Submersion and Drowning Injuries
May 1, 2015
Reprints
Related Articles
-
Is Artificial Intelligence Coming for Your Job?
-
Can Pulmonary Artery Pressure Help in the Decision to Operate in Chronic Aortic Regurgitation?
-
Combined TAVR and LAAO Studied in a Randomized Controlled Trial
-
Another Hemodynamic Variant of Aortic Stenosis
-
Clinical Features of Tachyarrhythmia-Induced Cardiomyopathy
Authors
Sara W. Nelson, MD
Department of Emergency Medicine,
Maine Medical Center,
Assistant Professor of Emergency Medicine,
Tufts University School of Medicine.
Scott C. McCorvey, MD
Maine Medical Center,
Portland, ME.
Peer Reviewer
Ken Zafren, MD, FAAEM, FACEP, FAWM
Emergency Medical Services Medical Director,
State of Alaska;
Clinical Professor,
Division of Emergency Medicine,
Stanford University Medical Center,
Stanford, CA;
Staff Emergency Physician,
Alaska Native Medical Center,
Anchorage, AK.
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Dr. Dietrich (editor in chief), Dr. Nelson (author), Dr. McCorvey (author), Dr. Zafren (peer reviewer), and Ms. Behrens (nurse reviewer) report no relationships with companies related to this field of study. Mr. Landenberger (continuing education and editorial director) and Ms. Mark (executive editor) report no relationships with companies related to the field of study covered by this CME activity.
Executive Summary
- Drowning is a process of primary respiratory impairment from submersion or immersion in a liquid medium in which the airway is covered by liquid.
- Drowning causes a large burden of disease and injury, with more than 500,000 deaths worldwide. Drowning is the second leading cause of unintentional pediatric deaths in the United States. These numbers are likely underreported.
- Patient rescue and immediate resuscitation improve outcomes in drowning victims. Survival trends correlate with the time interval between initial airway compromise and ventilatory efforts.
- The critically ill drowning victim may develop acute respiratory distress syndrome (ARDS), hypotension, and acidemia. Advanced treatment modalities such as NIPPV, intubation, bronchoscopy, post-arrest cooling, and ECMO may be necessary.
Submersion and Drowning Injuries
Unfortunately, drowning remains a too frequent event in the pediatric population. Survival depends on a coordinated effort to minimize the interval between airway compromise and ventilatory efforts. Children younger than 4 years of age and between 15 and 19 years of age are at highest risk. Certain medical conditions, including epilepsy, cardiac disease, and predisposition to cardiac dysrhythmias (for example, prolonged QT syndrome), increase a child’s risk of drowning. The authors review the critical aspects for the evaluation and management of a child who has sustained a drowning injury.
- Ann M. Dietrich, MD, Editor
Introduction
The purpose of this article is to review the definitions, epidemiology, pathophysiology, prehospital management, emergency department management, and advanced treatment modalities in patients who suffer submersion and drowning injuries. This article will review risk factors for drowning, pathophysiology of drowning, and management guidelines. We will present a systematic approach for both prehospital care and definitive care once the patient arrives in the emergency department. Finally, we will present common pitfalls in evaluating a suspected drowning patient, and will make recommendations regarding the initial evaluation and the ultimate disposition of these patients.
Definitions
Drowning. For the past 40 years, multiple entities and authors have tried to define the medical phenomena that follow a submersion injury.1 A publication by the International Liaison Committee on Resuscitation (ILCOR) highlighted this as they discussed confusion around “delayed death subsequent to near drowning, drowning without aspiration, near drowning without aspiration, near drowning with aspiration, dry drowning, wet drowning, silent drowning, active drowning, passive drowning, and secondary drowning.”2 Confusing terminology and inconsistencies in the literature have stymied efforts to track and characterize the efficacy of therapeutic interventions and to study the epidemiology of disease.
At the World Congress on Drowning, held in Amsterdam in 2002, participants came together and agreed upon a common definition for the medical sequelae surrounding submersion injuries. At this conference, drowning was defined as “a process resulting in primary respiratory impairment from submersion/immersion in a liquid medium. Implicit in this definition is that a liquid/air interface is present at the entrance of the victim’s airway, preventing the victim from breathing air.”2
The ILCOR recommends that the terms dry and wet drowning, active and passive drowning, near drowning, and secondary drowning no longer be used as they are confusing and not clinically relevant. Instead, a simpler, more uniform “Utstein” style of terminology should be used.2
In accordance with the ILCOR guidelines, patients should be referred to as drowning victims if they have suffered a suspected respiratory injury following submersion in a liquid medium, regardless of their clinical status, which may vary from essentially asymptomatic to severely ill at time of presentation. Additional descriptors such as whether there was a precipitating event that led to drowning or whether the drowning was witnessed may be used as necessary. The primary outcome of a drowning episode is either death or survival. Adopting this clinical nomenclature will allow future studies to better characterize, study, and risk stratify drowning victims.
Immersion. To be immersed is for a body part to be covered in a liquid medium; it does not require the entire body to be underwater. For an immersion victim to drown, the oral and nasal airways must be under water or other liquid medium, limiting the victim’s ability to breath.
Submersion. To be submersed is for the entire body to be covered in a liquid medium. Explicit in this definition is that the airway, in its entirety, is under the liquid medium.
Interval Time. Survival trends directly correlate with the time between initial airway compromise and ventilatory efforts by either the victim, spontaneously, or through the rescuer through basic life support.3-5 This time difference is known as the interval time.
Epidemiology
Drowning accounts for more than 500,000 deaths worldwide each year. Despite this staggering number, drowning deaths are thought to be underreported, due in part to the confusing nomenclature used to classify these deaths.1,6 Ninety-seven percent of deaths from drowning occur in low- and middle-income countries, and in many regions of the world drowning is either the first or second leading cause of death in the pediatric population.7,8 Although the incidence of pediatric death due to drowning in the United States has significantly decreased over the past 30 years (2.68 per 100,000 children to 1.96 per 100,000), it is still a frequently encountered injury pattern and an area in which physicians should be well versed.9
The leading cause of death in the United States between 2006-2010 among children (1-18 years of age) was unintentional injuries.10 In the Center for Disease Control’s database on all-cause mortality, drowning was responsible for roughly 4500 deaths during this time period, which equates to roughly 12% of all pediatric deaths. This is second only to motor vehicle crashes. To put this into perspective, more children died from drowning in the United States between 2006 and 2010 than from sepsis, chronic lung disease, influenza, and pneumonia combined. For all age groups, there were more than 17,000 U.S. deaths from drowning during this same time period.10
A study by Burford et al. showed that age, gender, and ethnicity are all independent risk factors for drowning in the United States.11 There is a bimodal distribution of drowning deaths, with children having the highest risk between 0-4 years of age and 15-19 years of age. Males are at higher risk of death from drowning than females in all age groups. Overall, African-American children are more likely to suffer a drowning-related death than Caucasian children, except between 0-4 years of age. In this age group, Caucasian children are more likely to drown than their African-American counterparts. This is thought to be due to greater access to residential pools for Caucasians in this age group.
The location of drowning, particularly pediatric drowning, has been well studied.9,12-14 In the United States, children younger than the age of 1 year most often drown in bathtubs, buckets, and toilets, while children ages 1 to 4 are more likely to drown in a pool. It is often under appreciated that young children can drown in as little as 5 cm of water.9 After the age of 4, children and adolescents are more likely to drown in open water. Almost 50% of all fatalities occur in open water.10,14
Additional risk factors associated with drowning of infants and toddlers are unsupervised bath/pool time and the use of bath seats while in the bathtub.9 In the adolescent population, the majority of drownings are related to risky behavior, such as the use of alcohol or illicit drugs, or diving-related trauma.15,16 In all age groups, medical conditions such as epilepsy, cardiac disease, and predisposition to cardiac arrhythmias (e.g., prolonged QT syndrome) increase the risk of drowning. (See Table 1.)
Pathophysiology of the Drowning Process
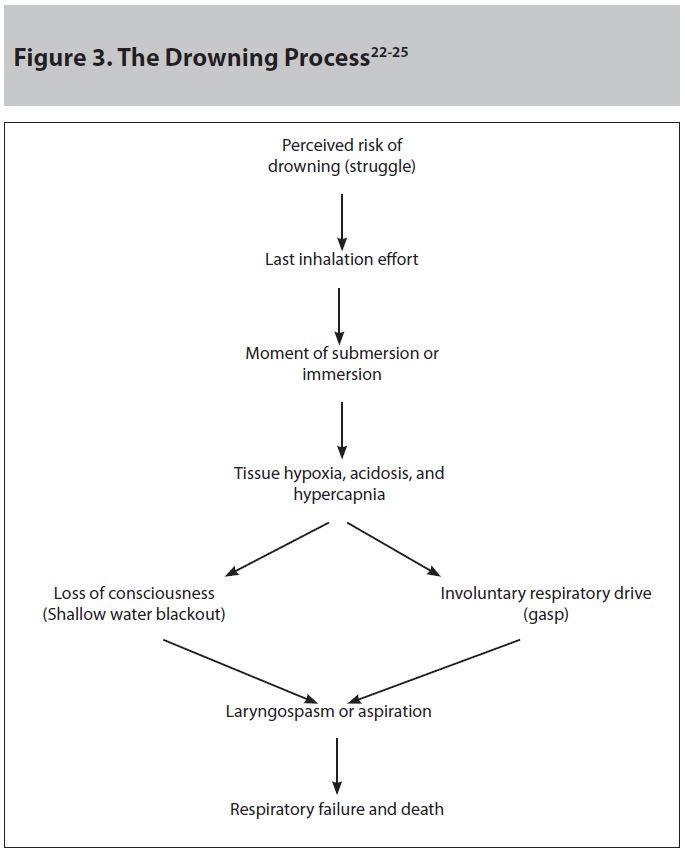
The Drowning Process. The “drowning process” is the stepwise progression of events leading to respiratory failure, hypoxia, and death.17-19 (See Figure 3.) When the human body is submersed, there is an unconscious drive to breath-hold. Breath holding occurs when the victim closes the larynx to prevent air from being inhaled or exhaled. Once submersed, the victim will quickly deplete oxygen stores. As the drowning process continues, the victim becomes progressively acidotic, hypoxic, and hypercapnic. Hypercapnia is the primary stimulus of the respiratory drive.20 If the victim hyperventilates prior to the incident, there may be a loss of consciousness from cerebral hypoxia prior to feeling the hypercapnic drive to breathe, a phenomenon referred to as “shallow water blackout.”21 This phenomenon is sometimes seen in swimming competitions and in military training. Without hyperventilation, the victim will swallow water due to involuntary inspiration caused by the hypercapnic respiratory drive. In rare cases of laryngospasm, no initial aspiration of water will occur. However, eventually there is a relaxation of the laryngospasm, likely due to both cerebral hypoxia and tissue fatigue, and the victim usually aspirates.
The amount of fluid ingested during the drowning process varies among victims, but ingestion of water is thought to be the main contributing factor to the vomiting seen in the majority of drowning victims.2,22
Please see the simplified flow diagram for the progression of the drowning process and prognostic factors in drowning victims. (See Figure 3.)
Cardiovascular and Pulmonary Systems. The cardiovascular system undergoes a variety of changes prior to and during the drowning process. Starting from the first moment of immersion, there is an increase in systemic venous return from compressive forces on the upper and lower extremities and, in cold water, from peripheral vasoconstriction. These processes result in central hypervolemia. This causes an elevation in sensed circulatory volume that results in increased myocardial stretch, increased pulmonary artery pressure, and an increase in stroke volume, leading to increased cardiac output.23 In patients with pre-existing illness, such as congestive heart failure or pulmonary hypertension, central hypervolemia can be lethal.
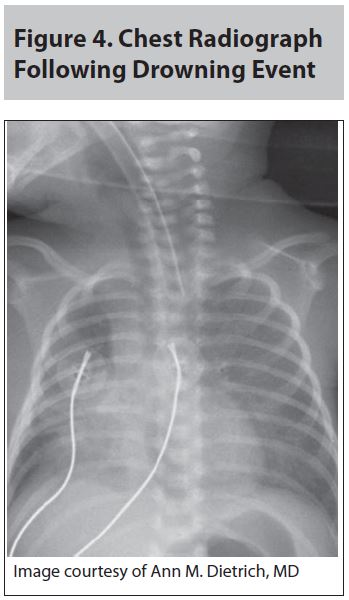
The pulmonary system undergoes tremendous changes following a submersion event and drowning. As little as 1-3 mL/kg of water may be sufficient to compromise surfactant in the alveoli, leading to alveolar collapse, shunting, and V/Q mismatch. This damage can lead to profound hypoxia, tachypnea, acid/base disturbances, and, ultimately, acute respiratory distress syndrome (ARDS). In addition, as fluid enters the lung, there is a potential osmotic shift between the alveoli and the systemic circulation, worsening the alveolar collapse. Finally, the aspirated medium may carry debris and infectious organisms, which can promote lung infections.24 Following a significant aspiration event, there is often early evidence of intra-alveolar consolidation. It can be very difficult to differentiate infection from aspiration pneumonitis in the acute setting. (See Figure 4.)
Renal System. The kidney plays an important role in the regulation of hemodynamic stability and fluid balance during and after the drowning process. As discussed above, following a submersion event, the victim may experience shunting of blood to the core, known as “central hypervolemia.”25,26 The increase in circulatory pressure in the thorax and abdomen promotes natriuresis and diuresis through a rapid and elegant series of neuroendocrine feedback systems. Atrial natriuretic peptide, an endocrine hormone released from the myocardium due to increased myofibril stretching, causes increased glomerular blood flow, decreased free water reabsorption, and decreased vasopressin release from the hypothalamus.25,27-29 Combined, these effects will result in an overall free water deficit and dehydration over time.
Central Nervous System. In drowning, the primary mechanisms of injury to the central nervous system are tissue hypoxia and ischemia. Over the past half-century, numerous clinicians and researchers have attempted to enhance cerebral perfusion in hopes of promoting a favorable neurological outcome after a drowning event. Even after creating an ideal environment for the brain to heal (i.e., normal intracranial pressures, normal glucose levels, permissive hypothermia for the first 12-24 hours after the incident, normal arterial oxygen concentrations, and sufficient cerebral perfusion pressures), there has been no improvement in outcomes. The biggest determinants of outcome and long-term neurologic sequelae are the duration of submersion and the interval time between drowning and ventilation efforts.30 (See Table 2.)
Evaluation and Treatment
Prehospital Care. In the management of the drowning victim, scene safety, rapid extraction, and prompt basic life support are the keys to improve survival.
Rescue and Extrication. Submersion and drowning incidents often occur in bodies of water that pose a potential danger to the rescuers. Prehospital care must be attuned to scene safety to ensure that rescuers are not injured.31 Scene safety is a key concept of wilderness and remote medicine practice. The National Fire Protection Association (NFPA) and other swift water rescue training programs teach the adage “Reach, Throw, Row, Go.”32 These are the four steps in water rescue with “progressively more risk to the rescuer.” Rescuers should start by reaching for the victim with an object, such as a paddle or branch. If this fails, rescuers should throw a flotation device such as a throwbag or personal flotation device (PFD) to the victim. If necessary, rescuers should proceed to take a boat to the victim. As a last resort, rescuers should enter the water to rescue the victim. The U.S. Corps of Army Engineers (USACE) advocates “Reach, Throw, Row, Go for help,” to emphasize that only those trained in water rescue should enter the water and that all others should go for help. (See Figure 1.)
Regardless of the method, rapid, safe extrication of victims from the water is crucial to decrease morbidity and mortality. Rescue and immediate resuscitation by bystanders improve outcomes.33 The reported incidence of cervical spine injury in drowning victims is very low. The American Heart Association (AHA) recommends against routine spinal immobilization during water extrication.34 Unnecessary spinal precautions can delay extrication.35 However, if there are clinical signs of a spine injury or if there is a mechanism of injury that could have damaged the spinal column, such as diving, surfing, or high-speed boating, spine stabilization should be considered during the extrication and rescue, if possible. Airway, breathing, and circulation should always take precedence over stabilization of the spine. (See Figure 2.)
It was once thought rescuers could effectively “drain fluid from the lungs” through actions such as the Heimlich maneuver, abdominal thrusts, or suspending the patient with the head down. These practices have been abandoned. Current AHA Basic and Advanced Cardiac Life Support (BLS and ACLS) algorithms call for standard chest compressions and ventilations for a pulseless drowning victim with the adjunct of suctioning if available.35
For the unconscious drowning victim, the EMS system should be activated. For a patient in cardiopulmonary arrest, an automatic external defibrillator (AED) should be applied as soon as possible and BLS/ACLS algorithms should be followed. In order to avoid endangering rescuers or bystanders, a drowning victim should be removed from the water before attempting defibrillation. Wet clothes should be removed and the chest dried as much as possible before AED pads are placed.31 For all victims of cardiopulmonary arrest, resuscitation should be started as soon as possible at the scene. Patients should be transported to the emergency department (ED) unless there are obvious signs of death (e.g., rigor mortis, dependent lividity, decomposition, decapitation, etc.).35 There have been case reports of successful resuscitation and full neurologic recovery after prolonged submersions, especially in icy water.38-40 According to the 2010 AHA ACLS Guidelines, all victims of drowning who require any form of resuscitation (including rescue breathing) need to be transported to a hospital for evaluation and monitoring, even if they appear well following the event.35
EMS personnel should do a primary survey on all drowning victims, including aggressive airway management and restoration of adequate oxygenation and ventilation.36 If oxygen saturations are less than 92%, supplemental high-flow oxygen should be provided. In patients with persistent hypoxia or respiratory difficulty, positive pressure ventilation, such as continuous positive airway pressure (CPAP) ventilation, should be started. EMS should consider intubation or supraglottic airway devices in patients with decreased level of responsiveness or persistent hypoxia despite high-flow oxygen or CPAP.36 Victims of drowning are at risk for hypothermia, and active external rewarming should be initiated on hypothermic patients as they are transported to the hospital. If there is concern for cervical spine injury, either by mechanism of injury or by exam, the cervical spine should be stabilized.
Emergency Department Care
On arrival in the ED, resuscitation, including ACLS algorithms, should be continued as appropriate. In general victims of drowning will fall onto one of three categories: the asymptomatic patient, the symptomatic patient, and the severely symptomatic patient or patient in cardiopulmonary arrest. (See Table 3.)
The Asymptomatic Patient. Much of the confusion with drowning terminology and classification concerned the asymptomatic or mildly symptomatic patient. By current consensus, a patient who was immersed in a liquid and suffered any sort of respiratory event suffered a drowning. The respiratory compromise may have been subtle, such as coughing or aspirating a small amount of water. Simply being submersed and breath holding does not constitute a drowning event if no respiratory compromise occurred. Sometimes this subtle distinction between drowning and submersion without respiratory compromise is difficult or impossible for the patient or the provider to distinguish. In these cases, a conservative approach and the assumption that a drowning occurred is prudent.
Asymptomatic patients who have suffered a drowning incident have no cough or dyspnea. Their vital signs are normal, without hypoxia or tachypnea, and their chest exam is normal, without crackles or wheezes. There is limited evidence regarding management of these patients. A reasonable approach is to take a complete set of vital signs, including temperature and pulse oximetry, to do a full physical exam, and to look for evidence of pulmonary or traumatic injury.43 A chest X-ray is recommended to look for early evidence of aspiration. While most pulmonary signs and symptoms develop almost immediately after drowning, respiratory symptoms can develop up to 24 hours after the event.42 Most symptoms, however, will develop early. A review of 75 pediatric patients who suffered a drowning in fresh water found that all symptoms developed within seven hours of the event.44
Emergency physicians may choose to discharge asymptomatic drowning victims after they have been evaluated in the ED. This practice is supported by a 1997 paper by Szpilman et al. that proposed a classification system based on 1,831 drowning victims seen over a 20-year period in Brazil. This system risk stratifies patients to very low risk (grade 1) if they had no dyspnea and had normal pulmonary auscultation with or without cough. None of these 1,189 grade 1 patients died in the study follow-up.41 While this grading system has not been prospectively validated, it is reasonable to discharge asymptomatic drowning victims from the ED as long as they receive education and good return precautions. Emergency physicians may also choose a more cautious approach and observe asymptomatic patients for 4-6 hours after the drowning event. This practice is supported by a handful of studies showing that patients with normal exams and normal room air oxygen saturations at 4-6 hours after the drowning event do not deteriorate.43,45
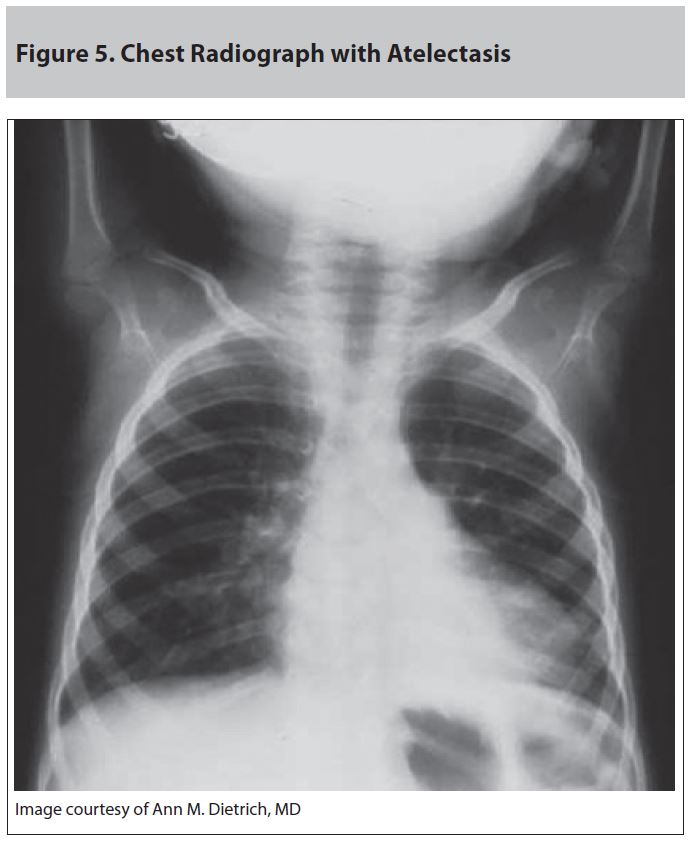
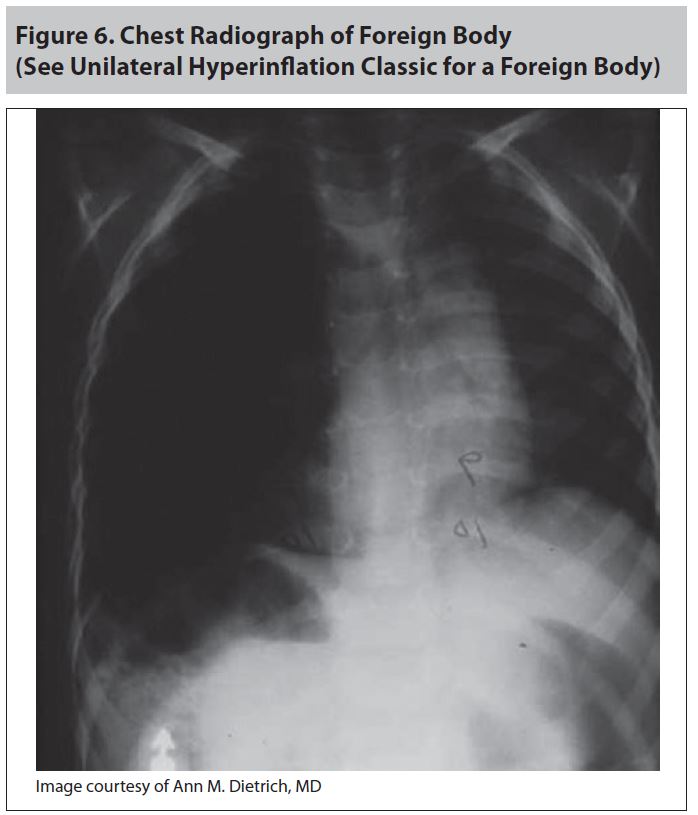
The Symptomatic Patient. The management of mildly to moderately symptomatic victims of drowning is challenging. These patients present with respiratory compromise such as cough, sore throat, or dyspnea. On exam, they may have subtle wheezes or crackles. In these patients, standard ACLS and Advanced Trauma Life Support (ATLS) protocols should be followed with a focus on airway, breathing, circulation, and spinal stabilization as indicated. A full set of vital signs should be taken, including temperature. Oxygen should be given to maintain an oxygen saturation of greater than 92%. Wet clothing should be removed and rewarming should be started on any hypothermic patient. Patients should be placed on telemetry to monitor for dysrhythmias. A chest X-ray should be performed to look for evidence of aspiration, pneumonitis, atelectasis (see Figure 5), pulmonary edema, and inhaled foreign bodies (see Figure 6).
It is not uncommon for drowning victims to suffer aspiration pneumonitis. This is a chemical pneumonitis. Antibiotics can be held unless the patient develops clinical signs of pneumonia such as fever, leukocytosis, new or persistent consolidation on X-ray, or a new oxygen requirement.46 Only a small percentage of drowning victims will develop a clinical pneumonia. There is no evidence to support the routine use of prophylactic antibiotics for patients who drowned in clean water. Because of the risk of bacterial lung infections, antibiotics should be given to patients who were submersed in grossly contaminated water (e.g., water containing sewage or manure).47 Empiric steroids are thought to be ineffective for drowning victims, but inhaled bronchodilators should be considered for the bronchospasm that is often seen in non-fatal drowning.19
Basic labs, including electrolytes and coagulation panels, should be sent on drowning victims who are symptomatic. As stated earlier, prolonged submersion and drowning events may cause intravascular volume changes and may promote diuresis and dehydration. In addition there is a theoretical risk of electrolyte changes and coagulopathies from inhaling or swallowing large amounts of fresh or salt water. While electrolyte shifts have been seen in animal models with large volume aspirations,20,48,49 such shifts have not been found in human studies.50
Mildly to moderately symptomatic patients and patients with abnormal vital signs, including low oxygen saturation, should be admitted for observation and supportive care for at least 6-24 hours.44,46 The length of admission depends on clinical status. Patients should not be discharged until symptoms have resolved.
Severely Symptomatic/Cardiopulmonary Arrest Patients. When a severely symptomatic victim of drowning arrives in the emergency department, ACLS, ATLS, and emergency stabilization guidelines should be followed with a focus on prompt correction of hypoxemia and acidosis.
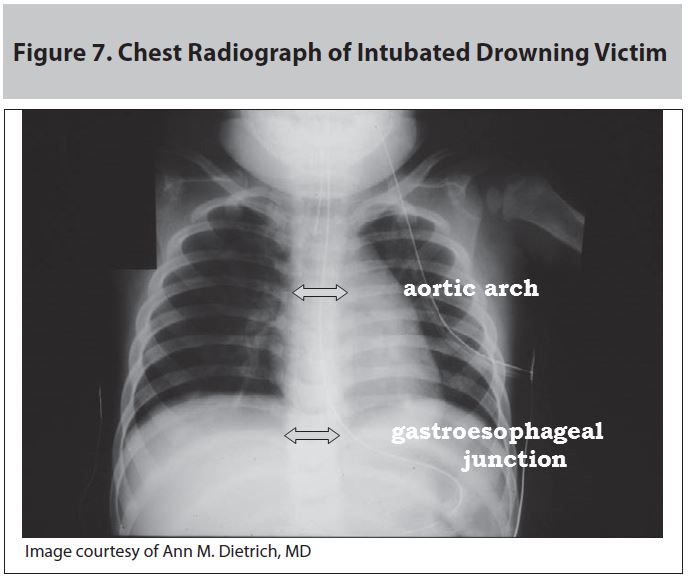
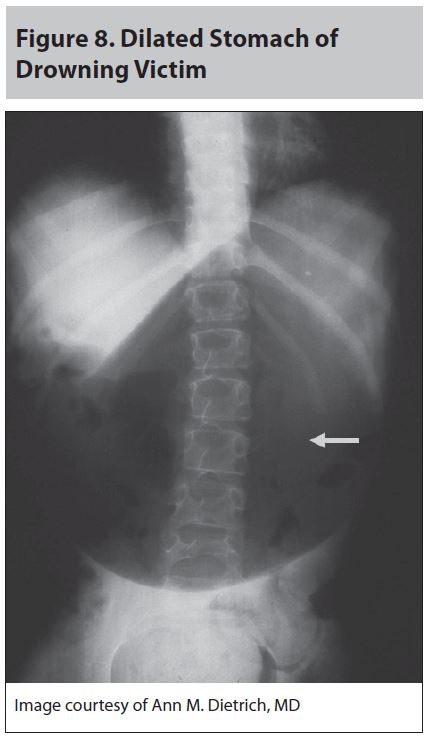
Adequate ventilation and oxygen support are essential. Initially supplemental oxygen should be given by non-rebreather facemask with 100% oxygen. The FiO2 can be titrated down once the patient is stabilized. Aspiration of water and solutes may result in alveolar collapse, a significant A-a gradient, and difficulty with oxygenation. In addition, a decrease in lung compliance and an increase in airway resistance may lead to difficulty with ventilation. Trials of non-invasive positive pressure ventilation (NIPPV) may overcome these challenges and should be considered.19 In patients with persistent poor ventilation, poor oxygenation, or depressed mental status, intubation and positive end-expiratory pressure (PEEP) may be necessary.19 (See Figure 7.) As stated earlier, drowning victims can develop ARDS requiring ventilatory support and ICU admission. Bronchoscopy to clear aspirated debris (sand, organic material, vomit) may be necessary. An orogastric or nasogastric tube should be placed to decompress the stomach and to remove any water and debris that may have been ingested. (See Figure 8.) Chest X-ray or chest CT should be obtained to assess for consolidations, atelectasis, and inhaled foreign bodies.
Severely symptomatic drowning victims will often present in critical condition with evidence of hypoxemia, hypothermia, dysrhythmias, and altered mental status. Full vital signs, including a core temperature, should be measured. In addition to blood chemistries, a complete blood count and coagulation studies are recommended. Hypothermic drowning victims can experience a “cold diuresis,” resulting in hypovolemia, hypotension, and renal dysfunction.29 Supportive care including appropriate volume resuscitation with normal saline and rewarming of patients is appropriate.
Some drowning victims will present in cardiopulmonary arrest. ACLS and ATLS algorithms should be followed with a focus on oxygenation, ventilation, volume support, and correction of acidosis. Some patients with prolonged submersion in cold water may appear “cold and dead.” In these severely hypothermic patients, resuscitation and warming should be continued until the core temperature reaches 32°C-35°C.51 If the patient is still in cardiopulmonary arrest following rewarming, resuscitation can be terminated.
Hypothermic drowning victims who have ROSC after cardiopulmonary arrest should not be rewarmed completely. Instead, therapeutic hypothermia or targeted temperature management should be maintained for 12-24 hours.52 While hospital guidelines may vary, recent literature suggests that there is no significant outcome difference between a targeted core temperature of 33°C or 36°C for post-arrest victims.53
Advanced Care Management
Many submersion and drowning victims will present to community hospitals that lack specialized intensive care units and the ability to manage post-arrest or critically ill patients. Following initial evaluation, stabilization, and treatment, patients who are critically ill should be transferred expeditiously to a facility that offers intensive care appropriate to the age and condition of the patient. Restoration of normal physiology offers the best prognosis. Aggressive intervention may be warranted.30
Therapeutic hypothermia or targeted temperature management should be considered in drowning victims for the first 12-24 hours following an arrest. Previous guidelines recommended a targeted core temperature between 32°C-34°C, however a recent study on targeted temperature management for victims of cardiac arrest suggests a temperature of 36°C may be equivalent.60,61,51 This initial window of temperature control below normal core temperature is thought to decrease the metabolic demands of the body and may help reduce the production of radical oxygen species, which are responsible for significant cellular damage. Targeted temperature management has been studied in patients with normothermic cardiac arrests and the benefit in hypothermic drowning victims is speculative.
If the victim has suffered a significant aspiration event that has progressed to ARDS, that patient may benefit from a lung-protective ventilatory strategy such as the ARDSNet Protocol, which uses lower tidal volumes, PEEP, and low plateau pressures to prevent barotrauma while increasing oxygenation.62 A small percentage of patients may continue to decline clinically despite pressor support, fluid resuscitation, and mechanical ventilation. These patients may benefit from extracorporeal membrane oxygenation (ECMO).62,63 Good evidence supporting the use of ECMO is lacking. Over the past three decades, there have been several case reports of successful resuscitations in which ECMO was used. Access to ECMO is often limited, and may require transfer to a quaternary health care center.40,65,66
Special Consideration: Cold-Water Drowning
Although cold-water drowning is often considered to be neuro-protective (i.e., offering a higher likelihood of good neurological outcome), the data are mixed. There have been several case reports suggesting better outcomes if hypothermia is present.54,66 Other studies have shown no benefit of accidental hypothermia with regard to morbidity and mortality after drowning when compared to case controls.7,57 The mixed results likely reflect the fact that accidental hypothermia is an uncontrolled, unmonitored event that is different than induced therapeutic hypothermia. The apparent protective effects of environmental hypothermia in drowning, based on case reports, may occur when hypothermia happens quickly, preceding the asphyxia of drowning.57
Conclusion
Drowning pathophysiology and management are important topics for the emergency practitioner. Drowning is a process in which there is respiratory impairment after submersion or immersion in liquid. Old terms, such as wet and dry drowning, as well as active and passive drowning, should be abandoned to simplify the definitions and to gather more accurate data regarding epidemiology and treatment. Drowning causes significant morbidity and mortality worldwide, especially among high-risk groups such as children and people with underlying medical conditions. While the drowning process affects many physiologic systems, the final common pathway is respiratory failure and resultant hypoxia either from aspirated fluid or from laryngospasm. The morbidity and mortality associated with drowning are due to direct pulmonary injury and to brain ischemia.
In the prehospital management of the drowning victim, there should be an emphasis on scene safety followed by immediate resuscitation. Initial BLS should focus on opening the airway and on high quality ventilation. In the emergency department, asymptomatic patients can usually be discharged. Symptomatic patients often need chest X-rays, blood work, telemetry, warming, and supplemental oxygen. They may need admission for supportive care. In the severely symptomatic patient, consider a trial of non-invasive positive pressure ventilation, intubation with PEEP, bronchoscopy, and gastric decompression. For drowning victims who have suffered cardiopulmonary arrest, consider targeted temperature management and transfer to a center that can perform extracorporeal membrane oxygenation.
References
- Papa L, Hoelle R, Idris A. Systematic review of definitions for drowning incidents. Resuscitation 2005;65(3):255-64.
- Idris AH, et al. Recommended guidelines for uniform reporting of data from drowning: the “Utstein style.” Circulation 2003;108(20):2565-2574.
- Nussbaum E. Prognostic variables in nearly drowned, comatose children. Am J Dis Child 1985;139(10):1058-1059.
- Quan L, et al. Outcome and predictors of outcome in pediatric submersion victims receiving prehospital care in King County, Washington. Pediatrics 1990;86(4):586-593.
- Suominen P, et al. Impact of age, submersion time and water temperature on outcome in near-drowning. Resuscitation 2002;52(3):247-254.
- DeNicola LK, et al. Submersion injuries in children and adults. Crit Care Clin 1997;13(3):477-502.
- Peden MM, McGee K. The epidemiology of drowning worldwide. Inj Control Saf Promot 2003;10:195–199. ?
- G S. Global burden of drowning, in Paper Presented at World Congress on Drowning; 2002.
- Weiss J. V. American Academy of Pediatrics Committee on Injury, and P. Poison, Prevention of drowning. Pediatrics 2010;126(1):e253-e262.
- Control CfD. WISQARS - Web-based Injury Statistics Query and Reporting System. [cited 2014 April 26, 2014]; Leading Causes of death in ages 1-18 in the United States].
- Burford AE, et al. Drowning and near-drowning in children and adolescents: A succinct review for emergency physicians and nurses. Pediatr Emerg Care 2005;21(9):610-616; quiz 617-619.
- Pearn JH, et al. Drowning and near-drowning involving children: A five-year total population study from the City and County of Honolulu. Am J Public Health 1979;69(5):450-454.
- Wintemute GJ. Childhood drowning and near-drowning in the United States. Am J Dis Child 1990;144(6):663-669.
- Brenner RA, et al. Where children drown, United States, 1995. Pediatrics 2001;108(1):85-89.
- Hwang V, et al. Prevalence of traumatic injuries in drowning and near drowning in children and adolescents. Arch Pediatr Adolesc Med 2003;157(1):50-53.
- Howland J, et al. Why are most drowning victims men? Sex differences in aquatic skills and behaviors. Am J Public Health 1996;86(1):93-96.
- Idris A, Bierens J, Bossaert L, et al, ed. Recommended Guidelines for Uniform Reporting of Data from Drowning: The Ustein Style, Handbook on Drowning. BJ Heidelberg, ed. Springer-Verlag; 2006: 377-385.
- Szpilman D, et al. Drowning. N Engl J Med 2012;366(22):2102-2110.
- Layon AJ, Modell JH. Drowning: Update 2009. Anesthesiology 2009;110(6):1390-1401.
- Modell JH, et al. Physiologic effects of near drowning with chlorinated fresh water, distilled water and isotonic saline. Anesthesiology 1966;27(1):33-41.
- Dumitru AP, Hamilton FJ. Underwater blackout - a mechanism of drowning. GP 1964;29:123-125.
- Modell JH, Graves SA, Ketover A. Clinical course of 91 consecutive near-drowning victims. Chest 1976;70(2):231-238.
- Pendergast DR, Lundgren CE. The underwater environment: Cardiopulmonary, thermal, and energetic demands. J Appl Physiol (1985) 2009;106(1):276-283.
- Orlowski JP, Szpilman D. Drowning. Rescue, resuscitation, and reanimation. Pediatr Clin North Am 2001;48(3):627-646.
- Epstein M. Renal effects of head-out water immersion in humans: A 15-year update. Physiol Rev 1992;72(3):563-621.
- Arborelius M, Jr., et al. Hemodynamic changes in man during immersion with the head above water. Aerosp Med 1972;43(6):592-598.
- Epstein M. Water immersion and the kidney: Implications for volume regulation. Undersea Biomed Res 1984;11(2):113-121.
- Valenti G, et al. Water immersion is associated with an increase in aquaporin-2 excretion in healthy volunteers. Biochim Biophys Acta 2006;1758(8):1111-1116.
- Gabrielsen A, et al. Cardiovascular and neuroendocrine responses to water immersion in compensated heart failure. Am J Physiol Heart Circ Physiol 2000;279(4):H1931-1940.
- Warner D, Knape J. Handbook on Drowning: Prevention, Rescue, and Treatment. Bierens J, ed. Springer-Verlag; Berlin; 2006.
- Cross AR, ed. American Red Cross Lifeguarding Manual. 2012, United States of America.
- Association, N.F.P., NFPA 1670: Standard on Operations and Training for Technical Search and Rescue Incidents. 2004, National Fire Protection Association.
- Venema AM, Groothoff JW, Bierens JJ. The role of bystanders during rescue and resuscitation of drowning victims. Resuscitation 2010;81(4):434-439.
- Watson RS, et al. Cervical spine injuries among submersion victims. J Trauma 2001;51(4):658-662.
- Vanden Hoek TL, et al. Part 12: Cardiac arrest in special situations: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010;122(18 Suppl 3):S829-S861.
-
Medical Directors Council, National Association of State EMS Officials. National Model of EMS Clinical Guidelines. NASEMSO 2015;11-14:
229-231. - Manolios N, Mackie I. Drowning and near-drowning on Australian beaches patrolled by life-savers: A 10-year study, 1973-1983. Med J Aust 1988;148(4):165-167, 170-171.
- Siebke H, et al. Survival after 40 minutes: Submersion without cerebral sequelae. Lancet 1975;1(7919):1275-1277.
- Southwick FS, Dalglish PH, Jr. Recovery after prolonged asystolic cardiac arrest in profound hypothermia. A case report and literature review. JAMA 1980;243(12):1250-1253.
- Bolte RG, et al. The use of extracorporeal rewarming in a child submerged for 66 minutes. JAMA 1988;260(3):377-379.
- Szpilman D. Near-drowning and drowning classification: A proposal to stratify mortality based on the analysis of 1,831 cases. Chest 1997;112(3):660-665.
- Auerbach PS. Wilderness Medicine. 2012: Elsevier Mosby.
- Causey AL, Tilelli JA, Swanson ME. Predicting discharge in uncomplicated near-drowning. Am J Emerg Med 2000;18(1):9-11.
- Noonan L, Howrey R, Ginsburg CM. Freshwater submersion injuries in children: A retrospective review of seventy-five hospitalized patients. Pediatrics 1996;98(3 Pt 1):368-371.
- Pratt FD, Haynes BE. Incidence of “secondary drowning” after saltwater submersion. Ann Emerg Med 1986;15(9):1084-1087.
- van Berkel M, et al. Pulmonary oedema, pneumonia and mortality in submersion victims: A retrospective study in 125 patients. Intensive Care Med 1996;22(2):101-107.
- Ender PT, Dolan MJ. Pneumonia associated with near-drowning. Clin Infect Dis 1997;25(4):896-907.
- Modell JH, Moya F. Effects of volume of aspirated fluid during chlorinated fresh water drowning. Anesthesiology 1966;27(5):662-672.
- Modell JH, et al. The effects of fluid volume in seawater drowning. Ann Intern Med 1967;67(1):68-80.
- Modell JH, Davis JH. Electrolyte changes in human drowning victims. Anesthesiology 1969;30(4):414-420.
- Jolly BT, Ghezzi KT. Accidental hypothermia. Emerg Med Clin North Am 1992;10(2):311-327.
- Bierens JJ, Knape JT, Gelissen HP. Drowning. Curr Opin Crit Care 2002;8:578-586.
- Nielsen N, et al. Targeted temperature management at 33°C versus 36°C after cardiac arrest. N Engl J Med 2013;369(23):2197-2206.
- Biggart MJ, Bohn DJ. Effect of hypothermia and cardiac arrest on outcome of near-drowning accidents in children. J Pediatr 1990;117(2 Pt 1):179-183.
- Dean JM, Kaufman ND. Prognostic indicators in pediatric near-drowning: The Glasgow coma scale. Crit Care Med 1981;9(7):536-539.
- Habib DM, et al. Prediction of childhood drowning and near-drowning morbidity and mortality. Pediatr Emerg Care 1996;12(4):255-258.
- Orlowski JP. Drowning, near-drowning, and ice-water drowning. JAMA 1988;260(3):390-391.
- Quan L, Mack CD, Schiff MA. Association of water temperature and submersion duration and drowning outcome. Resuscitation 2014;85(6):790-794.
- Lavelle JM, Shaw KN. Near drowning: Is emergency department cardiopulmonary resuscitation or intensive care unit cerebral resuscitation indicated? Crit Care Med 1993;21(3):368-373.
- Williamson JP, et al. Near-drowning treated with therapeutic hypothermia.Med J Aust 2004;181(9):500-501.
- Topjian AA, et al. Brain resuscitation in the drowning victim. Neurocrit Care 2012;17(3):441-467.
- Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. The Acute Respiratory Distress Syndrome Network. N Engl J Med 2000;342(18):1301-1308.
- Farstad M, et al. Rewarming from accidental hypothermia by extracorporeal circulation. A retrospective study. Eur J Cardiothorac Surg 2001;20(1):58-64.
- Ruttmann E, et al. Prolonged extracorporeal membrane oxygenation-assisted support provides improved survival in hypothermic patients with cardiocirculatory arrest. J Thorac Cardiovasc Surg 2007;134(3):594-600.
- Guenther U, et al. Extended therapeutic hypothermia for several days during extracorporeal membrane-oxygenation after drowning and cardiac arrest Two cases of survival with no neurological sequelae. Resuscitation 2009;80(3):379-381.
- Eich C, Brauer A, Kettler D. Recovery of a hypothermic drowned child after resuscitation with cardiopulmonary bypass followed by prolonged extracorporeal membrane oxygenation. Resuscitation 2005;67(1):145-148.
- Bierens JJ, et al. Submersion in The Netherlands: Prognostic indicators and results of resuscitation. Ann Emerg Med 1990;19(12):1390-1395.
MONOGRAPH: Survival depends on a coordinated effort to minimize the interval between airway compromise and ventilatory efforts.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.