ECG Review: A History of "Falling Out"
ECG Review
A History of "Falling Out"
By Ken Grauer, MD Dr Grauer is Professor and Associate Director, Family Practice Residency Program, College of Medicine, University of Florida, Gainesville. Dr. Grauer is sole proprietor of KG/EKG Press.
|
|
|
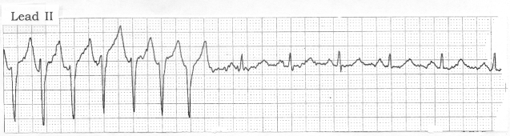
Figure: Rhythm strip recorded on telemetry from a 70-year-old woman admitted to the hospital for episodes of "falling out." |
Clinical scenario: The rhythm in the Figure was obtained from a 70-year-old woman who was admitted to the hospital with a history of "falling out" on several occasions during the week prior to admission. Her initial 12-lead electrocardiogram (ECG) was unremarkable, and acute serum markers were negative for recent infarction. Telemetry monitoring was described as "unremarkable," except for the tracing shown in the Figure. This rhythm strip was interpreted as sinus rhythm with a brief run of "SVT." Your thoughts on the case?
Interpretation: It is difficult to determine from the history provided what may have occurred. The patient's description of "falling out" on several occasions during the week prior to admission could represent a variety of benign phenomena, or could reflect true syncope from a recurrent and serious cardiac arrhythmia. Potentially life-threatening arrhythmias may occur without associated acute infarction and on an infrequent, intermittent basis. Documentation by telemetry monitoring in such cases may be unrevealing because no abnormalities may be seen over an extended period of time. That condition could be what is happening for this patient.
In view of the history given for this case, the rhythm strip shown in the Figure is worrisome. Baseline artifact is present, accounting for undulation in the baseline that distorts ST segments and alters P-wave morphology. Nevertheless, it seems clear that the underlying rhythm is sinus, as evidenced by regular occurrence of narrow QRS complexes at a rate of 80/minute for the last six beats on the tracing. Each of these beats is preceded by an upright P wave, albeit the artifact slightly changes the P wave appearance. The QRS complex looks very different for the first seven beats on the tracing. Although the rS complex for these seven beats does not appear to be widened, one cannot be sure where the QRS begins and ends from this single monitoring lead. The rhythm is fairly regular at a rate of about 150/minute, and no definite atrial activity is seen; it has to be assumed to be ventricular tachycardia (VT) until proven otherwise.
Unfortunately, the beginning of the run of abnormal beats is cut off, such that one has no idea of the duration of the episode. Further evaluation of the tachycardia (e.g., thyroid function studies, serum electrolytes levels measurement, oxygenation status study, and history of potentially causative drugs) is warranted. If no obvious precipitating cause is found however, the occurrence of the arrhythmia seen here in a patient with a history of "falling out" may warrant electrophysiologic study with consideration of an implantable cardioverter-defibrillator (ICD).
The rhythm in the Figure was obtained from a 70-year-old woman who was admitted to the hospital with a history of "falling out" on several occasions during the week prior to admission. Her initial 12-lead electrocardiogram (ECG) was unremarkable, and acute serum markers were negative for recent infarction.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.