Medical Conditions that Mimic Psychiatric Disease: A Systematic Approach for Evaluation of Patients Who Present with Psychiatric Symptomatology
Author: Steven T. Dorsey, MD, Associate Staff Physician, Department of Emergency Medicine, The Cleveland Clinic Foundation; Assistant Residency Director, Case Western Reserve University/MetroHealth Medical Center/Cleveland Clinic Foundation Emergency Medicine Residency Program; Consultant, Department of Emergency Medicine, MetroHealth Medical Center, Cleveland, OH.
Peer Reviewers: Jeffrey J. Bazarian, MD, MPH, Assistant Professor of Emergency Medicine, University of Rochester Medical Center, Rochester, NY; Travis Roth, MD, Assistant Professor, Emergency Medicine, Emory University, Atlanta, GA.
Most emergency physicians (EPs) encounter patients with psychiatric chief complaints on a daily basis, and not infrequently, such patients are a source of undue frustration. Evaluation of patients with psychiatric complaints can be a time-consuming process, and can be complicated by a number of factors, including difficulty obtaining an accurate history; physician biases; disruptive behavior; and mandatory involvement and consultation from psychiatric consultants, case workers, and social workers.
The concept of sufficient medical clearance always must be addressed, and its exact definition often is a matter of dispute. Consultants from the psychiatry service often question whether the patient’s symptomatology represents a psychiatric disorder or whether behavioral and cognitive changes reflect manifestations of an acute, or chronic, medical condition, thereby making admission to the medical ward a more appropriate course of action.
The busy emergency physician, pressured by time constraints and a full waiting room, may be tempted to limit laboratory and other ancillary testing when a patient with a psychiatric chief complaint appears clinically well in all other respects. Nevertheless, multiple medical conditions commonly encountered in the emergency department (ED) setting can present in an atypical fashion and mimic psychiatric disorders. A missed organic cause of psychopathology can lead to significant morbidity and mortality, in particular, for those individuals inappropriately admitted to a psychiatric unit for therapy.
Following a discussion of some of the incorrect assumptions and pitfalls encountered by EPs in the evaluation of patients presenting with declared or presumed psychiatric chief complaints, this report will outline in detail those medical conditions that mimic psychiatric disorders, and present streamlined, effective approaches for making clinical distinctions that will optimize patient outcomes.—The Editor
Incorrect Assumptions and Pitfalls
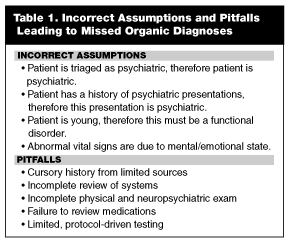
When patients present with psychiatric complaints, assumptions by EPs and specific pitfalls, such as errors of omission, can lead to misdiagnosis of a primary psychiatric disorder when an organic mimic of a psychiatric condition actually is responsible for a patient’s presumed psychiatric symptoms. (See Table 1.)
 |
Unintentional labeling of patients can occur at the point of triage. The triage nurse and staff indirectly can influence the caregivers in the department through their initial assessment and entries in the ED ledger. Note the potential inference that may be drawn because of a chief complaint worded as follows: "25-year-old female, feeling anxious and can’t breathe,’ history of panic attack,’" vs. "25-year-old female, short of breath, tightness in chest, two weeks postpartum." In the first case, one is dealing with a possible anxiety attack, while the wording of the second example demonstrates clinical suspicion for pulmonary embolism (PE). Clearly, unintentional labeling of patients in triage can raise or lower the clinical antennae of physicians and nursing staff, and thus negatively impact the patient’s care. The above example also highlights another potential assumption that serves to limit the extent that other organic causes are explored. Caregivers may assume that a patient with a history of prior psychiatric diagnosis, treatment, or admissions most likely is presenting with an exacerbation of the same condition. Most EDs provide care for patients with frequent ED visits for psychiatric and social complaints who are often facetiously labeled as "frequent flyers," and the presentation of such patients to triage often is assumed to be the particular patient’s typical/usual visit. EPs also must consider whether an organic condition is exacerbating or provoking psychiatric symptoms in patients with underlying psychiatric disease and prior psychiatric admissions.
Most EPs make the safe assumption that altered mental status in a geriatric patient is of organic etiology until proven otherwise. However, the assumption that younger patients are more likely to have a functional disorder, while statistically accurate, is risky. Tintinalli et al found that patients younger than age 55 were four times more likely to have a missed organic cause for their presumed psychiatric condition.1
The EP must address and justify any abnormal vital signs. Although a patient’s level of agitation or anxiety may cause tachycardia or hypertension, an EP who assumes such abnormalities simply are due to a patient’s mental state or agitation may miss not only a correctable, but also a life-threatening, etiology. Reassessment and documentation of serial vital signs, particularly after an initially agitated patient appears clinically calm, may detect persistent vital sign abnormalities indicative of organic illness.
In the evaluation of patients with psychiatric complaints, the astute EP must avoid the temptation to rush through a cursory history of present illness. The patient may be unwilling or unable to provide sufficient detail, and thus the input of family, friends, case workers, and the patient’s primary psychiatrist must be sought with reasonable effort. Reeves et al reviewed the records of 64 patients erroneously admitted to psychiatric units, as defined by need for medical intervention within several hours of admission and transfer to a medical floor or unit within 24 hours. Deficiencies in documentation of readily available historical data were found in 34% of the cases reviewed.2 After a patient voices an admissible symptom at the point of triage, such as suicidal ideation, EPs may limit their history taking and, as a result, miss vital information. Completion of a thorough review of systems may highlight physical complaints or symptoms suggestive of an organic cause and aid the EP in tailoring an appropriate work-up.
A number of factors may lead a busy EP to cut corners on physical examination of patients with psychiatric complaints. The patient who is agitated or violent may intimidate the EP, and any restraints, whether physical or pharmacologic, may limit the patient’s ability to cooperate with the exam. The EP may limit the exam of younger patients who appear clinically well, and thus may overlook specific physical exam findings that suggest organic disease.
Retrospective analyses have demonstrated that omitted portions of the neuropsychiatric exam promote inappropriate admission of medical mimics to psychiatric services. Tintinalli et al reviewed the charts of 298 ED patients admitted to a psychiatric inpatient service, and found that proper mental status exams were not documented on 20% of charts, and cranial nerve exams were documented only on 55% of charts.1 None of the charts reviewed by Reeves et al indicated that a detailed mental status examination had been performed; documentation of neuropsychiatric exam was limited to "oriented times three" in 51 out of 64 charts.2
For many medical conditions that can cause psychiatric symptoms, the general physical exam may offer no diagnostic clues. Thus, a detailed neuropsychiatric exam is of paramount importance; specifically, it can help the EP to identify delirium, and thus broaden the evaluation and detect a medical mimic. Delirium is an organic brain syndrome, characterized by a fluctuating level of attention and concentration.3 By definition, delirium always has a medical cause. It usually evolves over hours to days. Labile affect, persecutory delusions, and loose associations may be prominent presenting symptoms, and easily can be mistaken for symptoms of a psychotic disorder. Sleep-wake cycles often are disrupted or even reversed. The occurrence of visual hallucinations and the acuity of onset, along with other risk factors gleaned through a careful history, help distinguish delirium from functional disorders.4 (See Table 2.)
 |
Elderly patients especially are prone to develop delirium due to their existing co-morbid medical conditions, diminished physiologic reserve, and sensitivity to side effects of medications. Polypharmacy increases the risk for serious drug interactions. Disease affecting any organ system can cause delirium in the geriatric patient; pulmonary, genitourinary, and intra-abdominal infections are frequent culprits.5 The geriatric patient presenting to the ED with altered mental status or presumed psychiatric symptoms requires intensive work-up for organic cause.
To further challenge the EP, elderly patients with baseline dementia often present with overlying delirium, a situation referred to as beclouded dementia. Patients with baseline dementia are at increased risk for developing delirium.3 Dementia is defined as cognitive decline manifested as memory impairment plus one of the following: apraxia ( impaired ability to carry out motor functions), aphasia, agnosia (failure to recognize or identify objects), or disturbance in executive functioning.6 Unexplained injuries and poor compliance with medications may be the earliest signs of cognitive decline.3 The EP must discriminate delirium from baseline dementia through a thorough mental status exam, although this may be difficult when a patient has advanced dementia. Acuity of onset and fluctuation of level of attention help discriminate the two disorders; a detailed history from family and caregivers is vital if the patient cannot cooperate with the mental status exam. Lastly, demented patients also may not voice specific symptoms, such as chest pain, that would broaden the differential diagnosis and prompt broader ancillary testing.
Many medications can cause neuropsychiatric side effects, even at therapeutic doses. The EP carefully must review a patient’s list of medications, and often this will require review of the medical record and contact with the primary care physician, family, or caregivers. Certain drug categories are notorious for causing delirium or symptoms that mistakenly are attributed to a functional psychiatric disorder (see discussion below). Careful history taking may find that psychiatric symptoms are coupled with a recent dosage adjustment or introduction of a new medication. The EP may consider further ancillary testing based on a patient’s medication list; for example, obtaining an electrocardiogram (ECG) and serum electrolytes when a patient is taking a diuretic.
Limiting the work-up to protocol-driven, "cookbook" testing of patients with presumed psychiatric presentations must be avoided. Often such protocols are dictated by psychiatric facilities that demand a certain minimum amount of ancillary testing for medical clearance before a patient is considered for admission. A routinely ordered battery of tests, such as a serum alcohol, urine toxicology, and basic metabolic panel with renal function tests, will catch many (but not all) medical mimics. Life-threatening conditions can be missed by limited testing, while excessive "shotgun" testing is inefficient, time-consuming, and expensive. The EP must approach each patient encounter as unique and tailor an appropriate work-up beyond what an accepting inpatient facility mandates. In the case of selected patients with first-time psychiatric presentations, advanced age, or multiple co-morbidities, the EP must consider further testing such as a serum thyroid stimulating hormone (TSH) assay, computed tomography (CT) scan of the head, and additional electrolyte assays such as serum calcium and magnesium. Interestingly, Korn et al found through a retrospective chart review that there is little value to laboratory or ancillary screening when patients present with an isolated psychiatric complaint and meet the criteria of having a prior psychiatric history, normal vital signs, and negative physical findings.7 Future prospective validation of their findings could translate into real-time and laboratory cost savings; nevertheless, EPs should address each patient presentation as unique and have a low threshold to expand a work-up with targeted testing.
Common Medical Mimics and the ABC Mnemonic
A number of acute conditions, all with a propensity to cause neuropsychiatric symptoms, present to the ED with some regularity. Mnemonics have been developed to assist the EP in considering these frequently encountered disorders.8 An ABC mnemonic for medical mimics of psychiatric disease is presented here for the first time. (See Table 3.) It organizes the most common organic mimics in an ABC format familiar to most EPs; the alphabetic grouping facilitates recall and mirrors the approach that EPs employ when treating critically ill patients. The list of conditions detailed in the remainder of this report is not comprehensive for medical conditions that can cause neuropsychiatric symptoms, but includes common conditions that present to the ED that could be misdiagnosed or missed entirely without careful exam and evaluation.
 |
Airway and Breathing. Most conditions causing airway compromise or impairing gas exchange never would be mistaken for a psychiatric disorder. However, certain conditions that can cause hypoxemia or hypercarbia may present in a subtle or atypical fashion. (See Table 4.) Compromised airway and breathing can be fatal within minutes if not recognized. A patient’s complaint of feeling "smothered" or "closed in" may be mistaken for acute anxiety or a panic attack, especially if the EP misinterprets the patient’s tachypnea for hyperventilation. A patient with impending respiratory failure may rush into triage panicked and combative, be presumed psychotic, and during restraint and sedation, his tracheal deviation and unilaterally decreased breath sounds may be missed. A spontaneous pneumothorax requires tube thoracostomy, not leather restraints and intramuscular haloperidol. An underlying pulmonary disorder may present as delirium in an elderly patient, and only a thorough physical exam and chest radiograph would uncover common conditions such as pneumonia or mild congestive heart failure. In the absence of obvious air hunger or accessory respiratory muscle use, the EP’s first clue to a problem with oxygenation may be the finding of tachypnea or tachycardia, and the etiology for either must be explored fully.
 |
PE remains a challenging diagnosis in the ED setting. Dyspnea is by far the most common presenting symptom, reported by 70-90% of patients. Pleuritic chest pain is the second most common symptom and, interestingly, is reported more often for smaller emboli, as opposed to patients with massive or centrally lodged emboli. Smaller emboli may be more likely to lodge peripherally, cause pulmonary infarction, and thus generate pleuritic pain.9 The third most common symptom in patients with angiographically proven PE is apprehension.10 Apprehension as a presenting symptom also correlates with massive PE.9 The EP must approach the patient presenting with a sense of doom or anxiety symptoms, even without any chest pain complaint, as a potential cardiopulmonary emergency.
PE also must be considered in the delirious patient, or the elderly patient with altered mental status who is unable to complain of the typical symptoms, perhaps due to aphasia or advanced dementia. In the evaluation of such patients, PE must be considered for unexplained tachypnea or tachycardia, and the presence of either sign warrants additional testing. The EP must consider risk factors for thromboembolic disease, such as immobility or underlying malignancy, and recognize findings supportive of deep venous thrombosis if present. Specific findings on lung auscultation, such as rales or consolidation, are rare in most cases of acute submassive PE. A number of non-specific tests have demonstrated utility in the ED setting in the evaluation of acute PE, although none in isolation has proven robust enough to exclude PE at the bedside.11 A proposed combination of two indirect tests, the D-dimer assay and alveolar dead space analysis, has demonstrated a high sensitivity and negative predictive value.12 Absolute exclusion of PE is impossible in the ED setting; extremity ultrasonography (to assess for deep venous thrombosis), ventilation/perfusion scanning, and spiral CT scan of the chest are still the most practical studies, with the EP’s clinical suspicion ultimately determining whether anticoagulation and admission are warranted.
EPs must be vigilant for cases of carbon monoxide (CO) poisoning. Although more common in colder climes and during the winter months, it can occur whenever a combustion engine operates in a poorly ventilated area. Failure to suspect the diagnosis can lead to catastrophe, for both the undiagnosed patient, who is discharged back to the unsafe point of exposure and unsuspecting others. The most common presenting symptoms of CO poisoning are headache, impaired concentration, confusion, irritability, muscle weakness, and nausea. The EP may attribute the patient’s symptoms to a simple viral syndrome if the somatic symptoms dominate, while problems with concentration or irritability may be attributed to anxiety or depressive symptoms. Patients with serious toxicity may present primarily with confusion or hallucinations; the EP may suspect primary psychosis. Although a controlled study has demonstrated that exposure to even low CO levels causes neuropsychologic impairment detectable on standard testing instruments,13 evidence is lacking that intermittent exposure to low CO levels can cause depression.14
The EP must have a low threshold to consider CO exposure in patients with the chief complaint of headache, and must query patients on the pattern of their symptoms. Suggestive historical details include headache or other symptoms that repeatedly occur in a particular location, or close personal contacts who have the same symptom complex. Standard pulse oximeters cannot distinguish carboxyhemoglobin from oxyhemoglobin, and thus a patient may have a falsely high or normal pulse oximetry reading despite significant hypoxemia.15 Serum co-oximetry is necessary to screen for CO exposure; a venous blood sample is as accurate as an arterial sample for this purpose.16 Severity of symptoms does not correlate with absolute carboxyhemoglobin level.17,18 Oxygen delivered by 100% non-rebreather mask is standard therapy for CO poisoning, reducing the half-life of carboxyhemoglobin by 50-75%. Hyperbaric oxygen therapy may prevent chronic neurologic sequelae of CO poisoning and is used liberally at some centers.18
More than 16 million people in the United States suffer from chronic obstructive pulmonary disease (COPD), and it is the fourth leading cause of death after heart disease, cancer, and stroke.19 An exacerbation of COPD can present insidiously, with hypoventilation resulting in progressive hypercarbia. The resulting somnolence, confusion, and inactivity can resemble an affective disorder. The EP should utilize arterial blood gas (ABG) analysis for any patient with history of COPD and behavioral change. In patients with history of chronic hypercarbia, elevated partial pressure of carbon dioxide (pCO2) should be compared to prior ABG results in the patient’s medical record. Evidence-based analysis supports inhaled bronchodilators and a short course of systemic corticosteroids when patients with acute COPD exacerbations present to the ED; in cases of severe respiratory failure, noninvasive positive-pressure ventilation is efficacious and can obviate the need for intubation.19 These interventions markedly can improve minute ventilation; serial ABG analysis may demonstrate this objectively, while improvements in mental status are realized at the bedside.
Cardiovascular and Central Nervous System (CNS). Even without a firm history of head trauma, EPs should be wary of occult head injury in patients with acute behavioral change (See Table 5), especially in the case of geriatric patients.20 The elderly are particularly at risk for subdural hematoma, due to generalized cerebral atrophy and their propensity for falls. EPs meticulously must examine the head and scalp of elderly patients who present with altered mental status, and obtain the history behind any fresh or healing contusions. Even in the absence of any signs of recent or remote head trauma, any contusions or bruising of the extremities suggestive of falls must be investigated. In the case of an elderly patient with acute behavioral change, the EP must have a low threshold to obtain a non-contrast CT scan, even if no gross symptoms of traumatic brain injury are discovered on neurologic exam. Out of a prospective cohort of 58 closed head injury patients with a Glasgow Coma Scale of 15, one study found 5% had CT scan findings for acute intracranial injury, while two patients had a completely normal neurologic exam.21 Other populations at risk for intracranial bleeding with relatively minor head trauma include chronic alcoholics, due to their risk for falls and relative coagulopathy, and patients taking warfarin.
 |
On rare occasions, an acute cerebrovascular accident (CVA) presents with only mood or behavioral change. Apathy, paucity of speech, and sleeplessness may occur in the absence of any apparent classic stroke symptoms such as weakness, facial droop, or ataxia. This underscores the need for a detailed neuropsychiatric exam in all patients with presumed psychiatric symptoms, because subtle findings like dysarthria, dysprosody (lack of affective inflection in speech,) aphasia, alexia, and agraphia are suggestive of a neurologic, and thus organic, etiology.3 In the absence of obvious deficits, presentation may be delayed beyond 24 or 48 hours, and thus non-contrast head CT may demonstrate the hypodensity of a subacute infarct. In one series, depression after CVA was associated significantly with right hemispheric infarcts.22
CNS neoplasms, particularly slow-growing frontal lobe tumors, can cause behavioral or affective symptoms without focal neurologic signs, and thus their diagnosis often is delayed.6 Lesions that arise in the temporal lobe and limbic structures tend to cause visual and auditory hallucinations, psychosis, panic attacks, and amnesia.23,24 Interestingly, one prospective series of surgical patients with CNS tumors found no difference between left- and right-sided lesions with respect to depressive symptoms, but patients with meningiomas had higher levels of anxiety and depression than those found with any other tumor type.25 If the EP has a high clinical suspicion for neoplasm despite a normal non-contrast head CT, further investigation with contrast-enhanced CT or magnetic resonance imaging is warranted.
The EP must consider acute myocardial infarction (AMI) or an acute coronary syndrome (ACS) in elderly patients with acute delirium or behavioral change of acute onset.26-28 Elderly patients often present in a delayed fashion, having had silent ischemia, and their symptom complex may include weakness, lethargy, loss of appetite, and decreased mobility.28 Such decline may be misinterpreted as depressive symptoms, particularly if the acuity of its onset is not evident by history. Physical findings after AMI may be subtle, such as an S3 gallop or fine basilar crackles of pulmonary congestion secondary to decreased pump function. A 12-lead ECG is quick, inexpensive, and non-invasive, and the EP should obtain one in every elderly patient with mental status change or psychiatric complaint. ACS as well as other life-threatening conditions, such as electrolyte disorders, may be evident on ECG (see below). Because the sensitivity of ECG in AMI is only 50%,28 admission to a telemetry bed for serial ECGs and cardiac enzymes may be required for full medical clearance. The inappropriate admission of an elderly patient with ACS or AMI to a psychiatric floor could be disastrous; elderly patients with AMI are at increased risk for complications such as arrhythmia, heart failure, and wall rupture.26-29
Thrombotic thrombocytopenic purpura (TTP) should be considered in patients with acute mental status change, particularly acute delirium or psychosis. The classic diagnostic pentad of TTP includes thrombocytopenia, microangiopathic hemolytic anemia, altered mental status, renal function abnormalities, and fever. TTP and hemolytic uremic syndrome (HUS) widely are considered to be variations of a single disorder, due to their being clinically and pathologically identical, with both conditions resulting from diffuse vascular endothelial cell damage.30 TTP is associated with the postpartum state, invasive bacterial dysentery, autoimmune diseases, bone marrow transplantation, and certain medications (i.e., quinine, clopidogrel, and ticlodipine). Except for the rare finding of a petechial rash, physical exam tends to be unrevealing in cases of TTP, and it enters the differential diagnosis as the laboratory abnormalities included in the classic pentad are noted. George and Vesely advocate initiation of plasma exchange therapy for any patient with thrombocytyopenia and hemolytic anemia documented on peripheral smear, since the other clinical features are variable in frequency and severity. For example, proteinuria and hematuria are common, while frank renal failure is less common. Fever, if seen, is usually low-grade; high fever with rigors is suggestive of systemic infection.30 The altered mental status that often occurs in TTP may be multifactorial, although 10% of the TTP patients in one series were found to have nonconvulsive status epilepticus on electroencephalogram (EEG), suggesting a role for anticonvulsants in the acute management of TTP.31 Since the recognition of its utility, plasma exchange therapy has increased survival in cases of TPP to 80%.
By definition, the hallmark of hypertensive emergencies is clinical evidence of end-organ damage, such as respiratory failure from pulmonary edema, myocardial ischemia, acute renal failure, or encephalopathy. Because of violence or combativeness, caregivers may omit early assessment of vital signs, or mistakenly may ascribe hypertension to emotional or situational distress. Hypertensive encephalopathy also may present as a generalized depression of sensorium. The careful EP must utilize intravenous medications and arterial pressure monitoring in cases of true hypertensive emergency requiring rapid reduction of blood pressure, and initially should aim for a modest reduction of 10-15 %, or reduction of diastolic pressure to 110 torr.32 Because of cerebral autoregulation of blood flow in the face of chronic hypertension, over-aggressive reductions can precipitate acute cerebrovascular ischemia or stroke.33 Labetalol and the dopamine receptor antagonist feneldopam are first-line agents; nitroprusside is potent and short-acting, but its metabolites are potentially toxic.32
Drugs and Medications
Without testing for specific agents, EPs may mistake acute intoxication with certain drugs of abuse (DOAs) as a primary psychiatric presentation.34 (See Table 6.) Symptoms of agitation, aggressive behavior, and hallucinations may occur with use of agents such as cocaine, marijuana, inhalants, hallucinogens, phencyclidine (PCP), and methylenedioxymethamphetamine (MDMA, ecstasy). First-time marijuana users also are prone to an acute panic-like reaction, which usually resolves without treatment within several hours.35 In recent years, abuse of gamma-hydroxybutyrate (GHB), a substance promoted as a body-building supplement and rave/party drug, has increased dramatically. Although overdoses of GHB present with obtundation and often respiratory depression requiring intubation, stimulation can trigger sudden violent and aggressive behavior.36 Several of these agents (MDMA, PCP, GHB) are not included in routine urine toxicology screens, and the EP will have to rely on careful history and clinical presentation to make the diagnosis.
 |
Early onset alcohol withdrawal syndrome may mimic psychosis or mania, with symptoms of anxiety, hyperalertness, impaired judgment, and hallucinations.34,37 The EP should recognize the physical signs of withdrawal, such as hypertension, tachycardia, diaphoresis, and vomiting. Advanced/late onset withdrawal, often termed delirium tremens, is unlikely to go unrecognized in the ED setting; hallmarks include marked autonomic instability, hyperthermia, and obvious delirium with fluctuations of mental status between agitation and markedly depressed sensorium.37 Upon recognition of an alcohol withdrawal syndrome, the EP should initiate intravenous fluids, thiamine supplementation, and administration of benzodiazepine for relief of autonomic symptoms and agitation, and for seizure prophylaxis.
The chronic alcoholic with nutritional deficiency, particularly for thiamine, also may present with Wernicke’s encephalopathy. The EP rarely will appreciate the classic triad of altered mental status, ataxia, and abnormal eye movements. Global confusion commonly is seen, along with apathy, inattentiveness, and paucity of speech. Although vertical nystagmus is considered to be a classic finding for Wernicke’s, the EP is much more likely to detect horizontal nystagmus on exam.38 EPs routinely should administer empiric thiamine to chronic alcoholics, although response among symptomatic individuals will vary; ocular findings and mental status changes respond most readily, while gait ataxia may not improve completely.34,36
Withdrawal from other DOAs may be misdiagnosed as a primary psychiatric disorder. Early benzodiazepine withdrawal can mimic anxiety, and thus can be misdiagnosed as inadequate titration of medication if the sedative was prescribed for an anxiety syndrome in the first place.34 Severe withdrawal from benzodiazepines resembles advanced alcohol withdrawal or delirium tremens, and its prominent physical signs would prevent a case being inadvertently admitted to a non-medical floor. Chronic heavy users of GHB who decrease their use may develop a withdrawal syndrome with prominent agitation and hallucinations, and most cases must be managed with prolonged sedation to prevent injury and complications such as hyperthermia and rhabdomyolysis.39
Numerous non-prescription and over-the-counter medications can have neuropsychiatric effects at normal dosage. When questioning patients about medications, EPs must be specific in their questions, as patients often will not mention non-prescription, herbal, or homeopathic preparations unless directly asked about their use. Allergy and cold preparations containing sympathomimetic decongestants, such as pseudoephedrine, can cause nervousness, insomnia, and anxiety-like symptoms.40 In the case of overdose, psychosis and hallucinations can occur.40,41 The opioid analog dextromethorphan has abuse potential and, in the case of overdose, can cause neuropsychiatric effects ranging from somnolence to excitability.42,43 Stimulants that contain high-dose caffeine or ephedrine and that are marketed as study aids and appetite suppressants can cause nervousness, panic-like symptoms, frank psychosis, or mania.44
Certain prescription medications are notorious for causing neuropsychiatric side effects. The EP must be suspicious for medication side effects when a patient presents soon after discharge from the ED or an inpatient setting. Systemic corticosteroids are notorious for provoking a spectrum of symptoms from mild euphoria to hypomania and frank psychosis.40,45 Non-steroidal anti-inflammatory drugs (NSAIDS) have been noted to elicit depressive symptoms and paranoia in patients with prior psychiatric diagnoses.46 Beta-blockers have been implicated as causing depression, although numerous trials do not support this association.47-50
Serotonergic medications, such as the selective serotonin reuptake inhibitors (SSRIs) and tricyclic antidepressants, can provoke the serotonin syndrome by themselves or through pharmacokinetic interaction with other medications. The serotonin syndrome is characterized by altered mental status, often confusion or agitation; autonomic instability, as manifested by hyperthermia, tachycardia, mydriasis, and gastrointestinal symptoms; and neuromuscular findings such as rigidity, myoclonus, and hyperreflexia. Mild cases may cause only restlessness, palpitations, and agitation, and thus may go unrecognized or be attributed to anxiety. Symptoms tend to occur within 24 hours of medication initiation, dosage adjustment, or overdose.51 Other than cessation of implicated medications, treatment is supportive.
The phenothiazine antiemetics can cause a variety of extra-pyramidal reactions, including acute dystonia and akathisia. Akathisia is a state of mental and motor restlessness, characterized by inability to remain still in the seated or standing position. Patients with akathisia often present with significant emotional distress, likely due to their inability to identify the cause of their restlessness; thus, by describing their symptoms as an anxiety attack at the point of triage, they may label themselves with a psychiatric chief complaint, and the iatrogenic root of their problem may be overlooked. In one prospective case-control study, 44% of patients developed measurable akathisia after intravenous administration of prochlorperazine for headache or nausea.52 If neuroleptic-associated akathisia is suspected, rapid relief of symptoms with intravenous diphenhydramine can be diagnostic.
Electrolytes and Endocrinology
 |
It is imperative that EPs obtain a serum glucose level early in the evaluation of patients with altered mental status, as hypoglycemia may be rapidly fatal if not recognized and treated. (See Table 7.) Neurologic symptoms of hypoglycemia may range from stupor and coma to agitation and combativeness. The commonly associated physical signs of tremor, anxiety, diaphoresis, and tachycardia in the context of an agitated and belligerent patient may lead to inappropriate physical or pharmacologic restraint, delaying diagnosis and increasing the potential morbidity.53 In a prospective series of 125 patients presenting to the ED with hypoglycemia, the etiology was related to complications of diabetes or alcohol abuse in 108 cases.54 Other causes identified included sepsis, fasting, and intentional insulin abuse. Recurrent episodes of hypoglycemia in the non-diabetic is suggestive of insulinoma; up to 80% of patients with insulinoma have psychiatric symptoms.55 Administration of thiamine and glucose in the ED should cause rapid clinical improvement. Because of the potential for prolonged effects and relapse, cases of sulfonylurea-induced hypoglycemia must be admitted to inpatient observation or an ED observation unit for serial serum glucose testing.
EPs always should obtain a serum electrolyte panel in cases of acutely altered mental status, and should consider electrolyte screening in the case of a presumed exacerbation of a previously diagnosed psychiatric condition. Disorders of serum sodium concentration can cause mental status change. Hypernatremia may result from free water losses or diabetes insipidus. On neurologic exam, affected individuals may demonstrate irritability or stupor. Ataxia, hyperreflexia, and muscle twitching can be seen. Treatment involves repletion of volume deficits with normal saline over 48 hours; too-rapid rehydration theoretically may cause neuronal edema due to idiogenic osmoles in the intracellular fluid. Hyponatremia generally is classified into hypovolemic hyponatremia, most often due to gastrointestinal or renal losses; euvolemic hyponatremia due to psychogenic polydipsia or the syndrome of inappropriate secretion of anti-diuretic hormone (SIADH); and hypervolemic hyponatremia as can occur in cases of CHF, nephrotic syndrome, and hepatic cirrhosis. The symptoms of hyponatremia are primarily neurologic, and can include lethargy, apathy, depression, and agitation. Physical signs include weakness, vomiting, ataxia, and, rarely, seizures. With rapid losses, symptoms tend to occur when the serum concentration drops below 120 milliequivalents (meq) per liter, whereas slow losses may present insidiously. Therapy for uncomplicated cases of euvolemic and hypervolemic hyponatremia involves fluid restriction, while hypovolemic hyponatremia is corrected by slow infusion of isotonic saline. Over-aggressive sodium repletion, particularly in cases of chronic hyponatremia, can cause central pontine myelinosis; therefore, goal repletion should be no more than 20 meq in a 24-hour period.56
Hypokalemia most commonly is due to renal or gastrointestinal losses, such as from diuretic use, vomiting, diarrhea, renal tubular acidosis, and ileostomies. Volume depletion facilitates further potassium loss by two mechanisms: Resultant aldosterone production promotes additional renal losses, and contraction alkalosis causes an intracellular shift of potassium, further lowering the serum concentration. Patients with hypokalemia typically present with muscle aches, fatigue, and paresthesias. Impaired cardiac conduction may be evident on ECG as repolarization abnormalities, particularly T wave flattening and development of U waves. Arrhythmias, including conduction blocks, atrial and ventricular fibrillation, and asystolic arrest, can occur. Neurologic manifestations may include irritability and depressive symptoms. Because a measured serum hypokalemia is indicative of a whole-body depletion of potassium, repletion often requires admission. Although oral loading is safer, it can be impractical in selected patients due to gastrointestinal upset. Intravenous repletion should not exceed 10-20 meq per hour to minimize risk for iatrogenic hyperkalemia and arrhythmia.56
Other, less commonly seen electrolyte disorders can present with alterations of mental status. Hypercalcemia may cause symptoms ranging from depression to agitation and psychosis.55 Causes of hypercalcemia include parathyroid-like protein generated by underlying malignancies and increased renal resorption due to thiazide diuretics. Hypocalcemia, most often caused by chronic renal failure or secondary hypoparathyroidism from ethanol abuse, can cause depressive symptoms, irritability, and confusion. Affected individuals may report symptoms of muscle cramps and paresthesias; careful neuromuscular exam may detect fasciculations or latent tetany by testing for Trousseau’s or Chvostek’s signs. Similar mental status changes and signs of neuromuscular irritability occur with magnesium deficiency. Causes of hypomagnesemia include diuretic use, chronic gastrointestinal losses, and malnourishment. The EP always should include a serum magnesium level in the medical evaluation of chronic alcoholics. The ECG in cases of hypomagnesemia may demonstrate prolongation of the PR, QRS, and QT intervals, as well as repolarization abnormalities. Some of these effects can be due to the hypokalemia that often co-exists with low serum magnesium levels.56
Primary hypothyroidism involves insufficiency of the thyroid gland itself, for example from thyroiditis or the effects of medications such as lithium or amiodarone.57 The less common phenomenon of secondary hypothyroidism is due to inadequate central stimulation of the gland by the hypothalamus or pituitary. Hypothyroidism typically presents as apathy, psychomotor retardation, and weight gain.38,55,57 However, delirium, psychosis, and anxiety-like symptoms may occur if the onset is acute, a situation sometimes referred to as myxedema madness.38,55 Physical findings supportive of hypothyroidism include a goiter, coarse hair, doughy skin, edema, bradycardia, alopecia of the eyebrows, and delayed relaxation of elicited deep tendon reflexes. An elevated thyroid-stimulating hormone (TSH) assay is diagnostic of hypothyroidism.
Hyperthyroidism can present as anxiety or mania. The dramatic presentation of thyroid storm can be mistaken for a primary psychosis or psychostimulant intoxication. Hyperthyroid elderly patients may present paradoxically with marked psychomotor retardation, apparent depression, and impaired executive function, a condition known as apathetic thyrotoxicosis.38,55,57 Secondary thyrotoxicosis, due to excessive central stimulation, is rare; most cases of hyperthyroidism involve primary glandular hyperactivity as occurs in conditions such as thyroiditis, toxic nodular goiter, and Graves’ disease. Common presenting symptoms of hyperthyroidism include nervousness, insomnia, tremulousness, palpitations, and difficulty concentrating.55,57,58 A careful review of systems may elicit supportive symptoms such as weight loss despite increased appetite; heat intolerance; heavy sweating; and euphoria. On physical exam, the EP may find a palpable thyroid nodule or goiter, and in the case of Graves’ disease, may detect the classic findings of pretibial edema or exophthalmos due to orbital ophthalmopathy. ECG findings in cases of hyperthyroidism may include frequent ectopy and supraventricular tachydysrhythmias, such as sinus tachycardia, AV node re-entrant tachycardia, or atrial fibrillation. ED management of true thyroid storm requires initial stabilization and symptomatic relief with antipyretics, beta-blockade, and benzodiazepines. Prevention of further synthesis and release of T4 is accomplished with administration of propylthiauracyl and iodine; intravenous hydrocortisone can decrease peripheral conversion of T4 to the more active T3.
The earliest symptoms of adrenal insufficiency, especially fatigue and poor appetite leading to weight loss, may mimic depression.55,58 Hypotension, nausea, and vomiting are seen in cases of acute adrenal crisis, along with hyponatremia and hyperkalemia resulting from lack of sufficient aldosterone. Primary adrenal insufficiency results from autoimmune destruction (Addison’s disease), infiltrative disease, or tuberculosis. Patients with primary adrenal failure may demonstrate hyperpigmentation; without cortisol’s negative feedback, the pituitary generates excessive levels of adrenocorticotropic hormone (ACTH), which in turn stimulates dermal melanocytes. Secondary adrenal insufficiency results most commonly from abrupt withdrawal of systemic corticosteroids. The EP aggressively should treat suspected adrenal crisis with volume resuscitation and intravenous hydrocortisone.
The hypercortisolemia of Cushing’s syndrome results from over-stimulation of the adrenals, either due to an ACTH-secreting pituitary adenoma or malignancy-associated ectopic ACTH production. Prolonged therapy with systemic corticosteroids also may cause a Cushing-like syndrome. Depression is quite common in Cushing’s syndrome; other neuropsychiatric symptoms include insomnia, difficulty concentrating, and decreased libido. Iatrogenic Cushing’s syndrome due to steroid therapy is more likely to result in euphoria, mania, or psychosis.58 Patients also may report other physical complaints, including fatigue, weight gain, easy bruising, or polyuria due to hyperglycemia. Physical signs suggestive of the diagnosis include central obesity, purple striae, moon face, and hirsutism.
Pheochromocytomas are rare adrenal tumors of the adrenal medulla that secrete epinephrine and norepinephrine. The resultant excess of circulating catecholamines can trigger paroxysmal attacks of anxiety and panic, often with a sense of impending doom. Physical signs of hypertension, tachycardia, headache, and sweating may occur, and half of affected patients have sustained baseline hypertension.58 The EP cannot make this diagnosis in the ED setting, but can contact the patient's primary care physician and facilitate an outpatient work-up if multiple episodes suggest the diagnosis and the patient is otherwise stable for discharge.
 |
Fever (and a Chill). Body temperature routinely is measured in triage, but can be overlooked or forgotten in the case of violent or presumed psychotic patients transported by paramedics or in the custody of police. Hyper- or hypothermia may occur in the context of both infectious diseases and conditions causing secondary thermal dysregulation, such as adverse drug reactions or environmental exposures. (See Table 8.) Mental status change, particularly encephalopathy and delirium, may be the first clinical sign of systemic sepsis.59 When evaluating an elderly patient with mental status change, the EP should evaluate for common occult infections such as pneumonia or urinary tract infections, and should obtain a screening urinalysis and chest x-ray. Careful palpation of the abdomen may find focal tenderness suggestive of appendicitis or cholecystitis, and may prompt further laboratory screening or imaging studies such as ultrasound or abdominal CT.
Acute bacterial endocarditis may present as fever and mental status changes resembling a panic attack or acute psychosis with hallucinations, particularly in cases of prosthetic valve or intravenous drug abuse-related endocarditis. The most common pathogens in both groups are virulent Staphlycocci species.60,61 The mental status changes observed may represent direct humoral effects on the CNS or microembolic showering of the brain. If acute endocarditis is suspected, blood cultures should be drawn and systemic broad-spectrum antibiotics initiated in the ED. Vancomycin and gentamicin are sufficient coverage for methicillin-resistant Staphlycocci, while an extended-spectrum penicillin or ceftazidime can be added in IV drug-associated cases if Pseudomonas infection is common in the local drug-abusing population.61
Although meningitis in the elderly host may cause mental status changes, in younger adults it typically does not alter behavior or sensorium. The EP should suspect viral encephalitis when a patient presents with mental status change and fever, especially if also is complaint of headache. The most common cause of viral encephalitis in the United States is herpes virus, most commonly HSV-1, which commonly occurs in the under-20 and over-50 age groups. CNS findings typically are generalized, but focal seizures and hemiparesis can occur and are suggestive of the diagnosis. Cerebrospinal fluid may demonstrate a monocytic pleocytosis or elevated protein, but may be completely normal with regard to routine analysis. Polymerase chain reaction assays for HSV DNA antibody can provide a firm diagnosis, albeit in a delayed fashion, and should be added to routine CSF assays when infection beyond simple meningitis is suspected. Because HSV-1 infection commonly localizes to the temporal lobe, CT and magnetic resonance imaging (MRI) may demonstrate a focal lesion or edema that is highly suggestive of the diagnosis, or EEG may demonstrate a characteristic spike and slow wave activity in the temporal area. Treatment for herpes encephalitis is a prolonged course of intravenous acyclovir, and should be initiated empirically in cases of altered mental status and fever, if CT and CSF studies do not reveal a firmer diagnosis. Despite treatment, high mortality and morbidity, including permanent devastating neurologic injury, occurs in more than half of cases. Encephalitis from arthropod-borne viruses may occur in certain endemic areas on a sporadic basis; examples include Western Equine virus in the West and Midwest, or St. Louis encephalitis virus in the Midwest and Mississippi River valley, and West Nile virus. Symptoms of these rare infections include fever and altered mental status, and CSF assays are the only means of diagnosis. There is no specific treatment for these infections, other than supportive care.62-64
Hyperthermia. Heat illness must be in the differential diagnosis for altered mental status and hyperthermia, particularly in warmer climes and the summer months. The earliest manifestations of heat illness may be heat cramps, progressing to signs and symptoms of heat exhaustion such as nausea, vomiting, dizziness, malaise, and tachycardia. Mental status remains normal, and body temperature tends to be normal, but may range as high as 41° C. Treatment for simple heat exhaustion is rehydration with intravenous fluids. Heat stroke involves hyperthermia usually greater than 41° C and mental status changes including confusion, combativeness, and odd behavior. The EP also may detect ataxia on neurologic exam, since the cerebellum is particularly sensitive to hyperthermia. There is a common misconception that patients with heat stroke no longer can respond physiologically to their elevated core temperature and thus stop sweating. Studies have shown that diaphoresis still may occur in advanced heat stroke. Once recognized, heat stroke must be treated aggressively, as duration of hyperthermia correlates with worse outcome, and increases the risk for complications such as acute tubular necrosis and renal failure. In addition to rehydrating the patient with IV fluids, the EP should initiate evaporative cooling techniques; application of mist and fans to promote evaporation are most effective. Placing ice bags at the site of high vascularity, such as the groin and scalp, can promote further heat loss. Benzodiazepines can be efficacious to limit shivering, reducing further heat generation, and to decrease agitation, which facilitates cooperation with cooling.65 The EP must consider neuroleptic malignant syndrome (NMS) in cases of altered mental status and hyperthermia, even if a medication list or past medical history describing neuroleptic therapy is unavailable. First described in 1968, NMS is clinically similar to heat stroke, but has added findings of cogwheel rigidity and overall hypertonicity of the musculature. Acute renal failure from myonecrosis can develop. Treatment is primarily supportive, including hydration, evaporative cooling, and benzodiazepines, although anecdotal improvement with muscle relaxants and dopamine agonists has been reported.66
Hypothermia. Hypothermia can occur year round, particularly in elderly patients and the homeless population. The stuporous, ataxic patient who presents at triage smelling of alcohol may require more than thiamine, folate, hot coffee, and an empty bed to "sleep it off." Hypothermia causes a predictable progression of shivering; mental status changes, including confusion and apathy; loss of shivering (generally below 32° C;) generalized prolongation of ECG intervals; bradycardia; and, ultimately, cardiac arrest due to ventricular fibrillation or, more commonly, aystole. The mildly hypothermic patient, with temperature between 35° and 32° C, requires removal of any wet clothing to prevent further conductive and evaporative loss and simple, passive rewarming with application of warm blankets. Active rewarming and cardiac monitoring are required for patients colder than 32° C. Active rewarming measures include external radiant sources; warmed IV fluids; and warmed, humidified oxygen. The myocardium is electrically sensitive in hypothermia, and patients should be handled gingerly to avoid precipitating ventricular fibrillation.67,68
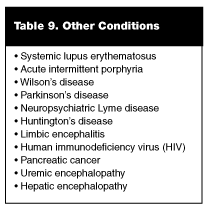 |
Other Conditions. Other medical conditions present with less regularity to the ED, but the astute EP should keep them in the differential diagnosis when evaluating patients with psychiatric complaints. (See Table 9.) Systemic lupus erythematosus (SLE) can cause both psychosis and depression, as well as subtle abnormalities on neuropsychiatric testing. Neurologic effects in SLE are associated with higher titers of antiphospholipid antibody, and thus may be due to occlusive vasculopathy.69 Rare genetic metabolic errors can cause psychiatric symptoms. Acute intermittent porphyria is a condition resulting from a metabolic error in the cascade of reactions that produce heme. It is an autosomal dominant trait, but demonstrates variable penetrance. In susceptible individuals, certain commonly prescribed medications are porphyrinogenic, i.e., they can provoke an attack of porphyria. Examples include antihistamines, sedatives, antibiotics, and anticonvulsants. Consumption of alcohol also can provoke an attack. Symptoms may include abdominal pain, vomiting, and mental status changes, including catatonia, mania, or frank psychosis.70 Wilson’s disease is a rare autosomal recessive disorder of copper metabolism. Psychiatric symptoms, such as depression, labile affect, and emotional outbursts can occur long before appreciation of chronic liver failure or classic physical findings like Kayser-Fleischer rings.71
Progressive neurologic diseases may present atypically with apparent psychiatric symptoms. Patients with Parkinson’s disease can present with panic-like symptoms or psychosis with visual hallucinations and paranoid delusions.72 Neuropsychiatric Lyme disease can present as depression, and should be higher in the differential diagnosis for new onset depression in endemic areas.73 The EP easily could mistake verbal outbursts, odd affect, and odd tics/movements for psychosis in the case of undiagnosed Huntington’s disease.57 Limbic encephalitis, an autoimmune paraneoplastic syndrome, can cause bizarre behavior, agitation, and hallucinations.57
Depression is common in cases of human immunodeficiency virus (HIV) infection, particularly in cases of advanced HIV dementia. Lyketsos et al warn against the "trap of understanding" that is common when dealing with HIV patients; i.e., assuming that anxiety, hopelessness, and depression are normal reactions to an ultimately incurable condition.74 New or acute onset behavioral changes in the case of HIV mandate broader testing, including neuroimaging and CSF analysis.
Symptoms of depression are common in cases of pancreatic carcinoma, and often precede more ominous symptoms like epigastric and back pain, postprandial nausea, and dyspepsia, causing a fear of eating and weight loss. Because pancreatic carcinoma has such a grim prognosis when diagnosed late, it should be considered in cases of new-onset depressive symptoms in the middle-aged patient without obvious psycho-social stressors.75
Uremic and hepatic encephalopathy are included in this discussion for the sake of completeness. Each theoretically could present as isolated mental status or behavioral change in the case of (very) acute organ failure, such as might occur in a case of acute interstitial nephritis or toxin-mediated hepatotoxicity; the acuity of onset would likely prompt broad laboratory investigation and facilitate diagnosis. Typically, patients with chronic hepatic or renal failure have concurrent findings (i.e., anuria, edema, cardiac ectopy, hepatomegaly, jaundice, ascites, asterixis) that are indicative of the underlying pathology.76,77
Conclusion
A definition of adequate medical clearance of presumed psychiatric patients is a frequently contested issue in the ED. EPs must be wary of organic causes of psychiatric symptoms in order to prevent inappropriate admissions to psychiatric units or facilities. Preconceived assumptions regarding psychiatric ED presentations and pitfalls of omission in the evaluation of patients with psychiatric symptoms allow medical mimics to go undetected. A thorough history and physical exam, particularly the neuropsychiatric exam, may clinch a diagnosis of delirium; by definition, delirium has an underlying medical cause. In the case of a geriatric patient with altered mental status or psychiatric symptoms, the EP must assume an organic cause until proven otherwise. Routine testing of serum glucose, electrolytes, and urine toxicology for first-time presentations of altered mental status is clearly beneficial in all age groups; some limited retrospective data suggest that no testing is required in patients with prior psychiatric presentations, normal exam and vital signs, and no other co-morbidities. Nevertheless, the prudent EP should approach each case as unique, and have a low threshold to judiciously expand the work-up when appropriate.
Numerous medical conditions frequently encountered in the ED can mimic psychiatric disorders, including acute cardiopulmonary and cerebrovascular diseases; medication and illicit drug effects; metabolic and electrolyte derangements; infectious diseases causing sepsis; and environmental exposure. The ABC mnemonic can be used by the EP as a logical framework for the broad differential diagnosis of medical mimics that may be missed during a hurried or cursory evaluation.
References
1. Tintinalli JE, Peacock FW, Wright MA. Emergency medical evaluation of psychiatric patients. Ann Emerg Med 1994;234:859-862.
2. Reeves RR, Pendarvis EJ, Kimble R. Unrecognized medical emergencies admitted to psychiatric units. Am J Emerg Med 2000; 18(4):391-393.
3. Lagomasino I, Daly R, Stoudemire A. Medical assessment of patients presenting with psychiatric symptoms in the emergency setting. Psych Clin North Am 1999;22(4):819-850.
4. Williams ER, Shepherd S. Medical clearance of psychiatric patients. Emerg Med Clin North Am 2000;18(2):185-198.
5. Marsh C. Psychiatric presentations of medical illness. Psych Clin North Am 1997;20(1):181-204.
6. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 4th Ed. Washington, DC, American Psychiatric Association, 1994.
7. Korn CS, Currier GW, Henderson SO. "Medical clearance" of psychiatric patients without medical complaints in the emergency department. J Emerg Med 2000;18(2):173-176.
8. Roberts JR, Watson S, Siegel E. Mnemonic for diagnosis of acute mental status change. Ann Emerg Med 1990;19(2):221-222.
9. Lee LC, Shah K. Clinical manifestations of pulmonary embolism. Emerg Med Clin North Am 2001;19(4):925-942.
10. Weiner SG, Burstein JL. Nonspecific tests for pulmonary embolism. Emerg Med Clin North Am 2001;19(4):943-956.
11. Kline JA, Johns KL, Colucciello SA, et al. New diagnostic tests for pulmonary embolism. Ann Emerg Med 2000;35(2):168-180.
12. Kline JA, Meek S, Boudrow D, et al. Use of the alveolar dead space fraction (Vd/Vt) and plasma d-dimers to exclude acute pulmonary embolism in ambulatory patients. Acad Emerg Med 1997;4(9): 856-863.
13. Amitai Y. Neuropsychological impairment from acute low-level exposure to carbon monoxide. Arch Neurol 1998;55(6):845-848.
14. Trimble MR, Krishnamoorthy ES. The role of toxins in disorders of mood and affect. Neurol Clin 2000;18(3):649-664.
15. Sinex JE. Pulse oximetry: Principles and limitations. Am J Emerg Med 1999;17(1):59-66.
16. Touger M, Gallagher EJ, Tyrell J. Relationship between venous and arterial carboxyhemoglobin levels in patients with suspected carbon monoxide poisoning. Ann Emerg Med 1995;24(4):481-483.
17. Burney RE, Wu S, Nemiroff MJ. Mass carbon monoxide poisoning: Clinical effects and results of treatment of 184 victims. Ann Emerg Med 1982;11(8):394-399.
18. Myers RA. Carbon monoxide poisoning. J Emerg Med 1984;1(3): 245-248.
19. McCrory DC, Brown C, Gelfand SE, et al. Management of acute exacerbations of COPD. A summary and appraisal of published evidence. Chest 2001;119(4):1190-1209.
20. Vicario S. Emergency presentation of subdural hematoma: A review of 85 cases diagnosed by computerized tomography. Ann Emerg Med 1982;11(9):475-477.
21. Vilke GM, Chan TC, Guss DA. Use of a complete neurological examination to screen for significant intracranial abnormalities in minor head injury. Am J Emerg Med 2000;18(2):159-163.
22. MacHale SM, O’Rourke SJ, Wardlaw JM, et al. Depression and its relation to lesion location after stroke. J Neurol Neurosurg Psychiatry 1998;64(3):371-374.
23. Filley CM, Kleinschmidt-DeMasters BK. Neurobehavioral presentations of brain neoplasms. West J Med 1995;163(1):19-25.
24. Tardiff K. Unusual diagnoses among violent patients. Psych Clin North Am 1998;21(3):567-576.
25. Pringle AM, Taylor R, Whittle IR. Anxiety and depression in patients with an intracranial neoplasm before and after tumour surgery. Br J Neurosurg 1999;13(1):46-51.
26. Aronow WS, Tresch DD. Management of the older patient with acute myocardial infarction: Difference in clinical presentation between older and younger patients. J Am Geriatr Soc 1998;46(9): 1157-1162.
27. Tresch DD. Atypical presentations of cardiovascular disorders in the elderly. Geriatrics 1987;42(10):31-36, 40-41, 44-46.
28. Ghaemmaghami CA, Brady WJ. Pitfalls in the emergency department diagnosis of acute myocardial infarction. Emerg Med Clin North Am 2001;19(2):351-369.
29. Maheshwari A, Laird-Flick HS, Cannon LA, et al. Acute MI: Age-related presentations and treatment options. Geriatrics 2000;55(2): 32-40.
30. George JN, Vesely SK. Thrombotic thrombocytopenic purpura-hemolytic uremic syndrome: Diagnosis and treatment. Cleve Clin J Med 2001;68(10):857-877.
31. Garrett WT, Chang CW, Bleck TP. Altered mental status in thrombotic thrombocytopenic purpura is secondary to nonconvulsive status epilepticus. Ann Neurol 1996;40(2):245-246.
32. Varon J and Marik PE. The diagnosis and management of hypertensive crises. Chest 2000;118(1):214-227.
33. Hoshide S, Kario K, Fujikawa H, et al. Hemodynamic cerebral infarction triggered by excessive blood pressure reduction in hypertensive emergencies. J Am Geriatri Soc 1998;46(9):1179-1180.
34. Brust JC. Acute neurologic complications of drug and alcohol abuse. Neurol Clin 1998;16(2):503-519.
35. Weiss RD, Greenfield SF, Mirin SM. Intoxication and withdrawal syndromes. In: Hyman SE and Tesar GE, ed. Manual of Psychiatric Emergencies, 3rd edition. Boston, MS: Little, Brown, and Co.; 1994:279-293.
36. Li J, Stokes SA, Woeckner A. A tale of novel intoxication: Seven cases of gamma-hydroxybutyric acid overdose. Ann Emerg Med 1998;31(6):723-728.
37. Hyman SE. Alcohol-related emergencies. In: Hyman SE and Tesar GE, ed. Manual of Psychiatric Emergencies, 3rd edition. Boston, MS: Little, Brown, and Co.;1994:294-303.
38. Talbot-Stern JK, Green T, Royle TJ. Psychiatric manifestations of systemic disease. Emerg Med Clin North Am 2000;18(2):199-209.
39. Dyer JE, Roth B, Hyma BA. Gamma-hydroxybutyrate withdrawal syndrome. Ann Emerg Med 2001;37(2):147-153.
40. Bender B, Milgrom H. Neuropsychiatric effects of medications for allergic diseases. J Allergy Clin Immunol 1995; 95(2):523-528.
41. Sauder KL, Brady WJ, Hennes H. Visual hallucinations in a toddler: Accidental ingestion of a sympathomimetic over-the-counter nasal decongestant. Am J Emerg Med 1997;15(5):521-526.
42. Murray S, Brewerton T. Abuse of over-the-counter dextromethorphan by teenagers. South Med J 1993;86(10):1151-1153.
43. Wolfe TR, Caravati EM. Massive dextromethorphan ingestion and abuse. Am J Emerg Med 1995;13(2):174-176.
44. Nelson L, Perrone J. Herbal and alternative medicine. Emerg Med Clin North Am 2000;18(4):709-722.
45. Alao AO, Yolles JC, Armenta W. Steroid-induced psychosis: An unusual presentation of a case. Resid Staff Physician 2002;48(1): 25-28.
46. Jiang HK, Chang DM. Non-steroidal anti-inflammatory drugs with adverse psychiatric reactions: Five case reports. Clin Rheum 1999; 18(4):339-345.
47. Sorgi P, Ratey J, Knoedler D, et al. Depression during treatment with beta-blockers: Results from a double-blind placebo-controlled study. J Neuropsychiatry Clin Neurosci 1992;4(2):187-189.
48. Gerstmann BB, Jolson HM, Bauer M, et al. The incidence of depression in new users of beta-blockers and selected antihypertensives. J Clin Epidemiol 1996;49(7):809-815.
49. Ried LD, McFarlan BH, Johnson RE, et al. Beta blockers and depression: The more the murkier? Ann Pharmacotherapy 1998; 32(6):699-708.
50. Bright RA, Everitt DE. Beta-blockers and depression. Evidence against an association. JAMA 1992;267(13):1783-1787.
51. Mason PJ, Morris VA, Balcezak TJ. Serotonin syndrome. Presentation of two cases and review of the literature. Medicine 2000;79(4): 201-209.
52. Drotts DL, Vinson DR. Prochlorperazine induces akathisia in emergency patients. Ann Emerg Med 1999;34(4):469-475.
53. Brady WJ, Duncan CW. Hypoglycemia masquerading as acute psychosis and acute cocaine intoxication. Am J Emerg Med 1999;17(3):318.
54. Malouf R, Brust JC. Hypoglycemia: Causes, neurological manifestations, and outcome. Ann Neurol 1985;17(5):421-430.
55. Hutto B. Subtle psychiatric presentations of endocrine diseases. Psych Clin North Am 1998;21(4):905-916.
56. Gibbs MA, Wolfson AB, and Tayal VS. Electrolyte disturbances. In: Rosen B, Barkin R, et al, ed. Emergency Medicine: Concepts and Clinical Practice, 4th edition. St.Louis, MO: Mosby-Year Book, Inc.;1998:2432-2456.
57. Bierer MF, Bierer BE. Psychiatric symptoms of medical illness and drug toxicity. In: Hyman SE and Tesar GE, ed. Manual of Psychiatric Emergencies, 3rd edition. Boston, MS: Little, Brown, and Co.; 1994:214-245.
58. Tardiff K. Unusual diagnoses among violent patients. Psych Clin North Am 1998;21(3):567-576.
59. Papadopoulos MC, Davies DC, Moss RF, et al. Pathophysiology of septic encephalopathy: A review. Crit Care Med 2000;28(8): 3019-3024.
60. Harrison EC, Rashtian MY, Allen DT, et al. An emergency physician’s guide to prosthetic heart valves: Valve-related complications. Ann Emerg Med 1988;17(7):704-710.
61. Roberts R, Slovis CM. Endocarditis in intravenous drug abusers. Emerg Med Clin North Am 1990;8(3):665-680.
62. Whitley RJ, Kimberlin DW. Viral encephalitis. Pediatr Rev 1999; 20(6):192-198.
63. Whitley RJ. Viral encephalitis: Familiar infections and emerging pathogens. Lancet 2002;359(9305):507-513.
64. Whitley RJ. Herpes simplex virus infections of the central nervous system: Therapeutic and diagnostic considerations. Clin Infect Dis 1995;20(2):414-420.
65. Waters TA. Heat illness: Tips for recognition and treatment. Cleve Clin J Med 2001;68(8):685-687.
66. Guze BH, Baxter LR. Neuroleptic malignant syndrome. N Engl J Med 1985;313(3):163-166.
67. Lloyd EL. Accidental hypothermia. Resuscitation 1996;32:111-124.
68. Scaletta TA, Schaider JJ. Emergent Management of Trauma. New York, NY: McGraw-Hill;1996:324-329.
69. Mok CC, Lau CS, Wong RW. Neuropsychiatric manifestations and their clinical associations in southern Chinese patients with systemic lupus erythematosus. J Rheumatol 2001;28(4):766-771.
70. Crimlisk HL. The little imitator—porphyria: A neuropsychiatric disorder. J Neurol Neurosurg Psychiatry 1997;62:319-328.
71. Akil M. Psychiatric and behavioral abnormalities in Wilson’s disease. Adv Neurol 1995;65:171-178.
72. Factor SA, Molho ES. Emergency department presentations of patients with Parkinson’s disease. Am J Emerg Med 2000;18(2): 209-215.
73. Fallon BA, Kochevar JM, Gaito A, et al. The underdiagnosis of neuropsychiatric Lyme disease in children and adults. Psych Clin North Am 1998;21(3):693-703.
74. Lyketsos CG, Fishman M, Treisman G. Psychiatric issues and emergencies in HIV infection. Emerg Med Clin North Am 1995;13(1): 163-177.
75. Joffe RT, Rubinow DR, Denicoff KD, et al. Depression and carcinoma of the pancreas. Gen Hosp Psychiatry 1986;8:241-245.
76. Wolfson AB. Chronic renal failure and dialysis. In: Rosen B, Barkin R, et al, ed. Emergency Medicine: Concepts and Clinical Practice, 4th edition. St. Louis, MO: Mosby-Year Book, Inc.;1998: 2278-2293.
77. Jones EA. Pathogenesis of hepatic encephalopathy. Clin Liver Dis 2000;4(2):467-485.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
