Updates and Future Direction on Medical Uses for Probiotics
December 1, 2014
Reprints
Executive Summary
The probiotic movement is rapidly growing and, although to date no probiotics have been approved by the FDA, they are actively marketed to the public as either foods or dietary supplements. It behooves the primary care physician to be familiar with the science, indications, and appropriate usage of probiotic therapies.
Advances in DNA sequencing, resulting in the new field of study called metagenomics, and the recently launched Human Microbiome Project by the NIH have propelled interest and research into probiotics.
Infants born by cesarean section have an altered microbiota, with epidemiological studies reporting increased risk of allergic rhinitis, asthma, celiac disease, type I diabetes, and obesity.
Probiotic usage in newborns has been shown to prevent severe necrotizing enterocolitis and all-cause mortality in preterm infants.
Increasing evidence indicates an association between the human microbiome and a wide range of diseases including C. difficile infection, irritable bowel syndrome, and inflammatory bowel disease.
Oral probiotics seem to evoke their effects through regulating function including gene expression and metabolism of established gastrointestinal microbiota ecosystems rather than actually changing existing microbial composition itself.
The risk of probiotic use is extremely low, but caution is advised in immunocompromised patients, premature infants, and those patients with intravascular catheters and advanced valvular heart disease.
Probiotics are defined by the World Health Organization as live microorganisms that, when administered in adequate amounts, confer a health benefit.1 Probiotics are available in "functional foods” that contain live active cultures of various bacterial species — such as yogurt, sauerkraut, tempeh, kombucha, and others — or as dietary supplements in the form of capsules, tablets, and powders. Governmental regulation in the United States depends on the product’s intended use: a food ingredient, dietary supplement, or a drug. To date, probiotics have only been marketed to the public as either foods or dietary supplements. While no probiotics have been approved by the FDA for specific therapeutic purposes as a medication, some are undergoing FDA review. Although the FDA allows dietary supplement manufacturers to advertise structure and function claims — e.g., stating that probiotics help maintain normal gut function — it does not allow supplement manufacturers to make unproven health claims (i.e., describing a purported relationship between a certain product and the reduced risk of a disease or illness).
Probiotics, Then and Now
Interest in probiotics has proven to be a growth industry for both consumers and supplement manufacturers. In 2011, sales of probiotic supplements in the United States totaled nearly $770 million and they continue to be one of the fastest growing dietary supplements.2 Since the early 20th century when Russian Nobel Laureate Elie Metchnikoff first proposed the idea of ingesting microbes for health benefits, there has been ongoing investigation into both the basic and applied clinical sciences.3 Two events have dramatically enhanced researchers efforts to understand the role of probiotics and human health. First, advances in DNA sequencing technologies have resulted in a new field of study called meta-genomics, which allows researchers to analyze microbial species and communities by their genetic material alone without the need to culture organisms. Second, the National Institutes of Health launched the Human Microbiome Project in 2008, with the mission to identify and characterize the microbial communities that inhabit both healthy and unhealthy people. In addition, the National Center for Complementary and Alternative Medicine has increased efforts to investigate both mechanism of action as well as the clinical effects of probiotics, which are now considered a "high priority” for future studies.
Gut Flora, The Early Years
More than 100 trillion microbes reside within the human gastrointestinal (GI) tract. The GI microbiota develop quickly during the early newborn period, with subsequent windows of susceptibility and alteration throughout childhood development prior to the establishment of a relatively stable "adult” gut microbiota.4 Acquisition of this GI microbiota is initiated at birth through the labor and delivery process, with cesarean-delivered infants demonstrating an altered microbiota in terms of diversity, quantity, and quality compared to infants born vaginally.5 The potential long-term consequences of this altered microbiome have raised concerns due to cesarean delivery rates in the United States reaching 33% in 2012. This is especially important since epidemiology studies report increased risk of allergic rhinitis, asthma, celiac disease, type 1 diabetes, and obesity (among others) associated with cesarean delivery.6,7,8 The causal relationships between these variably acquired microbiomes and childhood diseases continues to be an active area of research.
Therapeutically, the use of probiotics in newborns has been shown to prevent severe necrotizing enterocolitis and all-cause mortality in preterm infants, as well as to provide benefit in preventing atopic dermatitis development and severity in newborns.9,10 Another example is that the rate of invasive candidiasis infections — which occur in low birth weight infants at a rate of up to 15% and have a high mortality and morbidity rate — is decreased by introducing oral combination preparations of Bifidobacterium infantis and longum, Bifidobacterium lactis, and Lactobacillus acidophilus. It also appears that multiple strains of probiotics at this vulnerable stage of life have greater efficacy compared to single species.11,12 Another double-blind, randomized, controlled trial (RCT) found that, compared to controls, low birth weight neonates who were given probiotics to modulate the developing gut microflora were able to establish full enteral feedings quicker, and had shorter hospitalizations and reduced fungal colonization and infection rates.13
Clinical Research Overview and Updates
This established GI microbiota can shift due to influences as such as aging, diet, geographical location, intake of food supplements and medications, infectious disease, chronic illness, and likely other yet unknown factors.14 Current research challenges with probiotic interventions include what probiotic strains should be used for what conditions, in which people, for how long, and at what dose and type of delivery. Although probiotics and gut microbiota research is still in its infancy, there are several promising examples to help guide therapy considerations.15 (See Table 1.) There is increasing evidence that indicates an association between the composition of the human microbiome and a wide range of diseases, including Clostridium difficile infection (CDI), irritable bowel syndrome (IBS), inflammatory bowel disease (IBD), colonization with multidrug-resistant organisms, cancer, osteoporosis, cardiovascular disease, obesity, allergic diseases, autoimmune disorders, and neuropsychiatric illnesses.14,16,17,18
Lactobacillus reuteri treatment in ovariectomized menopausal mice was found to significantly reduce osteoclastic activity, which led to reduced bone loss.19 This was also observed in humans, noting that the presence of colonic Lactobacillus and Bifidobacteria increase the bioavailability of calcium and other minerals through various complex mechanisms of enhanced absorption and bioavailability.18
|
Table 1. Summary of Reported Uses of Specific Probiotic Strains for Various Health Effects |
||
|
|
Reported potential |
|
|
Bifidobacterium infantis |
Helps ICI among newborns |
Betta 2014 Sepp 2013 |
|
Bifidobacterium longum |
Helps ICI among newborns |
Betta 2014 Sepp 2013 |
|
Bifidobacterium bifidum |
Reduces severity and incidence of pouchitis |
Tomasz 2014 |
|
Lactobacillus & Bifidobacteria spp. |
Increases bioavailability of calcium and other minerals through enhanced absorption and bioavailability Improves hepatic venous pressures and ascites in cirrhosis Improves acute respiratory infections Benefits type 1 and 2 diabetes and obesity Improves gas and bloating in irritable bowel syndrome |
Parvaneh 2014 Rincon 2014 Lehtoranta 2014 Mykhal’chyshyn 2013 Kondrashova 2014 Torres-Fuentes 2014 Chen 2014 Cash 2014 |
|
Lactobacillus casei |
Alleviates tender swollen joints and decreases inflammatory cytokines in rheumatoid arthritis |
Alipour 2014 |
|
Lactobacillus plantarum |
Lowers cholesterol, glucose, homocysteine, and inflammatory biomarkers in metabolic syndrome |
Barreto 2013 |
|
Lactobacillus paracasei |
Prevents antibiotic-associated diarrhea |
Lenoir-Wijnkoop 2014; |
|
Lactobacillus delbrueckii |
Reduces severity and incidence of pouchitis |
Tomasz 2014 |
|
Lactobacillus acidophilus |
Helps ICI among newborns Reduces severity and incidence of pouchitis |
Betta 2014 Sepp 2013; Tomasz 2014 |
|
Lactobacillus bulgaricus |
Reduces severity and incidence of pouchitis |
Tomasz 2014 |
|
Lactobacillus reuteri |
Reduces osteoclasts and bone loss Reduces cariogenic Streptococcus mutans |
Britton 2014; Duse 2014 Laleman 2014 |
|
Doses range from 10 to 99 x 109 CFUs |
||
|
Bifidobacterium lactis |
Helps invasive candidiasis infection (ICI) among newborns; Reduces cariogenic Streptococcus mutans |
Betta 2014 Sepp 2013 Duse 2014 Laleman 2014 |
Relevant to rheumatoid arthritis, one recent RCT concluded that probiotic supplementation with a capsule of 108 colony forming units (CFU) Lactobacillus casei taken orally every day for 8 weeks helped alleviate symptoms of tender, swollen joints and improve overall disease activity scores by decreasing various inflammatory cytokines when compared to controls.20
A review on the effect of probiotics on the incidence of dental caries found only two suitably qualified articles in terms of quality and methodology; nonetheless, these studies showed that patients who were treated with probiotics had significantly lower Streptococcus mutans — the bacteria responsible for caries — compared to controls at the end of treatment. However, there were no noticeable differences between groups regarding beneficial Lactobacillus counts.21 The authors concluded that probiotic supplementation might have a positive effect in preventing dental caries by reducing S. mutans activity. In corroboration of these findings, a laboratory study used breast milk that was fermented with L. reuteri and B. lactis. Compared to non-fermented samples, milk containing these probiotics showed significantly less growth of S. mutans after 24 hours of inoculation and incubation,22 showing the direct inhibitory effect of these probiotics on cariogenic S. mutans.
Regarding patients with cirrhosis and ascites, one small study of 12 participants found that administration of oral VSL#3 (a proprietary blend of several probiotic strains of Lactobacillus and Bifidobacterium species) resulted in improved hepatic venous pressures and overall systemic hemodynamics and serum sodium levels, which are problematic in liver disease of this severity. What’s more, no adverse effects were observed over the 6-week intervention.23 This also hints at the potential cost effectiveness of probiotics as an adjunctive therapy against the progression of portal hypertension and its serious complications.
When it comes to acute respiratory infections, probiotics have been shown in more than 28 clinical trials to impart significant benefit compared to five trials that showed no benefit.24 Incidentally, none of these studies reported any harm from probiotics use. Based on these and other studies, probiotics appear to exert direct antiviral properties in addition to immune system upregulation of the host. This is not surprising given the evolutionary adversarial relationship bacteria and viruses share (e.g., bacteriophages, competition for hosts), in addition to the growing understanding of the intimate and complex interactions of the gut microbiota with the gut-associated lymphoid tissue. However, these studies varied greatly in quality and design, and further research is still needed.
There is considerable excitement for the potential use of probiotics in metabolic disorders, including obesity, diabetes, and metabolic syndrome. Considering the negative impact that cardiovascular disorders impart on individuals and society at large, probiotics may prove to be an inexpensive, safe, and efficacious tool in these lifestyle-related disorders.
In patients with type 2 diabetes and non-alcoholic fatty liver disease, oral administration of the multi-probiotic product Symbiter — along with usual standard of care (i.e., diabetic medications) — decreased inflammatory cytokine and liver transaminase levels over 30 days compared to controls.25
In type 1 diabetes, in which enteroviruses are a known trigger for the autoimmune destruction of pancreatic insulin-producing beta cells, the possible protective effects from various probiotics have been investigated in both animal and epidemiological studies. Certain microbes and gut microbiota patterns have been observed to be associated with a lower risk of developing type 1 diabetes, suggesting the possible protective effect of probiotics in having a significant benefit during early childhood.26
Further along the age spectrum, 24 postmenopausal women diagnosed with metabolic syndrome who were given dietary milk fermented with Lactobacillus plantarum daily demonstrated lower cholesterol, glucose, homocysteine, and other inflammatory biomarker levels over 90 days compared to those who were given non-fermented milk.27
Going further yet, obesity — which is at epidemic proportions worldwide and quickly is becoming the most significant health risk overall — may benefit from modulation of gut microbiota through diet changes and probiotic supplementation (in addition to essential changes in regular physical activity). Strains of Lactobacillus and Bifidobacteria, in combination with other lifestyle changes, have been shown to confer health benefit and appear to directly combat obesity.28,29
IBS and Other Gut Disorders
Of all disorders, derangements of the gut and microbiota alteration are the most hopeful in terms of research and therapy. The prevention and treatment of various GI disorders by manipulation of dysfunctional microbial ecosystems — often referred to as dysbiosis — with orally administered probiotics has been widely studied with varying strengths of evidence. However, overall, the strongest evidence for use of probiotics includes GI-related disorders such as IBS, IBD, pouchitis, CDI, antibiotic-associated diarrhea (AAD), and various other forms of infectious diarrhea.30,31 Most studies and clinical regimens have used oral probiotic doses in the range of 10 to 900 x 109 CFUs.32 Unfortunately, as previously mentioned, there are significant limitations and variation among studies that raise many more questions regarding efficacy, viability, optimal species and genus selection for specific conditions among different people, single vs combination products, optimal CFU dosing, and adequate treatment duration.15
Although incompletely understood, purported mechanisms of benefit from probiotic use include the direct remodeling of microbial communities, competition to/suppression of pathogens, enhanced immune function/modulation, upregulation of anti-inflammatory factors, suppression of pro-inflammatory factors, and proliferation and promotion of intestinal epithelial barrier function.31 Interestingly, however, few studies have actually documented the survival of orally administered probiotics after passage through the caustic upper GI tract environment. Further, probiotic effects have been demonstrated using both viable and non-viable bacteria.33,34 What’s more, colonization of the GI tract from orally administered probiotics appears to be temporary at best, with noted disappearance of introduced strains from the stool soon after discontinuation. In general, oral probiotics appear to have their effects via regulating the function — including gene expression and metabolism — of the already established GI microbiota ecosystem, rather than actually changing the existing microbial composition itself.35
Pursuit of the modulation of intestinal microflora is an intuitive therapy for many gut disorders. Foremost is IBS, which involves disruption of the colonic microbiota in various ways. There are various manifestations of IBS, such as constipation, diarrhea, bloating, and mixed symptom variations. Overall, IBS is a heterogeneous disorder characterized by abnormal GI motility, altered GI microbiota composition, low-grade chronic inflammation, visceral hypersensitivity and hyperalgesia, and disruption of the gut-brain communication axis. However, specific identification of biologic markers based on genetic polymorphisms remains undetermined and inconsistent.36 It is also important to keep in mind that IBS is a functional bowel disorder with many contributing factors, including a significant association with abuse and other trauma. The pathogenesis of IBS is multi-dimensional, and is heavily influenced by bio-psychosocial dysfunction in various forms. Stress, although not considered a cause of IBS, is nonetheless a significant trigger that is often present with IBS flares for many patients.36
Specifically regarding altered gut microbiota, there does appear to be a consistent theme of reduced Bacteroides and increased Firmicutes strains in IBS,37 but actual characterization of individual gut flora remains difficult and inconsistent. Nonetheless, research suggests that targeted treatment using certain antibiotics and select probiotics based on individual differences in intestinal microbiota composition may be effective in alleviating IBS symptoms.37 A recent meta-analysis reported that overall, all probiotic species and strains appear to improve flatulence and bloating in patients with IBS compared with placebo.38 This meta-analysis concluded that probiotics, in general, improve overall IBS symptoms for most patients.38 However, one RCT found no significant benefit from using a multispecies probiotic oral supplement for 6 weeks among 35 patients diagnosed with IBS. In this placebo-controlled trial, visceral hypersensitivity decreased significantly for both the probiotic group as well as the control group, but overall pain scores and mean symptom scores did not differ overall.39
In addition to probiotic therapy, use of non-systemic antibiotics neomycin and rifaximin also appear to improve IBS symptoms, but neomycin is limited by ototoxicity in some patients, and increased antibiotics use overall increases the risk of further antibiotic resistance. Nonetheless, RCTs have shown that rifaximin-treated patients were significantly more likely than placebo to achieve adequate relief of IBS symptoms.38
When it comes to iatrogenic AAD, one study found that older hospitalized patients being treated with antibiotics for various reasons were less likely to contract AAD when given Lactobacillus paracasei fermented milk prophylactically. This was also found to be very cost effective, with a total estimated cost savings of over $575 per hospitalized patient older than 65 years of age, which is a particularly vulnerable demographic.40 This finding is consistent overall in terms of using probiotics for the prevention of gut-associated disorders of nearly every kind, noting that one study concluded an average risk reduction of 35% compared to placebo in maintaining gut homeostasis for various GI conditions.41
In more severe disease states, such as IBD, altered gut microbiota (dysbiosis) appears to be a key player in the prolonged and relentless course of these disorders. Several studies have found an association with polymorphisms in genes that are involved in autophagy — a process that involves cell degradation of unnecessary or dysfunctional cellular components that helps maintain healthy cells — which is thought to be a result of the innate relationship of host cells with adjacent luminal gut bacteria. The inverse also appears to be true; specific gut pathogens may have a negative impact on the gut microbiome, which in turn generate protracted inflammation and immune dysfunction, which may result in the pathogenesis of IBD.42
In the setting of pouchitis, among patients who undergo restorative proctocolectomy for various reasons, including severe IBD, prolonged probiotic administration appears to be helpful. In a study of 43 randomized patients given a daily probiotic consisting of L. acidophilus, Lactobacillus delbrueckii, Lactobacillus bulgaricus, and Bifidobacterium bifidum for 9 months, the average severity and incidence of pouchitis decreased significantly over 9 months compared to placebo. Objective biomarkers for pouchitis were also lower in the treatment group, noting lower levels of fecal pyruvate kinase and calprotectin. This study also demonstrated that long-term probiotics use is safe and effective in preventing pouchitis episodes.43
Novel Probiotic Therapies: Fecal Transplantation
Microbiota restorative therapies, such as fecal microbiota transplantion (FMT), provides direct anatomical delivery of various healthy microbial species to diseased or dysfunctional colons. While FMT has yet to be fully approved by the FDA, it is permitted for use in select patients for the treatment of recurrent and treatment refractory CDI. Risk of recurrence of CDI is high with use of oral antibiotics such as vancomycin and metronidazole, particularly in recurrent disease. Despite use of new novel antibiotics, such as fidaxomicin, the threat of growing resistance continues. For this and other reasons, FMT is attracting increased attention from physicians and patients alike. There are currently more than 500 case reports of FMT for the treatment of CDI, with greater than 91% efficacy.17,44
Given its impressive success with severe CDI, there is growing interest for the use of FMT for additional GI disorders such as IBS and IBD, as well as other "extra-intestinal” conditions such as diabetes, obesity, multiple sclerosis, and idiopathic thrombocytopenic purpura among many others.45 While the potential application of FMT is expanding, there are concerns for risk of inadvertent transmission of various pathogens and infectious diseases. Appropriate donor selection, standardization of donor stool preparation, insurance reimbursement, and long-term safety and efficacy are ongoing concerns.17 Additionally, there is a general cultural aversion to the idea of "stool sharing.” Ideally, a clearer understanding of the optimal probiotic composition for specific disorders will likely lead to strategic microbiota "mining” from healthy donor stool samples vs production and selection of various specific bacterial strains in microbiology laboratories without the potential risks of FMT.
Direct Colonic Probiotic Delivery
Concurrent with the rising interest in FMT is the more facile idea of direct colonic delivery of probiotics (DCPD) in single or combination strains. The direct anatomical delivery of probiotics has also been explored in oral and vaginal disorders with some reported benefit.46,47 However, research into the rectal application of probiotic supplements for GI disorders has been largely absent, with the exception of a few small trials of an enema-supplied single-species probiotic for ulcerative colitis, which was well tolerated and showed some benefit.48,49
Due to research findings of altered GI microbiota in various illnesses (e.g., IBS, IBD, etc.) — including diminished bacterial diversity — combined with the promising results of whole GI microbiota transplantation through FMT, we have utilized multiple probiotic species using various over-the-counter probiotic products through DCPD.50
For gut-related disorders (such as IBS and AAD) for which a trial of daily oral probiotics for 2-4 weeks has not been helpful, the direct delivery of multistrain probiotics is a reasonable follow-up strategy, given that this approach circumvents the caustic upper GI environment.33,34,35 Although research supporting DCPD use is surprisingly lacking, anecdotal evidence and case reports are promising. In the clinical setting, for medically stable, non-immunocompromised patients who struggle with various GI-related symptoms, but who find only limited success from standard of care therapies including oral probiotic use, it is reasonable to consider DCPD as an adjunctive therapy when prescribed under careful clinical supervision.
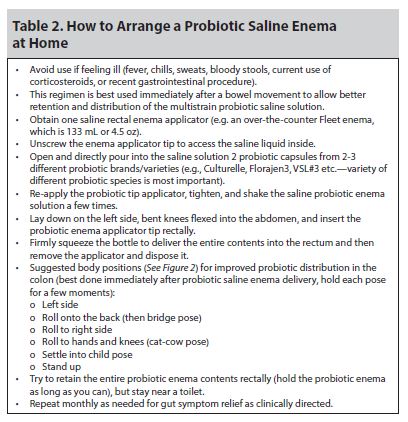
DCPD should use an isotonicsaline solution transport medium, which is the preferred delivery agent for FMT.51 While further research is needed, this approach has been used successfully and safely in the clinic setting. In addition to implementing a healthy diet and regular exercise (see www.meriter.com/wellness for exercise and nutrition prescriptions and Figure 1), DCPD can be considered and used in properly screened patients who are willing and able (See Table 2).
Adverse Effects of Probiotics
A 2011 Agency for Healthcare Research and Quality assessment of the safety of probiotics concluded that current evidence does not suggest widespread risk or negative side effects associated with probiotics. However, the data on safety and long-term safety are limited, and the risk of serious side effects may be greater in people who have serious and unstable underlying health conditions.52 Although probiotics fall under an FDA category of generally recognized as safe, or having been adequately shown to be safe for general consumption, there are some situations where caution should be used.
A case of Saccharomyces cerevisiae fungemia was reported in a patient with CDI who was being treated with oral Saccharomyces boulardii in association with vancomycin. Although fungemia is rare in this situation, it is a serious complication and risk when prescribing this probiotic, especially in unstable immunocompromised patients.53
A 2006 review reported that only 78 cases of Lactobacillus bacteremia and endocarditis had been reported in the literature, mostly related to dental procedures, an immunocompromised state, and recent colonoscopy procedure as predisposing conditions.54 A recent case of Lactobacillus paracasei endocarditis was reported in a 77-year-old patient who ate yogurt daily. Contributing events in this case were a recent colonoscopy and history of mitral valve prolapse and insufficiency. The authors concluded that probiotics in all forms should be stopped prior to any digestive surgery or procedure.55
Another example of caution involves the case of a 17-year-old patient diagnosed with ulcerative colitis who was being treated with corticosteroids and antibiotics. This patient was also given Lactobacillus rhamnosus GG (Culturelle) by his parents and subsequently became septic. However, there was some clinical question as to whether the septic symptoms were from a concurrent viral illness. Nonetheless, the authors concluded that an active immunocompromised status appears to be a risk factor for infection from probiotics, although the incidence is very low.56
In the setting of short bowel syndrome, small intestine bacterial overgrowth (SIBO) is common and oral probiotics should be used cautiously, being careful to avoid regimens that have CFUs > 20 billion CFU used more than once a day, if at all.57 Even in patients without short bowel syndrome, bloating and abdominal cramping from SIBO or SIBO-like passage of bacteria through the small bowel can occur, though it is typically self-limited and resolves with cessation of oral probiotic therapy.

In general, the risk of probiotics use is extremely low, but several conditions warrant close medical supervision and caution: immunocompromised state, premature infant patients in the neonatal period, presence of any type of intravascular catheter, impaired intestinal epithelial barriers, and advanced cardiac valve disease.58
Prescribing Oral Probiotics
Typical use of oral probiotics doses range from 1 million to 100 billion CFUs by most guidelines for infants, children, and adults. For example, to treat diarrhea, doses should be at least 10 billion CFUs per day until resolved.59 Most guidelines recommend taking probiotics on an empty stomach, 1-2 hours before or after eating to reduce gastric acid exposure, which can significantly reduce bacteria viability and successful passage through the gut.
Although use of daily probiotics is considered safe, data are sparse and mixed as far as chronic use of oral probiotics for health maintenance, and more research is needed. However, consumption of probiotic-containing foods, such as yogurt, can be safely used on a long-term daily basis for most people.
Probiotics should be used at the onset of antibiotic use, taken on an empty stomach 1-2 or more hours before or after antibiotic ingestion, and continued for 3-7 days beyond the completion of antibiotics.60 For example standard regimens include 1 capsule by mouth between meals, taken 1-2 times a day for 14 days if the antibiotic is used 10 days, and then 21 days if the antibiotic is use is 14 days. For longer antibiotic courses, probiotics can be taken daily for 6-8 weeks (e.g., twice daily doxycycline antibiotics for 28 days in the setting of treating Lyme infections).
Conclusion
There is accumulating evidence regarding the relationship of the GI microbiota with GI health and disease. Reasonable and safe adjunctive therapy options for various GI and other disorders can include use of oral probiotics. However, caustic upper GI limitations of orally administered probiotic supplements — along with the impracticalities, cost, and concerns of inadvertently introducing pathogens through FMT — support further investigation into the DCPD of various probiotic preparations as a second line of probiotic therapy for various GI disorders in treatment refractory situations where oral probiotics are not effective.

Bottom Line
Oral probiotic therapies appear to be safe for most people and may be helpful for various health problems, but the human microbiome research is only in its infancy. The strongest clinical evidence is for use as an adjunctive supportive therapy for GI-related disorders, especially in the setting of preventing and treating AAD. Although FMT and DCPD therapies appear promising, further research is needed.
IBS Clinical Vignette
NJ is a 38-year-old female nurse with long-standing IBS. Past medical history includes anxiety, depression, acid reflux, insomnia, migraine, and dyslipidemia. Past surgical history includes appendectomy. Previous medical evaluations include gastroenterology (GI) evaluation, including upper and lower endoscopies. Various medication and supplement trials (including oral probiotics) over several years offered limited or no relief. Various diet changes (including gluten- and casein-free among others) over time also offered little to no relief. In addition, alternative medicine trials (including acupuncture, relaxation techniques, massage therapy, and various supplements) also offered temporary or no relief.
Patient enrolled in a hospital-/clinic-based IBS collaborative that includes GI evaluation and referral to team-based therapy that includes nutrition, health psychology, and integrative medicine evaluations (See Figure 1). However, after seeing her primary care physician, who recommended DCPD, patient experienced marked improvement several days after one treatment at home. In follow-up, patient reports that after 1 month, she has no IBS symptoms for the first time in memory. She reports no difficulty in obtaining the materials from a local grocery store and pharmacy, as well as ease of use in following the instructions.
References
- Joint Food and Agriculture Organization of the United Nations/World Health Organization Working Group report on drafting guidelines for the evaluation of probiotics in food, London, Ontario, Canada, April 30 and May, 2002. Available at: ftp://ftp.fao.org/es/esn/food/wgreport2.pdf. Accessed March 28, 2014.
- Reddy S. Probiotics’ Benefits May Be More Than a Gut Feeling. The Wall Street Journal Nov. 26, 2012. Available at: http://online.wsj.com/news/articles/SB10001424127887324784404578143402702878118. Accessed March 28, 2014.
- Podolsky SH. Metchnikoff and the microbiome. Lancet 2012;380:1810-1811.
- Petschow B, et al. Probiotics, prebiotics, and the host microbiome: The science of translation. Ann N Y Acad Sci 2013;1306:
1-17. - Azad MB. et al. Gut microbiota of healthy Canadian infants: Profiles by mode of delivery and infant diet at 4 months. CMAJ 2013;185:385-394.
- Martin JA, et al. Births: Final data for 2012. National vital statistics reports. National Center for Health Statistics 2013;62:1-20. Available at: http://www.cdc.gov/nchs/data/nvsr/nvsr62/nvsr62_09.pdf. Accessed Nov. 17, 2014.
- Neu J, Rushing J. Cesarean versus vaginal delivery: Long-term infant outcomes and the hygiene hypothesis. Clin Perinatol 2011;38:321-331.
- Isolauri E. Development of healthy gut microbiota early in life. J Paediatr Child Health 2012;48(Suppl 3):1-6.
- AlFaleh K, Anabrees J. Probiotics for prevention of necrotizing enterocolitis in preterm infants. Cochrane Database Syst Rev 2014;10;4:CD005496.
- Foolad N, et al. Effect of nutrient supplementation on atopic dermatitis in children: A systematic review of probiotics, prebiotics, formula, and fatty acids. JAMA Dermatol 2013;149:350-355.
- Betta P. Not all probiotics are the same: Gut microbiota modulation with a multistrain probiotics. N Am J Med Sci 2014;6:58-59.
- Sepp E, et al. The association of gut microbiota with body weight and body mass index in preschool children of Estonia. Microb Ecol Health Dis 2013;24. doi: 10.3402/mehd.v24i0.19231.
- Roy A, et al. Role of enteric supplementation of probiotics on late-onset sepsis by Candida species in preterm low birth weight neonates: A randomized, double blind, placebo-controlled trial. N Am J Med Sci 2014;6:50-57.
- Bäckhed F, et al. Defining a healthy human gut microbiome: Current concepts, future directions, and clinical applications. Cell Host Microbe 2012;12:611-622.
- Verna EC, et al. Use of probiotics in gastrointestinal disorders: What to recommend? Therap Adv Gastroenterol 2010;3:307-319.
- Mai V, et al. Recent advances and remaining gaps in our knowledge of associations between gut microbiota and human health. World J Gastroenterol 2009;15:81-85.
- Khanna S, Tosh PK. A clinician’s primer on the role of the microbiome in human health and disease. Mayo Clin Proc 2014;89:107-114.
- Parvaneh K, et al. Effect of probiotics supplementation on bone mineral content and bone mass density. Scientific World J 2014;595962. doi: 10.1155/2014/595962.
- Britton RA, et al. Probiotic L. reuteri treatment prevents bone loss in a menopausal ovariectomized mouse model. J Cell Physiol 2014;229:1822-1830.
- Alipour B, et al. Effects of Lactobacillus casei supplementation on disease activity and inflammatory cytokines in rheumatoid arthritis patients: A randomized double-blind clinical trial. Int J Rheum Dis 2014;17:519-527.
- Laleman I, et al. Probiotics reduce mutans streptococci counts in humans: A systematic review and meta-analysis. Clin Oral Investig 2014;18:1539-1552.
- Duse M, et al. The growth of Streptococcus mutans in different milks for infant feeding. Int J Immunopathol Pharmacol 2014;27:137-141.
- Rincon D et al. Oral probiotic VSL#3 attenuates the circulatory disturbances of patients with cirrhosis and ascites. Liver Int 2014;34:1504-1512.
- Lehtoranta L et al. Probiotics in respiratory virus infections. Eur J Clin Microbiol Infect Dis 2014;33:1289-1302.
- Mykhal’chyshyn HP, et al. [Effect of probiotics on proinflammatory cytokine levels in patients with type 2 diabetes and nonalcoholic fatty liver disease.] Lik Sprava 2013;56-62.
- Kondrashova A, Hyoty H. Role of viruses and other microbes in the pathogenesis of type 1 diabetes. Int Rev Immunol 2014;33:284-295.
- Barreto FM et al. Beneficial effects of Lactobacillus plantarum on glycemia and homocysteine levels in postmenopausal women with metabolic syndrome. Nutrition 2013;30:939-942.
- Torres-Fuentes C et al. A natural solution for obesity: Bioactives for the prevention and treatment of weight gain. A review. Nutr Neurosci 2014;Jan 3. [Epub ahead of print].
- Chen J, et al. Diet effects in gut microbiome and obesity. J Food Sci 2014;79:
R442-451. - Goldin BR, Gorbach SL. Clinical indications for probiotics: An overview. Clin Infect Dis 2008;46(Suppl 2):S96-S100.
- Preidis GA, Versalovic J. Targeting the human microbiome with antibiotics, probiotics, and prebiotics: Gastroenterology enters the metagenomics era. Gastroenterology 2009;136:2015-2031.
- Sartor RB. Probiotics for gastrointestinal diseases. UpToDate Updated June 9, 2014.
- Kailasapathy K, Chin J. Survival and therapeutic potential of probiotic organisms with reference to Lactobacillus acidophilus and Bifidobacterium spp. Immunol Cell Biol 2000;78:80-88.
- Jijon H, et al. DNA from probiotic bacteria modulates murine and human epithelial and immune function. Gastroenterology 2004;126:1358-1373.
- McNulty NP, et al. The impact of a consortium of fermented milk strains on the gut microbiome of gnotobiotic mice and monozygotic twins. Sci Transl Med 2011;3:106ra106.
- Chang FY. Irritable bowel syndrome: The evolution of multi-dimensional looking and multidisciplinary treatments. World J Gastroenterol 2014;20:2499-2514.
- Hong SN, Rhee PL. Unraveling the ties between irritable bowel syndrome and intestinal microbiota. World J Gastroenterol 2014;20:2470-2481.
- Cash BD. Emerging role of probiotics and antimicrobials in the management of irritable bowel syndrome. Curr Med Res Opin 2014;30:1405-1415.
- Ludidi S, et al. Randomized clinical trial on the effect of a multispecies probiotic on visceroperception in hypersensitive IBS patients. Neurogastroenterol Motil 2014;26:705-714.
- Lenoir-Wijnkoop I, et al. Nutrition economic evaluation of a probiotic in the prevention of antibiotic associated diarrhea. Front Pharmacol 2014;5:13.
- Vitetta L, et al. Probiotics, prebiotics and the gastrointestinal tract in health and disease. Inflammopharmacology 2014;22:
135-154. - Hold GL, et al. Role of the gut microbiota in inflammatory bowel disease pathogenesis: What have we learnt in the past 10 years? World J Gastroenterol 2014;20:
1192-1210. - Tomasz B, et al. Long-term use of probiotics Lactobacillus and Bifidobacterium has a prophylactic effect on the occurrence and severity of pouchitis: A randomized prospective study. Biomed Res Int 2014;208064. Doi: 10.1155/2014/208064. Epub 2014 Jan 21.
- McCune VL, et al. Faecal transplantation for the treatment of Clostridium difficile infection: A review. Int J Antimicrob Agents 2014;43:201-206.
- Smits LP, et al. Therapeutic potential of fecal microbiota transplantation. Gastroenterology 2013;145:946-953.
- Stamatova I, Meurman JH. Probiotics: Health benefits in the mouth. Am J Dent 2009;22:329-338.
- Mastromarino P, et al. Bacterial vaginosis: A review on clinical trials with probiotics. New Microbiol 2013;36:229-238.
- Oliva S, et al. Randomised clinical trial: The effectiveness of Lactobacillus reeuteri ATCC 55730 rectal enema in children with active distal ulcerative colitis. Aliment Pharmacol Ther 2012;35:327-334.
- Matthes H, et al. Clinical trial: Probiotic treatment of acute distal ulcerative colitis with rectally administered Escherichia coli Nissle 1917 (EcN). BMC Complement Altern Med 2010;10:13. doi: 10.1186/1472-6882-10-13.
- Human Microbiome Project Consortium. Structure, function and diversity of the healthy human microbiome. Nature 2012;486:207-214.
- Borody TJ, et al. Fecal microbiota transplantation: Indications, methods, evidence, and future directions. Curr Gastroenterol Rep 2013;15:337. doi: 10.1007/s11894-013-0337-1.
- Hempel S, et al. Safety of Probiotics to Reduce Risk and Prevent or Treat Disease. Evidence Report/Technology Assessment no. 200. Agency for Healthcare Research and Quality. Available at: www.ahrq.gov/clinic/tp/probiotictp.htm. Accessed May 13, 2014.
- Santino I, et al. Saccharomyces cerevisiae fungemia, a possible consequence of the treatment of Clostridium difficile colitis with a probioticum. Int J Immunopathol Pharmacol 2014;27:143-146.
- Salvana EM, Frank M. Lactobacillus endocarditis: Case report and review of cases reported since 1992. J Infect 2006;53:e5-e10.
- Franko B, et al. Lactobacillus paracasei endocarditis in a consumer of probiotics. Med Mal Infect 2013;43:171-173.
- Grace E, et al. Review article: Small intestinal bacterial overgrowth — prevalence, clinical features, current developing diagnostic tests, and treatment. Aliment Pharmacol Ther 2013;38:674-688.
- Vahabnezhad E, et al. Lactobacillus bacteremia associated with probiotic use in a pediatric patient with ulcerative colitis. J Clin Gastroenterol 2013;47:437-439.
- Floch MH. Probiotic safety and risk factors. J Clin Gasteroenterol 2013;47:375-376.
- Kliger B, Cohrssen A. Probiotics. Am Fam Physician 2008;78:1073-1078.
- Rogers B et al. PURLs: Prescribing an antibiotic? Pair it with probiotics. J Fam Pract 2013;62:148-150.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
