Missed injuries: How not to miss the subtle findings
Missed injuries: How not to miss the subtle findings
Jonathan D. Lawrence, MD, JD, FACEP, Emergency Physician, St. Mary Medical Center, Long Beach; Assistant Professor of Medicine, Department of Emergency Medicine, Harbor/UCLA Medical Center, Torrance, California
Editor's Note: As is true in other specialties, emergency physicians (EPs) and nurses encounter certain medical conditions that engender a greater risk of malpractice litigation than others. Traumatic injuries are fraught with complexities that can catch the unaware physician in a malpractice trap. Maintaining an awareness of the pitfalls associated with traumatic injuries is one significant way to reduce the risk of malpractice litigation. To that end, Dr. Lawrence reviews many of the traumatic injuries that can become frequent sources of malpractice claims in the emergency department (ED). — Richard J. Pawl, MD, JD, FACEP
Introduction
Despite modern diagnostic aids, traumatic injuries continue to be missed in the ED. These missed injuries may lead to preventable long-term harm or even death to the patient and thus may become a source of litigation involving the EP and or emergency nurse. Often the emergency practitioner is one of a team caring for a trauma victim and gets caught in the 'shotgun spray' of a lawsuit. Or, the injury is an isolated complaint, appears minor or is subtle, and the subsequent discovery of a missed injury places the EP alone in the cross-hairs of a legal action. Traumatic injuries occur more frequently in young healthy individuals, and therefore, long-term disabilities are likely to cost more in terms of damages. Thus, any strategies that diminish missing traumatic injuries are likely to have disproportionately larger effects in curbing malpractice payments.
Most trauma centers apply extensive imaging of trauma victims at risk for significant injury. The head-to-pelvis scan is certainly becoming more common as trauma surgeons attempt to avoid missing any significant injury and computed tomography (CT) scanners become faster. Extending the CT procedure to include, at least, the cervical spine during CT evaluations for head injuries can be justified because of the increased likelihood of cervical spine injury with head trauma.1 Whether extending this strategy to include scanning the rest of the torso makes sense from a medical or economic standpoint has not been determined. From a medicolegal standpoint only, any strategy that avoids missing injuries requires careful consideration. Thus, the debate surrounding the practice of defensive medicine, its costs, and possible benefits continues.2
Attention to detail and a high index of suspicion remain the EP's best defenses against missing traumatic injuries; careful documentation, as always, remains the best defense in case of a lawsuit. This article addresses the topic of missed traumatic injuries, identifies the high-risk situations where injuries are missed, provides examples of litigation resulting from missed injuries, and discusses strategies for avoiding missing injuries and the litigation that can ensue.
Sources of Malpractice Claims
The landmark study by Karcz and colleagues remains the best source for statistics regarding the incidence and nature of malpractice claims against EPs.3 Because most malpractice insurers consider statistics regarding claims made, expenses incurred, and indemnification payments made to be proprietary information, data of the type included in this study are not otherwise readily available. In reviewing all 549 malpractice claims filed against EPs in Massachusetts from 1975-1993, the study identified the incidence of high-risk and low-risk diagnoses leading to litigation. The terms high risk and low risk were made based upon the total payouts and expenses (e.g., legal fees, court costs, expert witness fees) associated with each diagnosis. High-risk diagnoses included those conditions both occurring uncommonly but with large payouts per claim and those occurring frequently with smaller payments. Using these criteria, high-risk diagnoses included acute myocardial infarction, wounds (e.g., retained foreign bodies, missed tendon or ligament lacerations, and infections), fractures (including spinal fractures with paralysis), pediatric fever/meningitis, abdominal pain, central nervous system bleeding, and epiglottitis. (Author's note: With the widespread use of HIB vaccine, it is unlikely that epiglottitis remains in this high risk group today, and HIB meningitis is undoubtedly decreasing as well.) These high-risk diagnoses accounted for 63.75% of all claims and 64.23% of all payments and expenses. The study noted a trend for fewer claims for missed fractures and wound management.
Litigation related to missed or mismanaged traumatic injury remains problematic in the ED. The following are the major categories of traumatic injuries identified by Karcz and other problematic injuries with examples of each that led to litigation.
Wounds
Wound management litigation accounted for 25.09% of all litigation in the Karcz study before 1988, declining to 14.6% between 1988 and 1993. Despite the high number of claims, payments and expenses amounted to only 3.15% of the total amount spent by the insurance company because of the relatively small amount paid per claim. These mainly involve retained foreign bodies, infections, and missed tendon or ligament lacerations. The EP's best defense is to carefully pursue the possibility of foreign bodies with exploration, direct visualization, and imaging (plain films, ultrasound, CT, or MRI), if necessary. The possibility that a foreign body is in the wound should always be a consideration. A patient's history of a foreign body sensation should always be taken seriously. Likewise, carefully documenting motor and sensory function is vital. When pain or other factors prevent a thorough exam, documentation of the reason for the limited exam and advice to the patient for a repeat exam in the next 1 to 2 days is essential. Ironically, the use of skin adhesives may cause a less careful exploration because local anesthetic is not normally employed. Anesthetizing the wound for exploration partially negates the convenience of the skin adhesives. Nonetheless, the author is unaware of any study documenting an increase in retained foreign bodies since the advent of skin adhesive, although a trend toward increased infection has been noted.4 Regarding infection, documentation of irrigation, debridement when necessary, and administration of antibiotics when indicated for high risk wounds will indicate conformity with the standard of care.
Case #1. H. v. E. Medical Center, et al.5
Mr. H, a 55-year-old man, was working on a ladder when he lost his balance and fell, impaling his inner left upper arm on a fence with pointed 8-cm long finials. He was taken to the ED of the nearest medical center where Dr. J obtained a history and performed an injury-focused physical examination. A large laceration was noted on the medial side of the upper arm. No distal motor, sensory, or motor deficits were noted and documented as such. No x-ray was obtained. Before irrigation and exploration, Dr. J administered midazolam for sedation and closed the wound. Mr. H was referred to his own physician for follow-up. On follow-up, the wound was healing well, and sutures were removed after 2 weeks. During the next several months, Mr. H complained of continuing pain to the left arm at the site of injury. After several more visits to his primary care physician, a referral was made to an orthopedist. He performed an x-ray that revealed an 8-cm long finial imbedded in the patient's inner upper arm. It was removed, and a complete recovery followed. Mr. H sued Dr. J for negligence in not discovering the foreign body. During his deposition, Mr. H admitted that he noted a finial missing from the fence but thought someone had found it and thrown it away. Consequently, he didn't mention it to any of his health care providers. Dr. J's attorneys brought a motion for summary judgment against Mr. H. (A summary judgment means that the judge was asked to dismiss the case because the facts as discovered through deposition, etc., left no controversy to be ruled upon by the jury.) Dr. J prevailed, and the case was dismissed.
Discussion
Missed retained foreign bodies remain a frequent source of malpractice claims, although they rarely lead to high awards. An exception might be a foreign body in the eye leading to visual impairment. EPs can decrease the odds of missing these foreign bodies by considering that every wound may contain a foreign body until reasonably proven otherwise. A careful history may reasonably eliminate the possibility of a foreign body. For example, if the patient states he or she was cut by an intact knife, or on the edge of a piece of glass that did not break, the likelihood of a foreign body is virtually zero. However, in an accident that involved broken glass (e.g., automobile glass shattering in an accident, stepping on glass, or being hit on the head or face by a broken bottle) the likelihood that glass foreign bodies will be in the wound increases. Examination, irrigation, and exploration are the first steps in detecting foreign bodies. Even if a foreign body is discovered using these steps, imaging may be indicated because a second foreign body may be present. Special care must be taken in injuries to the eye where the history suggests a foreign body may be present despite a normal examination. Metallic foreign bodies anywhere in the body rarely pose a problem because they are readily visible on plain films.
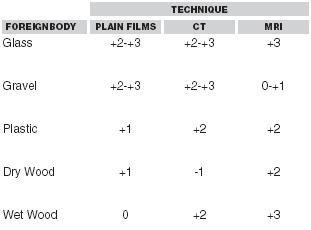
Several studies have explored the imaging modalities best suited for various foreign bodies of other composition. Plain x-rays remain the standard imaging for glass.6 The ability for seeing a glass foreign body is limited by size; approximately 99% of glass foreign bodies 2 mm or larger are seen on plain films. This figure drops to about 60% for glass only 0.5mm in size. There is probably no clinical significance of foreign bodies this small, except in the eye. Plain films also may be helpful for gravel foreign bodies.7 Wood and plastic, being radiolucent, present special problems because plain films are notoriously poor in demonstrating their presence. Ultrasound is advocated by many to detect these foreign bodies. Although a significant improvement over x-rays, false-negative ultrasound results occur in 10% or more of cases.8,9 Ultrasound is much more operator dependent, and its ability to detect foreign bodies is negatively affected by the presence of gas or pus surrounding the foreign body. CT appears to offer no advantage over a combination of plain films and ultrasound. Magnetic resonance imaging (MRI) has been studied as an imaging modality for foreign bodies, and it may best serve as backup in cases where other imaging results are negative in a suspicious wound. MRI was useful in finding most foreign bodies except gravel; it is excellent for glass and wet wooden fragments and good for plastic and dry wooden fragments.10 Table 1 summarizes the relative abilities of different imaging modalities to visualize soft-tissue foreign bodies.
| Table 1. Visualization of Soft-Tissue Foreign Bodies11 |
|
|
Finally, the information given to the patient must be realistic. The patient must be informed that despite all the careful exploration and results from any imaging studies, foreign bodies still may be missed a small percentage of the time. For this reason, follow-up instructions are vitally important. Although most small missed foreign bodies will cause no problems, occasionally infection, pain, or functional disturbances can occur as a result of their retention. Patients must be instructed on the signs and symptoms of infection and given specific follow-up care.
In the case outlined above, Dr. J's attorney argued that Dr. J had met the standard of care because a reasonable EP would not believe a large object, such as an 8-cm long fence finial, could be hidden in a wound without being obvious. However, admitting that he had missed such a large object might prove embarrassing in front of a jury. Additionally, factors here included the failure of Mr. H's subsequent physician to do further studies after a protracted period of pain and the failure of Mr. H to inform his physicians of the missing finial. The decision to file a motion for summary judgment was based upon these last two facts, and Dr. J was successful.
Fractures
Missed fractures constitute another major category leading to potential medicolegal problems for the emergency practitioner. Fractures are missed for a variety of reasons. First, the injured bone may not be x-rayed or suspected of injury. This most commonly occurs in the following conditions: 1) multiple injuries with a painful primary injury distracting the patient and the physician, 2) an alteration in the patient's mental status, or 3) unstable vital signs. Second, the x-ray may be misread either by the EP and/or the radiologist. Third, the x-ray misread by the EP may be read correctly by the radiologist, but a backup system to inform and follow up with the patient may not exist or may malfunction.
Missed fractures that lead to disability have a high potential for damages. Chief among these are fractures across joints leading to immobility and arthritis (e.g., navicular fractures of the wrist, hip fractures, and tibial plateau fractures). By far, the missed fractures with the highest potential for disability are those of the spine with spinal cord damage. Much has been written on the proper imaging strategy for the cervical spine. It is well established that applying a series of low-risk clinical criteria to the patient with blunt trauma can identify a patient in whom plain films of the cervical spine can be safely avoided.12 These criteria include 1) absence of posterior midline tenderness, 2) absence of focal neurological findings, 3) normal level of alertness, 4) no evidence of intoxication, and 5) absence of another painful injury. Patients meeting all these criteria have virtually no chance of a serious cervical spine injury. Six injuries were missed of 818 patients with cervical spine injuries from a larger pool of 34,069 patients with blunt trauma in the NEXUS study.13 A similar study has not been done for the thoracic or lumbar spines, and it is not clear if the criteria are valid for those areas. The incidence of multiple spinal fractures has been studied, supporting the saying: The most commonly missed fracture in trauma patients is the second one. Noncontiguous fractures of the spine occur from 3.2% to 16.7% of the time, with a mean near 8%.14 Disability from cord injury is limited to noncompression fracture injuries. Critical in not missing any fracture of the spine is a high index of suspicion. Documentation of neurological function (whether present or absent)— from the moment the paramedics attend the trauma patient in the field through the ED evaluation and hospital admission —is essential. This documentation, coupled with other information, can prove to a jury that a paralyzed patient had deficits from the moment of injury that were not caused by mishandling by health care providers. Many cases have been lost by testimony that there the patient had extremity movement in the field but a lack of movement in the ED. In some cases, this disagreement requires attempts by the defense attorney to impeach paramedics' testimony, a task most defense attorneys would rather avoid considering the public's positive view of firefighters and paramedics.
Although the NEXUS study was designed to determine when imaging could be safely avoided, it did not address the accuracy of plain films versus CT or MRI in detecting fractures of the cervical spine. CT has definitely been shown to be more accurate than plain films in detecting fractures1 in high energy trauma, but whether these findings have any clinical significance or are cost effective has not been determined. Likewise, MRI has been shown to be more accurate than plain films or CT in finding ligamental injuries (obviously important in cervical spine stability);16 but when to resort to MRI has not yet been determined nor is it feasible in multiply injured patients. The 'bottom line' is still that clinical suspicion should drive the imaging used. The high-risk situation of a patient with altered mental status, other painful injuries, or unstable vital signs should make the clinician very wary of clearing the cervical spine with plain films. (Also, consider that a high percentage of plain films are inadequate because they do not show the entire cervical spine from C1 through T1.) The safest course in the ED remains keeping the cervical spine immobilized unless one can be reasonably certain there is no significant injury.
| Table 2. The NEXUS Criteria for Clearing the C-Spine without Imaging15 |
|
No imaging studies of the cervical spine are needed in the patient with blunt trauma if: |
The concept of the tertiary survey has been developed to avoid missing injuries in the trauma patient.17 After the practitioner ensures the 'ABC's' in the primary survey and examines the patient head to toe in the second survey, in the tertiary survey the patient is reassessed head to toe again after initial stabilization and treatment. Missed injuries were noted in 9% of patients in whom a tertiary survey was performed. This group included 51% with musculoskeletal injuries, spinal fractures in 12%, facial fractures in 5%, thoracic injuries in 12%, abdominal injuries in 15%, and vascular injuries in 5%. Seventeen percent of the missed injuries required surgical treatment.18 Patients at particular risk and whose injuries are often detected on the tertiary survey include the usual suspects: 1) patients under the influence of alcohol and/or drugs, 2) patients with head injuries, and 3) patients with initial hemodynamic instability.
Finally, the use of high-dose steroids in spinal injuries deserves comment. Despite many years where the standard of care required high-dose steroids for spinal cord injury, studies have finally disproven the utility of this treatment and demonstrated the high incidence of serious side effects. EPs should let the attending neurosurgeon make the decision to offer steroids under these circumstances.19-21
Case #2. J.R v. L.A. Medical Center and Dr. B22
J.R., then 17 years old, was the driver of a small car involved in an accident on November 29, 2002. He was wearing a seatbelt, but the car was not equipped with airbags. During the collision, he injured his left hand and wrist but denied any other injuries. He was taken to L.A. Medical Center by the paramedics. There he was seen by Dr. B who noted tenderness and abrasions to the left hand. His chart included a diagram of a hand where he noted an 'X' for abrasions and tenderness in what appeared to be the dorsum of the palm in the area of the second and third metacarpals. X-rays were taken of the left hand and were read as negative by both Dr. B and the reviewing radiologist. J.R.'s hand and wrist were dressed and splinted, and he was referred to his own physician for follow-up. The final diagnosis was sprained left hand.
J.R. went for follow-up to his family physician on December 3 and December 7, 2002, where mild pain was noted. When his wrist continued to be painful, he sought a consultation with an orthopedist. CT imaging showed a non-union of the navicular bone. J.R. subsequently underwent corrective surgery and had some residual limitation of use of the wrist. He sued the hospital and Dr. B for failure to diagnose the fractured navicular bone. The case against both was dismissed after initial discovery failed to find a sustainable case against them.
Case #3. F. v. Dr. M, et al.22
The plaintiff, F., fell off his motorcycle at a motocross competition in the Sierra Nevada in California, injuring his right wrist. Five hours later, he presented to the ED of the small rural hospital closest to the site of the competition. A careful examination of the wrist by Dr. M specifically noted "no snuff box tenderness." X-rays were taken of the wrist and read as negative by the EP and on follow-up reading by the radiologist. F.'s wrist was splinted, and he was referred to his own physician when he returned home to Southern California. During his follow-up visit to his orthopedist, the wrist was x-rayed again, showing a displaced navicular fracture. F. underwent corrective surgery and had some residual wrist pain and limitation of movement. He sued the hospital, EP, and radiologist for missing his fracture. As in J.R. above, this case was dismissed completely after initial discovery failed to reveal a breach of the standard of care and no EP could be found to support F.'s contentions against Dr. M.
Discussion
These two cases underscore the continuing problems posed by this common and sometimes difficult- to-diagnose type of fracture. Classical teaching was that a navicular fracture should be suspected if, in the setting of trauma to the wrist, 'snuff box' tenderness was elicited. In such cases, an x-ray of the wrist (with navicular views) should be obtained. If negative, the wrist should be splinted and the patient referred to an orthopedist for repeat films in 10-14 days when the fracture would be more visible due to new bone growth at the fracture line. If a fracture were still suspected, a bone scan could be performed to detect new bone growth. The danger of this injury is avascular necrosis of the distal bone fragment leading to non-union and loss of wrist function.
A considerable amount of literature has been dedicated to this problem, and controversies still exist as to the proper type and length of immobilization, the clinical signs consistent with the injury, and the proper role of follow-up imaging. A key problem found in all the literature includes not knowing the denominator: How many people suffer this injury and never seek treatment? Additionally, it is un-known how many patients will have poor results despite optimum care or, how many heal well without any care. From the EP's perspective, staying within the established standard of care will be the best defense if a poor outcome occurs. Initial suspicion of the injury should trigger plain films and immobilization whether the navicular bone is broken or not. Referral for follow-up in a timely manner and provision of pain control are other elements considered under the standard of care.
Initial suspicion of the injury should be raised not only by the presence of snuff box tenderness but also by a positive compression test (in–line compression of the thumb along its axis eliciting pain). Nevertheless, clinicians should be aware that no good data exist to support the notion that these signs are more common in patients with navicular fractures than those without fractures.23 Nonetheless, a plaintiff's attorney will be looking for some documentation of at least the presence or absence of the snuff box tenderness. In the J.R. case, the documentation of pain away from the snuff box was a major factor in support of Dr. B's compliance with the standard of care and success in being dismissed.
Initial imaging includes a four-view wrist series (i.e., standard wrist series plus a navicular view). Controversy exists as to how many plain films are falsely negative, but the literature often cites the number as 40%.24 Whether the EP reads his or her own films, and regardless of a positive or negative result, the wrist should be immobilized pending further investigation. Patients with definite fractures need a referral to an orthopedist. Immobilization will avoid any accusation of the fracture worsening as a result of ED care. Patients whose initial x-rays are negative need immobilization until a fracture is ruled out for the same reason. These latter patients, however, can be referred to a primary care provider for the follow-up imaging. It is becoming evident that MRI is the best imaging modality for viewing a navicular fracture.25,26 CT is also useful, and both are replacing bone scanning. EPs do not have to concern themselves as much with this aspect of care, only that the patient must be fully informed as to the need for the follow-up studies.
Dr. B. was not found not liable because he documented the absence of pain in the anatomical snuff box, immobilized the wrist despite a negative x-ray, provided pain medication, and referred J.R. to his own physician for follow-up care.
Dr. M, likewise completely followed the standard of care and, despite the annoyance of being named in a law suit, was dismissed.
Lacerated Tendons and Nerves
Missed lacerated tendons and nerves carry the possibility for significant disability, and, therefore, are potential sources of malpractice awards. One of the most difficult tasks in emergency medicine is to fully examine the motor, vascular, and nerve function of an acutely injured extremity. A complete examination is often difficult in the anxious patient suffering from an acutely painful condition. If the patient is also intoxicated, the task is nearly impossible. Nonetheless, documentation of a complete functional exam or the reasons why a complete exam cannot be performed is essential. If a complete exam cannot be performed, the patient must be informed of the possibility of missed injuries and be referred for a repeat exam within the time frame when the injuries can be repaired without further long-term damage. Also the injured part must be immobilized pending a repeat exam.
A patient who has a normal motor, sensory, and vascular examination carefully documented but is later noted to have deficits and found at surgery to have a lacerated tendon or nerve is puzzling. The possibilities include 1) the exam was not done, 2) the exam not done carefully enough to appreciate the injury, or 3) the injury occurred after leaving the ED. There is no excuse for the first of these possibilities; an incomplete exam because of pain or anxiety has been discussed. A careless exam has no place in the ED. The possibility of delayed rupture of the tendon or nerve is the way most of these cases are defended when litigation occurs. A delayed rupture of a partially lacerated tendon is theoretically possible and no doubt occurs although its incidence is unknown. (Partial and complete Achilles, biceps, and quadriceps tendons from closed traumatic injuries are well known but not the subject of this article.) It is harder to theorize how a partially lacerated nerve, which is not under the same stresses as a tendon, can likewise rupture, or how a partially lacerated nerve would not have symptoms at the time of initial treatment.
Clinicians must be aware of the referral times in their own practices. EPs can repair extensor tendons in the hand but are usually not qualified to repair flexor tendons. Therefore, EPs rely upon specialist referrals for these injuries. While it is acceptable for tendon repair to be delayed for a few days with no loss of functionality, a physician who is aware that repair will be unduly delayed because of any number of logistical problems (e.g., insurance status or availability of specialists), may be asked why primary repair wasn't considered. Unfortunately, EPs are sometimes unfairly asked to bear the brunt of a dysfunctional medical care delivery system.
Case # 4. R. v. S.M. Regional Medical Center27
R., a 9-year-old male, was cut on his right calf while 'fooling around' with a kitchen knife. He was taken to S.M. Regional Medical Center by his mother. His leg was examined by the triage nurse, treating nurse, and EP, all of whom documented normal distal motor, vascular, and sensory function. The wound was cleansed and stapled. It was checked 2 days later by R.'s family physician, and the staples were removed the next week. During these visits, no complaints were voiced. Later— more than 2½ months after the injury— R. saw his primary care physician complaining of numbness in the right foot without any documented motor or sensory deficits. Two months later he presented again, this time with right foot drop. Neurology referral revealed a right peroneal neuropathy. R.'s mother sued the EP and the hospital for missing a peroneal nerve injury at the time the laceration was sutured. After discovery, the case was dropped by the plaintiff. The principal reasons cited were the good documentation by all the practitioners of the normal motor and sensory exam, the diagram by the EP in the chart that the laceration wasn't near the peroneal nerve, and the admission during deposition by R. that he would frequently injure his legs while performing skateboard jumps, even after the laceration was repaired.
Discussion
One can easily see how this case may have ended differently without the good documentation by the emergency nurses and physician and the honest admissions by a young plaintiff. Such admissions aren't always going to happen, therefore, the best defense is always careful documentation.
Intracranial Hemorrhage
Missed traumatic intracranial hemorrhage has a very high potential for litigation because of its associated disability and death. Some of the largest malpractice awards go to plaintiffs who must have 24-hour care for prolonged periods. Performing CT scans on blunt head injured patients has become so ubiquitous in the United States that much of the current literature is focused on the question: When it is permissible not to order a CT in a head injury? Virtually all head trauma patients with a Glascow coma scale score less than 15 are routinely scanned. Litigation is more likely to occur as a result of delays in treatment rather than failure to order CT imaging. An example would be the intoxicated patient whose altered mental status is attributed to the effects of drugs or alcohol rather than trauma. When the patient doesn't regain normal consciousness within the expected time, CT imaging then is ordered. If an intracranial hemorrhage is noted and a poor outcome ensues, litigation can be the result.
'Dueling' criteria purport to allow the clinician to avoid CT scanning in minor head injury patient under certain circumstances. Note that neither set of rules applies to the young child. (See Tables 3 and 4.)
|
|
In comparing the two rules, one problem immediately noticeable is that they aren't dealing with the same set of patients. Most clinicians would not classify a patient with a GCS score of 13 to be 'minor' as is done using the Canadian rule. However, the New Orleans rule is so inclusive of all head trauma patients that it does not reduce the number of CT scans done. Using either rule, practitioners indeed will find the head injury needing surgical intervention, but in one study, use of the New Orleans rule only reduced the number of scans by 3-5%.29
Other investigators have questioned the use of these rules outside the health care systems that developed them.30 Neither set of rules deals with patients taking anticoagulant medications. Although some studies report no greater incidence of intracranial hemorrhage in these patients,31 others disagree and find an increased risk.32,33
Case #5. F.A. v. A.G. Hospital34
F.A., an 85-year-old male taking digoxin and warfarin for chronic atrial fibrillation, suffered a nonsyncopal fall when he tripped over a low barrier in a parking lot. He hit his head and sustained a laceration to his scalp and an injury to his right wrist. There was no loss of consciousness. He was taken to A.G. Hospital and was evaluated by the EP. The scalp laceration was sutured, and the right wrist was x-rayed and showed no fracture. The patient was sent home with no change in his mental status. Three hours after arriving home, the paramedics were called to the house when F.A. had a decrease in mental status and a seizure. He was taken to another facility where a large subdural hematoma was identified. Surgery was delayed until the next morning because the neurosurgeon attempted to normalize the prothrombin time through administration of fresh frozen plasma. F.A. died after surgery without ever regaining consciousness. F.A.'s estate sued A.G. Hospital and the EP for wrongful death. After initial discovery, the hospital and EP settled before trial.
Case #6. J. v. H.M.H.P. Medical Center35
J, a 55-year-old female, was the driver of a car hit from behind. She was brought to H.M.H. P. Medical Center by ambulance complaining of pain to the right shoulder and right upper back. She denied head trauma. She had a history of a mitral valve replacement and was taking warfarin. The physical examination revealed only minor musculoskeletal injuries. An x-ray of the right shoulder was taken and was normal. She was discharged to the care of her private physician. On her first follow-up appointment two weeks later, she complained of a cough and was prescribed azithromycin for bronchitis. Days later, she saw her physician again and complained of a migraine headache, although she had no history of migraines. She was treated symptomatically. Four days later, she returned complaining of a worsening headache. She was sent to H.M.H.P. Medical Center for further evaluation. J.'s protime was 7.1 INR, and a CT scan showed bilateral subdural hematomas. She recovered with minimal disability, but sued the hospital and EP for failure to diagnose her intracranial hemorrhage. After discovery, the hospital and physician were dismissed from the suit, which continued against J.'s primary care physician.
Discussion
As noted previously, it is rare that a head trauma patient in the United States doesn't get CT imaging. Intracranial hemorrhage continues to be missed for much more subtle reasons. One reason may be that the history of trauma is not obtained or may be so trivial as to not be deemed significant, certainly a factor in Case #5. The fall was nonsyncopal, and the injury appeared minor. However, two factors should have prompted the EP to order brain imaging: 1) the elderly are at increased risk because of cerebral atrophy, and 2) the risk that the bridging veins may rupture with even minor trauma. Secondly, F.A. was taking warfarin, which meant that if bleeding occurred it may not stop spontaneously. A factor to be considered and an unknown is how long it takes for blood to accumulate in the subdural space in the anticoagulated patient. Bleeding while taking warfarin is generally slow and oozing. If the bleed is slow, CT imaging obtained early after the trauma may not show any abnormality. It was this logic that led A.G. Hospital's counsel to be able to negotiate a lower settlement.
In J. v. H.M.H.P. Medical Center there was no history of head trauma at all. The damage to the car was minimal, and the examination revealed no injury to the head. This type of patient would not receive CT imaging using either the New Orleans or Canadian criteria. Only the most cautious EP would image J.'s brain solely because of the history of warfarin use. The symptoms of the subdural hematoma were not evident until nearly a month after her accident. J.'s highly elevated INR of 7.1 was probably as a result of her use of azithromycin , which interfered with warfarin metabolism. H.M.H.P. Medical Center's attorney used these facts to negotiate a dismissal in exchange for waiver of costs.
The bottom line on minor head trauma is to be cautious with the elderly and those with special medical problems. If imaging is not done, or if it is done and interpreted as normal, documentation and follow-up examinations remain the cornerstones of litigation prevention. Strategies in pediatric head trauma are similar, but the criteria for imaging are not as well established. The additional problem of sedating children for CT imaging poses more opportunities for therapeutic misadventures.
Missed Internal Abdominal Injuries
Although trauma care has made tremendous advances during the last 30 years, certain injuries remain difficult to diagnose and can be disastrous when missed. Chief among these are ruptured hollow viscus injuries. These injuries do not produce immediate symptoms, are difficult to visualize with current imaging techniques, and may cause serious infections often leading to death. Ironically, before CT imaging of every serious trauma victim became routine, ruptured viscus injuries had a better chance of early discovery. In the days of early exploratory surgery and diagnostic peritoneal lavage, bowel contents could either be discovered upon direct visualization or in the lavage fluid. Reliance upon CT imaging misses many of these injuries.35 Likewise, injuries to the pancreas, diaphragm, and bladder are diagnostic challenges. The EP's role in the treatment of the severely injured patient is often peripheral to that of the surgeon who admits the patient. Thus, even if named in a suit because of a poor outcome or missed injury, the EP will not likely be found liable. More legally important for the EP are the victims of minor trauma who are sent home and later discovered to have intra-abdominal injury.
In the absence of other serious injuries, certain findings should lead the clinician to order, at a minimum, imaging of the abdomen. Diffuse abdominal tenderness, the presence of a 'seatbelt' sign and costal margin tenderness, especially with radiation of pain to the shoulders, are all associated with an increase in intra-abdominal injuries. The FAST exam (ultrasound) should be able to detect free fluid and blood around the liver or spleen. Free fluid on ultrasound or CT imaging has been associated with increased risk of injury.36 The seatbelt sign has been associated with an increased risk of intra-abdominal injury.37 Because approximately one-third of patients with this finding will have a significant injury, it poses a high enough risk that a surgical consultation should be considered, even if the patient is otherwise stable. Costal margin tenderness also is associated with increased risk of solid organ injury.38 EPs should have an increased suspicion for a delayed rupture of the spleen. It probably represents a subcapsular hematoma sustained at the time of injury that ruptures causing hemodynamic instability days to weeks after even minor trauma.39-40 Clinicians should be alert to this injury in participants of contact sports, where medical attention is often delayed.
Case # 7. J.G. v. V.H. Hospital, et al.41
J.G., a 17-year-old football player was 'speared' in the abdomen (tackled by ramming with the helmeted head) during a high school game and was taken by the coach to V.H. Hospital. There, Dr. C. examined him and noted pain and tenderness to the lower left anterior ribs but otherwise J.G's vital signs were stable. A chest x-ray was taken, and Dr. C. noted a possible rib fracture in the area of tenderness. J.G. was given an injection of meperidine and promethazine, a prescription for hydrocodone/APAP, and discharged to home with the diagnosis of rib fracture. The next morning, J.G. had a syncopal episode and was taken to another hospital where the ruptured spleen was diagnosed. There, he was taken to surgery, bleeding was controlled, and he recovered uneventfully without a splenectomy. J.G.'s parents sued V.H. Hospital and Dr. C. for failure to diagnose the ruptured spleen.
After discovery, the plaintiffs dropped the suit for lack of damages. Remember that for a malpractice action to be successful the plaintiff must show that the defendant had a duty to the plaintiff, that the duty was breached, and, that as a result of the breach, damages were suffered. J.G. suffered no damages as a result of Dr. C.'s actions. His pain was the result of injuries sustained in a football game, not at the hands of Dr. C. He would have required the same medical care including surgery had his splenic rupture been diagnosed earlier. (It remains possible that the spleen hadn't ruptured until the morning after the game.) He didn't miss any more school than he would have if his splenic injury been discovered earlier. Finally, his spleen was not removed, thus sparing any immune system problems that might have been anticipated with a splenectomy.
Case #8. M.M. v. L.R. Medical Center42
M.M., a 19-year-old male was trying out his new dirt bike on a city street when he lost control and flipped off the bike, sliding under a nearby stationary car. The paramedics noted an obvious open left tibial/fibular fracture. The leg was splinted, and M.M. was given 10 mg of morphine by the paramedics for pain. He was transported to L.R. Medical Center. In the ED, the only injuries described were the obvious leg injury and abrasions to the right arm and hands. His mental status was described as awake, alert, and oriented. Evaluation included normal laboratory and normal urine test results and a normal chest x-ray. A repeat abdominal exam was documented as normal. M.M. was taken to the operating room for open reduction, internal fixation of the leg fractures. The next morning, M.M. was noted to be acidotic and hypotensive. CT imaging of the abdomen revealed a ruptured stomach and interrupted celiac plexus. He was taken back to the operating room, where his injuries were repaired. His postoperative course was stormy with pulmonary emboli and multiorgan failure. He died on the fourth postoperative day. His family brought an action against L.R. Medical Center and the EP for wrongful death. The defendants settled for an undisclosed amount before trial.
This case illustrates many of the points discussed above. Although the orthopedic injury was the most obvious one, another concern in the ED should have been the evaluation of the abdomen in a patient with major trauma, who had received morphine in the field, and who had a painful distracting extremity fracture. These facts were more important because the patient was going to the operating room where he was going to be unconscious and his abdomen could not be re-examined frequently. Although the NEXUS criteria were not designed for evaluation of abdominal trauma, the same principles apply. Not only was the patient given morphine, but he also had a distracting painful orthopedic injury. These facts should have led the clinicians to at least consider scanning the chest and abdomen before going to the operating room. The same would not be true if the mechanism of injury involved only the extremity. Mechanisms involving significant force (e.g., a driver thrown from a motorcycle) should make EPs very cautious and conservative in their work-up.
Conclusion
Recurrent themes for injuries missed in the ED are lack of suspicion and lack of documentation. Injuries are not suspected when the history and clinical exam are not suggestive. EPs and emergency nurses should keep a high index of suspicion in those dangerous clinical situations involving a significant mechanism of injury, in a patient with an altered sensorium, or in a patient with an obviously painful primary injury. Suspicion also should be increased in situations where retained foreign bodies can occur, and imaging best suited for the suspected foreign body should be considered. Even the best clinicians still can get into legal 'hot water' if they don't document their findings or don't give appropriate aftercare instructions with a specific time for follow-up and specific reasons to return to the ED.
Endnotes
1. McCulloch PT. Helical Computed Tomography Alone Compared with Plain Radiographs with Adjunct Computed Tomography to Evaluate the Cervical Spine After High-Energy Trauma. J Bone Joint Surg (American) 2005;87(11):2388-94.
2. Schriger DL, Brown TB. Decisions, Decisions, Emergency Physician Evaluation of Low Probability-High Morbidity Conditions. Ann Emerg Med 2005.46(6).
3. Karcz A, et al. Malpractice Claims Against Emergency Physicians in Massachusetts: 1975-1993. Amer J Emerg Med 1996;14;341-5.
4. Hollander, J.E., Singer, A.J., Laceration Management. Ann Emerg Med 1999;34 356-367.
5. H. v. E. Medical Center, et al., Riverside Superior Court, California
6. Courter BJ. Radiographic Screening for Glass Foreign Bodies: What Does a "Negative" Foreign Body Series Really Mean? Ann Emerg Med 1990;19(9):997.
7. Russell RC, et al. Detection of Foreign Bodies in the Hand. J Hand Surg 1991;16A(1):2.
8. Jacobson JA, et al. Wooden Foreign Bodies in Soft Tissue: Detection at US. Radiology 1998;206(1):45.
9. Crawford R, et al. Clinical Value of Ultrasonography in the Detection and Removal of Radiolucent Foreign Bodies. Injury 1989; 20(6):341.
10. Russell RC, supra.
11. Russell RC, supra.
12. Hoffman JR, et al. Validity of a Set of Clinical Criteria to Rule Out Injury to the Cervical Spine in Patients with Blunt Trauma. NEJM 2000; 343(2):94.
13. Hoffman JR, supra.
14. Keenen TL, et al. Non-Contiguous Spinal Fractures. J Trauma 1990; 30(4):489.
15. Hoffman JR, supra.
16. Hogan GJ, et al. Exclusion of Unstable Cervical Spine Injury in Obtunded Patients with Blunt Trauma: Is MR Imaging Needed When Multi-Detector Row CT Findings Are Normal? Radiology 2005;237(1):106.
17. Enderson BL, et al. The Tertiary Trauma Survey: A Prospective Study of Missed Injury. J Trauma 1990;30(6):666.
18. Enderson, BL, supra.
19. Canadian Association of Emergency Physicians, Steroids in Acute Spinal Cord Injury. Ca J Emerg Med 2003;5(1):9.
20. Hurlbert RJ, The Role of Steroids in Acute Spinal Cord Injury: An Evidence Based Analysis. Spine 2001;26(24S):539.
21. Nesathurai S. Steroids and Spinal Cord Injury: Revisiting the NASCIS 2 and NASCIS 3 Trials. J Trauma 1998;45(6):1088.
22. R v. L A. Medical Center, et al. Los Angeles Superior Court, CA
23. F. v. M, et al. San Bernardino Superior Court, CA
24. Waizennegger M, et al. Clinical Signs in Scaphoid Fractures. J Hand Surg 1994;19B(6):743.
25. Breederveld RS, et al. Investigation of Computed Tomographic Scan Concurrent Criterion Validity in Doubtful Scaphoid Fracture of the Wrist. J Trauma 2004;57(4):851.
26. Brydie A, et al. Early MRI in the Management of Clinical Scaphoid Fracture. Brit J Radiology 2003;76:296.
27. R. v. S.M. Regional Medical Center, Riverside County Superior Court, CA
28. Stiell IG, et al. The Canadian CT Head Rule For Patients With Minor Head Injury. Lancet 2001;357:1391.
29. Haydel MJ, et al. Indications for Computed Tomography in Patients With Minor Head Injury, NEJM, 2000;343(2):100.
30. Smits M, et al. External Validation of the Canadian CT Head Rule and the New Orleans Criteria for CT Scanning in Patients With Minor Head Injury. JAMA 2005;294(12):1519.
31. Rosengren D, et al. The Application of North American CT Scan Criteria to an Australian Population With Minor Head Injury. Emerg Med J Australasia 2004;16(3):195.
32. Garra G, et al. Minor Head Trauma in Anticoagulated Patients, Acad Emerg Med 1999; 6:121.
33. Li J, et al. Mild Head Injury, Anticoagulants and Risk of Intracranial Injury. Lancet 2001;357:771.
34. F.A. v. A.G. Hospital, et al., Orange County Superior Court, CA
35. J. v. H.M.H.P. Medical Center, Orange County Superior Court, CA
36. Malhotra AK, et al. Blunt Bowel and Mesenteric Injuries: The Role of Screening Computerized Tomography. J Trauma 2000;48:998-1000.
37. Cunningham MA, et al. Does Free Fluid on Abdominal Computed Tomographic Scan After Blunt Trauma Require Laparaotomy? J Trauma 1998;44(4):599.
38. Chandler CF, et al. Seatbelt Sign Following Blunt Trauma Is Associated With Increased Incidence of Abdominal Injury. Am Surg 1997;63:885.
39. Holmes JF, et al. Do All Patients With Left Costal Margin Injuries Require Radiographic Evaluation for Intra-abdominal Injury? Ann Emerg Med 2005;46(3):232.
40. Kluger Y, et al. Delayed Rupture of the Spleen: Myths, Facts, and Their Importance-Case Reports and Literature Review. J Trauma 1994;36(4):568.
41. J.G. v. V.H. Hospital, Los Angeles Superior Court, CA
42. M.M. v. L.R. Medical Center, Ventura County Superior Court, CA
Despite modern diagnostic aids, traumatic injuries continue to be missed in the ED.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.