A Wide Tachycardia of Uncertain Cause
ECG Review
A Wide Tachycardia of Uncertain Cause
By Ken Grauer, MD, Professor Emeritus in Family Medicine, College of Medicine, University of Florida. Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
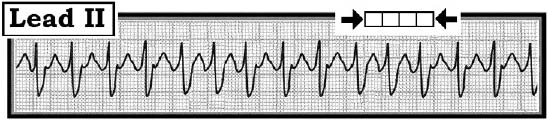
Scenario: The lead II rhythm strip shown above was obtained from a woman with new-onset palpitations. How would you interpret this tracing? How certain are you of your answer? Clinically — what would you do?
Interpretation: The rhythm is fast and fairly (but not completely) regular. The QRS looks to be wide (i.e., more than half a large box) and there are no definite P waves. Thus, this appears to be a wide complex tachycardia (WCT) of uncertain etiology. This case, therefore, highlights many of the points emphasized in last month’s ECG Review (A WCT with P’ Waves?, October 15, 2011, page 152).
The key piece of information that we have not been told is whether the patient in this case is hemodynamically stable. If she was having chest pain, shortness of breath, mental confusion, and/or was hypotensive at the time this tracing was recorded — then immediate synchronized cardioversion would be indicated as the most time-efficient means for converting her out of a potentially life-threatening tachyarrhythmia. On the other hand, if the patient was alert, normotensive and asymptomatic, then there is at least a moment of time to devote to rhythm diagnosis.
By far, the most common cause of a regular WCT of uncertain etiology is ventricular tachycardia. That said, QRS widening with supraventricular tachycardia may result from either preexisting bundle branch block and/or aberrant conduction. Obtaining a 12-lead ECG during tachycardia may prove invaluable for suggesting atrial activity in other leads, as well as providing a look at QRS morphology. In this case, QRS morphology during the WCT was identical to that seen in previous tracings when this patient was in sinus rhythm. As a result, an IV bolus of adenosine was given. The result (shown below in Figure 2) confirmed that the rhythm was atrial flutter with 2:1 AV conduction, with QRS widening due to the preexisting conduction defect. Retrospectively in Figure 1, one can see regular negative deflections at about 300/minute occurring just before and just after the T wave. This case highlights how definitive rhythm diagnosis is not always known at the time treatment is begun.
The lead II rhythm strip shown above was obtained from a woman with new-onset palpitations. How would you interpret this tracing? How certain are you of your answer? Clinically what would you do?Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
