'There's Something in My Ear': Tools of the Trade for Foreign Body Entrapment and Retained Penetration
'There's Something in My Ear': Tools of the Trade for Foreign Body Entrapment and Retained Penetration
Authors: Jonathan I. Singer, MD, FAAP, FACEP, Associate Program Director for Emergency Medicine, Professor of Emergency Medicine and Pediatrics, Boonshoft School of Medicine, Wright State University, Dayton, Ohio; Debra Edwards, MD, Resident Physician, Emergency Medicine Residency, Boonshoft School of Medicine, Wright State University, Dayton, Ohio; Scott VanDeHoef, MD, Resident Physician, Emergency Medicine Residency, Boonshoft School of Medicine, Wright State University, Dayton, Ohio.
Peer Reviewer: Steven M. Winograd, MD, FACEP, Attending, Emergency Medicine, St. Joseph Medical Center, Yonkers, NY.
Entrapments and retained foreign bodies represent a common cause of emergency department (ED) visits. A majority of these pediatric presentations are easily assessed and managed by emergency physicians. However, even when accurately identified, this injury pattern may present therapeutic challenges.
The authors detail approaches to and therapeutic options for these minor trauma cases. They highlight the equipment needs (i.e., "tools of the trade") and treatment modalities for retained foreign bodies and entrapments.
- The Editor
Interaction with the Parent or Caregiver
Foreign body management may be challenging in the ED. The physician must be prepared with several options for potential removal and effectively communicate the options to the patient.
The physician should communicate to the caregiver the absolute and relative indications for immediate physician action, as well as the anticipated outcome if there is no attempt at retrieval initiated in the ED. The impact, if any, of delayed intervention should be communicated. When an immediate retrieval attempt is in the patient's best interest, the emergency physician should share his or her evidence-based knowledge of, and anecdotal experiences with, the same or similar encounters. Any involved anatomy should be communicated to the patient and/or caregiver, as well as any possible complications associated with the method. Initially indicate what will be done should the attempt fail (i.e., the chosen method will be repeated a certain number of times, or an advance will be made to another technique that may be more invasive). Clinicians should define, in advance, the number of planned efforts and obtain caregiver acceptance. Reassure the patient and caregiver that if failure occurs, assistance with any referrals will be available.
In addition to recruiting the parent into decisions concerning the retrieval methods and sequence of methods used, parental preferences for analgesia, sedation, local anesthesia, and restraint should be sought. The technique should be selected based on the child's personality and coping strategies and parental preferences.
As the parent is engaged in decision-making, the parent's emotional state, personality, and interaction with the child should be assessed. Parental desire to be present for the procedure should be determined. Parents who specifically request to be present during the procedure should be encouraged to participate, and should be forewarned of the sights and sounds associated with the projected procedure. Parental presence neither adversely influences the patient, nor increases the likelihood of a missed procedure.1 An eagerly participative and guided parent may help restrain, comfort, and support the child. Participating parents may speak encouragingly to the child, provide anxiolytic discussions, or simply provide physical contact.2 If a parent has an aversion to being present or the clinician senses that the parent would be intolerant of the visual or auditory stimuli, the parent's desire to leave should be supported. If a parent at the bedside proves to be excitatory to the patient, the procedure should be stopped; suggest to the parent that he or she may wish to leave the bedside-or perhaps the room-because the parent's presence may aggravate the child's basic response to the painful stimulus.
The outcome of these activities is that the parent has greater confidence in physician skills and is more knowledgeable of the risk/benefit of anticipated techniques. The parent is more likely to become a positive resource if informed, in advance, of any activity that has the capacity of frustration and complication. The likelihood is for a positive and lasting impression of their experience.
Interaction with the Patient
The physician should have four broad goals for interaction with the injured child, including: assessment of the emotional state, education of the patient, provision of pain relief if any is required, and monitoring of the circumstances.
The clinician should estimate the child's degree of anxiety and attempt to uncover any previous traumatic experiences. Both verbal and nonverbal clues should be noted to support the child's degree of anxiety. An innate or preexisting fear of physicians from prior painful procedures likely will inhibit a child's cooperation. If deemed appropriate, procedural sedation should be administered. The physician should exhibit patience, empathy, and tolerance in circumstances of higher anxiety.
Delivery of a truthful explanation to the patient of what is to occur is imperative, and the instruction should be age-appropriate. The patient should be informed of what equipment will be involved, and if possible, invited to see and touch the equipment that will be used. The physician should explain the likelihood of pain, the degree of pain, and the anticipated ameliorating influence of analgesia and/or sedation. If any pain is likely, the patient should receive appropriate analgesia. Both medical personnel and parents can effectively augment appropriate analgesia with comforting and empathetic delivery of touch and speech.
During the procedure, the physician should assess the state of the child, observing for changes in facial expression and alteration in physiologic parameters, such as changes in heart rate, blood pressure, or respiratory pattern. If pain or anxiety persists, reassess the need for additional analgesia or sedation.3
General Equipment Needs
Most EDs are well stocked with equipment and supplies suitable for minor pediatric trauma care, including management of entrapments and retained foreign bodies. To expedite emergency procedures, a minimum amount of equipment should be retained at all times within the ED. (See Table 1.) Additional equipment needs are chronicled in sections that follow.
 |
Aural Foreign Bodies
With the exception of insect excursion, developmentally normal adults typically lodge a foreign body in the external auditory canal (EAC) during self-instrumentation of the ear. After a failed attempt at self- or assisted retrieval, adults present shortly thereafter for ED care. Adults with an EAC foreign body do not have coexisting external or middle ear pathology. They will be cooperative for examination and attempts at ED extraction. In contrast, children will insert foreign bodies into their ear canal because the orifice exists, or they are annoyed by some aural pathology.4 For children, the time to presentation for ED care tends to be extended. There is a higher incidence of coexisting ear pathology such as otitis media or otitis externa at the time of ED presentation. Case studies have demonstrated coexisting ear pathology from 17%-47%.5 Children's cooperation for extraction is highly variable.
Epidemiology. There is a sense that aural foreign bodies are a common pediatric ED complaint, although exact documentation of the incidence for patient visits to the ED for EAC foreign bodies is unavailable. In a retrospective review of consecutive patients over a two-year period, one institution encountered this complaint in 0.26% of visits.6 EAC foreign bodies are more common in male children and in patients of lower socioeconomic status.4 Foreign bodies of the ear are seen throughout the pediatric spectrum, but are more common in the 5-8 year range.6,7 A myriad of items may be inserted by a child. In reviews, as many as 27 different objects have been encountered.7 The objects are best characterized in four categories:
Inanimate, non-vegetative (pebbles, beads, plastic toy parts, paper wads, fragmented matchstick, eraser tips);
Animate (cockroach, maggot, fly);
Vegetative (popcorn, bean); and
Caustic (button battery).
The objects retained in the ear are limited only by the areas of anatomical narrowing. The largest foreign bodies are wedged at the junction of the cartilaginous and osseous portion of the EAC. Modest-sized foreign bodies may make it to the portion lateral to the tympanic membrane. Smaller foreign bodies may be wedged against the tympanic membrane.8
Clinical Presentation. Verbal children may tell their parents, or the event may be witnessed, with the resultant chief complaint of "foreign body in the ear." Other common presenting symptoms are otalgia, otorrhea (clear, purulent, or bloody), ear fullness, and foreign body sensation, with or without movement.9 A less common complaint is altered hearing. Patients may have decreased hearing or complain of a persistent noise that is exacerbated by chewing or yawning. Dizziness or vertigo are more common in adults, but may be seen with the pediatric patient. Bleeding from the external auditory canal suggests there has been a traumatic membrane rupture. Rarely, there may be a nonspecific complaint secondary to vagus stimulation, such as cough or hiccup.4,10,11 Erosive perforation of the tympanic membrane or caustic injury to the facial nerve leading to facial paralysis can result from leaking button batteries.12
ED Retrieval. Emergent removal is indicated for button batteries, insects, and vegetative material. To avoid potentially rapid, destructive erosion from impacted battery leakage, ED retrieval must be attempted with button batteries.12 To preserve equanimity, insecticidal preparation is mandated to immobilize and kill intra-aural insects.13,14 Expedited removal is suggested for vegetative matter, which may swell within the ear canal, furthering the impaction if management is delayed. In all other circumstances, EAC foreign body extraction should be considered elective. Although studies have reported a 70%-90% success rate,4,6,11 the emergency physician should not create iatrogenic trauma. The parent should be warned that any abrasion of the external auditory canal may result in 1-2 days of bleeding. Advise the patient and parent that instrumentation will be attempted, but will be abandoned if there is resultant bleeding. Announce in advance how many attempts, over a finite period, will be performed. Indicate that in circumstances of failed retrieval, referral will be made. Failed retrieval is among the most common cause for otolaryngologic referral. Other suggested indications are found in Table 2.
 |
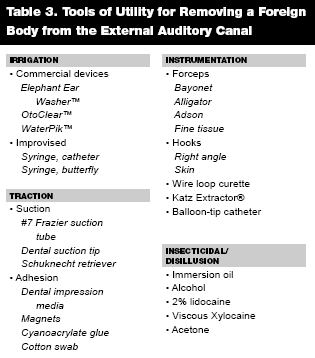
Management. A diagnostic-type otoscope head is suitable for identification of a foreign body and surrounding landmarks. However, an operating-type head is necessary to introduce the otoscope and any additional instruments under continuous direct visualization. If only a diagnostic otoscope head is available, the magnifying lens will need to be slid laterally to allow simultaneous introduction of instruments. The largest-bore speculum (≥ 9 mm) should be introduced into the external auditory canal to permit maximum visualization. The additional equipment needs depend upon which method of removal is chosen. Table 3 outlines the tools of the trade for auricular foreign body removal by irrigation, traction, and instrumentation. There are no prospective comparative studies of these methods to guide the physician's choice.4
 |
Irrigation. In most circumstances of aural foreign bodies, irrigation alone is the initial technique of choice. Irrigation is ideal for small objects adjacent to the eardrum, and for small to moderate-size round objects. The method is reserved for circumstances where a perforation of the tympanic membrane can be excluded. Irrigation is the least invasive method and associated with the least number of complications.15 The method requires no direct visualization. Several commercial apparatuses, such as the Elephant Clear WasherT or OtoClearT, may be utilized for irrigation. A WaterPik, manufactured for oral hygiene, also may be used. Alternatively, two types of intravenous catheters can be employed. A 16-18 ga. flexible intravenous catheter can be attached to a 20 mL syringe or a 1-2 inch section of butterfly needle tubing from which the needle has been cut off. Sterile saline at body temperature or saline warmed to 32.2°C-37.8°C, as confirmed by digital thermometry, can be used as an irrigation solution.16 Whichever device is used, a pulsatile stream of the irrigant is directed against the posterior, superior canal wall such that back pressure extrudes the object. Care should be taken not to direct the stream against the foreign body itself as this may push it back further towards the tympanic membrane. Dizziness, nystagmus, and vomiting are complications of stimulating the labyrinths. Battery button lodgement in the external auditory meatus is a contraindication to irrigation as this may promote leakage of the battery's electrolyte solution.12 Irrigation of vegetative foreign body is relatively contraindicated as wetting of organic materials may cause them to swell. Isopropyl alcohol and water are reported to minimize swelling of organic materials.4
Traction. Traction can be applied to the foreign body by two different techniques. A negative force can be applied to suction an object, or an adhesive can be used to engage an object.
Suction. Suction can be employed as an adjunct to failed irrigation, or suction may be used as a primary methodology. Suction is particularly useful for smooth, rounded objects, particularly those that are large, for which irrigation would likely push the object further into the ear canal. Wall-mount suction or portable suction (100-120 mm) is applied to the object with a handheld instrument. A dental suction tip or a blunt, metal Frazier suction catheter can be unmodified and affixed to the foreign body. Alternately, the Frazier suction catheter tip can be softened by attaching a segment of intravenous tubing or a tympanostomy tube. A Schuknecht device has the benefit of a soft, malleable, umbrella-shaped suctioning cap. This cap can be applied easily to a spherical or smooth object. There are no contraindications to suction methodologies. Whether commercially available soft-tip devices or improvised devices are utilized, the potential complication is pushing the foreign body deeper into the ear canal.
Traction. A firm bond via traction can be created with the foreign body, and the object is manually withdrawn. There have been case reports of success utilizing semifluid dental impression material and magnets.17 Lastly, a drop of cyanoacrylate glue can be applied to the tip of a paper clip, camel's hair paintbrush, or the blunt end of a wooden cotton swab stick.18 The instrument is introduced into the EAC and held to the foreign body surface for one minute, until a bond forms. Complications utilizing a cyanoacrylate glue include the inadvertent contact of the glue with the EAC surface or the tympanic membrane. This adherence may be broken with the application of acetone.19
Instrumentation. Instrumentation can be chosen as the primary technique or attempted after irrigation and/or suction have failed. There are three techniques for instrumentation: grab-and-snatch, hook, and insufflate. All methodologies of instrumentation require direct visualization and may be associated with abrasion of the EAC. Patients should be warned in advance of the procedure of the potential for bleeding and irritation.
The grab-and-snatch technique is suitable for small or moderate-size foreign bodies that are irregularly shaped and are in the distal half of the external canal. Bayonet, alligator, Adson, or fine tissue forceps can be used to grasp the foreign body.
Hook techniques can be used for moderate-size spherical or smooth objects as well as irregular objects. A right-angle hook probe is passed distal to the object and gently pulled forward out the auditory canal. Either a wire-looped ear curette that is bent to a 90° angle or a skin hook can be utilized in the same fashion.4,8
Instrumental manipulation can be facilitated with insufflation. Smaller foreign bodies in the external half of the canal can be successfully removed with the use of balloon-tip catheters. A Fogarty embolectomy catheter, a Fogarty biliary catheter, or the commercial Katz Extractor® can be used. The physician passes the catheter beyond the foreign body, insufflates a balloon, and withdraws the object.20 Complications include injury to the EAC, particularly if the balloon is overinflated.21
Insecticides/Disillusion. If the foreign body is a living insect, it should be immobilized or killed before removal from a person's ear canal, facilitating removal and diminishing the distress associated with the insect's movements. There are recommendations for a variety of substances including alcohols, ether, mineral oil, microscopic immersion oil, 2% lidocaine solution, and viscous lidocaine.7,14,22 In a controlled trial, Leffler and colleagues demonstrated the superiority of microscopic immersion oil.13
Impacted Styrofoam is not easily retrieved by conventional methods. Styrofoam breaks into fragments with irrigation or grasp-and-pull techniques. Success is achieved with application of acetone. As little as 0.03 mL is applied directly to the impaction using a 22-ga catheter affixed to a 1-mL syringe. The Styrofoam will shrink and can be successfully irrigated with sterile water.5
Nasal Foreign Bodies
Foreign bodies are placed in the nose by young children for reasons that are unapparent. Their amusement with a small cavity may be self initiated or result from an assisted action by a playmate or sibling. Older children sustain retained nasal foreign bodies as a result of playing with connecting magnets from two body lights or imitating body piercing with magnet-backed jewelry.23
Epidemiology. Epidemiologic information comes from case reports and small case series. Children hide foreign bodies in the nose with half the frequency of placing objects in their ears.6 Nasal foreign bodies are more common in female children, with a 2:1 ratio. The distribution of age ranges from 1 year to 12 years.6,23,24 Children younger than 2-3 years constitute nearly three quarters of the patients with nasal foreign bodies.6 As with the external auditory canal, any object small enough to fit into the orifice may become a foreign body in the nose. The types of nasal foreign bodies are limited only by the imagination of the patient and their access to objects. The objects requiring removal fall into four categories. The most common include inanimate, non-vegetative objects such as buttons, pebbles, plastic hair beads, toy parts, marbles, magnets, washers, nuts, sponges and chalk.25 Vegetative objects such as beans, peas, popcorn kernels, and seeds are second in frequency.15 Button batteries are placed less commonly in the nose than in the ear. Inanimate objects such as fly maggot larvae, screw worms, and black carpet beetles are common in warmer climates of the U.S. and are more commonly found under low socioeconomic conditions. The young pediatric patient may have one or multiple foreign bodies impacted within a naris, or bilateral involvement of the nares.21 The majority of foreign bodies are wedged inferior to the middle turbinate. Most are found adjacent to the inferior turbinate.21,25
Clinical Presentation. Patients may present to the ED with a chief complaint of nasal foreign body. They may have been observed to insert the object into the nose or have related this event to their caretakers. A foreign body within the nasal passages may be an incidental finding following an imaging study for an unrelated problem.26 The most common presentation of a retained, unrecognized, longer-standing foreign body is that of painless, unilateral nasal discharge.27 The discharge, which is usually mucoid, will progress to a serosanguineous and finally a mucopurulent discharge over time.8 Other chief complaints that result from chronic retention of a nasal foreign body include halitosis, severe body odor, recurrent epistaxis, and recurrent sinusitis.9,15 Less common manifestations are facial pain or localized swelling about the nose or orbital region.25,26
ED Retrieval. A nasal button battery may produce mucosal turbinate and septal ulceration in as little as three to six hours. Necrosis of the inferior turbinates has been reported within 24 hours.28 Similarly, magnets that are adherent across the septum may cause a time-dependent ischemic injury. Septal necrosis, including perforation, may happen within hours of injury.23 Therefore, immediate removal should be attempted for button batteries and paired magnets. Vegetative matter is a relative urgency, as there is a tendency for organic matter to swell. Myasis of the nose is an urgency in that tissue destruction has been reported with more prolonged infestation. In other circumstances, nasal foreign body extraction should be considered elective. ED success rates of removal have been in the 90%-100% range.6,29
Management. A planned approach is of greatest benefit to the patient, nursing staff, and physician. Successful retrieval with greatest patient satisfaction is most likely with one uninterrupted session. The physician and assisting personnel should not proceed until there is adequate lighting, restraint, various-sized nasal speculums, topical anesthesia such as Cetacaine® (14% benzocaine, 2% tetracaine) spray, and topical vasoconstrictors, such as 0.05% oxymetazoline solution or 0.5% phenylephrine spray, on hand. The physician needs to explain in advance to the caretaker and patient that one should expect a positive retrieval with a single technique in one attempt in the majority of cases. However, multiple attempts are needed in 25% of cases and multiple techniques 15% of the time.30 The emergency physician should assemble in advance the materials that are reasonably expected to be used for the primary technique and subsequent rescue techniques. Table 4 outlines the tools that are of utility for foreign body removal from the nose.
 |
Positive Pressure. Four varieties of positive pressure can be employed for nasal foreign body removal: forcible self-exhalation, "kissing." Ambu Bagä, and "Beamsley blaster" techniques. Positive pressure is most useful for large, round objects. The larger the foreign bodies, the more likely they are amenable to positive pressure. Foreign bodies that are uniform in size and reduce the available patency of the affected nares are also more successfully removed. The child and the caretaker need instruction and rehearsal before actual attempts are made.
Self-exhalation. Success is atraumatically achieved in the cooperative child with this technique: Place the patient in a sitting position. Compress the uninvolved nostril of the child, and instruct the child to deeply inhale through the mouth and close the mouth. The child forcibly exhales (or sneezes) through the impacted nostril or nostrils.31
"Kissing" Technique. If self-exhalation fails or the child cannot cooperate for self-exhalation, the kissing technique can be employed. Ask a caretaker who is a relative to assist. Place the child in a supine position. The caretaker explains that they want to kiss the child. The caretaker places their entire mouth over the child's entire mouth. The physician operator occludes the unaffected nostril. The caretaker performs a forced exhalation that is equivalent to a one-second forced expiratory volume measurement. The patient's glottis will spontaneously close, and the forced air column will expel the object. The operator must be prepared with a 4 x 4 sponge to catch the object to prevent passage into the child's mouth.32
"Ambu bagä" Technique. When the caretaker is a non-relative, or for other reasons prefers to not perform the kissing technique, the physician operator uses an Ambu Bagä and appropriate-size face mask. Positive pressure is applied to the child's mouth while the uninvolved nostril is compressed.33 The same precautions need to be taken to avoid potential aspiration in the airway.
"Beasley Blaster" Technique. This nasal positive pressure technique uses air pressure from a wall oxygen or air outlet. Oxygen tubing is connected to the outlet and to a male-male tube adapter. The male-male adapter attached to the oxygen at 10-15 L/min is then placed in the contralateral nostril. The pressure forces the nasal foreign body out of the affected nostril. The operator must prevent oropharyngeal entry.29
Traction. Traction can be applied to a nasal foreign body via suction devices or adhesives.
Suction. Suction techniques are most useful for smooth, pliable, or round objects. Taking care not to push the foreign body further into the nasal cavity, apply 80-120 mm suction to the object with a #7 Frazier catheter tip. An alternate method employs a Schuknecht device.30,34
Traction. Traction is of utility for a firm, smooth foreign body. Place cyanoacrylate glue on the top of a wooden stick or the cut surface of a hollow plastic swab stick. Taking care to avoid touching the walls of the nasal cavity, advance the stick directly to the surface of the foreign body. Gently press against the object for 30-60 seconds. Permit a bond to form and withdraw the stick.35
Instrumentation. Direct instrumentation is the preferred technique that is employed for smaller and irregular-shaped objects. As for aural foreign bodies, instrumentation may be performed by a grab-and-snatch, hook, or insufflation technique.
The grab-and-snatch technique is suitable for smaller objects, irregular-shaped and readily visible, with or without the assistance of a nasal speculum. An alligator or fine bayonet forceps may be used to directly grasp the object.8
Hook techniques can be used for larger or more spherical-shape objects. A 90°-angled hook may be used, or a 90° hook can be created by bending a paper clip, a wire loop, or a Calgiswab. The instrument is advanced beyond the foreign body and the foreign body is slowly extracted. As the foreign body is advanced to the nasal aperture, rotate the patient's head and block the oral passage to avoid inadvertent aspiration.
A balloon-tip catheter is good for solid, round objects that are not easily grasped with forceps. The objects must not completely occlude the nasal passage. Lubricate a 5 French or 8 French catheter. Pass the catheter beyond the object with the balloon deflated. Inflate the balloon and withdraw the catheter, sweeping the object out of the nose. A balloon catheter may also be used as an adjunct to stabilizing foreign bodies for direct instrumentation.36
Nasal Wash. The nasal wash technique may be employed for any type of foreign body. It is best employed for objects that are not amenable to instrumentation and objects that may be friable, such as food or paper wads.37 Place the patient in an upright sitting position with arms restrained. Maintain the neck in a neutral position. Fill a bulb syringe with 7-10 mL of normal saline. Place the syringe in the opposite nostril from the nostril that contains the foreign body. Advance the bulb syringe into the nasal cavity until a tight seal is maintained. Forcibly squeeze the bulb syringe, expelling the foreign body. As saline passes from one nostril through the posterior pharynx to the opposite nostril, choking and cough may occur. There is a theoretical risk of aspiration.38
Retained Penetrations
Retained penetrations in adults often involve intentional injury. Many adult penetrations are from high-velocity projectiles. In contrast, most penetrations throughout childhood are accidental. Most pediatric penetrations are of low velocity. They involve household items such as kitchen utensils, writing implements, hair accessories, or occur as a result of injury from outdoor objects during play. Significant morbidity and mortality can occur in rare circumstances where penetrations violate a critical space (such as orbit, cranium, parapharyngeal space, or cervical region).39 However, in a majority of cases, penetrations result in little disability. The physician's major concerns are controlling bleeding, reducing pain and removal of a foreign body when it is retained.
Epidemiology. The pediatric patient of any age may be a passive recipient of a projectile that leads to a penetrating wound. If the mechanism of injury involves a higher-speed projectile (for example, from a lawn mower) or involves a metal-on-metal object (for example, a grinding wheel), there is a greater likelihood of an occult retained foreign body. Passive lower-speed penetrations result from playmates who mobilized projectiles such as eating utensils, frog gigs, fish hooks, metal nails, pencil lead, and lawn darts.3 A child must be mobile to incur an active penetration. Toddlers are most likely to run with an object in their mouth, fall, and sustain an intraoral penetration of the palate or posterior pharyngeal wall.40 Preschool-age and school-age children are prone to foot penetrations, and school-age children are more likely to have impalement injuries from metal poles, fence wires, and fishing barbs. Collectively, puncture wounds and penetrations with or without foreign body account for 5%-10% of minor traumatic events that are evaluated in an ED setting.3
Clinical Presentation. There are two broad presentations of penetrating injuries. The first is that of a chief complaint of penetration. The child may have revealed the injury to the parent, or the caretaker has witnessed the event. Alternately, a retained foreign body is suspected or a retained foreign body is visible. A second presentation is that of pain, erythema, and induration as a result of foreign body reaction or secondary infection from penetration that was overlooked.
ED Retrieval. Several factors influence the decision of when and where a retained, penetrating foreign object is removed. Evaluation in an operating room setting may be required if the extent of the injury requires exploration (such as orbit, retropharyngeal, lateral pharyngeal space, cranium, or joint space). An operating room may additionally be required if penetration has violated the airway or has created neurovascular compromise. ED removal at the time of the encounter is warranted in penetrants characterized by easy access, where injuries are superficial and unassociated with violation of deeper structures. Delayed or referred services for removal on an outpatient basis are suitable in circumstances where removal will need to take place under ultrasonographic or fluoroscopic guidance.
Management. The techniques that are employed to remove a foreign body at the time of the ED encounter depend upon whether the object is visualized, the available equipment, and the nature of the penetrating object.
Complete visualization of the penetrating object is the ideal. Hemostasis and lighting are necessary in searches where full visualization is impaired. Cooperation or immobility achieved through conscious sedation is necessary for adequate exploration if removal is done under direct visualization.
Most foreign body removal can take place with readily available "general" tools available in the ED setting. (See Table 1.) Superficial objects that are fully visualized can be pulled from a wound. If wound exploration is necessary, Metzenbaum scissors or a hemostat, if spread, can aid in the visualization and removal of an object. If a foreign body is difficult to visualize or grasp, then dissection may be appropriate. An elliptical incision can be made around the wound entrance, with removal of the foreign body and contaminated tissue. Additional equipment will be of assistance for barbed objects, needles and nails, splinters, and spines. (See Table 5.)
 |
Specific Objects
Fish Hooks. There are several methods to remove an embedded fish hook; the various techniques have not been subjected to head-to-head comparisons. The chosen method should be determined by individual preference combined with the location of the embedded barb. Irrespective of the technique chosen, use Betadine solution to prep the skin, perform local infiltration overlying the point of the hook, or perform a regional block.
Retrograde Technique. This technique is useful if the fish hook is superficial and the barb is not caught on fibers in the skin.21 Use the index finger to depress the tip of the hook, and disengage the barb. Use gentle downward pressure on the shank of the hook while backing out the hook.
Needle Cover. This technique is used for smaller hooks that are superficially embedded, as larger or more deeply embedded barbs may be difficult to sheath within the bevel of the needle. Insert an 18- or 20-gauge needle through the wound along the shaft of the hook, with the bevel of the needle facing the inside of the hook's belly. Advance the needle along the hook's belly until the needle opening slides over the barb of the hook. Firmly hold the needle and hook together, and back the hook and needle out of the wound as a unit.
String Pull. This technique is ideal when the hook is deeply embedded or when tools beyond a string are lacking. The technique should not be used on body parts that cannot be fully immobilized. The technique is also contraindicated for hooks embedded near the orbit. Secure the body part containing the fish hook firmly to prevent movement during the procedure. Loop a 1- to 2-foot-long string or 1-0 silk suture around the belly of the fish hook. Wrap the string securely around the dominant clinician's index finger. Depress the shank of the hook with the opposite index finger and thumb, disengaging the barb from surrounding tissue. Without pause or hesitation, jerk the hook away from the embedded site.
Advance and Cut. This technique is ideal when the barb of the hook is near the surface of the skin, or the barb has already passed back through the skin. This push-through technique is typically applied when one of the other methods above has failed. Grasp the fish hook with a needle driver or needle-nose pliers, and advance the barb completely through the skin. Cut the hook behind the barb and remove the hook back through the entrance wound.
Excisional. This is a method reserved when all other methods for removal have failed. The principle is to surgically remove the barb under direct visualization. Extend a small incision from the entrance wound of the barb. Dissect and bluntly spread to improve visibility. Grasp the tip of the hook with a hemostat and lift it out.
Non-vegetative Penetrants. In the course of play, children penetrate various body parts with non-vegetative matter. The patient may present with a puncture wound alone, or there may be an obviously retained foreign body. These non-vegetative foreign bodies are most often in the form of needles and nails. Retained foreign bodies that are superficially located in acral regions can be removed with needle-nose pliers. Retained metallic foreign bodies that penetrate the skull require neuroimaging and neurosurgical consultation, as removal should take place in the operating room. Penetrations of joint spaces are best dealt with by orthopedics in the operating room. Intraoral injuries may be removed and repaired in the ED or can be performed by ENT physicians under anesthesia.41
Vegetative Penetrants. There are two broad categories of vegetative penetrants: wood and thorns, or spines from plants such as roses, brambles, or cacti. Wooden foreign bodies, if not completely removed, cause a significant inflammatory reaction. A very superficial splinter of wood can be removed by utilizing tweezers or forceps to grasp the protruding splinter. With large shards, it is best to abandon pulling the ends of the splinter. Instead, use a scalpel to make an incision along the axis of the splinter. Remove the splinter and cleanse the tract. Sutures can be used to approximate the edges of the incision. Medium to large cactus spines can be removed with tweezers or forceps by direct axial traction. Smaller spines are more difficult and tedious to remove. Adherents are best used for multiple fine spines. Apply one of several adherents, such as facial mask gel, rubber cement, or household glue, and permit the adherent to harden. An alternate is to apply a depilatory wax which has been melted in the microwave and applied warm, then permitted to dry. The edges are lifted and rolled, removing the cactus spines. Several applications of any of the adherents may be necessary.42,43
Entrapments
Various names have been used to describe the strangulation of an anatomical site by an inanimate object. In 1998, Barton proposed the term "hair-thread tourniquet syndrome" to describe the circumstances where a fiber of hair or thread had become tightly wrapped around an appendage.44 The term for this type of entrapment has remained. One of the earliest accounts of hair entrapment in the literature was a revengeful genital ligature.45 Intentional, abusive injury is rarely invoked today.46 A majority of entrapment circumstances are accidental. Typically, a fiber from clothing or a strand of hair inadvertently wraps around a finger, toe, penis, clitoris, or, rarely, a wrist.47 This impedes lymphatic drainage, initiating venous outflow obstruction and lymphedema. As soft tissue swelling advances, the constricting band cuts through the skin and becomes further embedded in the tissue of the appendage. In an acute entrapment, there ultimately may be restriction of arterial blood flow, necrosis, and loss of the distal appendage. In chronic entrapments, epithelialization may occur, obscuring the constricting device beneath an overlying skin bridge.
Epidemiology. Finger and toe entrapments from constricting hair or threads cross cultural, economic, and gender barriers. It has been reported worldwide.48 Infants are most frequently affected. There have been reports in children as young as 4 days of age.
Penile tourniquet syndromes from hair and threads are also most common during early infancy but have been depicted up until 6 years of age. Penile entrapments in children older than 6 years may involve rubber bands or plastic, ceramic, or metallic objects. These constricting bands are placed by individuals who are emotionally disturbed or who are attempting to carry out autoerotic behaviors. In contrast, a male of any age may accidentally entrap a portion of the penis during the zipping or unzipping process.49 School-age children can entrap the foreskin or penis in a bathing suit mesh.50
Female genital tourniquet syndromes occur from infancy throughout adolescence. Labial or clitoral entrapment in infants and toddlers is likely accidental, whereas clitoral tourniquet syndromes in older children, particularly recurrent, may reflect autoerotic behavior.51
There are no age barriers for inventive children who entrap other aspects of their anatomy. No age predilection has been depicted for entrapment injuries of umbilicus, nipple, earlobe, nasal septum, scrotum, uvula, or tongue.52-54
Clinical Presentation. Two presentations are seen with entrapments-a chief complaint rendered by the patient or parent that there is an entrapped body part, or a preverbal child who has been irritable for unexplained reasons. Depending upon the length of entrapment and the body part entrapped, there is usually a pedunculated, tender, hyperemic mass with an object wrapped around the base of the constricted organ. The soft tissue swelling may be severe enough that the constricting band becomes obscured by edema and becomes difficult to identify. Tissue distal to the band has a variable appearance depending upon the length and severity of the tourniquet syndrome.
ED Retrieval. The ED management of entrapment should be based on four factors.
Acuteness of Event. The degree of morbidity is somewhat correlated with the duration of the entrapment. If the entrapment has been extremely brief, conservative, potentially time-consuming ED case management can proceed.
Location of Entrapment. If the physician is capable of manipulating the involved tissue and the patient is accepting of manipulation or is pharmacologically sedated, ED care can be carried out. If airway compromise is possible, as in uvular entrapment, management should be deferred to the operating room.54
Type of Band. The entrapping device (band) causes pathophysiologic changes. Elastic or collapsible devices placed around a body part exert uncontrolled, excessive pressure. Within a short time frame they may injure neurovascular bundles. If neglected, deeper structures, such as tendon or bone, may be altered. Rigid bands impart relative protection to the deeper structures. With non-collapsible bands, erosions are limited to soft tissue structures. These embedded, non-elastic bands generally do not require immediate removal, in contrast to the collapsing bands.55
Severity of Injury. Entrapments that are airway-threatening or appendage-threatening at the time of presentation need rapid management. Embedded bands involving disruption of integument can be managed emergently. Injuries with nonviable distal tissue should be managed in the operating room.52
Management. There are two broad techniques for managing entrapments. These are referred to as intact and divisional removal. In intact removal the integrity of the banding object is maintained. The physician focuses on distal edema reduction and advances the band over the affected area. Intact methods are often referred to as conservative. The second, divisional management is often considered more aggressive management. In divisional management, the entrapment is displaced by physical disruption such as bending, cutting, sawing, or crunching.
Successful ED management requires equipment suited for entrapments of various body parts. There are both general equipment needs and specific equipment needs for intact and divisional care. (See Table 6.)
 |
Intact Removal. Intact removal is ideal for digital entrapment by non-elastic bands where the affected appendage is not immediately in danger. Retrieval is facilitated by reducing distal edema. The procedure is a wrap-slash-hang-cool distal-edema reducing technique. It is often referred to as a string technique.
String Wrap. After documenting the neurovascular status, consider a digital block. Using tape or string, tightly wrap the affected finger from the tip of the finger towards the constricting band. Elevate the hand above the patient's shoulder and allow 15 minutes to pass. In the interim, cool the swollen appendage with ice or cold water. Inflate the patient's forearm with a blood pressure cuff. Remove the tape and evaluate the edema. If edema is still significant to prevent removal of the constricting band, rewrap the finger with the string or tape and re-elevate the hand. Deflate the blood pressure cuff. Allow 10-15 minutes to pass. Repeat this process until the compression distal to the constricting band has redistributed the edema both distally and proximally to the band. Once this is accomplished, lubricate the digit. Firmly grasp the constricting band by using gauze or a Kelly clamp. Advance the band distally over the affected tissue.52,56
Alternate String Pull. An alternate method can be employed without awaiting redistribution of distal edema fluid. Lubricate the digit. Wrap a string or string equivalent, such as 0-silk suture, dental floss, nasal packing, gauze, umbilical tape, or Penrose drain, around the distal digit. Tightly wind the string proximally toward the constricting band. With the aid of a forceps or clamp, pull the thread or thread equivalent under the constricting band. Relubricate the digit. Use the proximal tail as a lever for distal advancement over the compressing object as it is unwound from the finger. If a Penrose drain is slipped under the constricting band, with the assistance of a clamp, the tube can be folded over the band. The formed "cuff" of the rubber is pulled distally, dislodging the band.52,56
Divisional Removal. Divisional care of an entrapped body part involves physical separation of the incarcerating device. In breaking the band, vascular compression is limited, restoring perfusion. Depending upon the location of the entrapped area and the attributes of the offending agent, several methods can be employed.
Unwrap. With the aid of a magnifying device, utilize a blunt probe to manipulate a constricting hair. If a loose end of the constricting hair can be located, grasp it with a fine forceps or a hemostat and unwind the constricting hair.
Manual Incision. In hair tourniquets of the penis, clitoris, or digits and in bathing suit mesh entrapment, where the hair tourniquet is visible and not penetrated deep into the tissue, manually incise the offending strand(s).50,51,57 Isolate the strand with a blunt probe and cut the thread with fine-tipped scissors, curved suture removal blade, or blunt-tipped scissors. Alternately, a scalpel blade may be used to dissect the hair onto a blunt probe, which serves to protect the underlying structure.
Despite exploration, when the hair thread is not visualized due to the depth of penetration, manual incision is performed to spare the entrapped body part. Surgical consultation is an option. For the digit, perform a nerve block. With a #11 blade, incise longitudinally along the digit with the blade perpendicular to the strand and skin surface. Incise deeply to ensure incision of the fiber. An alternate is a longitudinal incision on the dorsal surface at the 12 o'clock position. For the entrapped penis, perform a penile nerve block. Incise at the lateral, inferior surface at the 4 o'clock or 8 o'clock position. Make successive strokes through a superficial incision, with the goal of releasing the band without penetrating the fascial layer into the lumen of the corpora.58
Non-powered Cutters. Thin, impacted metallic bands can be removed with a cutting device that requires manual application of force. Wire or bolt cutters are poorly suited for cutting metallic bands. Misdirected force can be injurious to the entrapped body part. A hand-powered ring cutter is suited for smaller bands. For digital entrapment, lubricate the area liberally. Rotate the ring until the thinnest section is on the palmar surface. Place the cutter guard under the ring. Place the wheel on the ring and apply pressure while turning the wheel. A single cut may permit the ring edges to be pulled apart with a hemostat or clamp. If necessary, make a second cut to facilitate removal.
Powered Cutters. Battery-powered or motorized ring cutters are preferred for broad-shaped or large-girth constricting bands. These powered devices saw bands that are not amenable to division by hand-powered cutting. The Mooney GEM® Ring Cutting System has a diamond-impregnated disk that is useful for platinum, steel, iron, or brass. A carbide cutting device is used for gold, silver, and copper. Rotate the constricting band, maneuvering the thinnest portion of the band to the area of the appendage with the loosest skin. Pass the shield below the constricting band. Apply cooling gel (provided by the cutter manufacturer). Limit sawing to 30-second intervals to facilitate heat dissipation. Create two divisions to remove bands of a large girth.
A Dremel® MultiPro® Rotary Tool is effective in cutting metallic and plastic bands.59 Sawing is achieved by an AC-powered toothless, tungsten carbide-cutting wheel. Cut for less than 30 seconds and/or irrigate with an ice bath to allow the metal to cool. Two divisions are typically necessary.
Crushing. Finger rings made of tungsten carbide or ceramic can be removed by cracking them into pieces. Place vise grip-style locking pliers over the ring. Adjust the claws to clamp lightly. Release and adjust the tightener 1-3 turns and clamp again. Repeat until cracks are heard. Continue clamping in different positions until the material breaks away.60
Zip Fastener Disruption. The penile foreskin grasped by a zipper may be managed by disrupting the fastener of the zipper. The median bar between the faceplates of the zipper can be disrupted with a bone cutter, wire snip,61 or mini hacksaw.49 If the median bar is not amenable to cutting, a flat-head screwdriver can be used to disrupt the faceplate of the zipper. The screwdriver head is inserted between the outer and inner faceplates of the zipper, and a twisting movement is made toward the median bar. This widens the gap between the faceplates and disengages the prepuce.62
Conclusion
In delivering pediatric minor trauma care, emergency physicians typically apply a simple solution to a simple endeavor. Most encounters require neither complex clinical reasoning nor equipment. In certain circumstances, however, retained foreign bodies and entrapments pose treatment uncertainties. For specific circumstances, there is little in the literature to provide guidance. However, this article reviews much of the literature regarding specific management of retained foreign bodies and entrapments and presents each technique, necessary equipment, and helpful tips to facilitate performance of each procedure.
References
1. Bauchner H, Vinci R, Bak S, et al. Parents and procedures: A randomized controlled trial. Pediatrics 1996;98:861-867.
2. Sacchetti A, Lichenstein R, Carraccio CA, et al. Family member presence during pediatric emergency department procedures. Pediatr Emerg Care 1996;12:268-271.
3. Muenchen CC, Singer JI. Minor pediatric trauma: Tips and techniques. Resident and Staff Physician 2001;47:32-41.
4. Fritz S, Kelen GD, Sivertson KT. Foreign bodies of the external auditory canal. Emerg Med Clin North Am 1987;5:183-192.
5. White SJ, Broner S. The use of acetone to dissolve a Styrofoam impaction of the ear. Ann Emerg Med 1994;23:580-582.
6. Baker MD. Foreign bodies of the ears and nose in childhood. Pediatr Emerg Care 1987;3:67-70.
7. Yuca K, Yuca SA, Caksen H. Aural live foreign bodies in children. J Emerg Med 2003;25:102-104.
8. Votey S, Dudley JP. Emergency ear, nose, and throat procedures. Emerg Med Clin North Am 1989;7:117-154.
9. Brownstein DR, Hodge D. Foreign bodies of the eye, ear, and nose. Pediatr Emerg Care 1988;4:215-218.
10. Wagner MS, Stapczynski JS. Persistent hiccups. Ann Emerg Med 1982; 11:24-26.
11. Ansley JF, Cunningham MJ. Treatment of aural foreign bodies in children. Pediatrics 1998;101:638-641.
12. Bhisitkul DM, Dunham M. An unsuspected alkaline battery foreign body presenting as malignant otitis externa. Pediatr Emerg Care 1992;8:141-142.
13. Leffler S, Cheney P, Tandberg D. Chemical immobilization and killing of intra-aural roaches: An in vitro comparative study. Ann Emerg Med 1993;22:1795-1798.
14. Antonelli PJ, Ahmadi A, Prevatt A. Insecticidal activity of common reagents for insect foreign bodies of the ear. Laryngoscope 2001;111:15-20.
15. Brown L, Dannenberg B. A literature-based approach to the identification and management of pediatric foreign bodies. Pediatr Emerg Med Rep 2002:94-104.
16. Ernst AA, Takakuwa KM, Letner C, et al. Warmed versus room temperature saline solution for ear irrigation: A randomized clinical trial. Ann Emerg Med 1999;34:347-350.
17. Raz S, Stassen R, Hilding D. Impression materials for removal of aural foreign bodies. Ann Otol Rhinol Laryngol 1977;86:396-399.
18. Pride H, Schwab R. A new technique for removing foreign bodies of the external auditory canal. Pediatr Emerg Care 1989;5:135-136.
19. Bock GW. Skin exposure to cyanoacrylate adhesive. Ann Emerg Med 1984;13:486.
20. Virnig RP. Nontraumatic removal of foreign bodies from the nose and ears of infants and children. Minn Med 1972;55:1123.
21. Stewart C. Foreign body removal. Pediatr Emerg Med Rep 1998;3: 19-28.
22. O'Toole K, Paris PM, Stewart RD, et al. Removing cockroaches from the auditory canal: controlled trial. N Engl J Med 1985;312:1197.
23. Brown L, Tomasi A, Salcedo G. An attractive approach to magnets adherent across the nasal septum. CJEM 2003;5:356-358.
24. Pitetti RD, Mishra S, Hickey R. Magnet-backed earrings: Not just for decoration. Pediatr Emerg Care 1998;14:208-209.
25. Werman HA. Removal of foreign bodies of the nose. Emerg Med Clin North Am 1987;5:253-263.
26. Dane S, Smally AJ, Peredy TR. A truly emergent problem: Button battery in the nose. Acad Emerg Med 2000;7:204-206.
27. Cohen HA, Goldberg E, Horev Z. Removal of nasal foreign bodies in children. Clin Pediatr (Phila) 1993;32:192.
28. Tong MC, Van Hasselt CA, Woo JK. The hazards of button batteries in the nose. J Otolaryngol 1992;21:458-460.
29. Navitsky RC, Beamsley A, McLaughlin S. Nasal positive-pressure technique for nasal foreign body removal in children. Am J Emerg Med 2002;20:103-104.
30. Kadish HA, Corneli HM. Removal of nasal foreign bodies in the pediatric population. Am J Emerg Med 1997;15:54-56.
31. Messervy M. Forced expiration in the treatment of nasal foreign bodies. Practitioner 1973;210:242.
32. Backlin SA. Positive-pressure technique for nasal foreign body removal in children. Ann Emerg Med 1995;25:554-555.
33. Finkelstein JA. Oral Ambu-bag insufflation to remove unilateral nasal foreign bodies. Am J Emerg Med 1996;14:57-58.
34. D'Cruz O, Lakshman R. A solution for the foreign body in nose problem. Pediatrics 1988;81:174.
35. Hanson RM, Stephens M. Cyanoacrylate-assisted foreign body removal from the ear and nose in children. J Paediatr Child Health 1994;30:77-78.
36. Nandapalan V, McIlwain JC. Removal of nasal foreign bodies with a Fogarty biliary balloon catheter. J Laryngol Otol 1994;108:758-760.
37. Lichenstein R, Giudice EL. Nasal wash technique for nasal foreign body removal. Pediatr Emerg Care 2000;16:59-60.
38. Handler SD. Nasal wash technique for nasal foreign body removal. Pediatr Emerg Care 2000;16:307.
39. Koestler J, Keshavarz R. Penetrating head injury in children: A case report and review of the literature. J Emerg Med 2001;21:145-150.
40. Joseph MM, Lewis S. Stroke after penetrating trauma of the oropharynx. Pediatr Emerg Care 2002;18:179-181.
41. Marom T, Russo E, Ben-Yehuda Y, Roth Y. Oropharyngeal injuries in children. Pediatr Emerg Care 2007;23:914-918.
42. Martinez TT, Jerome M, Barry RC, et al. Removal of cactus spines from the skin. A comparative evaluation of several methods. Am J Dis Child 1987;141:1291-1292.
43. Putnam MH. Simple cactus spine removal. J Pediatr 1981;98:333.
44. Barton DJ, Sloan GM, Nichter LS, et al. Hair-thread tourniquet syndrome. Pediatrics 1988;82:925-8.
45. G. Ligature of the penis. Lancet 1832;2:136.
46. Garty BZ, Mimouni M, Varsano I. Penile tourniquet syndrome. Cutis 1983;31:431-432.
47. Sun KK, Choi KY, Chow YY. Injury by mittens in neonates: A report of an unusual presentation of this easily overlooked problem and literature review. Pediatr Emerg Care 2007;23:731-734.
48. Wang M, Schott J, Tunnessen WW Jr. Picture of the month. Hair-thread tourniquet syndrome. Arch Pediatr Adolesc Med 2001;155: 515-516.
49. Strait RT. A novel method for removal of penile zipper entrapment. Pediatr Emerg Care 1999;15:412-413.
50. Hoppa EC, Wiley JF 2nd. Bathing suit mesh entrapment: an unusual case of penile injury. Pediatr Emerg Care 2006;22:813-814.
51. Sylwestrzak MS, Fischer BF, Fischer H. Recurrent clitoral tourniquet syndrome. Pediatrics 2000;105:866-867.
52. Peckler B, Hsu CK. Tourniquet syndrome: A review of constricting band removal. J Emerg Med 2001;20:253-262.
53. Bank DE, Diaz L, Behrman DA, et al. Tongue entrapment in an aluminum juice can. Pediatr Emerg Care 2004;20:242-243.
54. Krishna S, Paul RI. Hair tourniquet of the uvula. J Emerg Med 2003; 24:325-326.
55. Fraser KE, Jamison DA. Embedded-ring syndrome. Ann Emerg Med 1995;25:856-857.
56. Cresap CR. Removal of a hardened steel ring from an extremely swollen finger. Am J Emerg Med 1995;13:318-320.
57. Alverson B. A genital hair tourniquet in a 9-year-old girl. Pediatr Emerg Care 2007;23:169-170.
58. Kerry RL, Chapman DD. Strangulation of appendages by hair and thread. J Pediatr Surg 1973;8:23-27.
59. Brock S, Kuhn W. Removal of constricting bands using the Dremel drill. Acad Emerg Med 1999;6:1182-1183.
60. Hajduk SV. Emergency removal of hard metal or ceramic finger rings. Ann Emerg Med 2001;37:736.
61. Nolan JF, Stillwell TJ, Sands JP Jr. Acute management of the zipper-entrapped penis. J Emerg Med 1990;8:305-307.
62. Raveenthiran V. Releasing of zipper-entrapped foreskin: A novel nonsurgical technique. Pediatr Emerg Care 2007;23:463-464.
Entrapments and retained foreign bodies represent a common cause of emergency department (ED) visits. A majority of these pediatric presentations are easily assessed and managed by emergency physicians. However, even when accurately identified, this injury pattern may present therapeutic challenges.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
