Patient Safety in Emergency Care Transitions
Patient Safety in Emergency Care Transitions
Authors: Zachary F. Meisel MD, MPH, Assistant Professor, Department of Emergency Medicine, Pennsylvania Hospital, University of Pennsylvania School of Medicine, Philadelphia; and Charles V. Pollack, MD, MA, FAAEM, FACEP, Chairman, Department of Emergency Medicine, Pennsylvania Hospital, Associate Professor of Emergency Medicine, University of Pennsylvania School of Medicine, Philadelphia.
Peer Reviewer: Shawna J. Perry, MD, FACEP, Associate Professor, Assistant Chair, Director of Clinical Operations, Department of Emergency Medicine, University of Florida Health Science Center, Jacksonville.
Case Study
A 75-year-old woman with a chief complaint of chest pain is brought to a university emergency department (ED) by a city-run emergency medical systems (EMS) service. The paramedic gives a verbal bedside report to the ED nurse, noting in the history that the patient's family stated that she had been at bed rest for the previous five days after straining her back. Her chest pain—a new symptom—started two hours ago. The paramedics return to their station-house where they complete the prehospital record. It includes notations of a pulse rate of 120 beats per minute and a pulse oximetry reading of 91%. The prehospital record does not arrive at the receiving hospital until the following day. Meanwhile, back in the ED, the nurse records a normal set of vital signs and a chief complaint of chest pain, but fails to note the recent history of decreased mobility. The patient, Mrs. Smith, is evaluated by a medical house officer who notes a story of new exertional chest pain with shortness of breath, and also notes from the patient's old records the additional history of an abnormal cardiac stress test in the past year. The resident presents the case to the ED attending. They review the patient's electrocardiogram together and note new nonspecific T wave abnormalities in the anterior and inferior leads. The physicians order aspirin, beta blockers, nitroglycerine paste, a chest radiograph, and cardiac biomarkers, and decide to admit the patient for inpatient care. As an admission diagnosis, the resident enters "chest pain, rule out acute coronary syndrome." The patient is taken to radiology by hospital transport. When she returns, she is placed in a different room in the ED and she is not placed back on a cardiac monitor, despite a recurrence of her tachycardia. At nursing change-of-shift, Mrs. Smith's nurse gives verbal report to the oncoming nurse who will be taking the assignment. It is noisy and busy during this time, as many nurses are performing similar sign-outs in the same area. Nursing sign-out is interrupted twice by a patient requesting a cup of ice. At the same time, the resident presents the patient as a moderate risk cardiac chest pain to the admitting house officer on the telephone, and the ED attending calls the hospitalist and reports the admission of a chest pain patient and a plan of action including evaluation for possible coronary angiography the following day. As there are no monitored beds available in the hospital, Mrs. Smith boards as an inpatient in the ED for the night. The admitting resident notes some transient tachypnea while evaluating the patient and plans to discuss it when she rounds with the hospitalist attending, but does not mention this to the ED attending. A new ED attending arrives, and the first attending provides his replacement with a verbal summary of all the patients under his care at the white-board in the center of the ED. They almost skip Mrs. Smith because she had been moved once again to another new ED room and is now an inpatient. On his way out, the first attending turns back and states: "Oh yeah, Mrs. Smith is a rule-out MI who has already been admitted." The next day, the patient is still in the ED. Three sets of cardiac markers are negative. The house team decides to discharge the patient home from the ED after scheduling a follow-up cardiac stress test. She has to wait an additional two hours for her son to borrow a neighbor's van in which to drive her home. During that time, she asks the nurse if she can have any pain medications for her back, but is told that she has been discharged and that she can take acetaminophen or ibuprofen at home. She is taken home with discharge papers and placed back in bed, complaining to her family that her chest is "OK" but that her upper back has "really started to hurt" again. The next morning she returns to the same ED, by ambulance in cardiac arrest, found at autopsy to be secondary to a massive pulmonary embolism.
Introduction
Transitions among providers and site of service are commonplace in contemporary medical care. They involve the transfer of information, responsibility, and authority, even though these exchanges may not be explicitly recognized by the caregivers involved. By definition, transitions involve an interruption of continuity of care. These gaps commonly are viewed as significant sources for medical error.1
As exemplified in the clinical scenario presented, poorly coordinated or ineffective transitions may negatively impact patient safety and quality of care. In particular, certain aspects of patient-related transitions have earned recent scrutiny and focus within the patient safety movement. The Joint Commission on Accreditation of Healthcare Organizations (JCAHO) added to its patient safety goals for 2006 an explicit direction to improve handoff communications.2
The Institute of Medicine (IOM) in its 1999 report "To Err is Human" cited the ED as the hospital location with the highest proportion of negligent adverse events.3 Emergency medical care, in particular, routinely involves multiple transitions in care for any given patient. EDs are designed as transfer stations for patients who ultimately are bound for hospital admission, transfer to yet another health care facility, or discharge back home. In addition, nearly all EDs are staffed with personnel, including physicians, who work in shifts. Therefore, responsibility and information related to patient care routinely are passed, internally and externally, from one health care provider to another during emergency medical care.
The weak links that these transitions represent in the continuum of care largely have been studied outside of emergency medicine environments. Many of the insights and lessons from this growing body of literature, however, can inform the practice of emergency medicine. In addition, certain aspects of transitions are unique to emergency care, not least of which is the sheer number of transitions through which any given ED patient must pass. Also complicating emergency transitions are the staggered timing of shift changes and the infrequency of multi-disciplinary signouts. The purpose of this review is multifold. First, it will examine what currently is known about care transitions in non-emergency care environments. Second, this article will examine transitions within EDs, exploring what makes emergency care transitions unique. Last, it will identify tools and strategies—and the evidence behind these efforts—that may be used to improve patient safety during ED transitions.
Communication
Among studies that evaluate patient care across transitions, the quality with which information is transferred has received the greatest scrutiny by far. Communication in health care occurs via verbal, electronic, and written means. One of the most widely used but least understood methods in communication is the sign over for the transition of care. Alternately called the sign-out, the handoff, handover, or report, this routine allows providers to transfer patient information, responsibility, and authority to their colleagues. Information that is transferred during transitions may include specific patient data, status of the health delivery system (i.e., no ICU beds available), and specific tasks that need to be completed. Responsibility is the assumption of accountability for the work that needs to be done for the patient and is paired with the authority to act as a caretaker and advocate for the patient.
Nurses, attending physicians, and resident physicians classically perform the handoff with similar types of caregivers. However, in the ED, this transfer of information can cross disciplines: for example a paramedic will handoff a patient to a physician, or an ED resident may give report to a hospitalist attending physician. The handoff is used to bridge the natural gaps or discontinuities that arise when a new provider assumes care of the patient.1 It is also a process that can result in adverse events when clinical information is not communicated properly.
Failures of communication are considered to be among the most common factors contributing to adverse events in all medical settings.4-6 Eighty-four percent of root causes of sentinel events reported to the JCAHO from multiple health care settings in 2002 were deemed at least in part due to a "breakdown in communication."7
Missing clinical information has been shown to be common at all levels of care. Up to 14% of all primary care visits involve missing clinical information: verbal, electronic, and written.8 One study surveyed Ohio family physicians, finding that 15% of all reported errors in primary care were associated with missing clinical information at the time of primary care evaluation.9 Similarly, multiple studies have shown that important clinical information—such as medication lists, test results, and follow-up plans—routinely is lost at the time of discharge from various inpatient settings.10-12 Lack of clinical information at the time of patient evaluation in an ED has been shown to be a particularly pervasive problem. One study evaluated 1002 ED visits and found information gaps in 29% of the documented care. The missing information was deemed to be essential to care in 47% of the patients.13
Within the health care setting, most studies of nursing sign-overs have been performed in intensive care unit (ICU) settings. Handoffs among medical and surgical residents who cover admitted patients for each other at night also have been studied. In addition, handovers in the ED have been subject to limited but insightful analyses. Finally, handoffs have been studied closely in non-health related occupations. These investigations and their conclusions will be discussed later in this review.
Handoffs in Non-Health Care Related Domains
High-risk transitions are not unique to health care. Exchanges of information, responsibility, and authority occur in many twenty-four hour operational industries outside of health care. Workers in the aerospace, nuclear power, and marine transportation industries routinely participate in such procedures. Lardner conducted an extensive review of shift changeovers in high-risk industrial processes in which multiple adverse events (some leading to human injury) were evaluated for miscommunication at the shift handoff.14 Both effective communication of poor information and ineffective communication of good information were found to be root causes of these incidents. Larder makes four recommendations that could be used to improve the quality of the handover and limit adverse outcomes secondary to communication errors. Handovers should:
- be conducted face to face;
- be a two-way exchange, with both participants taking joint responsibility for ensuring accurate communication;
- use verbal and written means of communication; and
- be given as much time as necessary to ensure accurate communication.
When these best practices are applied to high-risk industrial shift handovers, the incidence of errors and of injuries are significantly reduced.14
In a study of NASA Space Shuttle mission control shift change handoffs, Patterson et al identified and explored the consequences of three problems that potentially afflict the receiver of information at the shift turnover: failing to be told, misunderstanding the information, or forgetting information during the switch.15 The costs of these errors were significant and included:
- being unaware of significant data;
- being unprepared to deal with the impact of previous events;
- failing to anticipate future events;
- dropping or redoing activities that are in progress; and
- creating unwarranted shifts in goals, decisions, and plans.
The authors conducted a follow-up study in which shift handovers in nuclear power plants and in ambulance and railroad dispatching centers also were observed. They identified specific strategies that routinely are used by these high-risk industries to limit error.15 The potential role for these tools in emergency care transitions will be discussed later.
Inpatient Nursing Handoffs
Observations of nursing handovers have been published since at least the 1970s. These investigations far outnumber studies of physician signovers and have been more comprehensive in their scope. Written and verbal reports are routine for most inpatient nursing handoffs.16 In addition to communicating medical information, researchers have established that nursing handovers have ritual significance (for example, some nurses wait to receive a verbal report before beginning work), organizational functionality, and team-building functions.17
Researchers have identified certain problematic aspects of the traditional nursing handover. One study noted that nearly half of the content of the average handover was specifically unrelated to any nursing needs.18 In addition, of a cohort of handovers assessed, researchers found that these reports tended to underplay the significance of certain clinical features, giving the oncoming nurse a falsely reassuring bias about the condition of the patient.19
A unique aspect of the nursing signover is the high degree of socialization incorporated into this activity. Nurses may use the handover process to assess each other's work.16 This may put pressure on them to perform and can affect the content of the presentation. One study found that nursing handovers in elderly care were rapid, formulaic, and highly jargonized. In addition, the documentation at handover did not always reflect the content of the verbal handoff.16 Problems in nursing handovers can lead to adverse events, most commonly related to the administration of medications. Nursing change of shift was identified as contributing to nearly half of the adverse drug events (ADEs) in a retrospective study at a large Texas hospital.20
Despite the potential problems associated with nursing handovers, ethnographic studies of these turnovers have shown that, for the most part, these rituals are efficient, comprehensive, effective, and performed with relative ease.21 A study of the handoff in a busy ICU found that they were fluid, patient-focused, and seamless processes in which the extent and detail of the reports addressed the specific nursing needs for each individual patient.22 A British study evaluated six nursing shift handovers on a general medical ward and found that, in addition to exchanging patient information, nurses used the ritual to engage in team building and to reinforce cohesiveness within the team.23 In summary, nursing handovers are an essential, complex, and highly ritualized practice that, most often, meet the needs for the oncoming nurse to take care of his or her patient. However, even under the best of circumstances, the handover also is a process that is vulnerable to interruptions, inconsistencies, and subjectivity. A poor handoff has direct patient safety consequences and particular relevance to emergency care situations.
Resident Sign-Out
Increased scrutiny on house-staff work hours has resulted in changes in the division of labor for resident physicians taking care of patients. To comply with American Council on Graduate Medical Education (ACGME) regulations that limit the total and consecutive hours of hospital duty, many training programs have adopted a type of shift work model in which certain physicians take care of patients during the day and then sign out the patient in the evening to a night-float team. The sign-out involves the transfer of both patient care information and responsibility to another physician.24,25 Because residents have been moving toward a shift-work model that is not unlike what has long been done in EDs, data from studies that evaluate transitions for house-staff can help inform understanding of similar processes in EDs, including departments that do not utilize residents.
Resident sign-out is divided into two general categories. Cross-coverage is a temporary place-holding procedure in which a resident who has primary responsibility for the patient temporarily transfers patient care to another resident, with the plan that the original resident will resume active care of the patient when he or she returns to the hospital, often the following morning. Sign-over is a process that occurs when a new resident takes over the primary and active care for a patient, usually from a night-float admitting resident. The increased use of these procedures over the past 10 years among hospital-based house staff has provided observers with the opportunity to conduct natural experiments in process-improvement and patient-safety evaluation. These studies have yielded interesting findings.26,27
Handoffs among residents have been identified as common root causes of preventable adverse events. When 821 residents from multiple training programs at the Massachusetts General Hospital were surveyed on adverse events and their causes, 15% identified "problems with the handoff" as the leading factor perceived to contribute to mistakes in patient care.28
Cross coverage, in particular, has been shown to be strongly associated with preventable adverse medical events. Petersen et al conducted a case-control study of more than 3,000 nonsurgical patients. In a multivariate analysis of 32 candidate variables, cross-coverage was one of only three factors that independently correlated with preventable adverse events (odds ratio 6.1).29 In another study of internal medicine house staff cross coverage, omitted content (such as medications, problem lists, and pending tests), as well as poor process execution (such as lack of face-to-face sign-out) were identified as major causes of failed communication.30 Another study noted that cross-covering residents in a community internal medicine program often made medical decisions without using or reviewing the patients' charts.31 Finally, in a study of night-float admitting residents, Lofgren et al noted that when patient care is transferred to another resident on the day after admission, patients had significantly more tests ordered and experienced slightly longer inpatient stays.32
Despite the known problems with these transfers of care for admitted patients, resident sign outs often are informal and unstructured. They may take place over the telephone, via face-to-face conversation, or by checklists pinned to a bulletin board in a call-room.33 Various interventions to improve communication at the point of resident sign-out have been studied. In one study of surgical resident sign-out, a computerized system was developed to download patient information such as laboratory and radiographic results automatically, producing standardized lists for rounding and transfer of care. The tool was accepted and deemed successful by most of the house-staff using the system.34 Other studies have shown increased resident satisfaction with sign-outs after the implementation of computerized and standardized sign-out processes.35
In a more rigorous study, Petersen et al developed a computerized sign-out program to standardize the process. Included in the program were summaries of the patients' current medical status, resuscitation status, recent laboratory values, medication allergies, an active problem list, and a to-do list for the oncoming physician. After the computerized sign-out intervention was implemented, total preventable adverse events dropped from 1.7% to 1.2%, and the odds ratio (OR) for a patient suffering an adverse preventable event during the cross coverage period decreased from 5.2 to 1.5 (CI 0.2-9.0).36
Based on these and other studies on resident handovers, regulatory and graduate medical education monitors and advocates have joined forces to implement best practice procedures for the hand-over. The British National Patient Safety Agency and the Royal College of Physicians have recommended the following guides to handovers for clinicians.37 Handovers should:
- be multidisciplinary;
- occur at a fixed time and be of sufficient length;
- be free from distraction;
- have access to lab results, clinical information and communication devices;
- have a clear delineation of roles and responsibilities;
- include check lists of tasks to be done; and
- be a two-way process with questions and clarifications made routine;
These suggestions could be applicable to ED transitions as well.
Transitions in the ED
Emergency care settings differ from other hospital settings in many ways. EDs have a unique culture and pace. Emergency physicians and nurses interact with each other in particular ways to accomplish highly specific, specialized patient care goals. Transitions in the ED also have unique status. At the most basic level, EDs represent an environment in which transitions in patient care are exceedingly common and are incorporated into the culture of care. As outlined in the introduction, a single patient typically will endure several transitions in care during the course of his ED stay.
Although limited, specific studies have examined transitions in the ED. One study conducted observations of transitions in five EDs in the United States and Canada. Physician and nurse handovers were observed from an ethnographic perspective. Although there was large variation in the way many of the handovers were conducted, certain features were consistent. The investigators found nearly all the handovers to: be two-way dialogues; include discussions about the "status of the entire work unit," as opposed to being limited to specific patients; be conducted in a standardized order; and expand and contract according to the volume and acuity of the ED patients.38
Investigators from the same study audiotaped doctor and nursing signovers in the ED and found that nearly all transitions have four phases: pre-turnover (preparation), arrival of the replacement, exchange, and post-turnover. In addition, the investigators noted that:
- the medical record was seldom used by either doctors or nurses in the handover;
- physicians and nurses performed their handovers separately;
- the location of the signovers varied—taking place at the bedside or at a patient name board—but they tended not to be in a quiet or distraction-free area.39
Nursing care transitions in the ED also have been evaluated specifically. One study surveyed 48 ED nurses on the quality of handovers and found 50% and 45% of them cited missing information and distractions, respectively, as common problems in the handover process. The majority of nursing handovers occurred in the busiest and loudest part of the ED.40
Only one published study to date has examined the ED physician to admitting physician handover.41 This observational study at two hospitals demonstrated the structure of these handovers was highly variable; some occurred in person, some occurred by telephone. The intermittent use of admitting residents for a subset of the patients who needed to be hospitalized added more variation and less organization to the handover process. The authors observed that the length and detail of the admission handover was determined more by certain characteristics of the physicians who were performing the transition than by acuity or other patient characteristics.
Pitfalls in ED Transitions
Many of the problems that have been identified in inpatient nursing and physician handoffs are potentially exacerbated in the ED setting. For example, multiple studies have demonstrated the presence of excess noise in the ED.42,43 Patient flow and acuity tend to be higher in the ED than on the floors as well. Thus, the prevalence of distractions and interruptions—which has been noted to be a problem in inpatient settings—is likely greater in the ED. This has been validated by a study that demonstrated the high prevalence of overlapping conversations, interruptions, and heavy "communication loads" on physicians and nurses in an Australian ED.44 Similarly, asynchronous shift changes among residents, attending physicians, and nurses in the ED can be obstacles to multi-disciplinary transitions. Variability in style or training among attendings also will potentially limit the standardization or uniformity of sign-outs: ED attendings, out of professional courtesy, may be less willing to criticize each other than are residents or nurses, if they are unhappy with the quality of the handoff.45,46 In EDs, temporal variability of the signover in relation to where the patient is in the course of his or her care may exacerbate communication failures. If a patient arrives just prior to shift changeover, the content of the transition will be different than if the patient is deep into the medical work-up at the time of signout.
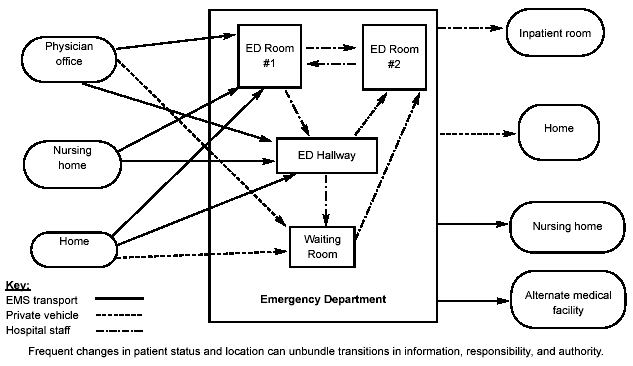
Patient transitions in emergency care settings may also be inherently more complex than in inpatient settings. In the ED, the three types of patient transitions—information, responsibility, and authority—can become unbundled during a change in status or location of the patient. For an inpatient, all components of the transition will occur simultaneously with the physical movement of the patient. This is not always so in the ED. Overcrowding has dramatically increased the prevalence of boarders.47,48 In such situations, change in location and nursing assignment lags behind the transfer of physician responsibility and the authority to treat. These delays can have the effect of two physician teams caring for a single patient, which in turn may lead to uncertainty in caretaking roles and lost clinical data. (See Figure 1.)
| Figure 1. Movement of Emergency Patients |
|
Unlike many inpatient hospital units in which the staff-to-patient ratios are fixed, EDs often pare their staff at times when patient volume is anticipated to be lower. In general, this translates into fewer nurses, physicians, and ancillary staff covering the ED at night. An outgoing nurse may transfer half of his patients to one nurse and half of his patients to another. Similarly, the overnight physician may take over patient care from multiple providers. This funnel effect of patient coverage is unique to the ED and adds particular complexity to the role of nursing and physician sign-outs. For example, a single caretaker may double or triple the number of patients for whom he is responsible within a span of five minutes.
Another example of increased complexity in emergency care transitions occurs when paramedics and EMTs deliver patients to the ED. In some states, written prehospital records are not mandated to be available until 24 hours after the patient received EMS care.49 In these cases, there is a disconnect in information flow caused by the transfer of responsibility and location of patients before the transfer of potentially important written information. Despite the use of prehospital bedside reports, three problems remain. First, these verbal-only reports are given simultaneously with actual physical movement of the patient from the ambulance gurney to the hospital bed. During the transfer of particularly critical patients, emergency care providers routinely engage in attaching lines and monitoring and evaluating the patient at the same time as they are engaged in the signover. Second, a bedside report often is a one-way transfer of information from paramedic or EMT to nurse. This process often excludes other caregivers, particularly physicians. Third, an EMS report may be obscured by cross-talk, often at loud decibels in small, noisy rooms. Thakore et al surveyed medical and ambulance staff on the perceived quality of patient handover by ambulance staff during resuscitations. While both staffs were, in general, satisfied with the quality of the handoffs, there was a notable lack of satisfaction with pediatric handovers. In addition, during critical transfers, ambulance staff felt that the ED staff did not listen well, and medical staff noted that ambulance crews did not give a thorough report—often omitting vital signs.50 The potential for lost information at the point of transfer from prehospital to ED is great.
Similar to the unique challenges posed by transfers from the prehospital environment, transitions out of the ED to ambulatory settings can be particularly challenging. Studies have shown high rates of error associated with discontinuity of care from inpatient to outpatient settings.12,51 Such discontinuities may be even more problematic in ED discharges to home. Hastings, in a literature review, notes that older patients discharged home from the ED suffer high rates of adverse outcomes-including death.52,53 Pitfalls in emergency care transitions are summarized in Table 1.
| Table 1. Potential Pitfalls in Emergency Trarnsitions |
|
Improving the Emergency Transition: Concepts and Strategies
The Institute of Medicine in its report "Crossing the Quality Chasm" explicitly identified the need to improve "coordination and integration of care … to manage smooth transitions from one setting to another."54 From this report and other calls for improved transitions, many health researchers and policy analysts have articulated the goals of smooth, robust, and error-limited transitions. Most of the suggested approaches, not surprisingly, come from non-ED settings.
One study identified 21 successful strategies used at shift turn-over in high-risk, non-medical settings and applied them to the ED handover.15 The authors suggest these tools for improving patient safety at the point of ED transitions:
- Use face-to-face reports only;
- Limit interruptions;
- Provide a written summary of the handoff;
- Provide unambiguous transfer of responsibility;
- Make it clear to others at a glance which personnel are responsible for which duties at a particular time; and
- Delay transfer of responsibility during critical activities.
The MedTeams Research Consortium evaluated 54 adverse events in EDs that were deemed to be preventable by improved teamwork. Employing teamwork or "crew resource management" (CRM) techniques culled from aviation safety programs, the authors identify how teams can improve various aspects of patient care, including transitions. Less hierarchy, sharing of tasks, cross-checking, and improved information sharing are the backbone of team approaches to patient safety.55,56 (When directed towards emergency transitions, team processes include: call out requests for information input; check-back processes to verify communication; systematic and standardized handover processes; and interdisciplinary/team signouts.)
Broadly recognized strategies for general patient safety may have indirect application to transitions. Despite limited evidence for many of these ideas, Leape et al argue that rigorous studies are not always needed to identify ways to improve patient safety.57 Thus, simplification, standardization, teamwork, and a culture of safety are concepts that may improve overall approaches to transitions of patient care and need to be tailored to meet specific clinical settings.58,59 The utility of computerized sign-out systems for inpatient cross coverage has already been discussed. Other standardized systems, such as templates, have also been shown to be helpful for hospitalists who must sign-out to each other.60 Mandatory checklists in trauma settings to prevent omissions at the time of patient transfer have been proposed.61 However, as has been discussed, EDs are highly unique, and no one intervention likely will achieve these goals. Many of these interventions have yet to be scrutinized; however, some researchers have noted that mechanizing this process risks neutralizing the effectiveness of the organic aspects of the personalized verbal sign-out.38
Barriers to implementing any of these strategies are formidable. Improving processes that cross multiple health care disciplines and segments requires a willingness among participants to alter routines and culture. However, both the promotion of improved communication and the culture of safety are movements that have gained considerable traction in the past few years. Momentum invariably will carry some of these concepts forward.
Conclusions
Transitions of care are common, complex, and high-risk processes in EDs. Presently, there is little uniformity in their structure and content, and most participants in the transfers of patient care believe that the processes remain problematic and could be improved. Understanding the complicated and interacting ways in which patient care is transferred in, out, and around emergency settings is the first step to improving ED transitions, limiting adverse events, and enhancing patient care and satisfaction.
References
1. Cook RI, Render M, Woods DD. Gaps in the continuity of care and progress on patient safety. BMJ 2000;320:791-794.
2. JCAHO's 2006 National Patient Safety Goals: Handoffs are biggest challenge. Hosp Peer Rev 2005;30:89-93.
3. Kohn LT, Corrigan J, Donaldson MS. To err is human: Building a safer health care system. Washington, D.C.: National Academy Press: 2000.
4. Bates DW, Gawande AA. Improving safety with information technology. N Engl J Med 2003;348:2526-2534.
5. Bogner MS. Human error in medicine. 1994, Hillsdale, N.J.: L. Erlbaum Associates. xv, 411 p.
6. Donchin Y, Gopher D, Olin M, et al. A look into the nature and causes of human errors in the intensive care unit. Crit Care Med 1995;23:294-300.
7. Delays in treatment. Sentinel Event Alert 2002;26:1-3.
8. Smith PC, Araya-Guerra R, Bublitz C, et al. Missing clinical information during primary care visits. JAMA 2005;293:565-571.
9. Elder NC, Vonder Meulen M, Cassedy A. The identification of medical errors by family physicians during outpatient visits. Ann Fam Med 2004;2:125-129.
10. Moore C, Wisnivesky J, Williams S, et al. Medical errors related to discontinuity of care from an inpatient to an outpatient setting. J General Intern Med 2003;18: 646-651.
11. Mageean RJ. Study of "discharge communications" from hospital. Br Med J (Clin Res Ed) 1986;293:1283-1284.
12. Dvorak SR, McCoy RA, Voss GD. Continuity of care from acute to ambulatory care setting. Am J Health Syst Pharm 1998;55:2500-2504.
13. Stiell A, Forster AJ, Stiell IG, et al. Prevalence of information gaps in the emergency department and the effect on patient outcomes. CMAJ 2003;169:1023-1028.
14. Lardner R. Effective shift handover. Health and Safety Executive 1996.
15. Patterson ES, Roth EM, Woods DD, et al. Handoff strategies in settings with high consequences for failure: Lessons for health care operations. Int J Qual Health Care 2004;16:125-132.
16. Payne S, Hardey M, Coleman P. Interactions between nurses during handovers in elderly care. J Advanced Nursing 2000;32:277-285.
17. Strange F. Handover: An ethnographic study of ritual in nursing practice. Intensive and Critical Care Nursing 1996;12:106-112.
18. Greenwood J. The apparent desensitization of student nurses during their professional socialization: a cognitive perspective. Journal of Advanced Nursing 1993;18
:1471-1479.
19. Luikkonen A. The content of nurse's oral shift reports in homes for elderly people. Journal of Advanced Nursing 1993;18:1095-1100.
20. Rex JH, Turnbull JE, Allen SJ, et al. Systematic root cause analysis of adverse drug events in a tertiary referral hospital. Jt Comm J Qual Improv 2000:26:563-575.
21. Kelly R. Goings-on in a CCU: An ethnomethodological account of things that go on in a routine hand-over. Nursing in Critical Care 1999;4:85-91.
22. Brandwijk M, et al. Distributing Cognition: ICU Handoffs Conform to Grice's Maxims, in Society for Critical Care Medicine 2003: San Antonio.
23. Lally S. An investigation into the functions of nurses' communication at the inter-shift handover. J Nurs Manag 1999:7;29-36.
24. Laine C, Goldman L, Soukup JR, et al. The impact of a regulation restricting medical house staff working hours on the quality of patient care.[see comment]. JAMA 1993;269:374-378.
25. Steinbrook R. The debate over residents' work hours. N Engl J Med 2002;347:1296-1302.
26. Philibert I, Friedmann P, Williams WT; ACGME Working Group on Resident Duty Hours. Accreditation Council for Graduate Medical Education. New requirements for resident duty hours. JAMA 2002;288:1112-1114.
27. Fletcher KE, Saint S, Mangrulkar RS. Balancing continuity of care with residents' limited work hours: defining the implications. Acad Med 2005;80:39-43.
28. Jagsi R, Kitch BT, Weinstein DF, et al. Residents report on adverse events and their causes. Arch Intern Med 2005;165:2607-2613.
29. Petersen LA, Brennan TA, O'Neil AC, et al. Does housestaff discontinuity of care increase the risk for preventable adverse events? Ann Intern Med 1994;121:866-872.
30. Arora V, Johnson J, Loringer D, et al. Communication failures in patient sign-out and suggestions for improvement: A critical incident analysis. Qual Saf Health Care 2005;14:401-407.
31. Jelley M. Tools of continuity: The content of inpatient check-out lists [Abstract]. J Gen Intern Med 1994;9(suppl 2):77.
32. Lofgren RP, Gottlieb D, Williams RA, et al. Post-call transfer of resident responsibility: Its effect on patient care. J Gen Intern Med 1990;5:501-505.
33. Murff H, Bates D. Making Health Care Safer: A Critical Analysis of Patient Safety Practices. Evidence Report/Technology Assessment: Number 43. AHRQ Publication No. 01-E058, July 2001. Agency for Healthcare Research and Quality, Rockville, MD. http://www.ahrq.gov/clinic/ptsafety/Evidence, 2001: 471-486.
34. Van Eaton EG, Horvath KD, Lober WB, et al. Organizing the transfer of patient care information: The development of a computerized resident sign-out system. Surgery 2004;136:5-13.
35. Ram R, Block B. Signing out patients for off-hours coverage: Comparison of manual and computer-aided methods. Proc Annu Symp Comput Appl Med Care 1992:114-118.
36. Petersen LA, Orav EJ, Teich J, et al. Using a computerized sign-out program to improve continuity of inpatient care and prevent adverse events. Jt Comm J Qual Improv 1998;24:77-87.
37. Safe handover: Safe patients BMA Junior Doctors Committee. http://www.npsa.nhs.uk/site/media/documents/1037_Handover.pdf. Accessed March 1, 2006.
38. Behara R, et al. A conceptual framework for studying the safety of transitions in emergency care. Advances in Patient Safety 2003;2:309-321.
39. Perry S. Transitions in care: Studying safety in emergency department signovers. Focus on Patient Safety 2004;7:1-7.
40. Currie J. Improving the efficiency of patient handover. Emergency Nurse 2002;10:24.
41. Matthews AL, Harvey CM, Schuster RJ, et al. Emergency Physician to Admitting Physician Handovers: An Exploratory Study Proceedings of the Human Factors and Ergonomics Society. 46th Annual Meeting. 2003;1511-1515.
42. Buelow M. Noise level measurements in four Phoenix emergency departments. Journal of Emergency Nursing 2001;27:23-26.
43. Zun LS, Downey L. The effect of noise in the emergency department. [See comment.] Acad Emerg Med 2005;12:663-666.
44. Coiera EW, Jayasuriya RA, Hardy J, et al. Communication loads on clinical staff in the emergency department. Med J Aust 2002;176:415-418.
45. Propp DA. Emergency care transitions. Acad Emerg Med 2003;10:1143.
46. Beach C, Croskerry P, Shapiro M. Profiles in patient safety: Emergency care transitions. Acad Emerg Med 2003;10:364-367.
47. Derlet RW. Overcrowding in emergency departments: Increased demand and decreased capacity. Ann Emerg Med 2002;39:430-432.
48. Weiss SJ, Derlet R, Arndahl J, et al. Estimating the degree of emergency department overcrowding in academic medical centers: Results of the National ED Overcrowding Study (NEDOCS). Acad Emerg Med 2004;11:38-50.
49. PA Department of Health EMS Regulations. 2005.
50. Thakore S, Morrison W. A survey of the perceived quality of patient handover by ambulance staff in the resuscitation room. Emerg Med J 2001;18:293-296.
51. Moore C, Wisnivesky J, Williams S. Medical errors related to discontinuity of care from an inpatient to an outpatient setting. J Gen Intern Med 2003;18:565-651.
52. Hastings SN, Heflin MT. A systemic review of interventions to improve outcomes for elders discharged from the emergency department. Acad Emerg Med 2005;12:978-986.
53. Aslin BR, Rhodes KV, Levy H, et al. Insurance status and access to urgent ambulatory care follow-up appointments. JAMA 2005;294:1248-1254.
54. Institute of Medicine. Crossing the quality chasm: A new health system for the 21st century. Natational Academy of Sciences 2000:49-50.
55. Risser DT, Rice MM, Salisbury ML. The potential for improved teamwork to reduce medical errors in the emergency department. Ann Emerg Med 1999;24:373-383.
56. Cosby KS, Croskerry P. Patient safety: A curriculum for teaching patient safety in emergency medicine. Acad Emerg Med 2000;10:69-78.
57. Leape LL, Berwick DM, Bates DW. What practices will most improve safety? Evidence-based medicine meets patient safety. JAMA 2002;288:501-507.
58. Berwick DM. "Taking Action to Improve Safety: How to Increase the Odds of Success." National Patient Safety Foundation Congress. 1998 Keynote Address.
59. Leape LL. Error in medicine. JAMA 1994:272:1851-1857.
60. Landucci D, Gipe BT. The art and science of the handoff: How hospitalists share data. Hospitalist 1999;3:4.
61. Graham CA. Interhospital trauma transfers: Room for improvement? Injury 2005;36:1058-1059.
CME Objectives
Upon completing this program, participants should be able to:
- Understand the roles of various health care providers in the transfer of patient care process;
- Define the unique elements involved in the transfer of patient care by emergency medicine providers; and
- Identify tools and strategies that allow for a safer transfer of patient care by emergency department providers.
Physician CME Questions
1. The JCAHO 2006 Patient Safety Goals include which of the following directives?
A. Reduce medical errors at the time of patient care transitions.
B. Improve handoff communications.
C. Standardize signout procedures.
D. Increase use of electronic medical records during health care transitions.
2. Transitions in emergency departments are:
A. rare events.
B. incorporated into the culture of care.
C. often performed with nurses and physicians together.
D. protected from interruptions and distractions.
3. Signovers do not necessarily include the transfer of:
A. authority.
B. location.
C. responsibility.
D. information.
4. The funnel effect:
A. occurs during most health care transitions.
B. disproportionately impacts physicians over nurses.
C. is exacerbated by ED overcrowding.
D. may involve the rapid assumption of care from multiple sources.
5. Most participants in ED transitions:
A. limit interruptions while performing the signout.
B. use the medical record to facilitate the process.
C. don't prioritize the signout as an important task.
D. adjust the process to meet the volume and acuity of the department.
CME Answer Key
1. B; 2. B; 3. B; 4. D; 5. D
A 75-year-old woman with a chief complaint of chest pain is brought to a university emergency department (ED) by a city-run emergency medical systems (EMS) service.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.