Peppermint Sticks It to IBS
Peppermint Sticks It to IBS
Abstract & commentary
By Allan J. Wilke, MD, Residency Program Director, Associate Professor of Family Medicine, University of Alabama at Birmingham School of MedicineHuntsville Regional Medical Campus, Huntsville. Dr. Wilke reports no financial relationship to this field of study.
Synopsis: Peppermint oil, psyllium, and antispasmodics are all effective in the treatment of IBS.
Source: Ford AC, et al. Effect of fiber, antispasmodics, and peppermint oil in the treatment of irritable bowel syndrome: Systematic review and meta-analysis. BMJ 2008;337:a2313.
The authors of this meta-analysis searched medline, Embase, and the Cochrane Controlled Trials Register for randomized controlled studies of treatment of irritable bowel syndrome (IBS) with fiber, antispasmodic drugs, or oil of peppermint. Treatment had to last at least a week to allow the plasma concentrations of the medications to reach steady state. They found 615 citations, of which only 101 were deemed potentially relevant. Of these, only 35 remained after exclusion. They were scored on the Jadad scale, which measures the quality of studies, and those studies that scored 4 or more, indicating good quality, were analyzed separately. The primary outcome was the percentage of subjects with "persistent or unimproved symptoms after treatment" (P/USAT), a lower percentage indicating a better result. The relative risk (RR) and the number-needed-to-treat (NNT) were calculated.
Twelve studies looked at fiber compared to placebo, 5 with bran, 6 with ispaghula husk (psyllium), and 1 with "concentrated" fiber. Seven of them were judged good quality. Although fiber significantly improved symptoms compared to placebo when all studies were analyzed, that disappeared when only the quality studies were examined. Bran had no effect on symptoms. Psyllium (Metamucil® and a host of others) was effective when all studies were included, but not when the analysis was limited to quality studies. The "concentrated" fiber was ineffective. The percentage of adverse events for fiber and placebo was the same, about 1%-2%.
Antispasmodics accounted for 22 studies, 12 of which were quality ones. The drugs studied were alverine, cimetropium, dicycloverine (dicyclomine), hyoscine (scopolamine), mebeverine, otilonium, pinaverium, pirenzipine, prifinium, propinox, rociverine, and trimebutine. Only dicyclomine (Bentyl® and others) and scopolamine (Scopace®, Transderm Scop®, and others) are available in the United States. A closely related drug, hyoscyamine (Anaspaz®, Levsin®, Levbid®, and others) is also available. When all 22 trials were considered, antispasmodics were significantly better than placebo, and this did not change when the analysis was restricted to quality studies. Patients receiving antispasmodics were more likely to experience adverse side effects, 14% vs. 9%, when compared to patients receiving placebo.
Oil of peppermint was the subject of 4 studies with 3 studies considered quality ones. It was significantly better than placebo, whether considering all studies or only the quality ones. Five of 174 (3%) subjects suffered adverse side effects from peppermint; no adverse effects were reported for the 171 placebo subjects.
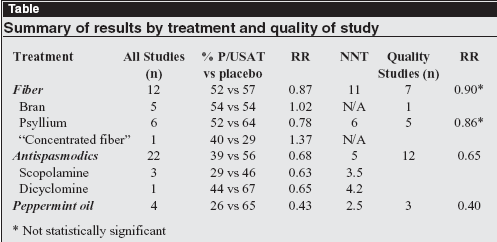 |
The table (above) summarizes the data for the active ingredients available in the United States.
Commentary
IBS "is a disorder characterized most commonly by cramping, abdominal pain, bloating, constipation, and diarrhea" that afflicts as many as 1 in 5 Americans.1 That puts it right up there with obesity and makes it more common than diabetes mellitus and heart disease. I find that disturbing, because when I think of my patient population, I can name a lot of patients with obesity, diabetes, or heart disease, but only a couple with IBS. That says much about my diligence in searching for the syndrome and my patients' willingness to disclose their symptoms. Its etiology is "multifactorial," code word for "we're not really sure." This is not surprising since the symptom complex includes both diarrhea and constipation. There is a concise primer on IBS available on the British Medical Journal web site (bmj.com).2 The American College of Gastroenterology recently updated its 2002 monograph on IBS.3 It was not impressed by the quality of the evidence for fiber, antispasmodics, and peppermint oil, but supported their use. Among its new recommendations is routine screening of patients with celiac sprue serology.
It wasn't too long ago that medications were marketed in the United States specifically for IBS. In particular, the serotonin receptor antagonists, Type 3 (alosetron [Lotronex®]) and Type 4 (tegaserod [Zelnorm®]), were sold to combat diarrhea- or constipation-predominant IBS, respectively, but now are on restricted access or withdrawn from the U.S. market, respectively. Other medications and modalities have been evaluated for IBS, including antidepressants4 and acupuncture,5 and were not found to be effective.
Of the 3 agents in this meta-analysis, peppermint oil provides the best combination of effectiveness and a low rate of adverse effects, and is available over the counter. Its mechanism of action appears to be reduction of colonic contractility by blocking calcium channels in smooth muscle. It should be taken as an enteric-coated capsule containing 0.2 or 0.4 mL of oil. Psyllium is only marginally effective, and the antispasmodics have a higher rate of adverse side effects (cholinergic, such as dry mouth or blurred vision). That particular order (peppermint oil, psyllium, antispasmodic) seems to be the best escalation of medications for IBS.
References
1. National Digestive Diseases Information Clearinghouse web site. Available at: http://digestive.niddk.nih.gov/ddiseases/pubs/ibs/. Accessed Dec. 14, 2008.
2. Agrawal A, Whorwell PJ. Irritable bowel syndrome: Diagnosis and management. BMJ 2006;332:280-283.
3. American College of Gastroenterology Task Force on IBS. An Evidence-based Systematic Review on the Management of Irritable Bowel Syndrome. Am J Gastroenterology 2009;104:S1-S35; doi:10.1038/ajg.2008.122. Available at: www.acg.gi.org/media/releases/ajg2008122a.pdf.
4. Quartero AO, et al. Bulking agents, antispasmodic and antidepressant medication for the treatment of irritable bowel syndrome. Cochrane Database Syst Rev 2005;(2): CD003460.
5. Lim B, et al. Acupuncture for treatment of irritable bowel syndrome. Cochrane Database Syst Rev 2006;(4):CD005111.
Peppermint oil, psyllium, and antispasmodics are all effective in the treatment of IBS.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
