ECG Review
ECG Review
A Cryptic Dialysis Tracing
By Ken Grauer, MD, Professor, Department of Community Health and Family Medicine, University of Florida. Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
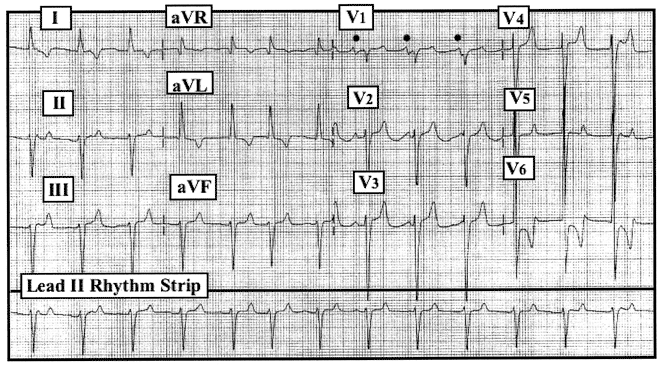 |
Figure: 12-lead ECG obtained from an 81-year-old man with bradycardia. |
Clinical Scenario:
The 12-lead ECG and lead II rhythm strip seen in the Figure was obtained from an unfortunate middle-aged dialysis patient with a dilated cardiomyopathy. He had missed his last dialysis treatment. The patient was hypertensive, fluid overloaded and dyspneic with chest pain at the time this tracing was recorded. Given this clinical context, how would you interpret his ECG?
Interpretation/Answer:
It is difficult to be certain what the rhythm is in this tracing. P waves are not consistently seen and QRS complexes are not completely regular in this Lead II rhythm strip. Nevertheless, small amplitude upright P waves do appear to precede at least some QRS complexes. That atrial activity of some kind is present is clear from lead V1 (dots in this lead), although the changing PR interval in lead V1 suggests that there may be at least transient AV dissociation with an intermittent accelerated junctional rhythm that is punctuated by sinus or other supraventricular beats. A longer rhythm strip in a lead showing more clearly defined P wave morphology would be needed to know for sure.
The QRS complex appears to be slightly prolonged (we estimate 0.11 second in duration). That said, QRS morphology and the suggestion that at least some of the P waves are conducting strongly favor this to be a supraventricular rhythm. There is marked LAD (left axis deviation), consistent with LAHB (left anterior hemiblock). QRS amplitude in the precordial leads is greatly increased, consistent with LVH (left ventricular hypertrophy). Transition is difficult to identify due to overlap of high amplitude QRS complexes, but the R wave appears to become greater than the S wave between leads V5 and V6. Deep S waves persist across the precordium. The most remarkable finding on this tracing resides in assessment of ST-T wave morphology. T waves are tall and peaked with a relatively narrow base in several leads (leads III, aVF, and V2 through V4). This T wave shape persists in the form of a smaller T wave complex in transitional lead V5, before development of a peaked and deeply negative T wave in lead V6. T waves are also inverted in leads I and aVL. Overall QRST morphology is consistent with LVH and "strain" and/or ischemia, with T wave peaking in this dialysis patient suggesting possible hyperkalemia. Serum potassium turned out to be significantly elevated. Clinical points to keep in mind are that it will be difficult to assess ST-T wave morphology for acute ischemia or infarction in the presence of hyperkalemia (ie, "competing conditions", in which ST depression and T wave inversion may at least in part be counteracted by hyperkalemic T wave peaking). Finally, some patients with hyperkalemia manifest deeply negative T wave peaking, as is evident here in lead V6.
The 12-lead ECG and lead II rhythm strip seen in the Figure was obtained from an unfortunate middle-aged dialysis patient with a dilated cardiomyopathy. He had missed his last dialysis treatment.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
