Methamphetamine
Methamphetamine
Authors: Robert G. Hendrickson, MD, Assistant Professor, Department of Emergency Medicine, Oregon Health and Science University, Associate Medical Director, Oregon Poison Center, Portland; and Laura Spivak, MD, Medical Toxicology Fellow, Oregon Poison Center, Instructor, Emergency Medicine, Oregon Health and Science University, Portland.
Peer Reviewers: Thomas G. Martin, MD, MPH, FACMT, FAACT, FACEP, Associate Professor of Medicine, Division of Emergency Medicine, Director, UW-TOX (UW Med Tox Consult Service), Associate Medical Director, Washington Poison Center, Attending Physician, UWMC Emergency Department, Seattle, WA; and John G. Benitez, MD, MPH, FACMT, FACPM, FAAEM, Director, Ruth A. Lawrence Poison and Drug Information Center, Associate Professor of Emergency Medicine, Environmental Medicine, and Pediatrics, University of Rochester, NY.
Methamphetamine is a synthetic substituted amphetamine with stimulant and euphoric effects. Over the last two decades, methamphetamine use has increased drastically in the United States and it has become one of the most popular illicit drugs in the country, particularly along the West Coast and in the Mid West. Widespread media attention has focused on the destructive and criminal behavior of users, the environmental toll of methamphetamine labs, the rise in abused and neglected children, and the victimization of the community via identity theft and other property crimes. In addition to these community concerns, the toll on emergency departments where methamphetamine use is endemic has been significant.
This article will detail the history and epidemiology of methamphetamine use and illicit methamphetamine production, describe the clinical manifestations of intoxication, and recommend diagnostic and management strategies. Decontamination of patients from active methamphetamine labs will be discussed, along with associated threats to hospital health care personnel. Methamphetamine's unique pharmacokinetics will be explained, shedding light on its persistence as a drug of abuse. Finally, the intricacies of laboratory testing for methamphetamine will be reviewed.
In my over 20 years of practicing emergency medicine, I cannot recall an abused drug that causes as many problems as methamphetamine, and sooner or later, these problems are seen in the ED. This article is therefore timely and useful to all emergency physicians.
—J. Stephan Stapczynski, MD, Editor
Definition
Methamphetamine [(S)-N-methyl-1-phenylpropan-2-amine], is a synthetic substituted amphetamine that is used for its stimulant, anorectic, and euphoric effects. Over the last two decades, methamphetamine use has increased progressively in the United States and it has become one of the most popular illicit drugs in the country.
History
Humans have been using amphetamines as stimulants for centuries. For more than 5000 years, herbs from the Ephedra family (Ephedra vulgaris, Ephedra sinica [Ma Huang], etc.) that contain the amphetamine ephedrine (an optical isomer of pseudoephedrine) have been used to make tea to treat asthma and cold symptoms.
Both amphetamine (1-phenylpropan-2-amine) and methamphetamine were synthesized in the late 1800s (1887 and 1893, respectively) and are structurally similar to ephedrine. Methamphetamine has more central nervous system (CNS) stimulant properties than amphetamine (due to higher lipid solubility), and became popular for use by military personnel in World War II to decrease fatigue during military campaigns. Popularized by the war and legalized in Japan in 1941, methamphetamine was touted to "fight sleepiness and enhance vitality."1,2 By the end of the 1940s, Japan had experienced a large-scale epidemic of methamphetamine use. Both amphetamine and methamphetamine were marketed by several companies in the United States and throughout the world. Amphetamine tablets and an amphetamine inhaler (Benzedrine) were available over-the-counter (OTC) in the United States during the 1930s, 1940s, and early 1950s.2 By the mid-1950s, the Food and Drug Administration (FDA) had banned the OTC sale and limited the prescription sale of amphetamines. Without an OTC or prescription source, methamphetamine production by home chemists arose.1
By the early 1960s, several simple methods of producing methamphetamine locally were perfected, and clandestine methamphetamine laboratories began to appear in Hawaii, Oregon, and northern California. The production and trafficking of "crank" along the West Coast, a mixture of d/l-methamphetamine (methamphetamine sulfate), largely was controlled by Bay Area motorcycle gangs. As these groups became targeted by law enforcement in the 1980s, the majority of manufacturing and distribution moved toward southern and central California.
During the 1980s, two developments increased methamphetamine usage in the United States: a simpler method of synthesis and the availability of a form of methamphetamine that was more easily smokable (crystal methamphetamine). Several simple methods of home-production of methamphetamine from ephedrine or pseudoephedrine gained popularity. A crystal form of methamphetamine (e.g., crystal meth, ice) arrived in Hawaii from Asia and achieved widespread popularity due to its higher purity.
In the 1980s and 1990s, small-scale methamphetamine laboratories (meth labs) increased across the West and Midwest. These small meth labs were fairly inefficient (approximately 1-4 ounces of methamphetamine per cook), and were found in transient enclosed areas, including homes, motel rooms, storage units, abandoned buildings, cars, and trailers.3 Methamphetamine largely was produced by inexperienced chemists ("cookers") with makeshift equipment in dangerous conditions. This methamphetamine was sold locally as well as consumed by the manufacturers.
In the early 1990s, Mexican criminal organizations became involved in methamphetamine synthesis and distribution. Crystal methamphetamine synthesis increased in Mexico and was trafficked throughout the western United States. In addition, Mexican gang-run meth labs on both sides of the border contained more advanced equipment and used standardized production methods. These superlabs produce larger volumes of methamphetamine (greater than 10 pounds of meth per cook) for trafficking throughout large geographic areas, are guarded heavily, and typically are located in rural areas. Clandestine laboratories in California and Mexico are now the primary sources of supply for methamphetamine available in the United States.
The Comprehensive Methamphetamine Control Act of 1996 broadened restrictions on the common chemicals used in methamphetamine production, increased penalties for production and trafficking of methamphetamine and listed chemicals, and expanded controls on ephedrine, pseudoephedrine, and phenylpropanolamine (PPA).1 Since this act, many states have required pseudoephedrine products to be sold from behind pharmacy counters.
A federal law signed on March 9, 2006 (the Combat Methamphetamine Epidemic Act of 2005), and effective September 30, 2006, requires that products containing pseudoephedrine, ephedrine, or phenylpropanolamine be stored out of reach of consumers (behind the counter or in a locked box) throughout the nation.5 In addition, consumers must present valid photo identification and be entered into a database each time they purchase a product. Consumers are limited to purchasing 7.5 grams of pseudoephedrine, ephedrine, or phenylpropanolamine base (eliminating the weight of the salt that the product is sold with, e.g., for pseudoephedrine hydrochloride only the weight of the pseudoephedrine is calculated, not the hydrochloride) per month.5 It remains to be seen whether these additional regulations will decrease usage or the community impacts of methamphetamine use.
Historically, legislation that has attempted to decrease supply of methamphetamine precursors has had a short-term effect on methamphetamine-related arrests and hospital admissions.4,6 However, after a period of 6-24 months, arrest rates, drug usage and supply, and hospital admission rates have rebounded to previous levels.4,6,7 This may be due in part to adaptability of drug suppliers. As legislation limits the supply of precursors, drug production habits change. For example, as precursors became more limited in the western United States in the late 1990s, the illicit shipment of precursors over the Mexican and Canadian borders increased,8 and as Canadian regulations tightened the supply through that country, shipments of pseudoephedrine from Asia have increased.9
Epidemiology: Current Scope of the Problem
Methamphetamine use appears to have increased nationwide over the past two decades. Currently, more than 9% of Americans aged 18-45 years report methamphetamine use once in their lifetime, and 0.6% reported use in the past month.10 The National Survey on Drug Use and Health reported that in 2005 among all persons aged 12 years or older, the rate of methamphetamine use in the past year was higher among males than females.11 The highest rates of methamphetamine use in 2005 were reported to be among Native Hawaiians or other Pacific Islanders, American Indians or Alaska Natives, and persons reporting two or more races.11 Use among whites and Hispanics was higher than use among blacks or Asians.11 States with the highest rates of methamphetamine use in the past year include Nevada, Wyoming, and Montana.11 Connecticut, New York, and North Carolina ranked among states with the lowest methamphetamine use rates.11 Methamphetamine use in 2005 was reportedly higher in counties in small metropolitan areas than in counties in large metropolitan areas.11
Methamphetamine Production
Methamphetamine is a unique illicit drug in that it may be produced fairly easily from readily available precursors such as pseudoephedrine and ephedrine. Meth may be converted from these products by over 150 methods, many of which can be obtained via the Internet. The specific method used depends largely on geography, distribution intent, and the regulations imposed on precursor chemicals in that local community. The method of methamphetamine production, as well as the skills of the chemist and quality of the manufacturing process/equipment, influence yield and purity.
Methamphetamine production begins with the isolation of the precursor chemical, which is most commonly pseudoephedrine. Pseudoephedrine is found in cold medications, typically in tablet form. The pseudoephedrine tablets are crushed and a solvent is added. The most common solvents used are gasoline additives (e.g., methanol) or denatured alcohol (e.g., ethanol). The solvent/powder mixture is then heated and allowed to separate and finally filtered to remove the unwanted tablet fillers.
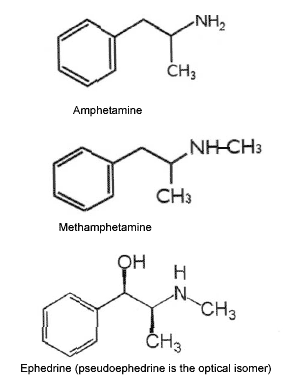
The next step is the conversion of pseudoephedrine to methamphetamine base by removal of a hydroxyl group from the beta carbon. (See Figure 1.) Several methods exist, but the two most popular are the "red phosphorous method" and the "Nazi (or anhydrous) procedure." Both of these procedures result in methamphetamine base.
| Figure 1. Chemical Structures of Pseudoephedrine/Ephedrine, Amphetamine, and Methamphetamine |
|
The red phosphorous method involves the addition of red phosphorous, iodine, and water, and boiling the solution for several hours. This step produces methamphetamine base as well as a small amount of phosphine gas as a byproduct.3 Other chemicals used in this method include sodium hydroxide (lye) and solvents such as ether, camping fuel (petroleum naphtha or "white gas"), or paint thinner (toluene).
The anhydrous procedure is also known as a Birch reduction, and as the Nazi procedure, as it was purportedly developed in Germany in the 1940s. This procedure involves adding sodium or lithium (or rarely potassium) metal to pseudoephedrine and heating. Anhydrous ammonia is then added to the mixture. Solvents used to dissolve the hydrophobic methamphetamine base include ether, petroleum naphtha, or toluene.
Methamphetamine base must then be converted to the methamphetamine hydrochloride salt. Sulfuric acid, from household drain cleaners, is typically added to rock salt (or table salt) in a separate container that is attached to the methamphetamine base solution. The acid and salt produce HCl gas, which bubbles into the methamphetamine base solution, forming methamphetamine hydrochloride which then precipitates. The mixture is then filtered and the powder that remains is methamphetamine hydrochloride. This is generally "cleaned" by adding acetone or ether and repeating the filtration process.
Once methamphetamine hydrochloride has been produced, it may be bulked with a variety of items to increase profit for dealers. Although data is limited on methamphetamine bulking agents, adulterants, and contaminants, white powders (e.g., talc, baking powder, inositol, etc.) may be used to increase the volume of the product, just as is used with powder cocaine or china white heroin.12 Alternative stimulants, such as caffeine, may be added to methamphetamine powder because it may be less expensive than meth but simulate some of the sympathomimetic physical effects.12,13
Although bulking agents are used for powder methamphetamine, impurities interfere with the crystallization of methamphetamine into "crystal meth." For this reason it is a commonly held belief that crystal methamphetamine is 100% pure. However, methylsulfonylmethane (MSM), a veterinary and human dietary supplement, crystallizes when mixed with methamphetamine.12 For this reason, MSM has been used to bulk crystal methamphetamine, although the fallacy that crystal methamphetamine is pure continues.
The Nomenclature, Appearance, and Economics of Methamphetamine
Methamphetamine exists in two main forms: powder methamphetamine and crystal methamphetamine. Powder methamphetamine is typically called "crank" as well as "meth" and "chalk." Powder meth is typically a fine white powder, but can be any number of colors (e.g., pink, brown, red, yellow, or green) depending on the chemicals used to synthesize the drug and the remaining contaminants.14
It is important to note that both forms are methamphetamine hydrochloride and that, unlike cocaine and crack/freebase cocaine, crystal methamphetamine is not the freebase form of methamphetamine. Crystal methamphetamine is produced by putting powder methamphetamine into a super-saturated solution in a solvent (typically ether or acetone) and allowing the solution to cool, resulting in the crystallization of methamphetamine hydrochloride. This crystal methamphetamine appears clear and forms chunks, hence the names "ice," "crystal," and "glass." Street names for both powder and crystal methamphetamine vary significantly with geography. (See Table 1.) An excellent resource for emergency physicians of street names of illicit drugs is the Office of National Drug Control Policy, which maintains a searchable list of street names, organized alphabetically and by drug type. This list may be found at: www.whitehousedrugpolicy.gov/streetterms.
| Table 1. Street Names for Methamphetamine | ||||
|
||||
Methamphetamine is typically purchased in dollar amounts (e.g., "dime bag" = $10) or by weight. Common weight-based purchase amounts include; 1 gram, 1/16th ounce (a.k.a. "teenager"), or 1/8th ounce (a.k.a. "eight ball"). One ounce is equivalent to 28 grams and an "eight ball" is equivalent to about 3.5 grams. To put this into perspective, one gram is physically equivalent to the contents of an artificial sweetener packet. The purchase price for a gram of methamphetamine varies due to geography and ranges from $20 to $300, and averages about $100.15
Pathophysiology of Methamphetamine
Methamphetamine may be smoked, insufflated ("snorted"), injected, ingested orally, or absorbed through mucous membranes. The most common method of use varies with geographic region, with some evidence suggesting that insufflation predominates in the upper Mid West, injection predominates in the Gulf Coast, and smoking predominates on the West Coast.16
Once absorbed, methamphetamine hydrochloride rapidly crosses the blood brain barrier and increases the concentration of biogenic amines (e.g., dopamine, norepinephrine, and serotonin). Although all stimulants increase CNS biogenic amines, methamphetamine's effects differ from other stimulant illicit drugs (e.g., cocaine, phencyclidine) in that methamphetamine produces a more substantial increase in dopamine concentrations.17,18 This unique effect may dictate many of the clinical effects that are seen after methamphetamine use.19
The clinical pattern of methamphetamine intoxication can be correlated directly to the effects of the individual neurotransmitter pathways that it alters: dopamine, norepinephrine, and serotonin. Dopaminergic pathways are involved in motor function, as well as feelings of pleasure and reward. Methamphetamine use can increase dopaminergic tone and lead to choreoathetoid movements, tremors, and repetitive movement (stereotypy) that typically have been related to Parkinsonian syndromes and schizophrenia/psychosis. Picking at the skin seems to be a particularly pervasive dopamine-related repetitive motion seen in methamphetamine users. Occasionally, as is seen in cocaine users, skin picking may be the result of the delusion that bugs are crawling on or beneath the skin (formication), however this seems to be less common than stereotypy in meth users.
At the neuronal level, in low doses methamphetamine binds to the presynaptic dopamine reuptake transporter and reverses the flow of dopamine so that, in addition to inhibiting dopamine reuptake, dopamine is transported from the presynaptic cytoplasmic neurotransmitter pool to the synapse. At moderate doses, the reuptake exchange continues, but methamphetamine also binds to the dopamine vesicles within the presynaptic bouton and reverses flow of dopamine from the vesicle to the cytoplasm, thereby indirectly increasing dopaminergic tone in the synapse. Finally, at high doses, methamphetamine diffuses into the vesicle, alkalinizes the vesicle and allows for release of the dopamine vesicle by reverse transport into the synapse.20 All of these mechanisms lead to an increase of dopamine in the synapse and therefore increased post-synaptic dopamine receptor stimulation.
Methamphetamines block the reuptake of norepinephrine in the CNS, perhaps leading to some euphoria in low doses. In larger doses, norepinephrine concentrations are increased independently of reuptake inhibition17 and may lead to agitation, seizures, and combative behavior. Secondary release of norepinephrine from peripheral sympathetic fibers and epinephrine from the adrenal glands may then stimulate alpha and beta-receptors peripherally. However, it is important to note that methamphetamine does not have any intrinsic alpha or beta-receptor stimulatory properties.21
Methamphetamine inhibits the reuptake of serotonin as well. Serotonin is involved in mood, sleep, and appetite regulation. Increased serotonergic tone is likely responsible for the anti-depressant effects and mood elevation, anorexia, and hallucinations that methamphetamine users report, as well as the resultant depression after withdrawal of the drug. In addition, serotonin plays a role in dopaminergic modulation and may affect euphoria, reward, and addiction with methamphetamine use as it does with cocaine use.22
Pharmacokinetics and Pharmacodynamics
Methamphetamine's unique pharmacokinetic profile is defined by its high lipid solubility and CNS penetration as well as its long duration of action. Methamphetamine can be used via the oral, intravenous, intramuscular, intranasal, or inhalational routes as well as absorbed through mucous membranes (i.e., vagina, rectum, etc). Regardless of how it is used, methamphetamine is absorbed quickly and has a rapid onset of effects (e.g., inhalation 0-2 minutes onset; insufflation 5-10 minutes; oral 20-60 minutes). Once absorbed, methamphetamine's serum half-life is 12 hours. Methamphetamine's duration of effect averages 4-16 hours as compared to cocaine (20-40 minutes), crack (5-15 minutes), and phencyclidine (4-6 hours). This prolonged duration of effect has contributed to its popularity.
Methamphetamine is metabolized to amphetamine (10%) via N-demethylation, and to a variety of other minor metabolites.23,24 It is excreted primarily as unchanged methamphetamine (30-50%) in the urine.23 Methamphetamine excretion into the urine is highly dependent on the urine pH and excretion can be nearly halted in alkaline urine.23,24 Sophisticated users know that concomitant ingestion of an alkaline compound (e.g., sodium bicarbonate) enhances bodily retention of the drug, and increases the time window for a negative urine drug screen.24
Tolerance to the stimulant (e.g., tachycardia) effects of methamphetamine develops rapidly,23,25 and users typically require increasing doses to achieve the same effect. Downregulation of receptors occurs in the face of supra-physiologic neurotransmitter surges and this is responsible for the rapidly diminishing clinical effect.24 A typical therapeutic, or recreational, dose of methamphetamine is 5-15 mg per dose, and users binging on methamphetamine have been reported to consume as much as several grams per day.24
Clinical Effects
The clinical effects that are associated with methamphetamine use, abuse, and overuse can be predicted by the affected neurotransmitters' mechanisms of action. Over stimulation of central nervous system (CNS) dopamine, norepinephrine, and serotonin receptors leads to the sympathomimetic stimulation, euphoria, and stereotypy/movement disorders that are present when methamphetamine users visit the ED. The most common ED presenting complaints are traumatic injuries, alteration of level of consciousness, abdominal pain, suicidality, chest pain, skin infections, miscarriage, and headache.26
Recreational Doses. After a recreational dose of methamphetamine, the user typically feels a period (5-30 minutes) of intense euphoria ("the rush"). (See Table 2.) A stimulant effect continues for 4-16 hours with continued euphoria ("the high") and is followed by sensations of depression and fatigue. If the user continues to use the drug while still intoxicated ("runs" or "binging"), then the prolonged stimulant effect may be followed by a "crash" where the user has both sleep deprivation and possibly neurotransmitter washout resulting in prolonged sleep, sometimes for days.24,27 "Tweaking" is a phenomena where users have the resolution of euphoric effects, but retain the paranoia and psychotic symptoms. Tweaking typically follows a prolonged binge and can leave the user with a sensation of depression, paranoia, and aggression.
| Table 2. Intoxication Cycle |
|
1. Rush: Initial euphoria following administration. Lasts 5-30 minutes. 2. High: Continued stimulation lasting as long as 16 hours. 3. Binge: Continued drug administration to maintain the high. 4. Tweaking: Depression, paranoia, and aggression following a binge prior to onset of the crash. Can last up to 24 hours. 5. Crash: Exhaustion following repeated use. Sleep can last up to 3 days. (Reference: DEA Drug Identification Bible, 2004-2005 edition. Grand Junction, CO: Amera-Chem Inc.;2004., p. 305-306) |
Acute Overdose. Overdose of methamphetamine may occur when users continue to use methamphetamine while intoxicated ("stacking"), when an inexperienced user takes a larger than typical dosage, or if a user ingests the drug in an effort to escape prosecution for drug possession or sale ("body stuffer").
The clinical symptoms of methamphetamine overdose relate to the CNS over-stimulation with both norepinephrine (e.g., hypertension, tachycardia, agitation, diaphoresis, mydriasis, seizures, and hyperthermia) and dopamine (e.g., tremor/hyperreflexia, choreoathetoid movements, bruxism, and paranoia). (See Table 3.) Agitated delirium with increased muscular activity may lead to hyperthermia and rhabdomyolysis, and to acidosis, hyperkalemia, and renal failure. Norepinephrine and serotonin release may predispose users to hypertension and vasospasm, including cerebrovascular accident, myocardial ischemia, aortic dissection, and intracranial hemorrhage.26,28,29
| Table 3. Acute Clinical Effects | |||
|
Trauma Patient. Methamphetamine use may be associated with traumatic injury28 in several ways. Methamphetamine users who feel both euphoric and stimulant effects may partake in risk-taking behavior in combination with poor judgment and poor coordination, leading to behaviors such as erratic driving and high speed collisions.30 Alternatively, methamphetamine users who are "coming down" may become hypersomnolent or unconscious while attempting to operate their vehicles.30
Methamphetamine use has been correlated with interpersonal violence as well as with self-mutilation and suicidality.31,32 This may also be the result of poor judgment and risk taking and is likely related to the combination of paranoia and aggression associated with "tweaking." Patients may report to the ED with the entire range of interpersonal traumatic injuries, including stab wounds, gunshot wounds, and blunt trauma.28
Stimulant-Associated Complaints. Patients who use methamphetamine may present to the ED with complaints that are related to their stimulant use, including headaches, palpitations, and panic attacks/anxiety.28,32 In addition, patients may present with complaints related to hypertension (e.g., headache, intracranial hemorrhage), or sympathomimetic stimulation (e.g., palpitations, dyspnea), or from vasospastic disease (myocardial infarction, chest pain, cerebrovascular accident).28,32
Chronic and regular users of methamphetamine report several chronic symptoms: poor appetite (63%), fatigue (58%), palpitations (56%), insomnia (55%), tremor (49%), forgetfulness (47%), headaches (44%), weight loss (43%), arthralgias (37%), myalgias (33%), abdominal aches (34%), nausea (33%), shortness of breath (28%), and chest pain (19%). Patients may present to the ED for any of the above complaints.32
Chest pain may be the chief complaint of up to 8% of methamphetamine users who utilize the ED.28 In one small retrospective study, up to 25% of these patients had an acute coronary syndrome (ACS). In fact, several patients, with and without risk factors, have developed ACS after amphetamine and methamphetamine use.33-37 Similar to other stimulants such as cocaine, methamphetamine may predispose patients to myocardial ischemia by inducing coronary artery spasm, increasing myocardial oxygen demand, or altering thrombosis; however, these etiologies have not been confirmed.
Methamphetamine-Induced Psychosis. Methamphetamine use increases release of dopamine and may lead to transient psychosis including agitation, hallucinations, delusions, paranoia, and suicidality. The symptoms of patients who have simple methamphetamine-induced transient psychosis typically resolve over 1-2 days. However, methamphetamine-induced transient psychosis and an acute psychotic exacerbation of schizophrenia may be difficult to distinguish prospectively.
A chronic psychosis has been reported after prolonged methamphetamine use, and after the pharmacologic effects of methamphetamine have resolved. Symptoms in this chronic stage include blunted affect, paranoia, and hallucinations. Although the paranoia and hallucinations typically resolve over weeks to months, the blunted affect and idleness may continue for years.38 Patients who use methamphetamine again, or have psychological stress, may have a spontaneous recurrence of the paranoia and hallucinations.39
Skin Infections. Injection drug use (IDU) of any illicit substance may lead to cellulitis and subcutaneous abscess formation. These infections may be caused by skin flora that are introduced due to lack of sterile technique; however, oral flora have been identified in many IDU-related abscesses and should be considered.40,41 This may be introduced when saliva is used to put the methamphetamine into solution for parenteral use ("cook the meth") or saliva is used to moisten the skin or needle prior to injecting. Community acquired Methicillin-resistant Staphylococcal aureus (MRSA) has become a significant issue and currently is the most common bacteria isolated in IDU abscesses in some communities.
Chronic Effects of Methamphetamines
Meth Mouth. Long-term methamphetamine users may develop a syndrome that is distinguished by the extent and severity of dental caries and wear. This decay may occur in a characteristic pattern that has been named "meth mouth."42-45 Methamphetamine use is associated with several factors that may accelerate dental decay. Although the relative weights of these factors in the pathophysiology of meth mouth are unclear, three factors appear to be the most likely causative agents: arterial vasospasm, xerostomia, and bruxism.45
Patients with meth mouth may have a characteristic pattern of decay at the base of the anterior maxillary teeth.43,44 Patients who insufflate (i.e., snort) methamphetamine are most likely to have this pattern of decay, suggesting that the topical deposition of methamphetamine may be causing arterial vasospasm of the arteries that supply these teeth as they travel through the nasal cavity.43
Patients who use prescription46 or recreational47 methamphetamine develop xerostomia, or a decrease in salivary gland production, that may be centrally mediated.42,45 Dry mouth, in combination with poor dental hygiene and consumption of carbohydrate-rich drinks (e.g., cola), may predispose patients to overgrowth of bacteria and the resulting dental caries.42 Patients with other syndromes that are associated with xerostomia (e.g., Sjogren syndrome) have similar patterns of dental decay.44
Grinding and clenching of teeth (i.e., bruxism) have been associated with users of both methamphetamine and the substituted methamphetamine "Ecstasy" (3,4 - methylenedioxymethamphetamine, MDMA). This involuntary grinding (or bruxing) may be due to dopamine-related movement disorder/stereotypy, and is likely due to spasm of the masseter muscles. Bruxism in methamphetamine users may lead to both dental wear (particularly in the molars), as well as fractures of carious teeth.
Clinical Signs of Chronic Methamphetamine Use. It is important to note that most methamphetamine users have no overt signs of methamphetamine use. However, patients who are heavy users may develop several signs that are fairly unique to amphetamine use. It may be helpful to recognize these signs in order to potentially address the patient's need for rehabilitation as well as for risk stratification in certain clinical scenarios.
Regular and chronic users of methamphetamine may display a variety of movement disorders while in the ED. These can range from rocking and fidgeting to complex involuntary repetitive movements (stereotypy). A particularly pervasive stereotypical movement is skin picking. Although occasionally patients may suffer from the delusion of bugs crawling on or under the skin (i.e., formication), more typically patients do not consciously pick at a hallucination or pruritic area. Scabs from skin picking typically are located in easy to reach areas such as the face and forearms.
Meth mouth is a syndrome of extensive dental caries that are characteristically located at the base of the anterior maxillary teeth. This syndrome often occurs in combination with bruxism (i.e., teeth grinding) and dental wear. Although dental caries are common in drug using populations, meth mouth can be distinguished by the characteristic pattern and extensive nature of the decay.
Signs of parenteral drug use may, of course, be present. Patients who smoke methamphetamine may have "meth fingers," or burn marks of the pad of the thumb and lateral surface of the distal second and third digits. This characteristic pattern develops when a methamphetamine pipe is held balanced on the first, second, and third digits, the (typically) glass pipe is heated, and the pipe held while inhaling until the glass becomes hot. These burns also are found in patients who smoke crack in small glass pipes. For patients who inject methamphetamine, track marks, or puncture marks that "track" the vein, may be found just as with any other injection drug.
Chronic and regular methamphetamine users may be cachectic due to the appetite suppressant and stimulant properties of methamphetamine. Fatigue and forgetfulness are common complaints in regular users.32 Hallucinations, agitation, rapid speech, tremor, and aggressive behavior are all possible.
Methamphetamine Withdrawal. After methamphetamine use is stopped, several withdrawal symptoms can occur. An initial acute phase of withdrawal peaks within 24 hours of abstinence and is characterized by increased sleeping and eating, a variety of depression symptoms (e.g., fatigue, anhedonia, hypersomnia, hyperphagia, irritability, and anxiety/agitation), and dysphoric crave-related symptoms. These symptoms peak on day one and slowly decrease until about days 7-10.27
Diagnostic Studies
Diagnostic studies in patients who use methamphetamine should be guided by their presenting complaints. The diagnostic utility of laboratory testing is the evaluation of disorders that contribute to the presentation. A bedside capillary glucose test should be performed on all patients with altered mental status. A complete blood count is indicated in patients with agitation and tachycardia to evaluate for infection and blood loss. Electrolyte evaluation may be helpful in patients with confusion, dehydration, electrocardiogram (ECG) abnormalities, ventricular dysrhythmias, and alteration of mental status.
It is important to have a high index of suspicion for vascular and hypertensive disorders in patients who use stimulants like methamphetamine, as methamphetamine use has been associated with aortic dissection, cerebrovascular accidents, intracranial hemorrhage, and myocardial infarction. Electrocardiograph and troponin evaluation should be considered in patients who use methamphetamine and present with chest pain. Computed tomography (CT) of the head should be considered in patients with agitation or alteration of mental status as the diagnosis of stimulant-induced agitated delirium may be mistaken for an intracranial hemorrhage. Thoracoabdominal CT can be considered in patients with symptoms consistent with aortic dissection.
The presence of methamphetamine may be initially detected via a urine drug screen. However, this initial urine testing has many false positives and false negatives and is unable to provide information on quantity and timing of the exposure. For these reasons, a urine immunoassay should not be used as a definitive evaluation, particularly in forensic, criminal, abuse, or legal cases.
Methamphetamine screens generally detect concentrations of methamphetamine (> 500 mcg/L) or amphetamine (> 200 mcg/L to 1000 mcg/L, depending on assay) in the urine. Methamphetamine is excreted unchanged in the urine (~ 40%) and may be detected as methamphetamine, or is metabolized to amphetamine (~ 10%) and is detected as amphetamine, depending on the specific immunoassay. After a single use of methamphetamine, the urine testing will remain positive for a period of approximately 24 hours (depending on the detection limit).23,48 After repeated doses over several days, the detection time increases to 3-4 days, or longer.23,48,49 The concentration of drug in the urine depends, of course, on the concentration of urine (well-hydrated patients have lower concentrations in the urine via dilution) and the urine pH (alkaline urine increases reuptake of amphetamines and thereby decreases the urine concentration).23
Unfortunately, many varieties and brands of urine immunoassay exist that have varied testing results. It is always best to call your hospital or laboratory personnel to determine the specifics of your immunoassay. The immunoassay detects a particular chemical structure, in this case methamphetamine or amphetamine. Unfortunately any other amphetamine will be detected to some extent by the amphetamine immunoassay. Examples of prescription amphetamines (see Table 4) and amphetamine-like substances that may be detected by the screen include d-methamphetamine (Desoxyn, Dexedrine), Selegiline (metabolized to methamphetamine), d/l-methamphetamine (Benzedrine), phenylpropanolamine (over-the-counter [OTC] decongestant), methylphenidate (Ritalin), ephedrine, and an OTC Vicks inhaler (l-methamphetamine). Substituted amphetamines, phenylethylamines, and tryptamines (aka the "designer drugs"), including MDMA (Ecstasy), MDA, MDE, DMT ("Dimitri"), DPT, 2CB ("Bees"), 2CT7 ("Blue Mystic"), 5-MeO-DIPT ("Foxy," "Foxy methoxy"), and 5-MeO-DMT ("the void"), may also cause positive screening immunoassay tests for amphetamine. Finally, structurally similar but pharmacologically unrelated medications have been reported to cause a positive amphetamine screen in some assays, including amantidine, bupropion, brompheniramine, chlorpheniramine, chlorpromazine, desipramine, doxepin, fenfluramine, labetolol, mexiletine, phenmetrazine, phentermine, propylhexedrine, ranitidine, ritodrine, sertraline, trazadone, trimethobenzamide, tryptamine, and tyramine.
| Table 4. Drugs/Medications that May Test Positive on an Amphetamine UDS Immunoassay |
|
In summary, a positive methamphetamine or amphetamine urine screen can mean several things: methamphetamine was used in the last 1-4 days; another amphetamine was used within the last 1-4 days; or another medication that cross-reacts with the amphetamine immunoassay was ingested recently.
When confirmatory testing by another method is necessary, both urine and blood samples should be sent to the laboratory for quantitative methamphetamine concentrations, generally by gas and liquid chromatography. Quantitation and enantiomeric identification occur with these methods, thus narrowing the range of possible explanations for the presence of methamphetamine.
Management
The management of the methamphetamine-using ED patient depends on the ED presentation and complaint. Patients who are agitated, combative, and psychotic may require chemical restraint and sedation. However, it is important to remember that the vast majority of patients who are dependent on methamphetamines and present to the ED will not be wildly agitated and that careful questioning and history-taking may be required to determine that methamphetamine use is related to the visit.
Acute Methamphetamine Intoxication/Overdose. Patients with acute methamphetamine intoxication or overdose may present to the ED with agitated delirium, tachycardia, hypertension, and hyperthermia. As with all critically ill patients, attention to the airway, breathing, and circulation (ABCs) and supportive care predominate the first few minutes of care. Adequate intravenous access is a necessity, oxygen should be supplied, and capillary blood glucose performed.
Acutely intoxicated patients posing a danger to themselves and hospital personnel require chemical and physical restraints. Methamphetamine increases muscular tone through CNS agitation that may lead to muscle breakdown (rhabdomyolysis, hyperkalemia, acidosis), hyperthermia, renal failure, and death. It is important to note that the majority of the morbidity of acute methamphetamine intoxication is due to CNS agitation and can be prevented and treated with CNS sedatives. Physically restraining an agitated patient without concomitant pharmacological restraint may exacerbate the hyperthermia and muscle breakdown and has been associated with increased morbidity and mortality.
The mainstay of treatment in methamphetamine overdose is the reversal of CNS adrenergic hyperactivity. (See Table 5.) This can be accomplished with GABAA agonists such as benzodiazepines, barbiturates, etomidate, and propofol, or with dopamine antagonists, such as droperidol or ziprasidone. Droperidol has been shown to be more effective than midazolam in sedating the methamphetamine intoxicated patient,50 however concerns over QT prolongation as well as anticholinergic side effects do exist. Other antipsychotic agents, such as ziprasidone, have been used with considerable efficacy in the undifferentiated (largely alcoholic) population, but have not been specifically tested in methamphetamine intoxication.51 Large doses of medication, including continuous infusions, often are required in severely agitated patients. Physicians should consider endotracheal intubation, mechanical ventilation, and pharmacologic paralysis for patients with hyperthermia, persistent hypertension, or combative behavior despite pharmacological interventions.
| Table 5. Treatment Agents |
|
Aggressive early management of these signs and symptoms will help prevent the occurrence of adverse sequelae such as hyperthermia, acidosis, hyperkalemia, rhabdomyolysis with resultant renal failure, myocardial ischemia, and secondary trauma.
These guidelines apply to pediatric patients, with the caveat that propofol infusions often are avoided due to the potential for hypotension and lactic acidosis with long-term use. Pediatric patients should receive the same GABA-agonist drugs for treatment. Other sedatives, such as chloral hydrate, diphenhydramine, and clonidine, all have adverse effects at the high doses required to maintain adequate sedation. Benzodiazepines can cause disinhibition in pediatric patients, but this can be treated by administering larger doses of benzodiazepines, concomitant use of other GABA agonists (e.g., barbiturates), or the use of a dopamine receptor antagonist in a low dose.
Seizures related to methamphetamine intoxication should be treated with GABA-agonists. Sodium channel blockade via anticonvulsants such as phenytoin and carbamazepine are unlikely to be effective.
Methamphetamine Body Stuffers. Body stuffers are individuals who hastily ingest or insert into bodily orifices poorly packaged or unpackaged drugs in an effort to evade police detection. The packaging, which can consist of plastic wrappers, baggies, glass vials, or aluminum foil, is not always radioopaque. Hence, x-ray studies (e.g., KUB) have poor sensitivity (0-9%) and specificity for drug packets.52,53 Additionally, although CT or ultrasound may occasionally detect packets, they are neither sensitive nor specific and cannot be relied upon to diagnose or evaluate ingestions.52,54-57
Due to the unpredictable nature of packet passage, unreliable patient histories, and high morbidity and mortality resulting from these ingestions, the safest course of treatment is to observe a patient for at least 24 hours post-ingestion, and possibly up to 36-48 hours.53 A cathartic agent such as polyethylene glycol (Go Lytely) can be administered at a rate of 1-2 liters per hour (in adults), assuming the patient has normal bowel anatomy and function and is protecting his or her airway. Of note, there is no definitive evidence that whole bowel irrigation decreases morbidity and mortality, and it is possible that polyethylene glycol may increase the dissolution and absorption of methamphetamine. Charcoal can be given at the same time as the cathartic. If the patient is known to have concomitantly overdosed on an agent that decreases bowel motility, such as antihistamines, opiates or opioids, or anticholinergic agents, additional observation time is warranted. Direct observation of patients is necessary as patients may attempt to re-ingest packets that pass through the gastrointestinal tract.
If life-threatening intoxication, bowel perforation, or mesenteric ischemia occurs, emergent surgery may be required for removal of the ruptured and unruptured packages. Endoscopy and colonoscopy may occasionally be employed in the evaluation of the stable methamphetamine body stuffer; however, there is a significant risk of package rupture and a surgical team should be standing by.
Patients Presenting to the Emergency Department from a Meth Lab. Patients may present to the ED directly from a methamphetamine laboratory with an acute exposure to the chemicals that are involved in its manufacture. Chemicals that are used in methamphetamine production include largely caustic agents (e.g., sodium hydroxide, hydrogen chloride, ammonia), solvents (e.g., naphtha, methanol, ethanol, toluene), and flammable materials. In these cases, thermal and chemical (acid and alkali) burns as well as thermal and chemical pulmonary inhalational injury are the primary concerns.58
Patients who are contaminated with a chemical at a methamphetamine laboratory (e.g., chemical smell to skin/clothes, visible chemical on skin/clothes, or have skin or mucosal burns/irritation) should have their clothing removed and bagged, and initial patient stabilization should be performed. The patient should be decontaminated with soap and warm water for 5 minutes or until any chemical residue and particulate matter from skin and hair is removed.59,60 Any clothing or jewelry that is removed should be placed into a paper bag, and the paper bag then placed into a biohazard bag. Paper containers are preferred as plastic may contaminate evidence. Patients who were in a meth lab but are asymptomatic and had no known contamination with a chemical, do not require decontamination.
Patients presenting directly from a lab who have skin burns should have the skin pH of burns checked to determine if they are thermal or chemical injuries. If the skin pH is abnormal (normal skin pH = 5.5 with a range of 4.5-6.0), the skin should be copiously irrigated with water or saline solution and consideration be given to early consultation with a burn specialist.
Delayed pulmonary edema is a possibility in patients brought in from active methamphetamine labs. Exposure to anhydrous ammonia, phosphine, or other caustic gases, such as hydrochloric and hydrosulfuric acid, easily can occur, particularly if the patient was immobilized in an enclosed space.58 Carbon monoxide and cyanide exposure also should be considered in all patients arriving from explosions or fires. Phosphine exposure in methamphetamine laboratories has been reported,4 and may lead to immediate dysrhythmias, hypotension, and seizures, or delayed-onset pneumonitis.4
Evaluating Children from a Meth Lab (Abuse and Acute Issues). Although meth labs are notoriously dangerous environments for all inhabitants, the pediatric population is especially vulnerable. Along with the risk of explosions and chemical injuries, children are at risk of inadvertent or unsupervised ingestion, injection, and inhalation of methamphetamine. They often are the victims of parental neglect, and are at heightened risk of physical, emotional, and sexual abuse. They may face long-term health risks from repeated or prolonged exposure to environmental contamination.
When evaluating a child who has been living in a methamphetamine laboratory, the history should include the caregivers' and child's (if able) explanation of the presenting complaint, growth trends, length of exposure (if known), and the time and date of removal from exposure. Verbal children also should be interviewed separately from the caregiver if possible. On physical examination, the child's affect, height, and weight should be noted. A full head-to-toe exam should be performed with all clothing removed. Skin lesions, stains, or foreign substances on skin and clothing should be noted. For example, iodine, a common precursor chemical, causes reddish-orange staining and skin irritation.
Patients who are asymptomatic do not require laboratory testing, however urine drug screens and quantitative urine testing may be helpful in cases of abuse or for legal issues in proving an exposure to the drug. Basic electrolyte testing and complete blood count are recommended on suspected or confirmed cases of abuse to detect chronic illnesses. Specific instances may require additional testing including a urine pregnancy test (in female victims of abuse), STD testing (in symptomatic patients or victims of sexual abuse), and testing for specific exposures (e.g., blood lead concentration if the meth lab used lead acetate). (See Table 6.)
| Table 6. Recommneded Laboratory Testing |
|
Whether children or infants are brought in for evaluation, removed directly from methamphetamine laboratories, or are present with a caregiver suspected of illicit methamphetamine use, consultation with an in-house social worker, as well as referral to outside agencies, are recommended. These agencies include, but are not limited to, child care protective services, law enforcement agencies, and outside clinics for child abuse victims. The Drug Endangered Children program (DEC), a national initiative for children with parents and guardians involved with illegal drugs, was designed to unite law enforcement officers with child welfare workers to unify and standardize the care that these children receive. These programs are expanding across the country, and information about them can be accessed on the internet at www.nationaldec.org.
Chest Pain/Stimulant Effects. Patients with methamphetamine-induced chest pain should be treated with oxygen and have a laboratory and ECG evaluation initiated. Patients should be given aspirin provided that there are no contraindications, such as intracranial hemorrhage, aortic dissection, and aspirin allergy. Patients who are agitated or tachycardic should be treated with a sedative/hypnotic agent preferentially over beta blockade. As methamphetamine acts centrally to cause agitation and cardiovascular effects, therapy should be aimed at decreasing the CNS hyperstimulation. Although there is little data to guide therapy, beta blockers should be avoided if possible if the patient is methamphetamine intoxicated because of the possibility of an unopposed alpha effect (i.e., coronary vasospasm). Although this effect has never been documented during methamphetamine intoxication, there is evidence of unopposed alpha effect in cocaine intoxication. It therefore seems reasonable to be cautious when treating methamphetamine-intoxicated chest pain patients with beta blockade. Sedation can be initiated with a GABAA agonist agent (e.g., midazolam or lorazepam) or with a dopamine receptor antagonist (e.g., droperidol or ziprasidone).51 In studies of patients who were not having chest pain, sedation with droperidol was slightly superior to midazolam and there were no differences in heart rate or blood pressure changes.50,61
Psychosis. Psychosis, whether from acute or chronic methamphetamine usage, can be treated with antipsychotic agents such as haloperidol, droperidol, ziprasidone, and olanzapine. Atypical antipsychotic agents, and newer agents such as aripiprazole, have a lower risk of dystonia and other extrapyramidal side effects, but have not been studied.
Skin Infections. Abscesses and ulcers resulting from trauma, injection drug use, and skin picking should be considered to be contaminated with flora from many sources. Users may lick needles prior to subcutaneous injection, introducing anaerobic species and oral flora such as Eikenella corrodens into wounds.40,41 Due to the polymicrobial nature of these types of skin infections,40,41 the high potential for an immunocompromised host, and the prevalence of MRSA,62 broad-spectrum antibiotic coverage is recommended, along with an agent to combat MRSA. All incised wounds should be cultured.
Meth Mouth. Meth mouth is a chronic syndrome, however patients may present to the ED with a variety of acute complaints: pain from dental caries, dental fractures, or dental abscesses. The acute therapy depends on the presentation and is not changed by their methamphetamine use and likely involves antibiotics, pain medication, and referral to definitive dental care.
It is important to explain the chronic cause of the patient's symptoms and refer the patient for rehabilitation if he or she is receptive, as decreased exposure to methamphetamine will likely slow the progression of decay. Patients may be counseled about cessation of drug use and appropriate dental hygiene, and trying to drink 8-10 glasses of water (not sugared beverages) per day to prevent dry mouth.44 Once in dental care, the patient may be treated with dental extractions, topical concentrated fluoride treatments, or even pharmacologic therapy for xerostomia (e.g., pilocarpine).44
Rehabilitation/Counseling. Between 1993 and 2003, the national treatment admission rate for methamphetamine and amphetamine abuse increased from 13 admissions to 56 admissions per 100,000 population aged 12 and older.63 The highest admission rates were in Oregon, Hawaii, Iowa, California, Wyoming, Utah, Nevada, Washington, Montana, Arkansas, Nebraska, and Oklahoma.63 Rates for Northeastern states were 5 or fewer per 100,000 population.63 Clearly, methamphetamine is an increasing problem for rehabilitation and detoxification facilities, but from an emergency medicine perspective, is it worth referring patients to rehabilitation?
Although the short-term completion rate of outpatient or inpatient rehabilitation is only 30% and 50%, respectively,64 it seems reasonable to refer methamphetamine-abusing patients to appropriate treatment programs, if they are receptive. A multi-faceted approach is likely necessary, but unfortunately often is not available. Psychosocial and behavioral therapies, as well as antidepressant medications, may increase the effectiveness of rehabilitation therapies.64,65
Conclusion
Methamphetamine has gained a strong foothold in America's drug culture due to the simplicity of its production and the duration of its clinical effects. These very characteristics render it an extremely destructive drug to individuals, families, communities, and the environment. Methamphetamine-related disorders now make up a significant portion of the ED census in endemic areas. Despite legislative attempts to decrease usage, it appears that methamphetamine use and abuse continues to increase.
References
1. Anglin MD, Burke C, Perrochet B, et al. History of the methamphetamine problem. J Psychoactive Drugs 2000;32:137-141.
2. Derlet RW, Heischober B. Methamphetamine: Stimulant of the 1990s? West J Med 1990;153:625-628.
3. Burgess JL. Phosphine exposure from a methamphetamine laboratory investigation. Clin Toxicol 2001;39:165-168
4. Cunningham JK, Liu L. Impacts of federal precursor chemical regulations on methamphetamine arrests. Addiction 2005;100:479-488.
5. House of Representatives, Report 109-333, "USA PATRIOT Improvement and Reauthorization Act of 2005," Title VII: Combat Methamphetamine Epidemic Act of 2005, Section 711: Scheduled listed chemical products; restrictions on sales quantity, behind-the-counter access, and other safeguards. December 8, 2005. Signed into law March 9, 2006. Effective September 30, 2006.
6. Cunningham JK, Liu LM. Impacts of federal ephedrine and pseudoephedrine regulations on methamphetamine-related hospital admissions. Addiction 2003;98:1229-1237.
7. Reuter P, Caulkins JP. Does precursor regulation make a difference? Addiction 2003;98:1177-1179.
8. Northern Ice: Stopping Methamphetamine precursor chemical smuggling across the U.S.-Canada border. Hearing before the subcommittee on criminal justice, drug policy and human resources of the committee on Governmental Reform, U.S. House of Representatives. Serial No. 108-284. U.S. Government Printing office, Washington, DC, April 20, 2004.
9. 35 million China-produced pseudoephedrine tablets seized from cargo at Port of Long Beach, California. Microgram Bulletin 2005; 38(1): 4.
10. Johnston LD, O'Malley PM, Bachman JG, et al. Monitoring the future national survey results on drug use, 1975-2004. Volume II: College students and adults ages 19-45 (NIH Publication No. 05-5728). Bethesda, MD: National Institute on Drug Abuse, 2005.
11. The NSDUH (National Survey on Drug Use and Health) Report: Methamphetamine Use, Abuse, and Dependence: 2002, 2003, and 2004. September 16, 2005. Office of Applied Studies, Substance Abuse and Mental Health Services Administration (SAMHSA).
12. National Drug Intelligence Center. Information bulletin. MSM—Methamphetamine Cutting Agent of Choice. June 2001. NDIC Document ID: 2001-L0424-005.
13. Hendrickson RG, Martineau B, Morocco AP, et al. Adulterants and contaminants in cocaine and heroin samples. J Toxicol Clin Toxicol 2002;40:654.
14. Office of National Drug Control Policy (ONDCP), Drug Policy Information Clearinghouse. Methamphetamine. Document No. NCJ - 175677, May 1999.
15. National Drug Intelligence Center (NDIC), United States Department of Justice (USDOJ). Methamphetamine Drug Threat Assessment. Document ID: 2005-Q0317-009. March 2005.
16. Hanson GR. National Institute on Drug Abuse, Research Report Series. Methamphetamine Abuse and Addiction. National Institutes of Health (NIH) publication Number 02-4210, January 2002.
17. Florin SM, Kuczenski R, Segal DS. Regional extracellular norepinephrine responses to amphetamine and cocaine and effects of clonidine pretreatment. Brain Res 1994;654:53-62.
18. Kuczenski R, Segal DS. Differential effects of amphetamine and dopamine uptake blockers (cocaine, nomifensine) on caudate and accumbens dialysate dopamine and 3-methoxytyramine. J Pharm Exper Ther 1992;262:1085-1094.
19. Newton TF, DeLaGarza R II, Kalechstein AD, et al. Cocaine and methamphetamine produce different patterns of subjective and cardiovascular effects. Pharm Biochem Behav 2005;82:90-97.
20. Sulzer D, Chen TK, Lau YY, et al. Amphetamine redistributes dopamine from synaptic vesicles to the cytosol and promotes reverse transport. J Neurosci 1995;15:4105-4108.
21. Hoffman BB. Catecholamines, sympathomimetic drugs, and adrenergic receptor antagonists. In: Hardman JG, Limbird LE, eds. Goodman and Gilman's The Pharmacological Basis of Therapeutics. 10th edition. New York: McGraw-Hill; 2001:235-237.
22. Mateo Y, Budygin EA, Hohn CE, et al. Role of serotonin in cocaine effects in mice with reduced dopamine transporter function. Proc Natl Acad Sci USA 2004;101:372-377.
23. Kim I, Oyler JM, Moolchan ET, et al. Urinary pharmacokinetics of methamphetamine and its metabolite, amphetamine following controlled oral administration to humans. Ther Drug Monit 2004;26:664-672.
24. Quinn DI, Wodak A, Day RO. Pharmacokinetic and pharmacodynamic principles of illicit drug use and treatment of illicit drug users. Clin Pharmacokinet 1997;33:344-400.
25. Perez-Reyes M, White WR, McDonald SA, et al. Clinical effects of daily methamphetamine administration. Clin Neuropharmacol 1991;14:352-358.
26. McGee SM, McGee DN, McGee MB. Spontaneous intracerebral hemorrhage related to methamphetamine abuse: Autopsy findings and clinical correlation. Am J Forensic Med Pathol 2004;25:334-337.
27. McGregor C, Srisurapanont M, Jittiwutikarn J, et al. The nature, time course and severity of methamphetamine withdrawal. Addiction 2005;100:1320-1329.
28. Richards JR, Bretz SW, Johnson EB, et al. Methamphetamine abuse and emergency department utilization. West J Med 1999;17:198-202.
29. Ohta K, Mori M, Yoritaka A, et al. Delayed ischemic stroke associated with methamphetamine use. J Emerg Med 2005;28:165-167.
30. Logan BK. Methamphetamine and driving impairment. J Forensic Sci 1996;41:457-464.
31. Ellinwood E. Assault and homicide associated with amphetamine abuse. Am J Psychiatry 1971;127:90-95.
32. Hando J, Top L, Hall W. Amphetamine-related harms and treatment preferences of regular amphetamine users in Sydney, Australia. Drug Alcohol Depend 1997;47:105-113.
33. Packe GE, Garton MJ, Jennings K. Acute myocardial infarction caused by intravenous amphetamine abuse. Br Heart J 1990;64:23-24.
34. Furst SR, Fallon SP, Reznik GN, et al. Myocardial infarction after inhalation of methamphetamine. N Engl J Med 1990;323:1147-1148.
35. Ragland AS, Ismail Y, Arsura EL. Myocardial infarction after amphetamine use. Am Heart J 1993;125:247-249.
36. Bashour TT. Acute myocardial infarction resulting from amphetamine abuse: A spasm-thrombus interplay? Am Heart J 1994;128:1237-1239.
37. Farnsworth TL, Brugger CH, Malters P. Myocardial infarction after intranasal methamphetamine. Am J Health Syst Pharm 1997;54:586-587.
38. Yui K, Ikemoto S, Ishiguro T, et al. Studies of amphetamine or methamphetamine psychosis in Japan: Relation of methamphetamine psychosis to schizophrenia. Ann New York Acad Sci 2000;914:1-12.
39. Yui K, Ishiguro T, Goto K, et al. Susceptibility to subsequent episodes in spontaneous recurrence of methamphetamine psychosis. Ann New York Acad Sci 2000;914:292-302.
40. Ebright JR, Pieper B. Skin and soft tissue infections in injection drug users. Infect Dis Clin North Am 2002;16:697-712.
41. Talan DA, Summanen PH, Finegold SM. Ampicillin/sulbactam and cefoxitin in the treatment of cutaneous and other soft-tissue abscesses in patients with or without histories of injection drug abuse. Clin Infect Dis 2000;31:464-471.
42. Shaner JW, Kimes N, Saini T, et al. "Meth mouth": Rampant caries in methamphetamine abusers. AIDS Pat Care STDs 2006;20:146-150.
43. Richards JR, Brofeldt BT. Patterns of tooth wear associated with methamphetamine use. J Periodontol 2000;71:1371-1374.
44. Rhodus NI, Little JW. Methamphetamine abuse and "meth mouth." NW Dentistry 2005;84:1-17.
45. Saini T, Edwards PC, Kimmes NS, et al. Etiology of xerostomia and dental caries among methamphetamine abusers. Oral Health Prev Dent 2005:3:189-195.
46. Howe AM. Methamphetamine and childhood and adolescent caries. Austral Dent J 1995;40:340.
47. Di Cugno F, Perec CJ , Tocci AA. Salivary secretion and dental caries: Experience in drug addicts. Arch Oral Biol 1981;26:363-367.
48. Oyler JM, Cone EJ, Joseph Jr. RE, et al. Duration of detectable methamphetamine and amphetamine excretion in urine after controlled oral administration of methamphetamine to humans. Clin Chem 2002;48:1703-1714.
49. Cook CE, Jeffcoat AR, Sadler BM, et al. Pharmacokinetics of oral methamphetamine and effects of repeated daily dosing in humans. Drug Metab Disp 1992;20:856-862.
50. Richards JR, Derlet RW, Duncan DR. Methamphetamine toxicity: Treatment with a benzodiazepine versus a butyrophenone. Eur J Emerg Med 1997;4:130-135.
51. Martel M, Serzinger A, Miner J, et al. Management of acute undifferentiated agitation in the emergency department: A randomized, double-blind trial of droperidol, ziprasidone, and midazolam. Acad Emerg Med 2005;12:1167-1172.
52. Eng JGH, Aks SE, Waldron R, et al. False-negative abdominal CT scan in a cocaine body stuffer. Am J Emerg Med 1999;17:702-704.
53. Hendrickson RG, Horowitz BZ, Norton RL, et al. "Parachuting" meth: A novel delivery method for methamphetamine and delayed-onset toxicity from "body stuffing." Clin Toxicol 2006;44:379-382.
54. Cranston PE, Pollack CV, Harrison RB. CT of crack cocaine ingestion. J Comput Assist Tomogr 1992;16:560-563.
55. Pollack CV Jr, Biggers DW, Carlton FB, et al. Two crack cocaine body stuffers. Ann Emerg Med 1992;21:1370-1380.
56. Marc B, Baud FJ, Aelion MJ, The cocaine body-packer syndrome: Evaluation of a method of contrast study of the bowel. J Forensic Sci 1990;35:345-355.
57. Hierholzer J, Cordes M, Tantow H. Drug smuggling by ingested cocaine-filled packages: Conventional x-ray and ultrasound. Abdom Imaging 1995;20:330-338.
58. Santos AP, Wilson AK, Hornung CA, et al. Methamphetamine laboratory explosions: A new and emerging burn injury. J Burn Care Rehabil 2005;26:228-232.
59. Occupational Safety and Health Administration (OSHA) Best Practices for Hospital-Based First Receivers of Victims from Mass Casualty Incidents Involving the Release of Hazardous Substances.: Occupational Safety and Health Administration (OSHA); 2004:1-32.
60. Houston M, Hendrickson RG. Decontamination. Crit Care Clin 2005;21:653-672.
61. Richards JR, Derlet RW, Duncan DR. Chemical restraint for the agitated patient in the emergency department: Lorazepam versus droperidol. J Emerg Med 1998;16:567-573.
62. Moran GJ, Amii RN, Abrahamian FM, et al. Methicillin-resistant Staphylococcus aureus in community-acquired skin infections. Emerg Infect Dis 2005;11:928-930.
63. The DASIS (Drug and Alcohol Services Information System) Report: Trends in Methamphetamine/Amphetamine Admissions to Treatment: 1993-2003. 2006; 9. Office of Applied Studies, Substance Abuse and Mental Health Services Administration(SAMHSA).
64. Brecht ML, Greenwell L, Anglin MD. Methamphetamine treatment: Trends and predictors of retention and completion in a large state treatment system (1992-2002). J Subst Abuse Treatment 2005;29:295-306.
65. Galloway GP, Newmeyer J, Knapp T, et al. A controlled trial of imipramine for the treatment of methamphetamine dependence. J Subst Abuse Treat 1996;13:493-497.
Over the last two decades, methamphetamine use has increased drastically in the United States and it has become one of the most popular illicit drugs in the country, particularly along the West Coast and in the Mid West.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.