Acute Appendicitis Diagnosis and Treatment in 2009: Part II
Acute Appendicitis Diagnosis and Treatment in 2009: Part II
This second part concludes our discussion of acute appendicitis, focusing on three patient populations where the diagnosis can be challenging and imaging modalities are commonly used: the elderly, children, and pregnant women. In addition, this article will discuss the use of pre-operative antibiotics and the evolving concept of delaying appendectomy until the operating room is available during day-shift.
J. Stephan Stapczynski, MD, FACEP, Editor
Special Populations
Elderly. Appendicitis in the elderly can be difficult to diagnose because many patients present atypically.1,2 The presence of fever and elevated white blood count are not reliably present in the elderly, and many patients may have minimal or no right lower quadrant pain. About one-third to one-half of elderly patients are misdiagnosed initially, and half have perforation at time of operation.1 Diverticulitis and bowel obstruction are common misdiagnoses in this age group. CT can be used more liberally in the elderly with abdominal pain, as the diagnostic yield is high and the risk of radiation-induced malignancy is less due to the time required to mainifest such complications.
Children. Acute appendicitis is the most common surgical emergency in childhood, responsible for 10% of all children admitted to the hospital.3 The classic clinical picture of acute appendicitis has been widely known for more than 110 years. However, it has been mostly described in adult patients. The pathophysiology of appendicitis in children differs from that of adults because of the changing anatomical location and shape of the appendix throughout childhood. Neonates develop appendicitis infrequently because they have a funnel-shaped appendix.4 Around age 1-2 years, the appendix assumes the typical tubular adult shape and becomes more susceptible to appendicitis.5,6 Lymphoid follicle hyperplasia and follicular size gradually increase throughout childhood and peak in the adolescent years, corresponding to the period of highest incidence of appendicitis.5,6
Children are at increased risk of misdiagnosis due to atypical signs and symptoms. Many children present with clinical findings that are considered not classic for appendicitis. In one study, more than 50% of patients with appendicitis had no fever, negative Rosving's sign, and no rebound tenderness. Almost half had abrupt onset of pain or lack of pain migration.7 In children younger than 3 years of age, diarrhea is reported in as many as 41% of cases of appendicitis and is more common in this age group than in older children. Additionally, local abdominal tenderness is not as frequent as in older children.8,9
In the past, ultrasound has been the radiologic test of choice to assist in the diagnosis of appendicitis in children. Ultrasound, however, is operator dependent, and wide ranges of sensitivity and specificity have been reported in the broad pediatric age population.10-12 One pediatric subpopulation where ultrasound may be more useful is in younger children. Chang et al studied the utility of ultrasound in diagnosing appendicitis in children age 3 and younger. They reported a positive predictive value of 93% and a negative predictive value of 93%.13
CT has been shown to be highly sensitive and specific for diagnosing acute appendicitis in children. Reported sensitivities for CT range from 87-100% and specificity from 89-98%.14-19 CT has a higher sensitivity for the diagnosis of appendicitis in children than ultrasound.20,21 There is also evidence that CT improves outcomes as well. Reduced negative appendectomy rates21,22 and reduced length of hospitalization17 have been reported. However, due to the radiation risk, attempts should be made to minimize CT use in children whenever possible.
US and CT can be used as complementary studies for the evaluation of acute appendicitis in children. One approach is to use risk stratification to determine the initial imaging study and the need for alternative studies. Garcia-Pena et al retrospectively analyzed this risk stratification in a cohort of children with equivocal presentations for appendicitis who were divided into low-, medium-, and high-risk groups for appendicitis. Three different imaging guidelines were utilized. Low risk was defined as neutrophils < 67%, bands < 5%, and no guarding on abdominal examination. High risk was defined as neutrophils > 67%, white blood cell count >10,000/mm3, guarding, and abdominal pain > 13 hours. Imaging guideline number one (the standard practice at the authors' institution) dictated that all children with equivocal signs and symptoms for acute appendicitis have ultrasound first. If the ultrasound is positive, the child proceeds to appendectomy. If the ultrasound is negative, the child undergoes CT. Under guideline number two, low-risk children undergo ultrasound and, if negative, are discharged from the hospital. High-risk children undergo CT, and medium-risk children undergo ultrasound followed by CT. Under the third guideline, low-risk children undergo no imaging and are admitted for observation. High-risk children proceed directly to appendectomy without imaging studies. Medium-risk children undergo ultrasound followed by CT. Of the total 958 children studied, 61% had appendicitis. Two hundred twenty-five patients were classified as high-risk. Under imaging guideline 1, there were 22 negative appendectomies, 35 missed or delayed diagnoses, and 958 ultrasounds and 673 CT scans performed. Under guideline 2, there would have been 23 negative appendectomies, 36 missed or delayed diagnoses, and 733 ultrasounds and 637 CT scans performed. Under guideline 3, there would have been 36 negative appendectomies, 37 missed or delayed diagnoses, and 590 ultrasounds and 412 CT scans performed. The authors concluded that selective imaging guidelines can reduce the number of radiographic studies performed with a minimal diminution of accuracy in the diagnosis of pediatric appendicitis.23
Children with a low likelihood of appendicitis may be spared the expense and risk of a more invasive and costly workup for appendicitis and may be sent home safely with careful followup. The use of the pediatric appendicitis scale can help determine which patients can be considered low-risk. However, in particularly young children in whom the diagnosis of appendicitis is difficult to make, clinicians will continue to rely on radiologic studies and surgical evaluation to assess the potential appendicitis patient since the clinical examination alone cannot definitively confirm this diagnosis.24
Women. Non-pregnant female patients with acute abdominal pain usually require a lengthier and more extensive evaluation because of the different nature of their anatomy and pathologic processes. With the reproductive tract's adjacent location to the abdominal cavity, referred pain from multiple spaces and organs can be referred to the right lower quadrant. CT often is necessary in these patients for accurate diagnosis. Pregnancy further complicates the search for a diagnosis.
Pregnancy. Acute appendicitis complicates approximately 1 in 1500 pregnancies and is one of the leading indications for surgery during pregnancy.25 Accurate diagnosis is important as delay in diagnosis leads to a higher rate of maternal and fetal complications.26,27
The clinical diagnosis of appendicitis in pregnancy is challenging, since some of the hallmarks of appendicitis, such as nausea, vomiting, and abdominal pain often are present in pregnant patients without appendicitis.26-28 Anorexia, nausea, vomiting, and initial periumbilical pain are similar in the pregnant and non-pregnant state. Gross peritoneal signs with rebound and guarding are not normal in pregnancy, although the laxity of the anterior abdominal wall and enlarged uterus may delay or diminish these signs.
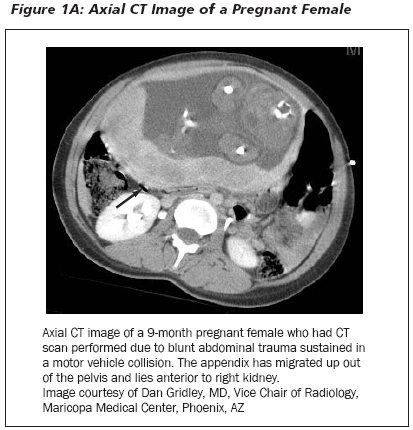
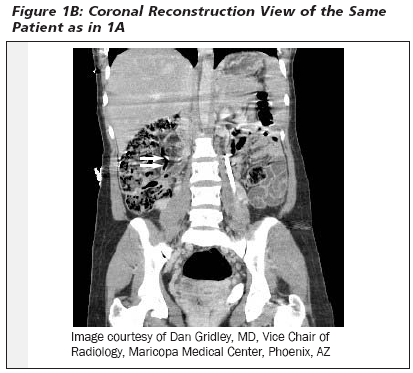
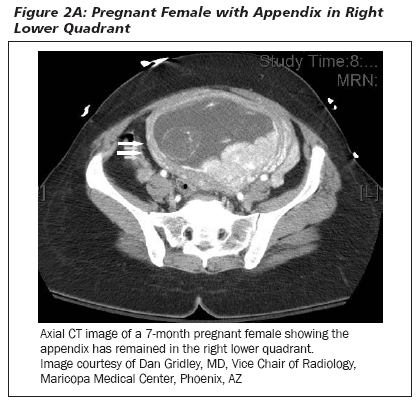
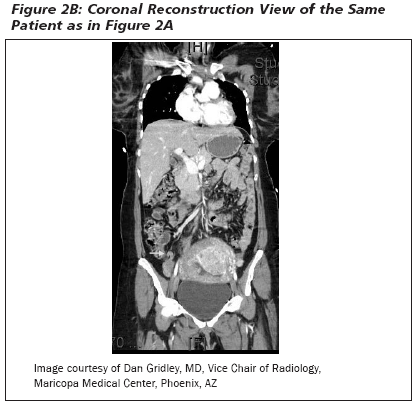
The physical examination may be unreliable and the location of the appendix variable, depending on the size of the gravid uterus, which may reposition the appendix within the peritoneal cavity.29,30 (See Figures 1 A-B and 2 A-B.) Early during pregnancy, peritoneal irritation develops in the right lower quadrant, but after the fifth month of gestation, the appediceal position and site of pain are shifted superiorly about the right iliac crest, and the appendix tip is rotated medially by the gravid uterus. The tenderness also becomes less localized as distention of the abdomen lifts the peritoneum away from the inflamed appendix and cecum.27 The location of the appendix traditionally has been described as rising in the peritoneal cavity as the uterus enlarges, beginning at 12 weeks and reaching the iliac crest by 24 weeks.31,32 More recently, this dogma has been challenged by a prospective study comparing the location of the appendix in women undergoing cesarean at term, in pregnant women undergoing appendectomy, and in non-pregnant women undergoing appendectomy, with no difference in appendix location among the three groups.33
 |
 |
 |
 |
The usefulness of ultrasound for diagnosing acute appendicitis in many pregnant patients is limited, as the appendix may be displaced from its expected location. The enlarged uterus may make graded compression difficult. If an abnormal appendix is seen on ultrasound, the specificity of sonography is high; however, if the appendix is not visualized, other imaging is needed.
MRI has been touted as a useful imaging modality for the detection of acute appendicitis in pregnant patients because it eliminates radiation exposure, avoids the operator dependency of ultrasound, facilitates alternative diagnoses, and is considered safe for use in pregnancy.34 The use of ultrasound is limited to less than 35 weeks gestation, as the graded compression technique is not able to visualize the appendix clearly and is less useful later in pregnancy.35 MRI can identify not only appendicitis, but also ovarian disease, colitis, abscesses, pyelonephritis, and fibroid degneration.36 A study by Pedrosa et al evaluated 51 pregnant patients with clinical suspicion of acute appendicitis who subsequently had MRI. The sensitivity of MRI in this study was 100%, and the specificity was 93.6%.37
Israel et al published a small, retrospective study of 33 pregnant patients with suspected appendicitis, each of whom had an ultrasound and MRI. Appendicitis can be excluded only by graded compression ultrasound when a normal appendix is identified. In their study, in 88% of the ultrasound examinations, the appendix could not be identified, including three patients with pathologically proven appendicitis.38 Similar results were seen by Pedrosa39 and Cobben.40 When the appendix was seen on MRI, 100% sensitivity, specificity, and positive and negative predictive value were achieved. When the appendix was seen on ultrasound, the sensitivity was 50%, specificity was 100%, PPV 100%, and NPV 66%.41
CT may be done in pregnancy if necessary. Fetal exposure from abdominal CT in the first trimester may double the likelihood of childhood cancer from 1/600 to 1/300.42 Information from atomic bomb survivors shows the greatest risk to the fetus is exposure at 8-15 weeks gestation,43 with radiation-induced mental retardation the highest specific potential danger. No single diagnostic radiographic procedure results in radiation exposure to a degree that would threaten the wellbeing of the developing fetus, according to the American College of Radiology.44
Pelvic Inflammatory Disease vs. Appendicitis. Part of the diagnostic dilemma of evaluating women of child-bearing age is differentiating appendicitis from pelvic pathology such as pelvic inflammatory disease (PID). Both conditions may present with abdominal/pelvic pain, nausea, vomiting, and fever. Vaginal discharge is not always present in PID. While the pain of appendicitis often begins in the epigrastrium or mid-abdomen, the pain from PID typically is in the lower abdomen. The afferent sensory nerves from the adnexae originate from T12 to L2 and L5 to S1-3. This results in the pain being confined to the lower abdomen.45 Morishita et al developed a clinical prediction rule to help distinguish the two conditions. The rule consists of 3 clinical criteria and can differentiate between appendicitis and PID with 99% sensitivity and 95% negative predictive value when a patient is classified as low risk for appendicitis by the following factors: no migration of pain; presence of bilateral abdominal tenderness; and no nausea and vomiting. Although these 3 factors cannot rule out appendicitis as a single criterion, the combination of these 3 findings could be used as a quick guide for clinical decision making.46
Inflammatory Markers. "What's the white count?" Medical mythology would have us believe that patients with presumed appendicitis need to have an elevated white blood cell count. Cardell et al demonstrated that a total WBC of > 10,000 cells/mm3 has a sensitivity of 76% and a specificity of 52% for appendicitis. The positive predictive value was 42%, and the negative predictive value was 82%. These data suggest that the total WBC count has insufficient sensitivity and specificity to be of clinical value in the diagnosis of appendicitis.47
Other inflammatory markers that have been investigated include C reactive protein (CRP), leukocyte elastase activity, D-lactate, phospholipase A2, and interleukin-6. Deballon et al prospectively studied 134 patients with right lower quadrant pain who had complete blood counts and CRP levels drawn. Normal range for CRP was < 6 mg/L; normal for WBC was considered 4500-9600/mm3, and normal for granulocytes was < 75%. The negative appendectomy rate in this study was 15%, while 66% of patients had appendicitis. Mean levels of CRP, WBC, and granulocytes were all significantly higher in patients with surgical diseases. CRP had the highest diagnostic accuracy of a single marker. However, when CRP was combined with WBC, it led to a diagnostic accuracy of 87% (p < 0.0005). WBC and CRP had better diagnostic accuracy in patients with greater than 12 hours of pain. The positive predictive value when CRP and WBC were elevated was 93%, while the negative predictive value if both were normal was 92%.48 However, no threshold value for WBC or CRP will reliably diagnose or exclude appendicitis. Testing of the white blood cell count, neutrophil count, and C-reactive protein are more effective in supporting a clinical diagnosis of acute appendicitis in patients with typical clinical features than in excluding the diagnosis.49
Differential Diagnosis
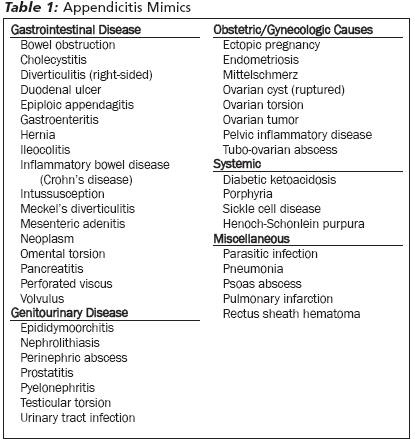
The differential diagnosis for appendicitis is extensive. Various types of gastrointestinal, genitourinary, obstetric/gynecologic, systemic, and other conditions can mimic the clinical presentation of appendicitis. (See Table 1.)
 |
In children, intussusception, Meckel's diverticulitis, gastroenteritis, and mesenteric lymphadenitis may be mistaken for appendicitis. Children with intussusception commonly present with vomiting and colicky abdominal pain interspersed with pain-free periods.50-52 Rectal bleeding and a palpable right-sided abdominal mass may be noted on examination.51,52 However, peritoneal signs usually are absent.50 CT may demonstrate a segment of bowel that has telescoped in on itself, a mass, and/or a proximal bowel obstruction.13 Plain abdominal radiographs can be used to rule out intussusception as well.
With Meckel's diverticulitis, children typically present with periumbilical pain and tenderness.50 CT may reveal inflammation adjacent to a loop of small bowel (Meckel's diverticuli are usually located about 60 cm from the ileocecal valve) and occasionally an obstructing fecalith.51,53
Gastroenteritis is a common misdiagnosis in both children and adults with appendicitis. Patients with acute gastroenteritis present with varying degrees of nausea, vomiting, and diarrhea that typically start before the onset of abdominal pain. Fever also may be present.52,54 However, these patients usually do not have focal abdominal tenderness or peritoneal findings on examination.50 In contrast, patients with appendicitis often have abdominal pain that precedes the onset of other gastrointestinal symptoms such as vomiting. In addition, diarrhea is less common in patients with appendicitis.
Mesenteric adenitis may occur following a viral infection.52,53 Its clinical presentation may be nearly indistinguishable from that of appendicitis. On CT, patients with mesenteric lymphadenitis have enlarged mesenteric lymph nodes in the right lower quadrant without any other inflammatory changes except possibly mild thickening of the terminal ileum. The appendix, if visualized, is normal.13,53
In older patients, Crohn's disease and right-sided diverticulitis are also considerations. Patients with an acute exacerbation of Crohn's disease may present with right lower quadrant pain, fever, and leukocytosis.13 CT may reveal mural stratification, skip lesions, thickened bowel wall (especially of the terminal ileum and cecum), creeping fat around affected bowel, and mesenteric fat stranding.53,55 The center of inflammation should be away from the appendix.13 Complications such as sinus tracts, fistulae, and abscesses also may be apparent on CT. Patients with diverticulitis may present with right lower quadrant pain if they have redundant sigmoid colon or right-sided diverticula.56 Associated signs and symptoms can include fever, nausea, vomiting, anorexia, and a palpable abdominal mass.56,57 The area of tenderness with diverticulitis may be larger than the classic McBurney's point of appendicitis.50 Typical CT findings include focal asymmetric thickening of the cecal wall, adjacent fat stranding, diverticula, and a normal appendix.13
Another important consideration in the differential diagnosis is pyelonephritis. Patients with pyelonephritis may present with right-sided abdominal pain, fever, leukocytosis, and pyuria.50 Some actually may have peritoneal signs on examination. CT commonly demonstrates low attenuation streaks and wedges in the renal parenchyma. Hydronephrosis and perinephric fat stranding also may be seen.58
The urinalysis can be deceptively benign in some cases of pyelonephritis, and this diagnosis may be found incidentally on CT obtained in patients with concerning abdominal examinations and unremarkable urinalyses.
In women presenting with right lower quadrant pain, ectopic pregnancy, pelvic inflammatory disease, ovarian torsion, and ruptured ovarian cysts also should be considered. The classic presentation of an ectopic pregnancy includes amenorrhea, abdominal pain, and vaginal bleeding. Although vaginal bleeding may be absent, abdominal pain is almost always present.59 Physical examination may reveal abdominal tenderness, a slightly enlarged uterus, cervical motion tenderness, and/or an adnexal mass.58 Ectopic pregnancy should be considered in the differential of any pregnant woman with right lower quadrant pain. Ultrasound may be helpful in ruling in (showing an adnexal mass, especially with a fetal pole) or ruling out (showing an intrauterine pregnancy) ectopic pregnancy or ovarian torsion (normal Doppler flow).
Pelvic inflammatory disease (PID) can be difficult to distinguish from appendicitis as patients with both can present with lower abdominal pain, fever, and leukocytosis. Abnormal cervical or vaginal discharge (mucopurulent) may also suggest PID.60,61
Patients with ovarian torsion may present with severe abdominal pain and nausea and vomiting. Unlike with appendicitis, the pain of a torsed ovary classically is abrupt in onset and described as sharp in nature. If intermittent torsion and spontaneous reduction occur, the pain may be more colicky.59 A tender adnexal mass may be appreciated on examination. CT findings may include an ovarian mass and adjacent fat stranding.13 However, if ovarian torsion is suspected, a pelvic ultrasound with Doppler is the preferred imaging study. With a ruptured ovarian cyst, women may present with peritoneal signs similar to patients with perforated appendicitis. If significant bleeding occurs, abdominal distention and hypotension may occur.59 CT in these patients should reveal an ovarian cyst, inflammation in the adnexal area, free fluid in the pelvis, and a normal appendix.13 Ultrasound is a useful imaging modality in these patients.
Complications
Perforation is the most common complication of appendicitis, occurring in about 15-20% of all patients, but perforation is significantly increased in the elderly and young children, in whom the rate may be as high as 50-97%.62-65 This is usually due to a delay in diagnosis.64,65 In children, there appears to be an inverse relationship between age and risk for perforation. Patients at the extremes of age are at increased risk for perforation. Overall, children have a 23-88% incidence of perforation.62,63,66 In this population, there appears to be an inverse relationship between age and risk for perforation.67 In children 10-17 years old, the rate of perforation is 10-20%.24,68 In those younger than 4 years old, it rises as high as 80-100%.6,24,69 Similarly, the elderly have a 29-70% incidence.62,63,67,70-72 Misdiagnosis and delayed diagnosis are common in both of these age groups due to atypical clinical presentations as well as limitations in obtaining a clear history and physicial exam, and may contribute to the higher perforation rates.62
After the appendix ruptures, patients may present with more severe or more generalized pain, higher temperature, and higher WBC counts with prominent left shifts.68 According to a meta-analysis by Andersson, a high WBC ( > 15 x 109/L) and granulocyte count ( > 9 x 109/L) and an elevated CRP level (> 10 mg/L) had positive likelihood ratios of 7.2, 4.16, and 4.24, respectively, making them relatively strong predictors for perforation. In contrast, a WBC count < 10 x 109/L, a granulocyte count < 7 x 109/L, and CRP < 10 mg/L had negative likelihood ratios of 0.11-0.20, making perforation unlikely in patients with these laboratory values.73
Another important risk factor for appendiceal rupture is the time from onset of symptoms to treatment.74 Bickell et al. performed a retrospective chart review of 219 patients with appendicitis and found that the risk of perforation was negligible within the first 36 hours after symptom onset (0-2%). However, for those with symptoms that were untreated for 36 hours or more, the risk rose to about 5% for each ensuing 12 hours without treatment.75 Inherent delay in obtaining CT did not lead to an increase in the perforation rate. Perforation tends to be dependent on a delay in the initial presentation to the hospital.76,77
Once appendiceal rupture occurs, it is associated with increased morbidity and mortality. In some studies, morbidity rose from 3% with uncomplicated appendicitis to as high as 60% after perforation.72,78 Perforation may result in a localized abscess, peritonitis, or sepsis.70,75 In the general population, the mortality for appropriately treated appendicitis is less than 1%.70-72 Appendiceal rupture has been associated with an 11-fold or greater increase in mortality.63,79 Some people consider perforation the single best predictor of mortality.70 Elderly patients with appendicitis also have a higher risk of death (4-15%) and account for half of deaths due to appendicitis.70-72,74,75
Management
Analgesia. Analgesia should not be withheld from patients for fear of masking a diagnosis. This practice dates prior to the development of the CT scan and has been debunked by multiple studies.80,81 Even Silen, the current author of Sir Zachary Cope's classic treatise on acute abdominal pain (first written in 1921), condemns withholding analgesia for patients who are in pain, even undifferentiated abdominal pain.80,82,83
What about the patient who has been given analgesia who subsequently has little or no abdominal pain when re-examined? One small study recently addressed this question. In study patients with pain at McBurney's point or a positive Murphy's sign, there was no misdiagnosis of appendicitis or cholecystitis when analgesia was given in the absence of imaging.83 Does administration of analgesia mandate imaging, a specific observation interval, or protocol incorporating both imaging and serial exams?80 Further research is needed to answer this question.
Antimicrobials. All patients should receive broad-spectrum antibiotics pre-operatively (1-3 doses), as their use has been shown to decrease the incidence of post-operative wound infection and intra-abdominal abscess formation.84
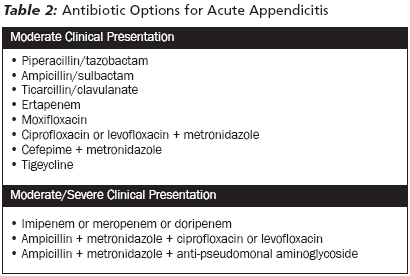
Unfortunately, there is no concensus among surgeons regarding antibiotic use in appendicitis. Some choose single agents, double agents, one-time dosing, and intra-operative dosing. (See Table 2.) There is no agreement on the length of treatment as well.85 Prospective cohort studies and randomized controlled trials are lacking, explaining why there is a poor agreement among institutions as to what constitutes optimal care.86
 |
Treatment. The timing and management of acute appendicitis has changed dramatically. The role of pre-operative imaging has extended beyond a diagnostic tool to become important in identifying those complicated cases that may be amenable to alternatives other than immediate operation, such as extended antibiotic therapy with or without percutaneous drainage of abscesses.38,87,88
In a survey of 344 pediatric surgeons, 75% indicated that a clinically stable child with suspected appendicitis could be operated on in an urgent (3-12 hours from presentation) rather than emergent manner.85 Twenty percent of these surgeons used imaging frequently, and 50% used imaging occasionally. When an imaging study is felt to be necessary in evaluating a child with possible appendicitis, a majority of respondents preferred CT to ultrasound (62% vs 30%).85
Laproscopic appendectomy is technically more difficult than open appendectomy, but in adults reduces wound infections, post-operative pain, and length of hospital stay, but may have an increased risk of intra-abdominal abscesses.89 Patients who have periappendiceal abscesses often are diagnosed preoperatively. These patients are best treated with nonoperative management and selective percutaneous drainage. Immediate operation in these patients results in higher complication rates and longer hospital stays.90,91
Acute appendicitis has long been considered a surgical emergency that requires emergent appendectomy. Recently, the concept of a surgical emergency has been challenged and a proposal has been advanced that appendectomy can wait up to 12 hours after diagnosis so that the procedure can be performed by fully rested and awake surgeons and support personnel during normal business hours without an increase in morbidity.92 While the data are only retrospective, there is no evidence that delaying appendectomy up to 12 hours after diagnosis increases morbidity.93,94 Some physicians and hospitals have devised protocols for patients to be held in the ED for observation, receive treatment with intravenous fluid, analgesics, and antibiotics while awaiting call to the OR in the morning.
Disposition
Patients in whom the physician believes the likelihood of acute appendicitis is low can be discharged with strict precautions to return if their symptoms or pain worsens.
A 23-hour admission for observation is a feasible option for patients whose pain is poorly tolerated in the emergency department and for whom a working diagnosis has not been found. This disposition also is an option for patients, particularly children, who might have poor follow-up and in whom the physician suspects a diagnosis of early appendicitis. Clear discharge instructions are particularly important in patients who have had a CT scan that was read as normal or nondiagnostic. The patient should be advised of the limitations of this test and that early appendicitis still may be present.
For ED providers, it is their role (medico-legally as well as ethically) to inform families of children with symptoms of short duration who request a CT scan that: if we image too early, we may miss the diagnosis; and CT scans expose children to radiation and future cancer risk. This is a hard decision made on a case-by-case basis with family/referring doctor and should take into consideration the risk of missing a diagnosis, the physician's responsibility to "do no harm" by the patient, and the ability to ensure safe and timely follow-up.
Summary
Patients with possible appendicitis can be risk-stratified based on their clinical findings and divided into groups. Patients with a high probability of uncomplicated appendicitis should undergo surgery. Patients suspected of having an appendiceal abscess should have a CT (or MRI if pregnant). For patients with a low likelihood of having appendicitis, an alternate diagnosis should be sought. Patients with intermediate probability will require either a combination of laboratory testing and imaging or extended observation. Most low-risk patients can be discharged with 12-24 hour follow-up. For patients who require imaging, the authors recommend CT for all patient groups except pregnant women. Pregnant women should undergo an ultrasound of the abdomen and pelvis in an attempt to visualize the appendix and to evaluate the fetus and adenexae. If these studies are non-diagnostic, an MRI is a reasonable next step for pregnant women. If MRI is not available, re-examine the patient's abdomen. If clinical suspicion still exists at this point, consultations with surgery and gynecology should be obtained, and the patient should be admitted.
References
1. Lee JF, Leow CK, Lau WY. Appendicitis in the elderly. Aust N Z J Surg 2000;70: 593-596
2. Gürleyik G, Gürleyik E. Age-related clinical features in older patients with acute appendicitis. Eur J Emerg Med 2003;10:200-203.
3. Reynolds SZ, Jaffe DM. Diagnosing abdominal pain in a pediatric emergency department. Ped Emerg Care 1992;8: 126-128.
4. Karaman A, Cavusoglu YH, Karaman I, et al. Seven cases of neonatal appendicitis with a review of the English language literature of the last century. Pediatr Surg Int 2003; 19:707-709.
5. Addiss DG, Shaffer N, Fowler BS, et al. The epidemiology of appendicitis and appendectomy in the United States. Am J Epidemiol 1990;132:910-925.
6. Rothrock SG, Skeoch G, Rush JJ, et al. Clinical features of misdiagnosed appendicitis in children. Ann Emerg Med 1991;20: 45-50.
7. Becker T, Kharbanda A, Bachur R. Atypical clinical features of pediatric appendicitis. J Acad EM 2007;14:124-129.
8. Horwitz JR, Gursoy M, Jaksic T, et al. Importance of diarrhea as a presenting symptom of appendicits in very young children. Am J Surg 1997;173:80-82.
9. Huang CB, Yu HR, Hung GC. Clinical features and outcome of appendicitis in children younger than two years of age. Chang Gung Med J 2000;13:28-32.
10. Puyalert JB, Rutgers PH, Lalisang RI, et al. A prospective study of ultrasonography in the diagnosis of appendicitis. N Engl J Med 1987;317:666-669.
11. Sivit CJ, Newman KD, Boenning BA, et al. Appendicitis: Usefulness of ultrasound in diagnosis in a pediatric population. Radiology 1992;185:549-552.
12. Siegel MJ, Carel C, Surratt S. Ultrasonography of acute abdominal pain in children. JAMA 1991;266:1987-1989.
13. Yu J, Fulcher AS, Turner MA, et al. Helical CT evaluation of acute right lower quadrant pain: Part II, Uncommon mimics of appendicitis. AJR Am J Roentgenol 2005;184:1143-1149.
14. Garcia-Pena BM, Taylor GA, Lund DP, et al. Effect of CT on patient management and costs in children with suspected appendicitis. Pediatrics 1999;104:440-446.
15. Sivit CJ, Applegate KE, Berlin SC, et al. Evaluation of suspected appendicitis in children and young adults: Helical CT. Radiology 2000;216:430-433.
16. Karakas SP, Guelfuat M, Leondias JC, et al. Acute appendicitis in children: comparision of clinical diagnosis with ultrasound and CT imaging. Pediatr Radiol 2000;30: 94-98.
17. Garcia-Pena BM, Taylor GA, Fishman SJ, et al. Costs and effectiveness of ultrasonography and limited CT for diagnosing appendicitis in children. Pediatrics 2000; 106:672-675.
18. Sivit CJ, Siegel MJ, Applegate KE, et al. When appendicitis is suspected in children. Radiographics 2001;21:247-262.
19. Lowe LH, Penney MW, Stein SM, et al. Unenhanced limited CT of the abdomen in the diagnosis of appendicitis in children: Comparision with sonography. AJR 2001; 176:31-35.
20. Sivit CJ, Applegate KE, Stallion A, et al. Imaging evaluation of suspected appendicitis in a pediatric population: effectiveness of sonography vs CT. AJR Am J Roentgenol 2000;175:977-980.
21. Garcia-Pena BM, Mandl KD, Kraus SJ, et al. Ultrasonography and limited CT in the diagnosis and management of appendicitis in children. JAMA 1999;282:1041-1046.
22. Applegate KE, Sivit CJ, Salvator AE, et al. The impact of cross-sectional imaging on negative appendectomy and perforation rates in children. Radiology 2001;103-107.
23. Garcia-Pena BM, Cook EF, Mandl KD. Selective imaging strategies for the diagnosis of appendicitis in children. Pediatics 2004;113(1 Pt 1):24-28.
24. Bundy DG, Byerley JS, Liles EA, et al. Does this child have appendicitis? JAMA 2007;298:438-451.
25. Wittich AC, DeSantis RA, Lockrow EG. Appendicitis during pregnancy: A survey of two army medical activities. Mil Med 1999;164:671-674.
26. Mourad J, Elliot JP, Erickson L, et al. Appendicitis in pregnancy: New information that contradicts long-held clinical beliefs. Am J Obstet Gynecol 2000; 182:1027-1029.
27. Stone K. Acute abdominal emergencies associated with pregnancy. Clin Obstet Gynecol 2002;45:553-561.
28. Birchard KR, Brown MA, Hyslop WB, et al. MRI of acute abdominal and pelvic pain in pregnant patients. AJR Am J Roentgenol 2005;184:452-458.
29. Owings MF, Kozak LJ. Ambulatory and Inpatient Procedures in the U.S., 1996. Vital and Health Statistics. Series 13. No. 139. Hyattsville, MD: National Center for Health Statistics, November 1998; p. 26 (DHHS publication no. {PHS} 2001-12500-0357.
30. Marudanayagam R, Williams GT, Rees BI. Review of the pathological results of 2660 appendiectomy specimens. J Gastroenterol 2006;41:745-749.
31. Baer J, Reis R, Arens R. Appendicitis in pregnancy with changes in position and axis of the normal appendix in pregnancy. JAMA 1932;98:1359-1363.
32. Oto A, Srinivisian PN, Ernst RD, et al. Revisiting MRI for appendix location during pregnancy. AJR Am J Roentgenol 2006;186: 883-887.
33. Hodjati H, Kazerooni T. Location of the appendix in the gravid patient: A re-evaluation of the established concept. Int J Gynecol Obstet 2003;81:245-247.
34. Shellock FG, Crues JV. MR Procedures: Biologic effects, safety and patient care. Radiology 2004;232:635-652.
35. Lim HK, Bae SH, Seo GS. Diagnosis of acute appendicitis in pregnant women: Value of sonography. AJR Am J Roentgenol 1992;159:539-542.
36. Singh A, Danrad R, Hahn PF, et al. MR imaging of the acute abdomen and pelvis: Acute appendicitis and beyond. Radiographics 2007;27:1419-1431.
37. Pedrosa I, Levine D, Eyrazzadeh AD, et al. MR imaging of acute appendicitis in pregnancy. Radiology 2006;238:891-899.
38. Oliak D, Yamin D, Udani VM, et al. Nonoperative management of perforated appendicitis without periappendiceal mass. Am J Surg 2000;179:177.
39. Pedrosa I, Levine D, Eyazzadeh AD, et al. MR imaging evaluation of acute appendicitis in pregnancy. Radiology 2006;238: 891-899.
40. Cobben LP, Groot I, Haans L, et al. MRI for clinically suspected appendicitis during pregnancy. AJR Am J Roentgenol 2004; 183:671-675.
41. Israel GM, Malguria N, McCarthy S. et al. MRI vs. ultrasound for suspected appendicitis during pregnancy. J Magn Reson Imag 2008;28:428-433.
42. Hurwitz LM, Yoshizumi T, Reiman RE, et al. Radiation dose to the fetus from body MDCT during early gestation. AJR Am J Roentgenol 2006;186:871-876.
43. Guidelines for diagnostic imaging during pregnancy: ACOG committee opinion number 299. American College of Obstetrics and Gynecologists 2004;104:647-651.
44. Gray JE. Safety of diagnostic radiology exposures. In: Janover ML, Linton WS, eds. American College of Radiology. Radiation Risk: A Primer. Reston (VA): ACR; 1996; p15-17.
45. Gray H, Standring S, Ellis H, et al. Gray's Anatomy: The Anatomical Basis of Clinical Practice. 39th ed. Edinburgh: Elsevier Churchill Livingstone; 2005.
46. Morishita K, Gushimiyagi M, Hashiguchi M, et al. Clinical predicition rule to distinguish pelvic inflammatory disease from acute appendicitis in women of childbearing age. Am J Emerg Med 2007;25: 152-157.
47. Cardall T, Glasser J, Guss DA. Clinical value of the total WBC count and the temperature in the evaluation of patients with suspected appendicitis. Acad Emerg Med 2004;11:1021-1027.
48. Ortega-Deballon P, Ruiz de Adara-Belbel J, Hernandez-Matias A, et al. Usefulness of laboratory data in the management of right iliac fossa pain in adults. ASCRS 2008;51: 1093-1099.
49. Birchley D. Patients with clinical acute appendicitis should have pre-operative full blood count and C-reactive protein assays. Ann R Coll Surg Engl 2006;88:27-32.
50. Maa J, Kirkwood KS. Ch. 49 The Appendix. In: Townsend CM, Beauchamp RD, Evers BM, et al. Sabiston Textbook of Surgery, 18th ed. Saunders: Philadelphia. 2008
51. Louie JP. Essential diagnosis of abdominal emergencies in the first year of life. Emerg Med Clin North Am 2007;25:1009-1040.
52. McCollough M, Sharieff GQ. Abdominal pain in children. Pediatr Clin North Am 2006;53:107-137.
53. Macari M, Balthazar E. The acute right lower quadrant: CT evaluation. Radiol Clin North Am 2003;41:1117-1136.
54. Ege G, Akman H, Sahin A, et al. Diagnostic value of unenhanced helical CT in adult patient with suspected acute appendicitis. Br J Radiol 2002;75:721-725.
55. Chang Y, Kong M, Hsia S, et al. Usefullness of ultrasonography in acute appendicitis in early childhood. J Ped Gastroenterol Nutr 2007;44:595-595.
56. Flasar MH, Goldberg E. Acute abdominal pain. Med Clin North Am 2006;90: 481-503.
57. Martinez JP, Mattu A. Abdominal pain in the elderly. Emerg Med Clin North Am 2006;24:371-388.
58. Ferentz KS, Nesbitt LS. Common problems and emergencies in the obstetric patient. Prim Care 2006;33:727-750.
59. Kamin RA, Nowicki TA, Courtney DS, et al. Pearls and pitfalls in the emergency department evaluation of abdominal pain. Emerg Med Clin North Am 2003;21:61-72.
60. Dixon JM, Elton RA, Rainey JB, et al. Rectal examination in patients with pain in the right lower quadrant of the abdomen. BMJ 1991;16:386-388.
61. Bergeron E, Richer B, Gharib R, et al. Appendicitis is a place for clinical judgment. Am J Surg 1999;177:460-462.
62. Birnbaum BA, Wilson SR. Appendicitis at the millenium. Radiology 2000;215: 337-348.
63. Rybkin AV, Thoeni RF. Current concepts in imaging of appendicitis. Radiol Clin North Am 2007;45:411-422.
64. Braveman P, Schaaf VM, Egerter S, et al. Insurance-related differences in the risk of ruptured appendix. N Engl J Med 1994; 82:166-169.
65. Grosfeld JL, Weinberger M, Clatworthy HW Jr. Acute appendicitis in the first two years of life. J Pediatr Surg 1973;8: 285-293.
66. Brennan GD. Pediatric appendicitis: Pathophysiology and appropriate use of diagnostic imaging. CJEM 2006;8: 425-432.
67. Graffeo CS, Counselman FL. Appendicitis. Emerg Med Clin North Am 1996;14: 653-671.
68. Rothrock SG, Pagane J. Acute appendicitis in children: Emergency department diagnosis and management. Ann Emerg Med 2000;36:39-51.
69. Wagner JM, McKinney WP, Carpenter JL. Does this patient have appendicitis? JAMA 1996;276:1589-1594.
70. Bobrow BJ, Mohr J, Pollack CV Jr. An unusual complication of missed appendicitis. J Emerg Med 1996;14:719-722.
71. Martinez JP, Mattu A. Abdominal pain in the elderly. Emerg Med Clin North Am 2006;24:371-388.
72. Kraemer M, Franke C, Ohmann, et al. Acute appendicitis in late adulthood: Incidence, presentation, and outcome. Results of a prospective multicenter acute abdominal pain study and a review of the literature. Langenbeck's Arch Surg 2000;385:470-481.
73. Andersson REB. Meta-analysis of the Clinical and laboratory diagnosis of appendicitis. Br J Surg 2004;91:28-37.
74. Storm-Dickerson TL, Horattas MC. What have we learned over the past 20 years about appendicitis in the elderly? Am J Surg 2003;185:198-201.
75. Bickell NA, Aufses AH, Rojas M, et al. How time affects the risk of rupture in appendicitis. J Am Coll Surg 2006; 202:401-406.
76. Rao PM, Rhea JT, Rattner DW, et al. Introduction of appendiceal CT: Impact on negative appendectomy and perforation rates. Radiology 2002;225:131-136.
77. McDonald GP, Pendarvis DP, Wilmoth R, et al. Influence of pre-operative CT on patients undergoing appendectomy. Am J Surg 2001;67:1017-1021.
78. Henry MC, Walker A, Silvermann BL, et al. Risk factors for the development of abdominal abscess following operation for perforated appendicitis in children. Arch Surg 2007;142:236-241.
79. Dominguez EP, Sweeney JF, Choi YU. Diagnosis and management of diverticulitis and appendicitis. Gastroenterol Clin North Am 2006;35:367-391.
80. Knopp RK, Dries D. Analgesia in acute abdominal pain: What's next? Ann Emerg Med 2006;48:161-163.
81. Gallagher EJ, Esses D, Lee C, et al. Randomized clinical trial of morphine in acute abdominal pain. Ann Emerg Med 2006;48:150-160.
82. Silen W. Cope's Early Diagnosis of the Acute Abdomen. 21st edition. London: Oxford University Press; 2005.
83. Thomas SH, Silen W, Cheema F, et al. Effects of morphine analgesia on diagnostic accuracy in emergency department patients with abdominal pain: A prospective randomized trial. J Am Coll Surg 2003; 196:18-31.
84. Anderson BR, Kallehave FI, Anderson HK. Antibiotics vs placebo for prevention of post-operative infection after appendectomy. Cochrane Database Syst Rev 2005;(3): CD001439.
85. Muehlstedt SG, Pham TQ, Schmeling DJ. The management of pediatric appendicitis: A survey of North American pediatric surgeons. J Ped Surg 2004;39:875-879.
86. Newman K, Ponsky T, Kittle K, et al. Appendicitis 2000: Variability in practice, outcomes and resource utilization at 30 pediatric hospitals. J Pediatr Surg 2003;38:372-379.
87. Gillick J, Velaydham M, Puri P. Conservative management of appendiceal mass in children. Br J Surg 2001;88:1539.
88. Janik JS, Ein SH, Shandling B, et al. Nonsurgical management of appendiceal mass in late presenting children. J Pediatr Surg 1980;15:574.
89. Sauerland S, Leferring R, Neugebauer EA. Laproscopic versus open surgery for suspected appendicitis. Cochrane Database Syst Rev 2004;(4):CD0001546.
90. Oliak D, Yamini D, Udani VM, et al. Initial non-operative management for periappendiceal abscess. Dis Colon Rectum 2001; 44:936-941.
92. Brown C, Abrishami M, Miller M, et al. Appendiceal abscess: Immediate operation or percutaneous drainage. Am Surg 2003;69:829-833.
92. Stahlfeld K, Hower J, Homitsky S, Madden J. Is acute appendicitis a surgical emergency? Am Surg 2007;73:626-629.
93. Ditillo MF, Dziura JD, Rabinovici R. Is it safe to delay appendectomy in adults with acute appendicitis? Ann Surg 2006;244: 656-660.
94. Clyde C, Bax T, Merg A, et al. Timing of intervention does not affect outcome in acute appendicitis in a large community practice. Am J Surg 2008;195:590-592
This second part concludes our discussion of acute appendicitis, focusing on three patient populations where the diagnosis can be challenging and imaging modalities are commonly used: the elderly, children, and pregnant women.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
