Emergency Department Evaluation of Stroke and TIA: Beyond the CT Scan: Part I
Emergency Department Evaluation of Stroke and TIA: Beyond the CT Scan: Part I
Authors:
Bentley J. Bobrow, MD, Clinical Associate Professor, Department of Emergency Medicine, Maricopa Medical Center, Phoenix, AZ; Medical Director, Bureau of EMS and Trauma System, Arizona Department of Health Services, Phoenix.
Shadi Rafael, Medical Student, University of Arizona College of Medicine, Tucson.
Peer Reviewer:
Joseph Shiber, MD, FACP, FACEP, Associate Professor, University of Florida, Jacksonville.
This issue of Emergency Medicine Reports is the first in a two-part series on imaging and evaluation of stroke and transient ischemic attack (TIA). This part will review risk factors, history and physical examination, and computed tomography imaging. Part 2 will review magnetic resonance imaging, duplex ultrasound imaging, and treatment.
Case Presentation
A 45-year-old African American female with a history of hypertension presents to the emergency department (ED) with chief complaints of right-sided headache, partial loss of vision, and feeling dizzy. Her symptoms began 3 hours prior to arrival to the hospital and have not changed in severity. She has had previous headache episodes accompanied by blurry vision, but has never been diagnosed with a migraine headache. Her surgical history is positive for cholecystectomy and mitral valve replacement secondary to rheumatic heart disease. She has a 30 pack-year history of smoking, and her family history is positive for migraine. Pertinent positive findings on physical examination include blood pressure of 170/100, right-sided homonymous hemianopsia, and gait ataxia (NIH Stroke Scale = 4).
An initial non-contrast computed tomography (CT) scan of the brain is obtained, which is normal. The patient continues to complain of dizziness and vision impairment. The decision is made to obtain a magnetic resonance imaging (MRI) scan of the brain, including T1, T2, diffusion-weighted imaging (DWI), and perfusion-weighted imaging (PWI) sequences along with magnetic resonance angiography (MRA). DWI-MRI shows an area of posterior cerebral infarct with diffusion/perfusion mismatch. An occlusion in the left PCA is visualized on MRA. The stroke team is consulted. The stroke team is consulted. The patient is informed regarding possible risks and benefits of thrombolysis treatment and, after obtaining consent, intravenous rtPA administration is started 4 hours after symptom onset. The patient is subsequently transferred to the stroke unit for monitoring and management, where she regains complete neurological function without any treatment complications.
Introduction
Stroke remains the third leading cause of death worldwide, with an annual incidence of 795,000 in the United States.1 Death within 30 days of stroke has been reported as 12.6% for all types of stroke (ischemic and hemorrhagic) in individuals older than 65 years of age.1 Additionally, survival from stroke results in some degree of disability in one-third of patients, with at least 15% suffering serious, long-term disability.1 In 2009, the direct and indirect cost of stroke in the United States was estimated at $68.9 billion, and this figure is estimated to increase as the population of baby boomers ages and the incidence of chronic illnesses increases.2
The ED evaluation for stroke is particularly challenging due to the wide range of clinical presentations, the presence of various stroke mimics, and evolving diagnostic and therapeutic guidelines. Historically, CT imaging of the brain has been the primary imaging technique used to assess ED patients for acute cerebrovascular disease. Newer imaging techniques have been developed in the past decade, allowing for earlier, more sensitive, and more accurate detection of stroke. The goal of these imaging modalities is the identification of all patients eligible for early treatments aimed at rapidly restoring cerebral blood flow. It is useful for emergency physicians (EPs) to understand the utility of these new imaging techniques and integrate them efficiently into their practice to optimize stroke and transient ischemic attack (TIA) outcomes.
This review article focuses on the pathophysiology, risk factors, ED diagnosis, and acute treatment of stroke and TIA, with special emphasis on new and evolving imaging techniques to improve early detection and outcomes from acute cerebrovascular events.
Definitions
Stroke is defined as a loss in neurological function secondary to a focal or global loss of perfusion of the brain, leading to permanent injury to cerebral tissue. Stroke is classified as either ischemic or hemorrhagic. Ischemic stroke is a result of reduced blood flow in a vessel supplying the brain, while hemorrhagic stroke is due to the rupture of a cerebral vessel with blood accumulating in the brain parenchyma (intracerebral hemorrhage) or around the brain (subarachnoid hemorrhage). In general, ischemic strokes comprise approximately 87% of all strokes, while roughly 10% of strokes are due to intracerebral hemorrhage (ICH), and 3% are secondary to subarachnoid hemorrhage (SAH).1 A more recent analysis, however, estimates the incidence of hemorrhagic stroke to be as high as 42% with the use of more sensitive imaging techniques and also as a consequence of the greater use of anticoagulant and antiplatelet agents in the general population.3
Even though SAH is considered a type of stroke, it will not be discussed in detail in this review article since SAH varies noticeably from other types of stroke and deserves a separate discussion.
On the same spectrum of disease as stroke, TIA was traditionally defined as a transient loss of neurological function lasting less than 24 hours and brought about by a temporary decrease in brain perfusion. The 24-hour threshold was an arbitrary one, developed under the assumption that symptoms lasting less than the indicated time are a reflection of uninjured brain tissue. With the advent of newer imaging technologies, however, it has become evident that one-third of ischemic episodes labeled as TIAs based on the traditional definition are associated with tissue infarction on diffusion-weighted MRI.4 As a consequence, in 2002, a new definition of TIA was proposed with a biologic end point (tissue injury) rather than a time limit of 24 hours.5 The American Stroke Association (ASA) adopted a revised version of the proposed definition, which is now widely accepted as the new definition of TIA: "a transient episode of neurological dysfunction caused by focal brain, spinal cord, or retinal ischemia, without acute infarction."4 According to various studies, the majority of TIA episodes (60%) last less than one hour, and longer symptom duration is typically associated with greater chance of infarction;4 this relationship, however, is not absolute.
Pathophysiology
Cerebrovascular disease can result from a variety of pathophysiologic processes at various locations in the body, with the universal outcome of insufficient oxygen and glucose delivery to some part of the brain. (See Table 1.) The process may originate in an intracerebral or extracerebral vessel (e.g., atherosclerosis, arterial dissection, aneurysmal rupture, etc.); the pathology could develop in a remote location with migration to the brain (e.g., cardiac or arterial embolus); or, alternatively, a systemic process can have a secondary negative effect on cerebral perfusion (e.g., cardiac pump failure, pulmonary embolism, sickle cell disease, etc.).
Table 1: Most Common Causes of Stroke and TIA
|
TIA and Ischemic Stroke |
Hemorrhagic Stroke |
|
|
The principal mechanism of injury in ischemic stroke is reduced cerebral blood flow. In hemorrhagic stroke, in addition to reduced blood flow distal to the site of hemorrhage, the formation of a local hematoma also results in local toxic effects and a global increase in intracranial pressure (thus further reducing blood flow and increasing ischemia). Neurological signs and symptoms that appear during an episode of stroke or TIA are a direct result of the above processes.
In a zone of hypoperfused brain tissue, energy metabolism is disrupted and anaerobic metabolism leads to the accumulation of lactic acid, free-radical production, cell injury, cellular edema, and, eventually, cell death. Tissue perfusion is variable in an ischemic zone and correlates to the distance from the blood source. Additionally, brain cells in different ischemic zones may be in various stages of the injury process, and some cells may even be salvaged if cerebral perfusion is re-established. This notion of salvageable brain tissue has led to the emerging concept of ischemic penumbra, describing ischemic tissue that is either uninjured or has only acquired reversible changes. The accurate recognition of this evolving zone of brain tissue is the goal of many new imaging techniques, and acute treatments are aimed at recovering cellular function in the penumbra.6
Risk Factors
Risk factors for stroke can be divided into two categories: modifiable and non-modifiable. (See Table 2.) Primary and secondary prevention of stroke is aimed at reducing an individual's modifiable risk factors.
Table 2: Risk Factors for Stroke
|
Modifiable Risk Factors |
Non-modifiable Risk Factors |
|
|
Some important risk factors include:
Age is by far the greatest risk factor for stroke, with a doubling of risk per decade after the age of 55.2
Hypertension significantly increases the risk of stroke, with a doubling of risk for each 10 mmHg increase in systolic BP or 5 mmHg increase in diastolic BP.7
The risk of stroke is greater for men and postmenopausal women in comparison to premenopausal women.2
African Americans and Hispanic individuals possess a greater risk of stroke than members of other races or ethnic groups.2
Cardiac disease may lead to such phenomena as embolic strokes and systemic hypoperfusion. Atrial fibrillation confers the greatest risk in this category, with a 5-fold increased risk of stroke.2
A former episode of TIA increases the risk of stroke up to 17% in the 90 days following the event and imparts an 18.8% risk of stroke in the subsequent 10 years.2
Differential Diagnosis
While assessing a patient for acute stroke in the ED, it is important to also consider other clinical entities that can act as "stroke mimics." These non-stroke conditions may also present with acute neurological signs and symptoms. (See Table 3.) In a study by Libman et al, among 411 patients evaluated for stroke in the ED, 19% were found to have a stroke mimic, most commonly postictal states, systemic infections, tumors, or toxic-metabolic disturbances.8 Migraine and conversion reactions are other common stroke mimics that can be associated with localizing neurological symptoms.8,9
Table 3: Most Common Stroke Mimics
- Seizure or postictal state
- Toxic-metabolic disturbances
- Intracranial malignancy
- Brain abscess
- Migraine
- Systemic infection
- Meningitis/encephalitis
- Subdural hematoma
- Conversion reaction
The history and physical exam are key to distinguishing between acute stroke and the stroke mimic conditions. Laboratory tests and imaging studies, which will be discussed in greater detail in the evaluation section, can also help discern the cause of a patient's acute neurologic symptoms.
Diagnosis of Stroke and TIA in the ED
The initial evaluation of suspected stroke or TIA consists of first ensuring medical stability of the patient and then concurrently obtaining a thorough history, performing a detailed physical examination, ordering laboratory studies, and obtaining appropriate brain and cerebrovascular imaging studies. Further testing, such as a toxicology screen or a lumbar puncture, may be indicated in selected patients to rule out possible stroke mimics. The decision to perform a lumbar puncture should be made carefully since the patient will no longer be eligible for receiving tissue plasminogen activator (tPA) after having undergone this procedure.
The recommended approach to the evaluation and management of patients suspected of having suffered an acute stroke were outlined in the 2010 American Heart Association (AHA) "Guidelines for Cardiopulmonary Resuscitation (CPR) and Emergency Cardiovascular Care (ECC)"(see Table 4).10 Stroke protocols help standardize the assessment and management of stroke patients and minimize delays in diagnosis and initiation of therapy.10 Hospitals are encouraged to devise and utilize personalized stroke protocols tailored to available resources at that specific clinical center. The development of such protocols should be a collaborative effort among EPs, neurologists, and neuroradiologists at each hospital.
Table 4: American Heart Association Goals of Ischemic Stroke Management
|
Source: 2010 AHA Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010;122:S818-S828. |
|
|
Time |
Activity |
|
Identify symptoms or signs of possible stroke Activate emergency response |
|
|
EMS response and critical actions
|
|
|
0-10 minutes |
ED Arrival
|
|
10-25 minutes |
Neurologic assessment by Stroke Team or designee
|
|
25-45 minutes |
Obtain CT or MRI interpretation
|
|
45-60 minutes |
CT scan or MRI does not show hemorrhage
|
|
Patient remains candidate for fibrinolytic therapy
|
|
|
1-3 hours |
Post-rtPA (alteplase) stroke pathway
|
Airway, Breathing, and Circulation (ABC)
The initial assessment of a patient with neurological complaints begins with a primary evaluation of the patient's airway, breathing, and circulation. Advanced airway placement may be necessary in patients who are not protecting their airways, have persistent hypoxia despite supplemental oxygen, or those without adequate ventilatory drive. Oxygen saturation should be continuously monitored and supplemental oxygen provided if patients become hypoxic (oxygen saturation < 94%).10 Supplemental oxygen is currently not recommended in non-hypoxic patients.11 Additionally, cardiac auscultation and checking peripheral pulses allows for a rapid evaluation of the circulation.
History and Physical Examination
The history and physical examination are important components of the initial evaluation, which will guide further testing, diagnosis, and therapeutic interventions. Many of the stroke mimics previously mentioned can be distinguished on the basis of history. Patients should be asked about risk factors for atherosclerosis and stroke. Since the administration of tPA in ischemic stroke is a time-sensitive intervention, it is imperative to note the time of onset of symptoms. If the onset of symptoms is not witnessed (e.g., patient awakens with neurological symptoms), it is important to determine when the patient was last known to be normal. In circumstances where patients are unsure about the precise time of symptom onset, interviewing available family and friends can be very helpful.
After the primary assessment, a complete physical examination should be performed. This includes a thorough examination of the patient's head, neck, heart, lungs, abdomen, skin, and extremities. A neurological examination should assess the patient's mental status, cranial nerves, motor function, sensory and speech capability, as well as cerebellar function. Focal neurological signs or a constellation of certain neurological signs can point to the location of the pathologic process in the brain.
The National Institutes of Health Stroke Scale (NIHSS) should be utilized as a standardized method of assessing a patient's level of neurological impairment. (See Table 5.) The NIHSS was developed in 1983 as part of the original tPA trial conducted by the National Institute of Neurological Disorders and Stroke to systematically determine eligibility for intravenous thrombolysis and measure response to tPA treatment.12 Over the years, NIHSS has been validated as an accurate and reliable method of defining stroke severity and measuring effects of interventions.13-15 Points are awarded for impairments detected during the examination. The level of stroke severity is then determined using the following scoring system:
Table 5: Abbreviated Version of National Institutes of Health Stroke Scale
|
Tested Item |
Responses and Scores |
|
* The full scale with complete instructions can be found at www.strokecenter.org |
|
|
Level of Consciousness |
0alert 1drowsy 2obtunded 3coma/unresponsive |
|
Orientation Questions (2) |
0answers both correctly 1answers one correctly 2answers neither correctly |
|
Response to Commands (2) |
0performs both tasks correctly 1performs one task correctly 2performs neither |
|
Gaze |
0normal horizontal movements 1partial gaze palsy 2complete gaze palsy |
|
Visual Fields |
0no visual field defect 1partial hemianopsia 2complete hemianopsia 3bilateral hemianopsia |
|
Facial Movement |
0normal 1minor facial weakness 2partial facial weakness 3complete unilateral palsy |
|
Motor Function (Arm) a. right b. left |
0no drift 1drift before 5 seconds 2falls before 10 seconds 3no effort against gravity 4no movement |
|
Motor Function (Leg) a. right b. left |
0no drift 1drift before 5 seconds 2falls before 5 seconds 3no effort against gravity 4no movement |
|
Limb Ataxia |
0no ataxia 1ataxia in 1 limb 2ataxia in 2 limbs |
|
Sensory |
0no sensory loss 1mild sensory loss 2severe sensory loss |
|
Language |
0normal 1mild aphasia 2severe aphasia 3mute or global aphasia |
|
Articulation |
0normal 1mild dysarthria 2severe dysarthria |
|
Extinction or Inattention |
0absent 1mild (loss 1 sensory modality) 2severe (loss 2 modalities) |
1-4 = minor stroke
5-14 = moderate stroke
15-20 = moderate/severe stroke
21-42 = severe stroke.
Laboratory Studies
The following laboratory studies are recommended in the evaluation of all patients for stroke:
Finger-stick blood glucose, followed by serum glucose
Complete blood count
Electrolytes, urea nitrogen, creatinine
Prothrombin time (PT) and international normalized ratio (INR)
Partial thromboplastin time (PTT)
12-lead electrocardiogram (ECG)
Cardiac markers.
Other laboratory tests may be obtained in selected patients:
Liver function tests (LFTs)
Toxicology screen
Blood alcohol level
Pregnancy test in women of child-bearing potential
Arterial blood gas if hypoxia is suspected
Type and cross blood if fresh frozen plasma (FFP) is needed to reverse a coagulopathy
Lumbar puncture if central nervous system infections is suspected
Electroencephalogram (EEG) if seizures are suspected
Chest radiograph, urinalysis, and blood cultures if fever is present.
General assessment and stabilization (including airway, breathing, and circulation, history, physical examination, and basic laboratory tests) should be accomplished within 10 minutes of the patient's arrival to the hospital according to AHA guidelines.
Imaging
Numerous options are now available for imaging cerebral parenchyma and vasculature. Modern imaging techniques, beyond a non-contrast CT scan (NCCT), allow for more accurate assessment of brain tissue and vascular lesions and can identify patients who may benefit from various medical and mechanical treatment modalities. Patients suspected of having suffered from either an acute stroke or a TIA should undergo immediate neuroimaging in the ED. While different advanced imaging techniques will be discussed below, it is imperative that advanced imaging not delay the initiation of intravenous thrombolysis in eligible patients.
The ASA notes that neuroimaging should address four essential issues:
"(1) The presence of hemorrhage;
(2) The presence of an intravascular thrombus that can be treated with thrombolysis or thrombectomy;
(3) The presence and size of a core of irreversibly infarcted tissue; and
(4) The presence of hypoperfused tissue at risk for subsequent infarction unless adequate perfusion is restored."11
These issues govern treatment and management decisions, and better imaging techniques lead to higher detection rates. The detection of hemorrhage on imaging has perhaps the greatest influence on patient management decisions and helps avoid potential treatment complications with the administration of tPA. Vascular imaging techniques are necessary to localize the site of vascular occlusion and determine the appropriate type of acute therapy (intravenous vs. intra-arterial vs. mechanical thrombectomy). The efficacy of thrombolysis and thrombectomy techniques varies with the site of the occlusion.16 Finally, identifying reversible ischemia (physiological penumbra) allows for appropriate selection of patients for reperfusion therapy, while the volume of the initial core of infarction also appears to have prognostic value.17
There are many factors to consider in choosing which imaging techniques to utilize in assessing patients with neurological symptoms in the ED. Some of these considerations include the differential diagnosis of the patient, availability and sensitivity of the technique, time required to obtain imaging, availability of experts to perform and interpret the exams, cost, and patient stability and need for monitoring. The following section will review the value and indications of use for each of the currently available cerebral parenchymal and vascular imaging techniques.
Non-Contrast Computed Tomography (NCCT). Since its introduction in the early 1970s as the first imaging modality to view the brain in two-dimensional slices, CT technology has become the central imaging tool to screen patients for acute stroke due to its capability in detection of hemorrhage, ischemia, and stroke mimics, as well as its widespread availability, speed of imaging, ease of patient monitoring, and relatively low cost. Nearly all hospital protocols and national guidelines were initially developed around the use of CT as the primary technique in evaluation of acute stroke. The 2010 AHA guidelines for CPR and ECC recommend that, at minimum, an NCCT scan of the brain be obtained within 25 minutes of the patient's arrival in the ED and interpreted within 45 minutes of arrival.10 More advanced imaging techniques may be utilized if they can be obtained within this same time frame.
EP assessment of the NCCT of the brain prior to an official reading by a radiologist is reasonably reliable and comparable to specialists.18 EPs are able to interpret brain CTs with an accuracy rate of 67% (in comparison to an accuracy rate of 83% for neurologists and radiologists), and EPs can also detect hemorrhage correctly on 73% of scans (compared to an overall sensitivity of 82% in this area).18 Furthermore, teaching interventions were shown to improve skills in reading cranial CTs in emergency medicine residents from a baseline accuracy rate of 59% to 76%.19
For the detection of acute hemorrhage, NCCT is highly sensitive based on various case studies, practical experience, and consensus of experts.11 Since the gold standard for detection of ICH or SAH is surgery or autopsy, the true sensitivity of NCCT for detection of acute hemorrhagic stroke is unknown. Figure 1 demonstrates the appearance of ICH and SAH on NCCT of the head.
Figure 1: CT of Subarachnoid Hemorrhage
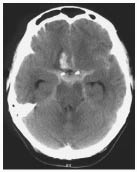
This patient, who had a long-standing history of smoking and hypertension, presented to the emergency department with severe headache with nausea and vomiting for four hours and had meningismus on physical examination. Initial CT of the head revealed a subarachnoid hemorrhage, a right frontal hematoma suggestive of an anterior communicating artery aneurysm, and hydrocephalus.
Reprinted with permission from: Suarez JI, Tarr RW, Selman WR. Aneurysmal subarachnoid hemorrhage. N Engl J Med 2006;354:387-396. Copyright © Massachusetts Medical Society. All rights reserved.
While recognizing hemorrhage is the essential first step in the evaluation of the NCCT of the head, the ECASS trial demonstrated that recognizing early CT signs of cerebral infarction (e.g., edema, loss of the insular ribbon, sulcal effacement, and mass effect) is also important, since their presence implies an increased risk for intracerebral hemorrhage in stroke patients who receive thrombolytic therapy.20-22 In detecting ischemic changes, the sensitivity of NCCT increases with time. Ischemic changes may not appear in the first few hours on NCCT, even on third- or fourth-generation scanners. For images obtained within 3 hours of symptom onset, the detection rate for ischemia is less than 67%.18,23-25 This rate, however, increases to 82% at 6 hours.26 Ischemia in the posterior fossa, notably, is difficult to detect at any time on NCCT due to limited resolution and the presence of artifact from the surrounding bone.27
Loss of gray-white differentiation (see Figure 2) is typically the earliest sign of ischemia on CT. Since the rate of metabolic activity is greater in gray matter, edema accumulates in this region at a faster rate with the onset of ischemia. Fluid increases the density of gray matter on CT and results in the merging of gray matter into white matter. Subtle edema may be noted as early as 46 minutes after the initiation of ischemia, but findings this early are rare. Seventy-five percent of patients show signs of edema on NCCT in the insular cortex by 6 hours.28-30 Within 12 hours, the lesion becomes even more prominent. Early in the process, however, it is virtually impossible to distinguish ischemia from infarction on NCCT.
Figure 2: Unenhanced CT Scan
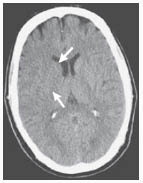
An unenhanced CT scan shows a slight loss of differentiation of gray and white matter in the basal ganglia (arrows). The scan was obtained 1 hour 40 minutes after the onset of symptoms suggestive of cortical stroke in the territory of the right middle cerebral artery.
Reprinted with permission from: van der Worp HB, van Gijn J. Acute ischemic stroke. N Engl J Med 2007;357:572-579. Copyright © Massachusetts Medical Society. All rights reserved.
Loss of gray-white differentiation when manifested in the insula results in the loss of the insular ribbon and is referred to as the insular ribbon sign.28,30,31 The insular ribbon normally appears on a head CT as a white stripe with a gray subcortical area medially and the dark Sylvian fissure laterally. This area of the brain is supplied by branches of the middle cerebral artery (MCA). During an ischemic event (especially in the MCA territory), cellular edema and tissue injury may ensue, leading to the obliteration of the ribbon on CT imaging. Figure 3 compares the insular ribbon sign of an ischemic stroke to the normal insular ribbon on the intact hemisphere.
Figure 3: Insular Ribbon Sign
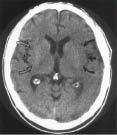
Insular ribbon sign of acute stroke on CT. In a 70-year-old man with acute right-sided weakness, emergent CT reveals loss of the left insular ribbon (solid arrows), consistent with cytotoxic edema, as compared with the normal-appearing right insular ribbon (open arrows).
Reprinted with permission of: Anderson Publishing Ltd., from Choksi V, Quint DJ, Maly-Sundgren P, et al. Imaging of acute stroke. Applied Radiology 2005;34:10-19. © Anderson Publishing Ltd.
An embolus or thrombus in a major cerebral artery (e.g., MCA, PCA, or ACA) may be seen as hyperdense artery sign on NCCT.32 Major arterial occlusion results in accumulation of blood behind the site of blockage, and this area may manifest as increased attenuation on CT. The hyperdense MCA sign, for example, has a sensitivity of 50% and specificity of almost 100% for ischemia secondary to blockage of the MCA and may appear prior to ischemic changes in the tissue.33-35
Cerebral edema secondary to ischemia may ultimately result in mass effect, detectable on NCCT. Evident by compression of ventricles and asymmetry of cortical sulci on CT, mass effect is another sign of cerebral ischemia, but requires more time to develop (on average 6 hours or more) than the previously mentioned changes. Hence, the appearance of mass effect on NCCT during what is thought to be the initial few hours of an ischemic event should prompt a reassessment of the time of onset of ischemia. The presence of severe edema and mass effect, generally, implies a poor prognosis.20,36
Even though the ECASS trial showed that early ischemic changes may increase the risk of intracranial hemorrhage, the presence of minor (localized and small) ischemic changes on NCCT is not currently a contraindication to administration of tPA. Large areas of cerebral tissue with irreversible ischemic changes, however, have been shown in various studies to have an increased incidence of hemorrhagic transformation with blood reperfusion.20,21,35,37 Hence, extensive ischemic changes observed on CT, defined as hypodensity or edema in greater than one-third of the MCA territory, preclude the use of tPA in such patients.
CT Angiography (CTA). CT angiography (CTA), obtained via the administration of intravenous contrast during CT, allows for the noninvasive imaging of both extracranial and intracranial cerebral arteries. Raw CT images are captured as the contrast enters the cerebral vessels, and a three-dimensional reconstruction of the extra- and intracranial carotid arteries, circle of Willis, and distal intracranial vessels is then created. Intracranial and extracranial vascular evaluation can alter management decisions but is only recommended acutely if it does not significantly increase the time to administration of tPA (if indicated) and also if an endovascular team is available to undertake such treatments as intra-arterial thrombosis or mechanical clot retrieval.11 Vascular imaging is also recommended as part of the evaluation of TIA patients.4
CTA has a sensitivity of 92% to 100% for detection of intracranial large vessel stenosis and occlusion when compared to conventional angiography. Similar sensitivity (80% to 100%) has been reported for extracranial lesions.11 Figure 4 shows an example of an intracranial lesion detected on CTA.
Figure 4: CT Angiographic Image
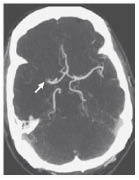
A CT angiographic image shows occlusion of the first segment of the right middle cerebral artery. The scan was obtained 1 hour 40 minutes after the onset of symptoms suggestive of cortical stroke in the territory of the right middle cerebral artery.
Reprinted with permission from: van der Worp HB, van Gijn J. Acute ischemic stroke. N Engl J Med 2007;357:572-579. Copyright © Massachusetts Medical Society. All rights reserved.
CTA Source Images (CTA-SI). The raw images obtained during a CTA are referred to as CTA source images (CTA-SI). Cerebral perfusion can be estimated using these images as the contrast passes through the brain vasculature. CTA-SI is a more accurate method of measuring cerebral perfusion than a CT perfusion (CTP) study due to the number of images available for analysis.11 Hypoperfusion and early ischemia are also more easily detected on CTA-SI than on NCCT.38 In fact, CTA-SI has been compared to MRI DWI for detection of early ischemia. DWI is superior in detection of small foci or posterior fossa ischemia, but CTA-SI is equivalent in all other areas.39,40 In many clinical centers where access to MRI is not available, CTA-SI is used as a substitute for DWI-MRI.
CT Perfusion (CTP). CT perfusion is acquired similarly to CTA, using a bolus of IV contrast, with subsequent imaging of the brain as the contrast dye traverses through cerebral vasculature. The difference lies in the construction of the perfusion map. CTP monitors the passage of the dye through certain portions of the brain parenchyma over time by repeatedly scanning the same regions. Hence, CTP is limited to only a few brain slices and potentially may miss areas of perfusion abnormalities in other regions. However, hypoperfusion detected on CTP typically precedes any detectable change on NCCT.41
The potential utility of CTP in acute stroke includes identification of the volume of core infarct that is irreversibly damaged and may be susceptible to hemorrhagic transformation, identification of at-risk areas that may be salvaged by reperfusion interventions, and monitoring of patients with abnormally perfused brain regions. (See Figure 5.) There are no current recommendations regarding CTP for the acute evaluation of stroke.
Figure 5: Perfusion CT Scan
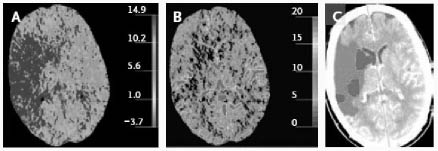
Perfusion CT scans obtained 1 hour 45 minutes after the onset of ischemia in the territory of the right middle cerebral artery. A large area shows prolongation of the mean transit time (in seconds) (Panel A), and a smaller area shows a reduction in cerebral blood volume (in milliliters per 100 g) (Panel B). These two maps suggest a large penumbra and a small infarct core (Panel C).
Reprinted with permission from: van der Worp HB, van Gijn J. Acute ischemic stroke. N Engl J Med 2007;357:572-579. Copyright © Massachusetts Medical Society. All rights reserved.
Multimodal CT. Multimodal CT allows for the acquisition of CTA and CTP immediately after conventional CT scanning and requires only 5-10 minutes of additional time. The major advantage of this combined scan is the rapid and simultaneous assessment of patients for ischemia, hemorrhage, vascular occlusion, and perfusion status using the various mentioned techniques. Multimodal CT has been shown to detect acute infarction at a higher rate than NCCT, CTA, or CTP alone.42 Multimodal CT, which can be performed with conventional CT equipment, is becoming increasingly popular in clinical centers. While relatively more expensive than conventional CT, it has been shown to be cost effective, at least in the short term, for the diagnosis of acute stroke in patients who would be considered for IV tPA or intra-arterial procedures.43 The disadvantages of this technique include increased exposure to ionizing radiation and limited ability to detect ischemia in the posterior fossa as compared to MRI techniques.44
References
1. Roger VL, Go AS, Lloyd-Jones DM, et al. Heart disease and stroke statistics 2011 update: A report from the American Heart Association. Circulation 2011;123(4):e18-e209.
2. Lloyd J. Heart Disease and Stroke Statistics-2009 Update: A Report From the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 2009;119:e21-e181.
3. Shiber JR, Fontane E, Adewale A. Stroke registry: Hemorrhagic vs ischemic strokes. Am J Emerg Med 2010;28(3):331-333.
4. Easton JD, Saver JL, Albers GW, et al. Definition and Evaluation of Transient Ischemic Attack: A Scientific Statement for Healthcare Professionals from the American Heart Association/American Stroke Association Stroke Council; Council on Cardiovascular Surgery and Anesthesia; Council on Cardiovascular Radiology and Intervention; Council on Cardiovascular Nursing; and the Interdisciplinary Council on Peripheral Vascular Disease. Stroke 2009;40(6):2276-2293.
5. Albers GW, Caplan LR, Easton JD, et al. Transient ischemic attack Proposal for a new definition. N Engl J Med 2002;347(21):1713-1716.
6. Fisher M, Ginsberg M. Current concepts of the ischemic penumbra Introduction. Stroke 2004;35(11):2657-2658.
7. Sharma M, Clark H, Armour T, et al. Acute stroke: Evaluation and treatment. Evid Rep Technol Assess 2005;(127):1-7.
8. Libman RB, Wirkowski E, Alvir J, et al. Conditions that mimic stroke in the emergency department Implications for acute stroke trials. Arch Neurol 1995;52(11):1119-1122.
9. Huff JS. Stroke mimics and chameleons. Emerg Med Clin North Am 2002;20(3):583.
10. Jauch EC, Cucchiara BL, Adeoye O, et al. 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science. Circulation 2010;122:S818-S828.
11. Latchaw RE, Alberts MJ, Lev MH, et al. Recommendations for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association. Stroke 2009;40(11):3646-3678.
12. Marler JR, Brott T, Broderick J, et al. Tissue-plasminogen activator for acute ischemic stroke. N Engl J Med 1995;333(24):1581-1587.
13. Brott T, Adams HP, Olinger CP, et al. Measurements of acute cerebral infarction a clinical examination scale. Stroke 1989;20(7):864-870.
14. Lyden PD, Lau GT. A critical appraisal of stroke evaluation and rating scales. Stroke 1991;22(11):1345-1352.
15. Goldstein LB, Bertels C, Davis JN. Interrater reliability of the NIH stroke scale. Arch Neurol 1989;46(6):660-662.
16. Delzoppo GJ, Poeck K, Pessin MS, et al. Recombinant tissue plasminogen-activator in acute thrombotic and embolic stroke. Ann Neurol 1992;32(1):78-86.
17. Jovin TG, Yonas H, Gebel JM, et al. The cortical ischemic core and not the consistently present penumbra is a determinant of clinical outcome in acute middle cerebral artery occlusion. Stroke 2003;34(10):2426-2433.
18. Schriger DL, Kalafut M, Starkman S, et al. Cranial computed tomography interpretation in acute stroke Physician accuracy in determining eligibility for thrombolytic therapy. JAMA 1998;279(16):1293-1297.
19. Perron AD, Huff JS, Ullrich CG, et al. A multicenter study to improve emergency medicine residents' recognition of intracranial emergencies on computed tomography. Ann Emerg Med 1998;32(5):554-562.
20. Hacke W, Kaste M, Fieschi C, et al. Intravenous thrombolysis with recombinant tissue-plasminogen activator for acute hemispheric stroke The European Cooperative Acute Stroke Study (ECASS). JAMA 1995;274(13):1017-1025.
21. Hacke W, Kaste M, Fieschi C, et al. Randomised double-blind placebo-controlled trial of thrombolytic therapy with intravenous alteplase in acute ischaemic stroke (ECASS II). Lancet 1998;352(9136):1245-1251.
22. Hacke W, Kaste M, Bluhmki E, et al. Thrombolysis with alteplase 3 to 4.5 hours after acute ischemic stroke. N Engl J Med 2008;359(13):1317-1329.
23. Grotta JC, Chin D, Lu M, et al. Agreement and variability in the interpretation of early CT changes in stroke patients qualifying for intravenous rtPA therapy. Stroke 1999;30(8):1528-1533.
24. Roberts HC, Dillon WP, Furlan AJ, et al. Computed tomographic findings in patients undergoing intra-arterial thrombolysis for acute ischemic stroke due to middle cerebral artery occlusion Results from the PROACT II trial. Stroke 2002;33(6):1557-1565.
25. vonKummer R, Holle R, Grzyska U, et al. Interobserver agreement in assessing early CT signs of middle cerebral artery infarction. Am J Neuroradiology 1996;17(9):1743-1748.
26. vonKummer R, Nolte PN, Schnittger H, et al. Detectability of cerebral hemisphere ischaemic infarcts by CT within 6 h of stroke. Neuroradiology 1996;38(1):31-33.
27. Lewandowski CA, Santhakumar S. Posterior Circulation Stroke. Foundation for Education and Research in Neurological Emergencies. Accessed Jan. 13, 2011. Available at www.uic.edu/com/ferne/pdf/posterior0501.pdf.
28. Marks MP, Holmgren EB, Fox AJ, et al. Evaluation of early computed tomographic findings in acute ischemic stroke. Stroke 1999;30(2):389-392.
29. Vonkummer R. Neuroradiology of early cerebral ischemia. Stroke 1995;26(2):329-330.
30. von Kummer R, Allen KL, Holle R, et al. Acute stroke: Usefulness of early CT findings before thrombolytic therapy. Radiology 1997;205(2):327-333.
31. Truwit CL, Barkovich AJ, Geanmarton A, et al. Loss of the insular ribbon Another early CT sign of acute middle cerebral artery infarction. Radiology 1990;176(3):801-806.
32. Tomsick T, Brott T, Barsan W, et al. Thrombus localization with emergency cerebral computed-tomography. Stroke 1990;21(1):180-180.
33. Flacke S, Urbach H, Keller E, et al. Middle cerebral artery (MCA) susceptibility sign at susceptibility-based perfusion MR imaging: Clinical importance and comparison with hyperdense MCA sign at CT. Radiology 2000;215(2):476-482.
34. Bastianello S, Pierallini A, Colonnese C, et al. Hyperdense middle cerebral artery CT sign Comparison with angiography in the acute phase of ischemic supratentorial infarction. Neuroradiology 1991;33(3):207-211.
35. Vonkummer R, Meydinglamade U, Forsting M, et al. Sensitivity and prognostic value of early CT in occlusion of the middle cerebral artery trunk. Am J Neuroradiology 1994;15(1):9-15.
36. Pullicino PM, Alexandrov AV, Shelton JA, et al. Mass effect and death from severe acute stroke. Neurology 1997;49(4):1090-1095.
37. Tanne D, Kasner SE, Demchuk AM, et al. Markers of increased risk of intracerebral hemorrhage after intravenous recombinant tissue plasminogen activator therapy for acute ischemic stroke in clinical practice. The multicenter rt-PA acute stroke survey. Circulation 2002;105(14):1679-1685.
38. Ezzeddine MA, Lev MH, McDonald CT, et al. CT angiography with whole brain perfused blood volume imaging Added clinical value in the assessment of acute stroke. Stroke 2002;33(4):959-966.
39. Schramm P, Schellinger PD, Fiebach JB, et al. Comparison of CT and CT angiography source images with diffusion-weighted imaging in patients with acute stroke within 6 hours after onset. Stroke 2002;33(10):2426-2432.
40. Schramm P, Schellinger PD, Klotz E, et al. Comparison of perfusion computed tomography and computed tomography angiography source images with perfusion-weighted imaging and diffusion-weighted imaging in patients with acute stroke of less than 6 hours' duration. Stroke 2004;35(7):1652-1657.
41. Reichenbach JR, Rother J, Jonetz-Mentzel L, et al. Acute stroke evaluated by time-to-peak mapping during initial and early follow-up perfusion CT studies. Am J Neuroradiology 1999;20(10):1842-1850.
42. Kloska SP, Nabavi DG, Gaus C, et al. Acute stroke assessment with CT: Do we need multimodal evaluation? Radiology 2004;233(1):79-86.
43. Young KC, Benesch CG, Jahromi BS. Cost-effectiveness of multimodal CT for evaluating acute stroke. Neurology 2010;75(19):1678-1685.
44. Ledezma CJ, Wintermark M. Multimodal CT in stroke imaging: New concepts. Radiologic Clin North Am 2009;47(1):109.
This issue of Emergency Medicine Reports is the first in a two-part series on imaging and evaluation of stroke and transient ischemic attack (TIA). This part will review risk factors, history and physical examination, and computed tomography imaging. Part 2 will review magnetic resonance imaging, duplex ultrasound imaging, and treatment.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
