Surviving Trauma: Identifying and Managing Post-Traumatic Stress Disorder
Surviving Trauma: Identifying and Managing Post-Traumatic Stress Disorder
Authors: Randy A. Sansone, MD, Professor, Department of Psychiatry and Internal Medicine, Wright State University School of Medicine, Dayton, OH; Director of Psychiatry Education, Kettering Medical Center, Kettering, OH; and Lori A. Sansone, MD, Family Medicine Physician, Wright-Patterson Air Force Base, Dayton, OH.
Peer Reviewer: Ashley B. Benjamin, MD, MA, Staff Psychiatrist, Ambulatory Mental Health Clinic, Oklahoma City VAMC, Assistant Clinical Professor, Department of Psychiatry and Behavioral Sciences, Oklahoma University Health Sciences Center, Oklahoma City, OK.
Post-traumatic stress disorder (PTSD) is a complex psychobiological syndrome that evolves in vulnerable individuals as a direct consequence of exposure to trauma. While different types of trauma such as natural disasters or rape may precipitate the disorder, the sequelae of symptoms are consistent among victims. After exposure, a cascade of neurohormonal and biological changes develops and appears to perpetuate the symptoms that represent PTSD. Victims initially tend to present to primary care clinicians—oftentimes with diffuse somatic complaints with no mention of prior trauma. Treatment tends to be multimodal and includes both psychotherapy and pharmacotherapy.
(Note: The views expressed in this article are those of the authors and do not reflect the official policy or position of the United States Air Force, Department of Defense, or United States government.)
The Editor
Historical Terminology
PTSD has masqueraded under different names during different eras. For example, following the Civil War in the United States, PTSD was labeled "cardiorespiratory syndrome"1 as well as "nostalgia."2 After World War I, victims were described as having "shell shock."2 Following World War II, victims of the disorder were diagnosed with "combat neurosis,"1 "combat fatigue," or "combat exhaustion."2 It wasn't until the advent of the third edition of the Diagnostic and Statistical Manual of Mental Disorders3 in 1980 that PTSD attained its current official nomenclature, as well as explicit diagnostic criteria.
The Diagnosis of PTSD
In the Diagnostic and Statistical Manual of Mental Disorders, 4th edition (DSM-IV),4 PTSD is classified under the anxiety disorders. The diagnosis of PTSD4 is contingent upon: 1) exposure to a significantly traumatic event such as being the victim of a crime, severe automobile or other accident, or natural disaster, or experiencing war; 2) the development of an intense fear response in the aftermath of the exposure; 3) a symptom duration of at least 4 weeks (for symptom durations less than 4 weeks, the diagnosis is acute stress disorder, and adjunctive symptoms may include a host of acute dissociative features such as detachment, being in a daze, derealization, depersonalization, and dissociative amnesia); and 4) residual functional impairment (e.g., social or occupational dysfunction). The specific symptoms themselves may be organized around the acronym RAH: reexperiencing, avoidance, and hyperarousal.
Reexperiencing. Reexperiencing is the psychological re-exposure of the victim to the traumatic event or some aspect of it. Reexposure may occur through intrusive and/or recurrent thoughts, images, or perceptions about the traumatic event; dreams or nightmares; a sense of reliving of the event; or bonafide flashback experiences (i.e., reexperiencing through images, smells, sounds, and/or feelings of some aspect of a past experience, which appears to be recurring). Reexperiencing oftentimes is accompanied by intense psychological distress or physiological reactivity, which also may occur when patients encounter psychological or environmental cues that trigger recollections of the trauma. Only one type of reexperiencing symptom in this category is required for diagnosis.
Avoidance. Avoidance refers to the physical and/or psychological evasion of any stimuli that the victim associates with the trauma. For example, victims may make active and fervent efforts to avoid any thoughts, feelings, or dialogue associated with the trauma. People affected by PTSD may avoid activities, places, or people that stimulate recollections of the trauma. On occasion, some exposed individuals may be unable to recall a particular yet important aspect of the trauma. In terms of overall demeanor, people with PTSD may experience a diminished interest in usual activities, social detachment with others, a restricted emotional range or affect, and the sense of a foreshortened future (i.e., no sense of a future career or marriage). Three avoidance symptoms in this category are required for diagnosis.
Hyperarousal. The final diagnostic feature of PTSD is increased arousal, which may manifest as difficulty with sleep, irritability or outbursts, concentration difficulties, hypervigilance or environmental scanning, and/or an exaggerated startle response. Two symptoms in this category are required for diagnosis.
Diagnostic Stability. In support of the RAH criteria described in DSM-IV,4 investigators5 recently examined the symptom structure of PTSD in a nationally representative sample and found empirical support for each. Interestingly, however, a principal-components analysis yielded a four-factor solution consisting of dysphoria, cued reexperiencing and avoidance, uncued reexperiencing and hyperarousal, and trauma-related rumination. These empirical findings suggest that the preceding symptoms also may be highly relevant to the diagnosis of PTSD.
Diagnostic Perspective. In summary, the diagnosis of PTSD is grounded on three fundamental criteria that can be organized around the acronym RAH (i.e., reexperiencing, avoidance, and hyperarousal). On a conceptual level, one way to view these three core symptoms is to envision them as potentially protective of the individual. Imagine that you burn your hand on the stove. In the aftermath, the development of RAH symptoms readily could be seen as adaptive. Reexperiencing continually reminds you that a specific danger truly exists in the environment. Avoidance enables you to maintain a safe distance between yourself and the feared stimulus, which in this case is the stove. Finally, hyperarousal enables you to maintain an ongoing scanning process for any stoves in the immediate environment.
Diagnostic Qualifiers. In the DSM-IV,4 PTSD is sub-classified according to the duration of symptoms. Acute PTSD is defined as the presence of symptoms for fewer than three months; chronic PTSD is defined as the presence of symptoms for more than three months. Interestingly, some patients may not experience any PTSD symptoms until many months after the trauma. When symptoms emerge six months or more after an initial traumatic exposure, the qualifying descriptor is delayed-onset PTSD.
Challenges to Diagnosis. While the preceding criteria appear fairly unambiguous, PTSD can be somewhat difficult to diagnose, particularly in primary care settings. First, in contrast to mental health professionals, primary care physicians are much more likely to see victims in the immediate aftermath of trauma and may misdiagnose them with PTSD. Recall that during the first four weeks of symptoms, the appropriate diagnosis is acute stress disorder, rather than PTSD. Not surprisingly, however, acute stress disorder appears to be a reasonably good predictor for the subsequent development of PTSD, both in short-term6 and long-term7 follow-up studies.
Second, some victims may be too embarrassed to acknowledge candidly what happened to them (e.g., a male rape victim). Such disclosure may depend on a number of factors, including the patient's relationship with the primary care clinician, the sexes of the patient and the primary care clinician, the nature of the insult, and the availability of family support.
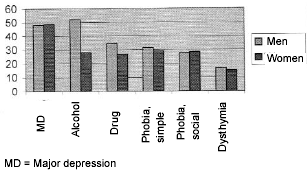
Third, victims initially may present with comorbid psychiatric difficulties, making the diagnosis of PTSD more difficult. Data indicate that PTSD has a relatively high level of comorbidity with other psychiatric disorders, particularly mood and various types of anxiety disorders.8 (See Figure 1.) In turn, patients may focus on these symptom constellations rather than on their trauma experience. While the rates of most types of psychiatric comorbidity are comparable between the sexes, note in Figure 1 that men are far more likely than women to have associated alcohol and drug problems.
| Figure 1. Psychiatric Comorbidity in Post-Traumatic Stress Disorder, by Gender8 |
|
|
Finally, victims may present with somatic concerns, which may distract the primary care clinician from exploring the possibility of PTSD. Somatic issues typically relate to the physical consequences of PTSD or a comorbid mood or anxiety disorder (e.g., insomnia, muscle tension/aches, weight change, non-specific gastrointestinal symptoms/discomfort). Indeed, empirical studies support these impressions and indicate that in PTSD patients, there are a higher frequency and greater intensity of somatic symptoms,9 a greater utilization of medical services,10,11 and greater healthcare costs.12 Some findings indicate that the presence of somatic complaints in PTSD patients are mediated by depression,13 but these conclusions are inconsistent.14
Assessment Measures
While a variety of PTSD assessments are available to the clinician, the Primary Care PTSD Screen15 is an attractive measure for use in primary care settings. This measure is a self-report design, and is brief, easily scored, validated for use in primary care settings, and in the public domain. The Primary Care PTSD Screen is shown in Table 1. Using this measure, research indicates that the endorsement of three or more items is highly suggestive of the diagnosis of PTSD.
| Table 1. Primary Care PTSD Screen* |
|
|
Epidemiology
Epidemiology traditionally refers to specific population characteristics or reliable contributory factors that are associated with a disease state. This approach to the characterization of the epidemiology in PTSD is not as feasible because of potentially diverse sources of trauma as well as the various populations that may be affected. For example, while a natural disaster indiscriminately affects both young and old, males and females, and individuals of all socioeconomic classes, the experience of rape is far more likely to be associated with young women. However, some epidemiological characteristics have been identified.
Demographic Profile. According to the National Comorbidity Survey Replication study,16 the lifetime prevalence of PTSD in the community is around 7%. (The initial National Comorbidity Survey17 in 1995 found a lifetime prevalence rate of 8%.) In examining the data according to age brackets, the highest frequency of PTSD is in the 45-59 year-old age group, while the lowest frequency is in the group older than age 60. However, this age distribution subsequently may be affected by world events, particularly with younger veterans returning from battle theaters in the Middle East. According to both community surveys, PTSD affects women twice as often as men. Not surprisingly, the symptoms of PTSD are consistent across cultures, indicating that the disorder is not culture-bound.18
Antecedent Risk Factors. There are a number of factors that appear to heighten the probability of PTSD development in exposed individuals. These are shown in Table 2.19 Overall, note that proximity and degree of exposure are extremely important factors as well prior trauma exposure and pre-existing psychopathology.
| Table 2. Factors that Increase the Likelihood of Developing Post-Traumatic Stress Disorder Following Traumatic Exposure19 |
|
|
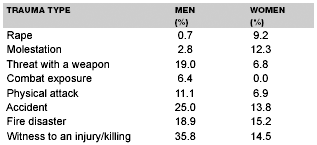
Trauma Exposure by Gender. According to the findings by Kessler and colleagues,8 men and women are prone to experience different types of trauma exposure. Not surprisingly, women are more likely to be victims of rape, whereas men are more likely to be threatened with a weapon or to witness a killing. These differences in trauma exposure are shown in Table 3.
| Table 3. The Lifetime Prevalance of Trauma Exposure in Adulthood, by Gender8 |
|
|
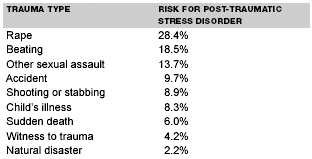
These differences in exposure may partially account for the higher prevalence rate of PTSD among women compared with men. Specifically, some empirical data suggest that both malignant intent and body violation of the victim heighten the risk of the development of PTSD. For example, in a study of soldiers exposed to the same combat conditions, Koren and colleagues20 found that those with physical injuries were significantly more likely to suffer from PTSD compared to those without such injuries. In a study comparing victims of terrorist attacks vs. motor vehicle accidents, Shalev and Freedman21 found a significantly higher rate of PTSD among the former. Extrapolating these data, victims of rape would seem to be at a very high risk for developing PTSD symptoms because of the malignant intent of the perpetrator as well as the violation of the body. Interestingly, these impressions are supported by data that illustrate the risk for developing PTSD as a function of trauma type.8 (See Table 4.) Note that the highest likelihood of PTSD is associated with rape, beating, and other types of sexual assault, whereas the lowest likelihood is associated with exposure to a natural disaster.
| Table 4. The Risk of Developing Post-Traumatic Stress Disorder by Trauma Type8 |
|
|
Overview of the Physiological Effects of Trauma
Trauma exposure appears to precipitate a cascade of physiological changes in the human body. While these are too numerous to review thoroughly here, several are fundamental to the basic understanding of the psychological symptoms as well as the secondary medical morbidity associated with PTSD. Perhaps the best way to conceptualize these neurohormonal and catecholamine changes is to relate them to the fight/flight response. These changes are compatible with the clinical observation of a hyper-activated state and may develop fairly quickly following trauma exposure.
The Hypothalamic-Pituitary-Adrenal (HPA) Axis. Among PTSD victims, the HPA axis undergoes activation with an expected increase in corticotropin-releasing factor.22 However, rather than the expected elevation in cortisol levels at the end of this cascade, levels are depressed, which is a uniquely distinguishing feature of PTSD.22 Newport and Nemeroff theorize that this paradoxical response of cortisol may be the consequence of exaggerated HPA negative feedback.22 These low cortisol levels may persist for decades after trauma exposure.23
The resulting low cortisol levels seen in PTSD victims may partially explain impairments in immunity,24 which have been confirmed by Japanese studies. In these studies, subjects with PTSD had significantly lower natural killer cell activity, lymphocyte counts, and interferon and interleukin levels.25 These findings may contribute to the observed higher levels of medical morbidity in PTSD victims.
The Hypothalamic-Pituitary-Thyroid (HPT) Axis. In addition to the activation of the HPA axis, the HPT axis also undergoes activation. Levels of T3, free T3, and T4 may be elevated, and T3 elevations tend to be disproportionately higher than T4 elevations.22 These findings may contribute to the hyperaroused state observed in individuals with PTSD.
Sympathetic Nervous System/Norepinephrine. An episodic increase in sympathetic tone in those with PTSD has been observed and appears to be secondary to periodic elevations in norepinephrine (NE). These increases may manifest clinically as tachycardia, hypertension, diaphoresis, and dizzinessagain, physiological evidence of hyperarousal. While baseline NE is within the normal range, elevations tend to occur with either physical exercise or exposure to trauma-associated stimuli.22
From a morbidity perspective, NE hyperactivity may influence lipoprotein metabolism, resulting in elevations of cholesterol, triglycerides, and low-density lipoproteins.22 This cascade may be a second contributory factor to the higher levels of medical disorders observed among PTSD patients, which is described further in the outcome section.
Hippocampus. As a possible consequence of low cortisol levels, glucocorticoid receptors appear to become exquisitely sensitive in PTSD. The hippocampus, which is associated with memory formation, is rich in these types of receptors. Paradoxically, while overall cortisol levels are low, this heightened receptor-site sensitivity may result in an overall neurotoxic effect on the hippocampus.26 In the aftermath of excessive stimulation and neurotoxicity, the hippocampus may degenerate, resulting in shrinkage or smaller volumes, which have been confirmed in PTSD patients.26-28 This, in turn, may lead to memory difficultiesspecifically, impairment in short-term verbal memory.
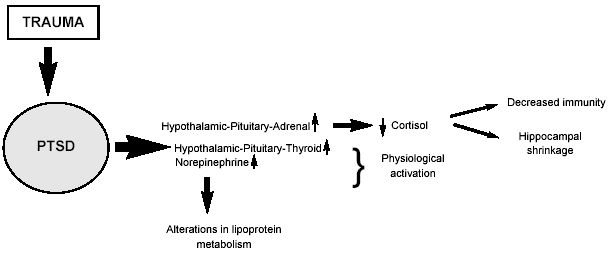
A summary of the various relationships between and effects of HPA and HPT activation, increases in NE, and hippocampal changes is shown in Figure 2. Note that the overall effect of these biological cascades is: 1) physiological hyperactivation and 2) an increased risk of medical morbidity, which is likely to occur through both impaired immunity and alterations in lipoprotein metabolism.
| Figure 2. Summary of the Major Physiological Changes in Post-Traumatic Stress Disorder (PTSD) |
|
|
Treatment of PTSD
The treatment of PTSD in the primary care setting is centered around education, supportive counseling, medication prescription and, when necessary, referral to a mental health professional. However, this section begins by briefly reviewing the various types of psychotherapy utilized for the treatment of this disorder in mental health settings.
Psychotherapy Treatment. Cognitive-Behavioral Therapy (CBT) is the most commonly discussed PTSD psychotherapy treatment in the literature. CBT, a relatively short-term intervention, focuses on the elicitation of negative or fear-provoking thoughts, the restructuring of these cognitions to promote better functioning (i.e., cognitive restructuring), and exposure therapy. Most treatments also include relaxation or anxiety-management techniques. Exposure therapy typically is undertaken in one of two ways: 1) imagined exposure, in which the patient recalls or envisions the trauma, or 2) in vivo exposure, in which the patient is directly exposed to the traumatic stimuli. In some treatments, patients are exposed to artificial stimuli that mimic the actual trauma (e.g., videos of combat scenes).
Another psychotherapy treatment for PTSD is Eye Movement Desensitization and Reprocessing (EMDR). In this approach, the patient imagines the trauma, and then is directed by the therapist to undertake a series of repetitive eye movements with the directive to "blank out." Then, the therapist assists the patient in developing an alternative, positive mental image. Other proposed psychotherapy treatments for PTSD include psychodynamic psychotherapy,29 interpersonal therapy,30 and Dialectical Behavior Therapy.31
Given the varied menu of psychotherapies, one might wonder about the relative efficacy of each. In comparing CBT and EMDR, outcomes are fairly comparable.32,33 So, at present, no specific psychotherapy treatment for PTSD overshadows the other treatments, and most result in symptom improvement.
While not a specific psychotherapy treatment for PTSD, debriefing is an acute intervention strategy that has been used to prevent symptom development. Debriefing consists of dialoguing one's personal experience of a given trauma, usually with other similarly exposed individuals, typically in a group setting. It is a controversial form of intervention. According to the Practice Guideline for the Treatment of Patients with Acute Stress Disorder and Posttraumatic Stress Disorder,34 debriefing is not recommended as it may worsen symptoms in some individuals. In addition, there is no firm evidence that debriefing genuinely reduces the subsequent risk of symptom development. However, anecdotally, some participants report beneficial outcomes.
Education. Education about a disorder, including PTSD, typically is helpful for patients. This can be accomplished during the office visit in a didactic yet informal manner by the primary care clinician. In addition, a resource list about PTSD, including Internet resources and illustrative movies, is provided here for patients. (See Table 5.) In follow-up care, anniversary dates may be particularly important to discuss in terms of symptom recurrence.
Supportive Counseling. Supportive counseling in the primary care setting is always a practical starting place in the management of PTSD. Helpful techniques include encouraging patient verbalization of the event, validation of feelings, and assessment of needed resources. Clinicians need to be aware that some patients may not tolerate detailed review of their trauma without psychological decompensation, and focusing on "here and now" issues may be more helpful. In sorting out needed resources, safety or a sense of safety is critically important, particularly in dealing with victims of rape. Other needs might be addressed through the identification of support networks, the use of local and state agencies for temporary financial assistance, and the recommendation of trauma-specific support groups (e.g., rape support groups).
Pharmacotherapy. From a primary care perspective, the initial pharmacological management of PTSD is unequivocally clear, given the general consensus of the empirical data. The Practice Guideline for the Treatment of Patients with Acute Stress Disorder and Posttraumatic Stress Disorder34 states that selective serotonin reuptake inhibitors (SSRIs) are the "medications of choice." SSRIs are effective in the treatment of the core RAH symptoms of PTSD and, because of their broad spectrum of clinical activity, may be helpful in the treatment of comorbid psychiatric disorders (e.g., depression), as well.34 In addition, SSRIs are known for their excellent tolerability and mild side effect profiles.
Two SSRIs are the only medications with FDA indications for PTSDsertraline and paroxetine. However, from a practical perspective, it is likely that all of the SSRIs are efficacious in the treatment of PTSD, but no comparative trials among SSRIs have been undertaken. The use of paroxetine carries a greater risk of weight gain than the other SSRIs (recall that the preponderance of PTSD victims are women) although the mildly sedating effects may be beneficial for some patients, and the use of fluoxetine has a greater potential for activating side effects (e.g., potentially beneficial with fatigue, but a risk of insomnia).
While usual dosing of SSRIs can be undertaken, some patients may be sensitive to serotonergic medications. Therefore, when using sertraline, for example, the authors suggest beginning at 12.5 mg per day for 3-4 days, with 12.5-mg increases every 3-4 days to an initial dosage of 50 mg per day. When using paroxetine, for example, the authors suggest beginning at 10 mg for 3-4 days, and then increasing the dose to 20 mg per day. PTSD symptoms tend to respond to standard-dose SSRIs within 2-4 weeks of treatment. If there is no response, it is recommended that the dose of the SSRI gradually be increased to the recommended upper limits. If an initial SSRI is ineffective, consider a second pharmacotherapy trial with a different SSRI using the same dosing principles (i.e., low starting dose, gradual increases to standard dose, increases to maximum doses if there is no response after 4-6 weeks). While the duration of treatment for PTSD remains unknown, the authors suggest an initial year or longer.
While SSRIs are drugs of first choice, in some cases the addition of a second psychotropic medication (i.e., augmentation) may be useful. (Bear in mind that none of the following medications is approved for PTSD, and their use as augmentors is off-label.) In this regard, anticonvulsants (divalproex, carbamazepine, topiramate, lamotrigine) have demonstrated some efficacy with specific PTSD symptom clusters.34 However, with the exceptions of topiramate and gabapentin, most anticonvulsants are difficult to use because of drug interactions, the need for serum levels, ongoing laboratory monitoring, and/or unusual side effects (e.g., the risk of Stevens-Johnson syndrome with lamotrigine). In the primary care setting, if necessary, augmentation with either topiramate (beginning at 25 mg per day, and increasing the dose by 25 mg every 10 days, up to 50-100 mg per day) or gabapentin (beginning at 100 mg at bedtime and titrating the dose to 300 mg or more per day in divided doses) can be considered. Note that these are very conservative dosing schedules. As a caveat, topiramate may lower serum levels of oral contraceptives, increasing the risk of pregnancy; for that reason, physicians should avoid prescribing it to women on birth control pills. In addition, rapid titration of Topamax may cause confusion.
A final augmentation option might be the addition of a low-dose atypical antipsychotic. Again, the use of the type of augmenting medication is off-label. Empirical data support the use of olanzapine, quetiapine, and risperidone in PTSD.34 Of these, risperidone is probably the least complicated to utilize (i.e., less likely to cause weight gain and metabolic consequences). However, future empirical studies may support the use of two other atypical antipsychotics, aripiprazole and ziprasidone, both of which have significantly better weight and metabolic profiles compared with the remaining atypical antipsychotics.
Clinically, insomnia is a frequent symptom among PTSD patients. Unfortunately, most of the available hypnotics are either benzodiazepines or affect benzodiazepine receptor sites (i.e., they are controlled substances and long-term use may result in physiological addiction). However, the authors have used trazodone successfully for insomnia at doses of 50-100 mg at bedtime. Males have a very small risk of developing priapism while taking trazodone and should be warned about this potential complication; prompt treatment in an emergency room is advised. Documentation in the patient's medical record of the disclosure of this risk and the recommended intervention is essential. Ramelteon, a melatonin agonist, also may be a consideration for long-term insomnia related to PTSD. Ramelteon is not a controlled substance and may be used for lengthy periods of time with no risk of addiction. The dose is 8 mg at bedtime.
Because many patients with trauma-based symptoms present in a hyperaroused state, there is the temptation to acutely prescribe benzodiazepines. According to the practice guidelines,34 there is no evidence to support their use. Studies of benzodiazepines in the treatment of acute trauma symptoms indicate ineffective35 as well as poorer outcomes.36 Additional concerns with benzodiazepines include the risks of physiological addiction, worsening of comorbid mood symptoms, and cognitive impairment both in the short- and long-term. At present, their use by primary care clinicians for the treatment of PTSD is not recommended.
Several other types of medications are being explored for the acute treatment of trauma symptoms. These include cortico-steroids and beta blockers.33 Both have been studied in medical settings and appear promising in terms of reducing the subsequent development of PTSD, but require further investigation.
Given the preceding pharmacological recommendations, psychiatric referral for medication assessment depends upon the experience and comfort level of the primary care clinician with psychotropic medications. Most practitioners likely will be fully comfortable with two individual SSRI trials should an initial trial be ineffective. Referral should take place when there is minimal patient response to medication and the primary care clinician has exhausted the psychotropic medications for PTSD with which he or she feels comfortable and experienced.
Outcome
Because of the many different types of possible trauma as well as the varying psychological complexions of those exposed to trauma, general outcome is difficult to summarize. According to Lindman and colleagues,37 prisoners of war tend to experience a gradual decline of symptoms, followed by an increase in symptoms in old age. Among community samples, Perkonigg and colleagues38 found that PTSD tends to be a chronic and persistent disorder. Overall, it appears that with treatment, most patients with PTSD experience significant reductions in symptomatology. However, many tend to have residual symptoms, and PTSD symptoms may undergo exacerbations and remissions throughout an individual's lifetime.
Medical morbidity is one of the more disturbing legacies of PTSD. PTSD has been associated with cardiovascular disease, diabetes, gastrointestinal disease, fibromyalgia, chronic fatigue syndrome, and musculoskeletal diseases;39 an increased risk of mortality following cardiac transplantation;40 a greater risk of myocardial reinfarction and death;41 and an overall increased risk of early mortality.42,43 These outcomes may be related to the physiological consequences of PTSD (i.e., altered immunity, alterations in lipid metabolism) as well as other factors, such as poor compliance or nonadherence to treatment.44
Conclusions
According to community studies, PTSD is a relatively common psychiatric disorder. Diagnosis requires the confirmation of a traumatic exposure, an intense fear response, symptom duration of at least 4 weeks, and impaired functionality. The core symptoms of PTSD relate to reexperiencing, avoidance, and hyperarousal (acronym: RAH). Proximity and degree of exposure, as well as pre-existing trauma and psychiatric disorders, heighten the risk of developing PTSD. Basic initial treatment strategies include education, supportive psychotherapy, and pharmacotherapy with SSRIs. While SSRIs are the initial pharmacological intervention, possible augmentation with anticonvulsants or atypical antipsychotics may be necessary. PTSD symptoms clearly respond to treatment; however, the overall course of the disorder for many is characterized by exacerbations and remissions, and residual symptoms.
References
1. Ramaswamy S, Madaan V, Qadri F, et al. A primary care perspective of posttraumatic stress disorder for the Department of Veterans Affairs. Prim Care Companion J Clin Psychiatry 2005;7:180-187.
2. Mendlowicz MV, Stein MB. Quality of life in individuals with anxiety disorders. Am J Psychiatry 2000;157:669-682.
3. American Psychiatric Association. Diagnostic and statistical manual of mental disorders, 3rd edition. Washington, DC: American Psychiatric Association; 1980.
4. American Psychiatric Association. Diagnostic and statistical manual of mental disorders, 4th edition. Washington, DC: American Psychiatric Association; 1994.
5. McWilliams LA, Cox BJ, Asmundson GJG. Symptom structure of posttraumatic stress disorder in a nationally representative sample. J Anxiety Disord 2005;19:626-641.
6. Birmes P, Brunet A, Carreras D, et al. The predictive power of peritraumatic dissociation and acute stress symptoms for posttraumatic stress symptoms: A three-month prospective study. Am J Psychiatry 2003;160:1337-1339.
7. Harvey AG, Bryant RA. The relationship between acute stress disorder and posttraumatic stress disorder: A 2-year prospective evaluation. J Consult Clin Psychol 1999;67:985-988.
8. Kessler RC, Sonnega A, Bromet E, et al. Posttraumatic stress disorder in the National Comorbidity Survey. Arch Gen Psychiatry 1995;52:1048-1060.
9. Zatzick DF, Russo JE, Katon W. Somatic, posttraumatic stress, and depressive symptoms among injured patients treated in trauma surgery. Psychosomatics 2003;44:479-484.
10. Schnurr PP, Friedman MJ, Sengupta A, et al. PTSD and utilization of medical treatment services among male Vietnam veterans. J Nerv Ment Dis 2000;188:496-504.
11. Deykin EY, Keane TM, Kaloupek D, et al. Posttraumatic stress disorder and the use of health services. Psychosom Med 2001;63: 835-841.
12. Marshall RP, Jorm AF, Grayson DA, et al. Posttraumatic stress disorder and other predictors of health care consumption by Vietnam veterans. Psychiatr Serv 1998;49:1609-1611.
13. Miranda R, Meyerson LA, Marx BP, et al. Civilian-based posttraumatic stress disorder and physical complaints: Evaluation of depression as a mediator. J Trauma Stress 2002;15:297-301.
14. Van Ommeren M, Sharma B, Sharma GK, et al. The relationship between somatic and PTSD symptoms among Bhutanese refugee torture survivors: Examination of comorbidity with anxiety and depression. J Trauma Stress 2002;15:415-421.
15. Prins A, Ouimette P, Kimerling R, et al. The Primary Care PTSD Screen (PC-PTSD): Development and operating characteristics. Prim Care Psychiatry 2003;9:9-14.
16. Kessler RC, Berglund P, Demler L, et al. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry 2005;62:593-602.
17. Kessler RC, McGonagle KA, Zhao S, et al. Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in the United States. Results from the National Comorbidity Survey. Arch Gen Psychiatry 1994;51:8-19.
18. Ruchkin V, Schwab-Stone M, Jones S, et al. Is posttraumatic stress in youth a culture-bound phenomenon? A comparison of symptom trends in selected U.S. and Russian communities. Am J Psychiatry 2005;162:538-544.
19. Culpepper L. Treating posttraumatic stress disorder in primary care settings: The expert consensus guidelines. Prim Care Companion Reports 2000;1-12.
20. Koren D, Norman D, Cohen A, et al. Increased PTSD risk with combat-related injury: A matched comparison study of injured and uninjured soldiers experiencing the same combat events. Am J Psychiatry 2005;162:276-282.
21. Shalev AY, Freedman S. PTSD following terrorist attacks: A prospective evaluation. Am J Psychiatry 2005;162:1188-1191.
22. Newport DJ, Nemeroff CB. Neurobiology of posttraumatic stress disorder. Curr Opin Neurobiol 2000;10:211-218.
23. Yehuda R. Post-traumatic stress disorder. N Engl J Med 2002;346: 108-114.
24. Raison CL, Miller AH. When not enough is too much: The role of insufficient glucocorticoid signaling in the pathophysiology of stress-related disorders. Am J Psychiatry 2003;160:1554-1565.
25. Kawamura N, Kim Y, Asukai N. Suppression of cellular immunity in men with a past history of posttraumatic stress disorder. Am J Psychiatry 2001;158:484-486.
26. Yehuda R. Neuroendocrinology. In: Nutt D, Davidson JRT, Zohar J, eds. Post-Traumatic Stress Disorder. London: Martin Dunitz; 2000:58-63.
27. Mahmutyazicioglu K, Konuk N, Ozdemir H, et al. Evaluation of the hippocampus and the anterior cingulate gyrus by proton MR spectroscopy in patients with post-traumatic stress disorder. Diagn Interv Radiol 2005;11:125-129.
28. Kitayama N, Vaccarino V, Kutner M, et al. Magnetic resonance imaging (MRI) measurement of hippocampal volume in posttraumatic stress disorder: A meta-analysis. J Affect Disord 2005;88:79-86.
29. Robertson M, Humphreys L, Ray R. Psychological treatments for posttraumatic stress disorder: Recommendations for the clinician based on a review of the literature. J Psychiatr Pract 2004;10:106-118.
30. Bleiberg KL, Markowitz JC. A pilot study of interpersonal psychotherapy for posttraumatic stress disorder. Am J Psychiatry 2005;162:181-183.
31. Spoont MR, Sayer NA Thuras P, et al. Practical psychotherapy: Adaptation of dialectical behavior therapy by a VA medical center. Psychiatr Serv 2003;54:627-629.
32. Bradley R, Greene J, Russ E, et al. A multidimensional meta-analysis of psychotherapy for PTSD. Am J Psychiatry 2005;162:214-227.
33. Cahill SP, Pontoski K, D'Olio CM. Posttraumatic stress disorder and acute stress disorder II: Considerations for treatment and prevention. Psychiatry 2005;2:34-46.
34. American Psychiatric Association. Practice guideline for the treatment of patients with acute stress disorder and posttraumatic stress disorder. Washington, DC: American Psychiatric Association.
35. Gelpin E, Bonne O, Peri T, et al. Treatment of recent trauma survivors with benzodiazepines: A prospective study. J Clin Psychiatry 1996;57:390-394.
36. Viola J, Ditzler T, Batzer W, et al. Pharmacological management of post-traumatic stress disorder: Clinical summary of a five-year retrospective study, 1990-1995. Mil Med 1997;162:616-619.
37. Lindman C, Engdahl B, Frazier P. A longitudinal and retrospective study of PTSD among older prisoners of war. Am J Psychiatry 2001;158:1474-1479.
38. Perkonigg A, Pfister H, Stein MB, et al. Longitudinal course of posttraumatic stress disorder and posttraumatic stress disorder symptoms in a community sample of adolescents and young adults. Am J Psychiatry 2005;162:1320-1327.
39. Boscarino JA. Posttraumatic stress disorder and physical illness: Results from clinical and epidemiologic studies. In: Yehuda R, McEwen B, eds. Biobehavioral Stress Response: Protective and Damaging Effects. New York: New York Academy of Sciences; 2004;1032:141-153.
40. Dew MA, Kormos RL, Roth LH, et al. Early post-transplant medical compliance and mental health predict physical morbidity and mortality one to three years after heart transplantation. J Heart Lung Transplant 1999;18:549-562.
41. Pedersen SS, Middel B, Larsen ML. Posttraumatic stress disorder in first-time myocardial infarction patients. Heart Lung 2003;32:300-307.
42. Johnson DR, Fontana A, Lubin H, et al. Long-term course of treatment-seeking Vietnam veterans with posttraumatic stress disorder: Mortality, clinical condition, and life satisfaction. J Nerv Ment Dis 2004;192:35-41.
43. Boscarino JA. Posttraumatic stress disorder and mortality among US army veterans 30 years after military service. Ann Epidemiol (in press).
44. Shemesh E, Yehuda R, Milo O, et al. Posttraumatic stress, nonadherence, and adverse outcome in survivors of a myocardial infarction. Psychosom Med 2004;66:521-526.
Post-traumatic stress disorder (PTSD) is a complex psychobiological syndrome that evolves in vulnerable individuals as a direct consequence of exposure to trauma. While different types of trauma such as natural disasters or rape may precipitate the disorder, the sequelae of symptoms are consistent among victims.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.