ECG Review: A "Run of VT"
ECG Review
A "Run of VT"
By Ken Grauer, MD, Professor, Department of Community Health and Family Medicine, University of Florida. Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
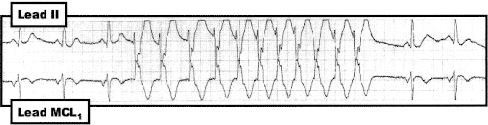 |
Figure: Simultaneously recorded leads II and MCL1 rhythm strip obtained from a middle-aged adult with heart disease. Despite this "run of VT", the patient remained alert, hemodynamically stable, and asymptomatic during tachycardia. |
Clinical Scenario:
Hospital-based physicians (especially those who work night shifts) will often be called about "a run of VT". When not immediately at the patient's bedside, what questions should you ask of the nurse who is caring for the patient? Apply this to assessment of the rhythm above.
Interpretation/Answer:
There are three principle issues to address when assessing a "run of VT (ventricular tachycardia)":
1. How is the patient during the run? Management decisions will vary greatly depending on whether the patient is symptomatic or not, and whether the patient is hemodynamically stable or about to go into cardiac arrest.
2. Is the run "real", and truly VT? What is the ventricular rate during the run, and is it sustained? Be sure that the rhythm is not rapidly-occurring artifact that may simulate VT. Realize that relatively slow ventricular rhythms (ie, less than 120/minute) represent AIVR (accelerated idioventricular rhythm) rather than true "VT". Hemodynamic compromise is far less likely with AIVR, and such rhythms rarely require specific antiarrhythmic treatment.
3. Clinically, what else is going on with the patient? A non-sustained ventricular rhythm that does not produce significant symptoms is preferentially treated by correction of underlying predisposing or exacerbating factors. These may include heart failure, ischemia, hypotension from a variety of causes, hypoxemia, acid-base and/or electrolyte disturbance (especially hypokalemia and hypomag-nesemia). Potentially arrhythmia-inducing pharmacologic agents such as sympathomimetics, cocaine, amphetamines, and alcohol should be stopped. The treatment approach will obviously be different for hemodynamically significant VT, in which case antiarrhythmic agents (ie, amiodarone) and/or acute cardioversion are indicated.
Applying these concepts to the rhythm in the Figure, the tracing begins with three beats of normal sinus rhythm. An 11-beat run of NSVT (non-sustained ventricular tachycardia) follows. The run is relatively slow and irregular at first ("warm-up" phenomenon), before speeding up to a more regular and rapid rate of 150/minute. This rhythm is clearly VT, as judged by QRS widening with a very different QRS morphology from sinus-conducted beats, lack of premature P wave prior to the onset of the run, and post-ectopic pause following the run. That said, the patient remained alert, asymptomatic and hemodynamically stable during the runergo, specific antiarrhythmic treatment was not needed. Instead, correction of hypoxemia and hypomagnesemia controlled the patient's ventricular ectopy and eliminated the runs of VT.
Simultaneously recorded leads II and MCL1 rhythm strip obtained from a middle-aged adult with heart disease. Despite this "run of VT", the patient remained alert, hemodynamically stable, and asymptomatic during tachycardia.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
