Evening Primrose Oil for Premenstrual and Menopausal Symptoms
Evening Primrose Oil for Premenstrual and Menopausal Symptoms
By Dónal P. O'Mathúna, PhD. Dr. O'Mathúna is Senior Lecturer in Ethics, Decision-Making & Evidence, School of Nursing, Dublin City University, Ireland; he reports no financial relationships to this field of study.
A shift has occurred in recent years from viewing menopause as "a natural life event" experienced by women to "a condition that requires medical management."1 Hormone replacement therapy (HRT) was commonly used to manage the symptoms of menopause until studies from the Women's Health Initiative in 2001-2002 reported higher risks than anticipated for some women. Many women continue to seek relief from their symptoms and commonly turn to complementary and alternative medicine (CAM). One survey found that 76% of women ages 45-65 years used CAM to treat menopausal symptoms, with 37% using herbal and natural remedies.2 A 2009 survey found that 45% of women who had discontinued HRT continue to use CAM, with evening primrose oil being one of the more common interventions used.1
Background
Evening primrose oil is obtained from the seeds of a North American wildflower (Oenothera biennis).3 Early English settlers brought the flower back to England where it was cultivated for its nut-flavored root. An oil was extracted from the seeds and became known as the King's Cure-All. Surveys have found that it remains very commonly used in England. Two evening primrose oil products were licensed by Britain's Medicines Control Agency. The products were available by prescription to treat atopic eczema and mastalgia (breast pain). However, in 2002 the licenses were revoked after a review of studies on its effectiveness found insufficient evidence to continue its official approval.4
Evening primrose oil contains a high proportion of essential fatty acids. The two most common types present in the oil are linoleic acid (about 65%) and gamma-linolenic acid (GLA, 8-10%).5 Evening primrose oil is valued primarily for its GLA. It is one of the richest plant sources of GLA, with only borage oil (24%) and black currant seed oil (16%) containing more GLA. GLA is converted into a number of anti-inflammatory prostaglandins in the body, which is why evening primrose oil is recommended to treat numerous chronic inflammatory diseases.
|
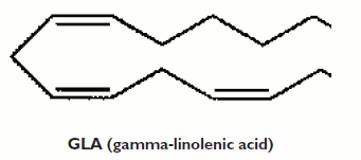
Gamma-linolenic acid Gamma-linolenic acid (GLA) is an n-6 (omega-6) poly-unsaturated fatty acid. It is composed of 18 carbon atoms and three double bonds. GLA is an a11-cis n-6 polyunsaturated fatty acid also known as 18:3n-6; 6,9,12-octadecatrienoic acid; (Z,Z,Z)-6,9,12-octadecatrienoic acid; cis-6,cis-9,cis-12-octadecatrienoic acid; and gamolenic acid. The structural formula of GLA is:
GLA is found naturally to varying extents in the fatty acid fraction of some plant seed oils. In evening primrose seed oil, it is present in concentrations of 7-14% of total fatty acids; in borage seed oil, 20-27%; and in black currant seed oil, 15-20%. GLA is also found in some fungal sources. GLA is produced naturally in the body as the delta 6-desaturase metabolite of the essential fatty acid linoleic acid. Under certain conditions, e.g., decreased activity of the delta-6 desaturase enzyme, GLA may become a conditionally essential fatty acid. GLA is present naturally in the form of triacylglycerols. The stereospecificity of GLA varies among different oil sources. GLA is concentrated in the sn-3 position of evening primrose seed oil and black currant seed oil and in the sn-2 position in borage seed oil. GLA is concentrated evenly in both the sn-2 and sn-3 positions of fungal oil. GLA, supplied in the form of evening primrose oil or borage seed oil, has been studied for many years for its possible effects in arthritis and other inflammatory processes. It has been shown to suppress inflammation and reduce joint tissue injury in many animal models. Adapted from: Evening Primrose. Herbals & Supplements. Available at www.pdrhealth.com/drugs/altmed/altmed-a-z.aspx?letter=E. Accessed May 5, 2009. |
Mechanism of Action
How evening primrose oil might treat premenstrual or menopausal symptoms is not clear. Some studies have shown that women with premenstrual syndrome tend to have lower than normal levels of GLA.5 Epidemiological studies have shown a connection between low dietary levels of GLA and a number of illnesses. However, a precise mechanism of action for evening primrose oil is not known.
Clinical Studies
Very few high-quality studies have been conducted using evening primrose oil for specific conditions in humans. A 1994 study remains the only controlled study of evening primrose oil and menopausal symptoms.6 The impact of evening primrose oil on hot flashes and night sweats was examined in 56 menopausal women randomized to either evening primrose oil (4 g/d plus 80 mg/d vitamin E) or placebo.7 Only 35 women finished the six-month study. Although all women showed some improvements, no significant differences were found between the two groups.
Evening primrose oil has been one of the more popular natural therapies for premenstrual syndrome (PMS). However, no new studies were identified since a 2001 systematic review identified four randomized controlled trials on the topic.8 This review concluded that evening primrose oil was no better than placebo in treating PMS. This conclusion was in agreement with an earlier systematic review that found most earlier studies had been of poor quality.9 A Cochrane systematic review is being conducted on the topic, but only the protocol for the review is currently available.10
Evening primrose oil's reputation for relieving PMS is based primarily on anecdotal evidence and older, uncontrolled studies. More recent randomized controlled trials have found no significant differences between the groups. Controlled trials are particularly important when studying PMS because it has been found to be highly responsive to placebos, with up to 80% of subjects improving after receiving a placebo.11
Evening primrose oil also has been used to treat mastalgia, including that associated with PMS. One of the largest studies ever conducted on mastalgia investigated this claim.4 A total of 555 women were randomized to one of four groups. Each woman took 4 g/d of capsules containing either evening primrose oil alone, evening primrose oil plus multivitamins, multivitamins alone, or placebo. After four months of blinded treatment, all groups showed an average 35% reduction in breast pain. No statistically significant differences were found between any of the four groups. The study continued as an open trial for another six months with all subjects receiving evening primrose oil, either with or without multivitamins. Breast pain was reduced by another 50%, but with no differences between the two groups. The researchers concluded that evening primrose oil was not superior to placebo in treating mastalgia. A meta-analysis of randomized controlled trials for mastalgia was published in 2007.12 While bromocryptine, danazol, and tamoxifen showed significant pain relief, evening primrose oil did not. This conclusion was based on results from four controlled trials.
Adverse Effects
The most commonly reported adverse effects of evening primrose oil in clinical trials are gastrointestinal. These are usually mild to moderate, with nausea being the most common. The effects of long-term use have not been examined. The withdrawal of evening primrose oil's medical license in Britain was not based on concerns about safety, but for lack of evidence of effectiveness. Evening primrose oil has been popularly recommended to shorten the duration of labor, but a retrospective study found that women taking the oil during their pregnancies were in labor for an average of 3 hours longer.13 Although causation could not be established, women who are pregnant or breast feeding should, in general, avoid herbs and dietary supplements until they have been demonstrated to be safe.
Formulation
Most studies have used four 500 mg capsules taken twice daily (a total of 4 g/d evening primrose oil). Recommendations range from 2-6 g/d.
Conclusion
A relatively small number of studies have examined the effectiveness of evening primrose oil in treating PMS and menopausal symptoms. The controlled studies consistently show that evening primrose oil is no more effective than placebo. Such symptoms are known to respond well to the placebo effect, which may explain why use of evening primrose oil is popular.
Recommendation
In spite of its popularity, evening primrose oil is no more beneficial than placebo in treating menopausal or PMS symptoms. Some women may have very low levels of GLA in their diet, or may not produce adequate amounts within their bodies. They may receive some general health benefits from supplementing their diet with evening primrose oil. However, its usefulness in treating any particular condition associated with premenstrual syndrome or menopause is not supported by clinical research.
References
1. Kupferer EM, et al. Complementary and alternative medicine use for vasomotor symptoms among women who have discontinued hormone therapy. J Obstet Gynecol Neonatal Nurs 2009;38:50-59.
2. Newton KM, et al. Use of alternative therapies for menopause symptoms: Results of a population based-survey. Obstet Gynecol 2002;100:18-25.
3. Haimov-Kochman R, Hochner-Celnikier D. Hot flashes revisited: Pharmacological and herbal options for hot flashes management. What does the evidence tell us? Acta Obstet Gynecol Scand 2005;84:972-979.
4. Goyal A, Mansel RE; Efamast Study Group. A randomized multicenter study of gamolenic acid (Efamast) with and without antioxidant vitamins and minerals in the management of mastalgia. Breast J 2005;11:41-47.
5. Hardy ML. Herbs of special interest to women. J Am Pharm Assoc (Wash) 2000;40:234-242.
6. Carroll DG. Nonhormonal therapies for hot flashes in menopause. Am Fam Physician 2006;73:457-464.
7. Chenoy R, et al. Effect of oral gamolenic acid from evening primrose oil on menopausal flushing. BMJ 1994;308:501-503.
8. Stevinson C, Ernst E. Complementary/alternative therapies for premenstrual syndrome: A systematic review of randomized controlled trials. Am J Obstet Gynecol 2001;185:227-235.
9. Budeiri D, et al. Is evening primrose oil of value in the treatment of premenstrual syndrome? Control Clin Trials 1996;17:60-68.
10. Wang W, et al. Evening Primrose Oil or other essential fatty acids for the treatment of pre-menstrual syndrome (PMS) (Protocol). Cochrane Database Syst Rev 2008;(2):CD001123.
11. Khoo SK, et al. Evening primrose oil and treatment of premenstrual syndrome. Med J Aust 1990;153:189-192.
12. Srivastava A, et al. Evidence-based management of mastalgia: A meta-analysis of randomised trials. Breast 2007;16:503-512.
13. Dove D, Johnson P. Oral evening primrose oil: Its effect on length of pregnancy and selected intrapartum outcomes in low-risk nulliparous women. J Nurse Midwifery 1999;44:320-324.
A shift has occurred in recent years from viewing menopause as "a natural life event" experienced by women to "a condition that requires medical management."Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.