ECG Review: Acute Stroke and More
ECG Review
Acute Stroke and More
By Ken Grauer, MD, Professor, Department of Community Health and Family Medicine, University of Florida. Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
 |
Clinical Scenario
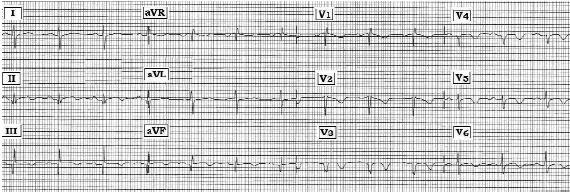
The ECG shown above was obtained from a 60-year-old woman who presented with an acute stroke. Is her ECG consistent with this diagnosis, and/or suggestive of something more?
Interpretation
Given the multiple findings seen on this tracing, discussion is best served by initial detailed descriptive analysis. The rhythm is regular and sinus at a rate of about 80/min. The PR and QRS intervals are normal; however, the QT interval appears to be at least borderline prolonged. There is RAD (right axis deviation) with a predominant S wave in lead I. There is no evidence of atrial enlargement, and voltage for LVH (left ventricular hypertrophy) is lacking. The most interesting findings relate to assessment for Q-R-S-T changes. Q waves are seen in several leads in each of the inferior leads, and in the form of QS complexes in leads V3 and V4. R wave progression is unusual due to the rSr' pattern in leads V1 and V2, which is followed by loss of R with the QS complexes seen in leads V3,V4. A small r wave returns in lead V5, and it is only between V5-V6 that transition (when R wave amplitude exceeds S wave depth) finally occurs. ST segment coving with slight elevation and T wave inversion is seen in the inferior leads and across the precordium. S waves persist in leads V5,V6. Given the finding of an S wave in lead I as well, the rSr' pattern in lead V1 is consistent with IRBBB (incomplete right bundle branch block). ST-T wave depression is common and expected in leads V1,V2 with incomplete or complete RBBB, but ST segment coving and deep T wave inversion should not persist across the precordium with the conduction disturbances seen here.
In the absence of a prior tracing for comparison, it is difficult to know which findings are new, and how the ECG fits with the patient's overall presentation of acute stroke. Of obvious concern are the inferior lead findings of Q waves, ST segment coving with slight elevation, and T wave inversion. Even in the absence of reciprocal ST segment depression, the possibility of acute evolving inferior infarction accompanying the patient's acute stroke needs to be strongly considered. There are several possibilities that might explain the precordial lead findings. The diffuse precordial ST segment coving and T wave inversion could be ischemic and part of the acute coronary syndrome. Alternatively, acute CNS events are known to prolong the QT interval and produce various patterns of disturbing ST-T wave abnormalities that may sometimes closely simulate acute infarction. RVH (right ventricular hypertrophy) or at least right ventricular "strain" could be present given the RAD, IRBBB, persistent precordial S waves, and diffuse T wave inversion. If these findings were acute, the constellation of abnormalities seen here could be consistent with acute pulmonary embolus, which might also be an accompaniment of the patient's acute stroke. Alas, abnormal serum markers and serial follow-up tracings confirmed the simultaneous occurrence of acute myocardial infarction that occurred in association with acute stroke.
The ECG shown above was obtained from a 60-year-old woman who presented with an acute stroke. Is her ECG consistent with this diagnosis, and/or suggestive of something more?Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
