2007 Salary Survey Results: Could CMS changes get hospital CEOs to open wallets ?
2007 Salary Survey Results
Could CMS changes get hospital CEOs to open wallets ?
ICPs could see more 'pay for performance' by preventing infections
There have been several unintended consequences projected about recent pay-for-performance changes by the Centers for Medicare & Medicaid Services (CMS), but could one of them be an unexpected boon to infection control budgets? Well, maybe that would fall under an "intended consequence," but either way it would be good news for infection control professionals who have struggled for years to reap salary gains and program revenue growth in the face of increasing and ever-changing responsibilities. Could infection control professionals get a little more "pay for performance" by preventing costly health care-associated infections (HAIs) that CMS says it is not going to cover?
Many CEOs and hospital financial managers have long since discovered the power of prevention and prove it through support of their infection control professionals. Such is the fortunate case for Marcia R. Patrick, RN, MSN, CIC, infection control director at MultiCare Health System in Tacoma, WA. "At my institution we have been given more, but our CEO is a nurse who 'gets it' that quality pays," she told Hospital Infection Control. However, she knows many infection control programs are still struggling for funding and support despite the heavy emphasis on making "the business case" for infection control in recent years.
"It's very hard to know what the impact will be at the local level, but will it take the implementation of the Medicare law to get [those] CEOs off the dime?" she said. "We have to be able to make the business case, but even then some CEOs just don't get it. I suspect that with the Medicare changes that will probably change when they realize to what extent they are going to lose money on patients who have bad outcomes of any description."
Indeed, CMS says its recently issued final rule takes significant steps to improve the accuracy of Medicare's payment under the acute care hospital inpatient prospective payment system (IPPS), "while providing additional incentives for hospitals to engage in quality improvement efforts." The new rules will go into effect in October 2008. The IPPS payment reforms would restructure the inpatient diagnosis-related groups to account more fully for the severity of each patient's condition. In addition, the rule includes important provisions to ensure that Medicare no longer pays for the additional costs of certain "preventable conditions" including infectious complications of mediastinitis, catheter-related urinary tract infections, and catheter-related vascular infections.
The language of money
Concerns raised have included that hospitals will have to pay for infections that could not have been prevented, patients may be put on unnecessary antibiotics to ward off possible infections, and that hospitals will be reluctant to offer special treatment programs to severely immune compromised patients. Others, such as Lucian Leape, MD, a member of the Institute of Medicine committee that issued the landmark report To Err is Human, say that CMS is finally talking in a language that hospital CEOs understand: "The language of money."1
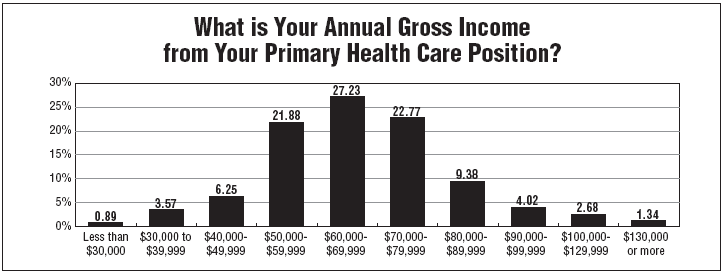
Currently, the language of money means a median salary for ICPs in the $60,000 to $69,999 range, according to the annual salary survey by HIC. The 2007 survey of 224 ICPs found that the median age range of respondents was 51 to 55 years old. In percentage breakdowns, 6% were making $40,000 to $49,999; 22% were paid $50,000 to $59,999; and 27% had salaries in the $60,000 to $69,999 range. Rounding out the lows and highs, 4% were making $30,000 to $39,999; and 23% were in the $70,000 to $79,999 range. Nine percent drew a salary in the $80,000 to $89,999 range.
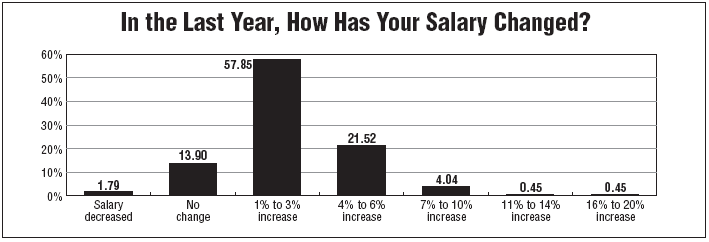
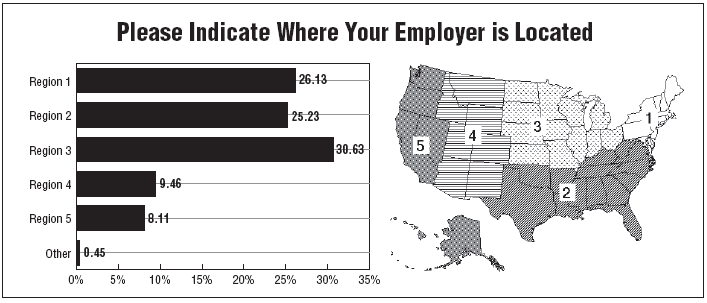
The 2007 survey found 58% of respondents drew wage hikes in the 1% to 3% range over the previous year. However, 22% of respondents drew raises of 4% to 6%, and 4% of respondents were given a raise in the 7% to 10% range. Still, 14% reported no raises for the period, but that was down from the 17% reporting flat compensation in 2006. Most survey respondents work in small- to midsize hospitals with 201-300 beds.
Regardless of facility size, the surge of regulatory activity and consumer activism about HAIs means hospitals are going to have to invest in infection prevention or be held accountable. "I'm hearing that some areas are getting more resources and others are still struggling to get that level of understanding from their administrative arm," Patrick said. "If CEOs have not become convinced through the other [national] quality initiatives that a number of organizations are adopting, then this [CMS change] will do it."
Consumer activism could drive IC resources
Kathy L. Warye, executive director of the Association for Professionals in Infection Control and Epidemiology (APIC) made a similar observation at the organization's 2007 meeting in San Jose, CA. "Changing trends such as pay for performance are going to have a dramatic impact on infection control," she said. "Consumers and payers are going to demand proactive programs. We must focus on prevention."
Indeed, when consumers are involved infection prevention is not simply a matter of compliance, but decreasing liability to lawsuits. With infection prevention now a matter of wide public discussion, health care administrators would be ill-advised to short change infection control departments.
"This a time of transition for the profession," Warye said. "Consumer awareness and expectations are really driving much of what we do, and I think personally in most cases it is in a very positive way. There is probably no better way to elevate the profession and bring pressure to bear on institutions to contribute more resources. Clearly, we are looking at a host of new legislative and governmental initiatives. We certainly don't want to see mandates, but these things in some ways are becoming part of our environment — increasing regulation and government activity."
Moreover, widely publicized studies and media coverage of methicillin-resistant Staphylococcus aureus have raised the profile of the ICP both in the hospital and community. "When there have been outbreaks or bad outcomes in the community they have utilized the local hospital infection control professional to provide information and education," Patrick said. "There are opportunities there [for ICPs]."
While much is in motion, many ICPs still battle for resources and respect within their institutions. "The current reality of the average infection control program is that there is more isolation than integration," Warye said. "There are no learning systems dedicated to infection prevention. There's a lack of authority to implement change, a poor understanding of the economics of HAIs and perhaps some disbelief that zero [infection rates] can be achieved. The ICP in many institutions is more cop than coach. Staff see infection prevention measures as a distraction or interruption to their work rather than hardwired into the work itself [as a] natural aspect of care."
As it looks to the future for ICPs, APIC is urging that health care take a systems approach and make infection control part of everyone's job. "The epidemic of HAIs in today's health care institutions is systemic of a structure that does not adequately support infection prevention and control," she said. "Errors result from faulty systems not from faulty people. So it is the system that must be addressed. We need a systems model where we design and engineer prevention into patient care, an infection prevention system that would hardwire infection control compliance into every single health care worker's job."
As the importance of infection control throughout health systems becomes more apparent to administrators and staff, ICPs could move up from cop to communicator, taking an appropriately compensated leadership role and guiding a comprehensive prevention program that everyone else — finally — sees as a vital aspect of patient care.
Reference
- Leape L. Why pay for mistakes? Boston Globe. Aug. 23, 2007.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
