Emergency Ultrasound Part I: Pelvic Ultrasound and the First Trimester Patient
Authors: Michael J. Lambert, MD, RDMS, Clinical Assistant Professor, Department of Emergency Medicine, University of Illinois College of Medicine; Fellowship Director, Emergency Ultrasound, Resurrection Medical Center, Chicago, IL; J. Christian Fox, MD, RDMS, Assistant Professor of Medicine; Director, Emergency Ultrasound, University of California-Irvine, Division of Emergency Medicine, Orange, CA.
Peer Reviewers: Anthony Macasaet, MD, Assistant Professor and Vice Chair, Director Emergency Medicine Ultrasound, Department of Emergency Medicine, Chicago Medical School, Chicago, IL; Kenneth H. Butler, DO, Associate Residency Director, University of Maryland Emergency Medicine Residency Program, University of Maryland School of Medicine, Baltimore.
Although the full impact of ultrasound in the emergency department (ED) has not yet been felt, the revolution has been ignited. The use of ultrasound as an integral part of an emergency physician’s practice has been embraced by the specialty. The American Academy of Emergency Medicine, American College of Emergency Physicians, and the Society for Academic Emergency Medicine have issued position statements and established committees supporting the use of ultrasound in the ED.1,2 The Council of Residency Directors firmly recognizes ultrasound as part of the core content of emergency medicine.3 Presently, every emergency medicine residency program in the United States provides some training in emergency ultrasound. Outside emergency medicine’s friendly confines, unequivocal support for the use of this imaging modality comes from the American Medical Association. In January 2000, the AMA passed Resolution 802, which clearly states that diagnostic ultrasound belongs to no single specialty. It stipulates that emergency physicians qualify for ultrasound privileges if they possess appropriate training in image acquisition and interpretation.4 Emergency physicians worldwide diligently are developing the sonographic skills necessary to expedite definitive diagnoses of life-threatening conditions, decrease patient length of stay, and improve patient care. While there have been foreseeable turf battles waged between radiologists and emergency physicians, these barriers are eroding as emergency physicians safely and methodically integrate ultrasound into their practice. Fast, accurate, and safe, no other diagnostic imaging modality is better positioned to serve the needs of a physician trained to recognize and treat life-threatening emergencies.
In this article and the succeeding two parts in this series, three distinctive applications of ultrasound in the ED will be discussed. In an effort to provide comprehensive education to a wide variety of emergency physicians who either may be considering ultrasound in their practice or sharpening their current skills, we will attempt to be as complete as possible. The ability to perform a proficient and diagnostically effective ultrasound examination requires a judicious understanding of the underlying principles. Although a discussion of ultrasound physics is beyond the scope of this article, the novice sonographer would benefit from a review of these principles prior to engaging in this ultrasound series.—The Editor
Introduction
Perhaps no other application of emergency ultrasound has changed the paradigm as significantly as pelvic ultrasound in the evaluation of the symptomatic, first-trimester pregnant patient. Regularly confronted with the pregnant patient with vaginal bleeding and/or abdominal pain, the emergency medicine physician, by default, has become an expert in first-trimester pregnancy complications. While the patient frequently is preoccupied with the well-being of the fetus, the differential diagnosis begins with ectopic, ectopic, and ectopic. There are no historical clues or physical findings that effectively can affirm or refute an ectopic pregnancy in these patients; therefore, ultrasound has become the diagnostic imaging modality emergency physicians rely on to rule out an ectopic pregnancy. Unfortunately, few EDs have on-site sonographers 24 hours a day. This is especially a problem in the unstable patient who must leave the ED to obtain a formal ultrasound examination. The emergency physician can truncate the traditional rate-limiting step of an ultrasound obtained in the radiology suite by performing this bedside skill as an extension of his or her physical examination. The ability to expedite time-to-diagnosis is reason alone to become proficient in ultrasound. There are, however, several other benefits to having the emergency physician perform emergency ultrasounds. (See Table 1.)

Cost Containment. After the emergency physician completes a history and physical examination, only a few of the components of the differential diagnosis may be excluded. Therefore, other diagnostic tests must be considered at this time. When the emergency physician performs an endovaginal ultrasound in tandem with the physical examination, a few of these tests might be inconsequential.
Urinalysis. The possibility exists that the source of the patient’s abdominal pain or vaginal bleeding might be a urinary tract infection. Although the patient may not have any specific genitourinary symptoms, a urinalysis commonly is obtained. A definite diagnosis of an incomplete abortion or an abnormal intrauterine pregnancy, for example, might alleviate this step.
Quantitative Serum BHCG. This serum test commonly is ordered in a knee-jerk effort to expedite patient length of stay while awaiting a formal ultrasound in radiology. Although a single quantitative level rarely helps in the decision-making process, a follow-up level in 48 hours in a patient without evidence of a live intrauterine pregnancy can help guide clinical decisions. However, when the bedside ultrasound reveals a single, live intrauterine pregnancy, there is no need for this blood test.
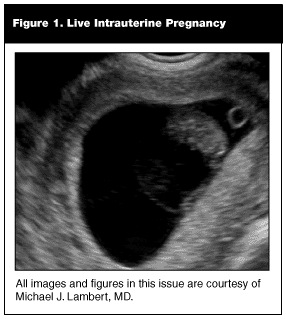
Better Patient Understanding. When the emergency physician performs an emergency ultrasound, he can share the real-time images with the patient on the ultrasound monitor screen. Although this may not be a common practice in the radiology suite where patients are scanned by a diagnostic medical sonographer, pictures are worth a thousand words in some instances. In the case of a live intrauterine pregnancy (See Figure 1), the mother frequently can see the heart beating within the fetal pole or cardiac tube. The mother’s visualization of a beating heart on the monitor relieves a lot of anxiety and promotes mother-baby bonding.6 However, it is important to verbalize and document a statement regarding the health of the baby, such as, "Although it is too early to tell you anything about the health of the baby, I can tell you that the fetus is in the correct location and is alive." Studies have shown that about 80% of pregnancies in which a heartbeat can be visualized within the uterus will deliver a live pregnancy.7,8,9 Likewise, the patients can better understand instructions when they have an understanding of their diagnosis.
Improved Patient Satisfaction. The overwhelming majority of patients undergoing emergency ultrasound of the pelvis will experience improved satisfaction with his or her care.10 Although specific literature is lacking in emergency medicine, there is support from other specialties. Common sense dictates that additional time spent with patients strongly correlates with their satisfaction. A single area of evaluation in the ED providing point-of-care service also is perceived as a higher level of care.
Better Patient Care. In well-trained emergency physician hands, ultrasound will provide better patient care by expediting time-to-diagnosis and, therefore, allowing definitive treatment to be started in a more timely manner.11 Although the literature is sparse, there is evidence that ultrasound at the patient’s bedside decreases morbidity and mortality.12
Pelvic Ultrasound Imaging Techniques
Evaluation of the pelvic organs is achieved using two sonographic methods of interrogation: the transabdominal and the endovaginal techniques. In the transabdominal approach, the probe is positioned over the lower portion of the abdomen and directed into the pelvis. In the endovaginal approach, the probe is inserted into the vaginal vault, where it lies in close proximity to the pelvic organs. These "windows" into the pelvis are illustrated and discussed below.
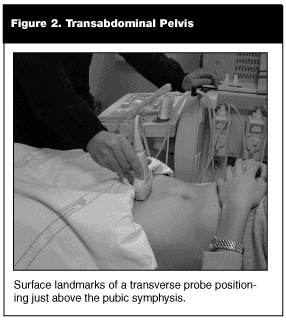
Transabdominal. The transabdominal technique has long been utilized to evaluate the first-trimester pregnant patient. (See Figure 2.) Prior to the ultrasound examination, a Foley catheter commonly is inserted, and the bladder filled. The practice of filling the bladder accomplishes two things. First, the full bladder displaces bowel out of the anterior cul-de-sac and acts as an acoustic window to the pelvic organs. Secondly, a full bladder generally aligns the uterus so that its long axis parallels the abdominal wall. This allows the transmitted sound waves to strike the uterus at a near-perpendicular angle, producing better reflections when the returning echoes are received by the transducer and plotted on the monitor. This optimizes image quality.
Disadvantages:
• Uncomfortable. Filling the bladder with a few hundred milliliters of sterile water and then providing intermittent pressure across the abdominal wall with a transducer is analogous to drinking several 12-ounce beverages and then tightening your belt.
• Image Quality. While filling the bladder provides an acoustic window, remember that the pelvic organs are several centimeters from the abdominal wall. When the bladder is filled, the distance between the transducer probe and the pelvic organs further increases. If you are attempting to visualize objects at a further distance, a lower frequency transducer must be used and, therefore, a lower resolution must be accepted.
Advantages:
• Overall view of the true pelvis. Lower-frequency probes will penetrate deeper into the pelvis. Although the image might be a little fuzzy, a "full" view of the pelvis is provided.
• Fast. In patients who are further along in the first trimester, or whose bladders are not completely empty, adequate transabdominal views can be obtained without filling the bladder. Less preparation time is needed to scan these patients, and enlisting the assistance of a coworker to chaperone is not necessary.
Endovaginal. The arrival of endovaginal transducers in the 1980s significantly improved the quality of ultrasound imaging in the female patient. Simplified, the engineering design placed an ultrasound transducer on the end of a stick, which could be placed into the vaginal vault. This permitted the transducer scan head to be in close proximity to the pelvic organs. This has several important implications in ultrasound imaging. First, there is a clearer path by which to transmit and receive echoes. Second, a shorter distance exists between the transducer and the pelvic organs, allowing higher transducer frequencies to be employed.13 In contrast to the transabdominal approach, the image quality from an endovaginal approach is enhanced with an empty bladder.
Disadvantages:
• Invasive. As the endovaginal probe is inserted into the vaginal vault, there is a small risk of introducing transmitted disease through an improperly sanitized probe.
• More time-consuming. The taboo of having an unknown physician insert a probe into the vaginal vault may require greater explanation of the procedure. The optimal examination utilizes a gynecological table, which may be a limited resource. More time is involved in preparing for the endovaginal study and obtaining a chaperone.
• Less field of view. The higher-frequency probes used in endovaginal scanning limit the range of the transmitted echo. Generally, a full view of the pelvis is not obtainable.
Advantages:
• Superior resolution. A shorter pathway from the transducer to the pelvic structures permits the use of higher frequencies. Sound attenuation is limited, and reflected waves from nearby objects are maximized. These higher-frequency probes with their inherent enhanced resolution provide the emergency physician with more clinical confidence when interpreting images.
• Wider field of view. Most endovaginal transducers incorporate a beam angle, providing a 120-180° field of view.
Interpreting First-Trimester Pregnancy Ultrasounds
Interpretation of first-trimester pelvic ultrasound ranges from the rather basic to the esoteric. On one hand, there is the live intrauterine pregnancy (LIUP) that even patients commonly identify and point out on the monitor. Conversely, a patient with no definitive intrauterine pregnancy (NDIUP) may require considerably more ultrasound expertise to properly evaluate and diagnose. To simplify the interpretation process of the first-trimester pregnancy, the ultrasound diagnoses have been categorized by location and specific diagnostic criteria. Prior to jumping into the categorizations, a brief review of early embryonic development ensues. This is important because some of these embryonic development stages can be visualized with ultrasound, and relied upon for confirmation of pregnancy.
Development of Embryonic and Fetal Structures
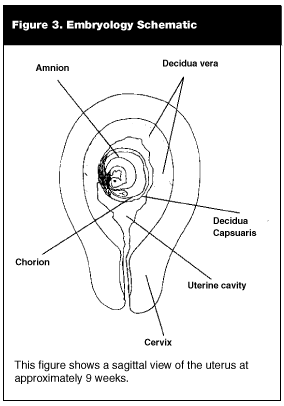
After fertilization within the fallopian tube, the zygote continuously divides into an initial solid ball of cells known as a morula. Through further cell division, the morula develops into an outer group of cells with an attached inner group of cells. This period of embryonic development is called a blastocyst. Approximately seven days following fertilization, the blastocyst burrows beneath the endometrial lining of the uterus (decidua vera). The outer cell layer of the blastocyst (chorionic membranes) nourishes and protects the inner cell layer (embryonic disc), which becomes the fetus. It is this area between the chorion and the embryonic disc (chorionic cavity) that contains the fluid seen sonographically as the "gestational sac." (See Figure 3.) The portion of the decidua vera that eventually surrounds the blastocyst now is termed the decidua capsularis. The decidual linings over the gestational sac (decidual capsularis) and uterus (decidua vera) are separated by a rim of fluid within the uterine cavity. These separate decidual linings can be visualized sonographically, which commonly is referred to as the "double decidual sac sign."14
Identification and Localization of the Pregnancy
Localization of first-trimester pregnancies can be categorized into three groups: intrauterine, extrauterine, or indeterminate. Although there are a myriad of diagnoses, they all can be classified sonographically into one of five diagnostic possibilities. (See Table 2.) The significance of this unambiguous classification scheme is that it corresponds with the emergency physician’s management of these first-trimester symptomatic patients.

Intrauterine Pregnancy. To define the pregnancy as intrauterine, it is imperative to have a clear understanding of embryonic development as outlined above. Keeping this in mind, several pearls of wisdom are addressed regarding the location and viability of patients with first-trimester vaginal bleeding. First, it is important to ensure that definitive signs of a pregnancy are observed, documented, and recorded. (See Table 3.)

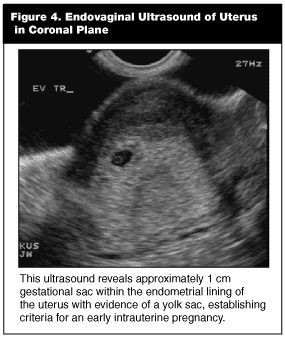
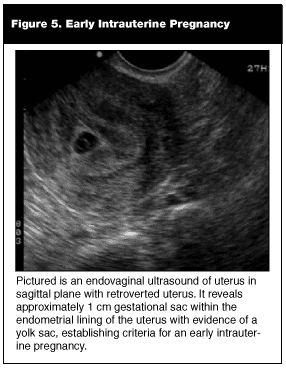
Secondly, these signs must be visualized clearly within the endometrial lining of the uterus. Whether scanning from a transabdominal or endovaginal approach, landmarks documenting a pregnancy within the uterus must be visualized on every sonogram. The novice sonographer occasionally will use the zoom feature and record or print an image of a pregnancy without any definite landmarks confirming the pregnancy as intrauterine. (See Figures 4 and 5.) The problem is that ectopic pregnancies can be indistinguishable from this particular example of a coned-down view. (See Figures 7 and 8.) The safest way to ensure that structures indeed lie within the uterus is to identify the bladder as a separate structure anterior to the uterus. Preferably, this is documented in real time or on a single window if stills are used for documentation. The next step in establishing the intrauterine pregnancy is identifying the gestational sac within the endometrial echo of the uterine fundus. Modern endovaginal transducers running at high frequencies are capable of identifying gestational sacs as small as 2 mm in diameter. However, at this stage, the gestational sac is nearly impossible to decipher from other conditions that cause intrauterine fluid collections. These include bleeding, endometritis, endometrial cysts, cervical stenosis, and, of course, the anxiety-provoking pseudogestational sac of ectopic pregnancy. It is only the latter condition that is associated with a positive beta-HCG level. To be considered a normal pregnancy, this sac also should have the "double decidual sac sign" and a yolk sac or fetal pole. Once these structures are present, one can be certain that at least one pregnancy is intrauterine. By identifying pregnancies as intrauterine, the physician effectively has ruled out an ectopic with reasonable certainty.
Live Intrauterine Pregnancy. Once the pregnancy is determined to be intrauterine, the next designation one must make is viability. This involves the real-time documentation of cardiac activity normally present at six weeks gestational age. Depending on the age of the fetus, this can be accomplished using either the transabdominal or endovaginal technique. We default to an endovaginal technique in any patient fewer than 10 weeks by dates or not obviously gravid. Simply having a gestational sac with a yolk sac or fetal pole does not suffice. For our purposes, an IUP is not live until cardiac activity is documented. The flickering of cardiac activity is an unmistakable sign of life identified by the novice sonographer and the patient.
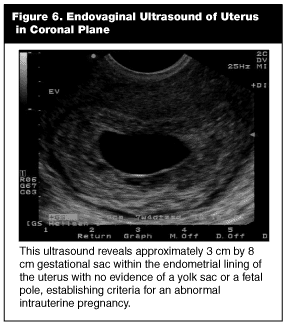
Abnormal Intrauterine Pregnancy. The criteria to define a pregnancy as abnormal are the same as an intrauterine pregnancy, except that the gestational sac is disproportionate to its contents. For example, by the time a gestational sac measures 13 mm in diameter, a yolk sac clearly should be visualized. Likewise, by 18 mm, all intrauterine gestational sacs containing live embryos should have cardiac activity. Therefore, using conservative criteria, it is safe to conclude that any sac greater than 13 mm without a yolk sac, or greater than 18 mm without evidence of cardiac activity, is termed abnormal. (See Figure 6.) It has been proven in the obstetrical ultrasound literature that gestation sacs reaching this size have virtually no viability and ultimately should result in miscarriage.14 Although it is safe to conclude that any pregnancy fulfilling this criteria is abnormal, the management will vary depending upon the individual patient’s clinical and emotional circumstances. In cases where the viability is equivocal, there is no rush to make a specific diagnosis (IUP vs abnormal IUP) as long as the pregnancy is clearly intrauterine. These cases should be re-evaluated in two days by obstetrical colleagues, at which time a repeat ultrasound and Beta-Quantative human chorionic gonadotropin (B-HCG) level may be considered.
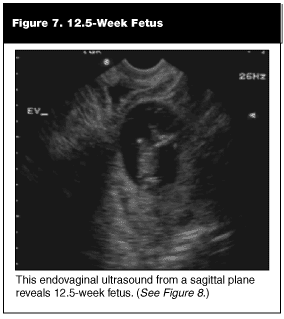
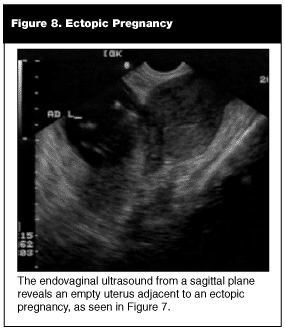
Extrauterine Pregnancy. Of the three locations that a pregnancy can exist, the ectopic frequently is difficult to diagnose. As opposed to the intrauterine pregnancies where ultrasound confirms a diagnosis, the extrauterine pregnancy rarely is substantiated by ultrasound. The incidence of ectopic pregnancy is one in every 64. The criteria for diagnosis of an extrauterine gestation is a gestational sac outside the endometrial echo of the uterus with evidence of a yolk sac or fetal pole. (See Figures 7-9.) In our ED, approximately 4% of symptomatic first-trimester pregnancies meet these criteria. The remaining ectopics will be confirmed either in the operating room (OR) or on an outpatient basis.
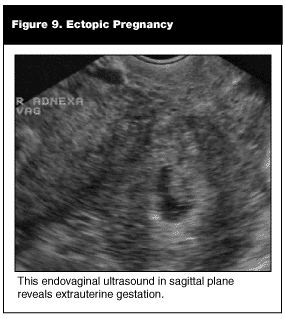
The "ruptured" ectopic frequently is suspected on clinical grounds. Supportive sonographic findings of an intraperitoneal fluid collection and/or an adnexal mass further strengthens this suspicion.15 Recent literature suggests that a transabdominal approach revealing a large intraperitoneal fluid collection will decrease the time-to-diagnosis and treatment.16 This information is tremendously helpful when discussing the case with OB/GYN consultants and leads to shorter door-to-OR times.
No Definitive Intrauterine Pregnancy (NDIUP). The diagnosis of NDIUP is established when a technically adept emergency ultrasound examination fails to diagnose an intrauterine or extrauterine gestation. (See Figure 10.) When this "location" of the first trimester is encountered, three possible diagnoses exist. First, it is possible that an early intrauterine pregnancy is present but no definitive signs are visualized within the uterus by ultrasound. Secondly, the products of conception have been aborted and cannot be discerned by ultrasound or physical examination. Lastly, a concealed ectopic pregnancy is unidentified by emergency ultrasound.
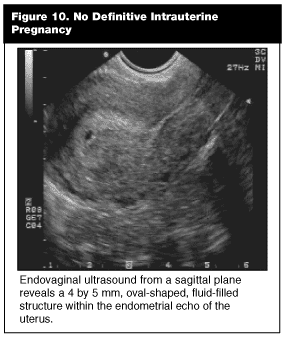
Absence of proof is not proof of absence. Bear in mind that patients diagnosed with NDIUP are high risk for an ectopic. In our institution, 40% of these patients eventually were diagnosed with an ectopic pregnancy. Similar data is supported by the literature in other academic emergency centers.11 Suspicion further is heightened by sonographic findings of intraperitoneal fluid or an adnexal mass. The take-home message is that all patients diagnosed with NDIUP should be managed closely by obstetrical colleagues, regardless of their beta-HCG level. An interdepartmental policy addressing this issue clearly would be advantageous to each specialty and the patient.
Discussion
The acquisition of ultrasound skills necessary to adequately evaluate the obstetrical patient requires considerable expertise. By directing the majority of our obstetrical ultrasound education to the symptomatic first-trimester pregnancy, we parallel our efforts to better identify patients with life-threatening emergencies. Ectopic pregnancy is responsible for more maternal deaths worldwide than any other obstetrical emergency.17 An imaging skill that rapidly can identify these high-risk patients should be readily available to every emergency physician at a moment’s notice.
Unfortunately, ultrasound is not a skill that can be mastered during a weekend course. In fact, it might take years for the average physician to become proficient in evaluating all aspects of the symptomatic first-trimester pregnancy. For some, this enlightenment might discourage the pursuit of integrating ultrasound into one’s practice, but be patient. There are various levels of sonographic skills at which even the dedicated beginner is capable of making important disposition decisions. For example, obtaining the basic skills necessary to safely and consistently identify a live intrauterine pregnancy is an excellent foundation. A graduated ultrasound educational process then might be undertaken to establish other areas of proficiency. Each successive level of competency then could correlate with an increased capacity of decision-making. In this conservative approach, new skills would be added in a graduated fashion instead of an all-or-none phenomenon. A lesson from obstetrical colleagues should be learned and applied to all areas in which emergency ultrasound is useful: Shoot for mastery and you will provide better care to your patients.
Despite good intentions of safely implementing an ultrasound program into a hospital or group practice, pitfalls are inevitable. After years of providing ultrasound education, a pattern of learning is so consistent that it’s worth sharing to help others forgo the same mistakes. The pattern goes something like this:
- Puzzled stage: "Those things they keep pointing out on the screen all look the same, with slightly varied shades of gray"
- Eureka: "Now I understand what they have been talking about"
- Embolden: "Now I’ve got it!" and, finally,
- Safe Again: "There are limitations, and I don’t like venturing out on that limb." The Embolden, or affectionately termed "sophomoric," phase of the emergency ultrasound learning curve, is the point at which you feel you have a pretty good handle on ultrasound.
Strive to systematically approach every patient in the technical aspect of the ultrasound examination. Define the boundary of each organ you are evaluating. Document the landmarks pertinent to every emergency ultrasound application you undertake. Always obtain confirmatory studies when you are unsure of the diagnosis or have inadequate quality of images. Lastly, develop a quality assurance process to share technical and interpretative teaching points and interesting cases.
References
1. SAEM position Statement: www.saem.org/publicat/ultrasou.htm. Accessed 12/10/2002.
2. Use of ultrasound imaging by emergency physicians. American College of Emergency Physicians web site: www.acep.org/1,684,0.html. Accessed on 12/10/2002.
3. Core Content for Emergency Medicine. Ann Emerg Med 1997;29:792-811.
4. Bahner D, Tayal V, Quick G. Emergency medicine ultrasound: The newest member of the AIUM. American College of Emergency Physicians web site www.acep.org.
5. Allison EJ Jr, Aghababian RV, Barsan WG, et al. Core Content for Emergency Medicine. Task Force on the Core Content for Emergency Medicine Revision. Ann Emerg Med 1997;29:6792-811.
6. Fletcher JC, Evans MI. Maternal bonding in early fetal ultrasound examinations. N Engl J Med 1983;308:392-393.
7. Durham B, Lane B, Burbridge L, et al. Pelvic ultrasound performed by emergency physicians for the detection of ectopic pregnancy in complicated first-trimester pregnancies Ann Emerg Med 1997;29:338-347.
8. Choi H, Blaivas M, Lambert MJ. Gestational outcome in patients with first-trimester complications and ultrasound-confirmed live intrauterine pregnancy. Acad Emerg Med 2000;7:200-203.
9. Jouppila P, Huhtaniemi I, Tapanainen J. Early pregnancy failure: Study by ultrasonic and hormonal methods. Obstet Gynecol 1980;55:42-47.
10. Durston W, Carl ML, Guerra W. Patient satisfaction and diagnostic accuracy with ultrasound by emergency physicians. Am J Emerg Med 1999;17:642-646.
11. Shih C. Effect of emergency physician-performed pelvic sonography on length of stay in the emergency department. Ann Emerg Med 1997;29:348-352.
12. Pandya PP, Snijder RJ, Psara N, et al. The prevalence of non-viable pregnancy at 10-13 weeks of gestation. Ultrasound Obstet Gynecol 1996;7:170-173.
13. Burke RK, Fine RA. Basic physical principle of ultrasonography for the practicing clinician. Infert and Reprod Med Clin North Am 1991;2.
14. Filly, R. Ultrasound evaluation during the first trimester. In: Callen PW, ed. Ultrasonography in Obstetrics and Gynecology. 3rd ed; Philadelphia W.B. Saunders 1994:63-69 1994.
15. Mateer JR, Valley VT, Aiman EJ. Outcome analysis of a protocol including bedside endovaginal sonography in patients at risk for ectopic pregnancy. Ann Emerg Med 1996;27: 283-289.
16. Rodgerson J, Heegaard W, Plummer D, et al. Emergency department right upper quadrant ultrasound is associated with a reduced time to diagnosis and treatment of ruptured ectopic pregnancies. Acad Emerg Med 2001;8:331-336.
17. Grimes DA. The morbidity and mortality of pregnancy: Still risky business. Am J Obstret Gynecol 1994;170:1489-1494.
18. Filly RA. Ectopic pregnancy: The role of sonography. Radiology 1987;162:661-668.
In this article and the succeeding two parts in this series, three distinctive applications of ultrasound in the ED will be discussed. The ability to perform a proficient and diagnostically effective ultrasound examination requires a judicious understanding of the underlying principles.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
