ECG Review: RBBB with a Twist
ECG Review
RBBB with a Twist
By Ken Grauer, MD, Professor, Assistant Director, Family Practice Program, University of Florida. Dr. Grauer reports no financial relationship to this field of study.
|
|
|
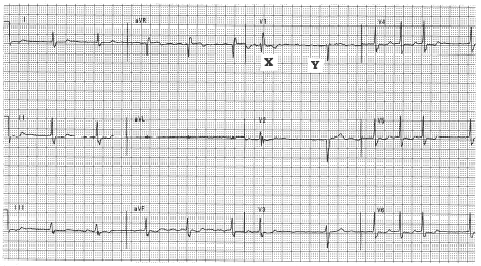
Figure. 12-lead ECG obtained froma 66 year old man with heart failure. |
Clinical Scenario: The 12-lead ECG in the Figure was obtained from a 66 year old man with heart failure. How would you interpret this ECG? Does the patient have RBBB (right bundle branch block)? Is there "a twist" to answering this question?
Interpretation/Answer: Although we are not provided with a lead II rhythm strip, the rhythm is clearly irregular. There are undulations in the baseline, but no definite P waves. Given the irregular irregularity and lack of P waves, the rhythm is atrial fibrillation, in this case with a relatively slow ventricular response.
The QRS complex appears to be widened (to about 0.11 second) in most leads. The typical rSR' morphology of the beat labeled X in lead V1, in association with QRS widening and wide terminal S waves in leads I and V6 is consistent with the diagnosis of complete RBBB (right bundle branch block).
The most interesting facet of this tracing is beat Y in lead V1. This QRS complex is not widened! Instead, QRS morphology of this complex in simultaneously recorded leads V1, V2, V3 is completely normal. This suggests that the RBBB conduction defect is not permanent. Instead, it is likely to be rate-related, with the relative pause seen between beats X and Y being long enough to allow the defective right bundle branch adequate time to recover its conduction capacity.
Rate-related bundle branch block is an interesting phenomenon that will be seen on occasion. The rate of onset of the conduction defect often differs from the rate at which the conduction defect goes away. Thus, a patient may manifest normal QRS conduction at a rate up to 80/minute, beyond which RBBB may develop. However, the heart rate may then need to slow down to well under 50 or 60/minute before the conduction defect goes away. Cardiac ischemia or hypoxia may both contribute to development of an intermittent or rate-related conduction defect. The diffuse ST-T wave flattening and slight depression seen in the tracing shown here may have reflected ischemia in this 66-year-old man with heart failure.
A 12-lead ECG was obtained from a 66 year old man with heart failure. How would you interpret this ECG? Does the patient have RBBB (right bundle branch block)? Is there "a twist" to answering this question?Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.