Congenital Anomalies: Congenital Heart Disease
Core Content: Emergency Management of Congenital Anomalies
- Know the anatomy and pathophysiology relevant to emergency management of congenital anomalies
- Know the indications and contraindications for emergency management of congenital anomalies
- Plan the key steps and know the potential pitfalls in the emergency management of congenital anomalies
- Recognize the complications associated with the emergency management of congenital anomalies
Congenital heart disease occurs in about 6-8 per 1000 live births and usually presents in the first 2 weeks of life. Clinical presentation may vary from the incidental finding of a heart murmur in an otherwise healthy neonate to cyanosis or life-threatening arrhythmias or cardiovascular collapse, including congestive heart failure or shock.1
Cyanosis is usually indicative of hypoxemia (decreased level of arterial oxygen saturation). The level of arterial desaturated hemoglobin must be above 3 g/dL for cyanosis to be clinically visible. Therefore, cyanosis is more readily evident in the infant with polycythemia compared to an anemic child. Cyanosis in any neonate should raise concern for a congenital heart defect. A quick screening test for possible ductal-dependent congenital heart disease in infants > 24 hours of age is post-ductal (lower extremity) pulse oximetry.2 SpO2 < 95% in room air should be further evaluated by echocardiogram.
The hyperoxia test or oxygen challenge test is used to screen patients for cyanotic heart disease: A preductal (right radial) blood gas is obtained with the infant breathing room air and then repeated after the infant has inspired 100% oxygen for 10-15 minutes. If significant right to left shunting exists, the PaO2 rarely rises above 150 mmHg and often the rise is not more than 10-30 mmHg. Non-cardiac causes of cyanosis include pulmonary disease, methemoglobinemia, or severe polycythemia.
National Guideline/Academic Resources
http://www.aap.org/en-us/advocacy-and-policy/aap-health-initiatives/PEHDIC/Pages/Newborn-Screening-for-CCHD.aspx
Cyanotic Heart Disease
Heart diseases often presenting with cyanosis:
- Tetralogy of Fallot
- Total anomalous pulmonary venous return
- Transposition of the great arteries
- Tricuspid atresia
- Truncus arteriosus
- Pulmonary atresia or stenosis
- Ebstein anomaly
CME Question
A 5-day-old infant presents with decreased feeding and perioral cyanosis. Pulse oximetry measures 75%. The infant was born at a birthing center without complications. The most likely cardiac lesion is:
- Tetralogy of Fallot
- ASD
- Coarctation of the aorta
- Aortic stenosis
- Small VSD
Start or Resume CME Test (Opens in a new Tab/Window)
Tetralogy of Fallot (TOF) accounts for 10% of all congenital heart diseases. Four main anatomic abnormalities exist: a ventricular septal defect (VSD), pulmonary stenosis (causing right ventricular outflow obstruction [RVOT]), an overriding aorta, and right ventricular hypertrophy (RVH). The degree of RVOT partially determines the size of the right-to-left shunt across the VSD, and therefore determines the degree of cyanosis (pink Tet vs blue Tet). Examination of the infant usually reveals a loud systolic ejection murmur at the left midsternal border and left upper sternal border with or without a thrill. The chest X-ray typically shows a boot shaped heart of normal size with or without decreased pulmonary vascular markings. (Figure: Boot shaped heart: Tetralogy of Fallot) EKG findings include right axis deviation (RAD) and RVH.
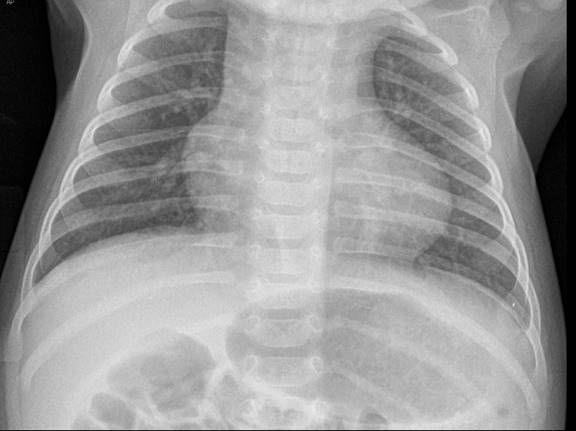
The infant may present with a hypercyanotic episode (“Tet spell”) due to increased RVOT and increased right to left shunting. A Tet spell may occur due to feeding, crying, or straining (defecation), fever, or hypovolemia. The pathophysiology is almost total RVOT resulting in increased right-to-left shunt through the VSD. The goals of acute treatment are increasing systemic vascular resistance (SVR) and decreasing pulmonary resistance, thereby decreasing right-to-left shunting. Calming the infant is important. Placing the child in the knee-to-chest position increases SVR. Oxygen is a potent pulmonary vasodilator. Morphine (0.1-0.2 mg/kg IM or IV) may also improve blood flow through the right ventricular outflow tract. If there is no clinical improvement with these interventions, the infant may be given an IV fluid bolus. Sedative medications such as ketamine (1-2 mg/kg) may be helpful. Phenylephrine (5-20 mcg/kg/dose IV) increases SVR by its alpha-adrenergic effects and may help to break the spell if all else fails. Paralysis and intubation may be necessary in refractory cases.
In addition to TOF, decreased pulmonary blood flow may be seen with tricuspid atresia, pulmonary atresia or stenosis, and Ebstein’s anomaly. Conversely, increased pulmonary blood flow occurs with total anomalous venous return, transposition of the great vessels, and truncus arteroisus.
CME Question
An infant with Tetralogy of Fallot presents with a hypercyanotic spell. The following are modalities used to treat this condition:
- Calming the infant.
- Morphine 0.1 mg/kg IM, IV or SC.
- A sedative such as ketamine.
- Phenylephrine 5-10 microgram/kg/dose.
- All of the above.
Start or Resume CME Test (Opens in a new Tab/Window)
CME Question
An infant is diagnosed with Tetralogy of Fallot. The components includes:
- Ventricular septal defect
- Pulmonary stenosis
- Overriding aorta
- Right ventricular hypertrophy
- All of the above
Start or Resume CME Test (Opens in a new Tab/Window)
Total Anomalous Pulmonary Venous Return
Total anomalous venous return (TAPVR) accounts for a small percentage of congenital heart disease. The pulmonary veins do not drain into the left atrium (LA), and may drain into the superior vena cava (SVC), the coronary sinus, or right atrium (RA), the inferior vena cave (IVC), or some combination. This causes an increase in systemic venous return and increased pulmonary blood flow (a right to left shunt). Examination may reveal a systolic murmur at the left upper sternal border and a mid-diastolic rumble at the left lower sternal border. The chest X-ray shows congested lungs, referred to as the “snowman’s sign.” TAPVR may not present clinically until about 4 months of age.
CME Question
An infant presents to the ED with cyanosis. An echocardiogram reveals total anomalous pulmonary venous return. Which of the following statements is true?
- The chest X-ray may show pulmonary venous congestion.
- It is a common cardiac cause of congenital heart disease.
- The pulmonary vein drains into the left atrium.
- All of the above.
Start or Resume CME Test (Opens in a new Tab/Window)
Transposition of the Great Arteries
Transposition of the Great Arteries (TGA) is the most common cause of cyanotic heart disease presenting in the immediate newborn period with an incidence of 3-4 per 10,000 live births. The aorta exits from the right ventricle, and the main pulmonary artery exits from the left ventricle. This produces parallel, separate circulations. A coexisting VSD, ASD, patent ductus arteriosus (PDA), or patent foramen ovale provides a connection between the two parallel circuits and is essential for life. When no ASD or VSD is present, newborns will present with cyanosis immediately after birth. Emergent balloon atrial septostomy (“Rashkind procedure”) is often a necessary temporizing procedure prior to definitive surgical repair. In the presence of an ASD or VSD, the infant first presents with cyanosis and cardiovascular collapse when the PDA begins to close, usually within the first few weeks of life. On examination the infant is cyanotic and may have a loud S2. A murmur is present only if there is an existing VSD or LVOT obstruction. The chest X-ray shows cardiomegaly and the classic “egg on a string.” There may be increased pulmonary vascular markings. The EKG shows RAD and RVH.
Tricuspid Atresia
Tricuspid atresia occurs in 1-2% of congenital heart disease. There is agenesis of the tricuspid opening with a hypoplastic right ventricle. The presence of a VSD, PDA, or ASD permits pulmonary blood flow and severe cyanosis may occur when the PDA closes
CME Question
An infant has tricuspid atresia. Which of the following statements is true about this condition?
- Severe cyanosis may occur when the PDA closes.
- The presence of a VSD or ASD permits pulmonary blood flow.
- There is hypoplasia of the right ventricle.
- All of the above
Start or Resume CME Test (Opens in a new Tab/Window)
Dextrocardia
Dextrocardia occurs when the apex of the heart is situated on the right side of the chest. It may be associated with situs inversus or normal position of the other organs. It may be associated with other cardiac anomalies and cardiology consultation is recommended. (See Figure. Dextrocardia)
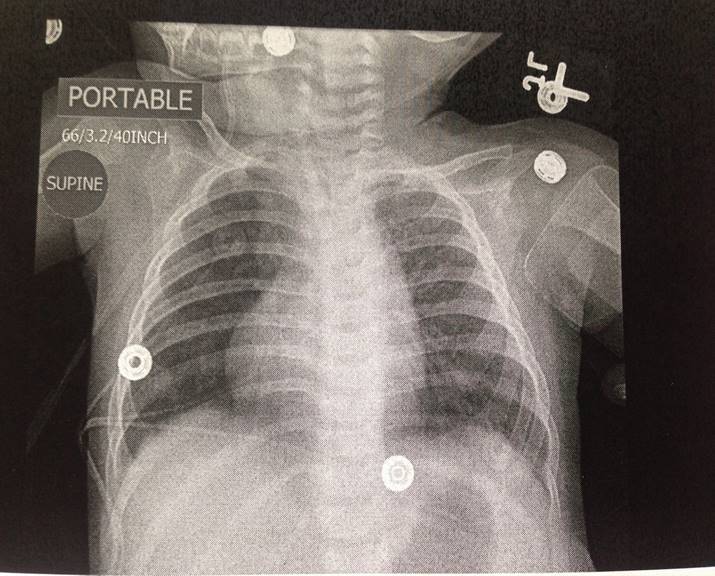
Acyanotic Congenital Heart Disease
Heart diseases that usually present without cyanosis:
- Ventricular septal defect
- Atrial septal defect
- Patent ductus arteriosus
- Atrioventicular septal defect
- Aortic stenosis
- Coarctation of the aorta
- Hypoplasic left heart syndrome
Ventricular Septal Defect
Ventricular septal defects (VSD) account for about 20-25% of congenital heart disease. Symptoms, including tachycardia and tachypnea, may not present until 4-8 weeks of life when pulmonary pressures drop and left-to-right flow across the VSD increases. Smaller defects may be asymptomatic and many will close by 2 years of age without intervention. On examination, there is a systolic murmur at the lower left sternal border (LLSB), and a systolic thrill may be present if there is a large shunt. The chest X-ray may reveal cardiomegaly with pulmonary venous congestion. EKG findings depend on the size of the defect. It may be normal in a small lesion or show LVH and left atrial enlargement (LAE) or biventricular hypertrophy (BVH) and LAE with very large lesions.
Atrial Septal Defect
Atrial septal defects (ASD) account for 10% of all congenital heart defects and are more common in females. Most patients are asymptomatic, but more severe cases may develop atrial arrhythmias. Classically, there is a systolic murmur at the left upper sternal border (LUSB) and a wide split S2. The chest X-ray may show cardiomegaly with increased pulmonary vascular markings. EKG may be normal or show RAD, RVH, or right bundle branch block (RBBB).
Patent Ductus Arteriosus
Patent Ductus Arteriosus (PDA) occurs in about 5-10% of term infants and 40-60% of preterm or very low birth weight infants with congenital heart defects. On examination, there is a continuous machinery murmur at the LUSB. A wide pulse pressure often exists. The chest X-ray may show cardiomegaly with increased pulmonary vascular markings (PVM). The EKG may be normal or may show LVH or BVH.
Atrioventricular Septal Defect
Most cases of atrioventicular septal defects (AVSD) occur in children with Down syndrome (30-60%). There is an active precordium with a systolic thrill and a holosysytolic murmur at the LLSB. The chest X-ray may show cardiomegaly. The EKG may show RVH and LVH.
Aortic stenosis
Aortic stenosis (AS) accounts for about 7% of cases of congenital heart defects. In mild cases, patients with AS present with exercise intolerance and in more severe cases patients may have poor feeding and dyspnea. On physical exam, patients present with a systolic thrill over the RUSB, suprasternal notch, or carotid arteries. There may be a systolic ejection murmur at the second or third right intercostal space with radiation to the apex and neck. If severe stenosis exists, there is a narrow pulse pressure. The chest X-ray is often normal. The EKG may be normal or show LVH with severe lesions.
Coarctation of the Aorta
Coarctation of the aorta occurs in about 8-10% of cases of congenital heart disease. Presentation varies with the severity of the obstruction. Critical coarctation of the aorta presents with cyanosis and shock when the ductus arteriosus closes. Classically, the blood pressure and pulse oximetry in the lower extremities is lower than in the upper extremities. Less severe obstructions may present with a systolic ejection murmur at the LUSB, shortness of breath with feeding or exercise, or asymptomatic hypertension. The chest X-ray may reveal cardiomegaly and pulmonary venous congestion. The classic rib notching due to collaterals is absent in the neonate. The EKG may show RVH or RBBB.
Hypoplastic Left Heart Syndrome
Hypoplastic left heart syndrome (HLHS) is associated with the highest mortality of all congenital heart diseases. There is left atrial and ventricular hypoplasia, atresia or stenosis of the mitral and aortic valves, and hypoplasia of the ascending aorta. There is significant RVH, as the right ventricle has to supply the systemic circulation via the PDA in addition to the pulmonary circulation. These infants often present with shock, poor peripheral pulses, and congestive heart failure when the PDA closes.
Management/Stabilization of Congenital Heart Disease
The immediate management of an infant with suspected CHD includes stabilization of the airway and circulation. Oxygen supplementation should be considered for hypoxemia, but if unsuccessful in improving oxygenation it should be decreased, since oxygen may hasten PDA closure. The head of the infant’s bed should be elevated to 30-45 degrees. Vital sign measurements should include right upper extremity (pre-ductal) and lower extremity (post-ductal) blood pressures and pulse oximetry. The hyperoxia test may be performed if condition and time warrant. The acute evaluation includes a chest X-ray, EKG, CBC, electrolytes, and brain natriuretic peptide (BNP). An echocardiogram should be obtained as soon as possible after the infant is stabilized.
The chest X-ray in congenital heart disease may reveal cardiomegaly or pulmonary congestion (curly B lines). Furthermore, certain heart defects have characteristic findings on chest X-ray: TOF has a characteristic boot-shaped heart. TGA is described as an egg on a string appearance. Ebstein’s anomaly shows a “wall-to-wall” heart. TAPVR classically shows severe pulmonary vascular congestion described as the “snowman’s sign”. A normal chest x-ray does not exclude the presence of CHD.
The EKG is usually abnormal but non-specific. It can show ventricular hypertrophy and T wave changes. A CBC may indicate anemia (a potential cause of heart failure). Acidosis may be evident. The BNP levels may be very high at birth and is usually below 33 pg/mL by the second week of life.
In patients with volume overload, a loop diuretic such as furosemide (0. 5-1 mg/kg) may be given to reduce preload. If the infant has signs of poor perfusion or shock, inotropic agents such as dopamine (5-10 mcg/kg/min) may be needed to increase contractility via ß1 adrenegic stimulation. However, at doses higher than 10 mcg/kg/min, dopamine has a predominantly a-adrenegic effect, causing vasoconstriction. Dobutamine (2.5-25 mcg/kg) also has inotropic effects via ß1 and ß2 adrenergic receptors, but lacks a-adrenegic stimulation. As a result, dobutamine is an inotrope that also causes vasodilation and reduces afterload. Milrinone, a phosphodiesterase (PDE) inhibitor, also has inotropic and vasodilatory actions and is often used in systolic heart failure to decrease systemic and pulmonary pressures. It is given as a loading dose of 50 mcg/kg over 15 minutes and then 0.35-75 mcg/kg/min.
If a neonate presents with shock/cyanosis and a ductal dependent lesion is suspected, an infusion of prostaglandin E1 (PGE1) (0.05-0.1 mcg/kg IV or IM) should be initiated, following discussion with a neonatologist/cardiologist, as soon as possible to prevent further closure of the ductus arteriosus and possibly open it further. Apnea is a major complication associated with prostaglandin therapy. The risk of apnea is dose dependent. Elective intubation should be considered. A 10 mL/kg crystalloid fluid may be given since many of these neonates also present with hypovolemia, followed by reassessment for signs of worsening pulmonary edema. Since it is often difficult to exclude sepsis in the infant presenting in undifferentiated shock, blood and urine culture should be obtained and empiric broad-spectrum antibiotics administered. A spinal tap for CSF cultures may be done when the infant is stabilized. Clinical deterioration immediately after starting prostaglandin E1 therapy may indicate the presence of pulmonary venous or left atrial obstruction, such as infra-diaphragmatic TAPVR. These infants require emergent echocardiography and interventional cardiology consultation.
Palliative surgical procedures:
- HLHS – Stage I/Norwood procedure includes connection of main pulmonary artery (PA) to the aorta, systemic to pulmonary shunt, atrial septectomy
- TGA – Emergent balloon atrial septostomy (“Rashkind procedure”)
- Lesions with decreased pulmonary flow – systemic to pulmonary shunt (Blalock–Taussig)
-
Lesions with excess pulmonary blood flow – Ligation of main PA or PA band
The definite treatment for various cardiac lesions: - PDA –Closure using indomethacin or surgical ligation
- TGA – Arterial switch procedure (Jatene); atrial switch procedure (Senning or Mustard)
- TOF – Patch closure of VSD, enlargement of the RVOT, +/- pulmonary valvotomy, +/- RV to PA patch, +/- RV to PA conduit
- Coarctation of Aorta – Resection or patch augmentation
- TAPVR – Reanastomosis pulmonary vein to left atrium, division of connecting vein
- TA – Closure of VSD, baffling LV to truncus, removal of PA from truncus, conduit from RV to PA
CME Question
An infant with congenital heart disease presents to the ED. Match the following X-ray findings with the associated heart disease.
X-ray findings:
- Boot-shaped heart
- Wall-to-wall heart.
- Egg on a string.
- Snowman’s sign.
- Apex of heart on the right.
Heart lesion
- A. Tetralogy of Fallot.
- B. Transposition of the great arteries.
- C. Ebstein’s anomaly.
- D. Dextrocardia.
- E. Total anomalous pulmonary venous return.
Start or Resume CME Test (Opens in a new Tab/Window)
Arrhythmias
Supraventricular tachycardia (SVT) is the most common tachyarrhythmia in neonates. Most children with SVT have structurally normal hearts, but it can be associated with congenital heart diseases, such as Ebstein’s anomaly or TGA, or as a postoperative complication. In structurally normal hearts, the most common cause is idiopathic. However, Wolff-Parkinson-White Syndrome (WPW) is the most commonly identified underlying etiology. The heart rate is often > 200 bpm with little or no beat-to-beat variation. The QRS is narrow and abnormal P waves may be evident.
Management of SVT. Management includes a 12-lead EKG and cardiac monitoring.3 If the infant is stable, vagal maneuvers such as an ice bag over the face for 15-30 seconds or rectal stimulation may disrupt and terminate the abnormal rhythm. Carotid massage or orbital pressure is not recommended in children. IV access, ideally placed in the antecubital area or similarly proximal site, with a 3-way stopcock is useful for the administration of adenosine (0.1-0.2 mg/kg) by rapid IV push with saline flush. A side effect of adenosine is apnea, so the patient’s airway should be closely monitored. If adenosine fails to convert the SVT, the dose may be doubled, and repeated doses every 2 minutes may be given to a maximum of 12 mg. Procainamide (< 1 year old: 7-10 mg/kg IV over 30 min; >1 year old: 15 mg/kg IV) is a second line agent that has the benefit of not provoking accessory pathway conduction in WPW syndrome. Verapamil (0.1-0.3 mg/kg IV) is also an alternative pharmacologic option, although it is contraindicated in children less than 1 year old and is no longer recommended by PALS.4 An unstable infant with poor perfusion should promptly undergo synchronized cardioversion (0.5-1 J/kg).
Prompt consultation with cardiology is needed for definitive management of the arrhythmia. In the absence of WPW syndrome, long-term treatment may include digoxin. If WPW syndrome is the underlying abnormality, propranolol is the preferred long-term agent.
CME Question
A 2-week-old infant presents with a heart rate > 220 bpm and no beat-to-beat variability on the monitor. The infant is afebrile and appears well. An EKG shows a heart rate of 228 bpm; abnormal or absent P waves are noted. The following statements about this infant are true:
- Supraventricular tachycardia is most likely present.
- WPW is the most common underlying etiology.
- The treatment may include administration of adenosine.
- All of the above
Start or Resume CME Test (Opens in a new Tab/Window)
CME Question
A newborn is seen for irritability and a heart rate > 220 bpm and no beat-to-beat variability on the monitor. The infant is afebrile and appears well. An EKG shows a heart rate of 228 bpm, abnormal or absent P waves are noted. The following is true regarding the treatment of this infant:
- Adenosine 0.1 mg/kg rapid IV push.
- Verapamil should be used acutely.
- Initial treatment is cardioversion with 2 J/kg.
- No treatment is necessary.
Start or Resume CME Test (Opens in a new Tab/Window)
Bradyarrhythmias
The definition of bradycardia varies by age. Neonatal Resuscitation Program (NRP) defines bradycardia as a HR < 100 bpm in newborns. PALS uses <60 bpm as its standard criterion for infants and children.3
Sinus bradycardia in the neonate may occur normally during sleep or with increased vagal stimulation, including nasal suctioning, laryngoscopy, and vagal maneuvers such as defecation. This is often transient, and the respiratory rate, blood pressure, and capillary refill time are normal during these episodes.
The most common non-cardiac cause of bradycardia in infants is hypoxemia. Elevated intracranial pressure, electrolyte abnormalities, and drug overdoses are also important etiologies.
First-degree AV block. PR interval is > 0.15 seconds in first-degree AV block. Bradycardia may occur due to medications such as digoxin or propranolol. Hypothyroidism, myocarditis, and AV canal may be the underlying cause of first-degree AV block.
Second-degree AV block may occur due to congenital heart disease, myocarditis, cardiomyopathy, cardiac postoperative changes, digoxin effect, or maternal lupus.
- Mobitz I/Wenkebach phenomenon –progressive lengthening of the PR interval until a QRS complex is not conducted.
- Mobitz II – a constant PR interval and intermittent loss of conduction of P wave; potential exists to degenerate into complete heart block.
Third-degree or complete heart block (AV Dissociation) is the absence of conduction of atrial activity to the ventricles. Potential etiologies include AV canal defect, maternal lupus, drug overdose, or postoperative complication.
National Guideline/Academic Resource
American Academy of Pediatrics and American Heart Association. Neonatal Resuscitation Program Textbook, 6th ed.; 2011. http://circ.ahajournals.org/content/122/18_suppl_3/S876.full
Management of Bradyarrhythmias
The goal of management of bradyarrhythmias is to treat the underlying cause if possible. Supplemental oxygen should be provided if the child is hypoxemic. If there are signs of poor perfusion or respiratory compromise but a pulse is present, it is important to maintain the airway and provide assisted ventilation and oxygen.5 If the bradycardia resolves with these measures, continue supportive care and obtain a cardiology consult. Intravenous or intraosseous access should be obtained. A 12-lead EKG is recommended. If the bradycardia persists with cardiopulmonary compromise despite the initial measures, the use of medications such as epinephrine (0.01 mg/kg or 0.1 mL/kg of the 1:10,000 concentration IV or IO) is indicated. This may be repeated every 5 minutes. It may be given via the ETT if IV or IO access is unavailable. The ETT dose is 0.1 mg/kg or 0.1 mL/kg of the 1:1000 concentration. Atropine (0.02 mg/kg, minimum dose of 0.1 mg) is indicated for bradycardia secondary to increased vagal tone or primary AV block. Transthoracic or transvenous pacing may be indicated. Cardiopulmonary compromise exists if there is hypotension, with altered mental status and signs of shock. If pulseless arrest occurs, chest compressions should be begun immediately and the pulseless cardiac arrest algorithm should be initiated
CME Question
A 1-week-old infant is referred to the ED by the pediatrician due to poor feeding and decreased activity. The initial heart rate is 70 bpm on the monitor. The heart rate then decreases to 50 bpm and the infant becomes apneic. The immediate management of this patient is:
- Oxygenation and airway management.
- Intravenous or intraosseous epinephrine 0.01 mg/kg (1:10,000).
- Chest compressions.
- Atropine 0.02 mg/kg.
Start or Resume CME Test (Opens in a new Tab/Window)
Congestive Heart Failure
Congestive heart failure (CHF) may occur due to volume overload, excess afterload, impaired contractility, or arrhythmias. In structurally normal hearts, common causes include cardiomyopathy, myocarditis, myocardial ischemia (usually associated with anomalous left coronary arteries in the first few months of life), and arrhythmias. Children with congenital heart defects, including ventricular septal defects, atrioventricular septal defects, patent ductus arteriosus, and large atrial septal defects, often develop large left-to-right shunts resulting in fluid overload. Infants with CHF typically present with sweating, feeding difficulties, failure to thrive, tachypnea, tachycardia, respiratory distress, wheezing, peripheral edema, hepatomegaly, gallop rhythm, cyanosis or shock.
Cardiac Etiologies of Congestive Heart Failure in Neonates With or Without Shock
- Left to right shunt: Large VSD, AV malformations, AV canal, large PDA
- Right to left shunt: TGA, TAPVR, truncus arteriosus
- Decreased left ventricular output: hypoplastic left heart syndrome, critical aortic stenosis, interrupted aortic arch
- Cardiomyopathies
- Tachyarrhythmias (usually SVT)
- Coronary artery fistula or anomalous origin.
The major goals of treatment are relief of systemic and pulmonary congestion, improvement of myocardial performance, and reversal of the underlying disease if possible. Treatment should be initiated in conjunction with a pediatric cardiologist to stabilize the patient while arranging inpatient admission. Potential treatments include inotropic therapy, diuretics, and afterload reduction.
National Guideline/Academic Resource
https://circ.ahajournals.org/content/122/18_suppl_3/S909.full.pdf+html
CME Question
An infant has poor feeding, with sweating during feeds, and shortness of breath. Cardiac causes of congestive heart failure include:
- Large ventricular septal defect.
- Atrioventricular canal.
- Large patent ductus arteriosus.
- Cardiomyopathy.
- All of the above.
Start or Resume CME Test (Opens in a new Tab/Window)
|
Lesion |
Exam |
Diagnosis |
Management |
|---|---|---|---|
|
Lesions presenting with shock: Hypoplastic left heart Critical aortic stenosis Coarctation of aorta Interrupted aortic arch |
Tachycardia, hypotension, poor perfusion, cyanosis. Midsystolic murmur Systolic murmur Murmur from other defects |
CBC, BC, CMP, to rule out other forms of shock. RVH, LVH CXR: CM, PVC RAD CXR: CM, PVC RAD, RVH CXR: CM, PVC RAD, RVH CXR: CM, PVC |
Maintain airway. Oxygen and cardiac monitoring. Antibiotics IV. Preductal (right upper) oximetry and blood pressure. IV access. NS bolus 10 mL/kg. Alprostadil 0.05-0.1 mcg/kg/minute) to open the closed ductus arteriosus. Urgent pediatric cardiology consultation. |
|
Lesions that may present with congestive heart failure (CHF): ASD, VSD, PDA, AV Canal |
Respiratory distress, diaphoresis, failure to thrive, tachypnea, tachycardia, murmur, wheezes, rales, hepatomegaly, gallop rhythm, cyanosis |
CBC, BC, CMP, BNP ABG CXR: CM, PVC, hyperinflation |
Airway management, oxygen. Elevate head of bed. Furosemide 0.5-1 mg/kg/dose IV. Dopamine 5-10 mcg/kg/min if poor contractility. Dobutamine 2.5-20 mcg/kg/min titrated to improve contractility and reduce afterload. Milrinone loading dose 50 mcg/kg over 15 minutes, then maintenance of 0.35-0.75 mg/kg/min. Improves inotropy and produces pulmonary and systemic vasodilation. |
|
Tet Spell |
Infant with TOF presenting with severe cyanosis |
Increase SVR and decrease shunting from right to left via the VSD. Calm infant. Knee to chest position. Increase SVR and decrease shunting right to left via the VSD. Calm infant. Knee to chest position Morphine (0.1-0.2 mg/kg/dose) IM, SC or IV IV access. NS bolus 10-20 mL/kg to increase preload. Sodium Bicarbonate (1 mEq/kg) IV for acidosis. Ketamine (1-2 mg/kg) IV or IM for sedation to help increase SVR. Phenylephrine (5-20 mcg/kg/dose) IV to increase SVR. Paralysis and intubation if needed |
Congenital Heart Disease References
- Silberbach M, Hannon D. Presentation of congenital heart disease in the neonate and young infant. Pediatr Rev 2007;28:123-131.
- Thangaratinam S, Daniels J, Ewer AK, et al. Accuracy of pulse oximetry in screening for congenital heart disease in asymptomatic newborns: A systematic review. Arch Dis Child Fetal Neonatal Ed 2007;92:176-180.
- Kleinman ME, Chameides E, Schexnayder SM, et al. Part 14: Pediatric Advanced Life Suppport: 2010.American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010;122(18 suppl 3):s876-908.
- Hansmann G. ed Neonatal Emergencies. A Practical Guide for Resuscitation, Transport and Critical Care of Newborn Infants. Cambridge University Press 2009.
- Dawson JA, Kamlin CO, Vento M, et al. Defining the reference range for oxygen saturation for infants after birth. Pediatrics 2010;125:e1340-1347.
- Stark AR, Levels of neonatal care. Pediatrics 2004; 114(5): 1341-712.
