Exercise During and After Cancer Treatment
Exercise During and After Cancer Treatment
By Dónal P. O'Mathúna, PhD, Dr. O'Mathúna is a lecturer in Health Care Ethics, School of Nursing, Dublin City University, Ireland; he reports no consultant, stockholder, speaker's bureau, research, or other financial relationships with companies having ties to this field of study.
About 10 million cancer survivors are living in the United States, with the numbers of long-term cancer survivors growing.1 All people diagnosed with cancer are considered cancer survivors for the rest of their lives.2 As cancer treatments become more successful physiologically, more attention is being given to patients' quality of life during and after treatment.
Various cancer treatments may have adverse effects that exercise could theoretically counteract, including pain, fatigue, impaired cardiorespiratory capacity, reduced quality of life, and suppressed immune function.1 Numerous controlled studies have examined the role of physical activity and exercise during and following cancer treatment, yet exercise is not generally incorporated into cancer care or discussed with cancer patients.3 Significant reductions in physical activity have also been observed in women diagnosed with breast cancer.4 The evidence regarding whether patients should be encouraged to exercise after being diagnosed with cancer will be reviewed here.
Background
One of the difficulties in reviewing this area of research is the range of variables introduced into clinical trials. Studies have involved patients with many different types of cancers, and the relevance of results from trials involving patients with one form of cancer for patients with other cancers is uncertain. Also, the studies have been conducted with patients at different stages of cancer. The impact of exercise on patients during chemotherapy may not be the same as when treatment is completed.
The Physical Exercise Across the Cancer Experience (PEACE) framework has been proposed to take account of such variation.5 This framework proposes six time periods related to cancer during which exercise could have different outcomes that should be considered in research and clinical guidance. Before diagnosis, exercise may have a role in general cancer prevention and then may impact the effectiveness of screening. The latter could occur directly by affecting the sensitivity and specificity of screening tests, or indirectly by reducing anxiety associated with testing and diagnosis. After cancer diagnosis, exercise may help patients build up their physical condition before treatment, and then may help them cope during treatment. Exercise may facilitate rehabilitation immediately after treatment and then have a role either in health promotion for those with positive treatment outcomes or in augmenting palliative care for those with negative treatment outcomes. All of these factors lead to complexity and variability in the designs of research studies and make general clinical recommendations difficult.
Mechanism of Impact
Exercise can counteract some of the symptoms of cancer and some of the adverse effects of treatment. These can include unintended loss or gain of body weight, loss of muscle mass, nausea, vomiting, and difficulties eating or digesting food.2 Mood changes, fatigue, and other psychological disturbances also can occur and may be amenable to treatment with appropriate exercise. Cancer or its treatment may require periods of rest or bed rest, which can result in reduced fitness, endurance, or muscle strength. At present, studies have not examined whether exercise impacts directly on the effectiveness of treatment regimens.2
Clinical Studies
More than 30 controlled clinical trials have been conducted with cancer patients in which one group was given an exercise intervention and compared to another group. Three systematic reviews of these studies have been published recently, all coming to the similar conclusion that exercise can be of benefit in specific clinical situations.1,3,6 The controlled trials have involved patients with a wide variety of cancers, the majority involving women with breast cancer.
The most recent general review included 32 controlled studies, of which 22 were rated as being of high methodological quality.1 Most studies included diagnostic and treatment data for only those who completed the trial, making it difficult to know which factors might influence people's adherence to the exercise regimens. In more than half of the studies, the exercise interventions were described incompletely to the extent that the reviewers did not think other researchers could replicate the studies. Most interventions involved moderate to vigorous aerobic activity for 20-30 minutes, 3-5 times per week. The interventions lasted between five and 12 weeks and were preplanned and usually supervised.
Of the included trials, approximately two-thirds studied the role of exercise concurrent with cancer treatment and one-third examined exercise immediately after treatment finished. The main findings were that physical activity has a moderately positive effect on cardiorespiratory fitness during and after treatment, and a small to moderate positive effect on various biomarker levels (e.g., interleukins, tumor necrosis factors, insulin, hemoglobin) and symptoms during treatment.
Fatigue is frequently reported by cancer patients, affecting more than half of all patients to a significant degree.3 The review unexpectedly found a lack of significant reduction in cancer-related fatigue during or after treatment or improvement in vigor during treatment. Earlier reviews had found benefit in these areas, but had also included results of several low-quality studies, which were excluded from this review.7 Exercise after treatment was found to have a moderate to large benefit on vigor and vitality.
A number of other outcomes were measured in different studies. The reviewers categorized the evidence for each of these into four types: that the evidence was insufficient, weak, strong, or showed exercise to be not effective. The Table (below) summarizes the reviewers' conclusions.
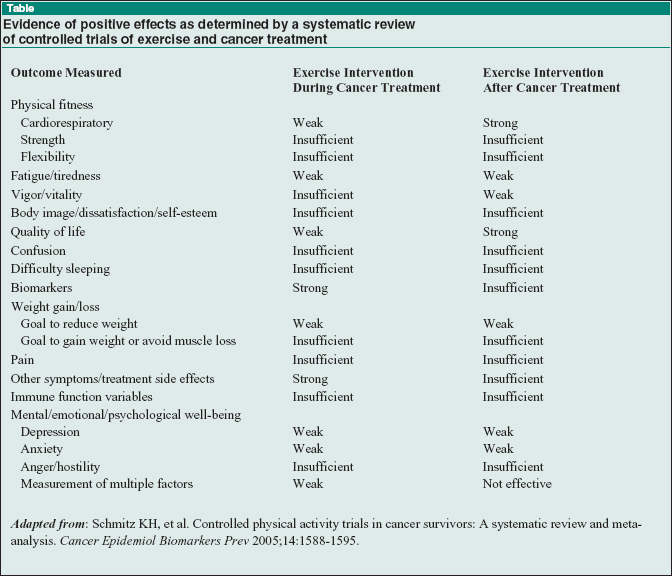 |
A Cochrane review of controlled trials of exercise while women were receiving treatment for breast cancer was published in October 2006.8 Nine intervention trials were included that assessed the effects of exercise together with various combinations of chemotherapy, radiation therapy, and hormonal therapy. Overall, small but statistically significant improvements were found for cardiorespiratory fitness, anxiety, sleep disturbance, and relief of nausea. No statistically significant differences were found for fatigue, quality of life, mood, depression, weight change, strength, or immune function. However, data on most outcomes could be extracted from only one trial, and most trials included a small number of participants.
Adverse Effects
In the 32 studies included in the above systematic review, 14 commented on adverse events.1 Of these, 12 found no harm resulting from exercise during or after treatment. In one study, one participant complained of nausea during one exercise session, with no further problems. In the other study, the rate of lymphedema in the exercise group was significantly higher than in the control group (the study involved women treated for breast cancer where the risk of lymphedema can be significant). In general, exercise does not appear to be contraindicated for most cancer patients. However, particular individuals may be at higher risk in specific circumstances. Thus, the American Cancer Society cautions that:2
- Cancer survivors with severe anemia should delay exercise until the anemia is improved.
- Cancer survivors with compromised immune function should avoid exercising in public until their white cell count returns to safe levels.
- Cancer survivors with severe fatigue should approach exercise cautiously.
- Cancer survivors undergoing radiation should avoid chlorinated swimming pools.
- Cancer survivors with catheters should avoid swimming.
- Cancer survivors with peripheral neuropathy or dizziness should engage in exercise that takes account of their restricted balance and coordination.
Exercise Protocols
Decisions about particular forms of exercise and when to initiate them should always be individualized. A person's level of exercise before diagnosis and treatment must be taken into account. In some cases, increased physical activity prior to surgery or radiation may have beneficial effects on recovery. For those exercising prior to diagnosis, maintaining exercise levels or returning to earlier levels should be the goal, where appropriate. For those who were not exercising before diagnosis, a program of low-intensity exercise that is tailored to the individual should be developed and gradually advanced. Account must be taken of other symptoms and conditions, along with patients' individual interests and enthusiasm for exercise. To develop and monitor individualized exercise programs, people should be referred to a physical therapist or personal trainer with expertise working with cancer survivors.
Conclusion
A growing number of small studies have shown that exercise can be beneficial for cancer patients during and after treatment. Cardiorespiratory fitness is improved, which should positively impact patients' daily activities. Improvements during treatment were also noted on biomarker levels and symptom management. After treatment was completed, improvements continued for fitness levels and for vigor and vitality. Exercise programs were tolerated well with few adverse events reported. However, many other exercise outcomes have been inadequately researched to allow evidence-based recommendations.
Recommendation
Cancer patients can be encouraged to continue or develop their physical activity levels during and after treatment. Exercise recommendations must be tailored to individual patients depending on their activity levels prior to diagnosis and other limitations imposed by their disease or treatment. Guidance should be sought from physical therapists or personal trainers with expertise working with people with cancer. Physical activity is connected to a number of physiological and psychological outcomes, which may prove beneficial to cancer survivors at different stages of their cancer experience. This complicates controlled studies of exercise in cancer patients.
Larger and better designed studies may reveal more specific guidelines for all cancer patients. After initial diagnosis and treatment of cancer, the American Cancer Society recommends that cancer survivors adopt an active lifestyle that includes at least moderate physical activity for 30 minutes on five or more days per week.2
References
1. Schmitz KH, et al. Controlled physical activity trials in cancer survivors: A systematic review and meta-analysis. Cancer Epidemiol Biomarkers Prev 2005;14:1588-1595.
2. Brown JK, et al. Nutrition and physical activity during and after cancer treatment: An American Cancer Society guide for informed choices. CA Cancer J Clin 2003;53:268-291.
3. Stevinson C, et al. Exercise interventions for cancer patients: Systematic review of controlled trials. Cancer Causes Control 2004;15:1035-1056.
4. Irwin ML, et al. Physical activity levels before and after a diagnosis of breast carcinoma: The Health, Eating, Activity, and Lifestyle (HEAL) study. Cancer 2003;97:1746-1757.
5. Courneya KS, Freidenreich CM. Framework PEACE: An organizational model for examining physical exercise across the cancer experience. Ann Behav Med 2001;23:263-272.
6. Knols R, et al. Physical exercise in cancer patients during and after medical treatment: A systematic review of randomized and controlled clinical trials. J Clin Oncol 2005:23:3830-3842.
7. Lucía A, et al. Cancer-related fatigue: Can exercise physiology assist oncologists? Lancet Oncol 2003;4:616-625.
8. Markes M, et al. Exercise for women receiving adjuvant therapy for breast cancer. Cochrane Database Syst Rev 2006;(4):CD005001.
MD Anderson to Study Effects of Tibetan Yoga on Women With Breast Cancer
Researchers at the university of texas md anderson Cancer Center in Houston have received a $2.4 million grant from the National Cancer Institute to study the effects of Tibetan yoga in women with breast cancer who are undergoing chemotherapy.
The award is the largest ever made to study Tibetan yoga in cancer patients, say the researchers, who published a 2004 study in Cancer that found the practice led to significant sleep improvements in patients with lymphoma. Another small study of Tibetan yoga also found improvements in cancer-related symptoms and intrusive thoughts in women with breast cancer.
With this grant support, the research team will randomly assign women with breast cancer who are scheduled to undergo chemotherapy to either a Tibetan yoga group, a control group that does simple stretching, or to a group that receives standard care. The participants will practice their assigned techniques for seven weeks during chemotherapy, and then will have five booster sessions over the next six months.
The study will assess the physical and psychological benefits of the yoga program, and will specifically examine such patient lifestyle factors as fatigue and sleep, mental health, and distress. Additionally, the study will evaluate cognitive and emotional processing, social networking and interactions, coping, and other psychosocial factors, the researchers say.
O'Mathuna DP. Exercise during and after cancer treatment. Altern Med Alert 2006;9(12):137-140.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
