Medical Problems of Diving and the Primary Care Physician — Part II
Authors: Michael B. Strauss, MD, FACS, AAOS, Medical Director of the Baromedical Department, Long Beach Memorial Medical Center, Long Beach California, Clinical Professor, Orthopaedic Surgery, University of California Irvine College of Medicine, Irvine, Calif; and Igor V. Aksenov, MD, PhD, Associate Dean and Professor, Saba University School of Medicine (Saba, Netherlands-Antilles), Director, Hyperbaric Medicine Program, Medical Director, Saba Marine Park.
Editor’s Note—Information from Part I of this manuscript is helpful for understanding the "how and why" of medical problems of diving. Now it is time to consider the actual medical problems associated with diving that the sports diver might incur. An easy and logical method for discussing medical problems of diving is to consider at what time of the diving activity they are most likely to appear. A dive can be divided into 4 phases: 1) Surface; 2) Descent; 3) Bottom; and 4) Ascent. For each phase, certain medical problems may occur (see Figure 1). Except for the problems associated with ascent, a problem likely to occur at a particular phase of a dive does not exclude it from occurring at other times in the dive. Problems such as cardiac arrest, near drowning/drowning, and shock while diving are frequently a consequence of one of the other medical problems of diving (MPD). The value of using this classification system is that it is very clinically oriented. By ascertaining in which phase of the dive the problem was first noted, the physician immediately is able to narrow the diagnostic considerations.
 |
The primary care physician (PCP) need not feel unprepared when a sports diver reports for management of a diving-related medical problem. There are several reasons for the validity of this statement. First, the causes of the majority of diving-related medical problems are usually obvious be it a puncture wound from a sea urchin spine, an ear squeeze associated with descent, or concern about confusion observed while diving too deeply. Second, the majority of MPD that occur in the sports diver are treated no differently than their terrestrial counterparts. Exposure problems associated with sports diving are a frequent occurrence attesting to this statement. Third, if the physician needs assistance with managing a MPD, 24-hour, 7-day a week help is no further than a phone call away (DAN = Divers Alert Network: (919) 684 4326/2948 or www.diversalertnetwork.org). Finally, the PCP has the exceptional opportunity to counsel and educate the patient diver on how to avoid future occurrences of the problem—the essence of preventive medicine.
Surface Problems. Four problems are primarily associated with the surface phase of the dive. The surface phase includes the time the diver leaves the shore or diving platform, enters the water, and swims to the location where he or she starts the descent. At the end of the dive, these events occur in the reverse order but are also considered part of the surface phase. Snorkeling and breath-hold depth excursions are types of diving where, for all practical purposes, the entire dive is conducted on the surface. The surface problems, however, can occur at other phases of the dive. The 4 problems associated with the surface phase of the dive are: 1) panic; 2) blackout; 3) exposure problems; and 4) injuries from marine animals. Each will be discussed from diagnostic, treatment, and prevention perspectives.
Panic
Significance. In our opinion, panic is one of the most important MPD. This is because it occurs frequently and may be the cause of more SCUBA diving deaths than any other problem (see Figure 2). Analyses of SCUBA diving deaths list drowning as the most frequent cause, but panic is implicated as the cause in about half the drowning deaths.1
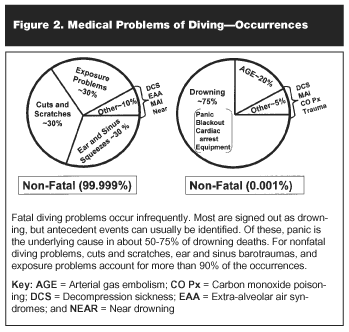 |
Etiology and Pathophysiology. Panic is associated with the diver losing control.2 Causes may be obvious like becoming entangled in kelp, being swept away by a current, or having one’s diving mask torn away by a crashing wave. Unrecognized causes are associated with anxiety and fear, such as sinking in the water because of too much weight, becoming disoriented due to turbidity in the water, poor physical condition, lack of confidence, incompetence, etc. Once the diver panics, the ability to make rational decisions is lost. Physiological responses include hyperventilation and tachypnea. This is due to struggling, which is the diver’s irrational and uncontrollable attempts to cope with the situation. Struggling very rapidly leads to exhaustion. This causes more panic, leading to a panic-exhaustion self-perpetuating cycle, ie, a "vicious circle." There are 3 possible outcomes: 1) Interruption of the panic-exhaustion cycle; 2) Near drowning/drowning secondary to loss of consciousness in the water; or 3) Cardiac dysfunction initiated by extreme exertion.
Primary Responses. The primary response for managing panic is interruption of the "vicious circle." Such simple responses as improving buoyancy by dropping a weight belt or unsheathing a diving knife and cutting free of an entanglement may be all that is needed. The victim’s diving buddy may be able to correct the problem before anything serious happens, and the divers nonchalantly go on to complete their living activities. When consciousness is lost, rescue, resuscitation, evacuation, and advance life support measures are required.
Definitive Treatment. Definitive treatment, if required, is medical management of near drowning, cardiac injury, or combinations of these. If the diver breathed compressed gas with a significant underwater exposure, recompression in a hyperbaric chamber may also be required.
Return to Diving. There are no guidelines, other than common sense about returning to diving after a panic episode. Panic-associated traits such as high anxiety states, low self esteem, inability to communicate well, insecurity, independence (or ego problems) to the point of being unwilling to accept help may be recognized and modified with therapy. Future diving experiences in very controlled settings such as clear, warm, calm waters, shallow depths, and with competent buddies who understand the diver’s problems should be recommended. If cardiac injury or residual neurological impairment (secondary to hypoxic brain injury) are present, return to diving is not recommended. Often, divers who have experienced a critical panic episode while diving decide to stop diving on their own accord even if there are no residuals of the problem. If not, and the PCP has treated the patient for complications of near drowning, then counseling about improving water safety skills and diving under strictly supervised conditions are appropriate recommendations for the patient. Good diving training programs contribute to divers’ confidence and avoidance of panic. Experienced divers rarely, if ever, get themselves into panic provoking situations.
Diver Blackout
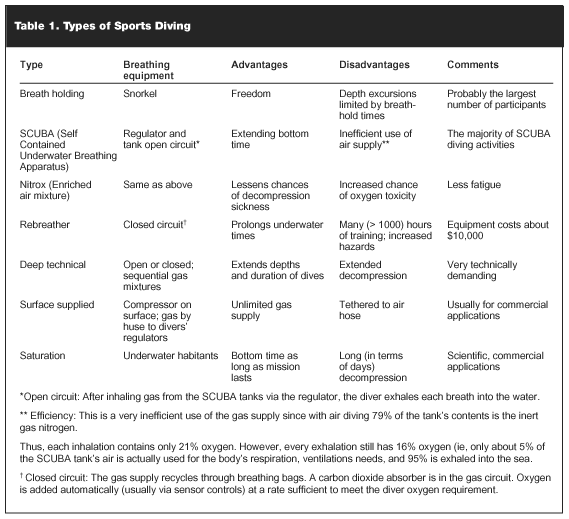
Significance. Whereas panic is, in our opinion, the most significant problem of the SCUBA diver, blackout is the most significant problem of the breath-hold diver. However, blackout can occur using rebreathing equipment or during SCUBA diving (see Table 1). Blackout, in contrast to panic, is characterized by the diver’s loss of consciousness without air hunger, anxiety, or struggling; that is to say "no panic" (see Table 2).3
 |
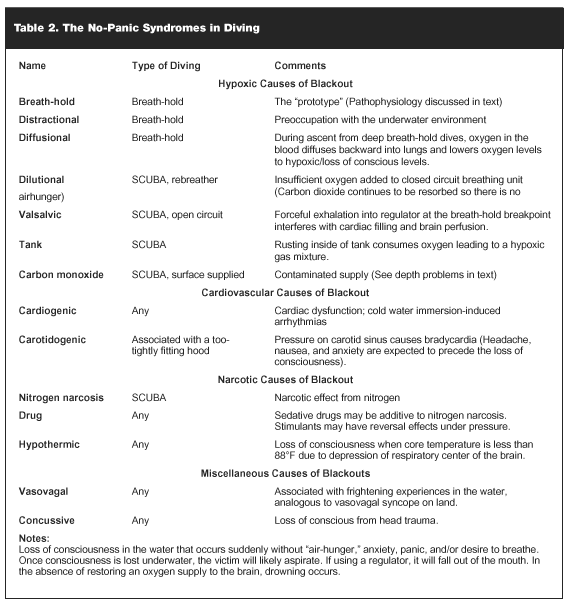 |
Etiology and Pathophysiology. The unified pathophysiology of blackout in divers is loss of consciousness from hypoxia before the body’s physiological control mechanisms signal to the diver that he or she must restore the brain’s oxygen supply. In the prototype blackout disorder, commonly referred to as shallow water blackout, the diver hyperventilates in an attempt to improve his or her breath-hold time. This effectively lowers blood carbon dioxide levels but does not increase the body’s oxygen stores to any significant degree. The consequence is that while the diver is breath-holding, the body’s oxygen stores are lowered to a point where consciousness is lost before the carbon dioxide levels increase to a level where there is an irrepressible desire to breathe.
Primary Responses, Definitive Treatment, Prevention, and Return to Diving. The information presented for the headers in the panic section are also valid for diver blackout. In no situation in water safety can the PCP be more helpful in preventing deaths in breath-hold diving and underwater swimming than explaining the dangers of hyperventilation (and perhaps the simplified physiology presented above) to their patients who are known to participate in these activities and/or have had a near-drowning event from them.
Exposure Problems
Significance. Problems from exposure to and around the underwater environment, while seeming to be minor in significance, probably account for more interruption of diving activities than any other problems. Exposure problems include hypothermia, hyperthermia, sunburn, and infections of the external ear canals (ie, swimmer’s ear). They are ever present hazards for the diver, but ones that can effectively be prevented.
Etiology and Pathophysiology. Hypothermia has been discussed in the environmental stresses section. Hyperthermia can occur in tropical waters when high work loads (such as in underwater archeological digs or military reconnaissance) are performed while in the water. In the water environment, evaporative heat losses no longer occur. The result is that with increased metabolic activity, heat dissipation by sweating is thwarted and the diver’s core temperature rises. Nausea, headaches, heat seizures, and cardiac arrhythmias are consequences. The acute effects of sunburn may not be appreciated until after the exposure has occurred and, once present, can greatly hamper the diver’s underwater activities for the remainder of the diving trip. For the SCUBA diver, sunburns arise during the surface intervals between dives when the diver is resting and "taking advantage" of the amenities of diving in a sunny environment. For the snorkel diver, sunburn develops while on the surface even though the diver mistakenly thinks he or she is protected by being in the water. Chronic effects from sunburn are caused by the effects of ultraviolet light on the DNA in the chromosomes of skin cells and the lenses of the eye. Skin cancers and cataract formation have a high association with sunlight exposure. Swimmer’s ear develops because of the increased moisture load to the external ear canals caused by immersion in water.4 The omnipresent bacteria in the ear canals then have the opportunity to multiply in a moist environment. This leads to their invasion of the linings of the ear canal with symptoms of itching, pain, and drainage of pus from the canals.
First Responses and Definitive Treatments. For the exposure problems, the first responses are usually the definitive treatments and are what is to be expected from an understanding of their pathophysiology. The hypothermic diver needs to have his or her wet suit removed to prevent additional cooling from evaporative heat losses and then be re-warmed. Usually dry blankets, placement in a sleeping bag, etc, are effective. Rewarming by total body immersion in water at 104°F is very effective. However, with obliteration of the shunting reflex, which preserves core temperature by preventing cold blood from the extremities and skin from entering the central circulation, there may be an initial drop in core temperature. This is termed temperature "afterdrop" and may lower core temperature enough to precipitate additional hypothermia symptoms. Temperature afterdrop may be mitigated by placing tourniquets on the extremities and then releasing one extremity at a time while monitoring the hypothermic victim’s core temperature. The breathing of warm humidified air is another effective method of rewarming the hypothermic victim since the surface area of the lungs is about the area of a tennis court thereby providing an enormous area for heat exchange. Infusion of warmed intravenous fluids is a third method of rewarming. Cooling for the hyperthermic diver requires cessation of the activity and institution of cooling measures similar to what would be done if the problem had occurred on land. Anesthetic, anti-inflammatory ointments are appropriate for managing sunburn. Ear canal infections are managed with desiccating agents, such as alcohol mixed with acetic acid or boric acid solutions. The solutions may also contain anti-inflammatory agents. If suppurative, antibiotic ointments and perhaps systemic antibiotics are necessary.
Prevention. Prevention is the key for dealing with these problems. Every predive briefing should include information about water temperature and instructions to end the dive if hypothermia or hyperthermia symptoms appear. PCPs need to inform their patients about the hazards of sun exposure and what preventive measures are necessary for the skin and eyes, especially if they learn that their patients are swimmers and divers. Ear canal hygiene use of desiccating agents should be taught to patients who regularly participate in swimming and diving activities.
Return to Diving. No standards exist as when to return to diving after these exposure problems occur. They are usually self-limiting, and the diver returns to the water when he or she feels comfortable to do so.
Injuries from Marine Animals
Significance. The observation of marine animals in their natural environments is one of the major reasons for sports diving. Fortunately, the serious type injuries such as shark bites and sea snake envenomations are almost nonexistent in the sports diver. Conversely, the minor problems like cuts and scratches from corals, barnacles, etc, are usually so mild that the divers manage these problems themselves. Although thousands of species of marine animals can inflict injury on the human, there are only 5 mechanisms of injury (see Table 3).5 With few exceptions, once the mechanism of injury is recognized, the emergency and definitive treatment becomes obvious.
 |
Prevention and Return to Diving. These injuries are largely preventable. Biting type injuries are only expected to occur when the diver threatens these animals’ habitats/ecosystems. Stings, lacerations, and puncture wounds are avoided by wearing protective equipment like diving suits, gloves, and booties. Most of the injuries are self-induced analogous to sustaining a puncture wound from a nail. They arise, for example, when entering the water and stepping on a stingray or falling into a bed of sea urchins. Carelessness and not wearing proper protective equipment are significant contributing factors. The slogan "Don’t Tread on Me" is very applicable for avoiding injuries from marine animals.
Since most of these injuries are minor, the diver usually resumes diving when he or she feels comfortable. Occasionally "minor" problems from marine animals persist. The PCP should be aware that calcareous debris from the shells of marine animals embedded in lacerations and infections from Mycobacterium marinum can be causes of nonhealing wounds. If sea urchin spines become embedded in joints, they cause a chronic, reactive synovitis that requires surgical excision to correct.
Descent Problem, The Squeezes
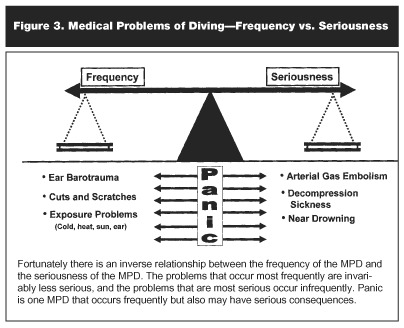
Introduction and Significance. Barotrauma to the otolaryngological structures of the body are among the most common of the nonfatal MPD (see Figure 3).6 Occasionally barotrauma occurs from the use of face masks, ear plugs, or exposure suits, which can produce "artificial" air-filled cavities. We label these "minor" squeezes. With minor squeezes, the sports diver usually continues diving activities as long as he or she is able to equilibrate pressures in these structures with descent. An extremely rare condition, thoracic squeeze, a "major" life-threatening squeeze is associated with breath-hold diving but will not be discussed further in this paper.7
 |
Etiology and Pathophysiology. The pathophysiology of ear, etc, squeezes was introduced in the pressure/hydrostatic effects section of Part I. Pressure differentials as minor as a couple of feet of seawater are sufficient to cause barotrauma. Symptoms include feelings of pain, "fullness" in the middle ear, and muted hearing. Blood tinged sputum or nasal secretions and/or bleeding from the ear canal suggest further injury. Symptoms correlate well with signs found on the otological exam and in the order of increasing severity include injection of blood vessels, transudates (Barotitis media) with loss of the tympanic membrane light reflex, hemotypmpanicum and perforation of the eardrum. Overly aggressive attempts at equilibrating pressures in the middle ear can lead to round and/or oval window rupture with associated disequilibrium, panic, and drowning. During ascent, reverse squeezes can occur if gas at increased pressure is retained in the cavities. Usually this does not occur because depressurization of the cavity is usually a passive process with ascent in contrast to the active process of pressurization of the cavity during descent. A rare condition, alternobaric vertigo, has been described during ascent and is attributed to asymmetrical depressurization of the middle ear spaces during ascent. Vertigo, nausea, vomiting, and loss of equilibrium sense may occur. With loss of visual clues, eg, in turbid waters, disorientation and panic may lead to a breath-holding ascent and precipitate an arterial gas embolism or further descent to the point nitrogen narcosis and the complications relating to it occur.
First Responses and Definitive Treatments. The first response for symptoms of minor squeezes is to stop the descent, ascend a few feet, and try to equilibrate pressures in the middle ear spaces or other sites of involvement such as the facemask. If successful, descent is resumed, perhaps at a slower rate. There are numerous techniques to equilibrate pressures in the middle ear. Valsalva-like techniques are frequently used, as well as swallowing and jutting the jaw forward. Yawning is also a very effective technique but, of course, is not feasible while underwater. All these techniques use the principles of forcing air into the middle ear spaces and sinus cavities and opening the ostia of the Eustachian tubes. For facemask squeezes, exhaling via the nose into the mask equilibrates the pressure. Unfortunately, over-pressurization can occur especially from valsalva maneuvers and in the inexperienced diver, their feelings of discomfort from this may lead them to try even more forcefully to pressurize the cavities and cause further injury. Vasoconstictors, via oral or nasal installation, are effective in reducing swollen mucus membranes. Antihistamines, in those divers with allergy histories, will decrease the production of secretions but may have side effects such as sedation and drowsiness, which can contribute to other problems such as nitrogen narcosis and inappropriate responses to potentially panic-provoking situations.
Prevention and Return to Diving. The minor squeezes exemplify the principles of preventive medicine. In patients who present with residual symptoms of minor squeezes, the PCP should inform them of the information in the above headers and prescribe vasoconstrictors and perhaps antihistamines to help resolve the symptoms. If inner ear symptoms are noted such as disequilibrium, profound hearing loss, nausea, etc, concern needs to be raised about a rupture of the round window from barotrauma, and referral for otolaryngological evaluation is indicated. Nearly, all tympanic membrane ruptures from diving heal spontaneously over a 3- to 4-week period. In the interim, diving must cease due to concern about infection developing from bacteria entering the middle ear spaces.
Bottom Problems
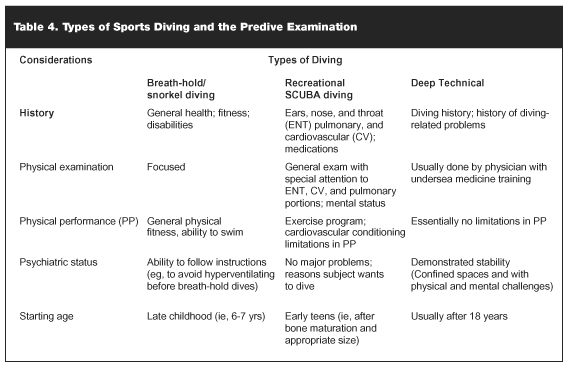
Problems arising during the bottom phase of the dive, with the exception of nitrogen narcosis, occur rarely in the sports diver. This is because most of the conditions are associated with use of special equipment, require extensive training, and require a checklist of safety measures including backup medical support in order to use. Consequently, the PCP is not likely to become involved in the care of divers with problems from this phase of the dive. For this reason we have only summarized the information for these conditions in table form (see Table 4).
 |
Ascent Problems
Introduction
Arterial gas embolism (AGE) and decompression sickness (DCS) are associated with the ascent phase of the dive. They are potentially serious problems that usually require hyperbaric oxygen recompression therapy for their management. Each has a spectrum of presentations from mild to life threatening. Serious cases will likely be referred directly to facilities where recompression chambers are available. For mild cases, the divers may seek consultation from their PCPs in order to discover the cause of their lingering symptoms. Because the most serious presentations of these disorders can be so similar, it is sometimes difficult to differentiate the two, and for this reason the all-encompassing term decompression illness may be used. For the purist, this might be unacceptable. In reality, the treatment is the same for both when the presentations are in their severest forms. Whereas, the question of returning to diving for the conditions we discussed previously was easy to answer—for AGE and DCS the decision has many contingencies.
Arterial Gas Embolism
Significance. Arterial gas embolism accounts for about 20% of the approximately 100 SCUBA diving-related deaths that occur yearly in the United States.1 Although AGE occurs infrequently, it is considered by many to be the most serious SCUBA diving problem since recovery is so dependent on immediate hyperbaric oxygen recompression treatment. AGE can occur with a single ascent from depths less than 10 ft after breathing a compressed gas. This type of history helps to differentiate AGE from DCS. Arterial gas embolism is but 1 component of a triad of disorders that is associated with overexpansion of gas in the lungs during ascent.
Etiology and Pathophysiology. AGE occurs when gas in the lungs overexpands while rapidly ascending. Usually it is associated with breath holding, but conditions that retain air in the lungs such as asthma, emphysema, emphsematous bleps, pleural adhesions, and bronchiolitis may be other causes. The retained gas in the lungs expands as predicted by Boyle’s law. The elasticity of the alveoli tends to restrain the expansion which, in turn, increases the pressure of the retained gas. When the pressure exceeds the elastic limit of the alveoli, "explosive" rupture of the alveoli and their adjacent capillaries occur. This provides an avenue for gas to enter the pulmonary circulation, be carried to the heart, and then become arterial gas emboli.8 With embolic occlusion of the brain’s circulation, AGE can present with any of the symptoms of a cerebral vascular accident. Embolization of the coronary arteries may lead to myocardial ischemia and infarction. Immediate bubble reduction is essential to restore circulation to the embolized areas and prevent permanent brain and/or heart damage. Animal models demonstrate that bubbles disappear from the arterial circulation within minutes of their entry. Residual symptoms are ascribing to the effects of the bubble-endothelium interaction.
When gas expansion is not as explosive as in AGE, it may diffuse out of the alveoli and dissect along tissue planes to the mediastinum or neck to cause emphysema in these areas. Another route the gas may take is to collapse the lung and cause a pneumothorax. For these reasons, subcutaneous/mediastinal emphysema, pneumothrorax, and AGE are linked together as a continuum of responses to overexpansion of gas in the lungs and collectively termed the extra-alveolar air, pulmonary overinflation, and/or over pressurization syndromes.
Primary Responses. The primary response for AGE is the immediate breathing of 100% oxygen on the surface. This is so effective that 50% of the victims presenting with AGE have complete remission of their symptoms.9 Although positioning the patient in the head down position would seem to reduce the bubble load to the brain due to the decreased density of the bubble compared to blood, in reality this effect probably does not occur, and the head down position may worsen cerebral edema associated with brain ischemia. More important is the positioning of the victim so the head can be turned to the side to prevent aspiration. Hence, if the victim is unconscious, positioning in the flat supine position is recommended. If the victim is alert, oral fluid administration is recommended to expand blood volume and increase perfusion to provide oxygen to the brain. Overzealous hydration can worsen cerebral edema.
Definitive Treatments. Hyperbaric oxygen recompression is the definitive treatment for AGE. For the previously discussed reason, maximizing the oxygen partial pressure seems equally important to reduction of bubble size by pressurization. Consequently, most physicians who treat AGE no longer pressurize the patient to 165 ft, but rather to 60-66 ft with pure oxygen. At these depths, risks from hyperbaric oxygen-induced oxygen seizures is minimal. If the victim becomes asymptomatic with breathing 100% oxygen, one "washout" hyperbaric oxygen treatment is recommended. If signs and symptoms of brain injury continue at the time of presentation to the recompression chamber, ancillary interventions including steroids, intravenous lidocaine at cardiac doses, intravenous fluids, and management of intercurrent problems such as seizures, pneumothorax, and hypoxemia/apnea are required. The use of steroids is controversial. They may aggravate the neural ischemic injury.8
If the presenting symptom is limited to pneumothorax, lung re-expansion is done with a chest tube. Hyperbaric oxygen is not required unless there are concomitant symptoms of DCS or omitted decompression (ie, the victim missed decompression stops during ascent). Subcutaneous/mediastinal emphysema, as long as respiratory distress is not present, is self-limiting, and appropriately managed by observation. The emphysematous gas gradually reabsorbs spontaneously usually within a week.
Prevention. Arterial gas embolism and the related extra-alveolar air syndromes are prevented by ascending slowly while breathing in a normal fashion. Training and experience seem to be the best prophylaxis for these problems, in as much as AGE is almost never observed in the experienced and/or commercial diver. The PCP can have a very important role in preventing extra-alveolar air syndromes, since recognition of conditions that retain air in the lungs would be reasons to disqualify individuals from diving (see Part III on Diver Evaluation, coming soon).
Return to Diving. No published criteria exist for returning to diving after AGE. If recovery is complete and the cause identifiable (ie, the diver panicked and breath-held during ascent), with proper counseling and retraining, the motivated diver may return to diving after a month or two. If there is residual neurological impairment, further SCUBA diving is not recommended. If a pneumothorax occurs spontaneously, US Navy diving regulations prohibit diving for 5 years. If traumatic, the patient may return to diving after complete lung and chest wall healing perhaps in 6 months. After an episode of subcutaneous/mediastinal emphysema, the patient may return to diving 1-2 weeks after symptoms resolve. However, causes of extra-alveolar air should be sought and a workup including plain x-rays, tomograms, and spirometry be done before clearing the patient to dive.
Decompression Sickness
Significance. When dealing with superlatives about MPD, decompression sickness (DCS) has the reputation for being the most "notorious." There is hardly anyone who has not heard of the bends. Whenever a diver has a problem the first question asked is, "Did he get bent?" This is in spite of the observation that DCS occurs only 2 or 3 times in every 10,000 SCUBA dives.10 Decompression sickness is rightfully labeled a syndrome because of its many presentations, and its signs and symptoms are not always clearly related to the causes. Presentations of DCS include death, shock, chokes, altered mental status, paraplegia, paralysis/paresis, joint pains, paresthesias/neuropathies, pruritis, flu-like syndromes, fatigue, and skin rashes. The earlier the symptoms appear, the more serious the DCS event is likely to be. Symptoms that appear during ascent from the dive must always be considered serious in the sports diver. Within 12 hours of completing the dive, about 90% of divers who develop DCS have manifested their symptoms. However, symptoms that first appear 3 or more days after diving should not be dismissed as being incompatible with DCS. Excellent responses to hyperbaric oxygen recompression treatments have been observed in such situations.
About half the cases of DCS occur in divers who do not violate their dive computers and/or the diving tables. When there are obvious violations of diving computer/tables and DCS occurs, we term this "deserved" DCS. When there were no apparent violations we term this "undeserved" DCS. In these situations, bends prone factors (eg, a patent foramen ovale) or disordering events (eg, the tourniquet effect of a too-tightly fitted dive strap during decompression from the dive) should be sought. Identification of this information is necessary before making a decision to allow the diver to return to diving after being treated for DCS. In terms of primary responses, definitive treatments, prevention, and return to diving, DCS is very similar to AGE.11
Etiology and Pathophysiology. Once bubbles form within blood vessels, they initiate an inflammatory reaction very similar to the reperfusion injury. Consequently, even if the bubbles are dissipated by pressure, the hypoxic injury to tissues continues with persistence of symptoms. For joints the mechanisms are different. It appears that bubbles form in pressure sensitive organelles of joint capsules (Ruffini 2 Corpuscles) and physically distend the capsule—causing pain much like a stretch injury from a dislocated joint would. Pressure alone appears to resolve the symptoms of this type of DCS presentation. Delayed onset of DCS may occur after ascending in altitude such as flying in an airplane or interfering with off gassing such as falling asleep with a limb in the cramped position. The venous circulation of the spinal cord especially at the lower thoracic level appears particularly susceptible to bubble formation, coalescence, and then enlargement during ascent because of the sluggish flow of blood in the Batson plexus of veins.12 This anatomical consideration correlates closely with the high incidence of paraplegia when neurological symptoms of DCS occur. Finally, divers with patent foramen ovale in their hearts appear to have increased susceptibility to DCS. The explanation for this is that venous gas emboli, a ubiquitous finding during decompression, can pass through the right to left shunt in the heart, bypass being filtered and exhaled via the lungs, and enter the arterial circulation to cause neurological symptoms of DCS.13
Primary Responses. The primary treatment response for DCS is oxygen breathing. Supplemental interventions include improving hydration (diving leads to dehydration) and, possibly, ingestion of aspirin to prevent hemostasis and sludging (Personal Communication; George Hart, Long Beach, Calif, 2002). The diver-fisherman of Hawaii, notorious for omitting decompression according to US Navy diving tables and avoiding DCS, use aspirin as part of their dive routine (Personal communication; Frank Farm, Honolulu, Hawaii, 1986). Rest is important since activity will likely worsen the symptoms. In remote areas, return to the water and breathing air to the depth of relief or pure oxygen at a 33 depth for a few minutes then gradually ascending has been recommended but is considered controversial by many authorities in diving medicine.14
Definitive Treatments. Hyperbaric oxygen recompression is the definitive treatment for DCS. When all symptoms do not clear with the first treatment, repetitive treatments are recommended as is frequently the situation when severe neurological deficits exist. The earlier the treatment, the more likely the complete resolution of symptoms with the initial treatment.15 Supplementary interventions as discussed for AGE should also be used. The use of a nonsteroidal anti-inflammatory drug with hyperbaric oxygen recompression for pain-only DCS was noted to reduce the number of repetitive treatments to control symptoms (Personal communication; Michael Bennett, 2002 Undersea and Hyperbaric Medicine Meeting).
Prevention. Usually DCS can be prevented by safe diving practices such as not violating diving tables or dive computer limits; maintaining good hydration, fitness, and body weight; and avoiding diving if bends proneness factors exist. Some obvious bends proneness factors are patent foramen ovales, disturbed circulation around joints following severe injuries, coagulopathies, polycythemia, and atherosclerotic cardiovascular disease. Age itself is not a contraindication to diving but may become an increasing risk factor due to decreased exercise capacity, and cardiovascular reserve. With this information, the PCP can make meaningful recommendations regarding the appropriateness of SCUBA diving for his/her patients.
Return to Diving. As in AGE, the criteria for returning to diving are quite subjective. If the diver had minor symptoms such as pain-only, violated diving practices, and had full resolution of symptoms with recompression, then we OK resumption of diving after a couple of weeks. Counseling about safe diving practices is also given. If the DCS was undeserved (ie, no diving practices were violated), the patient should be evaluated for bends proneness factors. If no risk factors are identified, even if all symptoms cleared with treatments, consultation with a physician experienced in undersea medicine is recommended before either clearing or not recommending the patient return to SCUBA diving. Finally, if significant residual neurological deficits exist after treatments, return to SCUBA diving is contraindicated.
Primary Complications from Medical Problems of Diving
Three serious problems can arise independently or can be direct complications of the MPD we just discussed. They include: 1) near drowning/drowning; 2) shock; and 3) cardiac arrest. Whereas, the inciting problem may have been self-limiting, the consequences of the complication may cause death or permanent residual injury. Often the complication is obvious such as near drowning, but the underlying problem not apparent, as is often observed with panic, nitrogen narcosis, and the other "no-panic" syndromes.
Near Drowning/Drowning
Anytime consciousness is lost in the water the victim is at risk of drowning. Aspiration is often associated with drowning since the breathing reflexes are usually the last to remain after a hypoxic injury to the brain. If the victim is rescued and resuscitated, then the incident is labeled a near drowning. Whereas aspiration and the resulting lung injury can be managed effectively with appropriate interventions, the consequences of hypoxic brain injury are usually irreversible and can range from imperceptible to persistent vegetative coma.
The brain is the most critical organ in the body with respect to injury from oxygen deprivation. After 4 minutes of anoxia, brain injury is likely to occur. Although breath-holding for several minutes is possible, the interruption of the brain’s perfusion for more than a moment of so, for example in a third-degree heart block, leads to immediate loss of consciousness. Conversely, loss of consciousness associated with water immersion has "protective effects’ in terms of preservation of brain function. This is ascribed to the oxygen conserving effects of the diving reflex and hypothermia from immersion in cold water. Remarkable recoveries have been reported from near drowning even after the victim has been immersed for 30 minute or longer durations.14
Consequently, the adage, "Never say drowned" is very appropriate for 2 reasons: First, for the remarkable recoveries that have been observed and second, the primary cause should be identified. Once the primary cause is identified, appropriate management becomes logical. For example, if the diver loses consciousness while at the bottom phase of the dive then hyperbaric oxygen recompression therapy is essential to off load the inert gas present in the tissues and prevent complications of decompression illness (ie, DCS and/or AGE). In addition concurrent optimal management of the pulmonary and brain injuries from near drowning must be given.
Shock
Medical problems of diving can lead to a variety of presentations of shock. Hypovolemic shock may result from massive bite injuries. Envenomations from marine animal toxins and anoxic injuries may cause cardiogenic shock. Massive intravascular bubbling from explosive decompression and/or arterial gas embolism are other diving-related causes of shock. Management, as in near drowning, is 2-fold; correct the cardiovascular causes of shock and treat the pathophysiology of the MPD that lead to shock.
Cardiac Arrest
As a cause of exertion stresses, sports diving is paradoxical. If the dive is performed according to good diving practices, exertion stresses may be minimal. This is the reason for the statement that SCUBA diving is a not a good activity for aerobic conditioning. In contrast, if the diver gets into a predicament such as becoming entangled in kelp, struggling will likely lead to maximal exertion efforts and the rapid onset of exhaustion. The consequence of this 100% effort may lead to a cardiac arrest especially in the poorly conditioned diver. Diving stresses may cause cardiac arrest from arrhythmias associated with diving in cold water or myocardial infarction secondary to ischemia. Usually the most stressful portion of the dive is during the surface phase, which requires carrying of gear to the dive site, donning the gear, entering the water (and experiencing its chilling effects while warming the entrapped water in the wet suit), negotiating the surf, and actively swimming to the dive site. If an exertion-related diving problem, eg, cardiac arrest, is to occur, it will probably be during this phase of the dive. The information as to when the cardiac event occurred in the dive profile is essential in establishing the underlying cause and whether or not HBO recompression therapy is required in addition to managing the cardiac injury. The question of diving with a history of cardiac problems will be discussed in the next section.
References
1. Report on Decompression Illness and Diving Fatalities. Dovenbarger J, Ugiccioni D, eds. Durham, NC: Divers Alert Network; 1999.
2. Strauss MB, The panic syndrome. The Physician and Sport Medicine. 1973;1:39-42.
3. Strauss MB, Shane SL, The no-panic syndromes in underwater diving. The Physician and Sport Medicine. 1982;10(8):89-99.
4. Dierker RC, Strauss MB, Treating swimmer’s ear. US Pharmacist. 1990;15(5):72-74.
5. Strauss MB, Orris WL. Injuries to divers by marine animals: A simplified approach to recognition and management. Mil Med. 1974;139(2):129-130.
6. Strauss MB, Cantrell RW. Ear and sinus barotraumas in diving. The Physician and Sport Medicine. 1974;2:39-43.
7. Strauss MB, Wright PW. Thoracic squeeze diving casualty. Aerosp Med. 1971;42(6):673-675.
8. Muth CM, Shank ES. Gas Embolism. N Engl J Med. 2000; 342(7):476-482.
9. Dick APK, Massy EW. Neurologic presentation of decompression sickness and air embolism in sport divers. Neurology. 1985;35:667-671.
10. Bove AA. Risk of decompression sickness with patent foramen ovale. Undersea Hyperb Med. 1998;25(3):175-178.
11. Moon RE, Sheffield PJ. Guidelines for treatment of decompression illness. Aviat Space Environ Med. 1997;68(3):234-243.
12. Hollenbeck JM, Bove AA, Elliott. Mechanism underlying spinal cord damage in decompression sickness. Neurology. 1975;25: 308-316.
13. Moon RE, Camporesi EM, Kisslo JA. Patent foramen ovale and decompression sickness in divers. Lancet. 1989;1:513-514.
14. Diving and Subaquatic Medicine. Edmonds C, et al, eds. Flagstaff, Ariz: Best Publishing; 2002.
15. Bayne CG. Acute decompression sickness. 50 cases. J Am College Emerg Phys. 1978;7:351-354.
Readers are Invited. . .
Readers are invited to submit questions or comments on material seen in or relevant to Primary Care Reports. Send your questions to: Robin Mason, Primary Care Reports, c/o American Health Consultants, P.O. Box 740059, Atlanta, GA 30374. For subscription information, you can reach the editors and customer service personnel for Primary Care Reports via the internet by sending e-mail to [email protected].
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
