Calcium for Weight Management
Calcium for Weight Management
By Lynn Keegan, RN, PhD, AHN-BC, FAAN. Dr. Keegan is Director, Holistic Nursing Consultants, Port Angeles, WA; she reports no consultant, stockholder, speaker's bureau, research, or other financial relationships with companies having ties to this field of study.
Obesity is increasing in the united states in epidemic proportions.1 Overweight Americans are well aware of the plethora of diets and exercise programs for weight management. Most people with weight issues have tried many courses of action.
Recent epidemiologic research suggests that dairy product intake or its components (calcium, vitamin D, and amount or source of protein) are associated with lower body weight or body fat. Clinical intervention trials designed to test this association during weight loss are promising, but still controversial.2
Mechanism of Action
The role of calcium in weight loss and management may be dependent upon the dietary environment. It is theorized that during periods of over-consumption of an energy-dense diet a high-calcium diet attenuates body fat accumulation and weight gain; whereas during caloric restriction, a high-calcium diet increases fat breakdown and preserves metabolism, thereby markedly accelerating weight and fat loss. Researchers believe that this effect is mediated primarily by circulating calcitriol, which regulates adipocyte intracellular Ca2+. Studies of human adipocyte metabolism demonstrate a key role for intracellular Ca2+ in regulating lipid metabolism and triglyceride storage: Increased intracellular Ca2+ stimulates lipogenic gene expression and lipogenesis and suppresses lipolysis, resulting in adipocyte lipid filling and increased adiposity. The increased calcitriol produced in response to low-calcium diets stimulates adipocyte Ca2+ influx and, consequently, promotes adiposity, while higher-calcium diets inhibit lipogenesis; promote lipolysis, lipid oxidation, and thermogenesis; and inhibit diet-induced obesity in mice.3
It is interesting that dairy sources of calcium exert markedly greater effects in attenuating weight and fat gain and accelerating fat loss. This augmented effect of dairy products versus supplemental calcium has been localized, in part, to the whey fraction of dairy and is likely due to additional bioactive compounds, such as angiotensin converting enzyme (ACE) inhibitors and the rich concentration of branched chain amino acids, which act synergistically with calcium to attenuate adiposity. However, these compounds do not fully account for the observed effects, as they are more readily absorbed and therefore have significantly greater bioactivity than do other compounds. These concepts are supported by epidemiological data and recent clinical trials showing that diets that include at least three daily servings of dairy products result in significant reductions in body fat mass in obese humans in the absence of caloric restriction and marked acceleration of weight and body fat loss secondary to caloric restriction compared to low-dairy diets.3
Studies in transgenic mice have demonstrated that calcium influences adipocyte metabolism. High-calcium intake depresses levels of parathyroid hormone and 1,25-hydroxyvitamin D. These decreased hormone levels decrease intracellular calcium, thereby inhibiting lipogenesis and stimulating lipolysis. High dietary calcium intakes increase fecal fat excretion and may increase core body temperature. Calcium from dairy products seems to have more of an impact than calcium from dietary supplements.1 The mechanisms proposed to mediate the putative effect of dietary calcium include the formation of fecal fatty acid complexes to reduce fat absorption and the regulation of energy metabolism, including lipolysis from adipocytes and fatty acid oxidation, through the calciotropic hormones, parathyroid hormone, and 1,25-dihydroxyvitamin D. Increased energy expenditure, increased satiety, or a shift from fat to lean mass must accompany these changes in lipid metabolism to achieve changes in fat mass.2
Clinical Trials
Studies suggest that high-dairy and high-fiber/low-glycemic index diets may facilitate weight loss, but data are conflicting.4 One animal and one human study support the hypothesis, other studies refute or simply do not support it.
Animal Studies
One group of researchers fed low-calcium (0.4% Ca) and high-calcium (1.2% Ca from CaCO3) obesity-promoting (high-sucrose/high-fat) diets to aP2-agouti transgenic mice and assessed regulation of reactive oxygen species (ROS) production in adipose tissue and skeletal muscle. They discovered that mice on the high-calcium diet gained 50% as much body weight and fat as mice on the low-calcium diet. The high-calcium diet significantly reduced adipose intracellular ROS production by 64% and 18% and inhibited adipose tissue nicotinamide adenine dinucleotide phosphate oxidase expression by 49% and 63% in visceral and subcutaneous adipose tissue, respectively. Although this study supports a potential role for dietary calcium in the regulation of obesity-induced oxidative stress,5 it is one of the few studies showing a positive correlation in support of the use of calcium for weight management, and it was done on mice.
Human Studies
One group of researchers performed two randomized trials in obese African-American adults and found positive effects of dairy consumption on adiposity and body composition. In the first (weight maintenance), 34 subjects were maintained on a low-calcium (500 mg/d)/low-dairy (< 1 serving/d) or high-dairy (1,200 mg Ca/d including three servings of dairy) diet with no change in energy or macronutrient intake for 24 weeks. In the second trial (weight loss), 29 subjects were similarly randomized to the low- or high-dairy diets and placed on a caloric restriction regimen (-500 kcal/d). In the first trial, body weight remained stable for both groups throughout the maintenance study. The high-dairy diet resulted in decreases in total body fat, trunk fat, insulin, and blood pressure and an increase in lean mass, whereas there were no significant changes in the low-dairy group. In the second trial, although both diets produced significant weight and fat loss, weight and fat loss on the high-dairy diet were approximately twice as high, and loss of lean body mass was markedly reduced compared with the low-dairy diet. In essence, substitution of calcium-rich foods in isocaloric diets reduced adiposity and improved metabolic profiles in obese African Americans without energy restriction or weight loss and augmented weight and fat loss secondary to energy restriction.6
Another group of researchers found no association between calcium intake and weight management in Arizona's obesity-prone population of Pima Indians. Sixty-five Pima Indian adults (35 men/30 women, age 33 ± 8 years) participated in a study of eating behavior and 78 Pima Indian children (36 boys/42 girls, age 10.4 ± 0.3 years) participated in a study of childhood obesity. Height and weight were measured, and body composition was determined by dual-energy X-ray absorptiometry. Food intake in adults was assessed using the Block 1998 Food Questionnaire; food intake in children was assessed using a 24-hour recall with parental assistance. The results found that in adults, mean energy intake was 3,163 ± 1,037 kcal/d, mean percentage of energy from fat was 41% ± 7%, and calcium intake was 914 ± 333 mg/d. In children, mean energy intake was 1,988 ± 733 kcal/d, mean percentage of energy from fat was 36% ± 9%, and calcium intake was 637 ± 352 mg/d, half the recommended daily intake for this age group. There were no significant associations between calcium intake and body weight, or body mass index (BMI) in either adults or children, respectively. One explanation for the lack of association between reported calcium intake and body size in Pima Indians may be that the high-fat, high-energy diet consumed by this population overwhelmed the "anti-obesigenic" effect of calcium.7
A cross-sectional study examined possible associations of intakes of calcium and dairy products to BMI in young Japanese women and found no relationship. A total of 1,905 female Japanese dietetic students who were 18-20 years of age had their dietary intake assessed over a one-month period with a validated, self-administered diet history questionnaire. BMI was computed using self-reported weight and height. BMI was compared among quartiles of energy-adjusted intakes (per 1,000 kcal) of calcium and dairy products while controlling for intakes of protein, fat, and dietary fiber, self-reported rate of eating, and other nondietary variables. Results showed a mean BMI (± SD) of 20.8 ± 2.6 kg/m2. Mean estimated intakes were 268 ± 93 mg/1,000 kcal for calcium and 80 ± 63 g/1,000 kcal for dairy products. Intakes of calcium and dairy products were not significantly associated with BMI. These results were also observed after excluding 481 energy under- and over-reporters for calcium and dairy products. Intakes of calcium and dairy products may not necessarily be associated with BMI among young Japanese women who not only are relatively lean but also have a relatively low intake of calcium and dairy products.8
The purpose of yet another study was to compare weight and body fat loss on a calorie-restricted, low-dairy (CR) vs. high-dairy (CR+D) diet. Fifty-four subjects were randomly assigned to calorie-restricted (-500 kcal/d) low-dairy calcium (n = 29; approximately 1 serving dairy/d, 500 mg/d calcium) or high-dairy calcium (n = 25; 3-4 servings dairy/d, 1,200-1,400 mg/d calcium) diets for 12 months. Main outcome measures included change in weight and body fat. There were no significant differences between groups at baseline. At 12 months, weight and body fat loss were not significantly different. These findings suggest that a high-dairy calcium diet does not substantially improve weight loss beyond what can be achieved in a behavioral intervention.9
Still another study showed no correlation between weight loss and body fat and diets high in dairy, or high in dairy and fiber and low in glycemic index, when compared to a standard diet. Ninety obese subjects were randomized to one of three diets designed to provide a calorie deficit of 500 calories/d over a 48-week period. The study compared a moderate-calcium diet with a high-calcium diet. Significant weight and fat loss occurred with all three diets. A diet with 1,400 mg of calcium did not result in greater weight loss than a diet with 800 mg of calcium. A diet with 1,400 mg of calcium, increased fiber content, and fewer high-glycemic index foods did not result in greater weight loss than the standard diet with 800 mg of calcium. Lipid profile, high-sensitivity C-reactive protein, leptin, fasting glucose, and insulin improved significantly, but there were no significant differences between the experimental diets and the control diet. These researchers found no evidence that diets containing more than 800 mg of calcium from dairy products, or diets high in fiber and low in glycemic index foods, enhance weight reduction beyond what is seen with calorie restriction alone.4
In a related study, overweight postmenopausal women proved to be more susceptible to bone loss with weight reduction than previously studied obese women. The influence of energy restriction and calcium intake on bone mineral density was assessed in 66 individuals. Weight reduction resulted in bone loss at several sites in women consuming 1 g Ca/d and was mitigated with higher calcium intake at 1.7 g/d.10
Finally, Bowen et al compared the effects of two high-protein diets that differed in dietary calcium and protein source on weight loss, body composition, glucose and lipid metabolism, liver function, fibrinolysis, endothelial function, and blood pressure.11 This randomized, parallel study (12 weeks of energy restriction, four weeks of energy balance) of high-dairy protein/high-calcium (2,400 mg Ca/d) and high mixed protein/moderate-calcium (500 mg Ca/d) diets (5.5 MJ/d, 34% protein, 41% carbohydrate, 24% fat) included 50 healthy, overweight (age 25-64 years; BMI 25-35 kg/m2) males (n = 20) and females (n = 30). Loss of total weight (-9.7 ± 3.8 kg), fat mass (-8.3 ± 0.4 kg), and lean mass (-1.6 ± 0.3 kg) were independent of dietary group. Improvements in fasting insulin, lipids, systolic/diastolic blood pressure, and markers of liver function, fibrinolysis, and endothelial function were independent of dietary intervention. This study, like others, found that increased intake of dietary calcium/dairy foods in an energy-restricted, high-protein diet does not affect weight loss or body composition.
Dosage and Implementation
It has yet to be learned what amount of calcium would be optimal for weight management and what influence, if any, an individual's current calcium intake and existing weight might play. Additionally, it is still difficult to pinpoint which component(s) in dairy foods have a role in weight reduction and whether they act alone or in synergism with calcium.12
The Food and Nutrition Board of the Institute of Medicine set the tolerable upper level of intake for calcium in adults at 2,500 mg/d.13
Calcium product labels should state the amount of elemental calcium in each tablet, i.e., 500 mg of elemental calcium in each 1,250 mg tablet. The amount of elemental calcium should be used to calculate true daily intake.
Products made from calcium carbonate are often recommended because they contain the highest percentage of elemental calcium per mg of calcium source.14 Calcium carbonate is best absorbed when taken with a meal or with a source of additional acid such as orange juice. Calcium citrate, on the other hand, usually provides less calcium per caplet than calcium carbonate, but it does not require extra stomach acid and can be taken anytime, even on an empty stomach.
Safety and Cautions
Abnormally elevated blood calcium (hypercalcemia) resulting from the overconsumption of calcium has never been documented to occur from foods, only from calcium supplements. Mild hypercalcemia may occur without symptoms, or may result in loss of appetite, nausea, vomiting, constipation, abdominal pain, dry mouth, thirst, and frequent urination. More severe hypercalcemia may result in confusion, delirium, coma, and if not treated, death. Hypercalcemia has been reported only with the consumption of large quantities of calcium supplements usually in combination with antacids, particularly in the days when peptic ulcers were treated with large quantities of milk, calcium carbonate (antacid), and sodium bicarbonate (absorbable alkali).15 This condition was termed milk alkali syndrome, and has been reported at calcium supplement levels of 1.5-16.5 g/d for two days to 30 years. Since the treatment for peptic ulcers has changed, the incidence of this syndrome has decreased considerably.13
Although the risk of forming kidney stones is increased in individuals with abnormally elevated urinary calcium (hypercalciuria), this condition usually is not related to calcium intake, but rather to increased excretion of calcium by the kidneys. Overall, increased dietary calcium has been associated with a decreased risk of kidney stones. However, in a large prospective study, the risk of developing kidney stones in women taking supplemental calcium was 20% higher than in those who did not.16 This effect may be related to the fact that calcium supplements can be taken without food, eliminating the beneficial effect of decreasing intestinal oxalate absorption.
Although dairy products have been found to be associated with an elevated risk of prostate cancer, studies investigating the potential effect of calcium are limited, and findings are inconsistent. A recent French study tested the relationship between the risk of prostate cancer and consumption of dairy products and calcium.17 The analysis included 2,776 men from the French SU.VI.MAX (Supplementation en Vitamines et Mineraux Antioxydants) prospective study, among whom 69 developed prostate cancer during the follow-up period. Food consumption was assessed at inclusion from repeated 24-hour records and nutrient intake was calculated using a food composition table. A higher risk of prostate cancer was observed among subjects with higher dairy product and calcium intake. Interestingly, they identified a harmful effect of yogurt consumption upon the risk of prostate cancer independent of the calcium content. These data support the hypothesis that dairy products have a harmful effect with respect to the risk of prostate cancer, largely related to calcium content. The higher risk of prostate cancer with linear increasing yogurt consumption seems to be independent of calcium and may be related to some other component.
Others find that higher milk intake has been relatively consistently associated with an increased risk of prostate cancer, especially advanced prostate cancer. Some data suggest that high intake of calcium might account for this association, but this relationship remains controversial. A Harvard study examined calcium intake in relation to prostate cancer risk using data from the Health Professionals Follow-up Study, a prospective cohort study of 47,750 male health professionals with no history of cancer other than nonmelanoma skin cancer at baseline.18 Researchers assessed total, dietary, and supplementary calcium intake in 1986, 1990, 1994, and 1998, using a validated food frequency questionnaire. Higher calcium intake was not appreciably associated with total or non-advanced prostate cancer but was associated with a higher risk of advanced and fatal prostate cancer. Dietary calcium and supplementary calcium were independently associated with an increased risk. For high-grade prostate cancer (Gleason > 7), an association was observed for high vs. low calcium, but a nonsignificant, inverse association was observed for organ-confined, low-grade prostate cancer. In a sample of this cohort, higher calcium intake was associated with lower circulating vitamin D levels. These findings suggest that calcium intakes exceeding 1,500 mg/d may be associated with a decrease in differentiation in prostate cancer and ultimately with a higher risk of advanced and fatal prostate cancer, but not with well-differentiated, organ-confined cancers.
A team from Tufts conducted a meta-analysis search of Medline for prospective studies published in English-language journals from 1966 through May 2005.19 They identified 12 publications that used total, advanced, or fatal prostate cancer as endpoints and reported associations as relative risks. Random-effects models were used to pool study results and to assess dose-response relationships between dairy product or calcium intakes and the risk of prostate cancer. Results showed that men with the highest intake of dairy products and calcium were more likely to develop prostate cancer than men with the lowest intake. Dose-response analyses suggested that dairy product and calcium intakes were each positively associated with the risk of prostate cancer, thus supporting the theory that high intake of dairy products and calcium may be associated with an increased risk of prostate cancer, although the increase appears to be small.
All three of these studies support the hypothesis that a high-calcium diet or supplements are not a good idea for men, especially those already diagnosed with prostate cancer.
Food Sources
Average dietary intakes of calcium in the United States are well below the adequate intake recommendation for every age and gender group, especially for females. Only about 25% of boys and 10% of girls ages 9-17 meet the adequate intake recommendations. Dairy foods provide 75% of the calcium in the American diet. However, it is typically during the most critical period for peak bone mass development that adolescents tend to replace milk with soft drinks.13,15
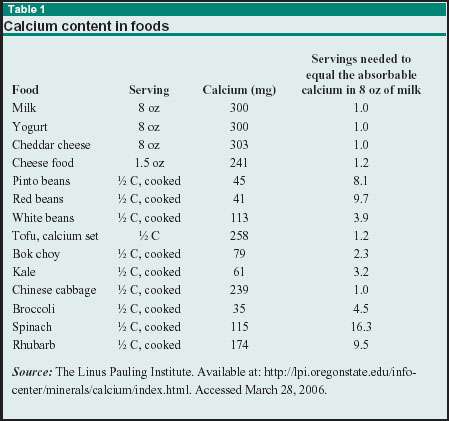
Dairy products represent rich and absorbable sources of calcium, but certain vegetables and grains also provide calcium. However, the bioavailability of that calcium must be taken into consideration.20 Table 1 lists a number of calcium-rich foods, along with their calcium content and the number of servings of that food required to equal the absorbable calcium from one glass of milk.
 |
Skim milk products provide as much calcium as whole milk with the added advantage of less fat and cholesterol. Some calcium-fortified soy beverages and orange juices may contain as much calcium as milk. Vegetables also provide calcium, as do fish products containing bones (canned salmon and sardines) and meat alternatives such as lentils and beans. However, some foods, such as those with excessive amounts of salt and caffeine, may cause calcium loss via excretion through the urine.
Although the calcium-rich plants in the kale family (broccoli, bok choy, cabbage, mustard, and turnip greens) contain calcium that is as bioavailable as that in milk, some food components have been found to inhibit the absorption of calcium. Oxalic acid, also known as oxalate, is the most potent inhibitor of calcium absorption, and is found in high concentrations in spinach and rhubarb and somewhat lower concentrations in sweet potato and dried beans. Phytic acid is a less potent inhibitor of calcium absorption than oxalate. Yeast possesses an enzyme (phytase) that breaks down phytic acid in grains during fermentation, lowering the phytic acid content of breads and other fermented foods. Only concentrated sources of phytate such as wheat bran or dried beans substantially reduce calcium absorption.15
Conclusion
Although the essentiality of calcium to bone health appears well established, the role of calcium and dairy product intake in obesity and weight management remains uncertain.7 In the studies cited above, however, there seems to be a preponderance of evidence that negates the relationship between calcium intake and weight loss. If dairy products or their components have an effect on altering fat mass, it is likely to be a small change that may have a substantial effect on the incidence of obesity over time.2 Based on much of the presently reported data, calcium, and even more so dairy foods, might help in weight reduction/maintenance when combined with energy-restricted diet. The scientific community is in agreement that there is a pressing need for large clinical trials to assess the effect of calcium on weight reduction and to investigate whether weight loss could be achieved more easily with calcium supplements or dairy products.
Recommendation
Considering the prevalence of overweight/obesity, its effects on public health, and the economic burden it entails, it is of crucial importance to develop effective weight loss and weight management strategies.
More research in this area is clearly necessary before specific recommendations can be made. However, given the calcium intake levels in the typical American diet and the need for calcium for bone health, a simple strategy to increase intake of low-fat dietary sources of calcium seems reasonable not only for those striving to reduce their weight, but for all patients.12 Again, men, especially those already diagnosed with prostate cancer, need to consult their health care provider before adding additional calcium to their diets; intakes above 600 mg/d may not be a good idea. Table 2 lists the recommended calcium intakes advocated by Osteoporosis Canada.
 |
The bottom line is that most women should consume about 1,000 mg/d of calcium, while those older than age 50 should strive for 1,500 mg/d. These are basic requirements and lower intake levels (< 600 mg/d) are advisable for men because of prostate cancer concerns. At this time no recommended requirements have been established for those using calcium for weight management. The state of the science for this concept is still too controversial and requires clarification.
References
1. Schrager S. Dietary calcium intake and obesity. J Am Board Fam Pract 2005;18:205-210.
2. Teegarden D. The influence of dairy product consumption on body composition. J Nutr 2005;135:2749-2752.
3. Zemel MB. The role of dairy foods in weight management. J Am Coll Nutr 2005;24(6 Suppl):537S-546S.
4. Thompson WG, et al. Effect of energy-reduced diets high in dairy products and fiber on weight loss in obese adults. Obes Res 2005;13:1344-1353.
5. Sun X, Zemel MB. Dietary calcium regulates ROS production in aP2-agouti transgenic mice on high-fat/high-sucrose diets. Int J Obes (Lond) 2006 Mar 7; [Epub ahead of print].
6. Zemel MB, et al. Effects of calcium and dairy on body composition and weight loss in African-American adults. Obes Res 2005;13:1218-1225.
7. Venti CA, et al. Lack of relationship between calcium intake and body size in an obesity-prone population. J Am Diet Assoc 2005;105:1401-1407.
8. Murakami K, et al. No relation between intakes of calcium and dairy products and body mass index in Japanese women aged 18 to 20 y. Nutrition 2006 Feb 22; [Epub ahead of print].
9. Harvey-Berino J, et al. The impact of calcium and dairy product consumption on weight loss. Obes Res 2005;13:1720-1726.
10. Riedt CS, et al. Overweight postmenopausal women lose bone with moderate weight reduction and 1 g/day calcium intake. J Bone Miner Res 2005;20:455-463. Epub 2004 Nov 29.
11. Bowen J, et. Effect of calcium and dairy foods in high protein, energy-restricted diets on weight loss and metabolic parameters in overweight adults. Int J Obes (Lond) 2005;29:957-965.
12. Ilich JZ. A lighter side of calcium: Role of calcium and dairy foods in body weight. Arh Hig Rada Toksikol 2005;56:33-38.
13. Institute of Medicine. Food and Nutrition Board. Calcium. Dietary Reference Intakes: Calcium, Phosphorus, Magnesium, Vitamin D, and Fluoride. Washington, DC: National Academy Press; 1997:71-145.
14. Osteoporosis Canada. Available at: www.osteoporosis.ca. Accessed March 30, 2006.
15. Weaver CM, Heaney RP. Calcium. In: Shils M, et al, eds. Nutrition in Health and Disease. 9th ed. Baltimore, MD: Williams & Wilkins; 1999:141-155.
16. Curhan GC, et al. Comparison of dietary calcium with supplemental calcium and other nutrients as factors affecting the risk for kidney stones in women. Ann Intern Med 1997;126:497-504.
17. Kesse E, et al. Dairy products, calcium and phosphorus intake, and the risk of prostate cancer: Results of the French prospective SU.VI.MAX (Supplementation en Vitamines et Mineraux Antioxydants) study. Br J Nutr 2006;95:539-545.
18. Giovannucci E, et al. A prospective study of calcium intake and incident and fatal prostate cancer. Cancer Epidemiol Biomarkers Prev 2006;15:203-210.
19. Gao X, et al. Prospective studies of dairy product and calcium intakes and prostate cancer risk: A meta-analysis. J Natl Cancer Inst 2005;97:1768-1777. Erratum in: J Natl Cancer Inst 2006;98:366.
20. Weaver CM, et al. Choices for achieving adequate dietary calcium with a vegetarian diet. Am J Clin Nutr 1999;70(3 Suppl):543S-548S.
Keegan L. Calcium for weight management. Altern Med Alert 2006;9(5):49-55.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
