Childhood Obesity in Practice
Childhood Obesity in Practice
Author:
Robert D. Murray, MD, Professor of Pediatrics, Department of Human Nutrition, College of Education and Human Ecology, The Ohio State University, Columbus, OH
Samantha Anzeljc, BS, Department of Human Nutrition, College of Education and Human Ecology, The Ohio State University, Columbus, OH
Peer Reviewer:
Philip R. Fischer, MD, Professor of Pediatrics, Mayo Clinic, Rochester, MN
Obesity currently is the nation's greatest public health challenge. Serious chronic disorders are rising rapidly among children, teens, and young adults.1-5 Despite the urgency, many primary care clinicians have failed to engage their patients and parents around the topic of obesity. Yet in early childhood, no other health proponent has the access and influence to reshape the family's collective habits. National guidelines now exist to guide primary care clinicians through the evaluation and counseling process.
Childhood Obesity
The prevalence of childhood obesity in the United States abruptly rose in the mid-1970s. Since then, rates steadily increased for nearly 30 years until the year 2000.6 In the first decade of the 21st century, rates of overweight seem to have plateaued, but at very high levels. Although obesity rates were 5% in the early 1960s, data collected by the National Health and Examination Survey (NHANES) through 2008 revealed that among all U.S. youth, 32% are overweight (above the 85th percentile body mass index [BMI]) and nearly 18% are obese (above the 95th percentile BMI). Examined by age group, the prevalence of obesity was 12.4%, 17.0%, and 17.6% for children ages 2-5 years, 6-11 years, and 12-19 years, respectively.7,8 This illustrates how early in life excess weight takes hold. Furthermore, the prevalence rates of extreme obesity, which is having a BMI > 97th percentile, was 8.5%, 11.4%, and 12.6% for children in those same age groups, respectively.
The Critical First Years
Of particular interest are the children in the first decade. This group continues to experience rising obesity rates of 1.2% to 2.1% in just the past 4 years alone.7,8 The highest risk factor for childhood obesity is parental obesity. Currently, more than two-thirds of U.S. adults are overweight and one-third are obese. The young adult parent of today represents the first wave of children caught in the obesity epidemic in the 1970s. This makes their children highly vulnerable to early and persistent excess weight.9-11 Being overweight in preschool raises by five-fold a child's risk of being overweight at age 12 years. Similarly, the child who is overweight or obese in the middle school years (10-14 years) has an 80% likelihood of being obese at age 25 years, compared with a mere 10% likelihood if normal weight.12 Collectively, the data indicate that the earlier the onset of obesity and the longer that it continues into the second decade, the greater the likelihood of maintaining obesity into adulthood.9-12
Primary Care is Front Line
Well-child visits to primary care providers offer the best public health opportunity to instill proper nutrition and physical activity habits in very young children. Nearly 95% of pediatricians obtain height and weight information on their patients during well-child visits; yet documentation of BMI and counseling are not commonly found on chart review.13-15 Only 12.5% and 13.3% of pediatricians and pediatric nurse practitioners, respectively, use BMI percentile to assess weight. The majority use their clinical impression.16 And another study showed that only 5% and 28% of overweight and obese children, respectively, had the diagnosis charted in their medical record.17 Following the trajectory of a child's rising BMI percentile can aid in an early recognition. Clinicians influence the parents' sense of urgency regarding the child's weight status by using the objective BMI information and a clear diagnosis of the problem. A recent sample of parents revealed that only 22% of patients with an obese child and 14% with an overweight child recalled the physician mentioning the child's abnormal weight.18
How to Discuss Weight
Many parents are overweight. Their experiences with weight may have been emotionally traumatic, so broaching obesity can be challenging. Physicians should focus on weight as a health issue. Making the child's BMI percentile a point of discussion during every well-child visit will heighten the family's sense of concern. Evidence of a changing BMI percentile can be useful to repeatedly raise awareness. If the child is already overweight or obese, the clinician can tie the BMI percentile with the family's health history to create a risk profile, linking the child's current and future health with diseases well known to the family.
Parental Perception
A family's readiness to change its health-related behaviors can begin only once the parents recognize that a child is overweight. Parental recognition of obesity in their own child is poor.18-21 In a sample of parents attending well-child visits who were asked to select words to characterize their child's weight status, parents of overweight and obese children were more likely to perceive their child as "about the right weight" rather than "a little overweight or obese." However, parents of overweight and obese children also were more likely to select visual images of a heavier child than an image of an average or lighter weight child, indicating a disconnect between the words they used to describe their child's weight status and their image of the child's body.18 In another study population, 71% of parents of overweight children and 28% of parents of obese children perceived their child's weight as "about right" and 72% of parents of obese children perceived their child as "somewhat overweight." Only 25% of parents of overweight children and none of the parents of obese children accurately categorized their child's weight status.21 Parental misperception of their child's weight status may be influenced by the age and sex of the child. Parents were more likely to classify their sons incorrectly than their daughters. Also, the child's age can influence a parent's concern.18,21 Parents with children younger than 6 years old were less likely to recognize that their child was overweight, but were more likely to be concerned about their child's weight status when they did become aware of it, making this age group a prime target for intervention.18
Evidence-Based Goals
Table 1: 9 Expert Committee Recommendations for Healthy Diet and Active Lifestyle Habits
Child and Adolescent Healthy Weight and Nutrition Tips
- Limit sugary beverages
- Eat 5 servings of fruits and vegetables per day
- Get 60 minutes/day of moderate physical activity
- Maintain screen time of 2 hours/day or less
- Remove TV/computer from child's bedroom
- Eat breakfast daily
- Encourage family meals
- Decrease frequency of eating out
- Limit portion sizes
Sources: Available at: www.nationwidechildrens.org/managing-obesity. Barlow SE. Expert committee recommendations regarding the prevention, assessment, and treatment of child and adolescent overweight and obesity: Summary report. Pediatrics 2007;120(Suppl 4):S164-S192.
The American Academy of Pediatrics (AAP) and 14 other collaborating organizations formed the Expert Committee on the Prevention, Identification, and Treatment of Childhood Obesity. In 2007, this group published its Expert Committee Recommendations (ECRs) to guide clinicians.22 (See Table 1.) These recommendations were rooted in scientific research and compiled to achieve optimal effectiveness in clinical practice. The primary behavioral targets included:
- Exclusive breastfeeding for the first 6 months of life
- Eating breakfast daily
- Encouraging family meals
- Limiting fast food consumption
- Increasing fruits and vegetables
- Limiting sugar-sweetened beverages
- Eating age-appropriate portion sizes
- Limiting screen time to 2 hours per day
- Participating in at least 60 minutes of physical activity
These messages can be delivered as anticipatory guidance for preventive purposes while children are younger, or they can be used as part of the intervention strategy when the child has been identified with a rising BMI or a BMI already exceeding the 85th percentile.
Toolkits, books, and programs have been developed to give clinicians resources for use in practice For example, see www.AAP.org for professional resources on obesity. (See Table 2.)
Table 2: Internet Resources
Serving sizes and specific www.MyPyramid.gov caloric needs
General information on www.MyPyramid.gov/kids feeding kids
Portion sizes www.theportionplate.com
http://hp2010.nhlbihin.net/portion
Information on fruits www.fruitsandveggiesmatter.gov and vegetables
Calcium-rich recipes www.3aday.org
School lunches, sleep habits www.kidshealth.org
Physical activity (for kids) www.kidnetic.org
Physical activity (for parents) www.cdc.gov/nccdphp/dnpa
Caffeine content of beverages http://kidshealth.org/teen/drug_ alcohol/drugs/caffeine.html
"An Ounce of Prevention" was developed in Ohio as a collaboration between medical and public health representatives and is available free to clinicians (see the Ohio Chapter of the American Academy of Pediatrics at www.OhioAAP.org). This series of visit-by-visit guides comprises a counseling process for obesity prevention, including resources that augment and amplify the basic recommendations of the Expert Committee. The materials are printed in English and acculturated Spanish. Parent handouts accompany each well-child visit and extend the physician's counseling on age-specific nutrition and activity behaviors. Figure 1 depicts the "Ounce of Prevention" handout for the 18-month well-child visit.
Figure 1: "Ounce of Prevention" Handout for the 18-month-old Well-child Visit
Clinicians can individualize each handout with the child's name, height, weight, and weight for length percentile. Handouts provide age-specific diet and activity behaviors. For the complete set of materials, see www.ohioaap.org/pediatrician-education/ohio-aap-educational-materials/ounce-of-prevention.

The BMI Charts
The BMI percentile is the most powerful tool for determining obesity. As a proxy for fat mass, it indicates whether the child is normal weight (or underweight) vs overweight (BMI 85th to 94th percentile) or obese (BMI greater than the 95th percentile).22 The Centers for Disease Control and Prevention (CDC) has provided many resources for clinicians about the BMI (available at www.CDC.gov). In 2006, the AAP, the CDC, and the National Institutes of Health convened to discuss the use of 2006 World Health Organization (WHO) growth charts in combination with the 2000 CDC growth charts. There were differences in the population of children studied and the methods used to create the CDC and WHO growths charts, and therefore, each growth chart describes growth in childhood from a different perspective.23 The CDC growth charts depict a snapshot of how a representative group of children were growing in a specific place and time. It is best used as a growth reference. For children younger than 24 months old, data were obtained from national vital statistics (for birth weights) and from Missouri and Wisconsin vital statistics (for birth lengths), the Pediatric Nutrition Surveillance Systems, and NHANES I, II, and III data, collectively. At least 50% of the infants included in the CDC charts were breastfed and 33% were breastfed until 3 months of age. Additionally, the CDC charts included infants and toddlers whose measurements reflected overweight.
The WHO charts, on the other hand, illustrate how healthy children thrived under the most favorable conditions, and therefore represent an optimal growth standard. The children included in the WHO growth charts were breastfed exclusively during the first 4 four months of life and continued breastfeeding until at least 12 months of age, meeting both the U.S. dietary reference intakes and the AAP's endorsement on breastfeeding. Additional selection criteria included low socioeconomic status, low altitude at birth, as well as inclusion of at least 20% of mothers who followed international feeding recommendations. Weight and length were measured weekly during the first 2 months of life, monthly until 12 months of age, and then bimonthly until the child was 24 months of age. For children 24-59 months of age, population demographics were similar. However, for children 24-59 months old, the WHO growth charts did not incorporate children whose weight was three standard deviations above the mean weight. Therefore, as a result, overweight children were not incorporated on the charts, even though these children were included as part of the study population.
Based on the different methodologies utilized, it has been recommended that the WHO growth charts be used for children less than 24 months old and the CDC growth charts for those above 24 months. If the WHO growth charts are utilized, physicians should use the 2nd and 98th percentiles to identify potential growth problems of under- or over-weight. The CDC charts not only provide physicians a well-researched screening method for children 2-19 years old, but also they incorporated overweight children in the study population. Physicians using the CDC charts were recommended to continue to use 5th, 85th, and 95th percentiles as indicators of unhealthy weight. But remember that the BMI is only a screening tool, not a diagnosis. Muscle mass or edema can contribute to BMI. So it is crucial that an abnormal BMI be followed by an examination to determine whether the child is at risk due to adiposity.
The Child at Risk
Once the clinician confirms that the child is either rapidly cutting across BMI percentile ranks or is already overweight or obese, the focus shifts to an assessment of the degree of health risk. There are four steps to assess health risk:
- A family health history centered on obesity, diabetes, and cardiovascular disease (hypertension, dyslipidemia, medications or surgeries, heart attacks or strokes, early death)
- A targeted review of systems centered on obesity-related disorders, such as sleep apnea, asthma, polycystic ovary syndrome, and psychological problems
- A targeted physical exam centered on the physical findings of obesity-related disorders, such as acanthosis nigricans to indicate insulin resistance, hypertension, enlarged liver, hirsutism
- Screening blood tests
The family history includes an assessment of current behavioral risks that affect energy balance, such as sedentary time and physical activity behaviors, meal and snacking habits, daily schedule, and sleep time. In this aspect of the history, the clinician is seeking to identify modifiable behavioral risks that are contributing to the child's energy imbalance. Behavioral risks fall into two categories: traditional and non-traditional risk factors. Traditional risks are those dietary behaviors and physical activity behaviors directly related to calories in and calories out. Non-traditional risk factors include factors that comprise the structure of a child's daily life, including regular breakfast time, day care or school time, sleep and wake times, family meals, play time, and study time. The compilation of traditional and non-traditional risks will identify for the clinician where to begin when counseling the patient and family on weight management.
The identification of a child at risk mandates screening labs, according to the Expert Committee Recommendations. Depending on the age of the child and the extent of overweight, the blood tests will include some or all of the following: a lipid panel (for all overweight or obese children), fasting glucose, ALT, and AST (for all obese children or those who are overweight and above age 10 years). Labs screen for high triglycerides, LDL or VLDL cholesterol, a low HDL cholesterol, glucose intolerance or early type 2 diabetes, and evidence of non-alcoholic fatty liver disease. Chart evaluations of obese children in pediatric practices showed that orders for a lipid panel, fasting glucose, ALT, and AST were found in charts in only 57.8%, 29.0%, and 10.8% of cases, respectively. Only 15% of pediatricians consistently followed all the recommendations set by the Expert Committee in 2007.16 Only 25% of pediatricians collected a complete family history; the remaining assessed some aspect of the health history 85% asked about overweight family members, 90% assessed the child's family history for cardiovascular disease and hypertension, and 64% asked about diabetes mellitus and dyslipidemia.16 Identification of signs such as acanthosis nigricans, symptoms such as amenorrhea, or abnormal laboratory findings such as high cholesterol values, are critical tools that allow the clinician to frame the problem in terms of the child's health. These signs and symptoms form the rationale for repeated counseling visits.
Promoting Change
A diagnosis of obesity will elicit a range of reactions from parents and caregivers. Many will be defensive. The most important determinant of successful weight management in a young child is the family's readiness to change. In one study evaluating parental attitudes, concern about excess weight (78%) was similar to that of their child experiencing multiple sunburns (76%) and only slightly higher than concern about watching too much television (67%).24 Parental lack of concern may relate to misperceptions about future problems associated with excess weight. Sixty-seven percent of parents believed that their overweight child was more likely than healthy weight children to be overweight as an adult; 74% believed that the child would have more difficulty with social relationships; and 76% believed that the child could develop diabetes.25
The starting point for health behavior change varies widely between patients. According to the Transtheoretical Process, there are five stages that categorize one's readiness to attempt behavior change: pre-contemplation, contemplation, preparation, action, and maintenance.26 The physician's role is to continue to express concern at each visit and encourage small, simple changes to get the family started. When the family has maintained a change in the child's health behavior for 6 or more months, the family is in the maintenance stage of change.27 Successful change builds upon itself. Particularly in obesity, relapses commonly occur. Rhee et al asked parents if they were thinking about making health behavior changes that would result in their child losing weight. Parents of obese children, compared with parents of overweight children, had an odds ratio of 4.5 for being in the preparation or action stage. This underscores the need for the physician to make families aware of their child's weight status. When parents believed that their child's weight posed a health risk, they had 16 times the odds of being in the preparation or action stage. There was increased odds for parents being in the preparation or action stage when they were overweight themselves, further supporting the need to raise the issue with families routinely.
Individually Based Risk
Despite a common assumption that obese patients share a common path to obesity, neither the causes of overweight, its development, nor the response to therapy are shared. Besides the child's familial genetic potential for obesity, race, ethnicity, and poverty are foremost contributors to risk.28-35 A study by Taveras et al illustrated ethnic differences. Hispanic and black children 2 years of age and older were more likely to have televisions in their bedrooms, to be consuming more fast food meals, and to be drinking more sugar-sweetened beverages than their white peers.28 Using the 2001 to 2003 Fragile Families and Child Wellbeing Study, Whitaker et al evaluated how race/ethnicity and several other socioeconomic indicators influenced the rates of obesity in preschool-aged children. Families were interviewed at the birth hospital (n = 4898), approximately 1 year after birth, and at 3 years of age (n = 2452).34 Despite their young age, the results were striking. Eighteen percent of children already were obese and 35.6% of children were at or above the 85th percentile for BMI. However, Hispanic children had an even higher prevalence of obesity of 25%, significantly higher than other groups. Interactions were not found between maternal education, income, or food security on the prevalence of obesity. Even with socioeconomic factors considered, Hispanic children had an 84%–104% higher risk than white children.
Obesity is fueled by genetics as well as by an individual's day-to-day life habits. A study of 4-year-old preschoolers by Anderson and Whitaker revealed that only 56.6%, 57.5%, and 40.4% ate meals with their families 6 or 7 days a week, slept an average 10.5 hours or more each night, or watched fewer than 2 hours of TV a day, respectively. Children were 23%–25% less likely to be obese if they displayed even one of those three behaviors. Cumulatively, a child further reduced the odds of being obese by 17% for each additional behavior manifested.29 This study brings attention to the benefits of encouraging structure in a child's life. Although not included in the ECRs as targeted behaviors, set sleep and wake times along with sleep duration have been independently associated with obesity in children. For instance, 7-year-old children were more likely to be obese if they fell into the lowest two quartiles for sleep duration when compared with children in the highest quartile for sleep duration, indicating that adequate sleep may reduce the risk of obesity.30
Barriers
Clinicians report that treating obesity appears overwhelming, even though 78.1% and 89.1% of pediatricians thought that obesity warranted intervention.36 Pediatricians perceived lack of patient motivation (85.7%), lack of parent involvement (81.2%), lack of support services (60.0%) lack of clinician time (58.0%), and lack of treatment skills (45.0%) as barriers to treatment.36 In another study, physicians cited environmental, practice-based, and individual patient and family factors as barriers to effective treatment. Fast food and soft drink availability were noted by 97% and 95% of physicians, respectively, as ubiquitous environmental factors, while the most common practice-based barriers were lack of reimbursement for non-MD staff (51%), lack of on-site dietitian (51%), and lack of patient education materials (44%).37 Sixty-five percent of physicians felt that the caregiver's failure to perceive weight as a problem was the most common barrier to treatment. Pediatricians thought that treatment of childhood obesity was more complex than treatment of adults because it involved changes within the entire family.38 But pediatricians also expressed interest in learning behavioral management strategies, tips for resolving family conflicts, and guidance in parenting techniques. They would prefer to learn this information and acquire additional skill sets by referencing professional guidelines and taking continuing medical education courses.38 Of all the practice barriers cited by physicians, 96% of physicians expressed a need for better counseling tools to help them shape behavior changes in their patients.37
Approaching Counseling
The clinician should set reasonable goals for counseling. The initial objective of counseling is not to induce weight loss, but to improve everyday habits, such as dietary choices and sedentary time. Increased physical activity and fitness are later goals to be achieved incrementally. In addition, evidence of a more structured daily schedule, improved family commitment and confidence, as well as a supportive network surrounding the child, are all fundamental foundations for weight management. So weight is not the sole, or even the most important, measure of success for the primary care counseling. Parents, especially mothers, are the most powerful agents of change for a young child.39,40 Thus, management of the child's weight should be viewed as a stepwise, incremental process, enacted through a series of office visits in a concentrated period of time by engaging the family in the process.41 The intervention goals should be individualized, designed in conjunction with the family, and initiated following the initial screening office visit.42 The simple guidelines outlined in Table 3 provide the foundation and basic framework for more intense counseling processes and resources that gradually should incorporate all nine of the Expert Committee Recommendations plus non-traditional risk factors. (See Table 4.)
Table 3: Approach for Management of Excess Weight During Primary Care Office Visits
Raise clinician awareness
Address parental perceptions
Raise parental awareness of child's weight status
Approach excess weight-related discussionsAnticipatory Guidance
Assess traditional and non-traditional risk factors
Collect child's history
Gauge family's readiness to change
Begin excess weight management discussions
Table 4: 10 Recommendations for Children
1. Improve food sold in schools.
2. Increase comprehensive health, nutrition, and physical education programs in schools and preschools.
3. Develop standardized national approaches to track BMI-for-age.
4. Develop national approaches for health care providers to improve nutrition, physical activity, and healthy weight gain during pregnancy.
5. Increase safe routes to schools and recreation areas.
6. Remove sugar-sweetened beverages and high-calorie snacks from schools, recreation centers, and other places where children gather.
7. Develop responsible zoning policies for fast-food around schools and other child-specific sites.
8. Promote a reduction in screen time and urge the removal of screens from the bedroom.
9. Develop policies on the marketing of foods to kids.
10. Establish affordable summer programs that support a healthy child.
Source: Center for Nutrition Policy and Promotion. Dietary Guidelines for Americans, 2010. Integrating the Evidence Available at: http://www.cnpp.usda.gov/dietaryguidelines.htm. Accessed March 14, 2011.
Sequential Counseling Visits
In a self-reported survey on office visits with preschool-aged children, only 50% of pediatricians made recommendations for weight control, compared with school-aged children where 82% of pediatricians made such recommendations.43 However, pediatrician recommendations often were not specific, such as changing "eating patterns" or "limiting specific foods," and in physical activity "increase free play" or "decrease sedentary behaviors." Pediatrician concordance with the ECRs was approximately 40% for dietary behaviors and 80% for physical activity.43 A tool to bolster self-efficacy may include obesity counseling training sessions as a continuing medical education activity. These often include information on the topics of detecting unhealthy weight trajectories, communicating sensitive weight issues to parents, providing evidenced-based messages on diet and physical activity, and following up on counseling messages.44 Perrin et al provided physicians with ways to initiate discussions on weight management, using "Promoting Healthy Weight" counseling tools, BMI color-coded charts, and tools to assess parental readiness to change. Physicians who participated in this intervention experienced an increase in their ability to interpret BMI and identify risky eating and physical activity behaviors, and their skill to counsel on risky eating and physical activity behaviors.44
Parents of overweight children offered insight for clinicians on how they should approach and facilitate discussions on pediatric overweight.45 Parents felt that such discussions should begin with pediatricians classifying the child's weight status, referring to national standards and discussing the associated health risk of excess weight. Two of the Expert Committee Recommendations, those urging parents to limit sugar-sweetened beverages and limit screen time to 2 hours, were considered especially challenging. Sugar-sweetened beverages should be clearly defined to include fruit drinks (sweetened water with little real juice), energy drinks, sweet teas, soft drinks, sugary powders, and other sources of added sugar. Instead, clinicians should promote water for thirst along with important nutrient-dense alternatives, such as 100% fruit or vegetable juice, low-fat or non-fat milk, and flavored milk. Recommendations should include age-appropriate serving size and frequency of consumption. For instance, preschool-aged children should consume no more than one 4-6 ounce glass of 100% fruit juice per day and teens should only consume 8-12 ounces per day.46 See Table 5 for additional information on healthy serving sizes for children.
Table 5: Healthy Servings for Children
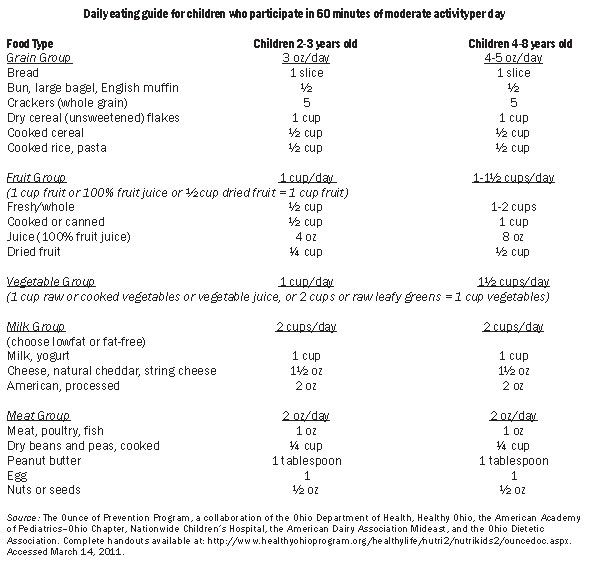
Source: The Ounce of Prevention Program, a collaboration of the Ohio Department of Health, Healthy Ohio, the American Academy of Pediatrics–Ohio Chapter, Nationwide Children's Hospital, the American Dairy Association Mideast, and the Ohio Dietetic Association. Complete handouts available at: http://www.healthyohioprogram.org/healthylife/nutri2/nutrikids2/ouncedoc.aspx. Accessed March 14, 2011.
Parents expressed difficulty in limiting screen time during inclement weather or limiting screen time when they felt it was educational. Although challenging, pediatricians can recommend planned screen time and planned non-screen time to encourage structure.47,48
Clinician counseling has been shown to be effective. To start, a simple mnemonic device, the 5-2-1-0 recommendation has been championed within the AAP for anticipatory guidance (see AAP.org or BrightFutures.AAP.org). The behaviors targeted are restricted to: 1) eating five or more servings of fruits and vegetables each day, 2) limiting screen time to less than 2 hours per day, 3) being physically active for at least 1 hour each day, and 4) consuming little or no sugar-sweetened beverages.49 In the Delaware Initiative, health care professionals were offered training to support a range of staff within the primary care setting, including receptionists, nurses, nurse practitioners, and physicians. A similar primary care intervention, Keep ME HealthyThe Maine Youth Overweight Collaborative, pioneered the use of the 5-2-1-0 materials and physicians engaged in a quality collaborative. To improve the quality of obesity care, teams collected baseline data from 70 well-child visits charts to evaluate documentation of height, weight, BMI, BMI percentile, diagnosis of overweight or obesity, and blood pressure. Families seen during the collaborative were asked if they had heard the 5-2-1-0 messages at previous office visits and were asked to rate the counseling they received during current visits. Providers were surveyed before and during the collaborative to obtain their knowledge, self-efficacy, and practices around the 5-2-1-0 messages. There was a 64% increase in obtaining BMI percentile, a 56% increase in weight classification, and an 82% increase in the use of the 5-2-1-0 behavioral screening tool. Parents also indicated that physicians began to discuss the 5-2-1-0 messages and provided increased nutrition, physical activity, screen time, and sweetened beverage counseling. Providers reported increased self-efficacy to counsel patients on obesity. With time, clinicians can expand their counseling to encompass the range of Expert Committee Recommendations plus inclusion of non-traditional behavioral risks, as well as an acknowledgement of cultural, literacy, and language differences between families.50
Making the Messages Work
In The End of Overeating, David Kessler identifies the primary problem to be treated as "conditioned hypereating."51 This term clearly frames the aims of counseling. Dietary habits are the result of repeated exposure to powerful food stimuli, particularly to high-sugar, high-fat, and high-salt items. Counseling, then, requires the gradual disconnection of the triggers, represented by food stimuli, from the patient's habitual responses, along with the substitution of new, more healthful habits. Each success decreases the power of the stimulus to evoke a conditioned eating response. To accomplish this, a number of behavioral techniques that are utilized by weight management centers may be useful for the primary care clinician during counseling:
- Create an awareness of the patient's food-response habits.
- Help establish competing behaviors meant to replace prior impulsive responses.
- Formulate specific thoughts and words that interrupt habitual responses by stating rules that reflect personal goals.
- Create a decision point, a momentary delay between the urge and the impulse to eat, to interject the new, planned action.
- Learn to identify satiety.
- Find individuals who can support the patient, reinforce their new habits, and encourage them to continue.
- Establish daily structure to minimize usual cues to eating, such as boredom or solitude.
- Expect relapses to occur and plan for them.
- Keep a diary of meals and snacks, the situations that set up successes and failures, and a regular record of weight.
Conclusions
The primary clinician who cares for children and adolescents has a unique opportunity to shape everyday eating and activity patterns. The well-child visits are particularly powerful in the first years when lifelong habits are established. The fundamental behaviors that prevent and treat obesity are the same, but they need to be approached differently in practice. Using the BMI percentile allows the family to see how they are doing. When the child is becoming overweight or is already obese, the clinician's goals change. The BMI percentile is used to raise awareness of growth trajectory and the health implications for the child, given the family's health history. Screening lab tests, a targeted history, and physicals can help reinforce the clinician's concerns. The treatment involves gradual replacement of old habits with newer, healthful behaviors. Counseling tools and behavioral motivation techniques are available to aid the primary care clinician in mastering this crucial skill in practice.
References
1. Battista M, Murray RD, Daniels SR. Use of the metabolic syndrome in pediatrics: A blessing and a curse. Semin Pediatr Surg 2009;18:136-143.
2. Daniels SR, Greer FR. Lipid screening and cardiovascular health in childhood. Pediatrics 2008;122:198-208.
3. Freedman DS, Dietz WH, Srinivasan SR, Berenson GS. The relation of overweight to cardiovascular risk factors among children and adolescents: The Bogalusa Heart Study. Pediatrics 1999;103:1175-1182.
4. Hansen ML, Gunn PW, Kaelber DC. Underdiagnosis of hypertension in children and adolescents. JAMA 2007;298:874-879.
5. McFarlin BK, Johnston CA, Tyler C, et al. Relation between adiposity and disease risk factors in Mexican American children. J Pediatr Gastroenterol Nutr 2009;49:450-455.
6. Ogden CL, Flegal KM, Carroll MD, Johnson CL. Prevalence and trends in overweight among US children and adolescents, 1999-2000. JAMA 2002;288:1728-1732.
7. Ogden CL, Carroll MD, Flegal KM. High body mass index for age among US children and adolescents, 2003-2006. JAMA 2008;299:2401-2405.
8. Anderson SE, Whitaker RC. Prevalence of obesity among U.S. preschool children in different racial and ethnic groups. Arch Pediatr Adolesc Med 2009;163:344-348.
9. Nader PR, O'Brien M, Houts R, et al. Identifying risk for obesity in early childhood. Pediatrics 2006;118:e594-e601.
10. Dubois L, Girard M. Early determinants of overweight at 4.5 years in a population-based longitudinal study. Int J Obes (Lond) 2006;30:610-617.
11. Magarey AM, Daniels LA, Boulton TJ, Cockington RA. Predicting obesity in early adulthood from childhood and parental obesity. Int J Obes Relat Metab Disord 2003;27:505-513.
12. Whitaker RC, Wright JA, Pepe MS, et al. Predicting obesity in young adulthood from childhood and parental obesity. N Engl J Med 1997;337:869-873.
13. Barlow SE, Bobra SR, Elliott MB, et al. Recognition of childhood overweight during health supervision visits: Does BMI help pediatricians? Obesity (Silver Spring) 2007;15:225-232.
14. O'Brien SH, Holubkov R, Reis EC. Identification, evaluation, and management of obesity in an academic primary care center. Pediatrics 2004;114:e154-e159.
15. Perrin EM, Flower KB, Ammerman AS. Body mass index charts: Useful yet underused. J Pediatr 2004;144:455-460.
16. Barlow SE, Dietz WH, Klish WJ, Trowbridge FL. Medical evaluation of overweight children and adolescents: Reports from pediatricians, pediatric nurse practitioners, and registered dietitians. Pediatrics 2002;110:222-228.
17. Dilley KJ, Martin LA, Sullivan C, et al. Identification of overweight status is associated with higher rates of screening for comorbidities of overweight in pediatric primary care practice. Pediatrics 2007;119:e148-e155.
18. Eckstein KC, Mikhail LM, Ariza AJ, et al. Parents' perceptions of their child's weight and health. Pediatrics 2006;117:681-690.
19. Parry LL, Netuveli G, Parry J, Saxena S. A systematic review of parental perception of overweight status in children. J Ambul Care Manage 2008;31:253-268.
20. Doolen J, Alpert PT, Miller SK. Parental disconnect between perceived and actual weight status of children: A metasynthesis of the current research. J Am Acad Nurse Pract 2009;21:160-166.
21. De La OA, Jordan KC, Ortiz K, et al. Do parents accurately perceive their child's weight status? J Pediatr Health Care 2009;23:216-221.
22. Barlow SE. Expert committee recommendations regarding the prevention, assessment, and treatment of child and adolescent overweight and obesity: Summary report. Pediatrics 2007;120(Suppl 4):S164-S192.
23. Grummer-Strawn LM, Reinold C, Krebs NF. Use of World Health Organization and CDC growth charts for children aged 0-59 months in the United States. MMWR Recomm Rep 2010;59:1-15.
24. McClaskey EL. A childhood obesity program in federally qualified community health centers. J Health Care Poor Underserved 2010;21:774-779.
25. Bibeau WS, Moore JB, Caudill P, Topp R. Case study of a transtheoretical case management approach to addressing childhood obesity. J Pediatr Nurs 2008;23:92-100.
26. Prochaska JO, Redding CA, Evers KE. The transtheoretical model and stages of change. In: Glanz K, Rimer BK, Lewis FM, eds. Health Behavior and Health Education. 4th ed. San Francisco: Jossey-Bass; 2008: 97-117.
27. Rhee KE, De Lago CW, Arscott-Mills T, et al. Factors associated with parental readiness to make changes for overweight children. Pediatrics 2005;116:e94-e101.
28. Taveras EM, Gillman MW, Kleinman K, et al. Racial/ethnic differences in early-life risk factors for childhood obesity. Pediatrics 2010;125:686-695.
29. Anderson SE, Whitaker RC. Household routines and obesity in US preschool-aged children. Pediatrics 2010;125:420-8.
30. Reilly JJ, Armstrong J, Dorosty AR, et al. Early life risk factors for obesity in childhood: Cohort study. BMJ 2005;330:1357.
31. Moss BG, Yeaton WH. Young children's weight trajectories and associated risk factors: Results from the Early Childhood Longitudinal Study-Birth Cohort. Am J Health Promot 2011;25:190-198.
32. Wang Y, Beydoun MA. The obesity epidemic in the United StatesGender, age, socioeconomic, racial/ethnic, and geographic characteristics: A systematic review and meta-regression analysis. Epidemiol Rev 2007;29:6-28.
33. Singh GK, Kogan MD, van Dyck PC. A multilevel analysis of state and regional disparities in childhood and adolescent obesity in the United States. J Community Health 2008;33:90-102.
34. Whitaker RC, Orzol SM. Obesity among US urban preschool children: Relationships to race, ethnicity, and socioeconomic status. Arch Pediatr Adolesc Med 2006;160:578-584.
35. Bouchard C, Tremblay A, Despres JP, et al. The response to exercise with constant energy intake in identical twins. Obes Res 1994;2:400-410.
36. Story MT, Neumark-Stzainer DR, Sherwood NE, et al. Management of child and adolescent obesity: Attitudes, barriers, skills, and training needs among health care professionals. Pediatrics 2002;110:210-214.
37. Perrin EM, Flower KB, Garrett J, Ammerman AS. Preventing and treating obesity: Pediatricians' self-efficacy, barriers, resources, and advocacy. Ambul Pediatr 2005;5:150-156.
38. Walker O, Strong M, Atchinson R, et al. A qualitative study of primary care clinicians' views of treating childhood obesity. BMC Fam Pract 2007;8:50.
39. Nsiah-Kumi PA, Ariza AJ, Mikhail LM, et al. Family history and parents' beliefs about consequences of childhood overweight and their influence on children's health behaviors. Acad Pediatr 2009;9:53-59.
40. West F, Sanders MR. The Lifestyle Behaviour Checklist: A measure of weight-related problem behaviour in obese children. Int J Pediatr Obes 2009;12:1-8.
41. Polacsek M, Orr J, Letourneau L, et al. Impact of a primary care intervention on physician practice and patient and family behavior: Keep ME Healthythe Maine Youth Overweight Collaborative. Pediatrics 2009;123(Suppl 5):S258-S266.
42. Golan M, Weizman A. Familial approach to the treatment of childhood obesity: Conceptual mode. J Nutr Educ 2001;33:102-107.
43. Barlow SE, Trowbridge FL, Klish WJ, Dietz WH. Treatment of child and adolescent obesity: Reports from pediatricians, pediatric nurse practitioners, and registered dietitians. Pediatrics 2002;110:229-235.
44. Perrin EM, Vann JC, Lazorick S, et al. Bolstering confidence in obesity prevention and treatment counseling for resident and community pediatricians. Patient Educ Couns 2008;73:179-185.
45. Bolling C, Crosby L, Boles R, Stark L. How pediatricians can improve diet and activity for overweight preschoolers: A qualitative study of parental attitudes. Acad Pediatr 2009;9:172-178.
46. American Academy of Pediatrics: The use and misuse of fruit juice in pediatrics. Pediatrics 2001;107:1210-1213.
47. American Academy of Pediatrics: Children, adolescents, and television. Pediatrics 2001;107:423-426.
48. Yackel EE. An activity calendar program for children who are overweight. Pediatr Nurs 2003;29:17-22.
49. Feinson J, Atkinson A, Hassink S. How a primary care quality improvement initiative is implementing the expert recommendations on childhood obesity. Del Med J 2010;82:57-65.
50. Glascoe FP, Oberklaid F, Dworkin PH, Trimm F. Brief approaches to educating patients and parents in primary care. Pediatrics 1998;101:E10.
51. Kessler DA. The End of Overeating: Taking Control of the Insatiable American Appetite. New York: Rodale, Inc; 2009.
Obesity currently is the nation's greatest public health challenge. Serious chronic disorders are rising rapidly among children, teens, and young adults.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
