Special Feature: The Electrocardiogram in Wellens’ Syndrome
The Electrocardiogram in Wellens’ Syndrome
By William J. Brady, MD
Among the many electrocardiographic findings indicative of acute coronary syndromes, the emergency physician (EP) must be familiar with the characteristics of the pre-infarction stage of coronary artery disease known as Wellens’ syndrome. Wellens et al first described a subgroup of patients hospitalized for unstable angina who were at high risk for the development of an anterior wall myocardial infarction (MI).1 This subgroup could be recognized by characteristic changes on the electrocardiogram (ECG) involving the ST segments and T waves in the precordial leads. Two basic patterns of electrocardiographic change are encountered; one features ST segment and T wave changes to be described below, whereas the latter manifests biphasic T waves in the right-to-mid precordial leads.2,3
 |
Historical and Clinical Highlights
In Wellens’ first study, 26 of 145 (18%) patients admitted for unstable angina had this electrocardiographic pattern.1 In a second prospective study, 180 out of 1260 hospitalized patients (14%) demonstrated the characteristic electrocardiographic changes.2 Further-more, all of these patients had significant disease of the proximal left anterior descending artery (LAD). In the first study, 12 of 16 patients (75%) with electrocardiographic changes who did not receive coronary revascularization developed an extensive anterior wall infarction within a few weeks of admission.1 In the second study, urgent coronary angiography was implemented, and all of the 180 patients with electrocardiographic changes were found to have stenosis of the LAD, varying from 50% to complete obstruction.2
Early detection of these electrocardiographic changes also is important because of the clinical presentation of a patient with Wellens’ syndrome. The characteristic electrocardiographic pattern often develops when the patient is not experiencing angina. In fact, during an attack of chest pain the ST segment/T wave abnormalities usually normalize or develop into ST segment elevation.2 Cardiac serum markers often are normal or minimally elevated. In Wellens’ prospective study, only 21 of 180 patients (12%) with electrocardiographic changes had elevated cardiac enzymes. These elevations were always less than twice the upper limit of normal.2 Therefore, the ECG may be the only indication of an impending extensive anterior wall MI in an otherwise asymptomatic patient.
Electrocardiographic Features
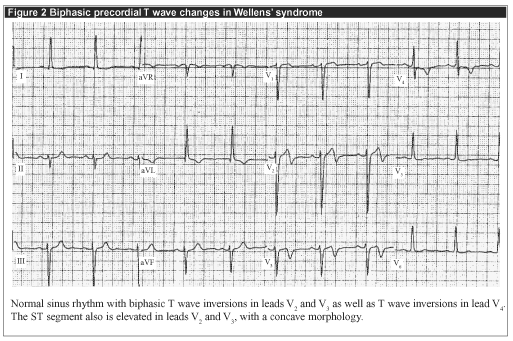
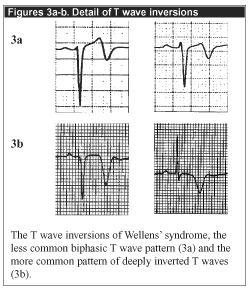
The electrocardiographic findings include significant involvement of the T wave with occasional alterations of the ST segment. The ST segment itself is often normal (i.e., isoelectric); if abnormal, it is minimally elevated, usually less than 1 mm, with a high take-off of the ST segment from the QRS complex. If the ST segment is elevated, it is either convex in contour or obliquely straight in appearance; concave morphologies also are seen.1 T wave findings, the key features of this electrocardiographic syndrome, may take the form of one of two patterns of T wave changes. In the more common pattern, which comprises approximately 75% of cases, the T wave is deeply inverted. (See Figures 1 and 3b.) As the ST segment terminates, the T wave assumes a very negative angle relative to the isoelectric baseline; this angle may approach 90 degrees. The inverted T wave is symmetric in contour. The less common variant, comprising 25% of Wellens’ syndrome cases, presents with biphasic T waves. (See Figures 2 and 3a.)1,2
 |
 |
 |
The ST segment and T wave changes are classically present in V2 and V3; in certain cases, the changes may also involve leads V1 and V4. In Wellens’ prospective study, approximately two-thirds of patients also had these changes in lead V1 and three-quarters in lead V4. Patients with abnormalities in lead V4 occasionally will demonstrate similar abnormalities in leads V5 or V6 (as in Figure 1).2 In Wellens’ study, 60% of patients diagnosed with Wellens’ syndrome had the characteristic electrocardiographic changes on admission. After admission, 56 (31%) developed the changes within 24 hours, 10 (5%) within two days, five (2.8%) within three days, and one (0.6%) within five days.2
The chest pain patient who presents with a convincing clinical description of an acute coronary syndrome (ACS) and manifests electrocardiographic change involving the T wave in the anterior distribution likely will be managed in appropriate fashion in terms of initial therapy, diagnostic studies, and disposition. This generally should include nitrates, aspirin, beta-adrenergic blockade, and other agents coupled with serial ECGs and serum markers, culminating in an inpatient admission. Morphologically, Wellens’ T waves either are inverted deeply or biphasic—both configurations that are highly characteristic of the syndrome and unlike other T wave inversions related to ACS. The major issue here is recognition of the syndrome and its relation to high-grade, proximal LAD obstruction, with the natural history of extensive anterior wall MI. Importantly, the avoidance of provocative testing, including stress imaging, is key in that such testing may precipitate an MI with significant acute sequelae.4
Dr. Brady, Associate Professor of Emergency Medicine and Internal Medicine, Residency Director and Vice Chair, Emergency Medicine, University of Virginia, Charlottesville, is on the Editorial Board of Emergency Medicine Alert.
References
1. de Zwann C, et al. Characteristic electrocardiographic pattern indicating a critical stenosis high in left anterior descending coronary artery in patients admitted because of impending myocardial infarction. Am Heart J 1982;103:730-736.
2. de Zwann C, et al. Angiographic and clinical characteristics of patients with unstable angina showing an ECG pattern indicating critical narrowing of the proximal LAD coronary artery. Am Heart J 1989;117: 657-665.
3. Tandy TK, et al. Wellens’ syndrome. Ann Emerg Med 1999;33:347-351.
4. Paul S, et al. Early recognition of critical stenosis high in the left anterior descending coronary artery. Heart Lung 1990;19:27.
Among the many electrocardiographic findings indicative of acute coronary syndromes, the emergency physician must be familiar with the characteristics of the pre-infarction stage of coronary artery disease known as Wellens syndrome.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
