ECG Review: What Would You Ask the Technician?
By Ken Grauer, MD
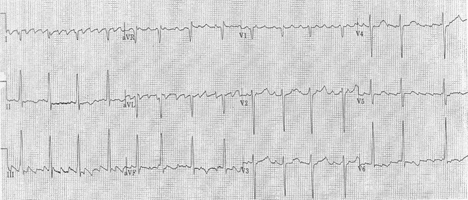
Figure. 12-lead ECG recorded from a 67-year-old woman with heart failure.
Clinical Scenario: How would you interpret the 12-lead ECG shown in the Figure? What is distinctly unusual about this tracing? What would you ask the technician who recorded this tracing?
Interpretation/Answer: There are a number of interesting findings on the 12-lead ECG shown in the Figure. Although the variation from beat to beat is not great, the rhythm is irregularly irregular. QRS duration is upper normal, suggesting a supraventricular mechanism for the rhythm. No P waves are seen in lead II. Instead, a sawtooth pattern of atrial activity is noted in a number of other leads at a rate of approximately 300/minute. This strongly suggests that atrial flutter is the rhythm, seen here with a variable but controlled ventricular response. Marked RAD (right axis deviation) is present. There is voltage for LVH (left ventricular hypertrophy). Assessment of ST segment morphology is difficult to ascertain because of baseline artifact and the effect of flutter activity, however acute ST-T wave changes do not appear to be present.
There are two distinctly unusual features about this tracing. The first relates to the cardiac rhythm. Despite the baseline artifact that is present, identification of repetitive atrial activity at a rate of approximately 300/minute in several leads (especially leads I, II, and V1) defines the rhythm as atrial flutter. The most common type of atrial flutter manifests a characteristic sawtooth pattern that is generally best seen in all three of the inferior leads. However, there is no indication at all of flutter activity in lead II of this tracing. Instead, the lead that is most suggestive of flutter activity is lead I, a lead which often shows no trace at all of flutter activity on a 12-lead ECG. The second unusual finding is also noted in lead I, which shows a predominantly (if not totally) negative QRS complex. While this finding may be indicative of lateral infarction, there is no suggestion of lateral infarction in the precordial leads. The most common type of lead reversal (ie, mixing up left and right arm electrodes) is also unlikely because lead aVR is predominantly negative as it should be (lead aVR shows a Qr pattern, instead of manifesting a positive QRS complex as would be expected if the arm leads were reversed). Thus, some technical mishap other than lead reversal should be suspected as a possible cause of the unusual appearance of the QRS complex in lead I and the unexpected presence of characteristic flutter activity in lead I instead of in lead II.
The patient in question was a 67-year-old woman with severe mental retardation, who was admitted to the hospital for an exacerbation of heart failure. She could not understand instructions, and would only allow an ECG to be recorded while she was lying on her right side. The importance of verifying proper body position during ECG recording is essential for understanding potential alterations in ECG complex morphology from what is normally expected. While this case is admittedly a more extreme example, it is important to appreciate that recording an ECG with a patient supine but with elevation of the bed even by a small amount may produce surprising changes in QRST morphology compared to ECG recordings made with the bed flat. Asking your technician to always indicate in writing on the ECG such alterations in body position during ECG recording would obviate many problems with interpretation.
Dr. Grauer, Professor, Assistant Director, Family Practice Residency Program, University of Florida, is Associate Editor of Internal Medicine Alert.
How would you interpret the 12-lead ECG shown in the Figure? What is distinctly unusual about this tracing? What would you ask the technician who recorded this tracing?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
