Propofol for Sedation in Pediatric Patients
Propofol for Sedation in Pediatric Patients
Author: David I. Magilner, MD, MSPH, Assistant Professor, Pediatric Emergency Medicine, Wake Forest University School of Medicine, Winston-Salem, NC.
Peer Reviewer: Teresa Wu, MD, Director of Simulation Education and Training, Graduate Medical Education; Ultrasound Faculty and Attending Physician, Department of Emergency Medicine, Orlando Health, Orlando, FL.
Introduction
Pediatric patients in the emergency department (ED) frequently require sedation for procedures that may be painful or require them to remain still. Although its use in the adult population has been studied for quite some time, propofol use in the pediatric population is relatively new. This article examines the indications for the use of propofol for the sedation of pediatric patients, its proper administration, and the potential minor and major risks and complications of its use, as well as comparisons between propofol and ketamine for pediatric sedation.
What Are Propofol's Pharmacologic and Clinical Properties?
Source: Barnett P. Propofol for pediatric sedation. Pediatr Emerg Care 2005;21:111-114.
Using sources from pharmacologic and anesthesia literature, this review article summarizes the properties of propofol (2,6-diisopropylphenol). Propofol is a sedative/hypnotic agent that is lipophilic, soy based, and has a rapid and extensive distribution in tissues. It is thought to act by potentiating the effect of gamma-aminobutyric acid (GABA) on chloride channels in the brain. It is largely metabolized by the liver and excreted in the urine. With a loading dose of 2-2.5 mg/kg, the half-life of the drug is between 1 and 8 minutes, and elimination half-life in children is approximately 9 minutes, which is shorter than in adults. Metabolic clearance occurs between 30 and 50 minutes.
Propofol has a rapid onset of action, with unconsciousness usually occurring within one minute of the administration of a 2 mg/kg loading dose. The duration of sedation is short, and redosing is often required. Because of these clinical characteristics, propofol is best suited for relatively brief procedures.
It is important to remember that propofol does not possess any analgesic properties. Therefore, if a procedure is likely to be painful (e.g. a fracture reduction), it is recommended that an analgesic such as morphine be used in addition to propofol. As a general guideline, a systemic analgesic should be administered to any patient undergoing a significantly painful procedure under propofol sedation. Simple procedures (e.g., laceration repair or abscess incision and drainage) may not require analgesic administration when propofol is used for the procedural sedation. Finally, propofol seems to possess some anti-emetic properties. Vomiting after sedation with propofol is less common than with other sedation agents.
Comment
Propofol's unique pharmacologic properties make it an ideal choice for procedures which are anticipated to be short. Onset of action is rapid, and the duration of action is short. For painful procedures such as fracture reduction, an analgesic should be used in addition to propofol. In most cases, it may be appropriate to give the analgesic at the time the IV line is placed so that adequate analgesia can be established prior to propofol sedation.
When Should Propofol Be Used?
Source: Burton JH,Miner JR, Shipley ER, et al. Propofol for emergency department procedural sedation and analgesia: A tale of three centers. Acad Emerg Med 2006;13:24-30.
Because of its short half-life and brief duration of action, propofol is most suited for use during brief and uncomplicated procedures. In this prospective, descriptive study of propofol use in three different medical centers, the authors characterized the patient population, indications for sedation, and complications when propofol was used. This study looked at propofol use in both children and adults, and found the following indications:
dislocation reduction (38%),
fracture reduction(35%),
cardioversion (10%),
abscess incision and drainage (I&D) (8%),
computed tomography (CT) imaging (2%), and
chest tube thoracostomy (1%).
For longer procedures, such as complex laceration repair, a different agent such as ketamine was found to be more appropriate.
Comment
Once all contraindications have been addressed, the sedative agent should be chosen based on the time required to perform the procedure.
While the emergency physician can usually make a reasonable time estimate, if a consultant is also involved in the procedure, it is important to discuss with the consultant how much sedation time may be required and potential alternative courses of action if the procedure requires more time than anticipated. Additionally, note that some consultants are not aware of the rapid onset of action of propofol, and may ask to be called once the patient is sedated. In situations where propofol is being used, all personnel involved in the procedure will need to be present and ready to proceed within two minutes of propofol administration. In most centers, it appears that propofol is an appropriate sedation agent for procedures ranging from simple abscess I&D to placement of a chest tube.
How Should Propofol Be Dosed?
Source: Patel KN, Simon HK, Stockwell CA, et al. Pediatric procedural sedation by a dedicated nonanesthesiology pediatric sedation service using propofol. Pediatr Emerg Care 2009; 25:133-138.
In this recent study, the authors examined induction and maintenance doses of propofol required to adequately sedate pediatric patients for procedures in the setting of a sedation service. Because they wanted to examine both induction and maintenance requirements for propofol, the authors examined data for patients who required more than 30 minutes of sedation. Sedation was administered by non-anesthesia pediatric subspecialists. In this study, patients were given an induction bolus dose of propofol followed by a continuous infusion.
The authors found that the mean bolus dose required for induction of sedation was 3.2 mg/kg, with a range of 0.9 mg/kg to 9.7 mg/kg. More variability in induction dose was noted in patients under 1 year of age than other pediatric age groups. The mean infusion dose required to maintain adequate sedation was 5.5 mg/kg/hr, with a range of 3 mg/kg/hr to 10 mg/kg/hr. No serious respiratory or hypotensive complications occurred; one child with a seizure disorder had a seizure during sedation.
From their data, the authors recommend that propofol should be administered as an initial bolus up to 3 mg/kg, followed by an infusion of 5 mg/kg/hr for prolonged procedures. The authors emphasized that there is large patient-to-patient variability in dosage requirements, and that dosing should always be titrated to effect for each individual patient.
Comment
The authors report a dosing regimen that utilizes higher doses than those suggested by protocols in most EDs. Many institutions have only recently adopted the use of propofol for use during procedural sedation in their EDs. Because most protocols have been designed to minimize risk and maximize patient safety, acute care physicians may be underdosing the amount of propofol utilized. Propofol has a short half-life and underdosing may lead to the need for frequent repeat dosing, an overall higher dose of propofol, and sub-optimal sedation. In situations where sedation will need to be maintained, a propofol infusion can be initiated at 5 mg/kg/hour and titrated based on the patient's hemodynamic profile and level of sedation required.
Minor Complication: How to Diminish Pain at the Injection Site?
Source: Picard P, Tramer MR. Prevention of pain on injection of propofol: A quantitative systematic review. Anesth Analg 2000;90:963-969.
One minor but distressful complication of the administration of propofol is pain at the injection site. This complication can be especially difficult to manage in children, where it may lead to patient and parental distress. The resultant agitation may make completion of drug administration more difficult. Picard and colleagues conducted a meta-analysis of studies that examined pain at the injection site of propofol to estimate its incidence and determine which preventative methods might be most effective.
In this study, the incidence of pain at the injection site was 70%. Neither changing the rate of propofol injection, changing the size of the IV catheter, nor changing the temperature (neither warming or cooling) of the drug were effective in preventing pain. The only methods that were found to be effective involved the use of local intravenous lidocaine. Various techniques for lidocaine administration were studied, including the injection of IV lidocaine before the administration of propofol, the administration of IV lidocaine mixed with the propofol, and the injection of IV lidocaine after the application of a tourniquet to the arm as in a Bier block. The tourniquet technique proved most effective, with a number needed to treat (NNT) of approximately 2. The next most effective technique called for lidocaine to be mixed with the propofol (NNT = 2.4).
Comment
Although it is a minor complication, pain at the injection site of propofol can cause distress and agitation, and may inhibit the ability to administer effective sedation. Although the tourniquet technique was shown to be the most effective technique to prevent pain in this study, applying a tourniquet distal to the infusion site can be painful to the patient and can also be time consuming. In most institutions, infusion pain is minimized by mixing a small amount of 1% lidocaine into the initial dose of propofol. By using a 1:10 mixture of 1% lidocaine in propofol, practitioners can minimize the risk of lidocaine toxicity while maximizing patient comfort.
What Are the Major Complications of Propofol Use?
Source: Vespasiano M, Finkelstein M, Kurachek S. Propofol sedation: Intensivists' experience with 7304 cases in a children's hospital. Pediatrics 2007; 120;e1411-e1417.
In this prospective observational trial, the authors examined the safety profile of propofol when used in a "sedation suite" in a critical care setting. Over the course of the study, 7,304 sedations were performed and a data sheet was completed to reflect complications of the sedation. The authors looked at several complications and noted the following incidences:
Mild oxygen desaturation (85-90%), 1.7%
Serious oxygen saturation (<85%), 2.9%
Laryngospasm, 0.27%
Regurgitation without aspiration, 0.05%
Regurgitation with aspiration, 0.01%
Bronchospasm, 0.15%
Hypotension (>25 mm systolic from "normal" baseline), 31.4%
Interventions required to manage these complications included:
Oral airway, 0.96%;
Nasal trumpet, 1.57%;
Rescue breaths for >1 minute, 0.37%;
Intubation, 0.03%;
Volume requirement of > 40 mL/kg per hour, 0.11%;
Sedation induced ward or PICU admission, 0.04%;
Cardiac arrest medications, 0%; and
Aborted sedation or procedure, 0%.
Of note, the two patients who required intubation were undergoing a prolonged sedation for MRI scanning. Assisted bag-valve-mask ventilation was not a practical option to enable completion of the procedure.
In addition, the authors of this study added an "airway score" to the routine ASA classification of patients. They used a questionnaire that examined a history of stridor, snoring, obstructive sleep apnea, morbid obesity, craniofacial malformation, symptomatic asthma or heart disease, gastroesophageal reflux disease, swallowing dysfunction, or previous airway problems. If any of these were present, the patient's risk of developing an airway complication that required intervention was significantly increased.
Comment
Although this study was performed in a critical care setting and may have included patients of higher acuity than the general emergency medicine population, the authors were able to evaluate a large number of both adult and pediatric patients. The results demonstrate that although there was a modest incidence of desaturation and hypotension, interventions required to manage these complications were simple. In addition, hypotension was more common in "prolonged" sedations for procedures such as MRI scanning. Intubation or other advanced airway techniques would not be expected to be needed in procedures that require a shorter sedation period. This study illustrates the need for close monitoring and emphasizes why sedation personnel should be familiar with simple airway interventions and adjuncts such as jaw thrust, oral and nasal airway insertion, and positive pressure ventilation. Patients who undergo procedural sedation with propofol should have adequate IV access and easily accessible resuscitation fluids.
How Do Propofol and Ketamine Compare?
Sources: Godambe SA, Elliot V, Matheny D, et al. Comparison of propofol/ fentanyl versus ketamine/midazolam for brief orthopedic procedural sedation in a pediatric emergency department. Pediatrics 2003;112;116-123. Vardi A, Salem Y, Padeh S, et al. Is propofol safe for procedural sedation in children? A prospective evaluation of propofol versus ketamine in pediatric critical care. Crit Care Med 2002;30:1231-1236.
In the first study, the authors compared the use of propofol/fentanyl with ketamine/midazolam for pediatric orthopedic procedures. Outcome measures included observers' satisfaction with sedation, time of sedation, and complications of sedation. The largest advantage of propofol over ketamine in the study was the combined sedation and recovery time. For patients given propofol, this time was 58 minutes, compared to 116 minutes for the ketamine group. Sedation time was 39 minutes in the propofol goup versus 62 minutes in the ketamine group, and recovery time was 21 versus 54 minutes. In terms of sedation adequacy, both groups received similar scores. Although independent observers noted statistically significant lower distress scores in the ketamine group, the authors did not feel the results were clinically significant.
Regarding complications, patients who received propofol were noted to have a significantly higher incidence of oxygen desaturation. These patients required only jaw manipulation, re-positioning, and/or supplemental oxygen to improve their oxygenation. No patient required assisted ventilation. There were no statistically significant differences in other complication rates. Of note, the authors did report that the patients randomized to the ketamine group had a greater incidence of vomiting, and experienced nightmares, behavioral changes, and nausea/vomiting that lasted several days after administration of the drug. No long-term effects were noted in the propofol group.
In the second study, the authors compared the use of ketamine and propofol for sedation in children. They found that complications, including the need for airway repositioning, bag-valve-mask ventilation, and hypotension, occurred in almost 50% of the patients who received propofol and that all of these occurred with greater frequency in the propofol group than in the ketamine group. However, once again, the interventions required to treat these complications were simple and effective in all cases. No patient required intubation or other aggressive resuscitation measures. Of note in this study, parents, physicians, and nurses were all more satisfied with the effectiveness of the sedation when propofol was used in comparison to ketamine.
Comment
These studies are consistent with published data regarding the use of propofol and ketamine. Specifically, propofol was noted to have a higher incidence of oxygen desaturation than ketamine, while ketamine increased the risk of nausea/vomiting and behavioral phenomena. The oxygen desaturation with propofol was minor, and easily corrected with minor interventions. Many authors recommend routine oxygen supplementation at the time of propofol administration to prevent this complication.
Although hypotension was common in the propofol group, no interventions were needed to address this complication.
Is Fasting Required Before Sedation?
Source: Green SM, Roback MG. Fasting and emergency department procedural sedation and analgesia: A consensus-based clinical practice advisory. Ann Emerg Med 2007;49:465-467.
This article is a consensus-based practice advisory released by a group of emergency physician researchers. They conclude that four significant factors should be addressed to determine if fasting is required prior to performing procedural sedation. The authors recommend that all practitioners:
Assess patient risk. Higher-risk patients may include:
Patients with known or suspected anatomical abnormalities of the airway
Conditions predisposing to esophageal reflux (e.g., elevated intracranial pressure, esophageal disease, hiatal hernia, peptic ulcer disease, gastritis, bowel obstruction, ileus, tracheo-esophageal fistula)
Extremes of age (e.g., > 70 years or < 6 months)
Severe systemic disease with definitive functional limitation (i.e., ASA physical status 3 or greater)
Other clinical findings leading the acute care physician to judge the patient to be at high risk (e.g., altered level of consciousness, frail appearance)
Assess the timing and nature of recent oral intake:
Nothing
Clear liquids only
Light snack
Heavier snack or meal
Assess the urgency of the procedure:
Emergent (e.g., cardioversion for life-threatening dysrhythmia, reduction of markedly angulated fracture or dislocation with soft tissue or vascular compromise, or intractable pain or suffering);
Urgent (e.g., care of dirty wounds and lacerations, animal and human bites, abscess incision and drainage, routine fracture reduction, hip reduction, lumbar puncture for suspected meningitis, arthrocentesis, neuroimaging for trauma);
Semi-urgent (e.g., care of clean wounds and lacerations, shoulder reduction, neuroimaging for new-onset seizure, foreign body removal, sexual assault examination); or
Non-urgent or elective (e.g., non-vegetable foreign body in external auditory canal, chronic embedded soft tissue foreign body, ingrown toenail).
Consider the appropriate depth of sedation:
Minimal sedation (anxiolysis): A drug-induced state during which patients respond normally to verbal commands. Although cognitive function and coordination may be impaired, ventilatory and cardiovascular functions are unaffected.
Moderate sedation (formerly "conscious sedation"): A drug-induced depression of consciousness during which patients respond purposefully to verbal commands, either alone or accompanied by light tactile stimulation. Reflex withdrawal from a painful stimulus is not considered a purposeful response. No interventions are required to maintain a patent airway, and spontaneous ventilation is adequate. Cardiovascular function is usually maintained.
Dissociative sedation: A trance-like cataleptic state induced by the dissociative agent ketamine characterized by profound analgesia and amnesia, with retention of protective airway reflexes, spontaneous respirations, and cardiopulmonary stability.
Deep sedation: A drug- induced depression of consciousness during which patients cannot be easily aroused but respond purposefully following repeated or painful stimulation. The ability to independently maintain ventilatory function may be impaired. Patients may require assistance in maintaining a patent airway and spontaneous ventilation may be inadequate. Cardiovascular function is usually maintained.
General anesthesia: A drug- induced loss of consciousness during which patients are not arousable, even by painful stimulation. The ability to independently maintain ventilatory function is often impaired. Patients often require assistance in maintaining a patent airway, and positive pressure ventilation may be required because of depressed spontaneous ventilation or drug-induced depression of neuromuscular function. Cardiovascular function may be impaired.
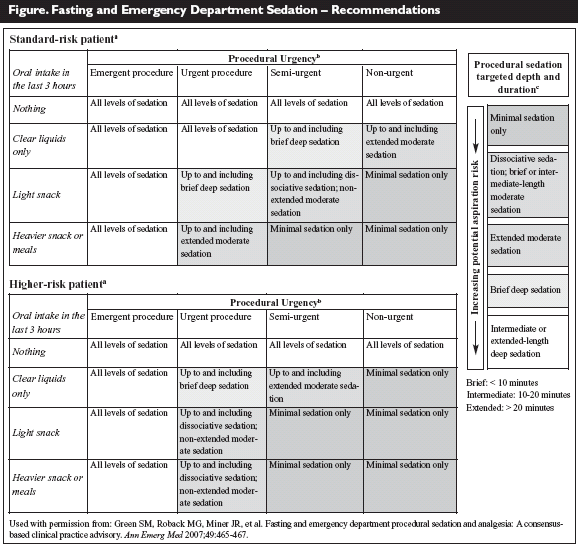
See Figure for summarized recommendations for sedation.
Comment
The consideration of fasting status has been controversial for some time in the setting of sedation in the ED. The above recommendations give the emergency physician an excellent tool for determining how to consider fasting status prior to a sedation, taking into account the individual patient's risk, the urgency of the procedure, the nature of the patient's oral intake, and the required depth of sedation.
 |
 |
What Personnel and Monitoring Does Sedation Require?
Source: Practice guidelines for sedation and analgesia by non-anesthesiologists. American Society of Anesthesiologists Task Force on Sedation and Analgesia by Non-Anesthesiologists. Anesthesiology 2002;96:1004-1017.
This is a thorough consensus statement regarding preparation, staffing, and monitoring for sedation. While not a comprehensive summary, salient points of their recommendations are included below:
Prior to the sedation, the practitioner must:
Obtain a thorough history and physical examination focusing on potential airway problems and fasting status;
Perform pre-sedation monitoring including vital signs and oxygen saturation;
Ensure that appropriate equipment is readily available for airway management, including suction equipment, a bag-valve-mask of appropriate size, and intubation equipment; and
Ensure that appropriate resuscitation medications and reversal agents are readily available.
During the sedation, the practitioner must:
Assign one physician exclusively to monitoring the sedation (one who is not involved in the procedure being performed);
Obtain continuous monitoring of respiratory rate, heart rate, oxygen saturation, and, for anything more than mild sedation, capnography; and
Assess the depth of sedation.
After the sedation is complete, the practitioner must:
Ensure proper monitoring of vital signs and mental status;
Observe the patient until his or her mental status has returned to baseline and vital signs are appropriate;
Ensure a responsible adult can take care of the patient upon discharge; and
Provide written instructions regarding home care after sedation.
Comment
These guidelines emphasize the importance of the presence of adequately trained staff, equipment, and pharmacologic agents in any setting where pediatric sedation occurs.
Conclusions
In the appropriate clinical setting, propofol can be an ideal sedation agent for use on pediatric patients in the ED. As its onset of action is rapid and its duration relatively brief, it is best suited to procedures that are anticipated to be short. In this setting, it may have several important advantages over ketamine, including decreased time in the ED, and decreased vomiting and behavioral complications. Complications of propofol are most commonly pain at the injection site, and suppression of blood pressure and respiratory drive. These can almost always be managed with simple interventions. Consideration of fasting status should be made, and adequately trained personnel equipped with appropriate tools for the management of respiratory and hypotensive complications should be present throughout the sedation.
Pediatric patients in the emergency department (ED) frequently require sedation for procedures that may be painful or require them to remain still. Although its use in the adult population has been studied for quite some time, propofol use in the pediatric population is relatively new.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
