Whooping Cough: Management and Diagnosis of Pertussis
Whooping Cough: Management and Diagnosis of Pertussis
Authors:
Margie S. Teng, MD, Stanford/Kaiser Emergency Medicine Residency Program, Stanford/Santa Clara, CA
N. Ewen Wang, MD, Associate Professor of Surgery/Emergency Medicine; Associate Director, Pediatric Emergency Medicine, Stanford University School of Medicine, Stanford, CA
Peer Reviewer:
James Wilde, MD, FAAP, Professor, Emergency Medicine; Associate Professor, Pediatric Emergency Medicine, Georgia Health Sciences University, Augusta, Georgia
This article originally appeared in the March 2011 issue of Pediatric Emergency Medicine Reports.
Pertussis, commonly known as the "whooping cough," is an infection of the upper respiratory tract leading to a protracted cough illness. Emergency physicians should become familiar with the diagnosis and management of this disease, given the potential of pertussis infections to cause serious morbidity and mortality in young infants. Furthermore, treating pertussis in a timely manner has a large public health impact given its extremely contagious nature.
Although the incidence of pertussis dropped sharply after the initiation of childhood vaccination programs, there still are cyclical epidemics of the disease affecting individuals in the United States. Patients with pertussis generally do not mount a febrile response, and affected individuals often present with nonspecific symptoms that make the illness difficult to diagnose. This paper will review the epidemiology, clinical diagnoses, and appropriate management for infections by Bordetella pertussis.
Ann Dietrich, MD, FAAP, FACEP
Epidemiology Scope of the Problem
The true incidence of pertussis at national and international levels is poorly defined. Accurate surveillance of pertussis is hindered by a wide range of clinical presentations along with limited diagnostic test sensitivity.1,2 During the prevaccine era in the United States, pertussis was the leading cause of death from communicable disease among children younger than 14 years. After initiation of infant and childhood vaccination, pertussis-related morbidity and mortality decreased by more than 90% since the early 1940s in the United States.3,4 However, the incidence of reported pertussis began increasing in the 1980s, with a substantial increase among persons aged 10–19 years.2,5,6 It is unclear whether this represents a true increase of disease incidence vs. improved diagnosis and surveillance. Studies estimate that between 13% to 20% of adolescents and adults with cough illness lasting longer than six days have infection by B. pertussis.1,7 Despite the increase in reported pertussis among adolescents and adults, the incidence of pertussis remains highest among infants < 6 months.4 Most hospitalizations and nearly all deaths from pertussis are found in this age group.2,5 In 2008, the incidence of pertussis in infants less than 6 months was 79.41 per 100,000.5
The incidence of pertussis peaks every 2–5 years in the United States (see Figure 1).8,9 The last peak in pertussis incidence in the United States, based on formally gathered data, was in 2004. However, once epidemiologic data from 2010 are processed, that year likely will represent a time of peak pertussis incidence in several states.5,8,10-12 For example, 2010 represented the highest incidence of pertussis infection recorded in California in 52 years.8,12
Figure 1. Reported Pertussis Incidence by Age Group
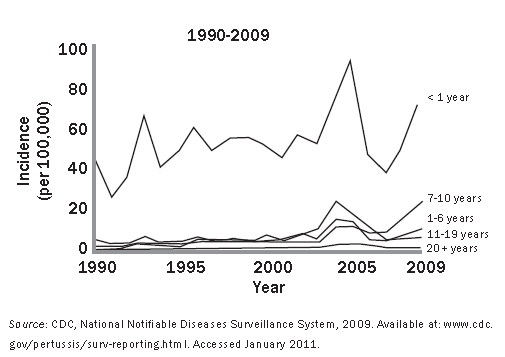
Death secondary to pertussis infection typically is isolated to very young infants. Young infants accounted for 64% of deaths during the 1980s compared to 98% of deaths in 2005.6 In infants less than 2 months of age, case-fatality rates are approximately 1%.13 In infants 2-11 months of age, case-fatality rates are approximately 0.5%.13
Etiology
Pertussis is caused by Bordetella pertussis, a fastidious, tiny, gram-negative coccobacilli.3 Humans are the only known hosts of B. pertussis. The organisms are transmitted by close contact with infected individuals via aerosol droplets.3,13 B. pertussis is an extremely contagious pathogen; attack rates are as high as 100% in susceptible individuals exposed to aerosol droplets at close range.3 The pathogen is highly labile and does not survive for sustained periods outside the host. Thus, transmission via fomites is not thought to be a significant vehicle for spread of the disease.3,13
B. pertussis is a strictly aerobic bacteria with a narrow tropism for the ciliated epithelium of the respiratory tract.3 Pathogenesis of B. pertussis is complex because of the wide range of infectious factors expressed by the bacteria and the complexity of the bacteria's toxins.3,14 Thus, the most effective vaccines contain two or more antigens toward pertussis because no sole factor can be inhibited to prevent disease.14 The genus Bordetella includes seven species that have been isolated from humans.15,16 Of these, B. pertussis and B. parapertussis are the most clinically significant. B. parapertussis causes a milder pertussis-like disease, which sometimes is clinically indistinguishable from cases of B. pertussis. B. bronchoseptica and B. holmesii also can infect humans, but are much less prevalent and typically are found in patients with prior pulmonary disease, such as cystic fibrosis, or in immunosuppressed individuals.16
Clinical Features
Pertussis represents a great diagnostic challenge for current health care providers. The disease presents with a wide range of clinical manifestations, dependent on several factors such as the age of the patient, vaccination or previous immunity status, and presence of comorbid conditions or coinfections. Clinical features of the disease evolve depending on the time course of the infection. Finally, there are few classic physical exam findings that establish diagnosis. For the majority of cases of pertussis, suspicion for the infection will rest largely on history and risk stratification.
Pertussis is a lengthy disease classically divided into three stages: the catarrhal, paroxysmal, and convalescent stages (see Figure 2). The incubation period for pertussis is typically 7–10 days, with a range of 5–21 days.1,13,14 The true duration of each of the three stages of the disease is influenced by the patient's age and immunization status.3 The first stage, or the catarrhal period, includes mild, nondistinctive upper respiratory tract symptoms similar to that of a common cold. Symptoms can consist of nasal congestion, mild sore throat, conjunctival irritation, low-grade fever, and a mild, occasional cough.17,18 During this time the affected individual is the most contagious.
Figure 2. Clinical Time Frame for Pertussis
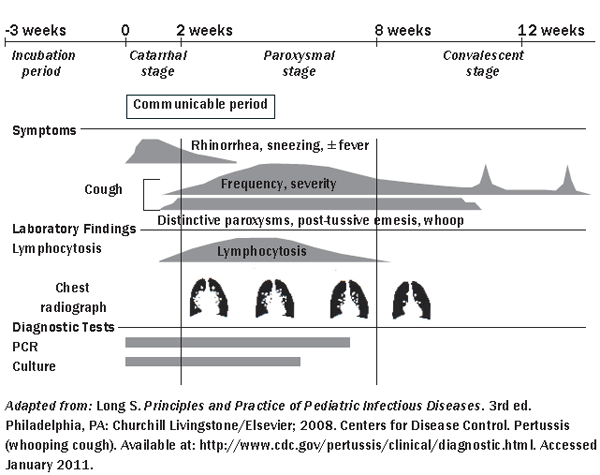
Symptoms then progress as the illness enters the paroxysmal phase. Individuals with classic B. pertussis infections will suffer from paroxysms, or fits, of repeated coughing during a single expiration which is then followed by an inspiratory whoop. The whoop is caused by breathing in against a partially closed glottis. Often the coughing paroxysms are followed by post-tussive emesis or exhaustion. The paroxysms often are associated with thick, tenacious mucus, but the production of purulent sputum does not occur.16
In non-complicated cases of pertussis, the patient typically will appear well between episodes of coughing. The paroxysmal stage may last for 2-6 weeks. As the illness advances to the convalescent stage, symptoms gradually improve over weeks to months. Despite clinical improvement during this phase, some patients will be victim to paroxysmal coughing triggered by respiratory infections for months after the initial infection by pertussis. This prolonged duration of cough distinguishes pertussis from many other respiratory tract infections; in the Chinese language, pertussis is known as "the cough of a hundred days."
Clinical suspicion for pertussis should be heightened in cases where coughing is the predominant complaint, especially if symptoms have lasted or are worsening over two weeks or longer. A careful social history is a critical component of the evaluation, as it may reveal close contact with another individual suffering from a prolonged cough illness. History of incomplete vaccination against pertussis or a significant lapse in time since last vaccination should increase suspicion for clinical infection. Typically, patients infected by pertussis appear well in between coughing fits.
Most cases of pertussis occurring after childhood occur in individuals who have had prior infection or immunization.1 This cohort often presents with a cough illness that is mild and difficult to recognize except for its prolonged time course. The majority of adult patients with pertussis have a cough of at least three weeks duration, and the cough may be only nocturnal.1,7 Adults and adolescents usually seek care late in the course of the infection. Often, delay in diagnosis also is compounded by clinicians who do not consider the diagnosis of pertussis in this age group.1 Additional symptoms that may be reported in this age group include episodes of sweating or the sensation of gasping or choking.7
One of the largest difficulties complicating the diagnoses of pertussis is that physical examination is generally uninformative. Barring the presence of clinical complications, the physical exam of individuals affected by pertussis is normal except for the coughing spells.16 If anything, it is the absence of certain clinical findings that can help strengthen the diagnosis. With uncomplicated pertussis, patients typically are afebrile or have only low-grade fevers. Furthermore, signs of lower respiratory tract disease, such as wheezes and rales, should be absent in uncomplicated disease. Conjunctival hemorrhages and petechiae on the upper body are a result of the force of repeated coughing, but otherwise patients should lack signs of a clinically significant rash.
Atypical Presentation in Young Infants. It is critical for health care providers, including emergency care professionals, to understand the atypical presentation of pertussis in young infants since they are at the highest risk for severe complications from the infection, including risk of death. The primary vaccination series against pertussis is not completed until infants are 6 months of age. Infants frequently lack the typical paroxysmal coughing and post-tussive whoop of pertussis. Furthermore, they often are brought to medical attention for symptoms other than a cough. Their caregivers may report symptoms such as gagging, gasping, or choking or symptoms consistent with an apparent life threatening event (ALTE).3,13 Further alarm symptoms that should raise clinical concern for pertussis include apneic episodes, cyanosis, and post-tussive emesis. In fact, young infants may be too weak to present with discernible coughing and may only exhibit apnea as a clinical manifestation of pertussis infection.16 Young infants typically will suffer from a prolonged convalescence period. Paradoxically, as infants grow and become stronger, the cough and whoop may become louder even as the infection is improving. The source of infection in infants is frequently an adolescent or adult family member; therefore, it is essential to perform a detailed history for possible exposure sources.16,19 (See Table 1.)
Table 1. Pertussis Clinical Pearls
Groups that are at high risk for complicated pertussis infections
- Infants under the age of 6 months, especially those under 3 months
- Infants with a history of prematurity
- Children with pre-existing cardiac, pulmonary, neurologic, or muscular disease
Clinical history that increases suspicion for pertussis
- Prolonged cough unchanged or worsening in second week of illness
- Paroxysmal ("fits") of cough
- Post-tussive emesis
- Close contact with a person with a prolonged cough
Alarm signs/symptoms in infants and young children
- Feeding intolerance/dehydration
- Respiratory distress
- Cyanosis
- Apnea
- Leukocytosis
- Pneumonia
Differential Diagnosis
The differential diagnosis for spasmodic and prolonged coughing mimicking B. pertussis infection is summarized in Table 2. Viral respiratory pathogens, especially adenovirus and respiratory syncytial virus, are among the most common agents mimicking pertussis infections.20 Furthermore, co-infection between B. pertussis and respiratory viruses is not infrequent; thus, diagnosis of a respiratory viral pathogen does not eliminate the diagnosis of pertussis. Bacterial species such as Bordetella parapertussis, Mycoplasma pneumoniae, and Chlamydia spp. often cause pertussis-like prolonged coughing.20,21 Additionally, it is critical to consider other causes of upper airway inflammation such as laryngotracheitis (croup) and bacterial tracheitis. Significant non-infectious causes of prolonged cough include foreign body aspiration, cardiogenic cough, reactive airway disease, cystic fibrosis, and congenital anomalies of the airway.22
Table 2. Differential Diagnosis for Pertussis
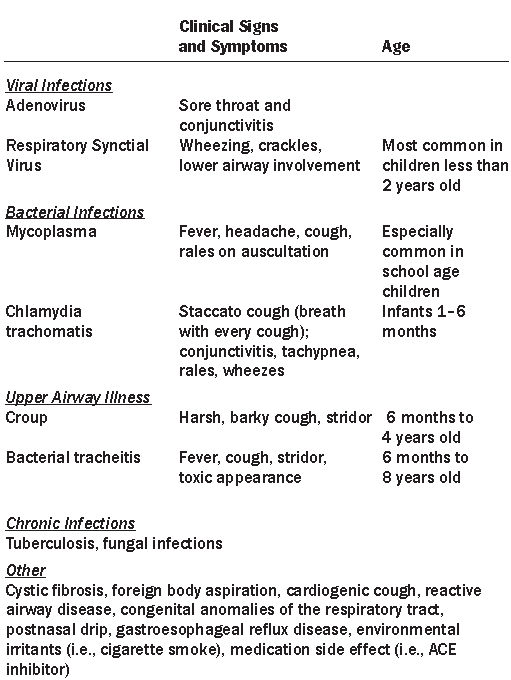
Disease Course and Complications
The majority of individuals infected with B. pertussis do not progress to develop severe complications. Typically, most patients make a gradual complete recovery with supportive care. Antibiotics given early lessen the course and severity of the disease. Severe complications, including respiratory failure and death, are most often seen in young infants less than 6 months of age. Medical comorbidities, such as an immunosuppressed state or underlying cardiac, pulmonary, muscular, or neurologic conditions, increase an individual's risk for severe disease, regardless of age at presentation.3 Typical complications of pertussis include apnea, pneumonia, otitis media, respiratory failure, and physical manifestations of forceful coughing.3,9
The paroxysmal coughing fits of pertussis infections can result in high intrathoracic and intra-abdominal pressures. Physical manifestations of this phenomenon include conjunctival and scleral hemorrhages, upper body petechiae, epistaxis, and urinary incontinence. Less frequently, severe complications of excessive pressure can occur, such as pneumothorax, subcutaneous emphysema, umbilical and inguinal hernias, rib fracture, or retinal hemorrhage.3
In infants, severe pertussis is often marked by episodes of apnea and bradycardia, which may be secondary to a toxin produced by the bacteria.23 Neurologic complications of pertussis are rare and include seizures, hypoxic encephalopathy, and even subdural hemorrhage resulting from the forceful coughing.17 Young infants may demonstrate decreased feeding tolerance with dehydration or failure to thrive.
Pneumonia is one of the most frequent complications of pertussis, occurring in 22% of infantile pertussis.3 Many cases of fatal pertussis are complicated by the development of pneumonia. Pneumonia can be caused by primary infection from B. pertussis or may be caused by a secondary co-infection with other respiratory bacteria.16 Historical and clinical features to suggest complication by secondary bacterial pneumonia include fever, respiratory distress between coughing fits, abnormal lung sounds, and tachypnea.3,23
Pulmonary hypertension can occur in cases of severe B. pertussis infection, and often is misdiagnosed as pneumonia.3 Alternatively, pulmonary hypertension may present together with bronchopneumonia. It is thought that infection by B. pertussis leads to a hyperviscosity syndrome. Circulating lymphocytes and neutrophils physically obstruct pulmonary vasculature, thus leading to vasoconstriction and severe pulmonary hypertension.24
Work-up and Diagnostic Testing
Infections by B. pertussis can present with subtle clinical presentations and the differential diagnosis for coughing can be very broad. In the emergency department, the diagnosis must be made clinically and treatment will be empiric. Radiographic and initial laboratory testing should be used to rule out other disease processes and complications. Specific diagnostic testing is important for public health and cohorting measures. In the appropriate context, testing also should be performed for other infectious causes that mimic B. pertussis infections, such as direct fluorescent antibody (DFA) or polymerase chain reaction (PCR) testing for viral agents. It is important to remember that respiratory viruses can infect the same individual concurrently; thus the presence of a viral infection does not rule out infection by B. pertussis.
Lymphocytosis is a nonsensitive and nonspecific finding that suggests infection by B. pertussis. An overall leukocytosis with white blood cell (WBC) counts ranging from 15,000 to > 100,000 cells per mL may occur.9,3,16 However, the WBC count and differential also may be normal in pertussis. An absolute lymphocytosis is often present in older infants and young children, but typically is not found in infants under the age of 6 months.9,25 A higher degree of leukocytosis correlates with a worsened clinical prognosis.16 Given its non-sensitive nature, the WBC count cannot be used to exclude the diagnosis of pertussis. An absolute increase in the number of neutrophils may be shadowed by the degree of lymphocytosis, but this finding suggests the presence of a secondary bacterial pneumonia and should not be overlooked.3
Findings on chest radiography are variable, depending on the severity of the disease and presence of co-infections such as secondary bacterial pneumonia. Uncomplicated disease may demonstrate only subtle changes such as peribronchial cuffing, interstitial edema, or atelectasis.3 Pertussis pneumonia often starts as a perihilar opacity that causes an irregular appearance of the right heart border. This often is referred to as the "shaggy heart border."23,25,26 The presence of significant parenchymal consolidation should suggest secondary bacterial infection. The chest x-ray also should be inspected for signs of pneumothorax and pneumomediastinum, which occur infrequently as a result of the high pressures generated during coughing fits.3
Bacterial culture and PCR are currently the recommended diagnostic tests for B. pertussis infections, but both tests are only of utility if obtained early during the course of the disease. In the United States, investigation by culture and PCR is recommended during the infectious period: 3 weeks from onset of cough or 4 weeks from onset of symptoms.7 (See Table 3.) Currently, there are few standardized tests available for diagnosis of pertussis after this time frame (serologic testing is used in some countries, but is not used widely in the United States).
Table 3. Comparison of Diagnostic Tests for Pertussis

Bacterial culture is considered to be the gold standard for diagnosis of pertussis; however, there are many considerations that decrease its utility.6 B. pertussis is a strictly aerobic bacteria requiring special media for its isolation. Fastidious growth requirements make B. pertussis challenging to isolate in culture; even if samples are taken early in the course of disease when bacterial load is highest, the sensitivity of culture can be as low as 15%–45%.2 The sensitivity of cultures falls steeply if the specimen is collected more than 3 weeks after the onset of cough, if antibiotic treatment has already been initiated, and if the patient has prior immunity from previous disease or immunization.1,13 Thus, although B. pertussis culture has a specificity of 100% and does not suffer from false positives found with some pertussis PCR protocols, cultures are relatively insensitive.27 A negative culture does not exclude the diagnosis of pertussis.
PCR assays for B. pertussis are increasing in popularity given their fast turnaround time and improved sensitivity. There are multiple genetic sequences that are targeted by various PCR assays. Currently, there is no Food and Drug Administration (FDA)-licensed PCR test, and there is no standardized protocol or reporting format for the test.6,13 Subsequently, the sensitivity and specificity of PCR assays for pertussis can vary widely between different laboratories.6 Unacceptably high rates of false-positive results are reported from some laboratories.13 Similar to culture techniques, the sensitivity of pertussis PCR testing is influenced by the duration of illness, whether treatment already has been initiated, and by previous immunization or previous exposure to the disease.2,13 Newer PCR testing is thought to have high specificity for the bacteria approaching 100%.2 Nevertheless, it is difficult to evaluate the true specificity of such tests, since PCR testing has higher sensitivity than the gold standard test of bacterial culture, and it is therefore difficult to confirm positive PCR tests if cultures are negative.2
Currently, the Centers for Disease Control (CDC) recommends that PCR be obtained together with B. pertussis culture, rather than as an alternative test.6 To improve the test characteristics of both pertussis bacterial culture and PCR testing, close attention must be paid to specimen collection technique and transportation of specimens to the laboratory. B. pertussis has very fastidious growth requirements, making it difficult to isolate in vitro. Samples should be obtained from a nasopharyngeal swab or aspirate taken from the posterior nasopharynx. (See Figure 3). Throat and anterior nasal swabs yield unacceptably low rates of recovery.6 The collection and sample medium used for testing is also very important. Samples need to be obtained with Dacron (polyethylene terephthalate) or calcium alginate swabs. It is important not to use cotton or rayon swabs (such as those used for standard throat cultures), which will inhibit growth of the bacteria.1,13 Specimens must be placed into special transport media immediately. Care must be taken to prevent specimens from drying and specimens must be transported promptly to the laboratory.13
Figure 3. Collection of Specimen for B. pertussis
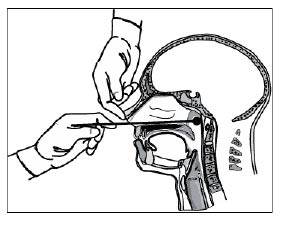
Appropriate collection of specimen for B. pertussis PCR or culture testing should come from the posterior nasopharynx.
Serologic testing is not widely recommended for the diagnosis of pertussis. Accurate serologic diagnosis ideally requires paired samples to compare levels between the acute and convalescent time frame, which prevents the utility of serologic tests for timely diagnosis.1,27 Currently, the use of a single serum specimen for diagnostic purposes is not well standardized outside of a research setting.1 DFA testing was used extensively to diagnose pertussis before PCR became widely available, but is no longer recommended due to the lack of standardization and its poor sensitivity and specificity.6,27
Management and Treatment
The treatment of pertussis in the emergency department will need to occur presumptively, prior to the return of confirmatory laboratory testing. If there is a strong suspicion for the diagnosis of pertussis based on the clinical picture, or if there is laboratory confirmation of infection, treatment with appropriate antibiotics should be initiated. Supportive care also is a critical component of management. Risk stratification based on age and comorbid health conditions will determine which patients will require admission to the hospital for cardiac and respiratory monitoring. Furthermore, attention must be paid to the public health implications such as case isolation, prophylactic treatment of close contacts, and case reporting. Both probable and confirmed pertussis cases should be reported to the state health department.6
Antimicrobial agents administered during the initial catarrhal stage of pertussis may attenuate the course of disease. After the cough is established, antimicrobial agents have no discernible effect on the course of illness.28 The main benefit of antibiotic treatment at this stage is the rapid elimination of the organism from the nasopharynx, thus decreasing the chances of pathogen transmission.13 Individuals infected with B. pertussis are infectious from the beginning of the catarrhal stage through the third week after the onset of paroxysms or until 5 days after the start of effective antimicrobial treatment. Thus, for children, adolescents, or adults, treatment is started if fewer than 3 weeks have passed since the beginning of cough symptoms.3 For patients who will be in contact with high-risk individuals and for health care workers, the time frame for treatment is extended to 6-8 weeks after onset of illness.7 The threshold for treatment for infants less than 1 year of age also is lengthened to within 6 weeks of cough onset.3 All patients with pertussis confirmed by bacterial culture or PCR testing should be started on antibiotic treatment, regardless of presence or absence of symptoms.
Individuals affected by B. pertussis may cough for up to three months after appropriate antibiotic treatment.29 Patients should be counseled that a prolonged cough after treatment is not an indicator of persistent infection, and that after appropriate antimicrobial treatment they are no longer considered contagious.29
Table 4. Recommended Antimicrobial Treatment for Pertussis
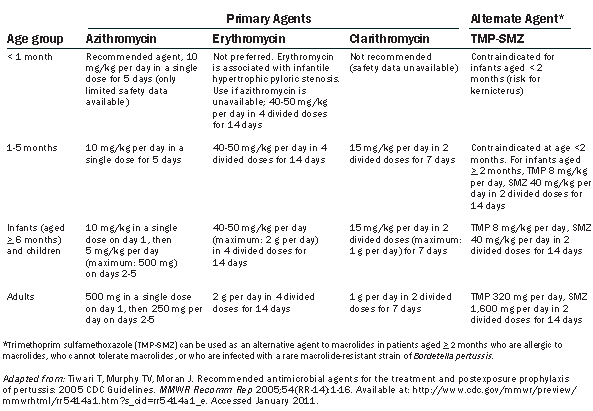
Macrolide antibiotics are the drugs of choice for infected people and their contacts (See Table 4). Historically, erythromycin was recommended as the first-line antibiotic for treatment of pertussis. However, azithromycin and clarithromycin have supplanted erythromycin for treatment and prophylaxis based on documented efficacy, ease of dosing, and improved adherence.1,28,30 Azithromycin tends to be the most popular treatment because it is given in a short, simple regimen of one dose each day for 5 days. Resistance of B. pertussis to macrolides is rare, and antimicrobial susceptibility testing is not routinely recommended. For patients who cannot take macrolide antibiotics, the CDC recommends use of trimethoprim–sulfamethoxazole (TMP-SMZ) as an alternative agent. TMP-SMZ is contraindicated as a treatment for infants younger than 2 months of age.
In addition to antibiotic treatment, supportive care is essential to appropriate management of pertussis, especially for infants. Such strategies include humidified air, supplemental oxygen, suctioning, and nutritional support. Possible triggers for paroxysmal coughing (such as cigarette smoke) should be avoided. Intubation and mechanical ventilation is indicated for respiratory failure. It is important to consider the possibility of concomitant respiratory co-infections such as bacterial pneumonia and to treat such infections appropriately.
Adjunctive therapiessuch as corticosteroids, salbutamol, pertussis immunoglobulin, and antihistamineshave been studied. However, a recent Cochrane review found that there was insufficient evidence to support the use of any of these therapies.31 The use of antitussives and opioid cough suppressants such as codeine is not recommended in infants and young children. The sedation associated with these medications may lead to adverse effects, especially in young infants.32,33
Extracorporeal membrane oxygenation (ECMO) therapy and double volume exchange transfusion have been used for treatment of severe cases of pertussis complicated by pulmonary hypertension or respiratory failure with varying rates of success. Double volume exchange transfusion must be started before the infant is in extreme distress with multiorgan failure in order to have a chance at success.34 Mortality for severe pertussis cases treated by ECMO is extremely high. The initiation of such therapies should be done in concert with specialist input, and is outside the scope of this review.
Patients admitted to the hospital should be placed on respiratory isolation to prevent further infections. Health care providers should observe droplet precautions and wear a respiratory mask when examining patients with suspected or confirmed pertussis infections.13
Management and Treatment of Young Infants
With young infants, the initial presenting symptoms of pertussis often are very subtle, yet the outcomes of missed cases can be devastating. The first step to properly manage pertussis in this age group is to have the appropriate index of suspicion for the disease. Many fatal pertussis cases in young infants initially were underestimated by both emergency physicians and primary care physicians.34 Delaying treatment until cough symptoms have lasted for more than a week and pertussis becomes the most suspicious diagnosis will miss the time frame for optimal treatment in this population.
There may be cognitive bias against widespread diagnostic testing and empiric treatment for a disease with subtle early symptoms such as mild cough, coryza, and upper respiratory tract congestion. Obviously, the differential diagnosis for these clinical signs is extremely broad, and the likelihood that such symptoms stem from a viral infection is high. One might ask whether increased testing for B. pertussis is truly worthwhile and cost effective. A strategy of increased surveillance and vigilance against the disease undoubtedly will result in a large proportion of negative tests; nevertheless, there is a potential for large cost savings and decreased mortality and morbidity if severe cases of pertussis are prevented. For example, a study of hospital charges during 1996–1999 across four states found 2,266 infants hospitalized for pertussis incurred an average cost per hospital stay of $9,580.35 Severe cases of pertussis require ICU level of care and resource intense modalities such as mechanical ventilation, ECMO, and double exchange transfusion.
The American Academy of Pediatrics (AAP) recommends that all young infants with a possible diagnosis of pertussis be treated immediately with azithromycin rather than delaying treatment for culture or PCR testing confirmation.36 If not treated, infants with pertussis remain culture-positive for longer periods than children and adults.17 Furthermore, the AAP also recommends all infants younger than 3 months of age with suspicion for B. pertussis be admitted to the hospital without exception for cardiopulmonary monitoring.3,36
Many children between 3 to 6 months of age with suspicion for pertussis require admission for observation as well, unless their clinical appearance is reassuring and witnessed paroxysms are not severe.3 Older children with medical comorbidities or children with severe pertussis associated with respiratory distress, pneumonia, feeding intolerance, or other complications also should be admitted to a hospital. In cases of severe pertussis complicated by apnea, respiratory distress, or pneumonia, it is most appropriate to admit to a facility with pediatric ICU capabilities, since the disease can quickly progress to respiratory failure or pulmonary hypertension requiring therapies such as ECMO or double-exchange transfusion.
The initial presentation of pertussis in young infants may not include cough symptoms, especially early in the course of disease. There are several clinical complaints in this age group that should prompt consideration of B. pertussis infection, such as ALTE, gagging, apnea, and cyanosis. These high-risk complaints typically require admission for cardiorespiratory monitoring, and it would be wise to consider testing for B. pertussis along with respiratory viral pathogens. In such cases, empiric treatment for B. pertussis should be started if clinical history is suspicious for high-risk exposure to the pathogen.
Although FDA has not licensed any macrolide for use in infants aged < 6 months, the CDC recommends that azithromycin be used for the treatment of young infants with pertussis and also for the prevention of pertussis in young infants who are exposed to pertussis.17,34 The risk of complications from antibiotic treatment in this age group is felt to be outweighed by the risks of severe, life-threatening complications.17 Azithromycin rather than erythromycin is recommended for young infants because erythromycin is a potential precipitating factor in infantile hypertrophic pyloric stenosis (IHPS). It is felt that IHPS is less likely to occur after azithromycin administration, although it still remains a possibility.13,34
Public Health Implications
In the evaluation of individuals with the suspected diagnosis of pertussis, it is important to screen household members and close contacts who would be at risk for severe infection or those who would serve as high-risk vectors for disease. These include young infants, children, pregnant women, or those with substantial exposure to infants/children.13 If the individual under evaluation does have exposure to such high-risk contacts, it may be appropriate to lower the clinical threshold for empiric treatment and postexposure evaluation of exposed contacts. As an example, a preschool teacher with an undifferentiated cough may warrant treatment even if the diagnosis of pertussis is not confirmed.
The CDC recommends administration of postexposure prophylaxis to all close contacts of infected individuals. Prophylaxis is attempted as an effort to prevent transmission and minimize the burden of disease. Prophylactic treatment should be given within 21 days of onset of cough in the index patient, regardless of the age and vaccination status of the exposed individual.6 The recommended antimicrobial agents and doses are the same for treatment and chemoprophylaxis. If 21 days have elapsed since onset of cough in the index case, chemoprophylaxis has limited value but should be considered for households with high-risk contacts.13 Furthermore, household members with symptoms such as cough should be treated as if they have pertussis, even if more than 21 days have passed in the index case.17
Individuals who are symptomatic or who have confirmed pertussis should be excluded from activities that could further transmit the disease (such as school or work) until they complete the 5 days of appropriate antibiotic treatment.13
Immunizations
Vaccination of susceptible persons is the most important preventive strategy against pertussis. The vaccines used in the United States are acellular vaccines against pertussis combined with diphtheria and tetanus toxoids.13 DTaP is used for pediatric populations and Tdap is formulated for use in adolescents and adults.13
The recommended vaccination schedule for children is a four-dose primary series of DTaP, administered at 2, 4, 6, and 15-18 months of age. A fifth booster dose is given between ages 4 to 6 years. 6,17 Neither disease nor vaccination provides complete or lifelong immunity against disease or reinfection.3 Immunity wanes 5–10 years after the last pertussis vaccine dose. Older children, adolescents, and adults can become susceptible to pertussis after a complete course of vaccination during childhood. Since 2005, increased vaccination coverage post-childhood has started to become available through the use of Tdap vaccination for individuals ages 11 to 64 years. Tdap vaccines were formulated for use in older individuals by reducing the amounts of diphtheria toxoid and some of the pertussis antigens.13
In adults requiring tetanus vaccination for wound management, a single dose of Tdap is recommended to replace the Td booster.3 Health care workers and those with infant contact are recommended to receive the vaccination on an accelerated schedule, and they should receive Tdap once 2 years have passed since the last receipt of Td.3,13,37
Conclusion
The greatest medico-legal pitfall surrounding pertussis in the emergency department setting is an inappropriately low level of suspicion for the disease. The presenting symptoms for pertussis can be very nonspecific, but there is high potential for significant morbidity and mortality in at-risk age groups. Emergency providers must screen for alarm symptoms or social history that would increase suspicion for infection by B. pertussis, even with a benign-appearing complaint such as an isolated cough. Risk stratification based on age, history, and physical exam will help dictate appropriate treatment and disposition. It is important to remember that young infants affected by pertussis may look well during the initial stages of the disease, but may rapidly progress to serious life-threatening complications such as pneumonia, pulmonary hypertension, and respiratory failure.
References
1. Wood N, McIntyre P. Pertussis: Review of epidemiology, diagnosis, management and prevention. Paediatr Respir Rev 2008;9:201-211; quiz 211-212.
2. Crowcroft NS, Pebody RG. Recent developments in pertussis. Lancet 2006;367:1926-1936.
3. Long S. Principles and Practice of Pediatric Infectious Diseases. 3rd ed. Philadelphia PA: Churchill Livingstone/Elsevier; 2008.
4. Centers for Disease Control. PertussisUnited States, 2001–2003. MMWR Recomm Rep 2005;54:1283-1286.
5. Centers for Disease Control. Summary of Notifiable DiseasesUnited States, 2008. MMWR Recomm Rep 2010;57(54).
6. Brown K, Cassiday P, Tondella M, et al. Chapter 10: Pertussis. In: Manual for the Surveillance of Vaccine-Preventable Diseases (4th Edition, 2008). 4th ed. Atlanta, GA: Centers for Disease Control and Prevention; 2008.
7. Hewlett EL, Edwards KM. Clinical practice. Pertussisnot just for kids. N Engl J Med 2005;352:1215-1222.
8. Centers for Disease Control. Notes from the Field: PertussisCalifornia, January–June 2010. MMWR Recomm Rep 2010;59:817.
9. McMillan J. Oski's Pediatrics: Principles & Practice. 4th ed. Philadelphia: Lippincott Williams & Wilkins; 2006.
10. Centers for Disease Control. Summary of Notifiable DiseasesUnited States, 2004. MMWR Recomm Rep 2006;53:1-79.
11. Roehr B. Whooping cough outbreak hits several U.S. states. BMJ 2010;341:c4627.
12. Pertussis Report. California Department of Public Health, Immunization Branch. 2010. Available at: www.cdph.ca.gov/programs/immunize/Documents/PertussisReport2010-11-30.pdf. Accessed December 2, 2010.
13. Pickering L, American Academy of Pediatrics. Red book: 2009 Report of the Committee on Infectious Diseases. Elk Grove Village, IL: American Academy of Pediatrics; 2009.
14. Crowcroft NS, Pebody RG. Recent developments in pertussis. Lancet 2006;367:1926-1936.
15. Heininger U. Update on pertussis in children. Expert Rev Anti Infect Ther 2010;8:163-173.
16. Mattoo S, Cherry JD. Molecular pathogenesis, epidemiology, and clinical manifestations of respiratory infections due to Bordetella pertussis and other Bordetella subspecies. Clin Microbiol Rev 2005;18:326-382.
17. Tiwari T, Murphy TV, Moran J. Recommended antimicrobial agents for the treatment and postexposure prophylaxis of pertussis: 2005 CDC Guidelines. MMWR Recomm Rep 2005;54(RR-14):1-16.
18. Atkinson W, Wolfe S, Hamborsky J, McIntyre L, eds. Centers for Disease Control and Prevention. Epidemiology and Prevention of Vaccine-Preventable Diseases. 11th ed. Washington DC: Public Health Foundation; 2009.
19. Wendelboe AM, Njamkepo E, Bourillon A, et al. Transmission of Bordetella pertussis to young infants. Pediatr Infect Dis J 2007;26:293-299.
20. Wirsing von König CH, Rott H, Bogaerts H, Schmitt HJ. A serologic study of organisms possibly associated with pertussis-like coughing. Pediatr Infect Dis J 1998;17:645-649.
21. Hagiwara K, Ouchi K, Tashiro N, et al. An epidemic of a pertussis-like illness caused by Chlamydia pneumoniae. Pediatr Infect Dis J 1999;18:271-275.
22. Stein MT, Spector SA, Olmsted N, Thombs P. Chronic cough in infants younger than three months. West J Med 1982;136:505-512.
23. Fisher R. Moffet's Pediatric Infectious Diseases: A Problem-oriented Approach. 4th ed. Philadelphia: Lippincott Williams and Wilkins; 2005.
24. Paddock CD, Sanden GN, Cherry JD, et al. Pathology and pathogenesis of fatal Bordetella pertussis infection in infants. Clin Infect Dis 2008;47:328-338.
25. Shah S, Sharieff GQ. Pediatric respiratory infections. Emerg Med Clin North Am 2007;25:961-979, vi.
26. Fleisher GR, Ludwig S. Textbook of Pediatric Emergency Medicine. Lippincott Williams & Wilkins; 2010.
27. Mandell G. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 7th ed. Philadelphia PA: Churchill Livingstone/Elsevier; 2010.
28. Altunaiji SM, Kukuruzovic RH, Curtis NC, Massie J. Antibiotics for whooping cough (pertussis). In: The Cochrane Collaboration, Altunaiji SM, eds. Cochrane Database of Systematic Reviews. Chichester, UK: John Wiley & Sons, Ltd; 2007. Available at: www2.cochrane.org/reviews/. Accessed January 19, 2011.
29. Cornia PB, Lipsky BA, Saint S, Gonzales R. Clinical problem-solving. Nothing to cough ata 73-year-old man presented to the emergency department with a 4-day history of nonproductive cough that worsened at night. N Engl J Med 2007;357:1432-1437.
30. Langley JM, Halperin SA, Boucher FD, Smith B. Azithromycin is as effective as and better tolerated than erythromycin estolate for the treatment of pertussis. Pediatrics 2004;114:e96-101.
31. Bettiol S, Thompson MJ, Roberts NW, et al. Symptomatic treatment of the cough in whooping cough. Cochrane Database Syst Rev 2010;(1):CD003257.
32. Shehab N, Schaefer MK, Kegler SR, Budnitz DS. Adverse events from cough and cold medications after a market withdrawal of products labeled for infants. Pediatrics 2010;126:1100-1107.
33. Vassilev ZP, Kabadi S, Villa R. Safety and efficacy of over-the-counter cough and cold medicines for use in children. Expert Opin Drug Saf 2010;9:233-242.
34. Cherry JD, Harrison R, Bradley J, et al. Pertussis in Young Infants. Available at: www.aap-ca.org/clinical/pertussis/pertussis_in_young_infants.html#ref_3. Accessed November 3, 2010.
35. O'Brien J, Caro JJ. Hospitalization for pertussis: Profiles and case costs by age. BMC Infectious Diseases 2005;5:57.
36. Pertussis in Young Infants. Available at: www.aap-ca.org/clinical/pertussis/pertussis_in_young_infants.html#ref_3. Accessed November 3, 2010.
37. Centers for Disease Control. Tetanus and pertussis vaccination coverage among adults aged > or = 18 yearsUnited States, 1999 and 2008. MMWR Recomm Rep 2010;59:1302-1306.
Pertussis, commonly known as the "whooping cough," is an infection of the upper respiratory tract leading to a protracted cough illness. Emergency physicians should become familiar with the diagnosis and management of this disease, given the potential of pertussis infections to cause serious morbidity and mortality in young infants. Furthermore, treating pertussis in a timely manner has a large public health impact given its extremely contagious nature.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
