Jury Awards Woman $200,000 After Hospital ED Sends Her Home to Deliver Her Dead 16-Week-Old Fetus
Correction: In the June 2011 issue of ED Legal Letter, the cover article, "Legal Issues Surrounding the Critically Ill Patient in the ED" listed Justin A. Eisenman, DO, MS as the only author. The article was co-authored by Gregory P. Moore, MD, JD, Attending Physician, Emergency Medicine Residency, Madigan Army Medical Center, Tacoma, WA. We apologize for the error.
Jury Awards Woman $200,000 After Hospital ED Sends Her Home to Deliver Her Dead 16-Week-Old Fetus
Court opinion and jury verdict create confusion and apprehension among emergency physicians regarding when EMTALA applies to pregnant women who are "having contractions" or who may be in "labor."
By Robert A. Bitterman, MD, JD, FACEP, Contributing Editor, President, Bitterman Health Law Consulting Group, Inc.
After a controversial court opinion and a highly charged emotional trial, a federal jury in Maine awarded Lorraine Morin $50,000 in compensatory damages and $150,000 in punitive damages against Eastern Maine Medical Center (EMMC) for failure to stabilize her prior to discharging her from the emergency department (ED) after a second-trimester miscarriage.
Facts of the Case Morin v. Eastern Maine Medical Center1
Ms. Morin was 16 weeks pregnant when she presented to the ED at EMMC at 4:30 a.m. with abdominal cramping but no vaginal bleeding. Her past history included two live births, one miscarriage, post-partum depression, and cervical cancer with cone biopsy. The emergency physician (EP) examined her, obtained an ultrasound, which revealed no fetal movement or cardiac activity, and consulted the on-call obstetrician.
The obstetrician examined Ms. Morin at 5:25 a.m., noting "lower abdominal pain and discomfort like Braxton-Hicks contractions," no leaking fluids, and a cervix that was neither dilated nor effaced. His repeat ultrasound confirmed intrauterine fetal demise. He recommended that Ms. Morin go home, take acetaminophen/codeine for her discomfort, and follow up in the morning with her private obstetrician.
The patient didn't want to go home, so she pleaded with the EP to admit her until she delivered the dead fetus. The EP again called the obstetrician, who told him that Ms. Morin's cervix was not ready for delivery, so he discharged her over her and her fiancé's "vehement protests."1 At around 9 p.m. later that day, Ms. Morin delivered the dead fetus in her bathroom at home.
Subsequently, Ms. Morin sued EMMC for damages and emotional distress, alleging the hospital failed to stabilize her emergency medical condition (EMC) before discharge in violation of the Emergency Medical Treatment and Active Labor Act (EMTALA).1,2
The Federal District Court's Opinion
The medical center asked the federal court to dismiss the lawsuit, claiming that EMTALA did not apply to her care because she did not have an EMC as defined by the law.
EMTALA has two definitions for an EMC. First, a general definition that applies to any ED patient, but Ms. Morin did not argue that she had an EMC under this definition.3 Instead, she claimed she had an EMC under EMTALA's second definition, a special provision for pregnant women, which holds that:
1) The term "emergency medical condition" means:
(B) with respect to a pregnant woman who is having contractions:
(i) that there is inadequate time to effect a safe transfer to another hospital before delivery; or
(ii) that transfer may pose a threat to the health or safety of the woman or the unborn child.4
Or explicitly in her case, that she was a pregnant woman who was having contractions and that her discharge ("transfer") posed a threat to her health or safety and, therefore, the hospital had a duty to "stabilize" her, which under the law requires the hospital to deliver the child and the placenta.5 Thus, she claimed because she had an EMC under the pregnant women provision of the statute, the hospital had to keep her until she expelled the dead fetus and the placenta. (Note that under EMTALA, all discharges from the ED are legally defined as "transfers.")6
Was Ms. Morin in "True Labor" and, Thus, Having an EMC?
EMMC tendered a number of arguments for why Ms. Morin was not suffering an EMC under EMTALA and, thus, it had no duty to "stabilize" her in the manner required by EMTALA. The hospital's main arguments were:
Ms. Morin was not diagnosed as being in labor; therefore, EMTALA's obligation to stabilize her never applied. EMMC argued that labor refers to childbirth of a viable baby and not to miscarriage of a non-viable (less than 20 weeks) fetus.
The court was distinctly perturbed at "EMMC's disquieting notion that EMTALA would allow hospital emergency rooms to treat women who do not deliver a live infant differently than women who do."1 It responded, first, that the plain language of EMTALA extends protection to any "pregnant woman who is having contractions;"4 second, nothing in the statute or regulations depends on the gestational age or viability of the fetus; and third, other courts have ruled that EMTALA protections apply regardless of viability.7 The court did not believe "Congress ever intended such a harsh and callous result for women who, like Ms. Morin, were carrying a non-viable fetus;" therefore, the court concluded that EMTALA's protections extended to pregnant women regardless of the fetus's viability.
In response, the hospital claimed that, "whether a pregnant woman is experiencing an emergency medical condition is not simply a legal determination, divorced from how physicians define and use terms like 'labor' and 'contractions,'"1 trying to convince the court that the practice of medicine didn't consider miscarriages to be "labor" or "contractions," as contemplated by the statute.
The court noted that CMS' regulations state that:
"A woman experiencing contractions is in true labor unless a physician, certified nurse-midwife, or other qualified medical person ... certifies that, after a reasonable time of observation, the woman is in false labor."8,9,10
And Ms. Morin argued since there was no certification of false labor in the medical record, the assumption was that she was in true labor, which she equated to having an EMC. The hospital countered that there could have been no certification by a physician that the plaintiff was "in false labor" because, medically, she would not have been considered by a physician to be in "false labor" (much less labor), since medical doctors do not define contractions at early stages of pregnancy as "labor." (The hospital seemed to miss the fact that the obstetrician documented in the medical record "discomfort like Braxton-Hicks contractions," which, by definition, are false labor.)
The court disagreed, stating bluntly for the first of many times in the case, that the medical practitioners' definition of an EMC was irrelevant under EMTALA; it was the legal definition that controlled for purposes of compliance with the law.1 It noted that regardless of what the physician may diagnose, the regulation says that a pregnant woman who is experiencing contractions is in true labor unless the hospital certifies that she is in false labor.
This is where the court started wavering off the path of the statutory construction of EMTALA.
First, the word "labor" does not appear anywhere in the statutory definition of an EMC in a pregnant woman.4 Thus, whether a pregnant woman is in "labor," "early labor," "active labor," or has "false labor" is absolutely irrelevant for legally determining whether she has an EMC under EMTALA.11
Second, in 1989, Congress amended the law, changing the definition of an EMC in pregnant women to specifically remove the word "labor" from the definition.12 Thus, no one can reasonably assert that whether the woman is in true labor or false labor has anything to do with the determination of whether an EMC is present in a pregnant woman. This is clearly borne out every day in real medical practice: Hospital labor and delivery units routinely send women home in early labor when no complications are found, and it is determined safe to allow them to remain at home for a period of time until labor progresses further and warrants hospitalization for observation or delivery.
Third, even if the hospital does certify the pregnant woman with contractions to be in "false labor," that alone is not sufficient to rule out an EMC under the pregnancy definition of an EMC in EMTALA. Review the definition again: "The term 'emergency medical condition' means with respect to a pregnant woman who is having contractions:
(i) that there is inadequate time to effect a safe transfer to another hospital before delivery, or
(ii) that transfer may pose a threat to the health or safety of the woman or the unborn child.4"
Regardless of the certification of false labor, the hospital must still comply with the statutory requirement that it be safe to transfer her to another hospital before delivery AND that the transfer, or discharge to home in Ms. Morin's case, not pose a threat to her health and safety. (Since the fetus was already dead, there was no issue with the health and safety of the unborn child in this case.) Thus, any time a physician declares the woman in false labor, he or she must ALSO determine and opine that the discharge will not pose a threat which is why the determination of whether a woman is in "true labor" or "false labor" is legally irrelevant for determining compliance with EMTALA.13
In other words, there are three elements to the pregnancy definition of an EMC under EMTALA: the existence of pregnancy, the presence of contractions, and the threat to the health and safety of the woman and unborn child related to transfer or discharge.
The court understood that the relevant question for Ms. Morin's failure to stabilize claim was not whether Ms. Morin was in labor, but whether she was "experiencing" or "having contractions;" however, it seemed to allow that "true labor" was an EMC that required stabilization, and permitted testimony on this issue at trial.1
Did the Hospital Diagnose Ms. Morin to Have an EMC?
EMMC's primary argument was really the crux of the case. It contended that before it could be held liable for failure to stabilize Ms. Morin's EMC, it must first determine that the EMC exists. In this case, that means it must have made the actual determination that all three elements of the pregnancy definition were present. The hospital essentially conceded the first two elements, pregnancy and contractions, so the sole key issue was whether it determined and knew that the discharge of Ms. Morin posed a threat to her health and safety.1,14 (Interestingly, the hospital never offered one very strong argument that Ms. Morin was NOT pregnant! The fetus was dead; therefore, at the time of her ED visit, she was no longer "pregnant," which, by definition, means carrying a developing embryo or fetus.)
The federal appellate courts have uniformly held that "determining the EMC exists" is an actual knowledge requirement, meaning that the hospital must subjectively, actually know/make the diagnosis that the EMC is present before it has a duty to stabilize that EMC.15 Therefore, at trial, plaintiffs have the burden of proving the hospital had actual (subjective) knowledge that such a threat existed. Not that the hospital or physicians "should have known" a threat existed (the malpractice standard), or that they considered "threats" in their differential diagnosis ... but that the hospital actually knew and made that determination.16,17
Although, unfortunately, documentation is key; if hospitals don't really understand EMTALA's scheme for pregnant patients, then it is unlikely and very difficult for them to properly document the necessary determinations in the medical record to reflect its considerations of the EMTALA issues before discharging the woman. Furthermore, this concept of proving subjective knowledge/actual knowledge is difficult for lay persons to comprehend during a trial.
The court in Morin agreed with the federal appellate courts: Ms. Morin would have to prove at trial that EMMC determined an EMC existed and knew that her discharge may pose a threat to her health and safety.1
However, the court viewed the "may pose a threat" language as a very low hurdle, and required only a "showing of possible threat" or "the presence of a possible threat of harm" to the health and safety of the mother.1,18 Furthermore, in keeping with the seminal civil case on this point, Burditt v. HHS, the standard for "may pose a threat" under EMTALA "does not require proof of a reasonable medical probability that any threat will come to fruition."19 The court noted that Congress rationally required less of a showing of probability and severity of harm for pregnant women than the general population under its emergency definition.19
Thus, the judge ruled that it was "a question of fact" and that the jury would decide whether EMMC subjectively knew that the discharge of Ms. Morin may pose a threat to her health and safety.1
The court did not mean to suggest that the discharge of every pregnant woman who is having contractions "may pose a threat to her health," but it did state, "Instead, here, where the hospital discharged a woman who is 16 weeks pregnant, who has just been informed her fetus is dead, who is having ongoing contractions, and who is in an extreme state of agitation and distress, the Court readily concludes that the Plaintiff presents sufficient evidence to allow the matter to proceed to trial."1
The Court concluded that if Ms. Morin was pregnant and having contractions, EMMC was obligated to allow her to remain at the hospital until she delivered the fetus and the placenta, unless her discharge would not pose a threat to her health or safety.1
Jury Trial and the Verdict
The trial should have been limited to whether the hospital had "actual knowledge" of the EMC (i.e., did it subjectively know that Ms. Morin was pregnant, had contractions, and that discharge may pose a threat to her health and safety). If it did have actual knowledge of the three elements of an EMC, the case was over, since the only way it could stabilize the EMC was by delivery of the fetus and the placenta, and that obviously didn't happen. If it didn't diagnose Ms. Morin with an EMC (i.e., it didn't know that discharge would pose a threat to her health and safety), the case was over this way too, since then, EMTALA would no longer apply and the hospital would not have had a duty to stabilize her by keeping her until she delivered the fetus.
Therefore, the only evidence admitted at trial should have been evidence that directly addressed exactly what the hospital had determined and what it knew at the time it discharged Ms. Morin.
Evidence from the medical record, testimony by the participants, and expert opinion bearing only on what was known to the hospital at that time was relevant.
The court acknowledged, correctly, that under EMTALA, the case was not about the standard of care. Yet, the case really became a standard-of-care exposé and the result was most likely due to the jury's outrage at the alleged callousness of the hospital regarding the patient's request for admission, inadequate pain control, "extreme state of agitation and distress," and lack of grief counseling (that would have been available had she been admitted), "delivery of her fetus on a cold, hard tile floor in her bathroom at home," and the fact that the hospital staff clearly missed some historical risk considerations that it shouldn't have in its decision-making process to send the patient home, such as a previous C-section or past history of post-partum depression; the fact that she lived an hour and half from the hospital, so it wouldn't be easy to come back if she developed complications; lack of attempt to call the patient's own obstetrician, despite her requests, etc.
The case really wasn't about law; it was more about raw human emotion and lack of compassion or concern for a fellow human being in a time of severe emotional distress (as the $150,000 in punitive damages attests). Did the hospital recognize her needs and concerns? Did it adequately listen/communicate with her on the relevant issues and illicit the necessary information and circumstances to make a reasoned decision? It is true that EDs send a significant number of these women home but also admit a significant number depending upon those circumstances.
Additionally, when sending someone home over the vehement objections of the family and of a patient who just lost a baby, the physicians and hospital had better be right and communicate and document their reasoning profusely. Couple anger with an adverse outcome and you breed litigation.
Undoubtedly in this case, the EP, the on-call obstetrician, the nurses, and the hospital had no idea of the EMTALA-mandated criteria they were required to use to judge whether the patient had an EMC under the law, and whether it was safe or reasonable to send the patient home under those criteria. Proper documentation, coupled with knowledge of the low threshold standard under the law, would have markedly improved the chances of the hospital avoiding the adverse financial and public-relations outcome of this case.
Interestingly, post verdict, and after the judge denied the hospital's motion for a new trial, a representative of the hospital commented that EMMC was confident that the appellate court would find that the hospital's treatment of Ms. Morin was consistent with long-standing national practices.20 "Long-standing national practices" are irrelevant if they don't comply with EMTALA.
Comment
One can understand the jury's decision, but, in truth, it was likely based more on their belief in the standard of care (and caring) that should have been provided to Ms. Morin than on the nuances of EMTALA. But the distinction is highly important because, if otherwise, it would turn every decision on whether a patient has an EMC into an EMTALA violation instead of a standard-of-care issue, which is wholly removed from the actual intent of the law.
It's no different than if a 55-year-old smoker who presents with chest pain, is diagnosed with heartburn, but dies of an acute myocardial infarction a few hours after leaving the ED. The EP may have misread the EKG, failed to obtain the right history, which would have pointed to ischemic heart disease, or misinterpreted the diagnostic enzyme studies, but those are what he "should have known" or "should have done" standard-of-care issues a failure to diagnose claim under state law, not an EMTALA claim for failure to stabilize the patient.
Similarly, assume a 3-month-old infant with a high fever diagnosed with a "viral syndrome" is discharged from the ED to follow-up with the pediatrician in the morning, but returns with obvious sepsis before the appointment. A plaintiff's attorney can argue that the EP should have recognized the sepsis, should have started antibiotics, should have ordered more diagnostic studies, or should have admitted the child, but he can't argue that the hospital failed to stabilize the sepsis, because the hospital didn't know the child was septic. It did not determine that the child had that particular EMC, or any other not-yet-diagnosed EMC.
Furthermore, including the possibility of sepsis in the differential diagnosis, considering the diagnosis of sepsis (such as evidenced by sending off a blood culture), being concerned about the potential for the diagnosis, or even having expert testimony certain that the physician should have determined the child was septic are all irrelevant for purposes of EMTALA.16 The issue is whether the physician/hospital subjectively actually knew actually determined that fact, and it should be readily apparent by the medical record and the discharge of the child to follow-up the next morning that it did not.
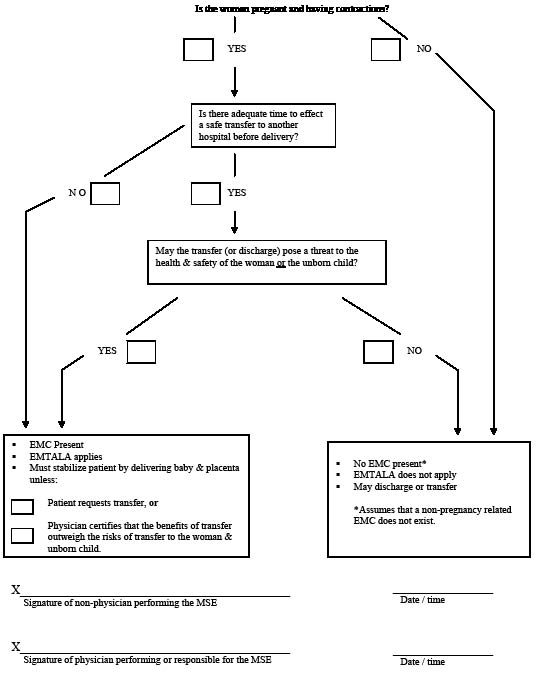
Figure 1: Obstetrics Medical Screening Exam Compliance with EMTALA
Call it an error in judgment or medicine delivered below the standard of care, but it is not a violation of EMTALA, and the physician/hospital cannot be held liable for failure to stabilize an EMC that they didn't actually know existed. Liable under state law standards of care, yes, but not liable under EMTALA.
Conclusion
The EMTALA statute, not this court or this jury's decision, long ago required hospitals and physicians to learn, understand, and apply the legal lingo required by the law to evaluate and process pregnant women with contractions through their EDs and labor and delivery departments. Pregnant women are a protected class under EMTALA and, as such, there is a very low threshold for error under the law. The care of these individuals will be highly scrutinized by the government enforcement agencies, as well as the courts.
Moreover, probably no other clinical scenario generates more emotion or attracts more adverse publicity, government retribution, and/or litigation than the perception that a hospital or a physician mistreated or denied care to a pregnant woman. This is one area of hospital-based practice in which being legally correct simply isn't enough. The evaluation of obstetric patients must be not only medically appropriate and lawful but also must be perceived to be in the best interests of the patient. Cultivating and projecting an attitude of genuine advocacy for the patients' interests at all times is paramount. Perception is the only reality.
Hospitals should adopt a risk-management approach to evaluating pregnant women. They should implement policies and procedures that maximize conformity to standard medical practice, ensure compliance with the law, and minimize regulatory and liability risks. This process includes educating all staff involved, conducting ongoing quality assurance and performance monitoring, and ensuring appropriate documentation. Checklists, forms, and algorithms must imbed knowledge of the law, but they must also be practical, user-friendly tools that guide physicians and hospital staff down the proper pathways, even if they don't understand the legal issues or their implications.
The Maine federal court's rulings and the jury's verdict really changed nothing. They did, once again, highlight the fact that many hospitals have yet to comprehend the broad scope of EMTALA's reach and its significant impact on the practice of medicine.
As the Morin court noted in quoting a 1991 appellate court opinion, "EMTALA's statutory definition renders irrelevant any medical definition."19 Hospitals have been quite slow to truly accept the fact that this statute forever changed emergency medicine to be a practice governed by law, and no longer a practice governed primarily by acceptable standards of care.
References
1. Morin v. Eastern Maine Med. Ctr., No. CV-09-258-B-W, 2010 U.S. Dist. LEXIS 76292 (D. Me. Jul. 28, 2010).
2. 42 USC 1395dd
3. 42 USC 1395dd(e)(1)(A). The term "emergency medical condition" means a medical condition manifesting itself by acute symptoms of sufficient severity (including severe pain) such that the absence of immediate medical attention could reasonably be expected to result in-- (i) placing the health of the individual (or, with respect to a pregnant woman, the health of the woman or her unborn child) in serious jeopardy, (ii) serious impairment to bodily functions, or (iii) serious dysfunction of any bodily organ or part.]
4. 42 USC 1395dd(e)(1)(B).
5. 42 USC 1395dd(e)(3)(A).
6. 42 USC 1395dd(e)(4).
7. Barrios v. Sherman Hosp., No. 06 C 2853, 2006 WL 3754922 (N.D. Ill. 2006); Thompson v. St. Anne's Hosp., 716 F. Supp. 8 (N.D. Ill. 1989).
8. 42 CFR 489.24(b). http://edocket.access.gpo.gov/cfr_2010/octqtr/pdf/42cfr489.24.pdf. See also: CMS State Operations Manual (SOM), Appendix V Interpretive Guidelines – Responsibilities of Medicare Participating Hospitals in Emergency Cases EMTALA, Effective May 29, 2009, with revision 60, effective July 16, 2010. Available at: http://www.cms.gov/manuals/Downloads/som107ap_v_emerg.pdf.
9. CMS Ref: S&C-02-14, January 16, 2002. Certification of False Labor-EMTALA. http://www.cms.gov/SurveyCertificationGenInfo/downloads/SCLetter02-14.pdf.
10. CMS Ref: S&C-06-32, September 29, 2006. Revisions to Special Responsibilities of Hospitals under EMTALA. (The definition of "Labor" is revised to expand the types of health care practitioners who may certify false labor.) http://www.cms.gov/SurveyCertificationGenInfo/downloads/SCLetter06-32.pdf.
11. Richard v. Univ. Med. Ctr. of S. Nevada, No. 2:09-cv-0244-LDG-PAL (D. Nev. Mar. 21, 2011).
12. Pub. L. No. 101-239 § 6211(h)(2) (1989). See also Joan M. Stieber & Linda J. Spar, EMTALA in the '90s Enforcement Challenges, 8 HEALTH MATRIX 57 (1998).
13. 71 Fed Reg 48096 (August 18, 2006).
14. Morin v. Eastern Maine Med. Ctr., No. CV-09-258-B-W, ORDER ON MOTIONS IN LIMINE (D. Me. Oct. 12, 2010.)
15. E.g., Baber v. Hospital Corp. of America, 977 F.2d 872 (4th Cir.1992); Vickers v. Nash Gen. Hosp., Inc., 78 F.3d 139 (4th Cir.1996); Brenord v. Catholic Med. Ctr. of Brooklyn and Queens, Inc., 133 F. Supp. 2d 179 (E.D.N.Y. 2001);Heimlicher v. Steele, 615 F. Supp. 2d 884 (N.D. Iowa 2009).
16. E.g., Urban v. King, 43 F.3d 523 (10th Cir.1994); Bryant v. Adventist Health System/West, 289 F.3d 1162 (9th Cir. 2002).
17. Bitterman RA. Providing Emergency Care Under Federal Law: EMTALA. Published by the American College of Emergency Physicians, January 2001; Supplement 2004. 2nd printing. (CMS does not accept the appellate courts' interpretation of the statute regarding the actual knowledge requirement. The government will examine the adequacy of the physician's judgment retrospectively regarding whether the decision to discharge or transfer was correct within reasonable medical probability.)
18. Burditt v. U.S. Dep't of Health and Human Services, 934 F.2d 1362 (5th Cir. 1991). See also Torretti v. Main Line Hospitals, Inc (d/b/a Paoli Mem'l Hosp.), 580 F.3d 168 (3rd Cir. 2009).
19. Bangor Daily News (Maine, March 29, 2011).
After a controversial court opinion and a highly charged emotional trial, a federal jury in Maine awarded Lorraine Morin $50,000 in compensatory damages and $150,000 in punitive damages against Eastern Maine Medical Center (EMMC) for failure to stabilize her prior to discharging her from the emergency department (ED) after a second-trimester miscarriage.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
