Emergency department nurses may be first to notice a smallpox outbreak
Emergency department nurses may be first to notice a smallpox outbreak
Do you know what to do with your suspicions? Here are exact steps to take
It’s the moment of truth: A woman comes to the ED with fever and body aches. Suddenly, you notice a distinctive rash on her face and arms. The patient reports having had chicken pox as a child. The steps you take next will have a dramatic impact on your community, your colleagues, and your own health. "I am sure the first case of smallpox will cause major panic," says Sue C. Felt, RN, MS, MPH, CIC, associate hospital epidemiologist and infection control coordinator at San Francisco General Hospital.
At the end of 2001, EDs nationwide reported scores of patients who presented claiming anthrax exposure.
Darlene Matsuoka, RN, BSN, CEN, CCRN, ED clinical nurse educator at Harborview Medical Center in Seattle, says, "The worried well have not come to EDs fearing smallpox because it has not yet been identified as a true, credible threat."
However, you should be prepared for this to occur, says Felt. "It probably will happen with all the hype on TV," she predicts. If a patient fears smallpox exposure, but there is no clinical evidence to support this, Felt advises assuring patients that there is no reason to believe that they have been exposed and that their symptoms are not consistent with smallpox.
Here are specific interventions to take if you suspect smallpox:
• Determine if the patient actually has chickenpox. You may think that chickenpox is easily confused with smallpox, but there are distinct differences in presentation, according to Maureen Titus, RN, CIC, director of infection control at Carolinas Medical Center in Charlotte, NC. "The smallpox patient has a rash with maculopapular lesions starting on the face and spreading to the truck, legs, palms, and soles," she notes. "The rash progresses uniformly, and all lesions have the same appearance." In contrast, the chickenpox rash starts on the trunk and then spreads to the face, and the lesions are in different stages at the same time on the same area of skin, Titus explains. (See chart for distinguishing between smallpox and chickenpox, below.)
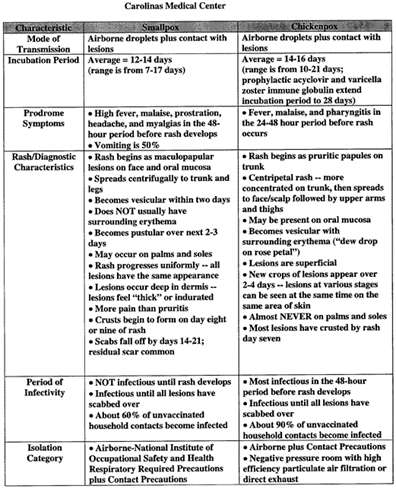 |
Source: Roger D. Lovell, MD, Infectious Diseases and Hospital
Epidemiologist,
Carolinas Medical Center, Charlotte, NC.
A smallpox patient probably would present with a two-day history of fever, malaise, body aches, and also a rash, says Felt. Smallpox rash has fewer lesions on the trunk than the distal extremities and face, she says.
• Look for clues when assessing patient. Matsuoka points to the following epidemiological "clues" pointing to a possible smallpox outbreak:
- a large epidemic with high illness and death rate;
- a predomination of respiratory symptoms;
- sick or dead animals of multiple types.
Immunosuppressed and HIV-positive individuals likely would present with the first cases of smallpox, says Matsuoka. "Like the canaries in the coal mines that were there to detect the presence of gases, these patients are most vulnerable," she says. Consider the following information when assessing a patient for smallpox exposure: infectious contacts, employment history, and activities during the proceeding three to five days. If working up a suspected case, you also should ask about the patient’s travel history, says Matsuoka. "Certainly the department of health would follow up on all contacts, but a preliminary screening of trips would identify the possibility of spread," she adds.
Matsuoka advises having a higher level of suspicion for anyone presenting with flulike symptoms, rash, changes in mentation, or hemorrhagic signs such as bloody conjunctiva, bruising, or bloody stools. However, Matsuoka cautions that these should only be considerations and should not heighten paranoia. "The clinical presentation of a sick patient with flu, rash, and altered mentation would be the red flag," she says.
• Isolate the patient immediately. Smallpox’s primary route is inhalation, and it is highly contagious, says Matsuoka. "There is a 20%-40% mortality rate in unvaccinated victims," she adds. "All contacts are quarantined for at least 17 days. It is infectious until all scabs are healed over." If smallpox is suspected, the patient should immediately be placed on airborne National Institute of Occupational Safety and Health respiratory required precautions and contact precautions, says Titus. "If the patient is at a triage desk or in a common waiting area, he or she should be given a mask to wear and taken to a private room with the door closed immediately," she says.
Next, quickly put the patient in a negative pressure room with high-efficiency particulate air (HEPA) filtration or direct exhaust to the outside, says Titus. Anyone who enters the room must wear a N95 respirator, gown, and gloves, she says. "Dedicated patient equipment also should be placed in the room," adds Titus.
Felt notes that although large hospitals usually have good respiratory isolation rooms, many public and smaller EDs may not. "If that is the case in your facility, you might look into purchasing portable isolation units that provide negative pressure," she suggests.
• Document appropriate information. You must document in the patient’s file, "Highly infectious disease. Strict respiratory and contact isolation," says Felt.
Signs and symptoms of the illness should be documented, along with the time the patient was placed in precautions and who has been notified of the suspicion for smallpox, says Titus. "Also, a list of household and other close contacts should be generated and documented," she adds.
• Contact the appropriate individuals. As soon as you suspect smallpox, contact your hospital epidemiologist and infection control practitioner, says Titus. "They in turn will contact the local and state health departments and the Centers for Disease Control and Prevention [CDC]," she says. (See excerpt of CDC guidelines for smallpox in this issue.)
Law enforcement also will get involved, says Felt. "One case is an epidemic and most certainly a bioterrorist event," she says. Only state public health departments can activate the systems necessary to receive specimens and provide vaccine through CDC, says Felt. "Assume you will get smallpox, and even if you receive vaccine, you might want to be isolated for 15-17 days," she adds. Remind public health and infection control to notify the laboratory, says Felt. "Chickenpox can be ruled out fairly quickly if the patient already has chickenpox history or a varicella immunity. PCR [polymerase chain reaction] of DNA would provide certainty," she says. "You would want to get the patient on an antiviral such as cidofovir as soon as possible."
• If exposed, take necessary measures. Treatment is supportive, and a CDC vaccine and immune globulin is available, says Matsuoka. "No antiviral medication is available. Vaccination is the best means of preventing infection," she says. (See "Do you know how to use PAPRs?" in this issue.) However, there is not a need for ED personnel to be vaccinated against smallpox, she stresses. If there is an exposure, there is emergency vaccine available and you have up to four days to receive it, says Matsuoka. "While there is a 30% mortality with smallpox in the unvaccinated, I agree with the CDC’s position to deploy the stockpile of smallpox vaccine only when necessary," she adds. "This is a surveillance-and-containment’ strategy."
No vaccine is free of side effects, notes Matsuoka. "Besides allergic reactions, there is the small risk of cerebral edema and death," she says.
Sources
For more information on smallpox, contact:
- Sue C. Felt, RN, MS, MPH, CIC, Infection Control, San Francisco General Hospital, 1001 Protreo Ave., Building 100, Room 301, San Francisco, CA 94110. Telephone: (415) 206-5466. E-mail: [email protected].
- Darlene Matsuoka, RN, BSN, CEN, CCRN, Harborview Medical Center, Emergency Department, Mail Stop 359875, 325 Ninth Ave., Seattle, WA 98104. Telephone: (206) 731-2646. Fax: (206) 731-8671. E-mail: [email protected].
- Maureen Titus, RN, CIC, Director, Infection Control, Carolinas Medical Center, P.O. Box 32861, Charlotte, NC 28232. Telephone: (704) 355-2327. Fax: (704) 355-7696. E-mail: [email protected].
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
