Diverticulitis: A New Perspective on an Old Disease
Diverticulitis: A New Perspective on an Old Disease
Authors: Grant Lipman, MD, Clinical Assistant Professor of Surgery, Associate Director, Wilderness Medicine Fellowship, Division of Emergency Medicine, Stanford University School of Medicine; and Amritha Raghunathan, MD, Stanford/Kaiser Emergency Medicine.
Peer Reviewer: Moira Davenport, MD, Department of Emergency Medicine, Department of Orthopaedic Surgery, Allegheny General Hospital, Pittsburgh, PA.
Introduction
Abdominal pain comprises 5-10% of all emergency department (ED) visits each year. 1
Diverticular disease is extremely common, with incidences of 5-10% in patients older than age 45 and approximately 80% in those older than age 85.2,3 In those with diverticuli, 10-25% will have at least one episode of diverticulitis, with a risk of recurrence of 7-35%.3,4 Diverticulitis ranges from patients with small, confined pericolonic abscesses (Hinchey stage I), to fecal peritonitis secondary to free rupture of a diverticulum or peridiverticular abscess (Hinchey stage IV).3,5 Other complications of advanced diverticulitis (often termed "complicated diverticulitis") include abscess, fistula (colovesicular, colovaginal, and colocutaneous), stricture, and obstruction. In fact, diverticulitis is the cause for 10% of all bowel obstructions.4
Undifferentiated abdominal pain is a diagnostic challenge for the acute care physician. Diverticulitis can be a particular challenge as it appears in many forms. Atypical symptoms such as changes in bowel habits, urinary tract symptoms, or even right-sided pain can occur. With the multiple treatment and imaging modalities available, questions arise about how to best approach a patent with suspected diverticulitis. This article reviews the recent literature to discuss varied clinical characteristics of diverticulitis, outcomes after medical and surgical treatment, and comparisons of differing diagnostic methods to assist the physician in diagnosing and treating this common disease process.
Epidemiology, management, and outcomes after treatment
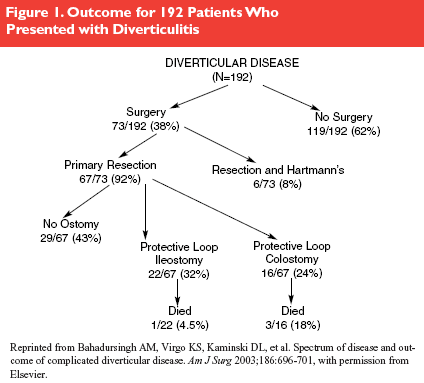
Source: Bahadursingh AM, Virgo KS, Kaminski DL, et al. Spectrum of disease and outcome of complicated diverticular disease. Am J Surg 2003;186:696-701.
This retrospective review analyzes the clinical presentation, extent of disease, management, and outcome for all patients diagnosed with diverticulitis over a 9-year period. The authors studied 192 patients and found the mean age was 61 years, with ages ranging between 28 and 90; females comprised 59% of the patients. Most patients reported symptoms lasting a few days, with an average of 14 days; however, some reported as little as 1 day of symptoms and others as many as 270 days of ongoing symptoms. The majority of patients (61%) had a history of diverticulitis. Two-thirds of patients had a CT scan of the abdomen and pelvis, approximately one-third had a colonoscopy, and one-fifth had a contrast enema. No patients in the study had an ultrasound evaluation. The abnormalities on CT scan included simple diverticulitis (37% of patients), diverticulosis without inflammation (15%), and complicated diverticulitis (27% total, with 16% having an abscess, 10% free air, and 1% a fistula). Of the patients with abscesses, 24% underwent percutaneous drainage and 16% had transrectal drainage.
Fifty-six percent of patients who attempted conservative treatment did not require any further intervention. Thirty-eight percent of patients required surgery, and all received a colon resection. Other than simple diverticulitis, they found a localized abscess in 22%, purulent/feculent peritonitis in 17%, and a phlegmon in 14%. Seven percent were in fact found to have a carcinoma. Ninety-two percent of patients had a primary anastomosis, with 56% of patients also having a protective stoma (ileostomy or colostomy) formed. Post-surgical morbidity was 15%, with post-operative infections being the most common cause; mortality was 2%. (See Figure 1.)
 |
Commentary
Diverticulitis is traditionally thought of as a disease of those older than age 60. However, it is important to realize that while the mean age in this large study was just above 60, people younger than age 30 also contracted the disease. In addition, while patients traditionally are thought to present early in the disease course, 2% of their patients had experienced symptoms for more than 100 days. The physician provider should maintain a high level of suspicion regardless of the age of the patient or how long the symptoms have been ongoing. The study authors postulate that as both colonoscopy and barium enema are relatively contraindicated in patients who are at risk for perforation, these imaging techniques were used only in those suspected of having an uncomplicated disease process. Therefore, a CT scan is the only technique utilized in those suspected of having a complicated disease process. The study shows that there was good concordance between the CT scan results and intraoperative findings, as well.
The authors mention that only 56% of those treated conservatively managed to avoid further intervention. However, they do not report how or why the conservative treatment failed or about the success of the percutaneous and transrectal interventions. This would be helpful information for both medical and surgical practitioners. One further critique is that all data from patients initially diagnosed with diverticulitis who on further investigation had an alternate diagnosis were included. For example, included in the study were: the data of the 15% of patients with simple non-inflammatory diverticulosis on CT scan, the 21% with no abnormalities seen on CT scan, and the 7% with carcinomas. Therefore, the epidemiologic information gathered can only be used as a useful approximation.
In the past, practitioners often waited to refer patients to a surgeon until after multiple episodes of diverticulitis because of the high mortality and morbidity rates (approximately 10% around World War II). However, advances in surgical devices currently allow more people to avoid a permanent colostomy. This study confirms that the majority of patients had a primary anastomosis, and at the most, a protective ileostomy. The current low morbidity and mortality of surgical intervention is important to keep in mind, so acute care providers should not hesitate to refer patients for a colorectal surgical evaluation after their initial diverticulitis attack.
Clinical factors in patients younger than age 40
Source: Marinella M, Mustafa M. Acute diverticulitis in patients 40 years of age and younger. Am J Emerg Med 2000;18:140-142.
With the majority of diverticulitis patients older than age 60, most research focuses on that age group. This study attempted to determine clinical criteria that increase the likelihood of a diagnosis of diverticulitis in the younger population. They conducted a retrospective review of 21 patients younger than age 40 who had been diagnosed with acute diverticulitis. The authors note that the admitting diagnosis was diverticulitis in 83% of patients with left lower quadrant tenderness but was mistaken to be appendicitis in 66% of patients with right lower quadrant tenderness.
The authors recommend that clinicians have a high suspicion for diverticulitis in young patients with nausea, fever, tachycardia, and leukocytosis, and that they consider obtaining a CT scan for increased diagnostic accuracy.
Commentary
Diverticulitis is a relatively rare diagnosis in the under-40 age group. While studies done in the 1960s showed that less than 5% of people younger than age 40 had diverticula, recent epidemiological studies have shown the incidence to be between 12-30%.6 Therefore, we can expect a larger number of young adults to present with diverticulitis in the future. It is crucial to avoid a delay in diagnosis, which may lead to complications and unnecessary morbidity.
While it is useful to remember atypical causes of abdominal pain in patients younger than age 40, the common clinical characteristics used as a guideline do not differentiate diverticulitis from other intra-abdominal inflammatory processes like appendicitis. This is a retrospective review, and data from only 21 patients was analyzed. As appendicitis was the most common alternate diagnosis given and nausea, fever, tachycardia, and leukocytosis are very common findings in appendicitis, it is unclear how useful these results will be. Moreover, another similar study by Minardi et al in which data from 22 young patients with diverticulitis was analyzed, found that only 45% had nausea and only 36% had fever.6 A larger study specifically comparing those with diverticulitis and other common intra-abdominal inflammatory processes will be of use to clinicians attempting to make the correct clinical diagnosis.
Clinical differentiation of right-sided diverticulitis
Source:Shin JH, Son BH, Kim H. Clinically distinguishing between appendicitis and right-sided colonic diverticulitis at initial presentation. Yonsei Med J 2007;48:511-516.
Right-sided colonic diverticulitis is particularly difficult to distinguish from other intra-abdominal inflammatory processes like appendicitis. Although left-sided diverticulitis is more common in the western world, right-sided diverticulitis is very common in the Asian population. The majority of disease caused by diverticulitis in Asians occurs in the cecum and ascending colon. It also presents at a younger age, often in the 20-40 year age group. As appendicitis also is common in this age group, it is very difficult to distinguish the two processes. Studies have found that a large percentage of patients with right-sided diverticulitis are misdiagnosed with acute appendicitis.7 This Korean retrospective study reviewed the medical records of 450 patients. Of these patients, 92 had right-sided diverticulitis. Simple appendicitis was diagnosed in 268 patients, and 90 patients had perforated appendicitis. They found that 7% of patients who were initially diagnosed with appendicitis were eventually found to have diverticulitis.
They found that prodromal symptoms such as fever, chills, nausea, and vomiting occurred less frequently in the diverticulitis group. The incidence of right-lower quadrant pain without rebound tenderness was significantly higher in those with diverticulitis. The maximum point of tenderness was lateral to McBurney's point in a much larger percentage of patients with diverticulitis than in those with appendicitis. The median white blood cell count was significantly lower in those with diverticulitis than in those with appendicitis.
Commentary
This study provides clinical criteria favoring either a diagnosis of appendicitis or right-sided diverticulitis. This, however, was a retrospective trial, and it was conducted in one hospital in Korea. Therefore, the general applicability of the results is debatable. A prospective trial that confirms or validates these findings would be ideal in forming clinical decision rules on this topic. At this point, our recommendation would be to have a high index of suspicion for right-sided diverticulitis, particularly in the Asian population, to avoid a significant delay in diagnosis or frank misdiagnosis. If any of the factors above are present or the clinical picture is at all suggestive of anything but appendicitis, the clinician is encouraged to obtain a CT scan for confirmation.
Diagnostic methods
Source: Liljegren G, Chabok A, Wickbom M. Acute colonic diverticulitis: a systematic review of diagnostic accuracy. Colorectal Dis 2007;9:480-488.
This recent meta-analysis examined the literature on all diagnostic techniques utilized for acute diverticulitis including, ultrasound (US), CT scanning, barium enema (BE), and MRI. A search of the PubMed, EMBASE, and Cochrane Library databases found 49 articles on this topic; of these, 29 studies were excluded for irrelevant data. The authors classified the level of evidence based on criteria of the Centre for Evidence-Based medicine in England. The authors found that only one study that evaluated CT scanning and US reached the level of evidence 1b. There were also two US studies and one study on MRI that reached the level 2b. All the remaining studies were at the level 4.
Commentary
There has been a lot of debate on which diagnostic imaging tool is the best for diagnosing colonic diverticulitis. This article discusses the fact that there have not been large, well-designed studies evaluating all four of the common methods of diagnosis. While that would certainly be helpful, the overall consensus in the literature appears to be that CT scan is the gold standard for diagnosis of diverticulitis.
CT scanning is noninvasive, fast, allows the visualization of the entire abdomen and pelvis, and offers the potential for percutaneous drainage of abscesses, which could potentially avoid surgical drainage.7 A large, prospective trial by Rao et al examined the role of the CT scan in 150 patients with diverticulitis. A scan of the abdomen and pelvis using rectal contrast had a sensitivity of 97%, specificity of 100%, positive predictive value of 100%, and negative predictive value of 98%.8 A similar study by Kircher that included 312 patients showed equally good numbers, with the sensitivity actually increasing to 99% in their study.9
Therefore, it is our recommendation that CT scanning should continue to be the diagnostic method of choice based on the high reliability and accuracy in the detection of diverticulitis and its complications.
Ultrasound evaluation
Source:Zielke A, Hasse C, Nies C, et al. Prospective evaluation of ultrasonography in acute colonic diverticulitis. Br J Surg 1997;84:385-388.
The validity of ultrasonography to evaluate suspected diverticulitis was investigated in this well-designed prospective trial. The diagnostic accuracy and clinical value of ultrasonography when performed by surgical residents was assessed; 143 patients were included in the study. There was a strong clinical suspicion of acute colonic diverticulitis in all of these patients. The surgical residents involved had all received standardized training in abdominal ultrasound, including supervised examinations. They conducted ultrasound examinations on all 143 patients, and the results were compared to the patient's final diagnosis at the end of their hospital stay. A hypoperistaltic segment with hypoechogenic mural thickness that was poorly compressible in transverse view was considered diagnostic of diverticulitis.
The surgical residents' results were compared to the patients' ultimate discharge diagnosis. These bedside ultrasound tests were able to diagnose diverticulitis in 62 of the 74 patients who were ultimately diagnosed with diverticulitis. Ultrasound had a sensitivity of 84% and a specificity of 93%. There was a false-positive result in 5 patients and a false-negative result in 12 patients. All 5 false-positive patients had colonic disease; two were diagnosed with colitis, two with carcinoma, and another with suppurative pyosalpingitis with involvement of the sigmoid colon. The accuracy of clinical evaluation alone on admission was worse than the ultrasound, with a sensitivity of 82% and a specificity of 55%.
Commentary
Ultrasound is a non-invasive, non-irradiating, cost-effective, and quick diagnostic imaging technique that can be done at the bedside by any trained practitioner.7,10 The sensitivity and specificity values shown by the group here are quite high and further suggest the potential value of ultrasound as a preliminary diagnostic technique in these patients.
It is of note that the authors utilized surgical residents, not ultrasound technicians, to do this study. While the technicians are clearly the most experienced and well suited to do the imaging study, they are not available all the time at most hospitals. Indeed, some small hospitals and rural centers may not even have an ultrasound department. Therefore, it is an important finding that resident doctors with little formal ultrasound instruction were able to produce reliable and clinically helpful results. Another recent article found that emergency medicine practitioners also were able to recognize what they called the pseudo-kidney sign and correlate it with a diagnosis of diverticulitis.11 This opens the door for a quick imaging option in the hands of all acute care practitioners interested in another diagnostic tool for diverticular abdominal pain.
Clinical and imaging prognostic indicators
Source: Shen SH, Chen JD, Tiu CM, et al. Colonic diverticulitis diagnosed by computed tomography in the ED. Am J Emerg Med 2002;20:551-557.
This paper retrospectively reviewed the clinical information and CT scan results from 38 patients who had been diagnosed with colonic diverticulitis in the ED. The authors found that 87% had abdominal pain and 82% had leukocytosis. However, only 34% had fevers/chills, 16% had nausea/vomiting, and only 11% had diarrhea.
The imaging data revealed that 63% of patients had left-sided diverticulitis, and the remaining 37% patients had right-sided diverticulitis. There was evidence of abscess formation in 34% of the patients, and 92% of those had left-sided diverticulitis. Complications found included 26% with free air, 3% (1 patient) with a colovesical fistula, and 5% (2 patients) with intestinal obstruction.
Only 40% had a recorded impression of diverticulitis prior to ordering the CT scan. Other impressions given as the reason for obtaining the CT scan included peritonitis, appendicitis, colon cancer, intestinal obstruction, and ischemic bowel disease. Half the patients received surgical treatment and the remaining half were treated conservatively. The authors do not compare these groups and their clinical and imaging factors or prognosis in the study.
There was a 16% mortality rate in this cohort. The clinical information and imaging results from these patients were directly compared against the others to determine prognostic factors. The authors found 3 parameters were associated with poor prognosis: older age (P=0.016), abscess formation (P=0.012), and the presence of free air (P=0.003). All the patients who expired had left-sided diverticulitis, but this was not statistically significant.
Comparisons between right-sided and left-sided diverticulitis showed that age, colonic length, and the presence of free air were all significantly different statistically between the two groups. The left-sided group was significantly older (mean age 70 years vs. 53 years in the right-sided group), had a much longer average involved length (15 cm vs. 7 cm), and had all the scans showing free air.
Commentary
While this study was limited by its small sample size, the paper highlights multiple useful facts about diverticulitis. The overall percentage of CT scans done was fairly low. However, in examining the impression prior to ordering the scan, it shows that in the majority of cases, diverticulitis was not the leading diagnosis at the time. This shows the efficacy of CT scanning in correctly diagnosing diverticulitis.
The authors also reconfirm that complicated diverticulitis, with abscess formation and free air, has a worse prognosis. They also show a few pertinent facts about the difference in presentation between left- and right-sided diverticulitis. Those findings suggest that we should have a high index of suspicion for and attempt to expedite the treatment of patients with left-sided diverticulitis as that group had significantly more advanced disease on presentation.
It would have been of benefit if the paper had included the treatment modality in the analysis. While 50% were treated surgically and the rest underwent conservative management, the authors do not reveal the mortality of each group. They also did not reveal how many of those patients had complicated diverticulitis (such as abscess formation, free air, a fistula or obstruction) and how many had simple diverticulitis.
Non-operative management
Source: Kaiser AM, Jiang JK, Lake JP, et al. The management of complicated diverticulitis and the role of computed tomography. Am J Gastroenterol 2005;100:910-917.
The authors sought to define the optimal management for intermediate stages of diverticulitis as well as to determine if CT evidence of a diverticular abscess has a prognostic impact. Patients with evidence of diverticulitis complicated by localized abscesses, Hinchey stages 1b and II, were included in the study.
A total of 511 patients who were admitted for acute diverticulitis over a 10-year period were retrospectively reviewed. Of this group, 99 (19%) had CT scan evidence of an abscess (74 of them had stage 1b disease and 25 had stage II disease).
Of those 99 patients, the findings included:
- Sixteen percent of patients had CT-guided drainage. The average size of abscesses that were drained was 7.1 cm. Drainage was successful in 15/16 (94%) of cases, with one patient requiring an emergency two-stage Hartmann's resection.
- After CT-guided drainage, 16% of patients had an elective resection a few months after the initial attack. None had a recurrence in the meantime. Of the others, 13% of pericolic abscesses (Hinchey stage 1b) had a recurrence, while 41% of those with a pelvic abscess (Hinchey stage II) did. Overall, 40% of those patients developed another abscess, and 20% had a fistula. The mean interval to the onset of the recurrence was 4.7 +/- 5.9 months.
- The remaining 84% of patients had abscesses that were not amenable to CT-guided drainage. They were treated with antibiotics, which was successful in 58% of those with stage Ib disease and 24% of those with stage II disease. However, 19% of those with stage I disease and 32% of those with stage II disease required an urgent resection.
- Patients requiring an urgent resection generally did well, with a mortality of 1.1%. However, 45% of these urgent surgeries were two-stage procedures with the patient receiving an ostomy. Furthermore, the stoma closure rate was only 64%, and the mean closure time was 6.6 months after the primary operation.
- All of the elective resections (scheduled after an episode of complicated diverticulitis) were one-stage procedures and many were done laparoscopically.
Commentary
This paper is extremely useful as it targets two vital questions: 1) do CT findings affect prognosis; and 2) what is the best treatment protocol for those with localized diverticular abscesses? Traditionally, the treatment modalities for the stage I and stage IV patients are well laid out. However, there has been controversy regarding the best protocol for those in the stage 1b and II groups. These data are compelling as they show a high recurrence rate, particularly for those with pelvic abscesses, even after CT-guided drainage. The authors also show that a large percentage of those undergoing an urgent surgery are forced to have an ostomy, and that 36% of the time it ends up being a permanent ostomy.
While this is one of the largest series on diverticulitis in the literature, their numbers in the subcategories are still small and they have not been able to conduct statistical analyses in all categories. A follow-up randomized, controlled trial should be conducted to further define the best treatment modality for those with stage Ib and II disease. However, until that is done, this group has given us a basis for defining a new protocol proceeding with elective resection for those with stage Ib and II disease after initial treatment that includes both CT-guided drainage (if possible) and antibiotic therapy (particularly if CT-guided drainage is not possible).
Conclusion
Diverticulitis is an extremely common disorder that can often present a challenge for the acute care practitioner. Recent research has given us a new perspective on the disease, including updated epidemiologic data regarding young patients with diverticulitis and specific clinical factors that should increase our index of suspicion for diverticulitis (both left and right-sided diverticulitis). There also have been recent advances in minimally invasive therapeutic options, including CT-guided percutaneous drainage of abscesses. This has resulted in a significant decrease in overall morbidity and mortality of advanced disease.
The diagnosis of diverticulitis is suggested in patients with left lower quadrant abdominal pain, particularly if they have a history of known diverticuli or prior episodes of diverticulitis. A change in bowel habits with either diarrhea or constipation predominating also is common. Dysuria, urinary frequency, and urgency may occur if the colonic inflammation is close to the bladder. Other symptoms and signs of advanced disease include pneumaturia, fecaluria, or peritoneal signs on exam.7 One recent prospective study12 on the clinical presentation of diverticulitis and a comparison to nonspecific abdominal pain showed that patients with diverticulitis had a longer duration of symptoms, as well as laboratory evidence of inflammation. Isolated left abdominal tenderness also was more common, while right-sided tenderness was more common in non-specific abdominal pain.
Given the spectrum of disease, it is important to have a high index of suspicion for diverticulitis, particularly in the elderly population. Even in the under-40 age group, while a smaller percentage of those patients have diverticuli, diverticulitis is a known entity. Marinella et al report that the suspicion for diverticulitis should be high in any young patient with a clinical presentation consistent with an intra-abdominal inflammatory process.13 Nausea, fever, tachycardia, and leukocytosis were the most common presenting findings in this study. The authors encouraged acute care practitioners to consider a CT scan to confirm the diagnosis in patients with such a constellation of symptoms.
Diverticulitis occurs in the sigmoid and descending colon (associated with left lower quadrant pain) in 85%.7 However, right-sided diverticulitis also occurs, and it can often be difficult to distinguish appendicitis from right-sided diverticulitis. The comparison of the clinical presentation and laboratory values of those diagnosed with appendicitis and diverticulitis found that prodromal factors like fever, chills, nausea, and vomiting, as well as laboratory values denoting an inflammatory process, were decreased and less frequently seen in diverticulitis.14 Therefore, it is again important to have a high clinical suspicion, especially in people of Asian descent, and to consider a CT scan if necessary.
Diverticuli can be demonstrated by both colonoscopy and contrast enema, but their presence alone does not confirm or rule out diverticulitis. The same ambiguity is seen in the presence of a stricture or extraluminal compression, which also may raise the possibility of malignancy.3 Ultrasound can correlate findings (such as a hypoechoic, thickened colonic segment, diverticula, and increased echogenicity surrounding the diseased colon) with patient factors such as pain on compression of the affected region. It also is non-invasive, relatively inexpensive, and widely available. Critiques of ultrasonography include operator-dependency and that intraabdominal contents may be inadequately visualized due to patient's intolerance of external pressure or body habitus.3 Multiple studies have shown that ultrasound can play an important role in the initial evaluation of a patient with undifferentiated abdominal pain, and Zielke et al present a well-designed prospective trial that found an ultrasound evaluation has a high sensitivity and specificity and could be utilized by doctors other than radiologists.15
The imaging modality of choice is CT scanning, as it is non-invasive, and allows the visualization of diverticula, inflammation of the pericolic fat, thickening of the bowel wall, or an intraabdominal abscess while ruling out alternative intraabdominal diagnoses.3,7
Patients with simple diverticulitis should be given 7-10 days of antibiotics, traditionally covering both gram-negative and anaerobic bacteria.3,7 Patients with abscesses can be percutaneously drained (with radiologic guidance) or drained surgically. The data on percutaneous drainage is very favorable, and CT-guided drainage is the standard treatment for abscesses of more than 5 cm in diameter (smaller abscesses should resolve with antibiotic treatment alone).3 Early surgical intervention is essential in those with frank peritonitis secondary to perforation and fecal contamination of the peritoneal cavity.7 The mortality and morbidity has decreased considerably over the last few decades and the percentage of patients who require an ostomy also is decreasing due to early intervention and the success of less-invasive or percutaneous intervention.16 Therefore, all patients should be referred to a colorectal surgeon after their first episode of diverticulitis.
Given the rapid aging of the population and the prevalence of diverticulitis, it is promising that recent trials have given us a new perspective on alternative imaging modalities and therapeutic options to assist in the diagnosis and treatment of this disease.
References
1. Clinical policy: critical issues for the initial evaluation and management of patients presenting with a chief complaint of non-traumatic acute abdominal pain. Ann Emerg Med 2000;36:406-415.
2. Rodkey GV, Welch CE. Diverticulitis of the colon: evolution in concept and therapy. Surg Clin North Am 1965;45:1231-1243.
3. Boulos PB. Complicated diverticulosis. Best Pract Res Clin Gastroenterol 2002;16:649-662.
4. Buckley O, et al. Computed tomography in imaging of colonic diverticulitis. Clin Radiol 2004;59:977-983.
5. Hinchey EJ, et al. Treatment of perforated diverticular disease of the colon. Adv Surg 1978;12:85-109.
6. Minardi AJ, et al. Diverticulitis in the young patient. Am Surg 2001;67:458-461.
7. Ferzoco LB, et al. Acute diverticulitis. N Engl J Med 1998;338:1521-1526.
8. Rao PM, et al. Helical CT with only colonic contrast material for diagnosing diverticulitis: prospective evaluation of 150 patients. AJR Am J Roentgenol 1998;170:1445-1449.
9. Kircher MF, et al. Frequency, sensitivity, and specificity of individual signs of diverticulitis on thin-section helical CT with colonic contrast material: experience with 312 cases. AJR Am J Roentgenol 2002;178:1313-1318.
10. Parks TG, et al. Limitations of radiology in the differentiation of diverticulitis and diverticulosis of the colon. Br Med J 1970;2:136-138.
11. Baker JB, et al. Diagnosis of diverticulitis by bedside ultrasound in the Emergency Department. J Emerg Med 2006;30:327-329.
12. Laurell H, et al. Acute diverticulitisclinical presentation and differential diagnostics. Colorectal Dis 2007;9:496-501; discussion 501-502.
13. Marinella M, Mustafa M. Acute diverticulitis in patients 40 years of age and younger. Am J Emerg Med 2000;18:140-142.
14. Shin JH, et al. Clinically distinguishing between appendicitis and right-sided colonic diverticulitis at initial presentation. Yonsei Med J 2007;48:511-516.
15. Zielke A, et al. Prospective evaluation of ultrasonography in acute colonic diverticulitis. Br J Surg 1997;84:385-388.
16. Bahadursingh AM, et al. Spectrum of disease and outcome of complicated diverticular disease. Am J Surg 2003;186:696-701.
17. Liljegren G, et al. Acute colonic diverticulitis: a systematic review of diagnostic accuracy. Colorectal Dis 2007;9:480-488.
18. Shen SH, et al. Colonic diverticulitis diagnosed by computed tomography in the ED. Am J Emerg Med 2002;20:551-557.
19. Kaiser AM, et al. The management of complicated diverticulitis and the role of computed tomography. Am J Gastroenterol 2005;100:910-917.
Abdominal pain comprises 5-10% of all emergency department (ED) visits each year.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
