Evaluation and Management of Appendicitis in the Emergency Department
Evaluation and Management of Appendicitis in the Emergency Department
Author: Stephen A. Shiver, MD, Assistant Professor of Emergency Medicine, Department of Emergency Medicine, Medical College of Georgia, Augusta.
Peer Reviewers: Ann M. Dietrich, MD, FAAP, FACEP, Associate Professor of Clinical Pediatrics, Ohio State University, Columbus; and Andrew D. Perron, MD, FACEP, FACSM, Residency Program Director and Associate Professor, Department of Emergency Medicine, Maine Medical Center, Portland.
Every medical student learns about the pathophysiology, symptoms, and signs of acute appendicitis, so the reader of this issue may legitimately ask, "Why is Emergency Medicine Reports covering this topic?" It is because acute appendicitis is a common disorder that continues to remain a diagnostic challenge despite clinical study during the past century and imaging advances in the past decade. Almost every practicing emergency physician likely has had the experience of hearing that a patient he or she discharged from the emergency department returned the next day and underwent surgery for acute appendicitis. Thus the challenge is to identify this disease in a timely and effective fashion out of the larger universe of patients who come to the emergency department with abdominal pain.
The author presents a clear and practical review of this condition, emphasizing the common uncertainties and dilemmas. If every patient presented like the classic textbook picture, then diagnosis would be clear. However, the textbook description is a theoretical construct derived from many patients; it is not specific for a single patient. It is the astute physician who can suspect the presence of appendicitis despite the lack of classic symptoms and signs.
I am old enough to remember when a "normal" white blood cell count was used, usually by general surgery residents who did not want to come to the emergency department to exclude the diagnosis of acute appendicitis. I have practiced long enough to see this approach applied to the ultrasound and computed tomography imaging studies that seem to be almost mandatory before calling the surgeon. The author (rightly, in my opinion) notes the limitations of the current imaging studies.
Acute appendicitis is a humbling disorder; we understand so much yet continue to miss some cases on initial assessment. Consider this review of appendicitis like an often-told sermon; we know the story well, but we all benefit from hearing it again.
—The Editor
History
Appendicitis has undoubtedly been present since antiquity. Drawings of the appendix by Leonardo DaVinci date back to the 15th century.1 Reports of appendiceal disease can be traced back to the early 1700s, with the initial report credited to a student of Boerhaave.2 Numerous other early reports of right lower quadrant inflammation exist, but the process remained poorly understood until the 19th century.
Harvard pathologist Reginald Fitz revolutionized the understanding of appendiceal inflammation in 1886 with the presentation of his landmark paper "Perforating Inflammation of the Vermiform Appendix: With Special Reference to its Early Diagnosis and Treatment."3 Fitz coined the term "appendicitis" and advocated surgical intervention at a time when the basic concepts of antisepsis and anesthesia were beginning to be understood. An ensuing explosion in scientific research on appendicitis followed, resulting in well over 2000 articles on the subject in the literature by the end of the 19th century.4 By the 1890s, appendectomy was well accepted by surgeons in the United States and was being performed safely on a regular basis.
Epidemiology
Appendicitis continues to be the most common acute surgical emergency in the United States, with approximately 250,000 cases annually. The estimated lifetime risk of acute appendicitis is approximately 7% in Western populations.5 Both genders are affected with near equal frequency. It is primarily a disease of adolescence and young adulthood, with the peak incidence occurring in the second and third decades of life. Though it can affect all age groups, it is much less common in children younger than 5 years of age and in adults older than 70 years of age.6
It is well established that the incidence of appendicitis is higher among Western industrialized nations than in the developing world. African studies have shown the rate of appendicitis to be only 10% of that seen in Great Britain, for example.7 The reason for this difference has long been thought to be due to decreased fiber intake among Westerners. However, some studies have failed to show a difference in the rate of appendicitis based on fiber intake alone.8 Thus, the observed differences in geographical incidence are likely multi-factorial in nature and not solely due to fiber intake.
Anatomy
The appendix is an outpouching of the cecum and is located in the right lower quadrant. It varies in length from 2 to 20 cm, with an average of 9 cm. Histologically, it is similar to the adjacent colon. Mucosa, submucosa, muscularis, and serosa are all present. One important feature that differentiates the appendix from the colon is the presence of lymphoid aggregates. Large numbers of lymphoid follicles are found in the appendix. Though the human appendix is considered a vestigial organ with no known function, the prominence of lymphoid tissue has led some investigators to suggest an immunologic role. No such function has ever been proved.9
Though the appendix consistently arises from the cecum, its exact position may vary significantly. A myriad of different positions have been described, including retrocecal, pelvic, subcecal, preilial, postilial, and paracolic. A postmortem analysis of 10,000 cases showed that the most common variant was retrocecal, occurring with a frequency of 65%.10 Series have shown the majority (69%) of cases of perforated or gangrenous appendicitis are associated with a retrocolic position.11 Such a "hidden" position is thought to result in later development of signs and symptoms, thus resulting in diagnostic delay and an increased incidence of complicating features such as perforation.
The blood supply is from the ileocolic artery, via the appendicular branch. Innervation is provided by the autonomic nervous system. No somatic pain fibers are found within the appendix itself, so pain secondary to appendiceal inflammation usually is poorly localized initially. It is not until the adjacent parietal peritoneum becomes inflamed that somatic pain fibers are activated, providing accurate localization to the right lower quadrant.
Pathophysiology
Luminal obstruction has long been postulated as the inciting event in the development of acute appendicitis. Such a mechanism explains some observations about the incidence of appendicitis, such as the infrequent occurrence in infancy. Infants are known to have a relatively wider appendiceal base than adults, thus rendering them less susceptible to luminal obstruction. Studies have shown, in fact, that luminal obstruction can be an inciting event.12 There are, however, some cases of appendicitis that do not appear to be consistent with the luminal obstruction model. In such cases, pathologic analysis has shown the appendiceal lumen to be patent. Though such cases clearly represent a minority, the precise pathophysiologic mechanism responsible for acute inflammation in the absence of luminal obstruction remains unclear.9
The exact cause of luminal obstruction is variable. Lymphoid hyperplasia and fecaliths have received the most attention and study. Lymphoid hyperplasia traditionally is thought to be responsible in younger age groups, whereas fecaliths are thought to be the offending agent in the older patient population. There are a myriad of potential causes for lymphoid hyperplasia including viral infections such as mononucleosis and bacterial infections such as salmonella and shigella. The term fecalith, or appendicolith, simply refers to inspissated stool or vegetable matter that may result in luminal obstruction.
In the usual state, particulate matter does not accumulate in the appendix due to an axial pressure gradient. Obstruction of the appendiceal lumen results in the entrapment of particulate matter and the inability of the appendix to clear normal secretions, such as mucus. The result is elevation of intraluminal pressure. The rising intraluminal pressure eventually occludes venous and lymphatic outflow, resulting in yet further congestion and pressure elevation. Eventually, arterial inflow is affected and ischemia ensues. Mucosal integrity becomes compromised, rendering the bowel wall susceptible to invasion by normal bacterial flora.13 If the process goes unchecked, gangrene and perforation occur. The time course is variable, but data suggest the onset of gangrene and perforation occur after a mean of 46 and 71 hours of abdominal pain, respectively.14
As mentioned above, bacterial invasion of the appendiceal wall does occur in acute appendicitis. However, it is important to recognize that microbes are not thought to be responsible for appendicitis per se. Rather, progressive ischemia results in a weakened mucosal barrier that then allows microbial invasion to occur. Though unclear in early microbiologic work, studies in the early 20th century showed that the secondary infectious process seen in acute appendicitis is polymicrobial.15 Both aerobic and anaerobic bacteria are isolated with regularity. Specifically, Bacteriodes fragilis and Escherichia coli are the most commonly occurring isolates and are found in greater than 70% of cases.6
Though most untreated cases of appendicitis result in perforation and clinical deterioration, spontaneous resolution appears to occur in some cases. The frequency of such an event is unknown.6 Perhaps the luminal obstruction somehow is relieved, and the inflammatory cascade resolves. Interestingly, a series of 1000 patients with acute appendicitis found that 9% reported similar symptoms previously that spontaneously resolved.16 Of course, it is not possible to know how many, if any, such patients actually had a prior episode of appendiceal inflammation.
Clinical Features
Appendicitis continues to be a diagnostic challenge despite all of the advances associated with 21st century medicine. In essence, it remains a clinical diagnosis that is supported by laboratory and/or radiologic studies. Timely diagnosis is critical; a delay in diagnosis and treatment may result in the conversion of a relatively straightforward case of non-perforated appendicitis into a complex case involving perforation. The importance of avoiding perforation is intuitive but nonetheless underscored by mortality statistics. The mortality rates associated with and without accompanying perforation are 5% and 0.6%, respectively.5
Essentially, all patients presenting with acute appendicitis will have a chief complaint of abdominal pain. Classically, patients will complain of vague periumbilical pain that localizes to the right lower quadrant as the disease progresses. The early discomfort carried by autonomic nerve fibers is poorly localized and crampy. It is not until the parietal peritoneum becomes irritated that somatic nerves become involved, producing well localized, sharp pain over the right lower quadrant. The pain typically increases over a 12- to 24-hour period and ultimately is the reason that patients seek medical attention. Pain lasting more than 36 hours is uncommon in non-perforated cases.
In addition to pain, patients will have various associated symptoms. Among them are nausea, vomiting, and anorexia. Of particular note is the observation that pain usually precedes all other symptoms. Much has been written concerning the sequence of symptoms in acute appendicitis. Classic surgical texts such as Cope's Early Diagnosis of the Acute Abdomen place significant emphasis on symptom sequence.17 As such, many surgeons doubt the diagnosis of acute appendicitis if symptoms such as nausea and vomiting precede the onset of pain. More than 90% of patients with appendicitis will have anorexia, and the diagnosis must be questioned in a truly hungry patient.6
The physical examination should begin with a review of the vital signs. An elevated temperature is quite common in acute appendicitis, but the absence of fever does not in any way rule out the disease. Twenty-five to fifty percent of patients with proven appendicitis have been found to have temperatures lower than 37.5°C.18 The remaining vital signs often are within the normal range in uncomplicated cases. In cases involving delayed diagnosis or perforation, significant abnormalities of the vital signs may be encountered. Tachycardia, hypotension, and tachypnea may be present to varying degrees and indicate severe, unchecked disease states.
A brief discussion of the term "peritonitis" is useful prior to introduction of specifics relating to the physical examination. Simply put, peritonitis is a term denoting inflammation of the peritoneum. It can occur in many abdominal conditions and is not specific for any particular disease process. Characteristics of peritonitis include extreme tenderness, rebound tenderness, jar tenderness, and guarding. Findings consistent with peritonitis may be seen locally or diffusely. For example, a patient with a perforated peptic ulcer with significant peritoneal soilage will have diffuse peritonitis, whereas a patient with uncomplicated appendicitis will have peritoneal irritation localized to the right lower quadrant.
Tenderness is self-explanatory. Rebound tenderness refers to a particular form of tenderness associated with peritoneal irritation. It is elicited by palpating deeply enough to depress the peritoneum. The pressure is applied with a constant intensity and then withdrawn quickly.19 If rebound tenderness is present, the patient will experience significant pain when the pressure is released due to the quick movement of the inflamed peritoneal lining. Jar tenderness simply refers to pain elicited when the patient is moved. To elicit the sign, an examiner may gently tap the heel of the patient or move the bed slightly. An astute clinician may obtain information on jar tenderness by asking questions such as "Do you feel better lying still or when moving about?" and "Does going over bumps in the car or on the stretcher cause worsening pain?" Guarding refers to a state of contraction of the abdominal wall musculature and comes in two varieties: voluntary and involuntary. Voluntary guarding occurs when a patient tenses the abdomen in anticipation of palpation by the examiner. Such voluntary guarding may be overcome with distraction. Involuntary guarding is associated with a more advanced disease state and cannot be overcome by distraction.19
Classically, the abdominal examination is described as being comprised of inspection, auscultation, percussion, and palpation. Simply observing the patient can be quite informative. Patients with appendicitis have peritoneal irritation. Because of this, they are reluctant to move about and usually lie quite still on the examination table or stretcher. In contrast, patients with colicky pain tend to writhe about in discomfort. Auscultation is not particularly useful as no finding is sensitive or specific enough to aid in accurate diagnosis.
Percussion and palpation should be thought of as one entity. Percussion is a good way to begin the palpation portion of the physical examination. It is a sensitive indicator of peritoneal irritation. Tenderness will be elicited over the precise location of the appendix. The exact location will vary, but a location approximately two-thirds of the distance from the umbilicus to the anterior superior iliac spine is a good generalization. This area is referred to by the eponym "McBurney's point." Palpation will produce similar results to percussion and should be performed last. It produces significantly more pain than the gentle percussion technique. Of particular note is the usual finding of pain localized to McBurney's point. Patients with appendicitis may present with diffuse or generalized peritonitis, but such a case implies severe, generalized peritoneal soilage as can occur with perforation. The vast majority of cases tend to present with relatively localized tenderness.
Several physical findings often are discussed in the setting of acute appendicitis and deserve mention. The oburator and psoas signs occur when an inflamed appendix lies in close apposition to these muscles. Both signs simply represent pain associated with passive stretch. The obturator sign is pain that occurs with internal rotation of the flexed right thigh, thus stretching the obturator muscle. The psoas sign is pain elicited with extension of the right hip, thus stretching the psoas muscle. By far the most useful of the commonly discussed signs is Rovsing's sign. It refers to pain in the right lower quadrant elicited by palpation in the left lower quadrant.
A pelvic examination should be performed on all women in whom the diagnosis of appendicitis is considered. The pelvic examination may suggest another potential etiology for the pain, such as pelvic inflammatory disease or ovarian cyst. The digital rectal examination (DRE) still is considered by some physicians to be part of the routine physical examination in patients presenting with acute abdominal pain. However, data suggest that the DRE need not be part of the routine physical examination in such patients. One prospective study of acute abdominal pain in adults found no cases in which the DRE altered management.20 Another study looking specifically at the value of the DRE in the setting of appendicitis found no benefit.21 Therefore, routine DRE in the setting of suspected acute appendicitis no longer is recommended.
By compiling and analyzing the data gleaned from multiple studies on acute abdominal pain (> 4000 patient encounters), a study attempted to identify those historical and physical examination findings most clearly associated with appendicitis.19 Three findings were noted to be the most useful: right lower quadrant pain, involuntary guarding, and migration of pain from the umbilical area to the right lower quadrant.19 The associated positive likelihood ratios with these signs were 8, 4, and 3.1, respectively. The study also identified findings with powerful negative likelihood ratios: absence of right lower quadrant pain and a history of similar pain previously. The negative likelihood ratios associated with these findings were 0.2 and 0.3, respectively.19
Diagnostic Studies
Appendicitis may be diagnosed in many cases without the aid of expensive diagnostic tests. However, the practice of modern medicine is becoming increasingly dependent on diagnostic tests, and essentially all patients suspected of having acute appendicitis will undergo laboratory and/or radiologic testing.
Laboratory Studies. The laboratory studies commonly obtained and recommended in the work-up of abdominal pain include a complete blood count, complete metabolic panel, amylase and/or lipase, and urinalysis. Of course, a urine beta-hCG should be obtained from all women of child-bearing age. Though not absolutely necessary in straightforward cases, surgical consultants usually will ask for most, if not all, of the above tests. Unfortunately, no laboratory test can rule in or rule out the diagnosis of acute appendicitis. This observation underscores the importance of clinical judgment.
Probably the most discussed laboratory study is the complete blood count, specifically the white blood cell (WBC) count. Numerous medical personnel, including some physicians, are under the false impression that appendicitis is exceedingly unlikely in the setting of a normal WBC count. Certainly, leukocytosis is supportive of the diagnosis. But a WBC count in the normal range in no way rules out the presence of appendicitis. Studies have shown that using leukocytosis alone to diagnose appendicitis results in poor sensitivity and specificity. In one series of nearly 500 patients with appendicitis, 37% had a WBC count less than 11,000.6,22 The overall sensitivity and specificity of leukocytosis for diagnosing appendicitis is estimated to be only 76% and 52%, respectively.23
Urinalysis results in the setting of acute appendicitis also warrant further comment. Presumably due to the appendix's proximity to the ureter, appendiceal inflammation may result in changes in the urine sediment. In a recent series, greater than 10 WBC/high power field and greater than 3 red blood cells/high power field were noted in 14% and 17% of cases of appendicitis, respectively.24 Thus, the urinalysis should be interpreted with caution.
Radiologic Studies. Plain Films. The physician has an ever increasing armamentarium of radiologic studies to order. The oldest of the modalities, the plain film, continues to be used in the evaluation of abdominal pain. Its greatest utility is in the assessment of pneumoperitoneum and obstructive processes. In general, it should not be ordered specifically for appendicitis because it lacks sufficient sensitivity and specificity to be useful. However, several plain film findings have been noted that are at least suggestive of appendicitis. These findings include right lower quadrant fecalith, scoliosis of the lumbar spine with the convexity away from the appendix, and obliteration of the right psoas shadow.25
Ultrasound. The use of ultrasound in the diagnosis of acute appendicitis has been a popular subject in the literature since the initial report of successful ultrasound visualization of the appendix in 1981.26 It can be performed rapidly at relatively low cost and lacks ionizing radiation. In addition, emergency physicians increasingly are performing ultrasound examinations at the bedside. Thus, ultrasound as a diagnostic modality has numerous desirable features.
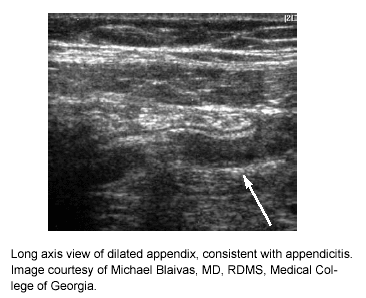
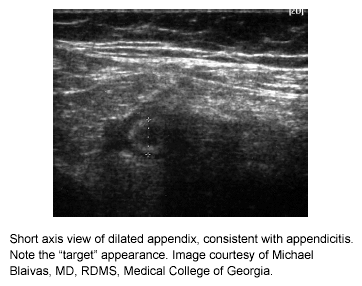
Certain characteristics have been noted that are suggestive of inflamed appendix as seen on ultrasound. These include noncompressibility, dilation, and a "target" appearance when viewed in transverse section.27 (See Figures 1, 2.) Occasionally, a fecalith may be seen. Reported sensitivity and specificity of the technique has ranged between 76-96% and 47-94%, respectively.6 The technique is highly operator- and equipment-dependent, so it is not surprising that there have been wide ranges of results published.
|
|
Additional factors that may decrease ultrasound's effectiveness as a diagnostic tool include large body habitus and the presence of significant bowel gas. Under such circumstances, merely finding the appendix can be challenging, and in many cases it cannot be located. Of note, a normal or noninflamed appendix is more difficult to identify than an enlarged, inflamed one. Reported success rates in finding a noninflamed appendix have ranged between 60-82%.6,28 Obviously, if the appendix cannot be located, appendicitis cannot be ruled out.
Undoubtedly, more studies on using ultrasound in the setting of acute right lower quadrant pain will be forthcoming. At present, ultrasound is a reasonable study to obtain, especially in certain patient groups such as pregnant women. However, it is critical to note that ultrasound's primary role is ruling in, not ruling out, the diagnosis. If clinical suspicion is high, a negative ultrasound should not dissuade the clinician from ordering additional, more definitive testing.
Computed Tomography. The widespread usage of computed tomography (CT) has revolutionized the management of many abdominal conditions. Appendicitis is no exception. At present, CT is considered the gold standard imaging study in the work-up of patients with suspected appendicitis, with reported diagnostic accuracy rates as high as 98%.6 Its use now is commonplace in the work-up of acute right lower quadrant pain.
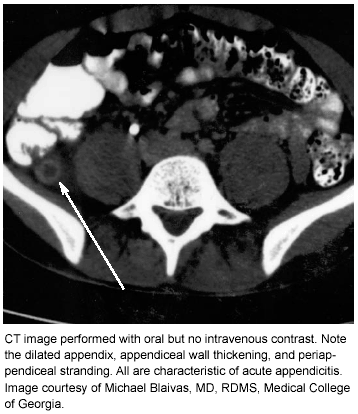
Numerous studies have assessed the sensitivity and specificity of CT in the setting of appendicitis. Reported sensitivity and specificity have ranged between 87-100% and 95-99%, respectively.6 Modern CT provides excellent anatomic detail, and several CT findings have been associated strongly with the presence of acute appendicitis. Among these are periappendiceal fat stranding, enlargement of the appendix (greater than 6 mm), appendiceal wall thickening, and appendiceal wall enhancement.29 (See Figure 3.)
| Figure 3. CT of Dilated Appendix |
|
Clearly, the use of CT has gained widespread acceptance in the diagnostic work-up of acute appendicitis. However, there is significant disagreement with regard to exactly which type of CT imaging to obtain. Specifically, the debate largely is centered around the use of contrast material.
CT may be performed without the use of either intravenous (IV) or oral contrast. Such is the case in the common usage of CT in the work-up of renal colic. There are some obvious advantages to the no-contrast approach. Oral contrast takes time to deliver, both to drink and to allow for adequate peristalsis to occur to get the contrast to the colon. Because the time to imaging is decreased when no contrast is used, the time to diagnosis may be decreased as well. Another problem with oral contrast is that many patients cannot tolerate it well secondary to nausea, vomiting, etc. IV contrast carries additional risks, primarily contrast-induced renal dysfunction and the possibility of an allergic reaction. In cases of underlying renal dysfunction, IV contrast should be avoided. Some studies have shown that unenhanced CT can be used to diagnose appendicitis with a high level of accuracy.6 However, the addition of oral and IV contrast does provide additional benefit and can improve the diagnostic accuracy of CT.30 The decision of whether to use contrast ultimately will depend on individual patient factors as well as the preferences of local radiology and surgical colleagues.
Despite its obvious attributes, CT does have some disadvantages. The technique continues to be quite expensive and delivers ionizing radiation. Additional problems have already been mentioned and include the potential for contrast allergy, contrast-induced nephropathy, and delayed time to diagnosis.
Impact of Modern Imaging on Negative Appendectomy Rate
A 2005 study published in the the surgical literature reviewed the records of a large health maintenance organization (150,000 patients) from 1980-1999 and found that 4058 patients underwent non-incidental appendectomy during that time frame.31 Neither CT nor ultrasound was used significantly in the study cohort prior to 1990, but the use of these modalities more than tripled during the 1990s. By 1999, 36% of patients undergoing appendectomy had preoperative testing. The overall negative appendectomy rate was noted to be 15%, and the authors found no significant change in this rate based on study year or era (pre- and post-1990).31
Other studies have assessed the impact of preoperative imaging on the negative appendectomy rate within certain patient populations. A study in the radiology literature published in 2002 found that the negative appendectomy rate was significantly lower in women who underwent a preoperative CT or ultrasound evaluation compared to those who did not (8% vs 28%).32 The use of preoperative imaging did not result in an alteration of the negative appendectomy rate in men.32
Role of Scoring Systems in Diagnosis
Numerous scoring systems have been developed over the years in an attempt to facilitate the diagnosis of acute appendicitis.33-36 The scoring systems consist of various combinations of history, signs and symptoms, and laboratory studies assessing the inflammatory response. Some have even incorporated radiologic studies such as ultrasound.37
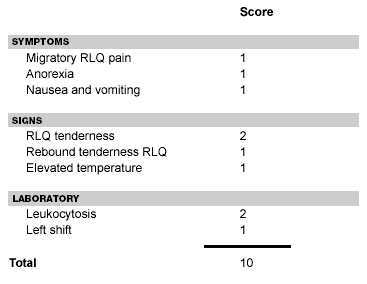
Probably the best known and most widely referenced scoring system was proposed by Alvarado in 1986.33 This particular system is referred to as the Alvarado score or MANTRELS, an acronym denoting the components of the scoring system. (See Table 1.) The scoring system consists of three symptoms, three signs, and two laboratory studies. The maximum score is 10, with increasing scores indicating a greater likelihood of appendicitis. Ideally, such a scoring system would facilitate the diagnosis of acute appendicitis and also decrease the negative appendectomy rate. Through a retrospective chart analysis of 305 patients with abdominal pain suggestive of acute appendicitis, Alvarado found the mean score for acute appendicitis and non-appendicitis to be 7.71 and 5.24, respectively.33 No specific cutoff was recommended in the Alvarado study. However, data suggested that using a value of 6 to either operate or observe a given patient would result in a potential missed appendicitis rate of 5.8% and a negative laparotomy rate of 8.7%.34
| Table 1. Alvarado Score (MANTRELS) |
|
Several studies have attempted to apply the Alvarado system in a prospective fashion. Using a cutoff score of 6, a study in 2000 found the sensitivity, specificity, positive predictive value, and negative predictive value to be 76%, 95%, 93%, and 84% respectively.38 These results along with a negative laparotomy rate of 24% were worse than the initial Alvarado study predicted. Another study assessed not only the Alvarado scoring system but also numerous other scoring systems as well. This study found results to be uniformly worse than those previously reported, with missed appendicitis rates as high as 35%.39
The data at present suggest that scoring systems may have some potential value. However, no scoring system can be relied upon solely to ensure accurate diagnosis in all cases. No scoring system available at present can replace the clinical judgment of an astute physician utilizing historical features, the physical examination, and laboratory/radiologic studies when appropriate.
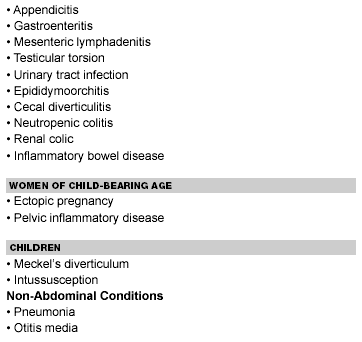
| Table 2. Acute Abdominal Pain Differential Diagnosis |
|
Differential Diagnosis
Appendicitis is the most common acute surgical emergency in the United States. As such, it must be in the differential diagnosis of any patient presenting with acute abdominal pain. Though sometimes straightforward, the diagnosis of appendicitis can present many challenges, and the differential diagnosis for acute right lower quadrant pain is extensive.
Perhaps the most challenging patient population from a diagnostic standpoint is women of child-bearing age. The highest percentage of misdiagnosis occurs in this population in large part because numerous obstetric and gynecological processes can be mistaken for acute appendicitis.6 The most dangerous and potentially life-threatening of these is ectopic pregnancy. The importance of obtaining a urine beta-hCG in all women of child-bearing age cannot be overemphasized. Though a pregnant patient certainly may have acute appendicitis, a positive urine pregnancy test should alert the clinician to the possibility of an ectopic pregnancy. Vaginal bleeding often is present in the setting of an ectopic pregnancy, but its absence does not rule out the condition. A ruptured ectopic pregnancy can present solely with acute lower abdominal pain. Thus, a positive urine pregnancy test should prompt the clinician to pursue the possibility of ectopic pregnancy further with diagnostic testing such as ultrasound.
Pelvic inflammatory disease (PID) is another common condition that may present diagnostic difficulty. Certain characteristics should point to PID, including purulent vaginal discharge, cervical motion tenderness, and adnexal tenderness. The adnexal tenderness usually is bilateral. None of these findings would be found without doing a pelvic exam. Thus, the pelvic exam in women of child-bearing age is critically important. Other gynecological conditions included in the differential of right lower quadrant pain are mittelschmerz, ovarian cysts, endometriosis, and ovarian torsion.6
Certain conditions in the pediatric population can be confused with appendicitis. Meckel's diverticulum is a true diverticulum that occurs 2 feet proximal to the ileocecal valve. It can become acutely inflamed in a condition referred to as Meckel's diverticulitis. Because of its usual location in the right lower quadrant, the process easily can be mistaken for acute appendicitis. CT and potentially the use of a Meckel's scan, a nuclear medicine study, may be beneficial in difficult cases. Intussusception also may present with right lower quadrant pain. Classically, the pain is episodic in nature, resulting in bouts of crying associated with drawing the legs up toward the abdomen. Heme positive or frankly bloody "currant jelly" stool and a palpable right lower quadrant mass occasionally may be noted. Especially in the pediatric age group, non-abdominal conditions such as pneumonia and otitis media can cause pain that is referred to the abdomen and must not be overlooked.6
Gastroenteritis is a very common cause of abdominal discomfort in all age groups. Such patients typically will have nausea, vomiting, diarrhea, and fever to varying degrees. The abdominal pain usually is relatively diffuse and certainly not localized to the right lower quadrant. Patients with appendicitis tend to have the onset of pain prior to other nonspecific gastrointestinal symptoms. Also, diarrhea is not a common accompanying feature of appendicitis but is a common symptom in the setting of gastroenteritis.
Mesenteric lymphadenitis can be confused with acute appendicitis. It is thought to be caused by an antecedent viral infection and results in lymph node enlargement within the mesentery. Despite the diagnostic confusion it sometimes presents, mesenteric lymphadenitis is non-surgical in nature and requires no specific therapy.
A myriad of other conditions may cause acute right lower quadrant pain. Included among these are testicular torsion, urinary tract infection, epididymoorchitis, cecal diverticulitis, neutropenic colitis, renal colic, and inflammatory bowel disease. The clinician must remain cognizant of other disease processes that may mimic appendicitis given the extensive differential.
Management
Patients with suspected acute appendicitis should have intravenous access obtained, appropriate laboratory studies sent, and intravenous hydration initiated. NPO status should be maintained. Patients need not be placed on a monitor unless they appear systemically ill or have significant underlying medical co-morbidities.
Appropriate analgesia should not be withheld from patients with acute abdominal pain. Despite popular belief to the contrary, judicious use of analgesics in the setting of abdominal pain does not result in significant alteration of physical examination findings. A recent study comparing morphine to placebo in adult patients with suspected appendicitis found no significant change in physical examination findings following morphine administration. Of note, significant pain relief was obtained in those patients receiving morphine.40 A recent pediatric study comparing the use of morphine to placebo in children with acute abdominal pain found a similar benefit. Specifically, the study showed that children receiving morphine had a reduction in pain, and the administration of morphine did not impede the diagnosis of acute appendicitis.41 Of note is the growing consensus among medical and surgical practitioners about the use of analgesics in the setting of acute abdominal pain. The referenced articles above are from non-surgical literature, but recent articles in the surgical literature also support the judicious use of analgesics in the setting of suspected appendicitis. A retrospective analysis published in the surgical literature in 2004 found that there was no difference in hospital stay, time to operating room, complication rate, negative appendectomy rate, or perforation rate in patients receiving analgesics prior to surgical evaluation.42
Antibiotics have been shown to decrease complications related to appendicitis. Specifically, rates of postoperative wound infections and intra-abdominal abscess are reduced by appropriate antibiotic usage.6,43 For maximum effectiveness, the antibiotics should be given preoperatively and should be broad spectrum, providing both aerobic and anaerobic coverage. An appropriate regimen would be cefoxitin or cefotetan. In patients with significant allergic reactions to beta-lactams, a combination of ciprofloxacin and metronidazole would be appropriate. Antibiotic administration usually is withheld until the diagnosis of appendicitis is confirmed or until a surgical colleague has made a decision to take the patient to the operating room. Surgeons will have differing opinions with regard to antibiotic specifics, and discussing antibiotic choice and timing is reasonable prior to administration.
Definitive treatment for appendicitis is surgical. As such, all patients with appendicitis require general surgical consultation. Historically, appendectomy has been performed as an open procedure via a right lower quadrant incision. Laparoscopic techniques now are widespread in general surgery, and laparoscopic appendectomy is gaining in popularity. Laparoscopic appendectomy more than doubled during the last several years and made up 43% of cases in 2003.44 Controversy still exists with regard to which technique is superior. Laparoscopic utilization will vary depending on individual surgeon preference and case-specific factors.
There is no clear consensus with regard to the timing of surgical consultation for patients with suspected acute appendicitis. It is certainly reasonable to consult a general surgeon based on the clinical picture alone, i.e., without confirmatory radiologic or supportive laboratory studies. Such early consultation could result in earlier definitive therapy and, in doing so, reduce complications such as rupture. A recent retrospective study confirmed that there is a direct relationship between time from symptom onset and rupture risk. Specifically, the study found that rupture risk was less than or equal to 2% if the symptoms had been present less that 36 hours. For each 12-hour period after 36 hours, the rupture risk increased by an additional 5%.45 Despite the evidence showing the importance of expeditious treatment, it is increasingly apparent that many surgeons simply will not operate in the absence of a confirmatory radiologic study such as CT. Obviously, situations will differ based on individual patient characteristics and individual surgeon practice patterns. For example, a teenage male with a classic history and physical examination is more likely to be taken to the operating room without a confirmatory study than is a woman of child-bearing age. A reasonable approach is to obtain early surgical consultation in what appear to be straightforward cases and to delay surgical consultation until a definitive radiologic study is performed in other more equivocal cases.
Options in Unclear Cases
Despite one's best efforts, there undoubtedly will be cases in which the diagnosis is unclear. Such is the nature of abdominal pain. The patients who fall into this category will be those with atypical histories and physical examinations. The most straightforward cases will be those that clearly do not have appendicitis and those that clearly are high risk. The patients who clearly do not have a surgical process may be discharged with a recommendation to seek further evaluation should the condition worsen. Such instructions should be articulated clearly in the discharge paperwork. Patients who are deemed to be high probability for appendicitis by history, physical examination, etc., will have either surgical consultation or a more definitive diagnostic study such as CT. Thus, it is the patients in the middle who will have the most difficult dispositions. In patients in whom the diagnosis of appendicitis is possible but not convincing enough to warrant surgical consultation or further radiologic testing, two basic options are available: an observation unit stay or a scheduled return visit for repeat evaluation.
Observation units are becoming more commonplace in emergency medicine. Such units represent a convenient location in which to monitor patients exhibiting questionable admission criteria. A retrospective study performed in 2002 assessing trends in emergency department observation unit usage showed that abdominal pain was the second most common reason for admission to emergency department observation units behind chest pain.46 Patients may have serial physical examinations and repeat laboratory studies while in the observation unit. Equivocal cases should become clearer over time through careful repeat evaluation and the selective use of further laboratory and/or radiologic studies as warranted by the patient's clinical course. Alternatively, low-risk patients with equivocal presentations may be discharged home and scheduled for a repeat emergency department evaluation in 24 hours. Of course, such patients should have explicit instructions to return prior to the time of the scheduled re-evaluation if the condition worsens.
Medicolegal Considerations
Abdominal pain, and appendicitis in particular, must be included in any discussion of malpractice as it applies to emergency medicine. It is rightfully included among other high-risk diagnostic categories such as chest pain, stroke, and traumatic injuries. Studies involving both adult and pediatric populations have found that appendicitis is one of the most common diagnoses resulting in litigation against emergency physicians.47,48
A retrospective review of appendicitis-related malpractice claims attempted to identify common features in such cases.49 The results were not surprising. Patients with missed appendicitis appeared less acutely ill and had atypical pain (not localized to the right lower quadrant) at the time of evaluation. The most common incorrect diagnosis given to patients ultimately found to have acute appendicitis was gastroenteritis.49 Of note, many patients with poor outcomes were not given appropriate discharge or follow-up instructions. This observation underscores the importance of documentation.
Conclusion
Despite the advances of modern medicine, the diagnosis of acute appendicitis continues to be a challenge for physicians. It is the most common acute surgical emergency in the United States and causes significant morbidity and occasionally mortality. Physicians charged with the responsibility of evaluating acute abdominal pain must keep it in the differential diagnosis of all such patients. To be most effective, physicians must have command of the classic history and physical examination findings, recognize atypical presentations, and be cognizant of the limitations and advantages afforded by the vast array of available diagnostic tests.
References
1. McMurrich JP. Leonardo DaVinci the Anatomist. Baltimore: Williams and Wilkins; 1930.
2. Major RH. Classic Descriptions of Disease. Third Edition. Springfield, IL: Charles C. Thomas; 1945.
3. Fitz RH. Perforating inflammation of the vermiform appendix: With special reference to its early diagnosis and treatment. Am J Med Sci 1886;92: 321-346.
4. Brooks SM. McBurney's Point: The Story of Appendicitis. New York: AS Barnes and Company; 1969.
5. Fischer AC. Acute appendicitis. In: Cameron JL. Current Surgical Therapy, 7th ed. St. Louis: Mosby; 2001: 267-272.
6. Prystowsky JB, Pugh CM, et al. Appendicitis. Curr Probl Surg 2005;42:694-742.
7. Walker AR, Segal I. Appendicitis: An African perspective. J R Soc Med 1995;88:616-619.
8. Naaeder SB, Archampong EQ. Acute appendicitis and dietary fiber intake. West Afr J Med 1998;17:264-267.
9. Matthews JB, Hodin RA. Acute abdomen and appendix. In: Greenfield LJ, Mulholland MW, Lillemoe KD, et al, eds. Surgery: Scientific Principles and Practice, 3rd ed. Philadelphia: Lippincott Williams and Wilkins; 2001:1224-1236.
10. Wakely CP. The position of the vermiform appendix as ascertained by an analysis of 10,000 cases. J Anat 1933;67:277-283.
11. Poole GV. Anatomic basis for delayed diagnosis of appendicitis. South Med J 1990;83:771-773.
12. Wangensteen OH, Dennis C. Experimental proof of the obstructive origin of appendicitis in man. Ann Surg 1939;110:629-647.
13. Bennion RS, Wilson SE, Serota AI, et al. The role of gastrointestinal microflora in the pathogenesis of complications of mesenteric ischemia. Rev Infect Dis 1984;6:132-138.
14. Bennion RS, Thompson JE, Baron EJ, et al. Gangrenous and perforated appendicitis with peritonitis: Treatment and bacteriology. Clin Ther 1990; 12 Supplement C:31-44.
15. Altemeier WA. The bacterial flora of acute perforated appendicitis with peritonitis. A bacteriological study based upon 100 cases. Ann Surg 1938;107:517-528.
16. Lewis FR, Holcroft JW, Boey J, et al. Appendicitis: A critical review of diagnosis and treatment in 1,000 cases. Arch Surg 1975;110:677-684.
17. Silen W. Cope's Early Diagnosis of the Acute Abdomen, 16th ed. New York: Oxford University Press; 1983.
18. Lewis FR, Holcroft JW, Boey J, et al. Appendicitis: A critical review of diagnosis and treatment in 1,000 cases. Arch Surg 1975;110:677-684.
19. Wagner JM, McKinney P, Carpenter JL. Does this patient have appendicitis? JAMA 1996;276:1589-1594.
20. Manimaran N, Galland RB. Significance of routine digital rectal examination in adults presenting with abdominal pain. Ann R Coll Surg Engl 2004;86:292-295.
21. Kremer K, Kraemer M, Fuchs KH, et al. [The diagnostic value of rectal examination of patients with acute appendicitis.] Langenbecks Arch Chir Suppl Kongressbd 1998;115:1120-1122.
22. Pieper R, Kager L, Nasman P. Acute appendicitis: A clinical study of 1018 cases of emergency appendectomy. Acta Chir Scand 1982;48:51-62.
23. Cardall T, Glasser J, Guss DA. Clinical value of the total white blood cell count and temperature in the evaluation of patients with suspected appendicitis. Acad Emerg Med 2004;11:1021-1027.
24. Tundidor Bermudez AM, Amado Dieguez JA, Montes de Ocal Mastrapa JL. [Urologic manifestations of acute appendicitis.] Arch Esp Urol 2005;58:207-212.
25. Graffeo CS, Counselman FL. Appendicitis. Emerg Med Clin North Am 1996;14:653-671.
26. Deutsch A, Leopold GR. Ultrasonic demonstration of the inflamed appendix: Case report. Radiology 1981;140:163-164.
27. Adams DH, Fine C, et al. High resolution real time ultrasonography. A new tool in the diagnosis of acute appendicitis. Am J Surgery 1988;155:93-97.
28. Rettenbacher T, Hollerweger A, Macheiner P, et al. [Ultrasonography of the normal vermiform appendix.] Ultraschall Med 1997;18:139-142.
29. Choi D, Park H, Lee YR, et al. The most useful findings for diagnosing acute appendicitis on contrast-enhanced helical CT. Acta Radiol 2003;44:574-582.
30. Jacobs JE, Birnbaum BA, Macari M, et al. Acute appendicitis: Comparison of helical CT diagnosis focused technique with oral contrast material versus nonfocused technique with oral and intravenous contrast material. Radiology 2001;220:683-690.
31. Flum DR, McClure TD, Morris A, et al. Misdiagnosis of appendicitis and the use of diagnostic imaging. J Am Coll Surg 2005;201:933-939.
32. Bendeck SE, Nino-Murcia M, Berry GJ, et al. Imaging for suspected appendicitis: Negative appendectomy and perforation rates. Radiology 2002;225:131-136.
33. Alvarado A. A practical score for the early diagnosis of acute appendicitis. Ann Emerg Med 1986;15:557-564.
34. Arnbjornsson E. Scoring system for computer-aided diagnosis of acute appendicitis. Ann Chir Gynaecol 1985;74:159-166.
35. Christian F, Christain GP. A simple scoring system to reduce the negative appendectomy rate. Ann R Coll Surg Engl 1992;74:281-285.
36. Eskelinen M, Ikonen J, Lipponen P. A computer-based diagnostic score to aid in diagnosis of acute appendicitis: A prospective study of 1333 patients with acute abdominal pain. Theor Surg 1992;7:86-90.
37. Tzanakis NE, Efstathious P, Danulidis K, et al. A new approach to accurate diagnosis of acute appendicitis. World J Surg 2005;29:1151-1156.
38. Saidi RF, Ghasemi M. Role of Alvarado score in diagnosis and treatment of suspected acute appendicitis. Am J of Emerg Med 2000;18:230-231.
39. Ohmann C, Yang Q, Franke C. Diagnostic scores for acute appendicitis. Abdominal Pain Study Group. Eur J Surg 1995;161:273-281.
40. Wolfe JM, Smithline HA, Phipen S, et al. Does morphine change the physical examination in patients with acute appendicitis? Am J Emerg Med 2004;22:280-285.
41. Green R, Bulloch B, Kabani A, et al. Early analgesia for children with acute abdominal pain. Pediatrics 2005;116:978-983.
42. Aydelotte JD, Collen JF, Martin RR. Analgesic administration prior to surgical evaluation for acute appendicitis. Curr Surg 2004;61:373-375.
43. Andersen BR, Kallehave FL, Andersen HK. Antibiotics versus placebo for prevention of postoperative infection after appendectomy. Cochrane Database Syst Rev 2004;4: 1-64.
44. Nguyen NT, Zainabadi K, Mavandadi S, et al. Trends in utilization and outcomes of laparoscopic versus open appendectomy. Am J Surg 2004;188:813-820.
45. Bickell NA, Aufses AH Jr, Rojas M, et al. How time affects the risk of rupture in appendicitis. J Am Coll Surg 2006;202:401-406.
46. Hostetler B, Leikin JB, Timmons JA, et al. Patterns of use of an emergency department-based observation unit. Am J Ther 2002;9:499-502.
47. Karcz A, Korn R, Burke MC, et al. Malpractice claims against emergency physicians in Massachusetts: 1975-1993. Am J Emerg Med 1996;14:341-345.
48. Selbst SM, Friedman MJ, Singh SB. Epidemiology and etiology of malpractice lawsuits involving children in US emergency departments and urgent care centers. Pediatr Emerg Care 2005;21:165-169.
49. Rusnak RA, Borer JM, Fastow JS. Misdiagnosis of acute appendicitis: Common features discovered in cases after litigation. Am J Emerg Med 1994;12:397-402.
... acute appendicitis is a common disorder that continues to remain a diagnostic challenge despite clinical study during the past century and imaging advances in the past decade.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.