Now How Much Vitamin D and Calcium Should We Take?
Now How Much Vitamin D and Calcium Should We Take?
Abstract & Commentary
By David Kiefer, MD. Dr. Kiefer is Clinical Instructor, Family Medicine, University of Washington, Seattle; Clinical Assistant Professor of Medicine, University of Arizona, Tuscon; Adjunct Faculty, Bastyr University, Seattle; he reports no financial relationships to this field of study.
Source: Ross AC, et al. The 2011 Report on Dietary Reference Intakes for Calcium and Vitamin D from the Institute of Medicine: What Clinicians Need to Know. J Clin Endocrinol Metab 2011;96:53-58.
Synopsis: An evaluation of medical research by the IOM establishes new RDAs for vitamin D (600-800 IU) and calcium (700-1300 milligrams).
The year 2010 ends with a re-visitation of two "hot" supplements, calcium and vitamin D, this time by the venerable Institute of Medicine (IOM). The IOM committee assigned to this task consisted of 14 scientists who met eight times, collecting input also from public meetings and from "stakeholders" via the internet. The committee conducted a literature review to augment two recent reviews (2007 and 2009) on calcium and vitamin D by the Agency for Healthcare Research and Quality. The committee reviewed evidence of both the skeletal and "extraskeletal" effects of these two nutrients, updating its recommendations from the prior 1997 report. Overall, they were convinced of a cause-effect connection between both vitamin D and calcium and bone health, leading them to establish Recommended Daily Allowances (RDA) for calcium of 700-1,300 milligrams daily and vitamin D of 600-800 International Units (IU) daily (see Table 1). These values are different for some of the age groups compared to the 1997 analysis. The IOM was less impressed by the data for non-bone related conditions, and did not factor that evidence into the dosage ranges listed.
Table 1: IOM RDA for Calcium (mg) and Vitamin D (IU) using bone health as an indicator, 1997 vs. 2010(Changes in Bold)
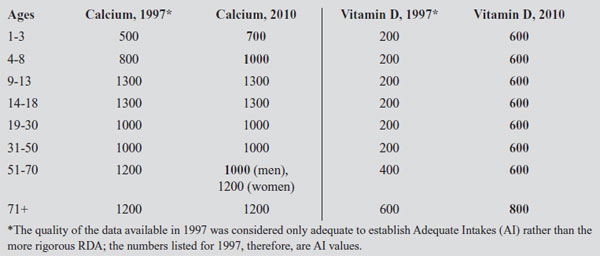
Source: Ross AC, et al. The 2011 Report on Dietary Reference Intakes for Calcium and Vitamin D from the Institute of Medicine: What Clinicians Need to Know. J Clin Endocrinol Metab 2011;96:53-58.
There are several characteristics of the IOM approach that will help to understand these recommendations and put them into context with other research results. First of all, a very important part of this analysis is that it was done in the context of the average "normal" person, that is, for people who don't have specific disease states. In addition, the vitamin D intake recommendations were set assuming little to no sun exposure, aiming to help 97.5% of the population (the definition of RDA) achieve a serum 25-hydroxyvitamin D (25(OH)D) of 20 ng/mL. The sun exposure variable was removed to avoid the unknowns regarding the effects of sunblock use, latitude, skin pigmentation, genetic factors, and extent of outdoor activity.
The IOM called the evidence inconsistent, inconclusive to causality, and insufficient to serve for establishment of dosages for cardiovascular disease, cancer, diabetes, falls, autoimmune disorders, and other chronic diseases. The IOM found some "U-shaped" effects for vitamin D, meaning that there might be increased risk at low and high dose ranges, and the lowest risk in moderate dose range for some medical conditions (all-cause mortality, cardiovascular disease, some cancers, falls, and fractures), leading to continued use of the Upper Limit (UL) values above which increased risk of adverse effects may exist. The actual 2011 UL values are different than in 1997; calcium's had been 2,500 milligrams daily, and is now 1,000-3,000 milligrams daily, depending on age, and the vitamin D UL increased from 2,000 IU to 4,000 IU for most age groups. The vitamin D UL was set lower than the 10,000 IU limit of toxicity due to possible adverse effects with longer term chronic administration (as opposed to acute toxicity) and the committee's stated concerns about serum 25(OH)D levels above 50 ng/mL.
The IOM pointed out the need for further research, especially in the area of laboratory parameters to establish safe high and low ranges, and concluded that the well-publicized "epidemic" of hypovitaminosis D was overestimated.
Although the IOM committee commented on serum 25(OH)D levels, it also stated that an in-depth review of this topic was beyond the scope of the report. As much as it recognized that 25(OH)D levels do represent vitamin D intake and sun exposure, the committee was less impressed by the evidence for 25(OH)D levels and connection to certain disease states, or lack of same. The committee states that 25(OH)D of 20 ng/mL covers the requirements of 97.5% of the population, and that the effects of chronically high serum levels (for example, 50 ng/mL) remain unproven, mandating a certain "margin of safety for public health."
Putting the recommendations in the context of dietary intake, the committee referred to nutritional research finding that most of the population meets basic calcium needs and vitamin D intake requirements to reach serum 25(OH)D of 20 ng/mL. The notable exceptions are girls aged 9-18 years because of their high calcium intake needs, and people with poor nutrition, in institutions, or those with dark skin pigmentation who might not reach sufficient serum vitamin D levels.
Commentary
When the IOM report was released, it sent waves of disbelief among many clinicians and researchers, especially due to the very conservative vitamin D dosing recommendations. Their serum 25(OH)D of 20 ng/mL cutoff for adequacy seems woefully low. Many studies on falls or fractures failed to find a benefit below 25-30 ng/mL,2 and some preliminary data on vitamin D and treatment of upper respiratory infections found thresholds of 30 ng/mL, above which there was benefit and below which no effect. Also, while serum 25(OH)D < 20 ng/mL is recognized as vitamin D deficiency, some data are accumulating that 20-29 ng/mL may be a relative vitamin D insufficiency, making 30 ng/mL and above close to optimal1; this would all make the IOM target less than ideal. With respect to vitamin D dosing, 600-800 IU seems very low, especially given that most experts are recommending 800-1,000 IU daily at the minimum for maintenance, with higher doses in high-risk groups or to correct vitamin D deficiency or insufficiency.1,2
The IOM report also seemed to overstate the vitamin D safety concerns. One expert continues to postulate the safety of 10,000 IU vitamin D daily, and the problems with vitamin D use in people with granulomatous disorders and lymphomas when serum 25(OH)D rises above 30 ng/mL could be avoided simply with lower (400 IU) daily vitamin D dosing in those groups without applying such conservative dosing recommendations to the population as a whole.1
In addition, there are issues regarding how applicable these recommendations are to real clinical situations involving real patients. Excluding the involvement of sun is probably an important research approach, but one that baffles physicians actually treating patients, few of whom would fall into such a limited category. In addition, the IOM focused on "normal" patients, or ones without relevant medical conditions. This is in contrast to many of the published research trials examining calcium, vitamin D, or both for the treatment or prevention of various diseases in specific populations. Therefore, the IOM recommendations may simply be different from other results in the medical literature for this reason.
With respect to calcium, the new IOM recommendations are mostly unchanged from the 1997 levels, with only three modifications (See Table 1). Compared to other expert groups and reviews, such as the NIH Consensus Statement from 1994, the new recommendations remain lower.3 Are these new doses still too low? Is this conservative approach warranted due to some of the known adverse effects with calcium intake? The medical literature continues to evolve in its pursuit of answers to these questions. For example, it is unclear whether the IOM Committee addressed recent concerns, albeit controversial, over the possible extra risk of cardiovascular events with calcium supplementation,4 or the possible connection with prostate cancer risk, as previously addressed in Alternative Medicine Alert.5 On the flip side, the positive effects of calcium supplementation on prevention of bone loss and osteoporosis occur in the range of 1,000-1,200 milligrams daily,6 and are adequately covered in the 2011 IOM report.
Overall, the IOM committee members failed to jump on the vitamin D bandwagon in its 2011 reassessment, setting a low-bar public health interventional strategy, and leaving physicians and patients alike without the official "OK" in repletion attempts. Closely paying attention to upcoming research trials will probably be the better course of action for clinical guidance. Calcium, in its own rite, is a mineral with a complicated history, still evolving in some respects (i.e., recent cardiovascular risks) but mostly unchanged in this current report; most health care practitioners continue to recommend calcium supplementation up to but not exceeding RDA levels for women in all age groups, paying particular attention to calcium dosing in girls ages 9-18.
References
1. Vieth R. Vitamin D supplementation, 25-hydroxyvitamin D concentrations, and safety. Am J Clin Nutr 1999;69:842-856.
2. Holick MF. Vitamin D deficiency. N Engl J Med 2007;357:266-281.
3. Optimal Calcium Intake. NIH Consensus Statement. 1994;12:1-31.
4. Bolland MJ. Effect of calcium supplements on risk of myocardial infarction and cardiovascular events: Meta-analysis. BMJ 2010;341:c3691.
5. Kiefer D. Guys need strong bones too: Calcium is not just for women anymore. Altern Med Alert 2009;12:25-27.
6. Shea B, et al. Calcium supplementation on bone loss in postmenopausal women (Cochrane Review). Cochrane Database Syst Rev 2004:CD004526. Cochrane Library Issue 3, 2004. Chichester, UK: John Wiley & Sons.
An evaluation of medical research by the IOM establishes new RDAs for vitamin D (600-800 IU) and calcium (700-1300 milligrams).Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
