Traumatic Amputations
Traumatic Amputations
Authors:
George C. Willis, MD, Instructor, University of Maryland School of Medicine, Attending Physician, Mercy Medical Center, Baltimore, MD.
Joshua Reynolds, MD, Research Fellow, Clinical Instructor, Department of Emergency Medicine, University of Pittsburgh.
Peer Reviewer:
Steven M. Winograd, MD, FACEP, New York Community Hospital, ED Attending, New York-Presbyterian Healthcare System, Weill Medical College of Cornell University, Brooklyn, NY.
Author's Note
When I was 6 years old, I had a bicycle accident that amputated the distal tip of my second, third, and fourth fingers on my left hand at the DIP joint. I remember that day like it was yesterday, even though it was more than 25 years ago, because it was such a tragic day in my life. One of the things that I remember the most is the conversation the ED physician had with my parents informing them that my fingers could not be reattached because my child-size fingers were too small. Now, after 25 years of coping with my "stubs," as I researched and wrote about this topic, I jokingly realize that my professional basketball career was ruined by faulty medical knowledge.
The purpose of this article is to inform emergency providers of the proper care and management of traumatic amputations to avoid stories like my own. Care for a patient who undergoes an amputation is often complicated and is time-sensitive. A lot of thought goes into whether replantation is attempted or not, but those decisions are reserved for the replantation team. The role of the emergency provider is to expediently evaluate the patient and prepare him or her for care by the replantation team. By assuming that replantation will occur, especially in children, treatment will be expedient and efficient and lead to the best results for the patient, even if the replantation ultimately cannot be carried out. The majority of the time, the replantation is attempted and often leads to a functional outcome very pleasing to the patient. I only wish my parents had this information 25 years ago.
Introduction
Traumatic amputations rarely occur in scenarios other than combat situations; however, when they do occur, they are emotionally and physically debilitating. Success in replantation depends on appropriate and time-sensitive care of the patient during the initial presentation to a health care facility, usually the emergency department (ED). It is the responsibility of the emergency care provider to know how to manage amputations and initiate proper care that will lead to a satisfactory outcome.
Pathophysiology
The majority of upper-extremity injuries are sustained in occupational settings, such as those involving power tools or machinery. Among children, upper-extremity injuries are caused by power tools, but also by getting caught between opposing surfaces, such as doors and doorframes.1 Lower-extremity amputations are usually the result of high-energy motor vehicle collisions (often sustained by motorcyclists) or occupational incidents.2 Amputations affecting body parts other than the extremities are usually the result of animal attacks, self-infliction, or falls.
Guillotine amputations often have better outcomes because of their straight edges, which are amenable to surgical repair. Avulsions and crush amputations are much more difficult to repair because of extensive tissue damage; unfortunately, these are the most common types of amputations.3 Avulsion amputations are severe injuries in that the structures are separated from portions of the amputation. Nerves usually tear from the proximal stump, whereas vessels tear from the distal amputated portion. Tendons separate from the distal portion, and bony structures either fracture or avulse from the joint, causing disarticulation.4
A partial amputation has some amount of tissue connecting the proximal and distal portions: vasculature (arteries and veins), connective tissue (muscles and tendons), or nerves. Even if only a small bridge of skin exists as the lone connection, it is still considered a partial amputation. The majority of the connecting tissue will likely remain functional as long as it is intact. A complete amputation has no tissue connecting the amputated portion to the body. All of the connective tissue, nerves, and vasculature have been severed and rendered nonfunctional in the amputated portion. When the vasculature is transected, it has a propensity to retract into the stump and to vasospasm, decreasing or ceasing blood flow through that vessel.5,6 On the other hand, partial amputations may contain vessels that have been only partially severed, which can result in continued hemorrhage as blood flow continues through the defect.
Prehospital Considerations
The adage "life over limb" accurately describes the priorities in the prehospital care of traumatic amputations.7,8 The prehospital care provider is tasked with caring for not only the injured patient but also the amputated part. Stabilization of life-threatening injuries, control of hemorrhage, and appropriate storage of the amputation are paramount in the prehospital care of a patient with an amputation.
Hemorrhage is the primary immediate complication of traumatic amputations. Direct pressure and elevation are always the preferred methods of controlling hemorrhage in the prehospital setting. Blind clamping or tying of tissues is not recommended to avoid damage to the tissue that may be needed for surgical repair.9 The tourniquet has been a controversial adjunct in prehospital medicine. Traditional teaching holds that the tourniquet is to be used only as a last resort or life-saving measure. A shift away from this axiom to more liberal use has actually increased the survival of critically injured patients.5,10-12 Tourniquets rapidly correct compressible hemorrhage and can be used safely during patient transport.5,12 There are many different models and versions, but each is designed to be applied easily and to multiply the force of application; many can be applied with one hand. A tourniquet may be left in place for up to 2 hours without causing significant tissue damage to the affected limb. Prolonged use can cause tissue ischemia and necrosis and, ultimately, decrease the likelihood of replantation success.8
The prehospital care provider should record the exact time of amputation because "ischemia time" is the major determinant in candidacy for replantation. If a patient is entrapped at the scene, the amputated part should be transported to the receiving facility ahead of the patient for appropriate storage. All amputated parts should be packaged properly and transported, no matter how damaged they appear, because some skin and tissue may still be usable for grafting.13-15 Since ischemia time is so vital to replantation, both the patient and amputated part should be transported, by air if necessary, to the nearest microvascular replantation center unless other injuries dictate transport to a closer trauma center.
Tissue that suffers prolonged ischemia time is prone to contractures, muscle loss, and nerve injury, which adversely affect its functional recovery. Because tissue can survive longer at cooler temperatures, there is a distinction between "warm ischemia time" and "cold ischemia time." Decreasing the tissue temperature decreases the tissue metabolic and oxygen demand, prolonging the amount of ischemia the tissue can withstand. Digits have the longest ischemia times (12 hours warm; 24 hours cold), whereas limbs have greater muscle mass and shorter ischemia times (6 hours warm; 12 hours cold). Efforts to cool an amputated part must never result in the freezing of tissue. Tissue freezing is more damaging at the cellular level than keeping an amputated part warm.9,16,17 Frostbite injuries will lessen the likelihood of replantation success.
The appropriate care and packing of an amputated part is very specific. Remove gross contaminants or foreign material and gently irrigate with saline solution. Do not use alcohol, iodine, formaldehyde, or other cleaning solutions. Wrap the part in saline-moistened gauze and place it in a sealed plastic bag or container. Then store the container in a water/ice slurry. Do not place the amputated part directly in contact with ice or allow it to freeze.7,9,17-21 Irrigate the stump with saline and cover it with saline-moistened gauze. Splint the stump and keep any partial amputations in anatomic position to avoid further injury.9,22
Emergency Department Management
The patient's arrival at the ED is usually chaotic, as patients with an amputation can be distraught. They may be agitated and combative, flailing a partial amputation around and, thus, making their injury worse. The emergency physician must maintain order because an efficient, timely, and thorough evaluation is necessary if any hopes of replantation are possible. Try to calm the patient with verbal de-escalation. If necessary, use chemical restraints with sedative agents. The use of physical restraints is not recommended unless all other means are unsuccessful, because it may worsen the injury.
Obtain a thorough history, giving special attention to the mechanism of the injury, other injuries sustained, timing of the injury, care of the stump and the amputated portion, method of transport of the amputated portion, the patient's occupation, hand dominance, if pertinent, allergies to medications, and tetanus status. This information is important for the surgical team to assess the feasibility of replantation. The patient may be too distracted emotionally by the amputation to give an adequate history or cooperate with the physical exam. If the patient, especially a child, is unable to provide a history, use other sources of information, such as parents, emergency medical services (EMS) providers, or witnesses.23
The initial assessment of the patient with a traumatic amputation is no different from that for any other trauma patient. Shock is associated with worse outcomes and must be addressed before any further interventions are performed. Unstable patients require resuscitation prior to addressing the amputation. Place at least one large-bore IV catheter into the unaffected limb and infuse isotonic crystalloid to maintain a euvolemic state. Blood products may be necessary, depending on the severity of the injuries.
If excessive bleeding becomes a problem, establish hemorrhage control. In most cases, a complete amputation will not cause life-threatening hemorrhage because the transected arteries retract proximally and induce vasospasm, which clamps off the artery. In most cases, arteries that are partially transected in partial amputations tend to continue to bleed. Hemostasis can usually be achieved by elevating the stump above the level of the heart and applying direct pressure to the source of bleeding. Never cauterize, tie off, suture, or clamp vessels in an attempt to control bleeding because this can cause damage that may make replantation less successful. If direct pressure is insufficient to control the bleeding, placing a blood pressure cuff proximal to the wound may be useful. Inflate the cuff until hemostasis is achieved, but avoid exceeding 30 to 40 mm Hg above the systolic blood pressure. This method can be a used as a temporizing measure to maintain hemostasis until the replantation team can evaluate the patient; however, do not use it for extended periods (i.e., for more than 2 hours) because the stump tissue can become devitalized. Reserve the use of tourniquets as a last resort.
A complete head-to-toe examination to evaluate for other injuries is necessary to rule out life-threatening injuries. Prioritize and address life-threatening injuries early before evaluating the amputation.3,23
Once life-threatening injuries have been identified and addressed, focus attention on the amputation. Evaluation of the wound should be exhaustive. With partial amputations, pay special attention to the viability of the tissues involved, cleanliness of the wound, excessive bleeding, and functional ability of the affected portion. Complete amputations or avulsion injuries should have the proximal portion, or stump, evaluated for viability, cleanliness of the wound, and excessive bleeding. The amputated portion requires similar evaluation, especially if replantation is feasible. Irrigate both the amputated portion as well as the stump with saline rinse to wash away any debris and contaminants. Avoid scrubbing wounds and using cleansing agents other than saline irrigation, as undue damage may occur to the tissue, making replantation more difficult.
A functional assessment of the affected area should involve a neurologic and vascular examination. Perform a sensory examination of the stump in a complete amputation or of the entire affected portion in a partial amputation. Intact sensation suggests minimal nerve damage and decreases the need for the replantation team to explore the tissue in the operating room to search for damaged nerve tissue.23 Motor function should be evaluated as much as possible. In avulsion injuries, tendons can be separated from their proximal attachments, so reattachment during replantation is necessary to retain function. Evaluate vascular structures by gross inspection, but, again, do not tag or clamp any of the structures. Evaluate distal perfusion, especially in partial amputations, by assessing tissue pallor and capillary refill times. Sometimes, distal portions of extremities retain their distal perfusion through collateral arterial anastomoses, which provides a greater possibility of replantation.
Once the examination is complete, expedite transfer of the patient to the replantation team. Send pre-operative laboratory studies, including a complete blood count, complete metabolic panel, coagulation panel, and a type and screen, so that the replantation team will not be delayed in getting the patient to the operating room. The patient will likely require pain control to remain comfortable. Opiates are often required and should be administered intravenously. Administer tetanus immunization if warranted. Administer broad-spectrum antibiotics to cover skin flora such as staphylococcal and streptococcal species; gram-negative organisms should also be covered, depending on the mechanism of injury. Obtain plain films of the amputated portion and the stump to evaluate the bony structures for damage.
Figure 1: Care of Complete Amputation
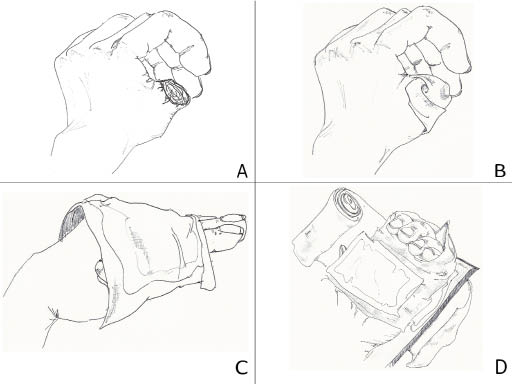
A. Wrap the stump in saline-moistened gauze. B. Wrap the rest of limb in saline-moistened gauze. C. Place cool compress or bag with ice-water slurry over stump. D. Then splint the limb and wrap tightly to prevent oozing.
Once the patient is more comfortable, assess the stump. The longer the stump remains warm, the less likely the replantation will be successful. The goal of managing the stump is to lower its temperature to 4ºC; this maximizes the amount of time before irreparable ischemia sets in without damaging the tissue directly by frostbite damage. (See Figures 1 and 2 for details.) Place gauze moistened (not soaked) with saline over the wound and cover it with a compression dressing to minimize oozing. Place cold compresses or bags of 50% ice and 50% water on the stump and elevate the stump above the level of the heart to further minimize oozing. Do not allow ice to directly contact the wound, even through the plastic bag. Splint the stump to prevent further damage and contamination of the wound. For partial amputations, pack the moistened gauze inside the wound and then place more moistened gauze over the wound before placing the cold compresses over the gauze. Splint these amputations for comfort and to keep the amputation in anatomic position as much as possible. In both circumstances, the wound should be wrapped adequately with pressure dressings to prevent oozing.23 The temperature of blood from the body will raise the stump temperature if the bandages become soaked. This will make maintaining cold ischemia more difficult and compromise replantation attempts. If the injury is a complete amputation, the amputated portion should also be packaged appropriately. Once the amputated part has been cleansed, wrap it in saline-moistened gauze and place it in a bag. Place the bag in a container filled with an ice-water slurry.
Figure 2: Care of Amputated Portion
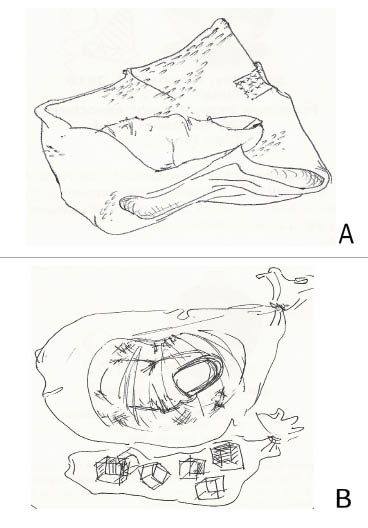
A. Wrap in saline-moistened gauze. B. Wrap it in a bag and place in a container with ice-water slurry.
Early consultation with the replantation team during the ED evaluation will enable them to mobilize the operating room in anticipation of the patient's arrival. Similar to the prehospital setting, if stabilization of the patient is delaying transport to the surgical team, it may be in the best interest of the patient to send the amputated portion ahead of the patient so that it can be prepared for replantation. Even if it appears that replantation would fail, parts such as nail bed or skin might be harvested from the amputated portion during reconstruction.
A multitude of complications can arise during the management of amputations. Acute hemorrhage and its physiologic consequences are a primary threat to the life of the patient, whereas ischemia is the primary threat to the amputated part.24 As stated before, the physiologic response to amputation is intense vasospasm at the site of injury to reduce blood loss.
One of the most feared complications is compartment syndrome, that is pathologically elevated interstitial pressure within confined fascia that envelopes a muscle group.6,9 It can be caused by intrinsic factors such as a vascular injury that bleeds into a confined fascial compartment, extrinsic factors such as external compression (e.g., dressings, splints, tourniquets), or prolonged pressure on an extremity. Compartment pressure that increases above the intravascular pressure causes physiologic devascularization of the distal tissue and subsequent ischemia. Skeletal muscle metabolic processes are disrupted and cell membrane integrity is compromised. Cytolysis and the release of osmotic contents into the compartment draw additional plasma into the interstitial space and create a cycle of increasing compartment pressures that compromises distal circulation and nerve conduction.6,9 Normal compartment pressure is below 10 to 12 mm Hg. Clinically significant impairment of circulation occurs at pressures above 20 mm Hg. The most precise way to determine abnormal compartment pressures is to measure the difference between the mean arterial blood pressure and the compartmental pressure, usually with a needle-tonometry device. The smallest difference compatible with normal metabolism is 30 mm Hg.9 Clinically, the first signs of compartment syndrome are pain out of proportion to the injury, pallor, or paresthesia. These findings develop within 30 minutes after the onset of ischemia. If left untreated, it can progress to paresis and pulselessness, which are usually late signs. (See Table 1.) Irreversible nerve damage begins after 6 hours.6,9
Table 1: "Ps" of Compartment Syndrome
- Pain out of proportion
- Pallor
- Paresthesias
- Pulselessness (late finding)
- Paresis (late finding)
Rhabdomyolysis is the destruction of skeletal muscle, with spilling of toxic cellular components into the systemic circulation.6,9 It can be caused by compartment syndrome from a crush or partial amputation. It causes plasma sequestration within myocytes, resulting in hypovolemia and myocyte edema, as well as systemic release of intracellular potassium, myoglobin, phosphate, and sulfate, resulting in hyperkalemia, acute renal failure, and acidosis.6,9 Hyperkalemia, the most immediate threat to life, occurs in 10% to 40% of cases.6,9
Other less common complications of amputation injuries are microbial infection of either the part or the patient, and fractures in the amputated part that may cause or exacerbate compartment syndrome and/or neurovascular compromise.
Surgical Techniques
Depending on the type and location of the amputation and the length of time since it occurred, the patient may be a candidate for replantation. The amputated part suffers similar physiologic derangements as the patient in shock.
Surgical replantation may be attempted; however, complete amputation may be necessary because of other life-threatening injuries, severe associated trauma with metabolic derangements, or lack of salvageability of the distal tissue.5,16 The prognosis is largely dependent on the type and quantity of tissue connecting the proximal and distal parts.
The goal of replantation is to provide a functional part with reasonable sensation and mobility. Thus, the decision to attempt surgical replantation is complex, with multiple factors to consider, including the severity and type of injury (e.g., crush, avulsion, transection) and patient factors (e.g., age, hand dominance, medical history, social history, presence of other life-threatening injuries). Lengthy rehabilitation is often required. The average time until return to work is 7 months.9,16 The decision of whether to proceed with replantation will depend upon several factors and will ultimately be decided by the replantation team. Contraindications to replantation are found in Table 2.
Table 2: Contraindications to Replantation
Relative
- Severe crush or avulsion amputation
- Injuries at multiple levels of the amputated part
- Pre-existing illness that affects wound healing or rehabilitation (e.g., diabetes mellitus, smoking)
- Gross contamination of the parts
- Prior surgery or trauma to the amputated limb
Absolute
- Concomitant life-threatening injuries that require stabilization
- Amputated portion in multiple pieces
Ischemia time is the main determinant of replantation success. Sharply transected amputations carry a better prognosis than avulsion or crush injuries. Repair of mangled parts with multiple vascular injuries may not be possible. The combination of vascular and nerve injuries complicates replantation success. The extent of muscle loss predicts function of the replanted part. Massive loss across multiple compartments carries a poor prognosis.6,25,26
Figure 3: Radiograph of a Distal Finger Amputation
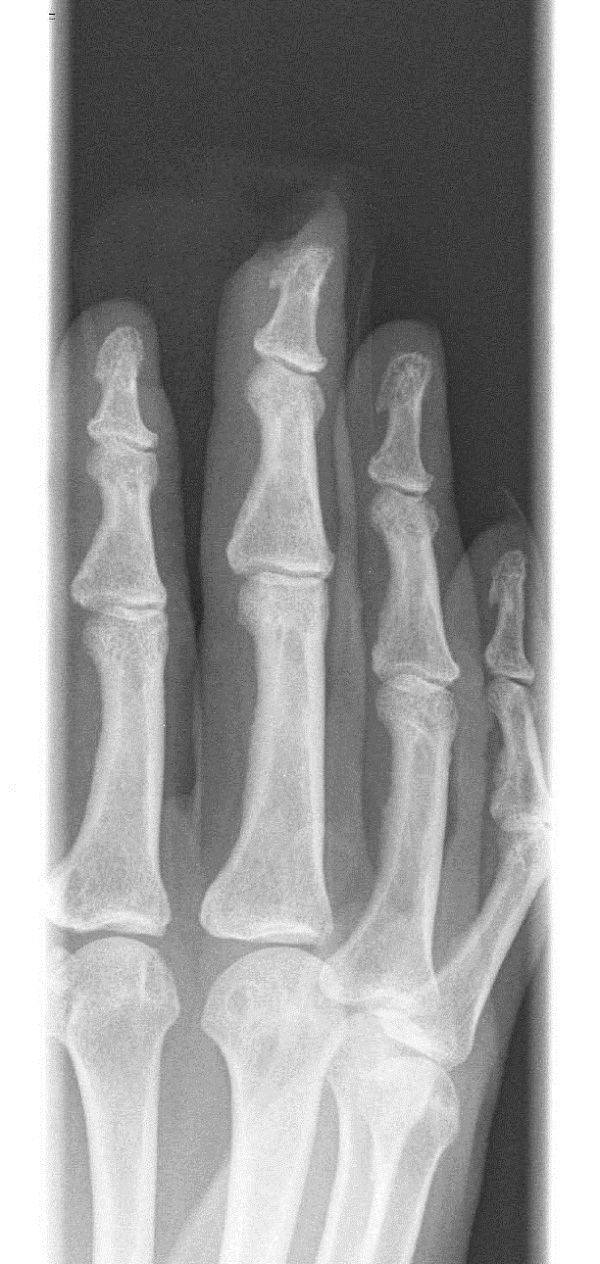
No fracture of the distal phalanx was identified.
Finger Amputations
Fingers are some of the most commonly injured and, therefore, the most commonly amputated portions of the body. Humans use their hands for a multitude of activities, making them susceptible to both occupational and nonoccupational dangers. This also highlights the amount of functional deficit that is experienced when fingers are amputated, as prolonged rehabilitation has occupational implications. More than half of all upper-extremity amputations involve a finger and the majority of them involve just the distal tip.27-29
Most finger amputations occur in the workplace and are related to the use of heavy machinery.30 The population most at risk for this type of injury is younger than 30 years old. Non-work-related finger injuries occur primarily in children younger than 5 years of age.27-29,31 In this population, the most common mechanism of injury is trapping a finger between two opposable surfaces, usually in a doorway.1,31 School-age children most frequently injure fingers in bicycle-related incidents.1 As age increases, so does the incidence of injuries caused by power tools. Power tools, such as chainsaws and lawnmowers, cause the majority of finger amputations in the teenage and adult populations; adults older than the age of 55 are at the next greatest risk after children.28 The incidence of injury is highest in males, with a 5:1 predominance.27-31 The most commonly amputated fingers are the index and middle fingers, but the finger associated with the most functional loss is the thumb, which is associated with a 40% loss of function of the affected hand.30
Figure 4: Radiograph of a Distal Finger Amputation Through the Distal Phalanx
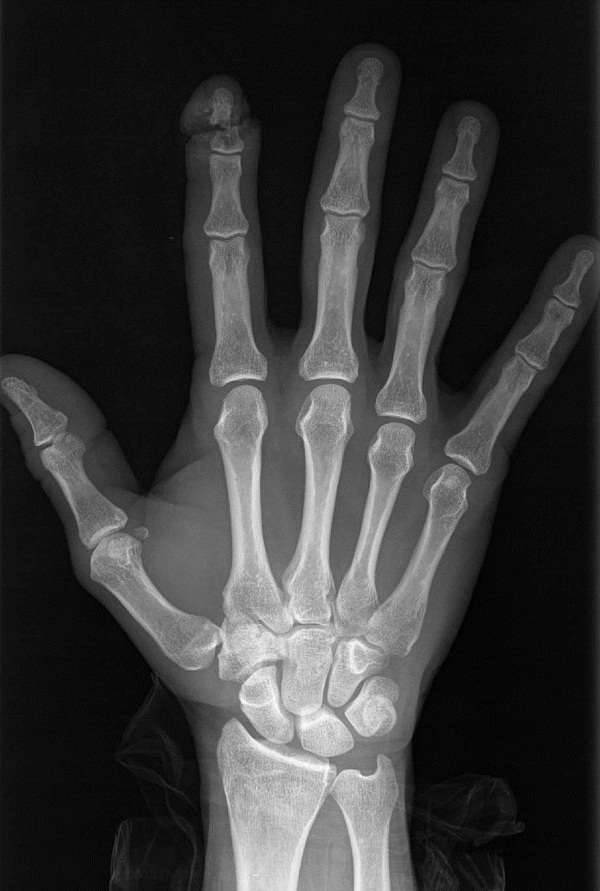
Management of fingertip amputations varies depending on the level where the amputation occurs. Distal tip amputations have the most significant implications because the majority of finger function, including grip and sensation, comes from the tip. Multiple classification systems have been designed for distal tip amputations. Their overlying themes are similar.
Figure 5: Radiograph of a Thumb Amputation Through the Distal Phalanx
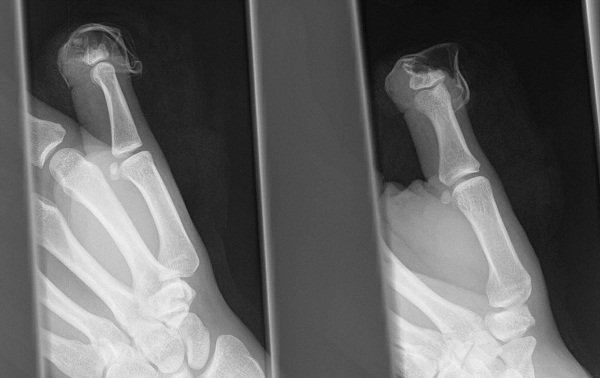
Most distal amputations that do not involve the bone or the nail bed can be managed conservatively. These injuries have a propensity to bleed extensively despite the application of pressure. Therefore, a compression bandage is often required to maintain hemostasis. Systemic antibiotics are not usually required; topical antibiotics such as bacitracin are often sufficient. Splint the finger for comfort and refer the patient to a hand surgeon. Sometimes, skin grafting is required to replace the skin defect, but the majority of these injuries heal and leave very little functional or cosmetic defect.
Figure 6: Radiograph of a Hand Mangled by a Piece of Machinery
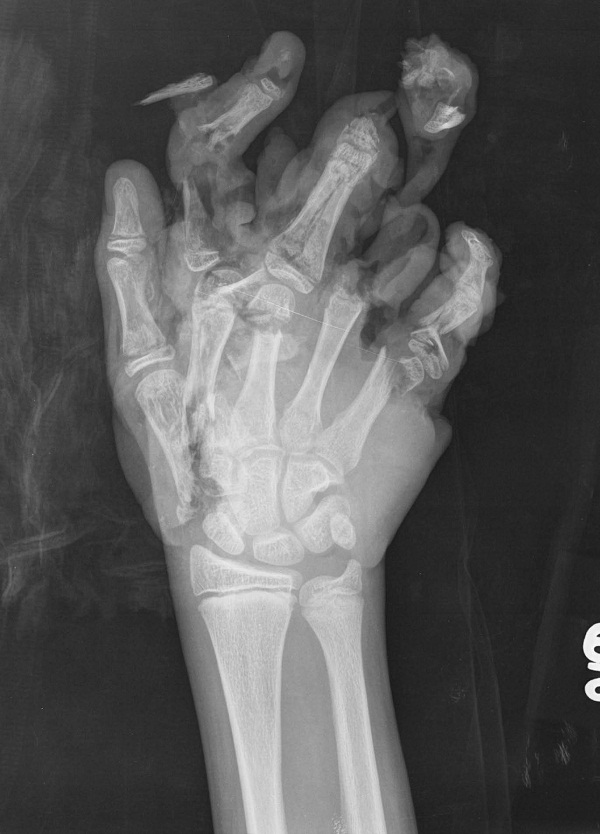
Multiple amputations and fractures are present.
Distal tip amputations that involve the nail bed but not bone are slightly more complicated. The fingernail is important not only for cosmetic function but also as a point of counterpressure for the distal finger and an instrument of accurate pinch.32 Nail bed conservation is in the best interest of the patient. Consult a hand surgeon early in the management of this type of injury. The majority of them are managed conservatively, but successful replantation procedures have been reported.33 For patients who are not referred for replantation, splint the injury for comfort and refer the patient for urgent outpatient hand surgeon evaluation. These patients will likely require an operative procedure such as a nail bed graft to retain nail length.
Figure 7: Radiograph of a Partial Upper-extremity Amputation Through the Humerus
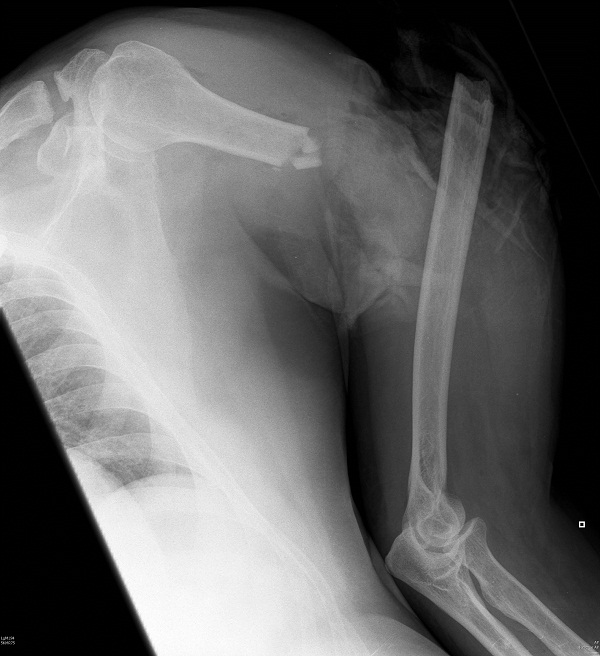
All other finger amputations, including distal tip injuries that do involve bone, are managed surgically. Replantation is the best option. The only absolute contraindication for replantation is the presence of other life-threatening injuries.
Figure 8: Radiograph of a Complete Upper-extremity Avulsion Amputation at the Level of the Humerus
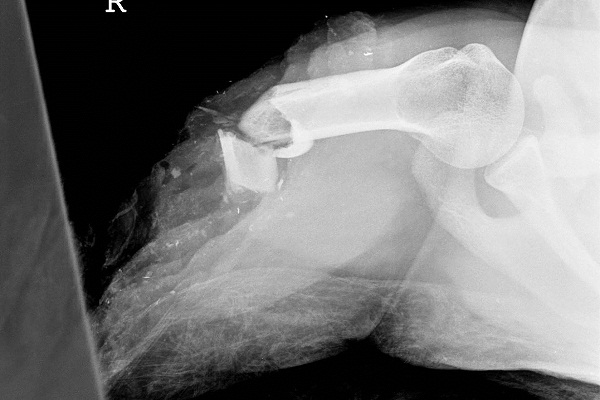
Treat all patients with fingertip amputations as if replantation is possible. Administer systemic antibiotics and tetanus booster if the immunization is not up to date. The stump should be cooled, bandaged, and splinted. The amputated portion should be packed in an ice slurry and should travel with the patient to the care of the replantation team.
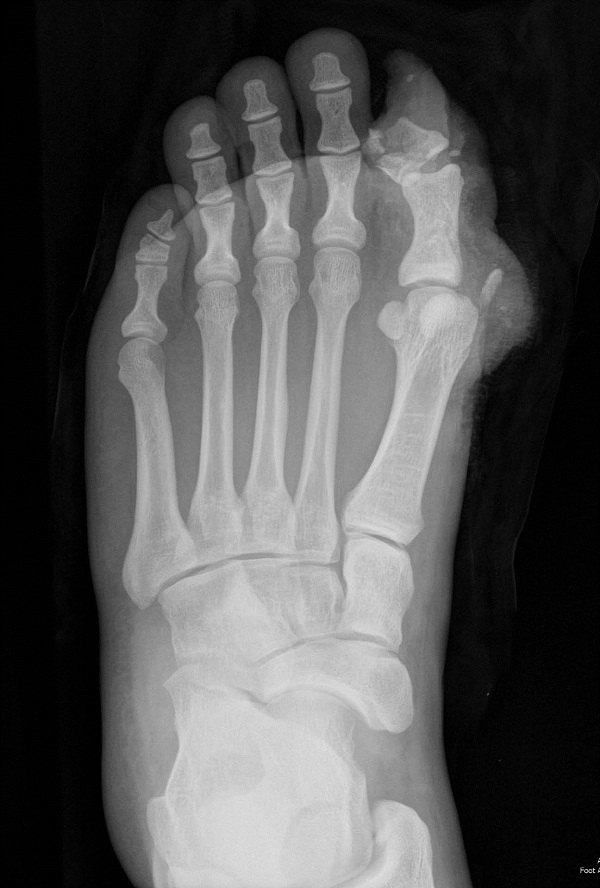
Figure 9: Radiograph of a Great Toe Amputation Through the Distal Phalanx
Success rates between 40% and 96% have been reported for digital replantation.34-37 This is true even with prolonged ischemia times, with one study claiming a successful replant after 33 hours of ischemia.35 Alternative treatment methods such as skin flaps have a number of unappealing results, such as cold intolerance, hyperesthesia, shortened length, inadequate nails, decreased sensation, and decreased motor function.33,37 Replantation, when successful, results in length preservation, nail preservation, and good motor and sensory functional outcomes.37
Upper-extremity Amputations
After fingers, the upper extremity is the next most common site of amputation. Injuries to the upper extremity are devastating and debilitating. This type of injury has more implications than most other amputations, as the patient's livelihood will probably be affected, as will activities such as eating, bathing, and brushing teeth. The performance of mundane tasks, usually taken for granted, will become much more difficult.
Upper-extremity amputations usually involve the hand or the wrist. The incidence decreases while moving more proximally. Distal amputations are most commonly caused by power tools and are usually of the guillotine type. Proximal amputations are most commonly caused by clothing becoming entangled in high-energy machinery and are usually avulsions,4,38 which obviously are more devastating and difficult to repair.4 Avulsion injuries are more prone to complications such as rhabdomyolysis and compartment syndrome due to the involvement of larger muscle groups.
Management of these injuries involves time-efficient stabilization and transfer. Because of the larger amount of tissue in more proximal tissue, cold ischemia time is much less in comparison with the fingers. Place at least one intravenous line in the unaffected arm and maintain euvolemia with isotonic fluids. Use blood products liberally. If both arms are affected, establish central venous access. Initiate broad-spectrum antimicrobial therapy and update tetanus status as needed. Rapid transport to a replantation operative suite results in better outcomes.
Success rates are relatively high for replantation of the upper extremity. The goal of operative treatment is to re-establish a functional limb as closely as possible. The main options are to replant the limb or revise the stump to fit a prosthesis. Graham and associates found that replanted limbs were functionally superior to a prosthesis from a motor standpoint.39 Prosthetic limbs can assist with a number of daily activities.3 However, a functional replanted upper extremity will perform similarly to the uninjured arm and is more aesthetically pleasing to the patient.40 Barring a life-threatening injury or severe mutilation of the amputated portion, replantation of an upper extremity should be attempted.
Lower-extremity Amputations
Lower-extremity amputations occur half as frequently as amputations of the upper extremity. These injuries are commonly caused by power tools as well, but the power tools are most likely pushed (e.g., lawnmowers and snow blowers). They are also caused by high-energy motor vehicle crashes, often involving motorcycles. Power tools are responsible for distal amputations (i.e., toes, midfoot), whereas motor vehicles are usually responsible for proximal amputations. These injuries more commonly occur in males than females. Similar to the upper extremity, the highest incidence of amputation occurs at the most distal portion, the toes, and the incidence decreases moving proximally up the extremity.
Management of these injuries is not far removed from the management of any amputation. Hemostasis is achieved with direct pressure and elevation. Ensure adequate volume resuscitation with isotonic fluids and use blood products liberally as needed to maintain euvolemia, especially if the long bones are involved. These injuries are also more prone to compartment syndrome and rhabdomyolysis due to the large amount of muscular tissue present in the lower extremity, especially in more proximal injuries.41
Because of the lack of functional complexity of the lower extremities, amputations usually were not salvaged in the past. Most people use their lower extremities for ambulation and relatively little else, unless there are occupational implications, such as in professional sports. Therefore, amputations usually were reduced to a stump and the patient was fitted for a prosthesis. However, newer microsurgical techniques have evolved in the past several years, making the possibility of replantation a viable option for more patients. In many cases, prosthetic legs are more appealing and functional than their replanted counterparts. A number of other factors contribute to the decision to replant a lower extremity or to prepare the stump for a prosthetic device. The replantation operation is a longer procedure, the number of additional operations is higher, the hospital stay and subsequent rehabilitation are longer, and the cost is significantly higher.41,42 Furthermore, patients who undergo replantation are forced to deal with numerous postoperative complications, such as skeletal shortening, infections, and impaired nerve regeneration, which is debilitating. In addition, patient factors must be considered such as medical history (e.g., diabetes) and smoking history, which bode poorly for replanted lower extremities. Good sensation and adequate motor function have been achieved in 80% to 90% of patients who were carefully selected for replantation.41 In most cases, replantation attempts are limited to children and adults in optimal circumstances. Overall, the decision of whether to replant or to fit a prosthesis is a discussion between the replantation team and the patient.
Penile Amputations
Penile amputations are rare injuries that are difficult to manage. The highest risk in is the psychiatric population and the pediatric population. The most common cause of amputation in the psychiatric population is self-mutilation. People most likely to self-mutilate are those experiencing acute psychosis, whether psychiatric or organic in nature, and depressed patients who become violent while intoxicated.43 They usually perform this act because of a psychogenic delusion, command hallucinations, or religious or sexual conflicts. The mutilation is usually perceived as an act of purification.44-48 There are also reports of self-mutilation by nonpsychotic patients attempting to expedite gender reassignment.43,45
The acutely psychotic and/or intoxicated patient usually continues to be impaired upon presentation for care and may require de-escalation, and possibly sedation, to facilitate examination.43,44,46 Time is crucial with these patients because most have delayed seeking medical attention due to their altered state or lack of desire for medical care. However, most individuals who self-mutilate while in an altered state of consciousness express remorse for their actions once their mental status is stabilized. Therefore, obtain psychiatric consultation early for mental stabilization and, above all, assume that the penis will be replanted.47,49
Among children, the most common causes of penile amputation are animal bites (including those inflicted by humans), iatrogenic accidents during circumcision, and child abuse.50,51 Child abuse is typically committed by a mentally disturbed parent experiencing a psychotic episode. In most cases, the patient is very young and is subject to significant ramifications that a shortened or absent penis will bring about later in life. Therefore, the replantation of a severed penis should be attempted if at all possible.
Penile amputations should be managed like any other amputation. These injuries have a high propensity to bleed, and blood transfusions may be necessary.45,46 A compressive dressing of saline-moistened gauze should be placed over the stump. Wrap the amputated portion in saline-moistened gauze and place it in a sealed bag in a container with an ice slurry. Foley catheterization should not be attempted to avoid injuring tissue further. If possible, divert the urine with a suprapubic cystostomy.45 Although urine is usually sterile, the warmth of urine can warm the stump and decrease the ischemia time. Antimicrobials should be tailored to the mechanism of injury, especially in the case of mammal attacks. Arrange rapid transport of the patient and the amputated part to a tertiary care center for attempted replantation.
Surgical repair has relatively high success rates. Even if the replantation fails, surgeons may be able to locate erectile tissue in the pubic tissue for use in penile restoration. If replantation fails or if inadequate erectile tissue remains with which to construct a functional penis, the use of a prosthesis or gender reassignment, especially in children, is usually the result.52
Facial Amputations
The face is not a common site for amputations. A few facial appendages are susceptible to trauma, namely the ears, nose, lips, and tongue. Amputation of these parts is debilitating to the patient because they constitute the most cosmetic portion of the body. Depending on which facial structure is affected, functional deficits can occur as well. The lips are important for phonation and expression and, in children, for eating (i.e., suckling) and early language development.53 The tongue is responsible for taste, speech, oral hygiene, swallowing, and airway protection.54 The ear is responsible for audition and the nose for olfaction.
Most facial amputations sustained on the anterior face (the lips, nose, and tongue) are the result of animal attacks or falls.53,55 Ear amputations are also caused by animal attacks, but they are most commonly sustained in motor vehicle collisions and interpersonal conflicts.56 The most common animal culprits in facial amputations are dogs, but humans are frequent perpetrators as well.55 Because of the proximity of these appendages to the face, the soft tissues of the face are often injured, including muscles of facial expression, neurovascular structures, and ducts (i.e., parotid), as well as underlying bone.
Facial amputations can have drastic implications regarding the airway. Tongue and lip amputation can occlude the airway, resulting in airway compromise that requires an emergent intervention such as endotracheal intubation or cricothyroidotomy. After the airway has been stabilized, establish hemorrhage control, keeping in mind that direct pressure is the preferred method of hemostasis. As in other amputations, life-threatening injuries should be stabilized before addressing the amputation. Vital structures in and around the face the carotid arteries, the cervical spine, the trachea, the brachial plexus, and the eye globe should be evaluated with neurovascular and ocular examinations. Check for facial fractures such as those involving the mandible or midface. After these injuries have been excluded or stabilized, evaluation of the amputation can begin. Assess the amputation, including the neurovascular status of the stump. Motor function should be tested thoroughly in the lips and tongue, looking for signs of muscular involvement.
Once the examination is complete, prepare the patient for transfer to an appropriate tertiary care center for operative intervention. Send preoperative blood work results to minimize delay at the receiving facility. Prepare the patient and the amputation for transport. Administer prophylactic antimicrobial therapy against skin and oral flora, especially in cases involving bites and those in which the oral mucosa has been disrupted. Update the patient's tetanus status, if indicated. Imaging is usually not necessary unless underlying facial fractures are suspected, since most of the appendages of the face do not contain bony structures.
Early consultation with the surgical team is important. The surgical service that is consulted is hospital-dependent and may be oral maxillofacial surgery, otolaryngology, or plastic surgery. Depending on the extent of the injuries, consultation with two or three teams may be necessary. Contraindications to replantation are very few, with the most significant being the severity of injury sustained and associated injuries that need to be managed and, thus, delay the replantation attempt.57 Replantation success rates for nose and ear amputations vary, usually due to factors beyond the emergency care provider's control.58 Microsurgical techniques are sometimes successful with good cosmetic outcomes and should be attempted, if possible.59,60 However, these techniques involve very small blood vessels, which are friable and easily injured, leading to necrosis and replantation failure. Fortunately, even if an initial repair "fails," adequate function and cosmetic results can be achieved through subsequent procedures with prosthetics and/or flap reconstruction.61 Oral injuries have a slightly higher replantation success rate with minimal loss of function.54
Conclusion
Traumatic amputations are devastating and debilitating injuries. The results of replantation are rarely perfect, but with a time-efficient and pragmatic approach to management, satisfactory cosmetic and functional outcomes can be achieved.
Acknowledgments
The manuscript was copyedited by Linda J. Kesselring, MS, ELS, the technical editor/writer in the Department of Emergency Medicine at the University of Maryland School of Medicine.
The artwork was provided by Miya Hunter-Willis.
References
1. Hostetler SG, Schwartz L, Shields BJ, et al. Characteristics of pediatric traumatic amputations treated in hospital emergency departments: United States, 1990–2002. Pediatrics 2005;116:e667-e674.
2. Cavadas PC, Landín L, Ibáñez J, et al. Infrapopliteal lower extremity replantation. Plast Reconstr Surg 2009;124(2):532-539.
3. Neumeister MW, Brown RE. Mutilating hand injuries: Principles and management. Hand Clin 2003;19:1-15.
4. Chuang DC, Lai JB, Cheng SL, et al. Traction avulsion amputation of the major upper limb: A proposed new classification, guidelines for acute management, and strategies for secondary reconstruction. Plast Reconstr Surg 2001;108:1624-1638.
5. Pasquina PF, Cooper RA. Textbooks of Military Medicine: Care of the Combat Amputee. Washington, DC: Office of the Surgeon General; 2009.
6. Wilson W, Grande CM, Hoyt DB. Trauma: Emergency Resuscitation, Perioperative Anesthesia, Surgical Management. New York: Informa Healthcare; 2006.
7. Greaves I, Porter K, Hodgetts T, et al. Emergency Care: A Textbook for Paramedics. 2nd ed. Edinburgh: Elsevier; 2006.
8. Pollack A. Medical Responder: Your First Response in Emergency Care, 5th ed. Sudbury, Massachusetts: Jones and Bartlett Learning; 2011.
9. Wolfson AB. Harwood-Nuss' Clinical Practice of Emergency Medicine, 5th ed. Philadelphia: Lippincott Williams & Wilkins; 2010.
10. Beekley AC, Sebesta JA, Blackbourne LH, et al. Prehospital tourniquet use in Operation Iraqi Freedom: Effect on hemorrhage control and outcomes. J Trauma 2008;64(2 suppl):S28-S37.
11. Doyle GS, Taillac PP. Tourniquets: A review of current use with proposals for expanded prehospital use. Prehosp Emerg Care 2008;12:241-256.
12. Fludger S, Bell A. Tourniquet application in a rural Queensland HEMS environment. Air Med J 2009;28:291-293.
13. Brown RE, Wu TY. Use of "spare parts" in mutilated upper extremity injuries. Hand Clin 2003;19:73-87.
14. Russell RC, Neumeister MW, Ostric SA, et al. Extremity reconstruction using nonreplantable tissue ("spare parts"). Clin Plast Surg 2007;34:211-222.
15. Shah M, Kulkarni J, Shelley M, et al. Refrigeration of a "spare part": A salvage procedure for preservation of the knee joint in a patient with multiple trauma. Plast Reconstr Surg 2001;108:1289-1294.
16. Brown DL, Borschel GH. Michigan Manual of Plastic Surgery. Philadelphia: Lippincott Williams & Wilkins; 2004.
17. Schaider JJ, Hayden SR, Wolfe RE, et al, eds. Rosen and Barkin's 5 Minute Emergency Medicine Consult, 3rd ed. Philadelphia: Lippincott Williams & Wilkins; 2007.
18. Lloyd MS, Teo TC, Pickford MA, et al. Preoperative management of the amputated limb. Emerg Med J 2005;22: 478-480.
19. Azzopardi EA, Whitaker IS, Laing H. Perception of correct preoperative storage and transfer of amputated digits: A national survey of referring emergency department. J Plast Reconstr Aesthet Surg 2008;61:1418-1419.
20. Pereira C, Oudit D, McGrouther DA. Policy for the handling of amputation parts in accident and emergency departments. Plast Reconstr Surg 2005;116: 346-347.
21. Day MW. Traumatic amputation. Nursing 2006;36(10):88.
22. Laskowski-Jones L. First aid for amputation. Nursing 2006;36:50-52.
23. Buncke GM, Buntic RF, Romeo O. Pediatric mutilating hand injuries. Hand Clin 2003;19:121-131.
24. Newton EJ, Love J. Acute complications of extremity trauma. Emerg Med Clin North Am 2007;25:751-761.
25. Schlenker JD, Koulis CP. Amputations and replantations. Emerg Med Clin North Am 1993;11:739-753.
26. Higgins TF, Klatt JB, Beals TC. Lower Extremity Assessment Project (LEAP) the best available evidence on limb-threatening lower extremity trauma. Orthop Clin North Am 2010;41:233-239.
27. Dillingham TR, Pezzin LE, MacKenzie EJ. Incidence, acute care length of stay, and discharge to rehabilitation of traumatic amputee patients: An epidemiologic study. Arch Phys Med Rehabil 1998;79:279-287.
28. Conn JM, Annest JL, Ryan GW, et al. Non-work-related finger amputations in the United States, 2001-2002. Ann Emerg Med 2005;45:630-635.
29. Dillinham TR, Pezzin LE, MacKenzie EJ. Limb amputation and limb deficiency: Epidemiology and recent trends in the United States. South Med J 2002;95: 875-883.
30. Chung KC, Alderman AK. Replantation of the upper extremity: Indications and outcomes. J Am Soc Surg Hand 2002;2:78-94.
31. Doraiswamy NV. Childhood finger injuries and safeguards. Inj Prev 1999;5: 298-300.
32. Hosnuter M, Kargi E, Isikdemr A. An improvement in dorsal reverse adipofascial flap for fingertip reconstruction: Nail matrix preservation. Ann Plast Surg 2005;55:155-159.
33. Akyürek M, Safak T, Keçik A. Fingertip replantation at or distal to the nail base: Use of the technique of artery-only anastomosis. Ann Plast Surg 2001;46: 605-612.
34. Ito H, Sasaki K, Morioka K, et al. Fingertip amputation salvage on arterial anastomosis alone: An investigation of its limitations. Ann Plast Surg 2010;65: 302-305.
35. Li J, Guo Z, Zhu Q, et al. Fingertip replantation: Determinants of survival. Plast Reconstr Surg 2008;122:833-839.
36. Lemmon JA, Janis JE, Rohrich RJ. Soft-tissue injuries of the fingertip: Methods of evaluation and treatment. An algorithmic approach. Plast Reconstr Surg 2008;122:105e-117e.
37. Dumontier C, Dubert T. Salvage of the nail in distal finger amputation. Tech Hand Up Extrem Surg 2002;6:73-85.
38. Oliveira IC, Barbosa RF, Ferreira PC, et al. The use of forearm free fillet flap in traumatic upper extremity amputations. Microsurgery 2009;29:8-15.
39. Graham B, Adkins P, Tsai TM, et al. Major replantation versus revision amputation and prosthetic fitting in the upper extremity: A late functional outcomes study. J Hand Surg Am 1998;23: 783-791.
40. Atzei A, Pignatti M, Maria-Baldrighi C, et al. Long-term results of replantation of the proximal forearm following avulsion amputation. Microsurgery 2005;25: 293-298.
41. Hierner R, Berger AK, Frederix PR. Lower leg replantation decision-making, treatment, and long-term results. Microsurgery 2007;27:398-410.
42. Bondurant FJ, Colter HB, Buckle R, et al. The medical and economic impact of severely injured lower extremities. J Trauma 1988;28:1270-1273.
43. Jezior JR, Brady JD, Schlossberg SM. Management of penile amputation injuries. World J Surg 2001;25:1602-1609.
44. Bandi G, Santucci RA. Controversies in the management of male external genitourinary trauma. J Trauma 2004;56: 1362-1370.
45. Wessells H, Long L. Penile and genital injuries. Urol Clin North Am 2006;33:117-126.
46. Morey AF, Metro MJ, Carney KJ, et al. Consensus on genitourinary trauma: External genitalia. BJU Int 2004;94: 507-515.
47. Landström JT, Schuyler RW, Macris GP. Microsurgical penile replantation facilitated by postoperative HBO treatment. Microsurgery 2004;24:49-55.
48. Clark RA. Self-mutilation accompanying religious delusions: A case report and review. J Clin Psychiatry 1981;42: 243-245.
49. Erdur B, Turkcuer I, Herken H. An unusual form of self-mutilation: Tongue amputation with local anesthesia. Am J Emerg Med 2006;24:625-628.
50. Shaw MB, Sadove AM, Rink RC. Reconstruction after total penile amputation and emasculation. Ann Plast Surg 2003;50:321-324.
51. Park JK, Min JK, Kim HJ. Reimplantation of an amputated penis in prepubertal boys. J Urol 2001;165: 586-587.
52. Ochoa B. Trauma of the external genitalia in children: Amputation of the penis and emasculation. J Urol 1998;160(3 Pt 2):1116-1119.
53. Baj A, Beltramini G, Laganà F, et al. Amputation trauma of the face: Surgical techniques and microsurgical replantations. Acta Otorhinolaryngol Ital 2009;29:92-96.
54. Egozi E, Faulkner B, Lin KY. Successful revascularization following near-complete amputation of the tongue. Ann Plast Surg 2006;56:190-193.
55. Taylor HO, Andrews B. Lip replantation and delayed inset after a dog bite: A case report and literature review. Microsurgery 2009;29:657-661.
56. Punjabi AP, Huag RH, Jordan RB. Management of injuries to the auricle. J Oral Maxillofac Surg 1997;55:732-739.
57. Duroure F, Simon E, Fadhul S, et al. Microsurgical lip replantation: Evaluation of functional and aesthetic results of three cases. Microsurgery 2004;24:265-269.
58. Alagöz MS, Uysal AC, Isgören S, et al. A new method in the treatment of ear amputation: Experimental and clinical study. Ann Plast Surg 2007;59:277-286.
59. Hammond DC, Bouwense CL, Hankins WT, et al. Microsurgical replantation of the amputated nose. Plast Reconstr Surg 2000;105:2133-2136.
60. Kayikçioglu A, Karamürsel S, Keçik A. Replantation of nearly total nose amputation without venous anastomosis. Plast Reconstr Surg 2001;108:702-704.
61. Kadlub N, Persing JA, Shin JH. Immediate or delayed nasal reconstruction in infant after subtotal amputation? Nasal reconstruction with forehead flap in a 2-year-old child. Ann Plast Surg 2008;60:487-490.
Care for a patient who undergoes an amputation is often complicated and is time-sensitive. A lot of thought goes into whether replantation is attempted or not, but those decisions are reserved for the replantation team. The role of the emergency provider is to expediently evaluate the patient and prepare him or her for care by the replantation team.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
