Cardiovascular Risk Reduction for Patients with Diabetes Mellitus
Cardiovascular Risk Reduction for Patients with Diabetes Mellitus
Author: Jay H. Shubrook DO, FACOFP, Assistant Professor of Family Medicine, Diabetologist, Ohio University College of Osteopathic Medicine, Athens.
Peer Reviewer: John A. Colwell, MD, PhD, MACP, Professor of Medicine, Director, Diabetes Center, Medical University of South Carolina, Charleston.
Introduction
Cardiovascular disease affects 25% of the U.S. population. It is responsible for more than 1 million deaths each year, which makes it the number one killer in the United States.1 Fifty percent of men and 64% of women who suffer from sudden cardiac death have no previous history or symptoms of heart disease.2
Diabetes is a major risk factor for cardiovascular disease. An important modifiable risk factor for type 2 diabetes is obesity. The U.S. population has become increasingly obese, and the number of people with diabetes continues to rise at an exponential rate. This rate of increase has far exceeded what was predicted even 10 years ago. The incidence of diabetes has increased by 14% in the last 3 years to a total of almost 21 million Americans, or 7% of the U.S. population. The CDC predicts that one in three people born in the United States in the year 2000 eventually will develop diabetes.3
Cardiovascular disease is responsible for 80% of deaths in people with diabetes mellitus. The Framingham study showed that diabetes increases the risk of cardiovascular death by two times in men and four to five times in women.4 In fact, according to one study, a person with type 2 diabetes has a cardiovascular risk that is equivalent to that of someone who already has had a myocardial infarction.5
It now is well recognized that people with diabetes are at increased risk of silent coronary artery disease (CAD) and have a 50% risk of having a silent myocardial infarction. In addition, once coronary artery disease becomes symptomatic, morbidity and mortality rates are greater than for people without diabetes.6
Unfortunately, Americans are complacent about their cardiovascular risk. According to a Harris Interactive Poll, 57% of Americans do not feel that they are at risk for cardiovascular disease, and 41% report that they don’t believe it is a major cause of death in the United States.7 Americans also are overly optimistic about their ability to control their own health. In the study referenced above, 76% of Americans reported they were trying to maintain a healthy weight, yet only 36% were able to do so. Sixty-eight percent said they tried to exercise regularly, but again, only 19% were able to achieve their goal. Sixty percent were trying to avoid high fat, high cholesterol foods, but only 10% actually followed the national nutritional guidelines.7 Lifestyle modifications to reduce cardiovascular disease will have to be comprehensive and will require a major shift in the habits of the average American.
Key Points
- Cardiovascular disease is the number 1 cause of death in the United States.
- Americans may not recognize the severity of this disease or their personal risk.
- The lifestyle of most Americans increases their risk of diabetes and cardiovascular disease.
- One in 3 Americans born in the year 2000 will develop diabetes.3
Diabetes is a multi-organ-system disease that is difficult for patients to understand and manage. Nearly every decision of every day can have an influence on glucose control. Diabetes is a chronic, incurable disease, and patients often tire in their efforts to maintain control. The modifiable risk factors for diabetes are well entrenched in our sociocultural habits and are very difficult to break.
The American Diabetes Association has published recommendations for diabetes self-care management. It has been estimated that for a person to complete all of the recommendations for diabetes self-care would require a great commitment of time and energy. In one study it was estimated that it would take more than two hours each day to complete the ADA recommended components for diabetes self-care.8 Such a time requirement could be seen as an unrealistic expectation for those who already are overwhelmed by multiple daily commitments.
Physicians must actively and comprehensively manage patients both in terms of the patient’s individual concerns as well as current and future health risks. The time needed to educate patients about reducing cardiovascular risk is a challenging task for physicians when patient visits often are limited to 5-10 minutes. This barely allows enough time to manage an acute problem, let alone to address that problem in the context of a chronic disease. This point is exemplified by the following case.
A 48-year-old female who presents for fatigue. She has been fatigued for the greater part of the year, but has not sought a health care provider as she attributed her symptoms to "getting older." At her annual bus driver physical she had high blood pressure and glucosuria. These findings caused her to fail her physical and she was told to follow up with her primary care physician. She has not been to the doctor in three years. She does not take any medications. She smokes one-half pack of cigarettes per day and does not drink any alcohol. She does drink two cups of coffee per day. She is married with two children, both teenagers. She feels she has a supportive family. Her main stressors are financial and work-related. She denies any other complaints.
Her BMI is 32. Her blood pressure is 148/90, and her fasting finger stick glucose is 149 mg/dL. Her exam reveals acanthosis nigricans around the posterior aspect of her neck, but the exam is otherwise normal. Her lab results revealed a fasting plasma glucose of 178 mg/dL; total cholesterol is 260 mg/dL; LDL-C is 172 mg/dL; triglycerides are 280 mg/dL, and HDL-C is 32 mg/dL.
She is diagnosed with hypertension, diabetes mellitus, dyslipidemia, and metabolic syndrome. She has the additional modifiable risk factors of smoking and obesity. Each diagnosis is a recognized risk factor for cardiovascular disease. When these risk factors are present in combination, the risk amplifies greatly.9
Patients who present with multiple medical problems present a challenge to the primary care physician. This patient presents with fatigue that may or may not be related to the diagnosis provided to her. Often, patient priorities and concerns are different than the physician’s. She may be concerned that her physician will load her up with medications that may make her feel even worse.
Prioritizing Treatment Strategies
In patients who present with numerous CV risks, including diabetes, the physician must decide on a strategy to treat each condition. Previous studies have shown that in many health care settings physicians tend to address the hyperglycemia first, then the lipids, and finally blood pressure in a person who has all three problems. In a study by Bergenstal, et al, physicians placed the highest priority on glucose control. When asked about treatment priorities, physicians selected glucose control as their top priority 68% of the time, blood pressure control 11%, lipids control 9%, and diet and exercise 9% of the time. (See Table 1.) Correspondingly, physicians have the most success meeting goals for glucose control (57.6%) and less success reaching ideal lipid levels (47.7%) and blood pressure levels (22.8%).10 Even in those physicians who placed the highest priority on achieving goal blood pressure levels, they were still less successful at achieving this goal than at reaching goals for glucose and lipid control.10 In contrast, population-based studies have shown that the greatest mortality benefits come from treatment of hypertension first, dyslipidemia second, and hyperglycemia last.11
| Table 1. Physician Treatment Priority and Success in Achieving Goal Levels of Treatment (Compared to Documented Mortality Benefit) |
|
|
National guidelines have been published and widely recognized for the treatment of hypertension, dyslipidemia, and diabetes. Yet, physicians have a low rate of success in controlling these diseases.
Key Points
- Guidelines exist for the treatment of hypertension, dyslipidemia and diabetes.
- Physicians often focus attention on glucose control first with limited success.
- Even less success is achieved with blood pressure and lipid control.
- Reaching blood pressure goals provides the greatest mortality benefits, followed by achieving goals for lipids, and lastly achieving recommended glucose goals.
Maximizing the cardiovascular risk reduction for the person with type 2 diabetes requires a systematic and programmed approach. The terrible triad of hypertension, dyslipidemia, and hyperglycemia must be monitored actively to allow optimal control. Therapeutic lifestyle measures should be the cornerstone of treatment for these conditions. The NCEP ATP III Panel recommends lifestyle changes as the primary and most cost-effective means of preventing coronary heart disease.12,13 Iestra showed in a systematic review that lifestyle measures such as diet, 5-10% weight loss, physical activity, and smoking cessation do yield significant benefits for people with diabetes and coronary heart disease.14
Hypertension
Acknowledging mortality benefits, hypertension should be addressed first. The JNC 7 guidelines for the treatment of hypertension15 now identify four stages of blood pressure control. (See Table 2.) Normal blood pressure is systolic less than 120 mmHg and diastolic less than 80 mmHg. Pre-hypertension is identified as a systolic blood pressure of 121-139 mmHg, or diastolic blood pressure of 80-89 mmHg. Stage 1 hypertension is defined as systolic blood pressures of 140-159 mmHg or diastolic of 90-100 mmHg. Stage 2 hypertension is defined as systolic blood pressure of greater than 160 mmHg or diastolic greater than 100 mmHg.
| Table 2. JNC 7 Classification of Hypertension |
|
|
A recent study demonstrated that even pre-hypertension will increase cardiovascular risk.16 Nationally, physicians have a very low rate of success in treating hypertension. Based on JNC 6 guidelines, only 27% of Americans achieved a blood pressure goal of below 140/90 mmHg.17 Success rates were even lower in people with diabetes. Only 11% met the goal recommended by the ADA of 130/85.17 Achieving blood pressure goals in a person with type 2 diabetes typically requires a minimum of two agents and often 3-4 blood pressure agents at effective doses. Yet, according to some studies, combination therapy is utilized as little as 18% of the time.10
A number of recent studies have shown that the treatment of hypertension will reduce cardiovascular events even more than in those without diabetes.
The HOT trial revealed a 51% risk reduction for cardiovascular events for people with type 2 diabetes when the diastolic blood pressure was decreased from less than 90 mmHg to less than 80 mmHg, supporting the lower blood pressure goal for people with diabetes.18 In the HOPE study, the use of ramipril for treating hypertensive people with diabetes reduced the risk of myocardial infarction by 22% and cardiovascular death by 37%.19 These results were greater than predicted from the drop in blood pressure alone. This was further supported by the findings in the LIFE trial using the angiotensin receptor blocker (ARB) losartan. The UKPDS study found that tight pressure control far exceeded the benefits of tight glucose control for reduction in stroke, any diabetes endpoint, death, and even micro-vascular complications.20
In treating hypertension, initial treatment should consist of an angiotensin-converting enzyme inhibitor (ACEI) or an angiotensin II receptor blocker (ARB). These agents are recommended for people with diabetes in the JNC 7 guidelines. The very low incidence of side effects allows patients to gain confidence, realizing they do not have to feel worse to "look better" in the physician’s eyes. Once it has been documented that there is not a substantial change in creatinine (less than 30%) from this first agent, the initial agent is titrated up to the maximum dose tolerated, or a normal blood pressure. If additional treatment is needed, the addition of a thiazide diuretic is appropriate. This is supported by the ALLHAT trial and the JNC 7 guidelines, which recommend thiazide diuretics for those people without other compelling indications.15,21 If further blood pressure reduction is needed, a third agent, such as an ACEI, an ARB, or non-dihydropyridine calcium channel blocker is recommended. If there are co-morbid illnesses such as coronary artery disease/angina or migraine headache a beta blocker may be helpful.
Ultimately, the focus of treatment should be on reaching the blood pressure goal level and finding a combination of medications that the patient will tolerate. Adherence to antihypertensive medications is one of the main challenges to treating hypertension.
Treatment Recommendations
- Treatment of hypertension should be the top priority in people with diabetes.
- Goal blood pressure should be below 130 mmHg systolic and below 80 mmHg diastolic.
- Use an ACEI or ARB as part of treatment (provided no contraindications exist).
- Combination therapy for hypertension should be standard.
Dyslipidemia
Atherogenic dyslipidemia is found regularly in people with diabetes. Type 2 diabetes often is associated with elevated total cholesterol, normal to high LDL levels (but the small dense particles), low HDL, and high triglycerides. The National Cholesterol Education Program Adult Treatment Panel III (NCEP ATP III) guidelines recommend LDL reduction as the primary treatment goal. People who are at high risk for cardiovascular disease should have an LDL below 100 mg/dL.13 The keystone of pharmacotherapy for people with cardiovascular disease and diabetes should be the use of the HMG Co-A reductase inhibitor (statin) regardless of initial LDL level.
Primary Prevention Studies. In the CARDS trial, people with diabetes and no known history of coronary artery disease benefited from lowering the LDL to very low levels (treatment LDL level below 80 mg/dL). This study demonstrated a 37% risk reduction in cardiovascular events, with a 48% reduction in stroke and 36% reduction in coronary heart disease events.22 In the Heart Protection Study, even people with normal cholesterol levels experienced a reduction in cardiovascular disease when treated with simvastatin, further supporting the premise that all people with diabetes would benefit from at least a 30% reduction in LDL cholesterol.23
Secondary Prevention Studies. Recent studies have shown that people with established cardiovascular disease should have an LDL cholesterol below 70 mg/dL, as this level is even more protective for this high-risk population. The ASCOT-LLA trial showed that atorvastatin reduced cardiovascular events and interventions by 23% compared to placebo in people with type 2 diabetes.24 In the Treating to New Target Study, diabetic patients placed on atorvastatin 80 mg daily experienced a reduction in cardiovascular events of 25% compared to atorvastatin 10 mg daily.25 In the PROVE-IT trial, patients received greater benefit from high-dose atorvastatin than from low-dose pravastatin.26 In light of these findings, the NCEP committee published an interim report recommending that people at very high risk could benefit from optional lowering of LDL cholesterol to below 70 mg/dL.27
These trials have shown the benefit of primary and secondary cardiovascular reduction with the use of statins. Furthermore, people with diabetes show even greater benefits from statins compared to those without. It has been suggested that all people with diabetes should be on a statin that will decrease their LDL cholesterol by at least 30%.
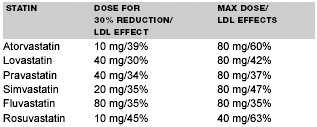
The American Diabetes Association recommends that if the LDL cholesterol is below 130 mg/dL, then diet and lifestyle modification can be attempted first.28 However, if the LDL cholesterol is greater than 130 mg/dL, it is recommended that pharmacotherapy be prescribed with a goal LDL reduction of 30-40%.28 Having knowledge of the potencies of each of the statins allows the physician to tailor treatment to the needs of each patient. (See Table 3.)
| Table 3. Comparative Potencies of the Starting and Maximum Doses of Statins (Recommended by ADA) |
|
|
All of the statins have similar profiles of efficacy beyond the starting dose. Each time the statin dose is doubled, an additional 6% reduction in LDL cholesterol is achieved. One way to have further reduction in LDL cholesterol while limiting additional side effects is to use an alternate medication such as ezetimibe in combination with a statin. This can reduce LDL cholesterol an additional 18%. This would be the equivalent of tripling the dose of the statin. This strategy has the potential benefit of lowering LDL-C with a lower incidence of statin side effects. Studies have shown that more patients reached their goal level with a combination of ezetimibe and a statin than with a statin alone.29
Estimates show that appropriate use of statin therapy could prevent 67,000 coronary deaths, 78,000 strokes, 117,000 non-fatal myocardial infarction, and 146,000 revascularization procedures each year. For the physician who treats 1000 high-risk patients, lipid lowering therapy and lifestyle modifications could prevent 1 myocardial infarction, stroke, or death every 12 days.30
Normalization of the triglycerides is a secondary treatment goal of the NCEP guidelines. Triglyceride levels are considered mildly elevated if the level is greater than 150 mg/dL but less than 400 mg/dL. Moderate elevation is between 400-600 mg/dL. Any level above 600 mg/dL is considered severe hypertriglyceridemia. Hypertriglyceridemia is especially common in people with type 2 diabetes and may be a marker of insulin resistance. Exercise has been shown to be beneficial for lowering hypertriglyceridemia. Fibrates and niacin also have been shown to be effective. In the VA-HIT study, gemfibrozil reduced combined cardiovascular risk by 32% in people with type 2 diabetes.31 In the recent FIELD study, the use of fenofibrate in people with type 2 diabetes was unsuccessful in reducing the primary outcome of coronary events, but it did reduce non-fatal myocardial infarctions and revascularization.32
Currently, the NCEP guidelines do not recommend treating HDL cholesterol as a primary or secondary endpoint. However, low levels of HDL cholesterol also can be a substantial risk factor for cardiovascular disease.33 Regardless of the level of LDL cholesterol, a drop in HDL cholesterol of 1 mg/dL increases cardiovascular risk by 3%.34 It is likely that future NCEP guidelines will include HDL treatment as one of the treatment targets.
HDL cholesterol can be raised by the following: exercise with greater than 1200 calories exerted per week, emphasizing duration over intensity; moderate alcohol intake; and weight loss. During the initial phase of weight loss HDL cholesterol drops. After weight loss is stabilized, for every 7 pounds lost, HDL cholesterol will rise 1 mg/dL. There are very few medications that raise HDL-C levels. Fibrates can raise HDL cholesterol by 25%. Niacin is the most potent agent in raising HDL and can raise levels as much as 30%. It is suspected that the HDL-C will continue to "creep" up over time on niacin therapy and that may translate into increasing benefits with long-term use.
Despite excellent medications to treat dyslipidemia, physicians have a low rate of success in meeting national recommendations. A recent study showed that only 49% of patients with diabetes reached an LDL goal below 100 mg/dL. Of the high-risk patients who would benefit from an LDL below 70 mg/dL, only 16% were at target.35
Treatment Recommendations
- Achieve LDL-C level below 100 mg/dL. The goal should be below 70 mg/dL if the person has documented cardiovascular disease.
- Use a statin for people with diabetes as the primary choice to lower LDL-C levels, if indicated.
- Triglycerides should be below 150 mg/dL with glucose control and primary lipid treatments.
- HDL should be greater than 45 mg/dL in men and 55 mg/dL in women.
Glucose Control
Despite the most intense efforts placed on glucose therapy, it has the least effect in reducing cardiovascular risk. However, some recent studies have emerged suggesting that glucose control can be beneficial. In the PROactive trial, pioglitazone was added to routine diabetes management, resulting in a 16% decrease in the secondary endpoints of death, non-fatal myocardial infarction, and stroke.36
In the United Kingdom Prospective Diabetes Study, a very large trial evaluating treatment for type 2 diabetes, researchers found that intensive glucose control was associated with a 25% reduction in diabetes-related deaths and treatment with metformin reduced cardiovascular deaths in obese patients.37 Each decrease in A1c of 1% was associated with a 21% decrease in diabetes-related deaths and a 14% decrease in myocardial infarction.38 This relationship was continuous with no lower threshold extending into normal A1c levels below 6%.38
The results of the Epidemiology of Diabetes Interventions and Complications (EDIC) trial recently were published and demonstrate profound benefits for intensive glucose control in people with type 1 diabetes.39 The EDIC trial was the continuation of the Diabetes Complications and Control Trial (DCCT). Patients were offered the opportunity to continue in the study, but their primary diabetes physician was allowed to control insulin therapy. In the 11 years that followed, the standard control group received greater intensity of glucose control with an improvement of HgA1c from 9.1% to 8.2%. The former intensively treated group loosened glucose control, and HgA1c rose from 7.4% to 8.1%. Despite the groups having similar glucose control in this second period, the former intensively treated group had a 42% reduced risk of any cardiovascular event and a 57% reduction in cardiovascular deaths. This is the first trial to show long-term cardiovascular benefit from intensive glucose control with insulin for people with type 1 diabetes.
Treatment Recommendations.
- Achieve HgA1c goal of at least below 7%.
- Use treatments that have been shown to decrease cardio-vascular risk (metformin and pioglitazone in type 2 diabetes).
- Intensive insulin control can reduce cardiovascular mortality use in type 1 diabetes.
Comprehensive Treatment Plan
In order to have a major impact on diabetes-related mortality, multi-modal therapy is necessary. Unfortunately, physicians have had a low rate of success in controlling hypertension, dyslipidemia, and glucose simultaneously. A study evaluating treatment at academic medical centers revealed that only 34% achieved a glucose goal of an A1c below 7.0%, 33% had a blood pressure below 130/80, and 46% had an LDL below 100 mg/dL. Only 10% of patients had all three at goal level.40
The Steno-2 study addressed this issue. This is a landmark study41 evaluating comprehensive cardiovascular care for people with type 2 diabetes mellitus. This was an open-label study that randomized patients with type 2 diabetes and micro-albuminuria to routine care vs. intensive treatment of glucose, blood pressure, and lipids. The primary endpoint was the composite of cardiovascular death, non-fatal myocardial infarction, non-fatal stroke, revascularization, and amputation. Patients were followed for 8 years.
Intensive treatment included dietary evaluation and treatment that reduced total fat calories to less than 30% and saturated fats to less than 10%. Participants were asked to exercise at least 30 minutes/day, 3-5 times per week. All participants who smoked (and spouses) were enrolled in smoking cessation classes. All participants were treated with an ACEI or ARB (captopril 50 mg BID or losartan 50 mg or equivalent) regardless of blood pressure status. For blood pressure control, other agents could be added. All patients were given 150 mg of aspirin per day. The HgA1c goal was 6.5%. Initially patients were started on either metformin or sulfonylurea monotherapy. If patients were not at goal level, the other medication was added. If the participant’s HgA1c still was above 7.0%, then insulin was added. For dyslipidemia, all patients were treated with a statin and increased to the maximum dose tolerated. Hypertriglyceridemia was treated with the use of fibrates.
Results of this study showed that intensive therapy decreased cardiovascular disease by 53%, nephropathy by 61%, retinopathy by 50%, and autonomic neuropathy by 63%. In addition, they were able to prevent one cardiovascular event for every five patients treated.41 This kind of comprehensive treatment is needed to change the burden of cardiovascular disease in the United States. It is worth noting that the staff and resources utilized in a "study" setting often are not available to community physicians and may not reflect real world challenges.
Ongoing Studies
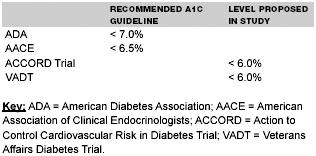
The National Institutes of Health is sponsoring an ongoing clinical trial with even more aggressive multi-modal therapies. In the Action to Control Cardiovascular Risk in Diabetes Trial (ACCORD), investigators are evaluating mortality benefits of decreasing HgA1c to below 6.0%, the addition of a fibrate to routine statin treatment, and attempting to determine the benefits of even tighter blood pressure control. Results of the study are forthcoming.
Another study looking at intensive glucose control is the Veterans Affairs Diabetes Trial (VADT). The VADT will include 1700 people with type 2 diabetes. The treatment group will include the early use of combination pharmacotherapy and a goal A1c of less than 6.0% vs. routine stepped care with a goal A1c of 8.0%-9.0%. Results may help to support setting lower A1c goals.42
Some physicians have recommended the development of a "super pill" that addresses multiple cardiovascular risk factors. Such a pill would include a statin, a diuretic, a beta-blocker, an ACE inhibitor, aspirin, and folic acid. It is believed that such a pill could reduce the incidence of coronary heart disease by 80% and stroke by 88%.43
| Table 4. Different Recommendations Regarding Goal A1c |
|
|
Making Office Visits More Efficient
Until this super pill becomes available physicians must utilize the resources at hand. These resources may include flow sheets for routine surveillance and tracking of preventive treatments. Quarterly visits can focus on specific concerns to ensure that all major issues are addressed. For example, one visit may focus on prevention. The physician can review the immunization status and update influenza and pneumococcal vaccines, confirm that the patient has a working glucometer and supplies, and determine if diabetes education is required. During the next visit, the physician would focus on cardiovascular disease by confirming that the patient is taking a daily aspirin, updating the annual electrocardiogram, reviewing the lipid panel, adjusting therapy, reviewing the current exercise program, and screening for symptoms of cardiovascular disease (i.e., angina, claudication, peripheral ischemia). During the third visit, the physician would focus on micro-vascular complications. This can include skin care and foot care, including prevention of neuropathy. Signs of gastroparesis also should be reviewed. Laboratory tests may be ordered at this point to determine the presence of nephropathy, micro-albuminuria, and creatinine clearance. The last appointment would focus on how the patient feels about his or her condition and the current treatment program. This is an opportunity for the patient to help the physician better understand the personal effects of diabetes. This would be an appropriate time to screen for depression. At every visit the physician will review the patient’s glucose logs and monitor the patient’s weight and blood pressure.
Treatment Recommendations
- Keep a running log of blood pressure, lipids, and A1c.
- Use flow sheets to monitor progress.
- Focus on blood pressure first, lipids second, and glucose control third when addressing cardiovascular risk.
- Make the diabetes-related visits themed, and stagger them to create a system for tracking the treatment plan.
Ancillary Treatments
Other ancillary therapies should be considered to reduce cardiovascular disease for people with type 2 diabetes. These therapies should include daily aspirin therapy and regular interval cardiovascular testing.
The American Diabetes Association recommends that all people older than age 40 who have diabetes and at least one cardiovascular risk factor should take a daily aspirin.44 Recent studies have identified that low-dose aspirin may be less protective in people with diabetes, so further studies are needed to determine the optimum dose for this population.45,46
All patients with diabetes who want to begin an exercise program should undergo cardiac stress testing first.47 The American Diabetes Association recommends that all people who have diabetes and two additional risk factors also should undergo cardiac stress testing. These additional risk factors include: total cholesterol greater than 240 mg/dL, LDL greater than 160 mg/dL, HDL less than 35 mg/dL, blood pressure greater than140/90 mmHg, current smoking, family history of premature coronary artery disease, or micro-albuminuria.48
In the Detection of Silent Myocardial Ischemia in Asymptomatic Diabetics Subjects Study, researchers found that this may not be adequate to identify those people at risk. In the DIAD study, people with type 2 diabetes who were considered to be of low cardiovascular risk underwent cardiac stress testing with nuclear imaging.49 All participants were thought to have no additional cardiovascular risk other than diabetes, and all patients were screened and felt to be asymptomatic. Twenty-two percent of these patients had evidence of silent ischemia, and 11% had evidence of critical ischemia. This confirms that all patients with type 2 diabetes are at substantial risk for cardiovascular disease despite perceived risk factors and the absence of symptoms. Interestingly, in this study people newly diagnosed with diabetes and people with diabetes for more than 11 years had the highest risk of having silent coronary heart ischemia.50
Treatment Recommendations
- All people with diabetes will benefit from regular exercise (1200 calories/week or 150 minutes/week).
- All adults with diabetes should undergo cardiac stress testing (with imaging) before starting an exercise regimen.
- All people with diabetes and at least one cardiovascular risk factor should take at least 75-162 mg of aspirin per day unless contraindicated.
- All people with diabetes should receive diabetes education, including strategies to work diabetes management into their lifestyle and education on healthy dietary practices.
Summary
The challenge for the physician is to provide comprehensive diabetes care focusing both on quality-of-life issues and attempting to reduce micro-vascular and macro-vascular disease. To be successful, physicians need to identify and utilize available community resources. Diabetes educators and diabetes treatment teams are critical to long-term success for both doctors and patients in the management of diabetes mellitus. Having visits that focus on certain aspects of the disease also may be beneficial. Using a systematic approach to chronic diseases like cardiovascular disease and diabetes mellitus allows the physician to prevent omissions in treatment. Studies have shown that without such a system, most physicians fall well below the ADA standards of care for the intensive management of people with diabetes. There are not enough endocrinologists to provide care for all those with diabetes, so primary care physicians will continue to be the primary provider of diabetes care for the majority of patients.
References
1, American Heart Association, Heart Disease and Stroke Statistics 2004. American Heart Association web site www.americanheart.org/statistics.
2. Ruoff GE. Evidence-based cardiovascular disease rrevention. Consultant 2005;11:1467-1482.
3. American Diabetes Association, Newly-released CDC Study on Diabetes Reflects Growing Diabetes Epidemic; Illustrates Need for Heightened Research and Prevention and Improved Health Care for Diabetes—20.8 Million Americans Now Have Diabetes, Up 14 Percent Since 2003, In: Diabetes Today, Diabetes News. 2005; October 26; 1-2.
4. Krolewski AS, Warram JH, Valsania P, et al. Evolving natural history of coronary artery disease in diabetes mellitus. Am J Med 1991;90;2A:58S-61S.
5. Haffner SM, Lehto S, Ronnemaa T, et al. Mortality from coronary heart disease in subjects with type 2 diabetes and in nondiabetic subjects with and without prior myocardial infarction. N Engl J Med 1998;339:229-234.
6. BARI Investigators. Seven-year outcome in the Bypass Angioplasty Revascularization Investigation (BARI) by treatment and diabetic status. J Am Col Cardiol 2000;35:1122-1129.
7. Harris Interactive Poll. The Pfizer Journal 2003;7:9.
8. Russell LB, Suh DC, Safford MM. Time requirements for diabetes self-management: Too much for many? J Fam Practice 2005;54(1):52-57.
9. Stamler J, Vaccaro O, Newton JD, et al. Diabetes, other risk factors, and 12 year cardiovascular mortality for men screened in the Multiple Risk Factor Interventional Trial. Diabetes Care 1993;16;434-444.
10. Bergenstal RM, Nag SS, Reusch JE, et al. Macrovascular risk factors in patients with diabetes: Physician treatment strategies and extent of control. Endocr Pract 2005;11:172-179.
11. Huang ES, Meigs JB, Singer DE. The effect of interventions to prevent cardiovascular disease in patients with type 2 diabetes mellitus. Am J Med 2001;111:633-642.
12. Olendzki B, Speed C, Domino FJ. Nutritional assessment and counseling for prevention and treatment of cardiovascular disease. Am Fam Phys 2006;73:257-264.
13. NCEP (National Cholesterol Education Program) ATP III. Third report of the national cholesterol education program expert panel on the detection , evaluation, and treatment of high blood cholesterol in adults. JAMA 2001;285:2486-2497.
14. Iestra JA, Kromhout D, Van der Schouw YT, et al. Effect size estimates of lifestyle and dietary changes on all cause mortality in coronary artery disease patients: a systematic review. Circulation 2005:112:924-934.
15. National Heart, Lung, and Blood Institute, National Institutes of Health, US Department of Health and Human Services. The Seventh Report of the Joint National Committee. Available at http://www.nhlbi.nih.gov/guidelines/hypertension.
16. Vasan RS, et al. Impact of high normal blood pressure on the risk of cardiovascular disease. N Engl J Med 2001;345:1291-1297.
17. Coresh J, et al. Prevalence of high blood pressure and elevated serum creatinine levels in the US: Findings from the Third National Health and Nutrition Examination Survey 1988-1994. Arch Internal Med 2001;161:1207-1216.
18. Hansson L, Lindholm LH, Niskanen L, et al. Effect of angiotensin-converting-enzyme inhibition compared with conventional therapy on cardiovascular morbidity and mortality in hypertension: The Captopril Prevention Project (CAPPP) randomised trial. Lancet 1999;353611-616.
19. HOPE Study Investigators. Effects of Ramipril on cardiovascular and microvascular outcomes in people with diabetes mellitus. Results of the HOPE Study and Micro-HOPE substudy. Lancet 2000;355:253-259.
20. [No authors listed.] Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38. UK Prospective Diabetes Study Group. BMJ 1998;317:703-713.
21. The ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group. Major outcomes in high risk hypertensive patients randomized to angiotensin converting-enzyme inhibitor or calcium channel blocker vs. diuretic. The Antihypertensive and Lipid Lowering Treatment to Prevent Heart Attack Trial. JAMA 2002;288:2981-2997.
22. Calhoun HM, Betterridge DJ, Durrington PN, et al. Primary prevention of cardiovascular disease with atorvastatin in type 2 DM in the Collaborative atorvastatin Diabetes Study (CARDS): Multicentre randomized placebo-controlled trial. Lancet 2004;364:685-696.
23. Heart Protection Collaborative Group. MRC/BHF Heart Protection study of cholesterol lowering with simvastatin in 5693 people with diabetes: A randomised placebo-controlled trial. Lancet 2003;361:2005-2016.
24. Sever PS, Poulter NR, Dahlof B, et al. Reduction in CV events with atorvastatin in 2,532 patients with type 2 DM. Diabetes Care 2005;28:1151-1157.
25. LaRosa JC, Grundy SM, Waters DD, et al. Treating to New Targets Investigators. Intensive lipid lowering with atorvastatin in patients with stable coronary disease. N Engl J Med 2005;352:1425-1435.
26. Improved outcomes after acute coronary syndromes with an intensive versus standard lipid lowering regimen: Results from the pravastatin or atorvastatin evaluation and infection therapy-thrombolysis in myocardial infarction 22 trial (PROVE IT TIMI 22). Am J Med 2005;118:28-35.
27. Grundy SM, Cleeman JI, Merz CN, et al. Coordinating Committee of the National Cholesterol Education Program. Implications of recent trials for the National Cholesterol Education Program Adult Treatment Panel III Guidelines. Circulation 2004;110:227239.
28. American Diabetes Association. Dyslipidemia management in adults with diabetes. ADA 2004 Standards of Care. Diabetes Care 2004;27:S68-S71.
29. Neal RC. Lipid lowering: Can ezetimibe help close the treatment gap? Cleve Clin J Med 2003;70:777-783.
30. Ballantyne CM, O’Keefe JH, Gotto AM, Dyslipidemia Essentials. Physician’s Press 2005.
31. Rubins HB, Robins SJ, Collins D, et al. Gemfibrozil for the secondary prevention of coronary heart disease in men with low levels of HDL-C. Veterans Affairs High Density Lipoprotein Cholesterol Intervention Trial Study Group. N Engl J Med 1999;341:410-418.
32. Field Investigators. Effects of long term fenofibrate therapy on cardiovascular events in 9795 people with type 2 diabetes mellitus (FIELD study). Lancet 2005;366:1849-1861.
33. Ferguson EE Jr. Preventing, stopping or reversing coronary artery disease-triglyceride rich lipoproteins and associated lipoprotein and metabolic abnormalities: The need for recognition and treatment. Disease a Month 2000;46:421-503.
34. Manninen V, Elo MO, Frick MH, et al. Lipid alternations and decline in the incidence of coronary heart disease in the Helsinki Heart Study. JAMA 1988;260:641-651.
35. Kennedy AG, MacLean CD, Littenberg B, et al. The challenge of achieving national cholesterol goals in patients with diabetes. Diabetes Care 2005;28:1029-1034.
36. Dormandy JA, Charbonnel B, Eckland DJ, et al. Secondary prevention of macrovascular events in patients with type 2 diabetes in the PROactive study: A randomized control trial. Lancet 2005;366:1279-1289.
37. United Kingdom Prospective Diabetes Study UKPDS. Effect of intensive blood-glucose control with metformin on complications in overweight patients with type 2 diabetes (UKPDS 34). Lancet 1998;352:854-865.
38. Straton IM, Alder AI, Neil HA, et al. Association of glycemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35). Prospective observational study. BMJ 2000;321:405-412.
39. The DCCT/EDIC Study Research Group. Intensive Diabetes Treatment and Cardiovascular Disease in Patients with Type 1 Diabetes. N Engl J Med 2005;353:2643-2653.
40. Grant RW, Buse JB, Meigs JB. Quality of diabetes care in U.S. academic medical centers: Low rates of medical regimen change. Diabetes Care 2005;28:337-342.
41. Gaede P, Vedel P, Larsen N, et al. Mulitfactorial intervention and cardiovascular disease in patients with type 2 diabetes. The STENO -2 Study. N Engl J Med 2003;348:383-393.
42. Duckworth WC, McCarren M, Abraira C. Glucose control and cardiovascular complications: The VA Diabetes Trial. Diabetes Care 2001;24:942-945.
43. Combination Pharmacotherapy and Public Health Research Working Group. Combination pharmacotherapy for cardiovascular disease. Ann Intern Med 2005;143:593-599.
44. American Diabetes Association. Aspirin therapy in diabetes. 2004 Standards of Care. Diabetes Care 27:S73-S73.
45. Sacco M, Pellegrini F, Roncaglioni MC, et al. PPP Collaborative Group. Primary prevention of cardiovascular events with low-dose aspirin and vitamin E in type 2 diabetes patients. Diabetes Care 2003;26:3264-3272.
46. Ridker PM, Cook NR, Lee IM, et al. A randomized trial of low dose aspirin in the primary prevention of cardiovascular disease in women. N Engl J Med 2005;352:1293-1304.
47. Lauer M, Froelicher ES, Williams M, et al. Exercise testing in asymptomatic adults: A statement for professionals from the American Heart Association Council on Clinical Cardiology, Subcommittee on Exercise, Cardiac Rehabilitation and Prevention. Circulation 2005;112:771-776.
48. ADA Consensus development conference on the diagnosis of coronary heart disease in people with diabetes. Diabetes Care 1998;21:1551-1559.
49. Wacker FT, Young LH, Inzucchi SE, et al. Detection of Silent Myocardial Ischemia in Asymptomatic Diabetic Subjects (The DIAD study). Diabetes Care 2004;27:1954-1961.
50. Haffner SM, Stern MP, Hazuda HP, et al. Cardiovascular risk factors in confirmed pre-diabetic individuals. Does the clock start ticking for coronary heart disease before the onset of clinical diabetes? JAMA 1990;263:2893-2898.
Cardiovascular disease affects 25% of the U.S. population. It is responsible for more than 1 million deaths each year, which makes it the number one killer in the United States. Fifty percent of men and 64% of women who suffer from sudden cardiac death have no previous history or symptoms of heart disease.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.