with a pin hole device if the patient is myopic. A pre-made pinhole device will correct most refractive errors to at least 20/30. If a pinhole device is not available, a quick alternative can be made using an 18-gauge needle and an index card, or a metal eye shield with multiple small holes also can be used. If a refractive error exists beyond 20/30, it should not be attributed to simple refractive error. When patients are unable to read the first line (20/200), shorten the distance to 10 feet and ask them to read the top line (10/200). Continued inability to read any letters will necessitate the physician counting his or her fingers for the patient and recording the distance at which the patient reports visualizing them (e.g., able to count 3 fingers at 3 feet). If the patient is unable to count fingers, then attempt to see if he or she can visualize gross hand motion or are able to detect light perception.10,11
Pupil examination should include size, shape, symmetry, and reaction to light. A unilateral dilated pupil raises concern for compression of the third nerve, which may be a sign of uncal herniation, especially when it is associated with traumatic head injuries. If this finding is present, the physician should perform a more detailed assessment, as there are other causes of unequal pupils, such as anisocoria or direct pupillary injury.
Tear drop pupils should alert the emergency physician that ocular perforation has occurred. After a penetrating injury to the eye, the pupillary margin and portions of the iris are drawn into the penetrating wound, causing a tear drop appearance with the apex pointing to the injury. During the pupillary exam, if a penetrating injury to the eye is suspected, avoid applying any pressure to the eye.
Examination of the eye should include evaluation for an afferent pupillary defect. A swinging flashlight test will determine if there is a relative afferent pupillary defect, also known as a Marcus Gunn pupil. A relative afferent pupillary defect can be seen in traumatic optic neuropathy. Shining a light on the uninvolved eye results in constriction of both the ipsilateral pupil (direct response) and contralateral pupil (consensual response). When the light is swung to the pupil with a damaged optic nerve or chiasm, it is as if the intensity of the light has diminished (reduced input along a damaged afferent system) and the pupil dilates. If the patient has suffered bilateral symmetric traumatic optic neuropathy, there will be no afferent pupillary defect (APD). Damage to the efferent system of the pupil, either cholinergic as in a third nerve palsy or sympathetic as in Horner's syndrome, results in unequal pupil size or anisocoria.12
External examination of the eye includes observing for proptosis (suggestive of retrobulbar hematoma) and enophthalmos (suggestive of ocular rupture or blow-out fracture). The eyelids should be examined for lacerations, contusions, and punctures. The inner aspects of the eyelids should be examined, looking for foreign bodies and subconjunctival hemorrhage. The cornea, sclera, and conjunctiva should be examined by gross inspection as well as by slit lamp examination. The anterior chamber should be examined after the patient has been upright for several minutes to allow visualization of a hyphema, if present. Evaluate the conjunctiva to detect lacerations, foreign bodies, or underlying scleral perforations.
Ocular motility should be assessed and documented. If a patient is unable to move the eye in a certain direction, concerns for entrapment oft a muscle from an orbital blow-out fracture, direct muscle injury, or central nervous problem should be considered. If the complaint is diplopia after trauma, evaluation should assess whether the diplopia is monocular (typically lens related) or binocular (entrapment, muscle injury, or CNS injury).
Visual field testing can be brief and simply involve the four major quadrants of vision; formal visual field testing can be done at a later time. Visual field testing is important to perform, especially if the history suggests the possibility of retinal detachment or vitreous hemorrhage (e.g., new floaters or flashes of light after eye trauma). Performing visual field testing is quick and easy. The patient should cover one eye and the physician should get at eye level and hold his fingers halfway between himself and the patient. The patient should be asked to look at the physician's nose while he or she slowly brings fingers from the outside in, making sure the patient does not look away from the physician's nose and toward the fingers. Binocular visual field loss is typically neurological in nature.
Slit lamp examination in older children is performed using the same technique as that used for adults. Younger children may feel more comfortable sitting on a parent's lap for the examination. Some tricks to making younger children more cooperative for the examination is to coax them into seeing something fun in the slit lamp (e.g., favorite cartoon character). Have parents place their chin in the device first to reassure the child, and tell the child that they will see a "pretty blue light." When examining infants, ask parents to sit and support the child's bottom with one hand while resting the other hand on the back of the infant's head. If the child is not cooperative, a Wood's lamp may be used as an alternative to diagnosing corneal defects; however, Wood's lamp examination does not allow the detail of inspection afforded by slit lamp examination. Some direct ophthalmoscopes have a cobalt blue light that can facilitate detection of a corneal abrasion.
Intraocular pressure (IOP) evaluation is useful in the setting of non-open globe trauma. IOP testing is contraindicated in suspected globe perforation, corneal abrasion, and foreign bodies. IOP evaluation is useful in patients with simple hyphemas in whom you do not suspect ocular rupture. IOP can be measured with a portable tonometer, or using slit lamp applanation tonometry. Normal IOP is 21 mmHg or less. Errors in tonometry can easily be made by placing too much pressure on the eye or the patient blinking or crying, all of which may artificially elevate IOP.
Finally, to view the posterior portions of the eye and retina, funduscopic examination is indicated. To assist in good visualization of the optic nerve and retina, have lights in the room turned off and turn the intensity of the ophthalmoscope to its lowest setting and smallest aperture. While examining infants, making creative noises and clicking sounds will enhance your success. Toddlers may be afraid of the ophthalmoscope, but allowing them to see it up close and possibly hold it may take away some of their anxiety. Another trick with toddlers is to ask them to look for their favorite cartoon character in the light as you are performing your examination. Ideally, funduscopic examination is best performed after dilation. Pupils should not be dilated if serial neurologic exams are to be performed or if acute angle closure glaucoma is suspected.
Corneal Abrasions
Corneal abrasions are one of the most common eye injuries and may occur from a variety of mechanisms, including, among others: projectiles, foreign bodies, direct trauma, fingernails, contact lenses, and bee stings.13,14 Symptoms of corneal abrasion may include pain, tearing, blepharospasm, photophobia, or foreign body sensation.
Examination should include evaluation of the location, depth, and surface area of the abrasion, using fluorescein staining and slit lamp examination. Lid eversion should be performed to rule out retained foreign body. Current treatment includes pain control, topical antibiotics, topical analgesics, and cycloplegic agents. Eye patching has no demonstrated benefit and is no longer recommended for corneal abrasions.15-18 Patching impairs depth perception and was shown in children to result in difficulty with ambulation.18
A topical antibiotic is indicated to prevent bacterial infection, although antibiotics do not have proven benefit in improved outcomes. Appropriate choices may include a topical quinolone, such as ciprofloxacin or ofloxacin drops, erythromycin ointment, polymyxin/trimethoprim drops, or numerous others.
Topical analgesics such as dicolfenac (Voltaren) and ketorolac (Acular) have shown a beneficial effect in reducing pain in corneal abrasions. A meta-analysis review of five randomized controlled studies showed a reduction of pain on a visual analog scale.19 Patients using topical nonsteroidal antiinflammatory drugs (NSAIDs) had greater relief of pain and used fewer oral analgesics and narcotics; however, an increase in initial transient stinging was commonly noted as an adverse effect.19,20
The use of a cycloplegic agent, such as homatropine or atropine, will relieve pain resulting from ciliary spasm. Home use of topical anesthetics should be avoided, due to negative effects on healing and increased risk of recurrent injury. Tetanus toxoid is routinely recommended for patients without an updated immunization status;21 however, a search of the literature from two separate sources did not identify any cases of clinical tetanus developing from a simple corneal abrasion.22
Most corneal abrasions heal well within 24 hours. Rarely, complications may occur; these include: delayed healing, scarring, infection, visual loss, or missed retained foreign body. Close follow-up is essential to ensure appropriate healing and relief of symptoms. In particular, injuries that result from vegetable or botanical matter or contact lens injury make the patient at higher risk for Pseudomonas infection and require close follow-up.
Corneal Foreign Bodies
A great variety of intraocular foreign bodies have been described, including metal fragments, wood, plastic, and others. Once it is determined that the injury to the eye is caused by a simple foreign body with resultant corneal abrasion, removal of the foreign body should be performed under slit lamp visualization. This should allow consistent and stable removal of the offending irritant.23
Corneal foreign bodies often can be safely removed in the ED. In an effort to remove an irritant from the pediatric eye, an attempt at removal with a moistened cotton tipped swab may be attempted first. If this effort is unsuccessful, the use of a needle is indicated to remove the foreign body. It is important to reassure the patient and parents that the needle does not go into the eye, but merely rests on the surface. In younger children, procedural sedation may be necessary to facilitate the removal of the foreign body. Attach a standard 5/8 inch 25-gauge needle to a 3 mL syringe for stability. Some prefer to bend the needle shaft 30 degrees to facilitate the approach to the eye. The foreign body can then be gently lifted off of the surface of the cornea. Once the foreign body is dislodged, use a moist cotton swab to remove it from the surface of the eye if necessary. If a rust ring remains following removal of a metallic foreign body, this also may be removed in the ED with either the needle or a burr. It also is acceptable to schedule ophthalmology follow-up for removal within 24-48 hours.24 If the child is unable to cooperate, ophthalmology consultation is indicated.
Following foreign body removal, reexamine the eye to make sure no signs of ocular penetration are present. Pay particular attention for any leak of fluid that appears to be a green stream after application of fluorescein dye (Seidel's sign). After the foreign body is removed and ocular perforation is excluded, then treat the injury as a typical corneal abrasion.
Penetrating Ocular Injuries
Common causes of penetrating ocular injuries include glass, BB's, metallic fragments, toys, sticks, and wood/plastic particles that have become projectiles.23,25 Bony fracture fragments also may cause intraocular foreign bodies or injury.26 Most injuries could have been avoided if proper safety equipment, mainly safety glasses, were worn.27 Factors associated with worse prognosis include objects with higher mass or objects with a blade shape, as opposed to disc, cylinder, or sphere shapes.28 Clinical factors predictive of poor outcome include visual acuity worse than 20/200, pupillary abnormalities, and hyphema.
Children are at higher risk for open globe injuries than adults; open globe injuries are the leading cause of monocular blindness in children world wide.29 Associated injuries may include corneal injury, scleral laceration, retinal detachment, or numerous other injuries. Thus, whenever a penetrating injury to the eye is suspected, a complete physician examination should be conducted, and ophthalmologic consultation obtained.30 Penetrating injuries may present immediately or up to years following the injury.31
Terms relevant to penetrating eye injuries include:
Laceration: a defect in the cornea or sclera caused by a sharp object;
Rupture: a disruption of the cornea or sclera caused by indirect forces or agents of blunt trauma, including low-velocity missiles such as BB's;
Penetration: any injury that traverses the partial thickness of the sclera or cornea;
Perforation: any injury that traverses the full thickness of the sclera or cornea; and
Double perforation: any injury that enters the eye and traverses the intraocular cavity and exits the sclera on the opposite side.30
The anatomy of the bony orbit protects the eye from most oblique and posterior injuries. Smaller missiles and sharp objects are often capable of entering the area within the orbital rim, increasing the likelihood of piercing the globe. Therefore, ocular penetration must be suspected whenever there has been a laceration, puncture, or disruption of the eyelids or orbital bone; or periorbital ecchymosis.32
In many cases, high-velocity projectiles that are small may penetrate the eyelid /globe and cause little pain or visual disturbance at all. The cornea may seal over the entry portal, leading to a paucity of eye findings. Intraocular foreign bodies should be considered in all penetrating eye injuries. If a penetrating globe injury is suspected, no pressure should be exerted on the eye because of risk of expelling intraocular contents. Perform a complete neurologic examination and obtain a through history of the events, keeping in mind that children may not tell the entire truth for fear of negative consequences. A detailed ocular examination should include visual acuity testing; pupillary testing; examination of the cornea, sclera and anterior chamber with slit lamp when possible; and funduscopic exam. Special attention should be made to look for signs of possible perforation, such as extensive subconjunctival hemorrhage and chemosis, collapse and hemorrhage in the anterior chamber, pupil and iris irregularities, positive Seidel's test, and traumatic cataract. Seidel's test is conducted by instilling fluorescein into the affected eye and examination under a slit lamp for a bright green stream of fluid resulting from the outflow of aqueous humor. If examination cannot be adequately performed due to emotional distress or poor cooperation, suspicion of a penetrating injury justifies an ophthalmologic consultlation for possible evaluation under anesthesia in the operating room where the nature and extent of the injury may be adequately addressed.
All penetrating eye injuries or suspected penetration warrant radiographic imaging. Be aware that x-ray may serve to reveal the size and number of metallic foreign bodies; however, it does not determine the exact three dimensional orientation of the foreign body with respect to the globe. Plain films also are not adequate for full evaluation of adjacent boney structures, sinuses, soft tissue, and the evaluation of non-metallic objects that may be readily seen on CT scan. Randomized retrospective study of the accuracy of CT scan in evaluating open globe injuries has shown a sensitivity of 75% and specificity of 95% for picking up such injuries in the absence of clinical examination or history.33 It is, therefore, recommended that patients with suspected intraorbital foreign bodies undergo CT scan with 1.5-3.0 mm cuts with coronal reconstruction when available.
Ultrasonography also may be helpful in the identification of intraorbital foreign bodies, although suboptimal sensitivity suggests that additional imaging should be performed if they are suspected clinically.34 In addition, intracranial foreign bodies may be associated with perforating ocular injuries, and intracranial imaging should be considered.35 (See Tables 1 and 2.)
| Table 1. Management of Perforating Eye Injuries |
1. Document visual acuity. |
| Table 2. Pitfalls in Management of Perforating Eye Trauma |
1. Intraocular foreign bodies may be missed in asymptomatic
patients with normal vision. |
Hyphema
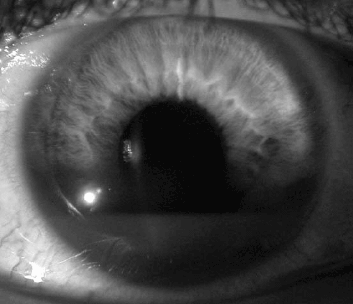
Hyphema (blood in the anterior chamber) is a common condition seen after blunt ocular trauma in pediatric patients, and results from rupture of the iris or ciliary body blood vessels.11,36 (See Figure 1.) Hyphema is more common among males, particularly those aged 15-18. Hyphema may occur secondary to blunt trauma, projectiles, or explosions, including specific examples of fists, balls, motor vehicle collisions, rocks, airbags, sticks, pellet guns, toys, tools, and numerous others.37,38 Hyphema usually occurs from a tear in the anterior portion of the ciliary body. Hyphema should be observed after the patient has been sitting upright for several minutes, to allow for layering and to accentuate visualization of the hyphema. Other associated eye injuries may occur, including corneal injuries (26-40% incidence), posterior segment injuries, and rebleeding. Hyphemas are classified according to amount of hemorrhage. (See Table 3.)
| Figure 1. Hyphema: Blood in the Anterior Chamber of the Eye |
Courtesy of Colin G. Kaide, MD, FACEP, FAAEM, The Ohio State University Department of Emergency Medicine. |
| Table 3. Classification of Traumatic Hyphema* |
|
Complications of hyphema may include corneal blood staining, visual loss, secondary glaucoma, secondary hemorrhage, and optic nerve atrophy. Factors related to poor outcome include grade of hyphema, intraocular hypertension, time for hemorrhage absorption, and associated posterior segment lesions.39 Good visual recovery occurs in only 35% of patients with total hyphema.
Corneal blood staining occurs in 2-11% of patients with hyphema, and occurs more commonly among higher grade hyphemas. Corneal blood staining may lead to visual loss or amblyopia.
Increased intraocular pressure is common; about one-third of patients with hyphema have increased intraocular pressure.
Secondary hemorrhage is associated with increased morbidity, including corneal blood staining, secondary glaucoma, optic nerve atrophy, and visual loss. It typically occurs 2-7 days after the primary injury. It occurs more commonly in patients with poorer initial visual acuity, large hyphema (more than 33% of anterior chamber), delayed medical attention, initial elevated intraocular pressure, and use of antiplatelet medications.40 It has been estimated that secondary hemorrhage occurs in 5-22% of patients with hyphema.40
Outpatient management is feasible for most patients with low-grade hyphema.39 Although traditional management in the past included strict bed rest, sedation, and eye patching, these treatments have not demonstrated improved outcomes. Hospital admission is usually not necessary and is not associated with improved outcome, although admission may be indicated for patients with secondary hemorrhage, markedly elevated IOP, sickle cell disease, hemophilia, visual loss, child abuse or those who are noncompliant.41 Elevation of the head to 30 degrees aids in hyphema clearance and facilitates the diagnosis of secondary hemorrhage. Patients should be told to avoid vigorous physical activity. The use of eye patching is controversial. Patching may improve comfort and reduce eye movement, although some authors argue that patching may raise the eye temperature and promote bacterial growth. Typically, topical antibiotics, cycloplegic agents, and topical corticosteroids are indicated. (See Table 4.) Other treatments remain controversial, and may include topical cycloplegics, systemic steroids, topical or systemic antifibrinolytics, topical beta-blockers, and carbonic anhydrase inhibitors. Surgical treatments, including paracentesis, hyphectomy, clot irrigation, or trabeculectomy, are indicated only for uncontrolled elevated IOP, corneal staining, or large hyphemas.
| Table 4. Management of Hyphema |
|
Thermal and Chemical Burns
Chemical burns to the eye occur as a result of direct exposure to a caustic chemical. Common sources of injury to the pediatric patient include household cleaning agents, automotive cleansers, swimming pool chlorine or other chemicals, battery acid, and other chemicals. Chemical burns are classified by tissue damage as associated with prognosis. (See Table 5.)
| Table 5. Chemical Eye Burns Classification |
|
Alkali burns often are more extensive than corresponding acid burns. Alkali rapidly penetrates the cornea and leads to increased pH of the aqueous fluid, causing liquefaction necrosis with extensive loss of corneal epithelium. Widespread tissue damage may follow the rapid rise in pH.
Acid burns also may be severe; however, the coagulation necrosis initiated by acid injury limits the extent of tissue injury in many cases. Following acid exposure, protein coagulation in the corneal epithelium produces a barrier to deeper penetration of acid. Hydrofluoric acid is an exception to this mechanism and may result in extensive corneal penetration and injury.
Chemical burns should be managed with immediate and copious irrigation, which improves prognosis and outcome.42,43 Rapid initiation of irrigation is more important than the precise irrigant solution used.44 Irrigation may be performed with a variety of readily available solutions. Normal saline (0.9%) has a pH of 4.5-6.0 and may be associated with mild discomfort. Alternative irrigants include water (readily available, but hypotonic); lactated Ringer's solution (pH 6.2-7.5); buffered normal saline (NS), with pH adjusted to 7.4 with sodium bicarbonate; and Balanced Salt Solution Plus (BSS Plus), with a pH of 7.4.45 The use of an intraocular irrigation lens may improve the contact of the irrigant with the cornea. Effective irrigation may require topical anesthesia and/or systemic sedatives. If the pH of the chemical-causing injury is unknown, it should be presumed to be alkali. Following alkali burns, regular pH assessment with litmus paper should be performed intermittently until the pH normalizes. Acid burns should be treated with irrigation for 15-20 minutes; alkali burns may require several hours of copious irrigation.
Thermal burns are less common, but may occur as a result of splash injuries, cigarettes/cigars, fireworks, matches, lighters, curling iron contact, and others. The eye is the most common body site injured by fireworks among pediatric patients, followed by injury to the face and hands.46 Thermal burns may be extensive and are proportionate to the time of contact and temperature of the burn surface. Often, eye protective mechanisms spare significant eye injury, including the blink, tears, bony orbit structure, and shielding of the face by the hands and arms.
Following either chemical or thermal burns, a complete eye examination and assessment should be performed, including visual acuity, intraocular pressure, and slit lamp examination. If devitalized tissue or foreign bodies are present, debridement and removal should be performed. Following irrigation for both chemical and thermal burns, supportive measures during the healing process for both chemical and thermal burns should include ocular lubricants, artificial tears, topical corticosteroids, and topical antibiotics. (See Table 6.)47-49 If intraocular pressure is elevated, appropriate therapy should be instituted. Appropriate pain management may include systemic nonsteroidal anti-inflammatory agents or opioids. Ophthalmologic consultation is indicated for most injuries. Surgical management may be indicated for significant necrotic tissue or severe injury.
| Table 6. Management of Chemical Burns to the Eye |
|
Blunt Eye Trauma
Blunt injuries to the eyes range in spectrum from simple contusion to retinal detachment or globe rupture. The most common cause of blunt trauma to the eye in children are sports and recreational events, which make up more than 59% of blunt injuries to the eye.2 Sport activities such as basketball, baseball, water sports, and racquet sports account for most injuries.12 The extent of the damage to the eye is dependent upon the size, velocity, hardness of the object, and the amount of direct force placed on the eye. It is well established that penetrating injuries to the eye have a history of poorer prognosis than blunt injuries; however, serious blunt injuries can cause a significant intraocular disruption that may cause vision threatening injuries that will need to be recognized and referred.6
There are two major blunt ocular injury patterns that every emergency physician should be aware of: direct globe injury and orbital fracture. A direct blow to the globe is usually caused by smaller objects that can by-pass the bony orbital rim and strike the eye directly. Forces that directly hit the eye cause a rapid compression of the globe anterior-posteriorly, with corresponding expansion/dilation of the middle of the globe. The transmission of these forces produces extensive tearing and stretching forces that cause several types of injuries.
When the eye is struck the anterior chamber is compressed and the pupil is forced to dilate rapidly. The iris may tear, causing rupture of sphincter pupillae, which can lead to traumatic mydriasis. Force distributed directly to the peripheral iris can cause the iris to detach from its root (iridodialysis). A traumatic cataract may be seen when compressive forces damage the lens. Alternatively, the lens can be dislocated from the tearing of its insertion at the zonules. Signs of lens subluxation or dislocation include blurry vision and monocular diplopia. The eye should be carefully inspected for the presence of a hyphema. The importance of finding a hyphema on physical exam is that it is an indicator of serious ocular injury and that structures in the anterior as well as posterior segments are likely to be damaged.
As forces are distributed beyond the lens, injuries to the posterior segment are possible. The vitreous humor is attached to the retina and large stresses are able to detach the retina, leading to retinal detachment. The choroid may be stretched and torn; due to the vascular nature of this structure, choroidal rupture may occur and present as subretinal blood on funduscopic exam. Finally, commotio retinae may be seen in the setting of blunt trauma. This localized injury is identified as a whitish discoloration of the retina on funduscopic exam, which is caused by edema of the photoreceptor cells in the retina.
Significant complications may arise as a result of blunt trauma, including visual loss, disfiguration, secondary glaucoma, or traumatic optic neuropathy.51 General treatment for blunt ocular injuries include prophylactic eye shield, pain control, and ophthalmologic consultation. Guidelines for immediate referral include: globe rupture or suspected rupture, pupil defect with dense periorbital hematoma, hyphema, significant visual loss, or subconjunctival hemorrhage (may be masking globe rupture). Blunt injuries that may require ophthalmologic consultation within 24 hours include: minor reduced visual acuity, retinal hemorrhages, eyelid lacerations, and blow-out fractures.
Orbital Wall Fractures
Orbital fractures typically are caused by blunt impact from objects larger than the orbital rim or by impacts with flat surfaces, including falls and motor vehicle collisions. Seven bones of the skull form the orbit: the maxilla, zygoma, lacrimal, ethmoid, sphenoid, palatine, and frontal bones. The term "blow-out fracture" refers to buckling of the orbital floor following intense intraorbital pressure associated with blunt trauma, which often protects the eye from more serious internal injury.52 Entrapment of periorbital tissues, commonly including muscle, may occur as a result of phase differences of the movement of various orbital structures.53
The most common area to fracture is the orbital floor and medial wall due to the bone being thinner in these regions. Orbital roof fractures make up about 5% of injuries; children younger than age 7 are more prone to these injuries. The orbital roof is a very thin structure and frontal sinuses are not fully pneumatized until approximately age 7. Blunt trauma that impacts the upper portion of the orbit is dissipated by the frontal sinus. Orbital roof fractures may communicate with the brain and are more serious injuries; intracranial hemorrhage and leakage of cerebrospinal fluid may occur. Symptoms of an orbital fracture include periorbital ecchymosis, diplopia, hypoesthesia in V2 (lower eyelid, cheek and upper lip) distribution, pain with ocular movement (especially vertical movement), and intraorbital emphysema on plain radiograph. Symptoms of nausea and vomiting may be associated with inferior rectus entrapment and a poor outcome.54
Diagnosis is made by radiographic imaging, with CT scan being the preferred method. Plain radiographs of the orbits have a high false-negative or non-diagnostic rate ranging from 30-50%. MRI does provide increased soft tissue detail but is not as readily available as CT scan and bone windows are much better with CT scan compared to MRI. Bone cortex is not well demonstrated on MRI; thus, CT scan is far superior for the detection of orbital wall fractures. Orbital CT scan exposes the patient to similar radiation as head CT scan and orbital series of plain films (0.02-0.03 Gy).55
Once the diagnosis is made, two management schema are available: surgical or non-surgical. Specific findings that are of particular concern include diplopia (entrapment), restriction of extraocular movements, and enophthalmos > 2 mm, or a large posterior fracture. Careful ophthalmologic examination is essential, as 26% of patients with orbital fractures have associated ocular injuries.56 Most orbital fractures requiring surgical intervention are repaired within two weeks.52 The initial ophthalmologic management of orbital blow-out fractures includes treatment of the area with ice for 48 hours, nasal decongestants, broad spectrum antibiotics, elevation of head of bed while sleeping, avoidance of aspirin, avoidance of nose blowing, and ophthalmologic follow up.
Retrobulbar Hemorrhage
Retrobulbar hemorrhage is a true emergency that may require urgent intervention to preserve vision. This condition is effectively a compartment syndrome within the orbit and must be managed with the same, if not more, haste as that given to any other compartment syndrome. The time until the oxygen sensitive tissues of the optic nerve are irreversibly damaged is 60 minutes.57
This sight-threatening injury typically arises from orbital bleeding following a non-displaced fracture of the orbital wall. As with other compartment syndromes the natural progression of the condition is increased pressure around the globe, which results in reduced retinal perfusion, compression of ciliary vessels, stretching of the optic nerve, and exophthalmos.58 In most cases, development of retrobulbar hemorrhage occurs within a few hours of injury; however, case reports have shown that delayed retrobulbar hemorrhages can occur after the initial injury.59 Retrobulbar hemorrhage must be treated immediately if there is evidence of visual loss. Clinical signs include pain, proptosis, loss of vision, and presence of an afferent pupillary defect. In the unconscious patient, a tense, proptotic globe and a dilated pupil may be all that is apparent in the presence of a retrobulbar hemorrhage. CT scanning of the brain and orbits will help identify orbital wall fractures and retrobulbar blood if the diagnosis is in question. The management of a retrobulbar hemorrhage is surgical and emergent ophthalmologic consultation is warranted. Emergent lateral canthotomy and cantholysis can be performed in the emergency department to definitively treat the compartment syndrome. Incising the lateral canthus and the canthal tendon allow for egress of trapped retrobulbar blood, thereby decreasing the harmful pressure on the optic nerve. Other medical treatments of potential benefit include intravenous steroids, acetazolamide, and mannitol.
Eyelid Lacerations
Eyelid lacerations are commonly seen in pediatric patients, and are often due to falls, motor vehicle collisions, dog bites, or direct impact. Evaluation should assess potential globe injury and should include visual acuity, slit lamp examination, intraocular pressure measurement, and facial nerve function. Potential bony fractures should be ruled out by examination and radiographs, if indicated.
Simple eyelid lacerations can be successfully repaired in the emergency department. Debridement of devitalized tissue may be indicated. Superficial wounds not involving the lid margins can be closed with single or two-layer closures with small absorbable suture material. Slight eversion of wound edges should reduce scar formation. The dermal layer should not be under tension. Complex wounds, including tarsal plate involvement, canaliculi involvement, lid margin involvement, or scleral involvement require ophthalmologic consultation.60 Tetanus toxoid should be administered if indicated.
Child Abuse
Certain eye findings may be indicative of child abuse. Any injury which does not fit the characteristic pattern and severity of the described injury should heighten suspicion of possible abuse. Retinal hemorrhage occurs rarely with accidental head trauma and is commonly associated with shaken baby syndrome, particularly when seen in association with subdural hemorrhage, abnormal mental status, or seizures.61,62 Bilateral subconjunctival hemorrhages may be seen in infants as a result of asphyxia.63
Conclusions
Eye trauma is a common chief complaint among emergency department pediatric patients. Many eye injuries can be prevented by appropriate supervision of children's activities and the appropriate use of protective eyewear during sports. Detailed physical examination is indicated for the evaluation of pediatric eye trauma, and should include visual acuity, pupillary reactions, external examination, ocular motility, visual field testing, slit-lamp examination, fluorescein staining, intraocular pressure, and funduscopic examination.
Most patients with eye injuries can be managed as outpatients with ophthalmologic follow-up and appropriate medical management. Certain eye injuries warrant emergent ophthalmologic consultation, including hyphema, penetrating globe injury, suspected or known open globe injury, retrobulbar hematoma, or any eye injury resulting in significant visual loss.
References
1. McCaig L, Burt CW. National Hospital Ambulatory Medical Care Survey: 2002 Emergency Department Summary. Centers for Disease Control: Advance Data from Vital and Health Statistics: no. 340. Hyattsville, Maryland: National Center for Health Statistics, 2004. http://www.cdc.gov/nchs/data/ad/ad340.pdf. Accessed on 6/18/07.
2. Brophy M, Sinclair SA, Hostetler SG, et al. Pediatric eye injury-related hospitalizations in the United States. Pediatrics 2006;117:e1263-1271.
3. McGwin G, Owsley C. Incidence of emergency department-treated eye injury in the United States. Arch Ophthalmol 2005;123:662-666.
4. Kumar NL, Black D, McClellan K. Daytime presentations to a metropolitan ophthalmic emergency department. Clin Experiment Ophthalmol 2005;55:586-592.
5. MacEwen CJ, Baines PS, Desai PS. Eye injuries in children: the current picture. Br J Ophthalmol 1999;83:933-936.
6. MacEwen CJ. Ocular injuries. J R Coll Surg Edinb 1999;44:317-23.
7. Garcia TA, McGetrick BA, Janik JS. Ocular injuries in children after major trauma. J Pediatr Ophthalmol Strabismus 2005;42:349-54.
8. Garcia TA, McGetrick BA, Janik JS. Spectrum of ocular injuries in children with major trauma. J Trauma 2005;59:169-174.
9. Handler JA, Ghezzi KT. General ophthalmologic examination. Emerg Med Clin North Am 1995;13:521-538.
10. Datner EM, Jolly T. Pediatric ophthalmology. Emerg Med Clin North Am 1995;13:669-679.
11. Ervin-Mulvey LD, Nelson LB, Freely DA. Pediatric eye trauma. Pediatr Clin North Am 1983;30:1167-1183.
12. Rodriguez JO, Lavina AM, Agarwal A. Prevention and treatment of common eye injuries in sports. Am Fam Physician 2003;67:1481-1488.
13. Baumeister M, uhli-Hattenbach C, Luchtenberg M. Corneal ulcer caused by a wooden foreign body in the upper eyelid 6 months after minor injury. Ophthalmologica 2006;220:397-399.
14. Caca I, Ari S, Ulu K, et al. Bee sting of the cornea: a case study and review of the literature. Ann Ophthalmol 2006;38:77-79.
15. Turner A, Rabiu M. Patching for corneal abrasion. Cochrane Database Syst Rev 2006;(2):CD004764.
16. Kaiser PK. A comparison of pressure patching versus no patching for corneal abrasions due to trauma or foreign body removal. Corneal Abrasion Patching Study Group. Ophthalmology 1995;102:1936-1942.
17. Wilson SA, Last A. Management of corneal abrasions. Am Fam Physician 2004;70:123-128.
18. Michael JG, Hug D, Dowd MD. Management of corneal abrasions in children: a randomized clinical trial. Ann Emerg Med 2002;40:67-72.
19. Calder LA, Balusubramanian S, Fergusson D. Topical nonsteroidal anti-inflammatory drugs for corneal abrasions: meta-analysis of randomized trials. Acad Emerg Med 2005;12;467-473.
20. Weaver CS, Terrell KM. Evidence-based emergency medicine. Update: do ophthalmic nonsteroidal anti-inflammatory drugs reduce the pain associated with simple corneal abrasions without delaying healing? Ann Emerg Med 2003;41:134-140.
21. Benson WH, Snyder IS, Granus V, et al. Tetanus prophylaxis following ocular injuries. J Emerg Med 1993;11:677-83.
22. Mukherjee P, Sivakumar A, et al. Tetanus prophylaxis is superficial corneal abrasions. Emerg Med J 2003;20:62-64.
23. Gallin PF. Pediatric Ophthalmology: A Clinical Guide. New York: Thieme Medical. 2000.
24. Webb LA. Manual of Eye Emergencies: Diagnosis and Treatment. Second Ed., London: Butterworth-Heinemann. 2004
25. Gopal L, Banker AS, Deb N, et al. Management of glass intraocular foreign bodies. Retina 1998;18:213-20.
26. Garg SJ, Benson W, Fineman M, et al. Bone from an orbital floor fracture causing an intraocular foreign body. Am J Ophthalmol 2005;139:543-545.
27. Smith D, Wrenn K, Stack LB. The epidemiology and diagnosis of penetrating eye injuries. Acad Emerg Med 2002;9:209-213.
28. Woodcock MG, Scott RA, Huntbach J, et al. Mass and shape as factors in intraocular foreign body injuries. Ophthalmology 2006;113: 2262-2269.
29. Narang S, Gupta V, Simalandhi P, et al. Pediatric open globe injuries. Visual outcome and risk factors for endophthalmitis. Indian J Ophthalmol 2004;52:29-34.
30. Lubeck D. Penetrating ocular injuries. Emerg Med Clin North Am 1988;6:127-146.
31. McGimpsey SJ, Rankin SJ. Presentation of intraocular foreign body 25 years after the event. Clin Experiment Ophthalmol 2005;33:665-666.
32. Ghazi-Nouri SM, Vote BJ, Sullivan PM. Periorbital ecchymosis as a sign of perforating injury of the globe. Clin Experiment Ophthalmol 2005;33:194-196.
33. Joseph DP, Pieramici DJ, Beauchamp NJ. Computed tomography in the diagnosis and prognosis of open-globe injuries. Ophthalmology 2000;107:1899-1906.
34. Shiver SA, Lyon M, Blaivas M. Detection of metallic ocular foreign bodies with handheld sonography in a porcine model. J Ultrasound Med 2005;24:1341-1346.
35. Turkcuoglu P, Aydogan S. Intracranial foreign body in a globe-perforating injury. Can J Ophthalmol 2006;41:504-505.
36. Brandt MT, Haug RH. Traumatic hyphema: a comprehensive review. J Oral Maxillofac Surg 2001;59:1462-1470.
37. Saunte JP, Saunte ME. 33 cases of airsoft pellet ocular injuries in Copenhagen, Denmark, 1998-2002. Acta Ophthalmol Sccand 2006;84:755-758.
38. Listman DA. Paintball injuries in children: more than meets the eye. Pediatrics 2004;113:e15-18.
39. Rocha KM, Martins EN, Melo LA Jr, et al. Outpatient management of traumatic hyphema in children: prospective evaluation. J AAPOS 2004;8:357-361.
40. Fong LP. Secondary hemorrhage in traumatic hyphema. Predictive factors for selective prophylaxis. Ophthalmology 1994;101:1583-1588.
41. Walton W, Von Hagen S, Grigorian R, et al. Management of traumatic hyphema. Surv Ophthalmol 2002;47:297-334.
42. Ikeda N, Hayasaka S, Hayasaka Y, et al. Alkali burns of the eye: effect of immediate copious irrigation with tap water on their severity. Ophthalmologica 2006;220:225-8.
43. Kuckelkorn R, Schrage N, Keller, G et al. Emergency treatment of chemical and thermal eye burns. Acta Ophthalmol Scand 2002;80:4-10.
44. Herr RD, White GL, Bernhisel K, et al. Clinical comparison of ocular irrigation fluids following chemical injury. Am J Emerg Med 1991; 9:228-231.
45. Saidinejad M, Burns MM. Ocular irrigant alternatives in pediatric emergency medicine. Pediatr Emerg Care 2005;21:23-26.
46. Witsaman RJ, Comstock RD, Smith GA. Pediatric fireworks-related injuries in the United States: 1990-2003. Pediatrics 2006;118:296-303.
47. Hammerton ME. Burns to the eye: an overview. Aust Fam Physician 1995;24:998-1003.
48. Hammerton ME. Management of ocular burns. Aust Fam Physician 1995;24:1006-1010.
49. Spencer T, Hall AJ, Stawell RJ. Ophthalmologic sequelae of thermal burns over ten years at the Alfred Hospital. Ophthalmic Plast Reconstr Surgery 2002;18:196-201.
50. Bouchard CS, Morno K, Perkins J, et al. Ocular complications of thermal injury: a 3-year retrospective. J Trauma 2001;50:79-82.
51. Wang BH, Robertson BC, Girotto JA, et al. Traumatic optic neuropathy: a review of 61 patients. Plast Reconstr Surgery 2001;107:1755-1764.
52. Brady SM, McMann MA, Mazzoli RA, et al. The diagnosis and management of orbital blowout fractures: update 2001. Am J Emerg Med 2001;19:147-154.
53. Fujino T, Makino K. Entrapment mechanism and ocular injury in orbital blowout fracture. Plast Reconstr Surg 1980;65:571-576.
54. Cohen SM, Garrett CG. Pediatric orbital floor fractures: nausea/vomiting as signs of entrapment. Otolaryngol Head Neck Surg 2003;129:43-47.
55. Mauriello JA, Lee HJ, Nguyen I. CT of soft tissue injury and orbital fractures. Radiol Clin North Am 1999;37:241-252.
56. Cook T. Ocular and periocular injuries from orbital fractures. J Am Coll Surg 2002;195:831-34.
57. Perry M, Dancey A, Mireskandari K, et al. Emergency care in facial trauma — a maxillofacial and ophthalmic perspective. Injury 2005;36:875-896.
58. Gerbino G, Ramieri G A, Nasi A. Diagnosis and treatment of retrobulbar haematomas following blunt orbital trauma: a description of eight cases. Int J Oral Maxillofac Surg 2005:34;127-131.
59. Ghufoor K, Sandhu G, Sutcliffe J. Delayed onset of retrobulbar haemorrhage following severe head injury: a case report and review. Injury 1998:29;139-141.
60. Chang EL, Rubin PA. Management of complex eyelid lacerations. Int Ophthalmol Clin 2002;42:187-201.
61. Pierre-Kahn V, Roche O, Dureau P, et al. Ophthalmologic findings in suspected child abuse victims with subdural hematomas. Ophthalmology 2003;110:1718-1723.
62. Bechtel K, Stoessel K, Leventhal JM, et al. Characteristics that distinguish accidental from abusive injury in hospitalized young children with head trauma. Pediatrics 2004;114:165-168.
63. Spitzer SG, Luorno J, Noel LP. Isolated subconjunctival hemorrhages in nonaccidental trauma. J AAPOS 2005;9:53-56.
Eye trauma is a common chief complaint among emergency department (ED) pediatric patients.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.