ECG Review: Sepsis and Tachypnea
ECG Review
Sepsis and Tachypnea
By Ken Grauer, MD, Professor, Department of Community Health and Family Medicine, University of Florida Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
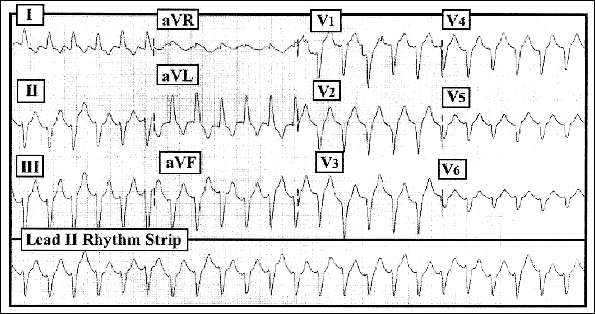 |
Figure: 12-lead ECG and rhythm strip obtained from an older woman with urinary sepsis and acute tachypnea. |
Clinical Scenario:
The 12-lead ECG and lead II rhythm strip seen in the Figure were obtained from an 81-year old woman with urinary sepsis. She had become acutely tachypneic at the time this tracing was recorded. How do you interpret her ECG? Are you certain of your diagnosis?
Interpretation/Answer:
The QRS complex is clearly wide. There is no sign of atrial activity anywhere on the tracing. The rhythm is regular at 140/minute. Thus, this 12-lead ECG and accompanying lead II rhythm strip show a regular WCT (wide complex tachycardia). Given the age of the patient, the odds that the rhythm is VT (ventricular tachycardia) exceed 90%. Although SVT (supraventricular tachycardia) with QRS widening from either preexisting bundle branch block or aberrant conduction are also possibilities, several additional findings on this tracing increase the likelihood that this is VT to the 98-99% probability range. QRS morphology during the tachycardia does not look like either a typical LBBB (left bundle branch block) or RBBB (right bundle branch block) in each of the 3 key leads (leads I, V1, and V6). QRS morphology in leads I and V1 is consistent with a LBBB pattern, but QRS appearance in lead V6 is not. Instead, the QRS complex is unidirectional (in this case negative) in all 6 precordial leads. There is almost always at least minimal positivity to the QRS complex in lead V6 when the rhythm is supraventricular. Finally, there is marked LAD (left axis deviation). Although mild to moderate axis deviation (either leftward or rightward) is common with SVT, extreme axis deviation (as seen here) is far less likely with supraventricular rhythms.
This elderly patient with urinary sepsis and multiple comorbidities, had been deemed "DNR" (ie, Do Not Resuscitate) via advance directives put forth by her and her family. As a result, she was admitted to a general floor in the hospital for conservative treatment with intravenous fluids and antibiotics. Miraculously, her VT spontaneously resolved without use of antiarrhythmics or electricity, and the patient recovered.
12-lead ECG and rhythm strip obtained from an older woman with urinary sepsis and acute tachypnea.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
