Pediatric Hand Injuries, Part I: Fractures and Dislocations
Pediatric Hand Injuries, Part I: Fractures and Dislocations
Authors: Carl Menckhoff, MD, FACEP, FAAEM, Associate Professor, Department of Emergency Medicine, Medical College of Georgia, and Chair, Education Committee, Georgia College of Emergency Physicians; Nicholas Kimpel, DO, Resident Physician (PGY3), Department of Emergency Medicine, Medical College of Georgia; and Daniel Kaminstein, MD, Resident Physician (PGY3), Department of Emergency Medicine, Medical College of Georgia.
Peer Reviewer: Steven M. Winograd, MD, FACEP, Attending, Emergency Medicine, St. Joseph Medical Center, Yonkers, NY.
Hand trauma is common, and children frequently present to the emergency department (ED) with these injuries. Early recognition and appropriate management, including timely reduction and appropriate referrals, are critical. Inappropriate management may have a significant impact on the child's eventual hand function. This article discusses the unique features of pediatric hand trauma, with special consideration for Salter-Harris fractures.
The topic of pediatric hand trauma has been divided into two parts to comprehensively cover this important area. The first part focuses on fractures and dislocations and their recognition and management. The second part will target amputations, lacerations, and bite wounds.
The Editor
Introduction
Injuries of the hand in children are frequently seen in the ED, and with children and adolescents participating in sports in record numbers, the frequency of these injuries is continuing to rise. Sports injuries in children and adolescents are by far the most common cause of musculoskeletal injuries treated in the ED, accounting for 41% of all musculoskeletal injuries.1
This two-part article outlines several important hand injuries in children and will review likely mechanisms of injury, radiographic findings and treatment. Part I addresses common fractures and dislocations, and Part II will cover amputations, lacerations, and bite wounds.
Physeal Injuries
One of the major differences between the pediatric and the adult skeleton is the presence of growth plates or physes.2,3 When seeing a pediatric patient with any injury to the extremity, physeal injury must always be considered. The physis is the site of ossification and longitudinal bone growth.4 It consists of four zones in order from the epiphysis to the metaphysis: the zone of resting cells, the zone of proliferating cells, the zone of hypertrophic/maturing cells, and the zone of provisional calcification. The third zone, consisting of hypertrophic maturing cells, is the weakest link in the physis.2 This area lacks mechanical strength and is more susceptible to injury than the surrounding ossified bone.2 Ligaments of children are stronger and more compliant, when compared to bone, than those of adults. This often leads to physeal or bony injury before ligamentous disruption. The main concern with fractures that involve the physis is premature closure of the physis and resultant growth arrest. The risk of complications increases with the severity of the fracture. Physeal injuries account for 15% to 30% of all pediatric fractures, and while complications are uncommon, significant growth disturbance may occur in approximately 10%.5,6 While injury to the physis can occur at any time prior to physeal closure, it is more common during the adolescent growth spurt, between the ages of 10 and 16 years, and is more common in boys than in girls.2,7,8 The distal radius is the most common site of physeal injury.
Drs. Robert Salter and J.J. Harris described the Salter-Harris Classification of physeal fractures in 1963.2,9,10 This classification system describes the five types of fractures involving the physis, and is based on the involvement of the metaphysis, physis, and epiphysis.
Type I. Salter-Harris type I fracture is a disruption through the physis.2,7 Approximately 6% of physeal fractures are type I fractures.9 These fractures do not involve any osseous fracture to the epiphysis or metaphysis. The more severe type I injuries involve displacement of the epiphysis, usually in the dorsal direction, and require gentle reduction by an orthopedic specialist. The hallmark of this injury is point tenderness. These can be difficult to detect radiographically because they involve only the physis, which is radiolucent. When a child presents with point tenderness over the growth plate but has normal radiographs, be suspicious of a Type I fracture and treat accordingly with immobilization and followup.7,9
Type II. Salter-Harris II fractures are the most common type, accounting for 75% of all physeal fractures.2,11 (See Figure 1.) They extend through the physis and metaphysis. The segment of metaphyseal bone is referred to as the "Thurston-Holland" fragment or sign.2 The germinal layer is not involved; therefore, growth disturbances are rare. These injuries may also require treatment with gentle reduction by a subspecialist if there is displacement, and immobilization along with outpatient follow-up. Excessive closed manipulation can lead to an increase in the amount of physeal damage, increasing the risk for growth plate arrest.5 A perfect reduction is not an absolute requirement, as the younger the child, the greater capacity for bone remodeling.
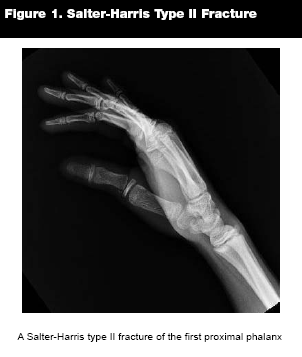 |
Type III. Salter-Harris III fractures are intra-articular fractures of the epiphysis that extend across the physis. (See Figure 2.) They account for approximately 10% of physeal fractures.11 The prognosis is generally good, but more guarded than with type I or II fractures and is related to the preservation of the blood supply.2 Since type III injuries occur predominantly in older adolescents, the physis has less remaining growth potential, and therefore seldom results in significant shortening. The subspecialist's treatment goal is to anatomically realign the joint surface.5 Orthopedic consultation in the ED is often required.
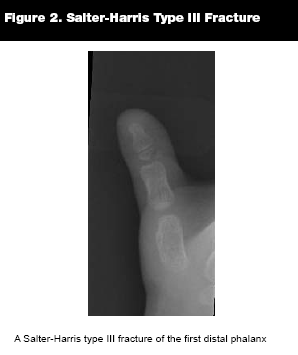 |
Type IV. Salter-Harris IV fractures represent approximately 10% of all physeal fractures.2,12 These are intra-articular fractures and have a high risk of growth disturbances. The fracture line originates at the articular surface crosses the epiphysis and extends through the full thickness of the physis, exiting through a segment of the metaphysis.2 As with type III fractures, anatomic reduction by an appropriate specialist is required to prevent the formation of bony bridges between the metaphysis and the epiphysis.5 Type IV fractures are more likely to require operative intervention to achieve anatomic reduction, and the risk of growth disturbance is dependent on the degree of blood supply disruption through the epiphysis.
Type V. Salter-Harris type V fractures are crush injuries of the physeal plate, usually produced by compressive forces. They account for only about 1% of all physeal fractures.2 They are by far the most likely of all of the physeal injuries to result in bone-growth arrest.2,10 The compressive forces crush the physis and injure cells of the reserve and proliferative zones,2 and there is minimal or no displacement of the epiphysis. One may see narrowing of the physis radiographically, but sometimes the only radiographic evidence is a joint effusion. The injury is commonly diagnosed retrospectively once a bone growth abnormality has been identified.11
Phalangeal Fractures
Epidemiology. Phalanx fractures are commonly seen in the ED. Distal phalanx fractures are the most common fractures of the hand, accounting for more than half of hand fractures.13,14 (See Figure 3.) Proximal and middle phalanx fractures are also common, and may be viewed as similar injuries by the emergency physician.13
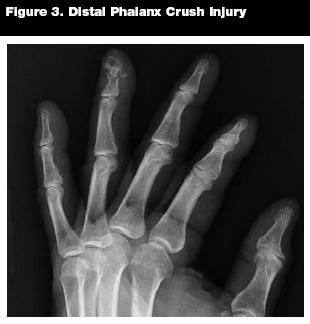 |
Patterns of Injury. Distal phalanx fractures often result from crush injuries and may be associated with soft-tissue injuries and/or nailbed lacerations.14,15 Proximal and middle phalanx injuries are often associated with sports such as basketball, but can result from any angular force to the finger.14,16
Evaluation. Evaluate the affected digit(s) for deformity, neurovascular status, associated dislocation, and tendon function.14 Subungual hematoma in distal fractures may indicate an open fracture due to nailbed laceration.17 Digital block may need to be performed (after assessing neurological status of the finger) to examine for tendon involvement.18
Imaging. Anterior-posterior, lateral, and oblique views of the affected hand should be obtained to determine fracture type and if displacement or angular/rotational deformity is associated with the fracture.15 The injured finger should be isolated on the lateral view.17
Management. The treatment of distal phalanx fractures depends on whether the fracture is at the distal tuft or the base of the phalanx. Tuft fractures need only pain relief and a short volar splint for a few days.13 Open distal tuft fractures should be copiously irrigated and treated with prophylactic antibiotics for 35 days.19 Base fractures of the distal phalanx should be treated by splinting in extension if there is minimal or no displacement, but more serious injuries may require surgical pinning.18 Management of mallet and jersey finger injuries, and tendon injuries that are sometimes associated with avulsion fractures of the distal phalanx, are covered in later sections.
Proximal and middle phalanx fractures are managed similarly.19 (See Figure 4.) Stable fractures that are not displaced can be treated with buddy taping and early range of motion.14 Displaced fractures may be treated with closed reduction and splinting; if this fails, surgical treatment may be needed.14,18 It should be noted that some authors prefer splinting over buddy taping in pediatric fractures.13
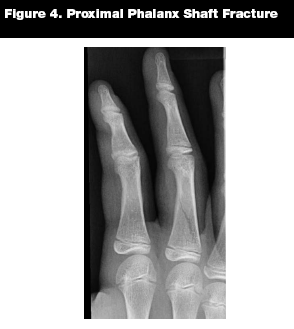 |
Key Points. Crush injuries to the distal phalanx may be open fractures requiring irrigation and antibiotics. Buddy tape or splint stable, non-displaced injuries. Refer all other injuries to a hand surgeon.
Metacarpal Fractures
Epidemiology. In children and adolescents, the hand is the most commonly injured body part. The metacarpals are involved in about 10% of all human fractures.20 In one prospective study of children presenting with hand injuries, bony fracture was the most common injury, with the metacarpals accounting for 40% of the fractures.16 Fracture of the neck of the fourth or fifth metacarpal (the "boxer's fracture") is a common and important subset of metacarpal fractures.
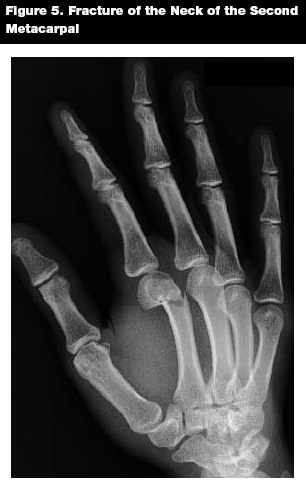
Patterns of Injury. Metacarpal fractures often result from athletic injuries in pediatric patients.21 Metacarpal fractures can be divided into fractures of the neck, head, shaft, and base. (See Figure 5.) Fractures of the metacarpal neck are the most common, and most often involve the small and ring finger,22 with fractures of the neck of the fifth metacarpal representing 80% of pediatric metacarpal fractures in one series.16 These fractures often occur when a closed fist strikes an object.23 Metacarpal head fractures, which can result from direct trauma and axial loading, often involve the joint, leading to late complications such as arthritis.20,22
 |
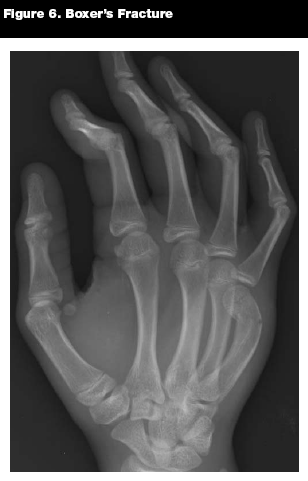
The boxer's fracture is a subset of metacarpal neck fractures that occurs in the fourth and/or fifth digits when a closed fist strikes an object. (See Figure 6.) This fracture is far more common in males. Approximately 25% of hand fractures in pediatric males are due to punching injuries, versus less than 2% in females.24
 |
Evaluation. The history of how the injury occurred should be obtained. The physical exam should document a sensory, vascular, and motor exam of the affected metacarpal and its finger. One must also check for any rotational deformity. This is best done by checking finger alignment while the metacarpophalangeal and interphalangeal joints are flexed.15,20 Also important to note are any skin defects when there is a possibility of a boxer's fracture. These so-called "fight bites" require antibiotics, as they occur when a fist strikes an opponent's tooth, allowing for deep inoculation of oral or skin bacteria into the hand.20
Imaging. Three views (posterior-anterior, lateral, and oblique) of the injured hand are needed to diagnose metacarpal fractures. Computed tomography (CT) can be of assistance to consultants when the fracture is comminuted.20 It is important to note the degree of angulation of the fracture to determine whether reduction is necessary.
Management. Proper management of a metacarpal fracture is dependent upon the location of the lesion. Fractures at different sites allow for different amounts of angulation. None of the metacarpal fracture types can tolerate rotational deformity.
Metacarpal neck fractures can be treated by closed reduction. Ten percent angulation is acceptable for the index and middle fingers, while the ring finger can tolerate 20%. The little finger can tolerate 30%40% angulation.15,18 Radial or ulnar gutter splints should be applied as appropriate, and timely subspecialty follow-up arranged, with the fracture typically immobilized for three to four weeks.22
Metacarpal head fractures can be treated nonoperatively if joint involvement is under 20%. Radial or ulnar gutter splints are appropriate for treatment, but the patient should be referred to a hand surgeon for possible open reduction and internal fixation (ORIF).22
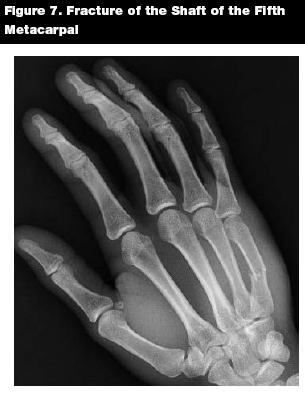
Fractures of the metacarpal shaft may be treated in a closed fashion with an appropriate splint. (See Figure 7) Very little angulation can be tolerated in the first two fingers. The ring finger can tolerate 20° of angulation, while the small finger can tolerate 30° of angulation.14,22
 |
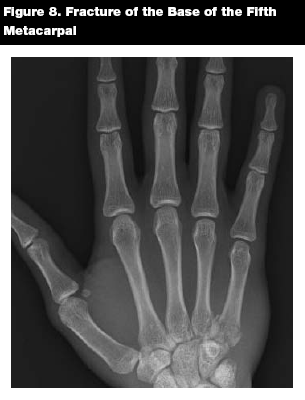
Metacarpal base fractures are uncommon and often require ORIF due to joint involvement. (See Figure 8.) If there is no joint involvement, closed reduction may be performed. Five percent angulation is tolerated in the first two fingers; in the ring and little fingers, 15% angulation is allowed.22 Appropriate consultation and referral are indicated.
 |
Key Points. Metacarpal fractures are common hand injuries in the ED. Most of these injuries are easily diagnosed with history, physical, and a three-view series of hand radiographs. The treatment depends upon the location of the fracture. In general, tolerance for angulation increases from the index finger to the little finger where up to 30° to 40° may be tolerated. Rotational deformities are not well tolerated in any type of metacarpal fracture. The boxer's fracture is a common type of metacarpal fracture involving the neck of the fourth or fifth metacarpal and is seen most often in males who have punched an object.
Phalangeal Dislocations
Epidemiology. The interphalangeal (IP) joints of the fingers are the most commonly dislocated joints in the body.15 Dislocations of the interphalangeal joint of the thumb, however, are uncommon.13
Patterns of Injury. Trauma and athletic injuries are common causes of IP joint injuries. Most IP joint dislocations are dorsal, meaning that the more distal bone is dorsally displaced in relation to the proximal bone. Lateral dislocations also commonly occur. Rarely, the distal bone will be displaced toward the palmar aspect of the hand, producing the uncommon volar IP joint displacement.25
Evaluation. Edema, deformity, and pain on palpation may be present at the site of the dislocation. The injured joint should be palpated and inspected in motion.26 Examine the affected hand for neurovascular status. A digital nerve block of the affected finger will allow for both thorough assessment and painless reduction.27
Imaging. Three-view (anterior-posterior, lateral, and oblique) radiographs should be performed both pre- and post-reduction. Avoiding a pre-reduction film is reasonable if the patient is being treated at a sporting event, although follow-up films should still be obtained to evaluate for fractures and proper joint position.15
Management. Dorsal dislocations are reduced with distal traction and pressure in a volar direction to the dislocated bone. (See Figures 9 and 10.) Digital nerve block allows for a painless reduction, but may not be necessary if the patient presents less than one hour after dislocating the joint.15 After relocating the joint, the affected digit should be splinted or buddy taped to the adjacent finger.
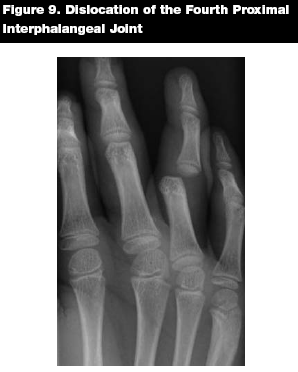 |
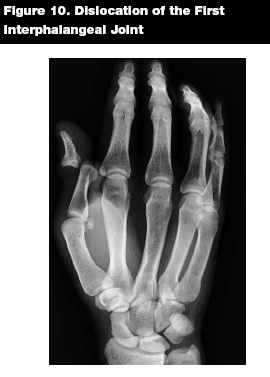 |
Volar dislocations can be more difficult to reduce in the ED, and may require consultation with the hand surgeon. Reduction may be attempted with distal traction and dorsal pressure on the dislocated bone.26 Assuming a successful reduction, the subspecialist will typically splint the injured digit in extension for six weeks.15
Key Points. Dorsal IP dislocations are more common than volar IP dislocations. Pre- and post-reduction radiographs should be obtained. Splint the affected digit after reduction. Volar dislocations may require referral to a hand surgeon for definitive management.
Metacarpophalangeal Dislocations
Epidemiology. Metacarpophalangeal (MCP) joint dislocation is not common, but it can be a serious injury that is typically associated with significant trauma.28 The index finger and thumb are the most commonly involved digits.15,28 (See Figure 11.) Even so, MCP dislocation of the thumb in children is rare.29
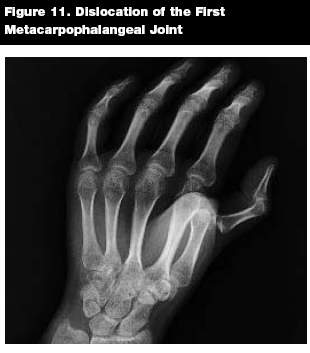 |
Patterns of Injury. Outdoor and sporting injuries are a common cause for MCP dislocations in children. Hyperextension and falls on an outstretched hand are common causes.30 Dislocations may be classified as simple or complex, with the latter involving soft tissue interposition between the articular surfaces of the joint. In the complex dislocation, the soft tissue trapped between the dislocated articular surfaces can sometimes prevent successful closed reduction.15,30
Evaluation. As with all hand injuries, a thorough neurovascular exam should be completed. The physical exam in MCP dislocation injuries can appear benign, even with severe injuries. The MCP joint is usually held in extension, while the IP joints are flexed. Skin dimpling on the palmar surface of the digit over the metacarpal head can be diagnostic of MCP dislocation.13,28
Imaging. Radiographs of the injured hand will reveal the dislocation and any associated fractures. A sesamoid bone seen in the joint is diagnostic of a complex dislocation.13
Management. Dorsal finger dislocations of the MCP joint are managed similarly to IP joint dislocations, with distal traction and volar pressure on the dislocated bone.15 Splint the joints in flexion, and refer to a hand surgeon. Closed reduction is successful about 50% of the time.31 Management of irreducible dislocations should be deferred to a hand surgeon.
Thumb MCP dislocations are rare injuries that usually require referral to a hand surgeon.32 An attempt at closed reduction can be made, however. A thumb spica splint should be placed with the MCP joint in 20° of flexion following successful reduction.13,15
Key Points. MCP joint dislocations are uncommon injuries in children. Simple dorsal dislocations are often successfully reduced by the emergency physician. Injuries may need to be treated by a hand surgeon if the attempted reduction is not successful.
Jersey Finger Injury
Epidemiology. Avulsion of the flexor digitorum profundus (FDP) tendon from the distal phalanx is an uncommon injury that typically afflicts young athletes.33 Due to lack of awareness of the diagnosis, or simply a delay in recognition, this injury is often missed.34
Patterns of Injury. Avulsion of the FDP tendon (commonly known as the "jersey finger") classically occurs when an athlete grabs a rival's jersey in an attempt to make a tackle. The FDP tendon is pulled away from the distal phalanx because the finger is actively flexing while being hyperextended by the jersey.35 The ring finger is the most commonly involved digit, in part because it extends slightly beyond the other digits when the hand grasps.34
Evaluation. Suspicion of this injury in the right clinical setting is key to diagnosis. Inability to flex actively at the distal interphalangeal joint is pathognomonic of an avulsed FDP tendon.35 (See Figure 12.) While examining the finger, the distal interphalangeal joint must be isolated by extending and preventing movement of the proximal interphalangeal joint.34 Otherwise, action of the flexor digitorum superficialis may falsely suggest normal flexion of the affected finger.
 |
Imaging. Standard three-view radiographs of the hand should be obtained to look for associated fracture or other injury.34 Radiographs will also help hand consultants plan their treatment of the injury based on which type of avulsion injury is present (type I, II, III, or IV; specifics are beyond the scope of this article).36 One study suggests that the use of ultrasound can also assist in diagnosing avulsion of the FDP tendon.37
Management. ED and office treatment consists of splinting the finger in a comfortable position and referring all cases of jersey finger to a hand surgeon for repair.34,35 If the injury is not fixed within seven to 10 days, contracture and poor outcome may result,36 so a timely referral is critical.
Key Points. Jersey finger most often affects athletes whose flexed fingers are hyperextended by their opponent's jerseys. The diagnosis may be missed unless flexion of the distal interphalangeal joint is isolated on exam. All jersey finger injuries need splinting and prompt referral to a hand surgeon.
Mallet Finger
Epidemiology. Mallet finger injuries typically occur while children are playing sports. The most commonly involved digits are the long, ring, and small fingers of the dominant hand.38
Patterns of Injury. Mallet finger is an avulsion injury of the extensor tendon where it inserts onto the distal phalanx. The injury occurs due to forced flexion of the DIP joint while the joint is in extension. The injury is named for the appearance of the digit with the DIP joint in fixed flexion. (See Figure 13a.) A true mallet finger injury occurs with partial or complete tears of the extensor tendon or through an osseous avulsion from the epiphysis of the distal phalanx.39 In children, these can be Salter-Harris IIV injuries
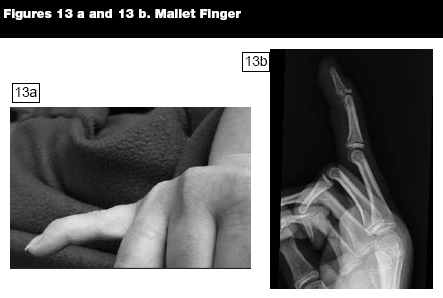 |
This fracture is often the result of a child having a finger jammed against a ball while playing sports. The child is typically preparing to catch the ball when the DIP joint is forcibly flexed, overloading the extensor mechanism causing injury to the extensor tendon. The patient presents with pain at the DIP joint and the inability to extend the distal phalanx.
Evaluation. Evaluation of a mallet deformity is similar to all other extremity injuries. It should include an evaluation of active and passive range of motion at the affected joint, stability of the joint, and a careful neurovascular exam. In addition, evaluation for extensor lag and rotational deformity should be performed. Extensor lag can be assessed by holding the PIP joint in a fixed position and asking the patient to extend the DIP joint. Rotation of the affected digit can be assessed by looking down the long axis of the digit while it is flexed 90° at the MCP joint and comparing this to the unaffected side.
Inspection of the nail is an important part in the evaluation of pediatric mallet deformities to rule out nail plate disruption. An injury pattern that is similar in appearance to a mallet deformity can occur in children when the physis of the distal phalanx is involved.39,40 If this is the case, the germinal matrix can become involved and may require specialist evaluation.
Imaging. An AP and lateral of the affected digit should be obtained to help determine the extent of a potential avulsion fracture. (See Figure 13b.)
Management. Treatment for mallet finger is accomplished by placing the affected finger in an extension splint that can allow for flexion at the PIP joint but keeps the DIP joint in extension. The splint must be worn at all times for six to eight weeks, allowing approximation of the extensor tendon to the distal phalanx. Off-the-shelf or custom-made splints are equally as effective, but need to be durable enough for the patient to wear them for six weeks.41 If the splint is removed at any point, the clock resets and the splint must be worn for another six to eight weeks. Prognosis is favorable if patients are compliant with splinting. Patients should be referred to a hand surgeon or a primary care doctor for outpatient follow-up for the injury in a timely manner to coordinate compliance and monitor functional outcome; surgical intervention is almost never required.
Studies have shown that even when mallet deformities are associated with significant fractures (including fractures into the joint) splinting alone can provide good long-term functional outcomes.42 Late presenting mallet deformities have been successfully treated with conservative management even up to three months after the injury.43 In rare cases, chronic mallet finger with significant impairment may require surgical treatment.39 In Salter-Harris III or IV fractures with greater than 50% of joint space involvement, surgery may be considered. Most studies, however, have found only minimal if any benefit to surgical therapy for chronic mallet finger.44,45 A recent Cochrane review found insufficient evidence to support surgical management of mallet finger injuries.41
Injury patterns that involve disruption of the nail bed, show evidence of a physeal fracture on radiography, or are associated with a subungual hematoma require special consideration. These are considered open fractures and the germinal matrix if involved can become interposed between the physeal fracture and prevent reduction. Children with suspicion for an open physeal injury (physeal fracture seen on radiography in association with subungual hematoma or nail bed dislocation) and children with mallet deformities with nail plate disruption should be referred to a hand surgeon, as they may require open reduction and repair of the nailbed.39,46
Long-term complications of untreated mallet finger include swan-neck deformity, decreased flexion and extension mobility at the DIP joint, degenerative joint disease, and cold intolerance. Swan-neck deformity, the most well known complication of untreated mallet finger, is caused when the lateral bands displace laterally, causing increased extension forces on the PIP joint.
Key Points. Most mallet finger injuries can be treated conservatively with the DIP joint splinted in extension. The DIP joint must be held in extension continuously for 68 weeks. If the joint is flexed at any time, the clock restarts at zero.
Conclusion
Pediatric hand injuries are a frequent ED visit. Children have unique patterns of injury, including Salter-Harris fractures, and timely recognition and appropriate management strategies optimize outcome. The diagnosis and management of common fractures of the phalanges and metacarpals were presented, with diagnostic evaluation and imaging highlighted as well as management options including strategies for reduction, splinting, and referral indications. Phalangeal dislocations and metacarpal dislocations were discussed, with a focus on accurate diagnosis and reduction procedures. In the second part of this two-part issue, amputations, lacerations, and bite wounds will be discussed with an emphasis on early recognition and management options.
References
1. Damore DT, Metzl JD, Ramundo M, et al. Patterns in childhood sports injury. Pediatr Emerg Care 2003;19:65-67
2. Perron AD , Miller M, Brady WJ. Orthopedic pitfalls in the emergency department: Pediatric growth plate injuries. Am J Emerg Med 2002: 20:54-57.
3. McQuillen K. Musculoskeletal Disorders. In : Marx JA, Hockberger RS, Walls RM, eds. Rosen's Emergency Medicine . Philadelphia, PA Mosby; 2006:2689-2692.
4. Iannotti JP. Growth plate physiology and pathology. Orthop Clin North Am 1990; 21:1-17
5. DeLee JC, Drez D Jr., Miller MD, eds. DeLee and Drez's Orthopaedic Sports Medicine, 2nd ed. Philadelphia, PA: WB Saunders; 2003.
6. Benjamin, HJ, Hang BT. Common acute upper extremity injuries in sports. Clinical Pediatric Emergency Medicine. Philadelphia, PA: WB Saunders; 2007: 15-30.
7. Uptod S, Chorley J. Acute Wrist Injuries in Children and Adolescents. Up to Date. 2007. Available at http://www.Uptodate.com.
8. Gill, TJ, Micheli LJ, The immature athlete. Common injuries and overuse syndromes of the elbow and wrist. Clin Sports Med 1996;15: 401.
9. Novelline R. Men, Women and Children. In: Squire's Fundamentals of Radiology. Boston, MA: Harvard University Press; 1999:448-449.
10. Salter RB, Harris WR. Injuries involving the epiphyseal plate. J Bone Joint Surg Am 1963;45:587-622.
11. Carson S, Woolridge D, Colleti J, et al. Pediatric upper extremity injuries. Pediatr Clin North Am 2006;52:1.
12. Jones E. Skeletal Growth and Development as Related to Trauma. In: Skeletal Trauma in Children, NE Green, MF Swiontkowsk, eds. Philadelphia, PA: WB Saunders; 1998.
13. Marx JA, Hockberger RS, Walls RM. Rosen's Emergency Medicine: Concepts and Clinical Practice, 6th ed. Philadelphia, PA: Mosby Elsevier; 2006.
14. Capo JT, Hastings H. Metacarpal and phalangeal fractures in athletes. Clin Sports Med 1998;17:491-511.
15. Leggit JC, Meko CJ. Acute finger injuries: Part II. Fractures, dislocations, and thumb injuries. Am Fam Phys 2006;73:827-834.
16. Vadivelu R, Dias JJ, Burke FD, et al. Hand injuries in children: A prospective study. J Pediatr Orthop 2006;26:29-35.
17. Cornwall R, Ricchetti ET. Pediatric phalanx fractures. Clin Orthopaed Rel Research 2006;445:146-156.
18. Lee SG, Jupiter JB. Phalangeal and metacarpal fractures of the hand. Hand Clin 2000;16:323-332.
19. Nofsinger CC, Wolfe SW. Common pediatric hand fractures. Curr Opin Pediatr 2002:14:42-45.
20. Chin SH, Vedder NB. Metacarpal fractures. Plast Reconstr Surg 2007;121:1-13.
21. Singletary S, Freeland AE, Christopher AJ. Metacarpal fractures in athletes: Treatment, rehabilitation, and safe early return to play. J Hand Ther 2003;16:171-179.
22. McNemar TB, Howell JW, Chang E. Management of metacarpal fractures. J Hand Ther 2003;16:143-151.
23. Mercan S, Uzun M, Ertugru A, et al. Psychopathology and personality features in orthopedic patients with boxer's fractures. Gen Hosp Psychiatry 2005;27:13-17.
24. Mahabir RC, Kazemi AR, Cannon WG, et al Pediatric hand fractures: A review. Pediatr Emerg Care 2001;17:153-156.
25. Freiberg A, Pollard BA, Macdonald MR, et al. Management of proximal interphalangeal joint injuries. J Trauma 1999;46:523-528.
26. Deshmukh NV, Sonanis SV, Stothard J. Irreducible volar dislocations of the proximal interphalangeal joint. Emerg Med J 2005; 22:221-223.
27. Tekkis PP, Kessaris N, Enchill-Yawson M, et al. Palmar dislocation of the proximal interphalangeal jointAn injury not to be missed. J Accid Emerg Med 1999;16:431-432.
28. Mudgal CS, Mudgal S. Volar open reduction of complex metacarpophalangeal dislocation of the index finger. Tech Hand Up Extrem Surg 2006;10:31-36.
29. Maheshwari R, Sharma H, Duncan RDD. Metacarpophalangeal joint dislocation of the thumb in children. J Bone Joint Surg 2007;80-B:227-229.
30. Ip KC, Wong LJ, Yu SJ. Dorsal dislocation of the metacarpophalangeal joint of the thumb: A case report. J Orthop Surg 2008;16: 124-146.
31. Gerrand CH, Jerrett PM. A dislocated finger. Postgrad Med J 1998;74:249-51.
32. Alioto RJ, Pellegrini VD. Complex palmar dislocation of the thumb metacarpophalangeal joint. Clin Orthopaed Rel Res 1993; 296:118-121.
33. Shabat S, Sagiv P, Stern A, et al. Avulsion fracture of the flexor digitorum profundus tendon ("Jersey finger") type III. Arch Orthop Trauma Surg 2000;122:182-183.
34. Cohen SB, Chhabra AB, Anderson MW, et al. Use of ultrasound in determining treatment for avulsion of the flexor digitorum profundus (Rugger Jersey Finger): A case report. Am J Orthop 2004;33: 546-549.
35. Lubahn JD, Hood JM. Fractures of the distal interphalangeal joint. Clin Orthopaed Rel Res 1996;327:12-20.
36. Wang QC, Johnson BA. Fingertip injuries. Am Fam Phys 2001;63: 1961-1966.
37. Tuttle HG, Olvey SP, Stern PJ. Tendon avulsion injuries of the distal phalanx. Clin Orthopaed Rel Res 2006;445:157-168.
38. Brzezienski MA, Schneider LH. Extensor tendon injuries at the distal interphalangeal joint. Hand Clin 1995;11:373-386.
39. Waters P. Operative carpal and hand injuries in children. J Bone Joint Surg 2007;89:2064-2074.
40. Seymour N. Juxta-epiphysial fracture of the terminal phalanx of the finger. J Bone Joint Surg Br 1966:48:347-349
41. Handoll HHG, Vaghela MV. Interventions for treating mallet finger injuries. Cochrane Database Syst Rev 2004, Issue 3. Art NO.:CD004574.DOI:10.1002/12651858CD004574.pub2.
42. Okafor B, Mbubaegbu C, Munshi I, et al. Mallet deformity of the finger: Five-year follow-up of conservative treatment J Bone Joint Surg Br 1997; 79-B:544-547
43. Stern PJ, Kastrup JJ. Complications and prognosis of treatment of mallet finger. J Hand Surgery Am 1988;13:329-334.
44. Lubahn JD. Mallet finger fractures: A comparison of open and closed technique. J Hand Surg Am 1989;14:394-396.
45. Warren RA, Kay NR, Ferguson DG. Mallet finger: comparison between operative and conservative management in those cases failing to be cured by splintage. J Hand Surg Br 1988;13:159-160.
46. Innis PC. Office evaluation and treatment of finger and hand injuries in children. Curr Opin Pediatr 1995;7:83-87.
Hand trauma is common, and children frequently present to the emergency department (ED) with these injuries.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
