Approach to Acute Thoracolumbar Spine Fracture Management in the Emergency Department
Approach to Acute Thoracolumbar Spine Fracture Management in the Emergency Department
Authors:
Pedro Roque, MD, Department of Emergency Medicine, Division of Research, Maricopa Medical Center, Phoenix, AZ.
Iman Feiz-Erfan, MD, Department of Surgery, Division of Neurosurgery, Maricopa Medical Center, Phoenix, AZ.
Frank LoVecchio, DO, MPH, Department of Emergency Medicine, Maricopa Medical Center, Phoenix, AZ.
Teresa S. Wu, MD, FACEP, Department of Emergency Medicine, Maricopa Medical Center, Phoenix, AZ.
Peer Reviewer:
Robert E. Falcone, MD, FACS, Clinical Professor of Surgery, The Ohio State University, Columbus.
Much attention has been given to injuries of the cervical spine, but injuries to the thoracolumbar region are actually more common. Because of the anatomy involved, these injuries are often accompanied by multiple serious injuries to other areas of the body and may be overlooked during resuscitation and stabilization.
Sandra M. Schneider, MD, FACEP, Editor
Introduction
Thoracolumbar spine (TLS) trauma is among the most common musculoskeletal injuries worldwide, with nearly 175,000 new spine fractures reported each year in the United States alone.1 Automobile accidents account for the majority of thoracolumbar injuries, followed by falls, sporting accidents, and penetrating trauma, in decreasing order of frequency.2 Emergency physicians (EPs) play an important role in the diagnosis and the initial management of acute thoracolumbar spine injuries. Failure to recognize unstable fracture patterns in the acute phase may lead to progression of neurologic injury and devastating long-term consequences for the patient. In the past 15 years, there have been significant advances in the diagnostic classification, imaging, and medical and surgical treatments of TLS injury. A thorough understanding and application of these principles by EPs will help maximize the recovery potential of all TLS injury patients.
Anatomy
The thoracic spine (T1-T10) is a rigid, fixed structure due to its attachments anteriorly to the sternum and posteriorly to the rib cage. The spinal canal at the thoracic levels is also narrower than in other areas of the spine. This rigid structure, combined with the small spinal canal and the great force required to impart damage at this level of the spine, accounts for the relatively high incidence of significant neurological deficits following fractures of the thoracic spine. In contrast, the thoracolumbar spine (T11-L2) has a unique anatomy, making it a particularly vulnerable area of the spine. Unlike the thoracic spine, the transverse processes do not articulate with either the sternum or the rib cage, resulting in a less rigid system.
The thoracolumbar region (T11 to L2) is the most common site of spine fractures, as the region forms a transition zone between the relatively fixed, kyphotic thoracic spine above, and the relatively mobile, lordotic lumbar spine below. These factors cause stress forces to concentrate upon the thoracolumbar vertebral column.3 The spinal canal is also wider at this level, resulting in a greater number of incomplete spinal cord injuries. Within the thoracolumbar spine lies the terminal segment of the spinal cord, which is called the conus medullaris. In adults, the conus medullaris typically ends at the level of L1. Individual nerve roots then extend distal to this segment, forming the cauda equina. Surrounding these nerves of the spinal cord is the dura mater and then the ligamentum flavum, which connects under the facet joints to create a small curtain over the posterior openings between the vertebrae. Anterior to each vertebra lies the anterior longitudinal ligament. The posterior longitudinal ligament runs immediately posterior to the vertebral body and forms the anterior portion of the spinal canal.
Spine anatomy is often divided into the anterior column, middle, and posterior column.4 The anterior column is formed by the anterior half of the vertebral body, the corresponding intervertebral disc, and the anterior longitudinal ligament. The middle column is formed by the posterior half of the vertebral body, the corresponding intervertebral disc, and the posterior longitudinal ligament. The posterior column containing the spinal canal is formed by the osseous and ligamentous structures posterior to the vertebral body. The osseous structures in the posterior column include the pedicles, articulating facets, spinous processes, and the transverse processes. These structures are held in alignment by the posterior ligamentous complex (PLC), which includes the supraspinous, interspinous, capsular ligaments, and the ligamentum flavum. The PLC protects the spine and the spinal cord against excessive flexion, rotation, translation, and distraction, effectively earning it the name "posterior tension band."5-12
Spine Stability
Assessing the stability of the spinal column is a crucial first step in the evaluation of TLS injuries. Defining stability has been a topic of great controversy. In 1977, Whitesides provided an intuitive explanation for spine stability.13 He compared the spine to a construction crane. The vertebral bodies are similar to the boom, and the posterior elements are similar to the guy wires. Guy wires, or tag lines, are the wires that attach to the payload and are used by the ground crew to control rotation and movement. According to Whitesides, the function of the spine is to hold the body erect and protect the neural elements that pass through it. He stressed that the center of gravity of the body is anterior to the spine in the erect posture, thereby imparting compressive forces to the vertebral bodies and tensile forces to the posterior elements.13 A stable spine, therefore, is one that can withstand compressive forces anteriorly through the vertebral bodies, tension forces posteriorly through the posterior ligamentous complex, as well as rotational forces, thus being able to hold the spine erect without progressive kyphosis and to protect the spinal contents from further injury.13
Table 1: Thoracolumbar Injury Classification and Severity Scoring
|
Parameter |
Points |
|
Morphology |
|
|
Compression fracture |
1 |
|
Burst fracture |
2 |
|
Translational/rotational fracture |
3 |
|
Distraction |
4 |
|
Neurologic Involvement |
|
|
Intact |
0 |
|
Nerve root |
2 |
|
Cord, conus medullaris |
|
|
Incomplete |
3 |
|
Complete |
2 |
|
Cauda equina |
3 |
|
Posterior Ligamentous Process |
|
|
Intact |
0 |
|
Injury suspected/indeterminate |
2 |
|
Injured |
3 |
|
Management |
Total Points
Non-operative
0-3
Non-operative or operative
4
Operative
≥ 5
Adapted from: Vaccaro AR, Lehman RA Jr, Hurlbert RJ, et al. A new classification of thoracolumbar injuries: The importance of injury morphology, the integrity of the posterior ligamentous complex, and neurologic status. Spine 2005;30:2325-2333.
The integrity of this posterior column cannot be overestimated it is the key to a stable spine. Studies have also shown that once disrupted, the PLC demonstrates poor healing capacity.5-12 PLC compromise is suggested by a range of radiographic parameters (see Table 1): kyphosis > 20°, loss of > 50% anterior vertebral body height, spinal dislocation of the posterior elements (i.e., facet dislocation), multiple adjacent compression fractures, and bony retropulsion with spinal canal compromise > 30%. 5-12 (See Table 2.) A fracture with any of the aforementioned radiologic characteristics is considered unstable and should be treated as such.
Table 2: Radiographic Criteria for Instability Defined as Posterior Ligamentous Complex Compromise
Radiographic Criteria for Instability
- Kyphosis > 20°
- Loss of > 50% anterior vertebral body height
- Multiple adjacent compression fractures with significant spinal deformity
- Spinal dislocation of the posterior elements (i.e., facet dislocation)
- Bony retropulsion into spinal canal with > 30% canal compromise
Also of note, a thoracolumbar spine fracture pattern can be classified as unstable if there is a new abnormal finding in the neurologic exam in the setting of blunt trauma or other significant mechanism of injury.
Injury Morphology
The three major trauma mechanisms for thoracolumbar spine fractures are rotation/translation, distraction, and compression. (See Figure 1.) Each mechanism of injury produces typical fracture patterns. Careful scrutiny of the fracture pattern provides valuable information regarding the trauma mechanism, the severity of the fracture, and possible associated injuries.
Figure 1: Thoracolumbar Spine Fracture: Major Mechanisms of Injury
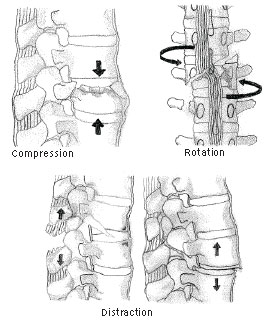
Rotational/translational injuries are identified by the horizontal displacement of one thoracolumbar vertebral body over another. Radiographically, these fracture patterns demonstrate significant vertebral body anterolisthesis with either unilateral or bilateral facet dislocations, with or without posterior element fracture. These injuries are unstable and warrant immediate spine surgery subspecialty consultation.
Distractional TLS injuries are caused by hyperextension at the fracture site, resulting in widening of the anterior intervertebral disc space and injury to the anterior longitudinal ligament. These injuries often lead to posterior element fractures because of the stress placed posteriorly as the spine hinges backward on the posterior elements. These injuries are also unstable and warrant immediate spine surgery consultation.
Rotation and distraction injuries should always be considered unstable during the initial diagnosis and management in the emergency department. Treatment for these patients will be dictated by the spine consultant, and there is no role for conservative management in the emergency department by the EP.
The third fracture morphology is due to compression (forward flexion and/or axial compressive force). Unlike rotational and distractive TLS injury patterns, compression injuries have the potential for conservative treatment and outpatient follow-up depending on the involvement of the middle column and the integrity of the PLC. These fractures are defined by a loss of vertebral body height. The two main thoracolumbar spine fracture patterns within this category are the compression fracture and the burst fracture.
To fully understand the difference between a compression and a burst fracture, one must revisit a historic thoracolumbar spine injury classification system proposed by Denis in 1983.4 Denis devised a three-column concept of spine stability based on a retrospective review of 412 thoracolumbar spine injuries using computed tomography (CT) as the main radiographic modality. He stressed the importance of the middle column and concluded that the integrity of the middle column determines the stability of the spine.4
Compression fractures are extremely common, constituting 50% to 70% of all traumatic TLS injuries.14 Compression fractures result in injury to the anterior column, with an intact middle and posterior column. The fracture generally results from forward flexion and is rarely associated with neural injury, unless multiple consecutive compression fractures are present with severe spinal deformity. A lateral radiograph demonstrates a kyphotic deformity with an unchanged posterior vertebral height, indicating that the posterior cortex of the vertebral body is intact. CT can be used to confirm that the middle and posterior columns are not involved. Bracing and bed rest remain the mainstays of treatment for patients who have sustained single or double compression fractures.
Compression fractures must be distinguished from more serious burst fractures, as neurologic injury has been reported to occur in 30% of the patients with thoracolumbar burst fractures.15 Burst fractures account for up to 17% of all major spinal fractures.3 The sudden application of a supraphysiological axial load results in vertebral end-plate failure as adjacent disc tissue is driven into the vertebral body. The vast majority of burst fractures are associated with some degree of canal compromise, as a result of bony retropulsion of an osseous fragment or fragments from the posterior superior end plate. Remember that the posterior vertebral body cortex forms the anterior wall of the spinal canal, so significant compression fractures can easily injure the adjacent nerve fibers. CT remains the radiographic modality of choice for characterizing a TLS burst fracture pattern. The two most important views on the CT scan are the sagittal reconstruction and the axial views. The sagittal reconstruction allows the EP to visualize posterior vertebral body height, the interpediculate distance, and the presence of bony retropulsion into the canal. It is important to note that one cannot estimate the degree of spinal canal compromise from the sagittal reconstruction alone, as this can only be done using the axial views. One should also look for signs of facet dislocation, posterior element fracture, and widening of the anterior or posterior intervertebral disc space. Axial views are ideal for identifying posterior vertebral body fracture and visualization of bony fragments in the spinal canal. Final take-home points are listed in Table 3.
Table 3: The Three Major Trauma Mechanisms for Thoracolumbar Spine Fractures
TLS Trauma Mechanisms Take-Home Points
I. All fracture patterns with an element of rotation or distraction are considered unstable.
II. Compression fractures involve only the anterior column and cannot cause neurologic compromise unless several continuous compression fractures are present with significant spinal deformity.
III. Burst fractures involve both the anterior and middle column ± bony retropulsion into the spinal canal and are considered unstable until proven otherwise by a spine specialist.
IV. Fractures may display characteristics of one or more of these injury mechanisms.
Classification System
EPs should become comfortable using a fracture classification system to rapidly and accurately analyze any TLS fracture pattern. Learning to describe TLS injuries via commonly accepted classification systems will make communicating with consultants much easier, as well as provide the team with some information regarding patient prognosis and treatment options.
There have been many classification systems for TLS fractures over the past 100 years, but none are more widely used than the Denis classification system and the more recent Magerl Arbeitsgemeinschaft für Osteosynthesefragen (AO) classification system. The Denis system is based on the three-column concept for spine stability, emphasizing the integrity of the middle column and the posterior ligamentous complex for stability of the post-injury thoracolumbar spine.4,14-19 This system categorizes all fractures into four basic fracture types: anterior compression fractures, burst fractures, fracture-dislocations, and seat-belt injuries. Although easily reproducible, this system is not detailed enough to account for all fracture patterns.4,16-19 In 1998, Magerl et al introduced the AO classification system.20 This new system accounts for most TLS fracture patterns unable to be classified previously under the Denis system and organizes them in a more clinically relevant manner. It is based on the principle that injury mechanism determines the morphology of the fracture, and is structured with a hierarchical ranking of progressive severity of instability. Critics of the AO system say that it is too complicated, difficult to remember, and provides no prognostic or treatment information.
Recently, a new classification system has been proposed called the Thoracolumbar Injury Classification and Severity Score (TLICS).16 It incorporates principles from the AO classification system as well as patient neurologic status, resulting in a proposed clinical prediction rule.16 It is the first classification system to specifically include the neurologic status of the patient and provide a clinical prediction rule for treatment of thoracolumbar spine fractures.16 TLICS is based on three major descriptive categories: injury morphology, integrity of the posterior ligamentous complex, and neurologic status. (See Table 1.) It then assigns an injury severity score to these categories.16 This system is based on a progressive score for each of the three major injury categories (injury morphology, integrity of the posterior ligamentous complex, and neurologic status) and is calculated by the summation of the individual scores. Three or fewer points suggest non-operative management, five or more points suggest operative management, and four points suggest either surgical or non-surgical management.16 (See Table 1.) This classification system has shown good intra- and inter-rater reliability among surgeons and is gaining momentum as the most intuitive and useful classification system.18,19,21-29
This classification system ties together three major concepts of thoracolumbar spine fracture analysis and overall management principles, incorporating them into a simple, efficient prediction rule. These three major concepts are: neurologic exam, fracture morphology, and posterior ligamentous complex integrity.
The first major concept is neurologic status. This is the first step in the evaluation process of any patient with a potential thoracolumbar spine fracture. The importance of a thorough neurological exam, including a perineal and rectal examination, cannot be overstated. The next important concept involves fracture morphology analysis. (See Figure 1.) Knowing the three major trauma mechanisms and their predictable fracture patterns will help determine the stability of the fracture pattern. The third major concept is posterior ligamentous complex integrity. It is well known that the posterior ligamentous complex is the key to spine stability. It resists the tensile forces and functions as the "posterior tension band" of the spine. Posterior ligamentous complex compromise is suggested by a range of radiographic parameters: kyphosis > 20°, loss of > 50% anterior vertebral body height, spinal dislocation of the posterior elements (i.e., facet dislocation), multiple adjacent compression fractures, and bony retropulsion with spinal canal compromise > 30%.10-12,16,30-38 (See Table 2.) These values are easy to measure and help identify an unstable fracture pattern.
In summary, use of the TLICS classification system incorporates essential information that has already been gathered by the EP (neurological exam, fracture morphology, and PLC integrity) and assimilates it into a simple, clinical prediction rule with prognostic information.
Evaluation and Immediate Management
In the assessment of a multisystem trauma patient, assessment of the patient's airway, breathing, and circulation (ABCs) takes priority. Proper spine precautions and immobilization must be maintained throughout the initial stabilization period. Long, rigid backboards should be removed as soon as possible after the patient is moved to a firm stretcher. Log-rolling the patient is the standard procedure for removing the board, with personnel rolling the shoulders and hips, along with supporting the extremities and the cervical spine. A fourth individual should examine the back for pain and other injuries. Patients should not be kept on a hard backboard even if injury is suspected because of pressure-sore formation. Immediately following initial stabilization, a careful neurologic examination is warranted. It typically includes tests of motor strength, sensory function (light touch, pin prick, and vibration), reflexes, rectal tone, and a thorough perineal examination. Any abnormality in the neurological exam in the setting of a thoracolumbar spine fracture should prompt immediate spine surgery consultation and continued strict spinal precautions. Neurologic examination in the unresponsive or comatose patient includes observing the patient for spontaneous movement, eliciting response to painful stimuli, testing of deep tendon reflexes, performing upper motor neuron tests (i.e., Babinski reflex, clonus), and conducting a careful perineal examination (i.e., bulbocavernosus reflex, anal wink reflex, rectal tone).
Special attention must be paid to documenting a thorough perineal examination to avoid missing injuries to the conus medullaris and the cauda equina. (See Table 4.) Typically, the conus medullaris in adults is located at the terminal point of the spinal cord at approximately the L1 level, with the nerve roots exiting distally in the shape of a "horse's tail," thereby forming the cauda equina. Thoracolumbar spine fractures at this level can cause a variety of patterns of neurologic deficit, ranging from subtle bowel and bladder findings to profound sensory and motor deficits.39,40 A thorough perineal examination includes sensory testing, bladder function testing, and several important reflexes, including bulbocavernosus reflex and the anal wink (anocutaneous reflex). (See Table 4.)
Bladder function can be easily tested using bedside ultrasound or catheterization in which a post-void residual is measured. In many practices, a post-void residual of > 100 mL is considered to be abnormal, but this cutoff varies with the practitioner and institution. The bulbocavernosus reflex is another important reflex involving the sacral nerve roots. This spinal cord-mediated reflex arc is elicited by squeezing the glans of the penis or clitoris (or applying traction on an indwelling catheter), resulting in palpable rectal contraction. In cases of cervical or thoracic spinal cord injury, absence of the bulbocavernosus reflex signals the presence of spinal shock, and return of this reflex signals the termination of spinal shock. Rectal tone can also be concurrently assessed. Another important reflex is the anal wink reflex (anocutaneous reflex), which involves various sacral nerve roots. It is elicited by gently stroking the peri-anal skin with a cotton swab. If present, it results in contraction of the external anal sphincter muscle.
The EP must next choose the proper imaging modality to assess the spine. Radiographic screening of the spine axis can be accomplished by a number of means, including plain radiography, CT, and magnetic resonance imaging (MRI). In many trauma centers, CT has replaced plain film as the primary modality for evaluation of spinal trauma. Magnetic resonance imaging is not indicated for all cases of spinal trauma but provides detailed information about soft-tissue structures, including the intervertebral disc, the ligaments, the epidural space, the blood vessels, and the spinal cord. Patients with spinal cord injury may suffer devastating long-term neurologic deficits, so prompt and efficient spinal imaging guidelines are necessary in all trauma centers.
Figure 2: Algorithm for Imaging Patients with Blunt Trauma and Possible Thoracolumbar Injury
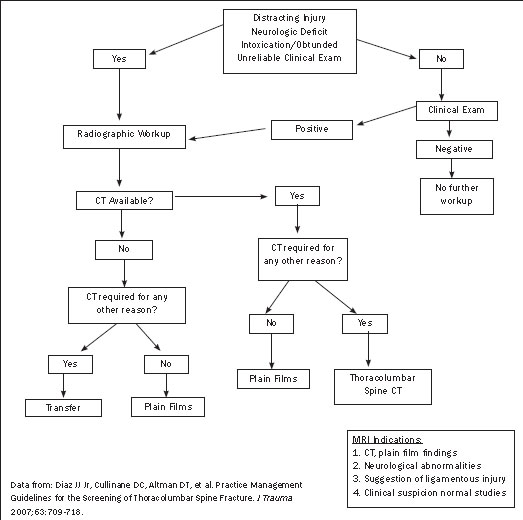
In 2007, Diaz et al proposed a set of clinical practice guidelines for the screening of patients with a suspected thoracolumbar spine fracture.41 (See Figure 2.) Articles were screened based on the following screening questions: Does a patient who is awake, non-intoxicated, and without distracting injuries require radiographic workup or solely a clinical examination? Does a patient with a distracting injury, altered mental status, or pain require radiographic examination? Does the obtunded patient require radiographic examination?41
Figure 2 illustrates their proposed algorithm for screening blunt trauma patients with potential TLS injuries in the emergency department. Any evidence of neurological deficit or spine tenderness on clinical examination, distracting injury, or altered mental status should warrant a radiographic workup. Patients without a significant mechanism of injury, distracting injury, abnormal clinical examination, and altered mental status may be cleared clinically without radiographic workup. It is clear that the role for plain films in the screening for TLS fractures in the emergency department is becoming less important with the widespread availability of CT. There are important details of fracture morphology that can be seen best by CT imaging as compared to plain radiographs, including posterior column injury, PLC integrity, and spinal canal compromise. CT is, therefore, the imaging modality of choice for patients with a concerning clinical examination, distracting injury, or altered mental status, especially if CT will be required for any other reason. If a CT scan is not immediately available, the patient may be transferred to the closest and most appropriate facility for continued care.
Many experts debate the question of whether or not a clinical exam is good enough to exclude spinal fractures. To answer this question, Inaba et al conducted a prospective observational study of 884 patients with blunt trauma injuries.42 The sensitivity and specificity of clinical examination for TL spine fractures were 48.2% and 84.9%, respectively, for all fractures, and 78.6% and 83.4% for those that were clinically significant. In addition, all clinically significant fractures that were initially missed by clinical examination were diagnosed on CT. Interestingly, in almost 40% of cases, although the physical examination was positive and was able to trigger imaging that ultimately found an injury, the examination localized the injury to an area where there was no injury. For this reason, any positive finding on clinical examination warrants full radiographic evaluation of the entire length of the spine and not just the area with tenderness or pain.
Yet another controversy in the screening of TLS fractures in the ED is whether patients with even a slight alteration in mental status (mild intoxication, lethargy, or concussion), who are often conversant and fully capable of reporting pain, should undergo imaging of their spine. Sava et al conducted a prospective data collection study of more than 3,000 blunt trauma patients. In his study, 166 patients had altered sensorium and were otherwise asymptomatic.43 Of these asymptomatic patients, 10 were found to have TLS fractures on typical radiographic imaging. Four of these patients required a brace, but none required surgery. This study illustrates that thoracolumbar spine fractures in blunt trauma patients with altered sensorium are often clinically silent, even when patients appear to be able to reliably report pain.43 This is why clinical examination as a stand-alone screening tool for evaluation of the TL spine in blunt trauma patients may be inadequate.
Role of High-Dose Steroids
The role of high-dose steroids (methylprednisolone) in the treatment of acute spinal cord injury has been a controversial topic. The exact mechanism through which steroids exert their effects remains uncertain; however, the leading theory is that steroids inhibit lipid peroxidation after spinal cord injury, which stabilizes the cell membrane.44-48 It is thought that the inhibition of lipid peroxidation likely minimizes ischemia and reduces necrosis.44-46 High-dose methylprednisolone also appears to decrease the release of inflammatory enzymes such as interleukins, prostaglandins, and thromboxanes systemically.
Three double-blind, randomized clinical trials conducted since 1977 have investigated the efficacy of methylprednisolone in the treatment of acute spinal cord injury: National Acute Spinal Cord Injury Studies (NASCIS) I, II, and III, published in 1984, 1990, and 1997.47,49,50
NASCIS I, published in 1984, found no improvement in neurologic recovery in the acute spinal cord injury patient after the administration of methylprednisolone.47 Animal data suggested that higher doses may have been necessary to be beneficial, thus leading to the NASCIS II trial in 1990.
NASCIS II compared the use of high-dose methylprednisolone (30 mg/kg intravenous bolus, then 5.4 mg/kg/h for 23 hours) with naloxone and placebo in 487 patients within 12 hours of sustaining an acute spinal cord injury.49 Overall, no difference in neurologic function was found among these groups. However, a subgroup analysis found that patients who had received methylprednisolone within 8 hours of injury had significantly greater motor function recovery at 6 weeks, 6 months, and 1 year compared with patients receiving methylprednisolone, naloxone, or placebo 8 hours after injury.49 High-dose steroids given after 8 hours actually caused significant worsening of neurologic scores. The authors also found an increased but non-significant risk of gastrointestinal bleeding and wound infection in patients treated with methylprednisolone.49 This study served to validate the practice of giving large doses of methylprednisolone to acute spinal cord injury patients despite its many methodological flaws.
In NASCIS III, 499 patients who sustained an acute spinal cord injury received a methylprednisolone bolus (30 mg/kg intravenously) within 8 hours of injury, then were randomized to receive methylprednisolone for 24 or 48 hours (at 5.4 mg/kg/h) or tirilazad mesylate, a steroid analog lipid peroxidation inhibitor without glucocorticoid effects, for 48 hours (2.5 mg/kg every 6 hours).50 In the subgroup of patients who received treatment within 3 hours of injury, there was similar neurological and functional benefit among the three groups. When treatment was initiated 3 to 8 hours after injury, the group receiving 48 hours of methylprednisolone saw significantly greater motor recovery at 6 weeks and 6 months and increased motor recovery at 1 year compared to the two other groups.50 Due to this, the authors concluded that patients who receive methylprednisolone within 3 hours of injury should continue therapy for 24 hours, while those who receive it 3 to 8 hours after injury should continue it for 48 hours, with the thought being that a longer duration may be necessary due to the greater extent of secondary injury suffered from the delayed treatment.50 The patients receiving 48 hours of methylprednisolone had higher rates of severe sepsis and pneumonia at 6 weeks, although mortality and other complications were similar between the groups.50 Thus, this landmark randomized, controlled trial conducted to date suggests that there may be a benefit to the use of high-dose methylprednisolone in acute spinal cord injury.
Despite the possible benefit of methylprednisolone for acute spinal cord injury patients within 8 hours from the time of injury, there are adverse side effects that must be addressed prior to use. Corticosteroids are known to increase blood glucose levels, which have been shown to lead to infectious complications such as those seen in the NASCIS studies (sepsis, pneumonia, and wound infections).47,49,50 In 2001, a landmark study by Van Den Berg et al published in the New England Journal of Medicine raised awareness about the importance of glycemic control in critically ill patients.51 These data have prompted stricter guidelines regarding blood glucose management in patients who are started on high-dose steroids following their traumatic injuries. Another important adverse side effect of high-dose steroid use is gastrointestinal bleeding. Patients who are started on a high-dose steroid regimen require prophylactic gastrointestinal (GI) protective agents, such as H2-blockers and proton pump inhibitors, to counter the potential erosive effects of high-dose steroid injections. Serial exams should also be performed to monitor for delayed GI bleeding and substantial internal blood loss.
In conclusion, use of high-dose methylprednisolone in spinal cord injury patients in the emergency department continues to be a topic of great controversy. The most recent ATLS guidelines published in 2008 state that there is insufficient evidence to support steroid use in spinal cord injury.52,53 Despite these guidelines, many spine surgeons continue to use high-dose steroids within 8 hours in patients who have suffered traumatic spinal cord injury.48,54-56 Based on the NASCIS II protocol, the suggested dose of methylprednisolone would be 30 mg/kg bolus over 15 minutes, then 5.4 mg/kg/h for 23 hours if started within 3 hours of injury, although consideration can be given to continuing treatment for 48 hours if started 3 to 8 hours after an acute spinal cord injury.49,50
Cauda Equina Syndrome and Conus Medullaris Syndrome
Conus medullaris syndrome (CMS) and cauda equina syndrome (CES) are complex neurological disorders manifesting as a myriad of symptoms such as back pain, unilateral or bilateral leg pain, paresthesias and weakness, perineum or saddle anesthesia, and rectal and/or urinary incontinence or dysfunction.57-61 Patients with CES typically present with symptoms of lumbosacral radiculopathies, whereas those with CMS present with symptoms consistent with spinal cord compression and dysfunction.62 Both syndromes may occur following traumatic injury to the thoracolumbar junction or the lumbosacral regions. Diagnosis is usually made from the patient's history and physical examination. If the diagnosis of CMS or CES is entertained, a thorough perineal neurological exam must be performed at the bedside, including a rectal examination, post-void residual sensory examination, and reflex examination (bulbocavernosus reflex, anal wink reflex). (See Table 4.) These are two "must-not-miss" diagnoses that require prompt diagnosis and treatment. Once the diagnosis is suspected on examination, evaluation and treatment are similar to what is done for other injuries of the TLS. CT imaging and surgical consultation are important, as well as consideration of steroid treatment, as noted above.
Table 4: Important Aspects of the Perineal Examination of Patients with a Potential Spine Fracture
|
Exam |
Technique |
Normal Findings |
|
Another important aspect of the perineal examination not listed above is sensory testing. |
||
|
Bladder function |
Measure post-void residual with either ultrasound or catheterization |
> 100 mL post-void residual (varies with treating hospital) |
|
Bulbocavernosus reflex |
Place finger in the rectum and squeeze the glans of the penis or clitoris (or apply traction on an indwelling catheter) |
Palpable rectal contraction |
|
Rectal tone |
Place finger in rectum |
Strong contraction of anal sphincter muscle |
|
Anal wink reflex (anocutaneous reflex) |
Gently stroking the peri-anal skin with cotton or gauze. |
Visible contraction of external anal sphincter muscle |
Disposition
In the absence of other serious injury, dispositions should be guided by the severity of the thoracolumbar spine injury. It is wise to include spine surgery consultants early in the decision-making process in most fractures. However, it may not always be necessary. All major TLS fracture/dislocations and burst fractures mandate emergency spine specialist consultation prior to admission. If a spine specialist is not available, the patient should be transferred to the nearest spinal cord injury center as soon as the patient is stabilized. If the patient has a spinal cord injury, consult with the spine surgery consultant for possible initiation of high-dose methylprednisolone therapy and possible emergent surgery.
Conclusions
Thoracolumbar spine fractures are common and can be difficult to diagnose in the emergency department. A careful and thorough workup of the blunt trauma patient with dedicated spinal imaging is necessary to identify these injuries. EPs can use the information provided in this article to improve the care provided to patients suspected of having TLS injuries.
References
1. Hu R, Mustard CA, Burns C. Epidemiology of incident spinal fracture in a complete population. Spine 1996;21:492–499
2. Price C, Makintubee S, Herndon W. Epidemiology of traumatic spinal cord injury and acute hospitalization and rehabilitation charges for spinal cord injuries in Oklahoma, 1988-1990. Am J Epidemiol 1994;139:37-47.
3. Gertzbein SD. Scoliosis Research Society. Multicenter spine fracture study. Spine 1992;17:528–540.
4. Denis F. The three-column spine and its significance in the classification of acute horacolumbar spinal injuries. Spine 1983;8:817–831.
5. Panjabi MM, Thibodieau LL, Crisco JJ, et al. What constitutes spinal instability? Ctin Neiirosurg 1988;(34):313-319.
6. James KS, Wenger KH, Schlegel JD, et al. Biomechanical evaluation of the stability of thoracolumbar burst fractures. Spine 1994;19:1731–1740.
7. Oxland TR, Panjabi MM, Southern EP, et al. An anatomic basis for spinal instability: A porcine trauma model. J Orthop Res 1991; 9:452–462.
8. Panjabi MM, White AA III. Basic biomechanics of the spine. Neurosurgery 1980;7:76-93.
9. White AA, Southwick WO, Panjabi MM. Clinical instability in the lower cervical spine: A review of past and current concepts. Spine 1976;1:25-27.
10. James KS, Wenger KH, Schlegel JD, et al. Biomechanical evaluation of the stability of thoracolumbar burst fractures. Spine 1994;19:1731–1740.
11. Oxland TR, Panjabi MM, Southern EP, et al. An anatomic basis for spinal instability: A porcine trauma model. J Orthop Res 1991; 9:452–462.
12. Panjabi MM, White AA III. Basic biomechanics of the spine. Neurosurgery 1980;7:76-93.
13. Whitesides TE. Traumatic kyphosis of the thoracolumbar spine. Clin Orthop 1977;128:78-92.
14. Holmes JF, Miller PQ, Panacek EA, et al. Epidemiology of thoracolumbar spine injury in blunt trauma. Acad Emerg Med 2001;8:866–872.
15. Tator CH, Koyanagi I. Vascular mechanisms in the pathophysiology of human spinal cord injury. J Neurosurg 1997;86:483–492.
16. Vaccaro AR, Lehman RA Jr, Hurlbert RJ, et al. A new classification of thoracolumbar injuries: The importance of injury morphology, the integrity of the posterior ligamentous complex, and neurologic status. Spine (Phila Pa 1976). 2005;30:2325-2333.
17. Joaquim AF, Fernandes YB, Cavalcante RA, et al. Evaluation of the Thoracolumbar Injury Classification System in thoracic and lumbar spinal trauma. Spine 2011;36:33-36.
18. Lee JY, Vaccaro AR, Lim MR, et al. Thoracolumbar injury classification and severity score: A new paradigm for the treatment of thoracolumbar spine trauma. J Orthop Sci 2005;10:671-675.
19. Rihn JA, Anderson DT, Harris E, et al. A review of the TLICS system: A novel, user-friendly thoracolumbar trauma classification system. Acta Orthop 2008;79:461-466.
20. Magerl F, Aebi M. A Comprehensive Classification of Thoracic and Lumbar Injuries. In: Thalgott JD, Webb JK, eds. AO ASIF Principles in Spine Surgery. Berlin Heidelberg, Germany: Springer-Verlag; 1998: 20-41.
21. Patel AI, Dailey A, Brodke DS, et al. Thoracolumbar spine trauma classification: The Thoracolumbar Injury Classification and Severity Score system and case examples. J Neurosurg Spine 2009;10:201–206.
22. Oner FC, Wood KB, Smith JS, et al. Therapeutic decision making in thoracolumbar spine trauma. Spine 2010;35;21S:S235–S244.
23. Whang PG, Vaccaro AR, Poelstra KA, et al. The influence of fracture mechanism and morphology on the reliability and validity of two novel thoracolumbar injury classification systems. Spine 2007;32:791–795.
24. Vaccaro AR, Andersson G. Spine Trauma Focus Edition: Summary. Spine 2006;31: S104.
25. Vaccaro AR, Baron EM, Sanfilippo J, et al. Reliability of a novel classification system for thoracolumbar injuries: The Thoracolumbar Injury Severity Score. Spine 2006;31:S62–S69.
26. Bono CM, Vaccaro AR, Hurlbert RJ, et al. Validating a newly proposed classification system for thoracolumbar spine trauma: Looking to the future of the Thoracolumbar Injury Classification and Severity Score. J Orthop Trauma 2006;20:567–572.
27. Harrop JS, Vaccaro AR, Hurlburt RJ, et al. Intrarater and interrater reliability and validity in the assessment of the mechanism of injury and integrity of the posterior ligamentous complex: A novel injury severity scoring system for thoracolumbar injuries. Spine 2006;4:118–122.
28. Koh YD, Kim DJ, Koh YW. Reliability and validity of thoracolumbar injury. Asian Spine Journal 4;2: 109-117.
29. Schweitzer KM, Vaccaro AR, Harrop JS, et al. Interrater reliability of identifying indicators of posterior ligamentous complex disruption when plain films are indeterminate in thoracolumbar injuries. J Orthop Sci 2007;12:437–442.
30. Cantor JB, Lebwohl NH, Garvey T, et al. Non-operative management of stable thoracolumbar burst fractures with early ambulation and bracing. Spine 1993;18:971–976.
31. Panjabi MM, Thibodieau LL, Crisco JJ, et al. What constitutes spinal instability? Ctin Neiirosurg 1988;(34):313-319.
32. Chow GH, Nelson BJ, Gebhard JS, et al. Functional outcome of thoracolumbar burst fractures managed with hyperextension casting or bracing and early mobilization. Spine 1996;21:2170–2175.
33. Danisa OA, Shaffrey CI, Jane JA, et al. Surgical approaches for the correction of unstable thoracolumbar burst fractures: A retrospective analysis of treatment outcomes. J Neurosurg 1995;83:977–983.
34. Krompinger WJ, Fredrickson BE, Mino DE, et al. Conservative treatment of fractures of the thoracic and lumbar spine. Orthop Clin North Am 1986;17:161–170.
35. Reid DC, Hu R, Davis LA, et al. The non-operative treatment of burst fractures of the thoracolumbar junction. J Trauma 1988;28:1188–1194.
36. Schnee CL, Ansell LV. Selection criteria and outcome of operative approaches for thoracolumbar burst fractures with and without neurological deficit. J Neurosurg 1997;86:48–55.
37. Shen WJ, Liu TJ, Shen YS. Non-operative treatment versus posterior fixation for thoracolumbar junction burst fractures without neurologic deficit. Spine 2001;26:1038–1045.
38. Shen WJ, Shen YS. Nonsurgical treatment of three-column thoracolumbar junction burst fractures without neurologic deficit. Spine 1999;24:412–415.
39. Marx JA, Hockberger RS, Walls RM, et al, (eds). Rosen's Emergency Medine: Concepts and Clinical Practice. Philadelphia, PA, 2006:1679-1681.
40. Heary RF, Bono CM. Conus medullaris injury after burst fractures. Top Spinal Cord Inj Rehabil 2002;8:21–40.
41. Diaz JJ Jr, Cullinane DC, Altman DT, et al; EAST Practice Management Guideline Committee. Practice Management Guidelines for the Screening of Thoracolumbar Spine Fracture. J Trauma 2007;63:709-18.
42. Inaba K, DuBose JJ, Barmparas G, et al. Clinical examination is sufficient to rule out thoracolumbar spine injuries. J Trauma 2011;70:174-179.
43. Sava J, Williams MD, Kennedy S, et al. Thoracolumbar fracture in blunt trauma: Is clinical exam enough for awake patients? J Trauma 2006;61:168-171.
44. Hall ED, Springer JE. Neuroprotection and acute spinal cord injury: A reappraisal. NeuroRX 2004;1(1):80-100.
45. Rozet I. Methylprednisolone in acute spinal cord injury: Is there any other ethical choice? J Neurosurg Anesthesiol 2008;20:137-139.
46. Dumont RJ, Verma S, Okonkwo DO, et al. Acute spinal cord injury, part II: Contemporary pharmacotherapy. Clin Neuropharmacol 2001;24:265-279.
47. Bracken MB, Shepard MJ, Collins WF, et al. A randomized controlled trial of methylprednisolone or naloxone in the treatment of acute spinal-cord injury. Results of the Second National Acute Spinal Cord Injury Study. N Engl J Med 1990;322:1405-1411.
48. Hawryluk GW, Rowland J, Kwon BK, et al. Protection and repair of the injured spinal cord: A review of completed, ongoing, and planned clinical trials for acute spinal cord injury. Neurosurg Focus 2008;25:E14.
49. Bracken MB, Collins WF, Freeman DF, et al. Efficacy of methylprednisolone in acute spinal cord injury. JAMA 1984;251:45-52.
50. Bracken MB, Shepard MJ, Holford TR, et al. Administration of methylprednisolone for 24 or 48 hours or tirilazad mesylate for 48 hours in the treatment of acute spinal cord injury. Results of the Third National Acute Spinal Cord Injury Randomized Controlled Trial. National Acute Spinal Cord Injury Study. JAMA 1997;277:1597-1604.
51. Van den Berghe G, Wouters P, Weekers F, et al. Intensive insulin therapy in the critically ill patients. N Engl J Med 2001;345:1359-1367.
52. Advanced Trauma Life Support for Doctors (ATLS). 8th edition. Chicago: American College of Surgeons Committee on Trauma; 2008.
53. Fix ML, Germann CA. ATLS update. Trauma Reports 2009;10:1-16.
54. Matsumoto T, Tamaki T, Kawakami M, et al. Early complications of high-dose methylprednisolone sodium succinate treatment in the follow-up of acute cervical spinal cord injury. Spine (Phila Pa 1976). 2001;26:426-430.
55. Hall ED, Springer JE. Neuroprotection and acute spinal cord injury: A reappraisal. NeuroRX 2004;1(1):80-100.
56. Rozet I. Methylprednisolone in acute spinal cord injury: Is there any other ethical choice? J Neurosurg Anesthesiol 2008;20:137-139.
57. Curtis LA, Dolan TS, Cespedes RD. Acute urinary retention and urinary incontinence. Emerg Med Clin North Am 2001;19:591-619.
58. Hussain SA, Gullan RW, Chitnavis BP. Cauda equina syndrome: Outcome and implications for management. Br J Neurosurg 2003;17:164-7.
59. Kostuik J. Medical realities of cauda equina syndrome secondary to lumbar disc herniation. Spine 2000;25:352.
60. Ahn UM, Ahn NU, Buchowski JM, et al. Cauda equina syndrome secondary to lumbar disc herniation. Spine 2000;25:1515-22.
61. Campana B. Soft tissue spine injuries and back pain. In: Marx JA, Hockberger RS, Walls RM, editors. Rosen's Emergency Medicine Concepts and Clinical Practice. St. Louis: Mosby; 2002:613-24.
62. Harrop JS, Hunt GE, Vaccaro AR. Conus medullaris and cauda equina syndrome as a result of traumatic injuries: Management principles. Neurosurg Focus 2004;15;16(6):e4.
Much attention has been given to injuries of the cervical spine, but injuries to the thoracolumbar region are actually more common. Because of the anatomy involved, these injuries are often accompanied by multiple serious injuries to other areas of the body and may be overlooked during resuscitation and stabilization.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
