Post Intensive Care Syndrome: Risk Factors and Prevention Strategies
March 1, 2015
Reprints
By Leslie A. Hoffman, RN, PhD, and Jane Guttendorf, DNP, RN, CRNP, ACNP-BC, CCRN
Dr. Hoffman is Professor Emeritus, Nursing and Clinical & Translational Science, University of Pittsburgh, and Jane Guttendorf is Assistant Professor, Acute & Tertiary Care, University of Pittsburgh, School of Nursing
Dr. Hoffman and Jane Guttendorf report no financial relationships relevant to this field of study.
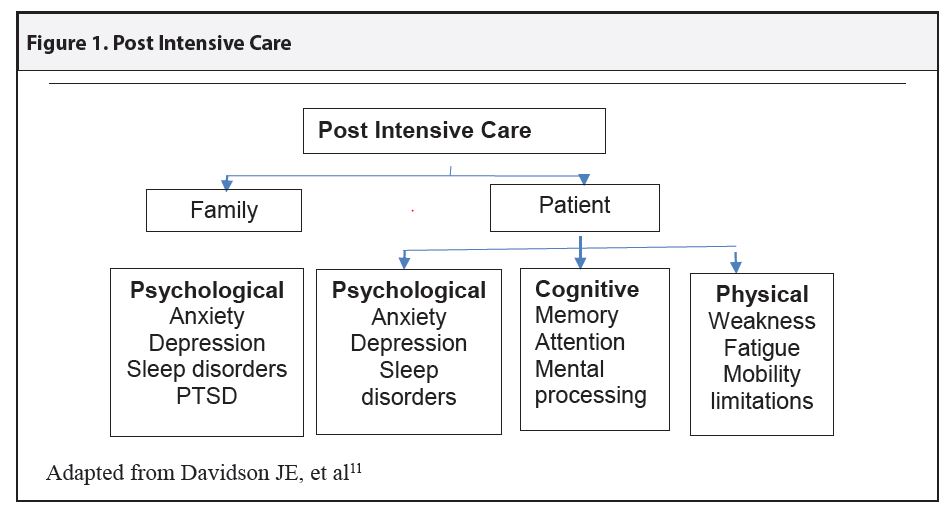
What is post intensive care syndrome (PICS)? Each year, approximately 800,000 patients in the United States develop an illness that results in admission to an ICU and need for mechanical ventilation.1 Most survive to hospital discharge. This transition, while positive, often begins a new, challenging phase of recovery. ICU survivors, particularly those who require prolonged mechanical ventilation, experience high mortality.2 Compromises in physical, psychological, and/or cognitive function are common.1-4 Both patients and family caregivers are at risk for symptoms of anxiety, depression, posttraumatic stress disorder (PTSD), and sleep disorders.5 Studies suggest that as many as 40% of ICU survivors and family members experience physical, psychological, and/or cognitive dysfunction.2-5 Termed post intensive care syndrome, this consequence is defined as “new or worsening impairment in physical, cognitive, or mental health status arising after critical illness and persisting beyond discharge from the acute care setting.”6 Both patients and family caregivers may be affected, a consequence termed PICS (patient) or PICS-F (family member).6 This review will discuss risk factors, clinical manifestations, and strategies for prevention and management of PICS.
SCOPE OF THE PROBLEM
PICS is a common and persistent, with symptoms lasting for months to years after ICU discharge. The following is a summary of findings from selected studies that illustrate the scope of the problem:7
- 85%-95% of patients with ICU-acquired weakness have symptoms that last for 2-5 years or longer.
- 74% of ICU survivors diagnosed with acute respiratory distress syndrome have cognitive impairment at ICU discharge and 25% 6 years after ICU discharge.
- 10%-50% of ICU survivors experience symptoms of depression, anxiety, PTSD, and sleep disturbance, which may persist for years.
- 50% of ICU survivors require caregiver assistance 1 year later.
- 33% of family caregivers have symptoms of depression and 70% have symptoms of anxiety.
- 33% of family members have symptoms of PTSD, which can persist for 4 years or longer.
RISK FACTORS
Commonly-cited risk factors for PICS include ICU-related factors (e.g., delirium, deconditioning, severity of illness) and pre-existing patient factors (e.g., dementia, comorbidity). Findings from the BRAIN-ICU study, which evaluated risk factors and incidence of neuropsychological dysfunction in more than 800 medical and surgical ICU survivors, indicated that 70% of patients developed delirium during the hospitalization, and longer duration of delirium in the ICU was associated with worse global cognitive and executive function at 3 and 12 months following ICU discharge.8 While this and other studies have identified a variety of risk factors, they are extensive in number and not particularly helpful because many critically ill patients share these characteristics.
Recent literature suggests that measures of pre-existing frailty, obtained retrospectively following ICU admission, and ICU-acquired weakness, obtained at ICU discharge, may be more predictive. This focus supports the intuitive observation that those who enter or leave the ICU with considerable deficits are at greatest risk. Bagshaw and colleagues9 recently explored the ability of the Canadian Study on Health and Aging Clinical Frailty Scale, a well-validated 9-point assessment tool, to identify vulnerable patients less likely to tolerate critical illness. In this prospective multicenter study (six ICUs, 421 patients), frailty was common, affecting 33% of participants. Frail patients had longer stays in ICU and greater mortality 12 months after admission. Frail patients were more likely to experience new functional dependence at hospital discharge and worse health-related quality of life. These outcomes persisted after adjusting for demographic factors, pre-admission health status, comorbidities, and illness severity. Findings of this study are particularly interesting as a simple 9-item questionnaire was able to identify patients most likely to experience post-discharge limitations. Similar findings were reported by Hermans and colleagues10 from a study that focused on the impact of ICU-acquired weakness on recovery.
CLINICAL MANIFESTATIONS
PICS can manifest in a variety of ways. Common symptoms include fatigue, weakness, limited mobility, anxiety, depressed mood, sleep disorders, and mental processing issues (e.g., preparing a meal, remembering appointments, shopping, etc). The burden of caregiving often leads to similar psychological symptoms in family caregivers.
PREVENTION AND MANAGEMENT ABCDE BUNDLE
|
Table 1. Recommendations for Improving Long-term Outcomes for ICU Survivors |
1. Provide high-quality acute intensive care. This should include resuscitation and initial stabilization but also evidence-based ventilator and sedation management, minimizing duration of mechanical ventilation.
2. Implement a process that enables structured assessment of pre-existing limitations and limitations that develop during critical illness.
3. Involve rehabilitation experts as early as possible. Such experts include physical therapists, occupational therapists, social workers, physical medicine, and geriatrics.
4. Provide the patient and family with education about resources that may assist in promoting rehabilitation and providing support. Recognize that patients are unlikely to seek and find resources independently.
5. Arrange close follow-up and work to avoid fragmentation of care by structured, routine hand-offs to both hospitalists and outpatient providers.
6. Find a way to get feedback on patients’ long-term outcomes so team members can learn from these experiences.
A consistent body of literature supports the benefits of mobility for ICU patients.12 Achieving the goal of mobilization requires clinician acceptance of a culture of mobility and work to promote this goal by all members of the healthcare team.11 The best way to achieve this goal appears to be through a protocol, such as the Awakening, Breathing, Coordination with daily sedation interruption and ventilator weaning, Delirium monitoring and management and Early ambulation when feasible (ABCDE) protocol.12 Benefits of daily awakening to determine ability to wean from mechanical ventilation, delirium monitoring and appropriate choice of medications, and early mobilization are well established and include reduced ICU and hospital lengths of stay, as well as decreased prevalence of delirium and shorter delirium duration.12-14 This is important because longer delirium duration is associated with increased odds of disability.8,13
ICU DIARIES
There is increasing evidence that unpleasant or delusional memories of the ICU experience are associated with distress after ICU discharge.15-18 Use of an ICU diary maintained prospectively during the patient’s ICU stay by family members, health care providers, or both, has been shown to decrease the incidence of PTSD when measured in randomized trials.16 It is thought that diaries assist patients in establishing factual memories, lost during their ICU stay.15-17 The Intensive Care Experience Questionnaire has been developed specifically for the purpose of measuring patients’ recall of their experience while in the ICU and may facilitate identifying those with distressing memories.15
SUPPORT GROUPS
Support groups have been shown to be a beneficial way to increase coping skills and resilience. Provision of a time and place where family members and friends of patients can meet to support each other while they are in the ICU and patients, friends, and family members of discharged ICU patients can meet to support after ICU discharge, with group leadership by a health care team member, offers another means to support caregivers and improve outcomes.
TEAM BUILDING
Families and, at times, the bedside nursing staff may not be included in daily patient care rounds. Reasons are multiple as are the adverse effects of this practice on team spirit. Family caregivers are an essential part of care following ICU discharge and can greatly benefit from being involved in care prior to discharge.18
PUBLIC AND PROFESSIONAL AWARENESS
An extensive body of literature describes challenges faced by ICU survivors. However, recognition of the scope and persistence of these challenges is relatively recent. The term PICS was created to focus attention on problems faced by ICU survivors and their family members and promote greater awareness. A number of resources exist for patients and families, including a Society of Critical Care Medicine (SCCM) webpage that provides education and resources to assist patients/families in understanding care in the ICU and problems that may be encountered after discharge, including content specific to PICS (http://www.myicucare.org/Adult-Support/Pages/Post-Intensive-Care-Syndrome.aspx). Patients and families should receive specific education about cognitive and psychiatric symptoms, as well as the physical signs and symptoms that may signal PICS. As most survivors of critical illness are not cared for by critical care providers during the follow-up period, extending education about risks and detection of PICS to primary care providers is important.
SYNTHESIS
The traditional view of ICU survivorship is that it is an issue to be addressed after recovery from critical illness and discharge from the ICU. Current practice with stroke, trauma, and cardiac surgery patients suggests that targeted care during critical illness has the potential to reduce symptoms of PICS. Iwashyna and Netzer19 propose the steps shown in Table 1 as a means to better assist patients and families cope with the challenges faced following ICU discharge. Notably, they advise that assessment begin prior to ICU discharge, handoffs to post-ICU care providers be specific, and feedback be obtained from patients and families to aid in better addressing issues they encounter and share potential solutions.
FUTURE DIRECTIONS
Additional research is needed in many areas with regard to evaluating long-term outcomes of ICU survivors. Further characterization of the associations between potentially modifiable physiologic predictors of PICS and outcomes, evaluation of interventions to reduce the use of ICU sedation, promote earlier awakening and extubation, active assessment for and treatment of delirium, and focused interventions to promote sleep, exercise, and mobility in ICU patients are all important targets for study. Benefits of aggressive post-ICU care to promote physical recovery and restoration of muscle strength is another important area for study. Developing models of focused follow-up care of ICU survivors, which include intensivists and other multidisciplinary team members interested in specifically recognizing and treating PICS, may prove beneficial.
CONCLUSION
Critical care clinicians have the potential to improve the long-term functioning and quality of life of the increasing number of patients surviving critical illness by initiating structured interventions to assess the extent of risk, test interventions to improve outcomes, and obtain stakeholder input from all involved (critical care and non-critical care clinicians, patients, families, support services) to affect continuous improvement. The ultimate goal is to improve the patient/family care experience during and following ICU discharge.
REFERENCES
- Elliott, D, et al. Exploring the scope of post-intensive care syndrome therapy and care: Engagement of non-critical care providers and survivors in a second stakeholders meeting. Crit Care Med 2014;42:2518-2526.
- Desai SV et al. Long-term complications of critical care. Crit Care Med 2011;39:371–379.
- Jackson, JC, et al. Depression, post-traumatic stress disorder, and functional disability in survivors of critical illness in the BRAIN-ICU study; a longitudinal cohort study. Lancet Respir Med 2014; 2:369-379.
- Jubran A, et al. Post-traumatic stress disorder after weaning from prolonged mechanical ventilation. Intensive Care Med 2010;36: 2030-2037.
- Davidson JE, et al. Family response to critical illness: post-intensive care syndrome-family. Crit Care Med 2012;40:618–624.
- Needham DM, et al. Improving long-term outcomes after discharge from intensive care unit: Report from a stakeholders’ conference. Crit Care Med 2012;40:502–509.
- Harvey MA. The truth about consequences — post intensive care syndrome in ICU survivors and their families. Crit Care Med 2012;40:2506-2507.
- Pandharipande PP, et al. Long-term cognitive impairment after critical illness. N Engl J Med 2013;369:1306-1316.
- Bagshaw SM et al. Association between frailty and short and long-term outcomes among critically-ill patients: A multicenter prospective cohort study. CMAJ 2014;186(2):E95-102.
-
Hermans G et al. Acute outcomes and 1-year mortality of ICU-acquired weakness. Am J Respir Crit Care Med 2014;190:
410-420. - Davidson JE, et al. Post-intensive care syndrome: what it is and how to help prevent it. Am Nurse Today 2013;8:32–36.
- Balas MC et al. Effectiveness and safety of the awakening and breathing coordination, delirium monitoring/management, and early exercise/mobility bundle. Crit Care Med 2014;42:1024-1036.
- Brummel, NE, et al. L. Delirium in the ICU and subsequent long-term disability among survivors of mechanical ventilation. Crit Care Med 2014;42:369-377.
- Reade MC and Finfer S. Sedation and delirium in the intensive care unit. N Engl J Med 2014; 370:444-454.
- Aitken LM and Marshall AP. Monitoring and optimizing outcomes of survivors of critical illness. Intensive Crit Care Nurs 2015;31:1-9.
- Jones C, et al. Intensive care diaries reduce new onset posttraumatic stress disorder following critical illness: A randomized, controlled trial. Crit Care 2010;14:R168.
- Garrouste-Orgeas M, et al. Writing in and reading ICU diaries: Qualitative study of families’ experience in the ICU. PLoS One 2014;9:e110146.
- Cypress BS. Family presence on rounds: A systematic review of literature. Dimens Crit Care Nurs 2012;31:53-64.
- Iwashyna TJ and Netzer G. The burdens of survivorship: An approach to thinking about long-term outcomes after critical illness. Semin Respir Crit Care Med 2012;33:327–338.
Each year, approximately 800,000 patients in the United States develop an illness that results in admission to an ICU and need for mechanical ventilation.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
