Pediatric Respiratory Failure
Authors
Erin Tromble, MD, Resident, Departments of Pediatrics and Emergency Medicine, University of Arizona, Tucson, AZ
Aaron Leetch, MD, Assistant Professor, Departments of Emergency Medicine and Pediatrics; Associate Program Director, Emergency Medicine/Pediatrics Residency, University of Arizona, Tucson, AZ
Dr. Tromble and Dr. Leetch report no financial relationships relevant to this field of study.
Objectives
Etiology- Know etiology of respiratory failure
- Differentiate etiologies of respiratory failure by age
Pathophysiology
- Understand the anatomy of the respiratory system
- Understand the progression of respiratory failure to arrest
Recognition
- Recognize signs and symptoms of upper airway obstruction
- Recognize the presentations of patients with hypoxia
- Recognize and interpret relevant monitoring studies for respiratory failure
- Recognize signs and symptoms of hypercarbia
- Recognize signs and symptoms of lower airway obstruction
- Recognize and interpret relevant laboratory studies for respiratory failure
- Recognize and interpret relevant radiographic studies for respiratory failure
Management
- Plan management priorities for patients in respiratory failure
- Know the use of pharmacologic agents in the management of patients in respiratory failure
- Know the indications and contraindications for surgical airway management
- Know the use of basic airway management techniques in patients with respiratory failure
- Know the use of advanced airway management techniques in patients with respiratory failure
- Know the use of surgical airway management procedures
Etiology
Respiratory failure is the most common cause of cardiac arrest in children. Failure occurs when the respiratory system is unable to exchange gases in order to meet the body’s metabolic need. This may involve a failure of oxygen exchange (PaO2 <60mmHg), a failure of carbon dioxide exchange (acutely, PaCO2 > 50 mmHg; chronically, 20 mmHg above baseline), or both. The underlying etiology may occur within one or multiple organ systems that participate in the process of respiration. These include the nervous, cardiovascular, musculoskeletal, and respiratory systems.
Table 1: Common Causes of Pediatric Respiratory Failure
| Lung and Airway |
| Extrathoracic/Upper Airway |
| Airway malformations |
| Vascular malformations |
| Foreign body |
| Infections (e.g., epiglottitis, croup) |
| Intrathoracic/Lung |
| Pneumonia |
| Bronchiolitis |
| Cystic fibrosis |
| Pulmonary edema |
| Acute respiratory distress syndrome |
| Respiratory Pump |
| Chest wall abnormalities (e.g., flail chest) |
| Restrictive disease (e.g., scoliosis) |
| Muscle weakness (e.g., muscular dystrophy) |
| Respiratory Center |
| Brain injuries |
| Central nervous system infections |
| Congenital malformation |
| Ingestion/medication side effects |
| Excess oxygen demand/Metabolic derangement |
| Sepsis |
| Diabetic ketoacidosis |
This failure can be due to a variety of reasons, including airway obstruction, CNS issues, parenchymal disease, and respiratory pump failure. Younger children have smaller airway diameters that are more easily obstructed. This, combined with an underdeveloped respiratory pump, can quickly cause a lower respiratory tract infection to progress to respiratory failure. Neonates and preterm infants are especially prone to manifest illness with apnea due to an underdeveloped central nervous system. As children grow older, airway size and chest wall compliance are improved, and the progression to respiratory failure is more common in those with parenchymal disease or chronic airway disease (e.g., asthma).
Table 2: Pediatric Respiratory Considerations
| Obligate nasal breathers:significant respiratory distress from nasal obstruction |
| Large tongue:more difficult visualization of larynx |
| Superior and anterior larynx:more difficult visualization of larynx |
| Large and floppy epiglottis:more difficult visualization of larynx |
| Large occiput:more difficult visualization of larynx; supine positioning on hard surface may cause flexion and obstruction upper trachea |
| Narrowest point of airway is subglottic at cricoid ring: risk of stenosis below glottis |
| Less rigid upper airway:more prone to obstruction such as in the supine position on a hard surface |
| Smaller and fewer alveolar:less surface area for gas exchange |
| Infants have fewer alveoli:more prone to atelectasis |
| Immature CNS:irregular respiration and risk of apnea |
| Immature musculature:increased risk of respiratory muscle fatigue |
| Higher basal metabolism: less respiratory reserve; prone to desaturation quickly |
CME Question
A 4-month-old female is brought to the emergency department in respiratory distress. She is febrile with a temperature of 38.3 C and is found to have nasal flaring, tachypnea, intercostal retractions, and diffuse bilateral rales with end-expiratory wheezing. Her oxygen saturation is 88% on room air. She is ultimately admitted for supportive care and tests positive for human metapneumovirus. What features make this patient more likely to develop respiratory distress than an older child?
- Obligate nasal breathing
- Anterior and cephaled larynx
- Smaller airways
- Large, floppy epiglottis
- Both A & C
- Both A & D
Start or Resume CME Test
(Opens in a new Tab/Window)
Pathophysiology
Respiratory failure is broadly classified into two categories. Type 1 respiratory failure occurs in the setting of hypoxemia with normal or low CO2. It results from a ventilation/perfusion (V/Q) mismatch, leading to non-cardiac mixing of venous and arterial blood. Type 2 respiratory failure occurs when alveolar ventilation is insufficient for physiologic needs, resulting in hypercarbia and hypoxemia that is relatively proportional. Respiratory pump failure is a classic example of Type 2 respiratory failure. An increase in respiratory demand that is greater than the patient’s ability to meet this demand results in hypercapnia and hypoxemia, which may subsequently lead to acidosis, poor myocardial perfusion, bradycardia and subsequent cardiac arrest.
Recognition
The signs and symptoms of respiratory distress and impending respiratory failure can be subtle in the pediatric patient and are dependent on the underlying etiology. The Pediatric Assessment Triangle(PAT) is a bedside tool that assists with rapid identification of children with respiratory distress and failure. Careful attention should be paid to the work of breathing and respiratory rate. Nasal flaring, retractions, abdominal breathing, and grunting are signs of significant increased work of breathing. Tachypnea is often an early sign whereas bradypnea is an ominous late finding. Hypercarbia often results in an increased respiratory rate and tidal volume to increase minute ventilation (Minute Ventilation = Respiratory Rate x Tidal volume).The normal response to hypoxia is also an increase in respiratory rate and tidal volume to allow for more alveolar gas exchange. A distinguishing clinical feature is the progression of hypoxia to agitation (“air hunger”) and hypercarbia to somnolence (“CO2 narcosis”).
Table 3: Rapid Assessment of Pediatric Patients (“Pediatric Assessment Triangle”)
| Appearance |
Level of alertness Interaction Response to stimuli |
| Work of Breathing |
Respiratory rate Respiratory effort (retractions, nasal flaring, grunting, abdominal breathing) |
| Color |
Cyanosis Pallor Mottling |
Most cases of pediatric respiratory distress can be differentiated into upper and lower airway dysfunction. Upper airway obstruction tends to cause audible stridor that is usually inspiratory or biphasic. Lower airway obstruction tends to cause wheezing that is audible only with auscultation and during the expiratory phase. Obstruction can progress to biphasic stridor or wheezing. Fixed obstructions can similarly cause biphasic airway sounds. When obstruction is severe, respiratory sounds will be diminished or absent.
Table 4: Signs and Symptoms in Respiratory Failure
|
Respiratory pattern/Work of Breathing Tachypnea Bradypnea Paradoxical breathing Tripod positioning Grunting Head-bobbing Nasal flaring Drooling Retractions (subcostal, suprasternal, intercostal, sternal)
Cardiovascular Tachycardia Bradycardia Hypertension |
Auscultation Stridor – upper airway obstruction (croup, foreign body) Wheezing – lower airway obstruction (asthma, foreign body) Crackles (PNA, bronchiolitis) Decreased breath sounds (effusion, severe asthma, pneumothorax)
CNS changes Irritability Lethargy Papilledema
General exam Flushing Pallor Cyanosis |
PNA = pneumonia, CNS = central nervous system
Figure 1: An Infant with Intercostal Retractions
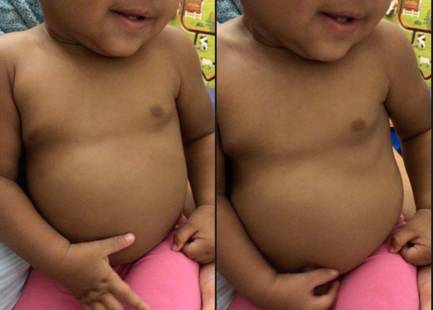
Diagnostic Studies and Monitoring:
- Pulse oximetry should be monitored continuously, but its interpretation must be considered carefully if supplemental oxygen has been applied.
- End tidal CO2 monitoring is useful when available, particularly when supplemental oxygen is administered.
- An arterial blood gas can help differentiate between ventilatory and oxygenation failure. A venous gas can be obtained if arterial access cannot be quickly established. Be wary of a normal PaCO2 in the setting of a severely distressed patient, as this likely indicates fatigue, an inability to compensate, and impending respiratory failure.
- Chest X-ray may reveal signs of focal parenchymal consolidation (pneumonia), bilateral hyperinflation (asthma), asymmetric hyperinflation (foreign body), enlarged heart/pulmonary congestion (congestive heart failure), pneumothorax,or perihilar/peribronchial thickening (viral process).
Figure 2: An Infant with a Left Pneumothorax
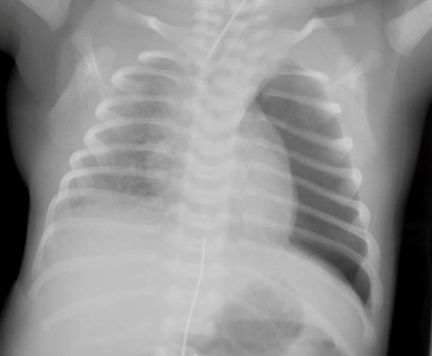
CME Question
A 6-month-old male with no prior medical history presents to the emergency department with a chief complaint of “difficulty breathing.” Vital signs include a temperature of 39.2 C, pulse 180, oxygen saturation of 80% in room air, and respiratory rate of 60. Initial exam reveals an irritable infant who is poorly consolable, with intercostal retractions, nasal flaring, and diffuse rales throughout the bilateral lung fields. Initial management includes establishing IV access and placing the patient on a non-rebreather at 15L, after which his oxygen saturation is 85% and respiratory rate is 53. Of the following, what information would confirm respiratory failure?
- End tidal CO2 monitoring with CO2 reading of 62
- Arterial blood gas with pO2 of 58
- Venous blood gas with pO2 of 59
- Chest X-ray with extensive bilateral perihilar thickening
- Further studies are not needed at this time. Intubation should be performed without delay
Start or Resume CME Test
(Opens in a new Tab/Window)
Management
Early recognition of impending respiratory failure and identification of the underlying cause are critical to the management of respiratory distress and failure. In an undifferentiated patient with respiratory distress, management begins with assessment and intervention, according to the American Heart Association Guidelines for Pediatric Advanced Life Support (PALS). Airway assessment and positioning to relieve obstruction is followed by assessment of work of breathing. Supplemental oxygen therapy is the first step in management of hypoxemia. Non-invasive modalities may range from simple nasal cannula to the use of positive pressure ventilation.
Obstructive processes of both the upper and lower airways may benefit from nebulized medications including albuterol, racemic epinephrine, and hypertonic saline. Heliox, a mixture of helium and oxygen, may also be beneficial for severe upper airway obstructions but is not first-line therapy. Systemic steroids should be used early in cases of dynamic upper and lower airway obstruction. When airway obstruction is caused by nasopharyneal soft tissue or the tongue, placement of a nasopharyngeal or oropharyngeal airway device may be helpful. If the respiratory distress is due to medication ingestion, any available antidote should be administered promptly (e.g., naloxone for opiate intoxication).
Table 5: Upper vs Lower Airway Disease & Early Management
|
Presentation |
Management |
|
|
Upper Airway (croup, epiglottitis, retropharyngeal cellulitis/abscess, foreign body) |
|
|
|
Lower airway |
|
|
CPAP = Continuous positive airway pressure, NPPV = noninvasive positive-pressure ventilation
Endotracheal intubation with mechanical ventilation is indicated for severe respiratory distress/failure refractory to other therapies and interventions. Respiratory failure is often evidenced by:
- Failure to adequately oxygenate or ventilate (according to monitoring or lab values)
- Failure to protect the airway (i.e., vomiting resulting in or at risk for aspiration)
- Altered mental status (i.e., hypercarbia)
- Agitation (i.e., hypoxia)
- Insufficient respiratory effort
Preparation for intubation should begin with pre-oxygentation with 100% oxygen until emergency providers are ready to place an advanced airway. Oxygen may be delivered by non-rebreather mask, bag-valve-mask ventilation, or other advanced positive pressure ventilatory techniques. Failure to successfully intubate or ventilate a patient in respiratory failure is an indication for surgical cricothyroidotomy (age ≥ 12 years) or needle cricothyroidotomy with jet ventilation (age < 12 years). Additional adjunct therapies include inhaled nitric oxide, surfactant, and initiation of ECMO.
National Guideline/Academic Resource
Pediatric Advanced Life Support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. http://pediatrics.aappublications.org/content/126/5/e1361.full
Resources
Pfleger A, Eber E. Management of acute severe upper airway obstruction in children. Paeaitr Respir Rev 2013;14:70-77.
Hammer J. Acute respiratory failure in children. Paediatr Respir Rev 2013;14:64-69.
Chameides L, Samson R, Schexnayder S, Hazinski F. Pediatric AdvancedLife Support: Provider Manual. Dallas, TX: American Heart Association; 2011.
