Medical Problems of Diving and the Primary Care Physician — Part I
Authors: Michael B. Strauss, MD, FACS, AAOS, Medical Director of the Baromedical Department, Long Beach Memorial Medical Center, Long Beach California, Clinical Professor, Orthopaedic Surgery, University of California Irvine College of Medicine, Irvine, Calif; and Igor V. Aksenov, MD, PhD, Associate Dean and Professor, Saba University School of Medicine (Saba, Netherlands-Antilles), Director, Hyperbaric Medicine Program, Medical Director, Saba Marine Park.
Editor’s Note—About half of the referrals that Doctors Strauss and Aksenov receive concerning medical problems of diving (MPD) come via the divers’ primary care physicians (PCPs). Consequently, with 5 million certified SCUBA (Self-Contained Underwater Breathing Apparatus) divers and perhaps 10 times this number of recreational swimmers and snorkelers, it is important for the PCP to be aware of the MPD, to recognize which ones need primary care management as the definitive treatment, and to know which ones require referral to an undersea and hyperbaric medicine specialist.
The following article by Strauss and Aksenov provides direction to the PCP for managing the medical problems of diving. Their experiences (as evidenced by their credentials and many citations in the references) provide logical and medically sound advice for the management and prevention of the MPD.
This paper includes several special features, in addition to the currently accepted management for the MPD. These include: 1) using a "clinically" friendly approach to classify the MPD based on the portion of the dive in which they are most likely to occur; 2) appropriate attention to the less infamous but more frequently occurring MPD (ie, putting the MPD in a perspective with respect to their frequency of occurrence); 3) a logical organization so the PCP can focus onto a problem to which he/she needs to refer; 4) effective use of tables to supplement the text and to provide immediate information pertinent to the MPD; 5) using the "stresses" the sports diver will encounter in the water environment as a basis for understanding the pathophysiology of the MPD; and 6) explaining the role of the PCP in the medical evaluation for fitness to dive.
The PCP has a special opportunity to become involved in the care of patients who are divers. With information in this report, the PCP will have the information to do so appropriately, and with confidence, as well as to recognize which MPD require the expertise of undersea and hyperbaric medicine trained physicians and the need for hyperbaric oxygen recompression treatments. Finally, through continuing medical education programs and references cited at the end of the text, the PCP has the opportunity to become an "expert" on this subject as well.
Introduction
MPD are not usually considered in the scope of practice of the PCP. However, the first physician contact a sports diver makes after an MPD occurs could be the PCP since most diving problems do not require the expertise of an undersea medicine trained physician and the use of a recompression chamber. Exceptions such as decompression sickness, arterial gas embolism, and altered mental status after hypoxic brain injury (ie, near drowning) occur infrequently in the total scope of sports diving activities. The goals of this report are 3-fold: 1) to introduce the PCP to the subject of diving medicine and physiology; 2) to review in a logical fashion the MPD that occur in sports diving; and 3) to explain the essential components of the fitness-to-dive evaluation including which conditions are contraindicated for diving. With the information from this paper the PCP should be comfortable in evaluating and managing the majority of the MPD as well as recognize which problems require referral for specialized care such as hyperbaric oxygen recompression treatments.
Physicians in remote diving sites are not necessarily insulated from MPD due to the accessibility of diving sites via airplane transportation. It is estimated that there are 5 million certified SCUBA divers in the United States.1 Perhaps 10% dive one or more times a week, while approximately 50% limit their diving activities to 1-2 exotic trips where they may dive 20 or more times in a few days. The reality of the situation is that millions of SCUBA divers dive each year, yet serious diving problems occur very infrequently. For example, it is estimated that 2-3 episodes of decompression sickness occur for every 10,000 SCUBA dives.2 However, the actual incidence is unknown and is probably higher due to under reporting. Even though the number of sports SCUBA divers has increased 10-fold in the past 2 decades, the death rate from diving accidents has remained level at about 100 per year.3 Five observations help to understand the frequency of occurrence and the variety of presentations of the MPD. First, MPD are either fatal or nonfatal (see Figure 1).
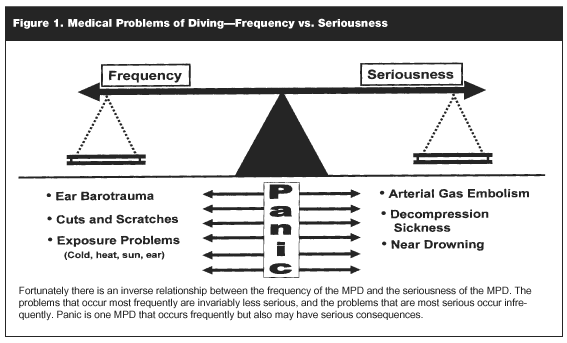 |
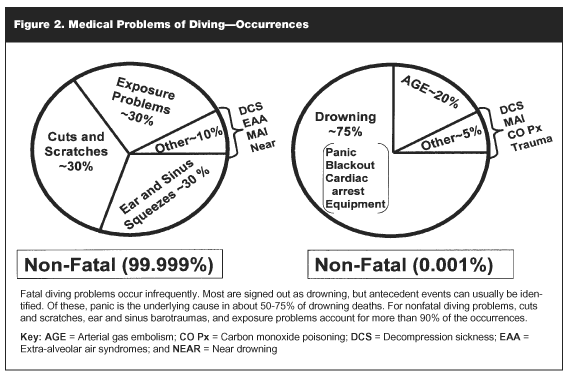
The number of fatal diving accidents is almost infinitesimal compared to the number of nonfatal problems. Second, of the nonfatal MPD, the majority are within the scope of practice of the nondiving medicine-trained PCP. Third, most nonfatal MPD are so minor that the first-line, nonphysician response is almost always adequate to manage the problem. However, the diver may contact the PCP for advice and whether further evaluation and management are necessary. Fourth, only a very small percentage of MPD are actually due to the breathing of compressed gases. Finally, the most serious diving problems occur infrequently while the most frequent diving problems usually do not have serious consequences (see Figure 2).
 |
An Introduction to Diving Medicine and Physiology
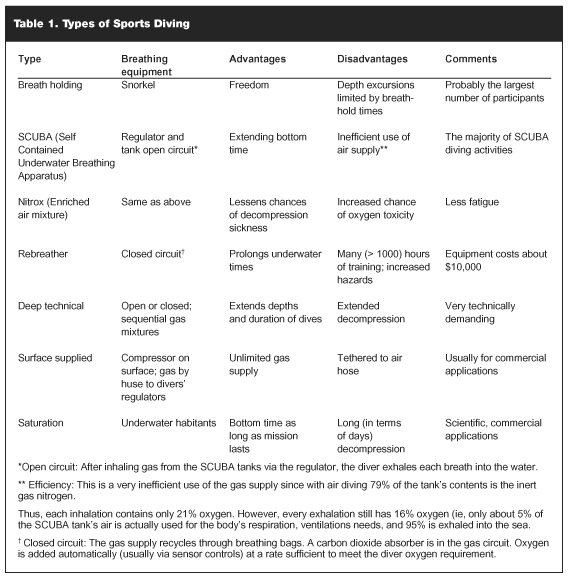
Sports divers use a variety of diving techniques from snorkeling to closed circuit SCUBA gear (see Table 1). The distinction between the sports diver and the commercial diver today is no longer as clear as it was in the past, when among other things the commercial diver used equipment unavailable to the sports diver. Today, in our opinion, the main distinction between the commercial and the sports diver is the former gets paid for his/her diving activity while the sports diver does not. However, the likelihood of the PCP treating a commercial diver, or deep technical diver, is much less than a sports diver. This is because commercial and deep technical divers usually establish a network of professional contacts during their training and in association with their diving activities. The network is likely to include physicians with special training in undersea medicine, as well as locations of recompression chambers and alternatives for emergency transport from diving sites to chambers. When diving activities of commercial divers are judged to be hazardous, Occupational and Safety Health Agency (OSHA) has directives such as requiring a recompression chamber at the diving site. Nonetheless, the PCP may be the first contact for nonemergency-related diving conditions from these divers such as joint pains, arthritis symptoms from bone necrosis, aquatic dermatidities, festering wounds from marine animal injuries, chronic infections from marine microbes, chronic sinusitis, and chronic Eustachian tube dysfunction.
 |
The undersea environment imposes many challenges for the divers who do not have terrestrial counterparts. These include ventilation, hydrostatic, thermal, and orientation/ psychological stresses. Through invention and ingenuity, the sports diver is able to modify these stresses to make almost all sports diving activities safe and enjoyable. An analysis of these stresses provides the basis for understanding diving medicine and physiology as well as the MPD.
Ventilation Stresses. The human body is not adapted to extract oxygen from water as fish and other species are. The amount of oxygen in seawater is about 1/40th of that in air. Although fluid breathing has many theoretical advantages for diving, such as eliminating the need to use an inert gas to dilute oxygen and eliminating pulmonary barotrauma, it is not practical at this time. In addition, the viscosity of water and the difficulty with carbon dioxide elimination place fluid respiration in the realm of science fiction at this stage of our knowledge.
One method to meet the ventilation stresses of going underwater is to breath-hold for brief depth excursions. Breath-holding durations are limited, usually 1-2 minutes at most, but with training these times can improve markedly. The physiology of breath-hold diving is fascinating and, in the human, incorporates many of the adaptations seen in diving mammals and other aquatic animals.4 Suffice it to say, the adaptations center around the oxygen conserving reflex that includes preferential shunting of blood to critical organs, bradycardia, increased tolerance to hypercapnia and improved oxygen extraction from blood. The oxygen conserving reflex is particularly relevant for understanding the pathophysiology of the "no panic" syndromes (ie, diver blackout) and near drowning which will be discussed later. The breath-hold diver should not mix breath-hold diving with a buddy using SCUBA or surface-supplied gear while underwater. If breath holding is continued during ascent after breathing compressed gas, the diver is at risk for lung rupture.
The other method to meet the ventilation stresses of diving is to provide a gas supply to the diver while he/she is underwater. Of course, this defines SCUBA diving and surface supplied (Tethered air hose) diving. As desirable as these technological achievements are, they incur side effects for the diver. Diving beyond 30-ft depths using 100% oxygen imposes unacceptable risks for seizures secondary to oxygen toxicity. To maintain oxygen at a safe level in the diver’s gas supply, it is diluted with an inert gas.
For ordinary SCUBA diving activities, air with 79% nitrogen is convenient and safe. However, the inert gas (nitrogen) causes problems for the diver also. With increasing pressure, as the diver descends, inert gas is deposited into all of the body’s tissues. The amount of tissue inert gas saturation is a function of depth, duration of the dive, gas mixtures, and blood flow. The first 3 items can accurately be calculated, but the latter (blood flow) cannot. This is because the flow of the 5 L of blood in the human body is distributed through a vascular system that has an estimated capacity of 150 L associated with a 24-fold potential venous system compliance, 20-fold alterations in muscle blood flow, venous reservoirs, sinusoids, and plexuses, arterial elasticity, and arterial-venous shunting.5 Therefore, blood flow must be highly regulated by neurointegretion of the vasomotor system. Critical tissues like the brain and heart have high blood flows while noncritical tissues like bone and ligaments do not. Alterations in the regulation of blood flow that deprive critical tissues of their perfusion needs through diversion of the 5 L finite blood volume to noncritical tissues and/or "storage" in the vast capacity of the vascular system may cause shock and loss of consciousness as well as set the conditions for decompression sickness to occur.
For diving physiology purposes, critical tissues, which also include lung and blood, are designated "fast" tissues because of the rapidity with which they saturate with the inert gas during the dive, and with which they release the inert gas during ascent and after the dive is completed. Noncritical tissues that also include joint capsules and adventitial tissues (eg, sheaths around nerves) are designated "slow" tissues because of the slowness of these processes. Rather than try to define the saturation/desaturation rates of each body tissue, diving physiologists use the concept of tissue half times, ie, the time it takes a theoretical tissue to become half saturated with the inert gas at the new depth. Fast tissues have tissue half-times of 5 minutes or less. Slow tissues may have half-times that are 240 minutes or longer. If the diver stays at depth long enough, all tissues eventually saturate with the inert gas. Further time on the bottom does not impose any additional gas load for the diver. This defines saturation diving. The technique is very useful for long, deep commercial dives or habitat diving for scientific studies. Whereas, a 1000-ft dive for 30-minute bottom time requires 5 days of decompression, a saturation dive to this depth allows the divers to stay and work an unlimited amount of time at depth and then decompress one time only (which may take 7-10 days). Naturally, while on land all tissues in our bodies are saturated with nitrogen at (or about) sea level.
During ascent and after surfacing when inert gas release from tissues to the bloodstream and exchange to the outside environment by the lungs exceeds the body’s capacity to handle the gas load, bubbles form in tissues and cause decompression sickness. If clinically significant bubbling occurs in nerve tissue, neurological problems occur; if in the bloodstream, hemodynamic shock will be observed; if in the joints, bends pain is noted; if in the lungs, chokes (ie, the Behnke triad of, tachypnea, bradycardia, and hypotension); and in the bones, dysbaric osteonecrosis. Normally, even with safe and acceptable ascents from dives, bubbles in the bloodstream are detectable by Doppler techniques. The diver remains asymptomatic as long as the bubble load is not overwhelming and is harmlessly exchanged to the outside environment with ventilation. Decompression sickness is not confined to diving alone. If we ascend rapidly enough and high enough into the atmosphere, our tissues will form bubbles just like ascending from the depths of water. This condition is termed aviator bends or altitude decompression sickness.
The dive computer has revolutionized sports SCUBA diving. Whereas, use of dive tables is based on the assumption that the deepest part of the dive is considered to be the depth of the entire dive, the dive computer considers the time at each depth. Consequently, the sports diver may do a bounce dive to 100 ft for less than a minute and then spend the rest of his/her dive time at the 50-ft depth. If dive tables were used for this profile, the diver would be limited to a 25-minute bottom time based on the maximum depth of the dive. However, the dive computer is able to appreciate that only a small amount of inert gas enters the tissues during the 1-minute time at maximum depth so the diver can spend an hour or more at the 50-ft depth. In addition, the dive tables impose restrictions of limiting dives to 2 in a 12-hour period. The diver, using the dive computer, many dive 4-5 times in this period of time since the computer more accurately reflects what the actual saturation and desaturation of the diver’s tissues are with respect to the inert gas.
The inert gas, nitrogen, poses an additional problem—namely narcosis. With increasing pressure, nitrogen acts like an anesthetic gas. This may lead to confusion, delirium, and unconsciousness and is similar to acute alcohol ingestion. The narcotic effect of nitrogen for each 50 ft of descent is said to be equivalent to drinking 1 martini. At a 200-ft depth (equivalent to drinking 4 martinis), the diver should expect to be quite narcotized. To avoid this, helium, an inert gas (lacking narcotic properties) is used for deeper dives. Deep technical divers may switch gases, that is, use sequential gas mixtures (this requires separate tanks for each) during a dive to avoid inert gas narcosis and possibly minimize decompression time.
Two other stresses are associated with ventilation but are usually of minimal significance to the sports diver. First, there is increasing viscosity of breathing compressed gas as depths increase. At 1000 ft there is a noticeable increased work of breathing from this effect. Second, compressed gas is dehumidified. Fluid from the diver’s respiratory epithelium is required to moisturize and warm the inhaled gas. With each doubling of atmospheric pressure, the fluid and heat requirements double because of the increased density of the compressed gas. This can lead to dehydration hypothermia and sludging, which may be precursors to decompression sickness.
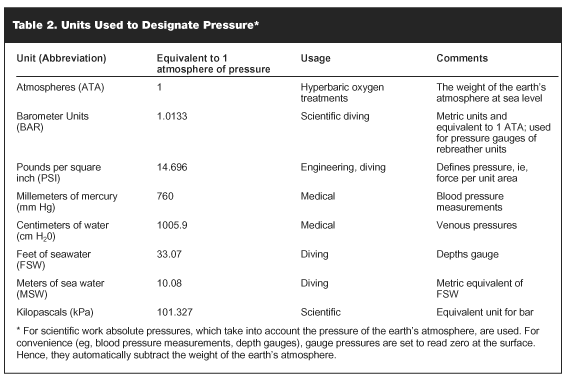
Hydrostatic (Pressure) Stresses: Hydrostatic stresses refer to the effect pressure and water density have on the diver. Water is 775 times as dense as air. This benefits the diver by providing buoyancy, but it also necessitates the use of weights to remain submerged especially if buoyanted by a diving suit. If the diver is neutrally buoyant, he or she may hover at any depth very much like a bird flying through the air. Density also impedes movement so swim fins are needed for propulsion. Pressure effects occur because of the "weight" of water. Many different units are used to designate pressure (see Table 2). Because of the density of water, a descent to 16 ft in the sea would have as much pressure changes on the body as descending from an 18,000 foot altitude to sea level. Fortunately, except for a few exceptions, the human body tolerates pressure at any depth without harmful effects from the pressure. This is because the human body is essentially a "bag of water" and correspondingly transmits pressure ala Pascal’s principle equally and undiminished in all directions. When horizontal in the water, the 1-foot gradient between the front and backsides of the body has no physiological consequences. When the diver is vertical in the water, the pressure gradient is sufficient to help mobilize fluid from the legs to the core of the body.
 |
The exceptions to the body tolerating pressure without any consequences are the air-filled cavities with flexible walls (eg, the gut) and the air-filled spaces with rigid walls (eg, the middle ear cavities). The former structures ordinarily collapse like a balloon subject to external pressurization in accordance with Boyle’s Law (ie, the volume of a gas is inversely proportional to the pressure around it). The air-filled rigid walled cavities, however, cannot collapse. A pressure differential arises as pressure increases with descent. This leads to swelling of the mucosal tissues, leakage of fluid, and bleeding into the cavities. Rupture of the tympanic membrane signals the end point of the continuum and with this event the pressure differential with the outside environment is obliterated. These events define the pathophysiology of ear and sinus squeezes and will be discussed further in Part II.
Thermal Stresses. The physical properties of water cause substantial challenges to the sports divers’ heat-conserving mechanisms.4 The specific heat of water is 1000 times greater than air. That is to say, it takes 1000 times more energy to heat a given volume of water 1 degree centigrade than it does to heat an equal volume of air the same amount. Furthermore, water conducts heat about 25 times as rapidly as air does. This means that survival in water can be measured in terms of minutes as compared to hours for survival in air of equal temperatures. Sudden exposure to near-freezing water such as in accidental immersions causes involuntary gasps for air. If the victim’s head is submerged, water will be aspirated and drowning is likely to occur. During World War II, more deaths of downed aviators in the cold North Seas waters were attributed to this than from any other cause.
Technology, as in dealing with ventilation challenges, makes hypothermia a preventable occurrence for the sports diver. Neoprene wet suits serve as insulation between the diver’s body and the surrounding cold water. Dry suits, which essentially separate the diver from the cold water with water-tight seals are more effective than the wet suit for protecting the diver from hypothermia. With thermal underwear placed between the dry suit and the diver, diving in near freezing water is possible with minimal cold stress.
In spite of this, thermal challenges still exist for the sports diver. For example, with descent and increasing pressure, the air cells in the neoprene wet suit compress and lose their effectiveness as an insulator. To aggravate the cold challenges, water typically becomes colder with increasing depths. There is layering of warm and cold masses of water especially in lakes, ponds, and quarries. This defines a thermocline. Consequently, on the surface the diver may feel entirely comfortable with his or her "100% efficient" neoprene wet suit, whereas at the 100-ft depth (4 atmospheres of pressure), the compression effect could substantially reduce the wet suit’s effectiveness (Theoretically 4-fold according to Boyle’s Law). This could cause the diver to chill rapidly.
Another occult thermal challenge for the sports diver is insensible heat loss associated with ventilation. About 25% of the body’s insensible heat losses are via the lungs. Respiratory heat loss occurs almost entirely by convection from the body’s heat stores. Thermoregulatory mechanisms such as shunting and vasoconstriction do not alter this mode of core heat loss. As previously mentioned, inhaled air must be warmed to body temperature by the time it reaches the terminal bronchi. If not, bronchospasm occurs. If the pressure is doubled, with diving to a 33-ft depth, the insensible heat loss is twice as great since each breath will contain twice as many molecules of air as required at sea level (1 atmosphere of pressure). At the 100-ft depth, the requirements are quadrupled because the pressure (and number of molecules of gas to warm) is 4 times as great as on the surface. Air warming devices are required for commercial divers when diving at great depths in cold water. At 1000-ft depth, hypothermia develops after only a few breaths in the cold environment even when wearing thermal protective clothing.
The clinical consequences of hypothermia can be insidious. It may contribute to other problems such as nitrogen narcosis, near drowning/drowning (especially if loss of manual dexterity interferes with the diver’s ability to free himself or herself from entanglements), exhaustion, fatigue, and rapid depletion of air supply. Another potentially serious problem of hypothermia is the precipitation of bradycardia or other heart arrhythmias. This may be the cause of some of the "unexplainable" drowning deaths of divers. The clinical effects of hypothermia correlate closely with the declines in core temperature. After the initial feelings of discomfort (with or without chilling) and chilling, which defines mild hypothermia with core temperatures in the 95°F to normal range, loss of manual dexterity and altered mental status occur. This defines moderate hypothermia and is associated with core temperatures of 90-95°. Loss of consciousness, arrhythmias, and respiratory arrest are manifestations of severe hypothermia and are observed when core temperatures are below 90°. A good principle for diving in cold water is that if shivering occurs the diver should exit the water and rewarm since shivering is a reliable sign of impending hypothermia.
Orientation and Psychological Stresses. The aquatic environment is not a "friendly place" with respect to the sports diver’s 5 senses. Vision is distorted by the water, causing cornea interface of the eye. A diving mask mitigates this effect by providing an air space between these 2 surfaces but limits peripheral vision and creates a rigid walled, air-filled cavity subject to facemask squeezes. The opacity of the water, which is highly variable due to turbidity, depth, sunlight obliquity, and plankton, limits distance vision. At night everything is "dark" except for the cone of light generated by the diver’s underwater lantern. Water filters out colors of the visible light spectrum. At the 30-ft depth, red disappears and yellow colors are lost at approximately 75 ft. All objects become a monotonous blue-grey color. With increasing depths, illumination is progressively lost. With loss of visual cues, the diver may become disoriented as to direction and panic. Even more serious is the loss of equilibrium sensation from ear barotrauma coupled with the losses of visual cues. In the disoriented state, the diver may think he or she is ascending, but in reality is descending into oblivion.
Although sound conduction in water is about 25 times as great as in air due to the density of water, auditory acuity is impaired. Audible speech is not possible without an air interface between the mouth and the water, a conducting or transmitting system for the sounds (eg, phone line) and a similar interface between the water and the ear. Furthermore, ear barotrauma is one of the most frequent problems of the sports diver. With fluid and/or blood accumulation in the middle ear space, sound perception is diminished. For communications while underwater, the sports diver needs to rely on hand signals and other forms of nonverbal communication, eg, witnessing the dive buddy swimming off in another direction indicating there is some interesting marine life to see, or "struggling" to stay down indicating buoyancy problems.
Obviously other sensations in the body are equally impaired such as taste, feeling, and smelling because of the water environment and the use of diving equipment. Ordinarily these go unnoticed due to the panorama of the underwater environment that is perceived by vision. Although the rule for the sports diver is "look, but don’t touch," the wearing of gloves is desirable for cold protection of the hands and avoidance of stings, cuts, and scratches from accidental contact with objects in the marine environment. These may occur unavoidably, for example, from a wave surge impaling a diver into barnacle encrusted rocks. Diving gloves markedly diminish tactile sensation and can make such safety procedures as unsheathing a knife, adjusting a strap, zipping up a wet suit, etc, very difficult. When a diver loses control in the water, panic is likely to develop. This is one of the most important medical problems of the sports diver.
Part II of this article will cover the medical problems of the sports diver, including panic, diver blackout, exposure problems, injuries from marine animals, descent problems, ascent problems, arterial gas embolism, decompression sickness, complications from medical problems of diving, near drowning/drowning, shock, and cardiac arrest.
References
1. Melamed Y, Shupak A, Bitterman H. Medical problems associated with underwater diving. N Engl J Med. 1992;326:30-35.
2. Bove AA. Risk of decompression sickness with patent foramen ovale. Undersea Hyperb Med. 1998;25(3):175-178.
3. Report on Decompression Illness and Diving Fatalities. Dovenbarger J, Ugiccioni D, eds. Durham, NC:Divers Alert Network; 1999.
4. Strauss MB. Physiological aspects of mammalian breath-hold diving; A review. Aerospace Med. 1970;41:1362-1381.
5. Textbook of Medical Physiology. 10th ed. Guyton AC, Hall JE, eds. 2000, Philadelphia, PA: WB Saunders; 2000:144-194.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
