2007 Salary Survey Results: ED manager salary 'dam' begins to break, as hospitals respond to shortages
ED manager salary 'dam' begins to break, as hospitals respond to shortages
In last year's report on the 2006 ED Management Salary Survey, we noted that while there was a shortage of ED nurses and physicians, compensation for ED directors and managers had failed to reflect that shortage. This year, however, experts tell us that hospital administrators have had to face the undeniable realities of supply and demand, and they — albeit grudgingly — are opening their pockets a bit more.
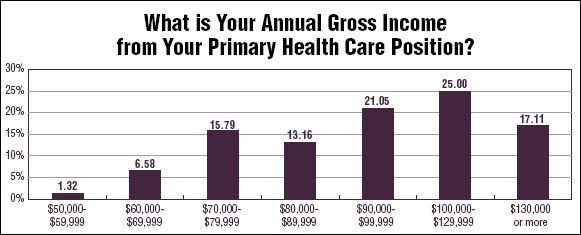
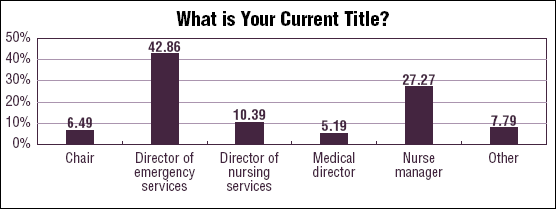
According to the 2007 EDM Salary Survey results, 50.65% of the respondents received a raise between 1% and 3%, compared with only 38.98% the previous year. In addition, 29.87% saw an increase of between 4% and 6%, compared with 27.12% last year. Only 11.69% of the respondents saw no change in their salary at all, compared with 15.25% in the 2006 survey. And, while only 15% of survey respondents in 2006 reported annual gross income of between $90,000 and $99,999, this year 21.05% said their income fell with that range. The percentages for those making $100,000-$129,999 also rose, from 21.67% to 25%. Those making over $130,000 remained virtually unchanged. (See chart, below.) For the 2007 report, 856 surveys were disseminated. There were 77 responses, for a response rate of. 9%. Of the respondents, 42.86% said they held the title of director of emergency services, and 27.27% said they were nurse managers. (See chart, below.)
 |
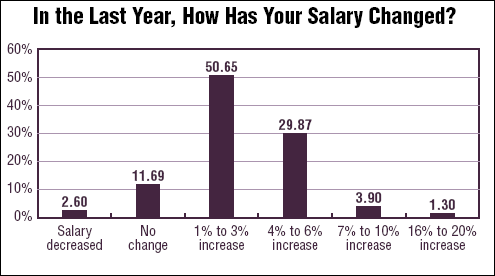 |
 |
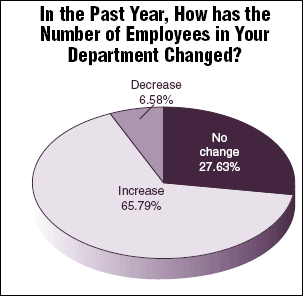
"Clearly, compensation is rising with the complexity of running an ED," says Mike Williams, MPA, HAS, president of The Abaris Group, a Walnut Creek, CA-based health care consulting firm specializing in emergency services. "With higher demand, but, in many cases with the same capacity as you had in the past, leaders are forced to work harder and smarter." ED managers also have larger staffs to manage: The survey indicated that 65.79% of respondents said the number of employees in their department had increased in the last year. (See chart, below.)
 |
At least one expert is not surprised at the survey results. "The work environment continues to be complex and challenging, the nursing shortage continues, and there is constant pressure to improve," says Diana S. Contino, RN, MBA, CEN, FAEN, senior manager of healthcare for Costa Mesa, CA-based BearingPoint Management & Technology Consultants, which provides management and technology consulting services. It makes perfect sense, that most nurse managers are seeing increases, "especially since the cost of living has also gone up," she says. "Hospitals are responding to that."
Hospitals "have to offer these compensation levels in order to get a qualified applicant who is master's-prepared; experienced in change management, recruitment and retention; and most importantly, has the ability to delegate and manage teams," she says.
Even rural EDs increase salaries
Most people have seen an upward migration of salaries, but it's been mostly in the 3%-5% range on average at Premier Health Care, a Dayton, OH-based ED physician group that sees about 1.2 million patients a year, reports William Cole, MD, FACEP, CEO. In the Midwest — Nebraska, Kansas, Oklahoma, Missouri, and Illinois — the headhunters are sending out a significant number of job openings, so even the smaller rural places have had to up their salaries in order to obtain expert managers, says Mitch Jewett, RN, CEN, the ED manager at Newton (KS) Medical Center. "Although I'm under the impression that hospitals are more willing to [spend more to] get the next person in; when they get you, they are less likely to 'up' it [in the future]," he says.
Observers agree that the shortage of talented individuals, plus the competition alluded to by Jewett, have combined to place upward pressures on salaries.
In today's complex environment, one person often can't do it all, Contino says. "Plus, there is pretty stiff competition for these people outside the hospital in managed care programs, and even in private industry where huge, nonhealth care companies want to manage health care within their corporate structure," she sys. "There's intense competition from those folks, which is good for nurse managers, and that is not going to change."
Williams agrees. "It's very difficult to recruit for ED managers these days," he says. "The 'top of the league' is harder to find, and the search is a two-way search; applicants now ask questions of the hiring hospital."
What kind of questions? "They ask them, for example, what they are doing to improve throughput," he says. "It not unusual when there is [an ED manager] vacancy that there is some historical level of dysfunction, so smarter applicants will ask what's wrong, and if it has been fixed." If it has not been fixed, he says, "applicants know there are other vacancies out there in facilities with the mindset to innovate, and that they have some choices."
Williams is quick to add that he's not implying that ED leaders are unwilling to move into complex situations. "However, the question is if there are enough resources available and enough hospital leadership that is willing to help," he explains.
Cole says the demand for managers, and therefore the competition and salary levels, varies greatly from region to region. "It's the opposite [of what you might expect]," he says. "The closer you are to the ocean, for example, the lower the salary."
That salary level is because more physicians want to live there, he says. "In places where it is less desirable to live, salaries tend to be higher," he says. "Right now we have a significant shortage of qualified ED physicians, and people generally want to live in bigger cities with more amenities, because there is more to do after they get off work."
So, for example, "We've had people take a pay cut to go to New York City, and the Midwest tends to have higher salaries than the coast," Cole says. With ED medical directors, however, that's all relative. Cole puts the average compensation at about $250,000.
Beyond health care
The demand for experienced ED managers outside the health care field "is still going strong; there is a lot of demand, and a lot of products being developed," says Williams. These products include electronic tracking systems, bedside testing systems, and others. "All of these companies are coming out and begging for experts in the emergency field," he explains.
Experienced ED managers can make as much as 100% more than they do in the ED, Williams says. "Some of these positions come with the possibility of traveling or national speaking assignments," he says. Other ED managers decide to stay within the hospital, but to move up into hospital administration.
Cole sees a similar trend. "A lot of doctors are going back and getting their MBAs," he says. "There is lots of interest in working in hospitals as chief medical officers, and a couple of them have jumped over to the insurance side."
Money, he says, is not the only draw. "Money is part of it, yes, but also as physicians get older, working the night shift and holidays gets tiresome," he says. "Also, this gives them an opportunity to diversify their careers."
'Creative' compensation continues
The trend for ED managers to seek, and receive, compensation above and beyond their base salaries continues to grow, say the experts. "Most leaders are looking for the entire package — financial and otherwise," says Williams. "That includes executive assistant support." He agrees with the survey's finding that staffs are growing.
Information technology (IT) is relieving some of the burden, he says. "Scheduling is a nightmare, with wild shifts and some nurses working only one or two days, but it is becoming an IT science, which has created more stability," says Williams. "Now, some nurses can even self-schedule online."
More facilities are matching performance to manager bonuses, Contino says. "Several of my colleagues have structures like this, so they may be seeing bonus income," she says.
Jewett agrees that such incentives "appear to be growing in some areas." He says he has heard of $2,000, $5,000, or $10,000 hiring bonuses for nurse managers. As for current managers, "bonuses I think are pretty common, usually tied to the pay for performance system that your hospital or system has in place."
There is more emphasis among physicians to try to get as much money as they can into a pension or tax-deferred plan, says Cole. "Also, there is definitely more money being placed at risk [due to pay-for-performance arrangements], not only for line docs, but managers as well," he says.
Several hospitals make money available to Cole's company that it "can use to incent our managers," he says.
What are some of the measures Cole uses to determine bonuses? "Hospitals are interested in customer satisfaction scores, [Centers for Medicare & Medicaid Services] indicators, and seeing throughput times in the ED improved," he says. The bonuses can range from 10% to 20% over salary, Cole says.
Cole adds that most raises are based on pay for performance relative value units (RVU) productivity as well. "In other words, how many relative value units per hour are you producing?" he says. "This is a measure, set up by Medicare, of the work you do in taking care of a patient." RVU bonuses, he adds, are paid every two weeks.
Future is uncertain
There is little hope for relief, in the short-term, from the dearth of qualified ED managers, or from the turmoil in the field. "I worked with a hospital on the East Coast that had had 10 ED managers in the last nine years," says Williams. "Late last year, they lost 50% of their experienced nurses due to leadership issues." The person in charge of the ED had no previous ED experience and was perceived to be dictatorial, he says.
Williams says his firm was called in after all this happened. "These problems have been systemic for a number of years — and that's part of the bigger problem," he says. A recent study in the Journal of Nursing Administration would seem to back him up. In examining safety issues and supplemental (part-time) nurses, it found that in facilities that used supplemental nurses and had poor outcomes, the problem was not the qualifications of the nurses (they were at least as qualified as the full-time nurses), but their work environment.1 Key issues cited included poor relationships with top management, nonresponsive management, the failure to invest in the education of the nursing work force, and poor nurse/patient ratios.
The continuing shortage will not guarantee steady salary increases for ED managers year after year, Contino says. "There continues to be the pressure on hospital operating margins, and decreasing revenues from Medicare as relates to new DRG implementation, and probably increasing costs of technology, so it will be a continuing challenge for hospitals to keep giving people increases," she predicts.
Is there anything ED managers can do to help free money for increases?
"If hospitals do lose [Medicare] reimbursement, the only way they have to offset those losses is to reduce salaries, so the ED and inpatient managers really need to focus and collaborate on ways to minimize hospital expenses on nonreimbursable services," she advises.
Reference
1. Aiken, LH, Xue Y, Clarke SP, et al. Supplemental nurse staffing in hospitals and quality of care. J Nurs Admin 2007; 37:335-342.
In last year's report on the 2006 ED Management Salary Survey, we noted that while there was a shortage of ED nurses and physicians, compensation for ED directors and managers had failed to reflect that shortage.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
