Damage Control Resuscitation
Authors
Jason R. Pickett, MD, FACEP, Assistant Professor, Department of Emergency Medicine, Wright State University, Dayton, OH.
Tyler Kallsen, MD, Wright State Emergency Medicine Residency, Dayton, OH.
Eric Schott, MD, Wright State Emergency Medicine Residency, Dayton, OH.
Peer Reviewer
Jay Menaker, MD, FACEP, Associate Professor, Department of Surgery; Associate Professor, Department of Emergency Medicine, University of Maryland School of Medicine, R Adams Cowley Shock Trauma Center, Baltimore, MD.
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Executive Editor Ms. Mark’s spouse works for a company that creates advertising for Uroplasty. Dr. Dietrich (editor in chief), Dr. Pickett (author), Dr. Kallsen (author), Dr. Schott (author), Dr. Menaker (peer reviewer), Ms. Behrens (nurse reviewer), and Mr. Landenberger (continuing education and editorial director) report no relationships with companies related to this field of study.
|
ACS Hemorrhage Class |
||||
|
Predictor |
Class I |
Class II |
Class III |
Class IV |
|
ACS — American College of Surgeons, bpm — beats per minute; percentiles based on 70 kg patient. Note that young patients may display fewer physiologic changes at higher stages of blood loss, whereas older patients or those which chronic disease/medications may demonstrate physiologic changes at lower stages of blood loss. |
||||
|
% Loss |
< 15% |
15-30% |
30-40% |
> 40% |
|
mL Loss |
< 750 mL |
750 mL-1.5 L |
1.5 L-2 L |
> 2 L |
|
Mental status |
Appropriate |
Anxious |
Confused |
Lethargic |
|
Blood pressure |
Normal |
Normal |
Decreased |
Decreased |
|
Pulse rate (bpm) |
< 100 |
100-120 |
120-140 |
> 140 |
|
Respiratory rate |
14-20 |
20-30 |
30-40 |
> 35 |
|
Capillary refill |
< 2 sec |
> 2 sec |
> 2 sec |
> 2 sec |
|
Urine output (mL/hr) |
> 30 |
20-30 |
5-15 |
< 5 |
|
Resuscitative fluids |
Saline |
Saline |
Saline, blood |
Saline, blood |
|
Severity of physiological decompensation |
Stable |
Mild |
Moderate |
Severe |
Key principles of damage control resuscitation include the rapid control/containment of exsanguinating hemorrhage (internal vs. external), hypotensive resuscitation (if indicated), avoidance of the overuse of crystalloids and colloids, and the prevention and correction of the “lethal triad” of acidosis, hypothermia, and coagulopathy. Resuscitation is primarily focused on early use of a balanced amount of red blood cells, plasma, and platelets.10
As described previously, this lethal triad of acidosis, hypothermia, and coagulopathy works synergistically to worsen outcomes of patients in shock. Coagulopathy in massive hemorrhage is due to multiple underlying etiologies and is present in as many as 25% of severely injured trauma patients on arrival. The coagulopathy primarily stems from depletion of clotting factors due to hemorrhage, dilution by excessive crystalloid resuscitation (normal saline, lactated Ringer’s solution, among others), platelet function inhibition from hypothermia, as well as significant acidemia resulting from poor tissue perfusion, which further inhibits pro-coagulant enzyme function.11 Recent studies have shown that objective measures of coagulopathy, including INR greater than 1.2, BD greater than 3 mmol/L, body temperature less than 35°C, serum lactate greater than 6 mmol/L, and hemoglobin less than 7 g/dL, on hospital presentation are independent risk factors of early mortality.12 Coagulopathy is worsened by both acidosis and hypothermia.13 As a patient loses blood and their subsequent ability to properly oxygenate the tissues, lactic acid begins to build up from anaerobic metabolism, which results in a progressively worsening acidosis. Hypothermia then follows with the loss of warm blood, and is further exacerbated by the administration of ambient to cool temperature resuscitative fluids. Ultimately, both of these factors worsen the bleeding by inhibiting the function of the clotting factors, with the cycle continuing until it is addressed. Given the significant deterioration and mortality associated with these processes, early detection/prediction using the factors in Table 2 to mobilize resuscitative blood products has been shown to significantly improve patients’ 30-day mortality.14
- Systolic BP < 110 mmHg
- HR > 105 bpm
- Hct < 32%
- pH < 7.25
- INR > 1.4
- SaO2 < 75%
Prediction criteria shown to increase likelihood that activation of an MTP (massive transfusion protocol — greater than 10 units of blood) will be required. Note that the presence of three vs. four of the four initial criteria (systolic blood pressure, heart rate, hematocrit, pH) indicates a 70% vs. 85% likelihood of eventual need, respectively.
Prehospital Management
In the prehospital setting, the critical first step in caring for a patient with massive hemorrhage is to quickly identify and control sites of bleeding. This has been most apparent in the application of lessons learned from recent military conflicts. The traditional ABC (airway, breathing, circulation) mnemonic has been re-arranged to address circulation, or more specifically the control of exsanguinating hemorrhage, even before establishment of an airway.15 The benefit provided to a casualty by the simple (yet effective) application of a tourniquet is perhaps the most important intervention that can be performed in the appropriate setting and should be considered and applied without hesitation. The benefit of popular tourniquets, including the CAT (Combat Application Tourniquet, available from North American Rescue www.narescue.com), have been demonstrated time and time again in both military and civilian settings. All medical personnel, regardless of intended area of practice (prehospital, emergency department, etc.), should be familiar with the operation of the most common tourniquet designs and have them easily accessible. (See Figure 1.)
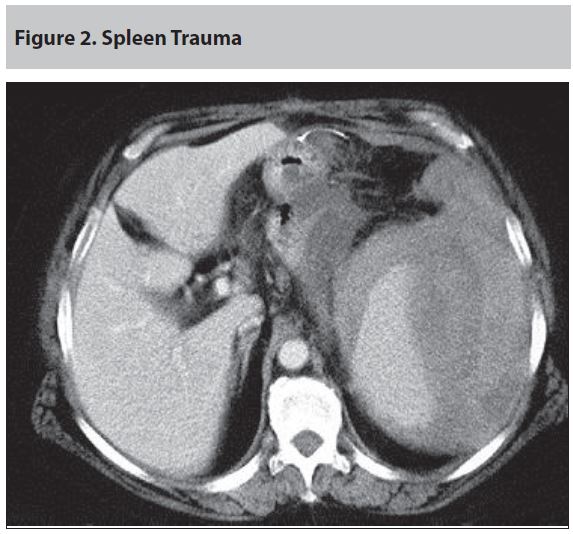
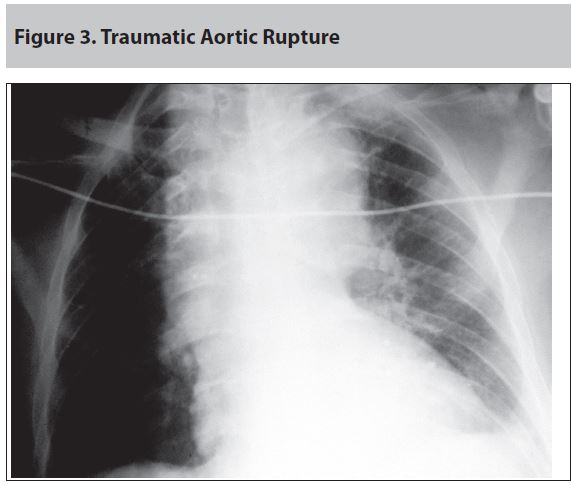
Hemorrhage can be internal, external, or a combination of both. Providers must have a high index of suspicion for potential internal blood loss in cases of penetrating trauma and blunt trauma to the abdomen, pelvis, and/or chest, evident from the primary survey. (See Figures 2 and 3.) In cases of internal bleeding, management priorities include limited fluid replacement (2 L of crystalloids) and rapid transport to a hospital for definitive care.16 External sources of bleeding should be readily identifiable on external exam, with priorities for extremity hemorrhage again to include hemorrhage control using compression devices as applicable, rapid transport to an appropriate facility, and judicious use of fluids to maintain systolic blood pressure at or above 90 mmHg. Consideration for permissive or controlled hypotension are discussed later. As was already described, hemorrhage control is achieved first and foremost by applying direct pressure to the wound with the addition of commercial adjuncts as necessary and available. Consistent with common sense, the earlier (prior to the onset of shock) the tourniquet is placed from the time of injury, the better the outcome.17-19 Improved outcome was demonstrated regardless of the level of medical training of the individual applying the tourniquet.
Hemostatic Dressings
Hemostatic dressings are an additional strategy to provide wound packing in a hemorrhaging patient. However, there has not been significant literature yet to provide a strong recommendation for a specific product. The 2009 Tactical Combat Casualty Care (TCCC) update recommends QuikClot Combat Gauze (QCG; Z-Medica, Wallingford, CT) as first-line treatment for life-threatening hemorrhage not amenable to traditional tourniquet application.20 This includes wounds in junctional areas (those involving the proximal most end of a long bone), torso, and elsewhere. The two primary mechanisms through which these clotting agents promote hemostasis are: absorption of water, which increases the concentration of clotting factors in the blood, and the production of chemical reactions that stimulate the intrinsic coagulation pathway.21 QuikClot gauze is impregnated with a kaolin, an inorganic material that demonstrates activation of the coagulation cascade.22 While there are many different agents and specific mechanisms available for purchase and use, the ideal agent should stop bleeding in 2 minutes or less, cause no toxicity to surrounding tissue, cause no pain or thermal injury, be ready to use with little training, be easily applied under all conditions, fit both simple and complex wounds, be easily removed, have a long shelf life, and be economical.23-24 The 2014 TCCC guidelines recommend Combat Gauze but also approve Chitogauze and Celox Gauze, chitosan-based hemostatic dressings that may even be slightly better in coagulopathic patients.25
While these agents are most commonly used in the combat or other prehospital scenario, they should be considered at any point in the treatment timeline when there is need for hemostasis and immediate surgical support is not available. As with tourniquets, hemostatic dressings should not be removed until in the operating theater or other setting within reach of definitive surgical intervention.
Transport Decision
Early notification to the emergency department of a possible need for massive transfusion has also shown a significant benefit.17 This allows hospital personnel time to coordinate the proper individuals and resources, being better prepared to act quickly upon the patient’s arrival. As mentioned earlier, use of prehospital data such as blood pressure, pulse, and level of consciousness can help estimate blood loss volume and predict the need for damage control resuscitation techniques.16 While assessing and transporting the patient, manage the airway as needed. Establish vascular access, but limit any infusion to the minimum amount necessary to correct obvious shock as evidenced by pallor, diaphoresis, weak peripheral pulses, altered mental status, and delayed cap refill. Time of transport to an appropriate definitive care facility is very important.
Consider bypassing hospitals in favor of quicker transport to a trauma center if indicated by local protocols. Studies have shown that care at a designated trauma center improves mortality and functional outcomes for survivors of major trauma.26 Judicious use of air medical resources also may be considered. In some cases, especially those with suspected internal hemorrhage or instances in which transport will be prolonged (i.e., rural setting, weather conditions), it may be appropriate to stop at a non-trauma center, especially if a surgeon is available to control bleeding and stabilize the patient before proceeding to a center for definitive care. Prehospital strategies for patient management is an active and on-going area of research that includes strategizing methods to bring lifesaving resources, such as plasma, to the point of patient contact in the field to reduce time to resuscitation and improve overall mortality.27-30
Emergency Department Management
When a patient arrives in the emergency department with massive hemorrhage, it is important to quickly perform a primary survey, establish two large bore IVs (18 gauge or larger), place the patient on telemetry, and assess volume status. As demonstrated in Table 3, the location of suspected injuries can give some insight to the potential extent of internal blood loss. It is important not to wait to control bleeding, and in some cases it will be prudent to make this the top priority before doing anything else. Initiate fluid resuscitation with crystalloids (if they have not already been initiated during prehospital transport) and immediately coordinate for the availability of blood products. An important part of resuscitation is permissive hypotension. The goal should be to keep the patient’s SBP above 90 mmHg but not much higher, as a high pressure can destabilize newly forming clots, worsening the bleeding.31-33
|
Type of Fracture |
Potential Internal Blood Loss (mL) |
|
Rib |
125 |
|
Radius or Ulna |
250-500 |
|
Humerus |
500-750 |
|
Tibia or Fibula |
500-1000 |
|
Femur |
1000-2000 |
|
Pelvis |
1000+ |
It is important to limit the total amount of crystalloid administered while at the same time minimizing the delay before blood products are given; this cannot be stressed enough.34-38 Overzealous fluid administration will aggravate bleeding by elevating blood pressure, dislodging blood clots, and diluting coagulation factors and platelets.39 A four-fold increase in morbidity was appreciated in patients who received a 24-hour crystalloid volume of between 5-10 L.40 While not yet supported by significant clinical evidence, initial studies looking at resuscitation of trauma patients with Plasma-Lyte vs. normal saline resulted in improved acid-base status and less hyperchloremia at 24 hours post injury.41 It should be noted, however, that normal saline is the only compatible fluid that can be given concomitantly with blood. In cases in which blood products may not be immediately available for use, colloids (such as hetastarch) should be considered, as they have demonstrated an improved survival when compared to traditional crystalloids in some studies.42
Many hospitals have a massive transfusion protocol that can be initiated for patients with suspected massive hemorrhage. This enables the coordinated and continued dispatch of blood products from blood bank stores and appropriate administration by providers. Massive transfusion is commonly defined as the administration (or need thereof) of more than 10 units of pRBCs within a 24-hour period.43 While there have been several scoring systems proposed to predict which patients will require MTP, their superiority to clinical judgment (and use of the basic predictors from Table 3) is unclear and warrants further review.44-47
The cornerstone of damage control resuscitation is 1 to 1 replacement of blood loss, better approximating the composition of fluids that the patient is losing, whole blood. There have been several ratios described in the literature, but perhaps the most widely used strategy is a 1:1:1 ratio of pRBCS, fresh frozen plasma, and platelets.2-3,48 Table 4 outlines the most common blood products utilized in damage control resuscitation. In trauma patients, consider administering tranexamic acid (TXA).49 This is an antifibrinolytic, which has been well studied in both the civilian and military settings with the CRASH-2 and MATTERs trials, respectively. TXA has been shown to reduce all-cause mortality, improve coagulopathy, and reduce blood transfusions if given within 3 hours of trauma. After 3 hours, it has been shown to increase thrombotic events.50-51 Another well-studied adjunctive treatment for coagulopathy is therapy with the recombinant factor VII (rFVII), a coagulation factor concentrate. This has been demonstrated to reduce overall transfused pRBCs but has not yet demonstrated a significant improved effect on mortality.52
|
Blood Product |
Volume |
Contents |
Grouping |
Storage |
|
HCT – Hematocrit, vWF – von Willebrand Factor |
||||
|
Whole blood |
450 mL |
Cross match |
21 days at 4°C |
|
|
Packed red blood cells |
250 mL, |
70% HCT |
Cross match |
21-42 days |
|
Fresh frozen plasma |
250 mL |
70% HCT, all factors |
Cross match |
1 year (frozen) 24 hours (thawed) |
|
Platelets |
30 mL/unit |
1010 platelets |
N/A |
5 days |
|
Cryoprecipitate |
10–25 mL/bag |
Fibrinogen, factors VIII/XIII/vWF |
ABO |
1 year (frozen) 6 hours (thawed) |
After the initial stabilization has been initiated, the physician can then complete a secondary survey. Ancillary studies including labs and imaging will vary depending on particular patient/situation specifics. Standard ordering should include complete blood count, coagulation studies, electrolytes, renal function, ionized calcium, and blood gasses. It is important to closely monitor potassium, as its concentrations can vary widely with dilution, acidosis, and fluid shifts affecting its concentration. Calcium is important to monitor as well, as the preservative citrate contained in pRBCs chelates the ionized calcium and leads to calcium depletion. Ionized calcium should be checked every few hours; keep levels greater than 0.9 mmol/L.53 Given the importance of maximizing the body’s ability to promote hemostasis during damage control resuscitation, the fibrinogen level should also be checked and managed as appropriate. Table 5 outlines the fibrinogen content of common blood products used in damage control resuscitation.
|
Blood Product |
Fibrinogen Content |
|
Fresh whole blood |
1000 mg |
|
Fresh frozen plasma |
400 mg |
|
Platelets |
80 mg |
|
Cryoprecipitate |
2500 mg |
Fibrinogen concentrate or cryoprecipitate should be strongly considered (and has shown some promise in small studies) when 6 U-12 U RBCs have been infused.54 For cryoprecipitate, the general rule is 1 unit of cryoprecipitate per 10 units of resuscitation at the 1:1:1 ratio. Remember throughout resuscitation to keep the patient warm. This can include use of blankets, active warming units, and warming the resuscitation fluids. There are a wide variety of fluid warmers, including dry heat, water bath, and countercurrent heat exchange technologies.
Response to the effect of transfusion should be monitored by laboratory analysis (Hgb, lactate, ABG) in addition to vital signs (HR, BP), as these will oftentimes improve after initial resuscitation despite a persistent hypoperfused state.55-56 Try to keep the patient’s hemoglobin between 7 gm/dL and 9 gm/dL.57 The goal is to adequately replace fluid loss while not over-transfusing and increasing the risk of transfusion-related injury.
While there is more than one potential reason for acidosis in the hemorrhaging patient, it is largely due to tissue hypoperfusion as described earlier. The best way to manage this acidosis is by promoting tissue perfusion by aggressive resuscitation with blood and blood products. The use of bicarbonate or tris-hydroxymethyl aminomethane (THAM) remains unclear. While use of these therapies can transiently improve acidosis and theoretically improve the negative effects of acidosis on coagulation factor efficacy, current literature has not shown evidence of improvement in mortality. If using these therapies, it is recommended to wait until pH is less than 7.2 before implementing.58-59
There are some special considerations for patients taking blood-thinning agents. Coagulation studies are important to assess if the patient is therapeutic on these agents. This has become more difficult with the growing use of newer agents that do not have ways of measuring effectiveness and do not have reversal therapies. If the patient is anti-coagulated with warfarin, reversal will require fresh frozen plasma and vitamin K. If available, prothrombin complex concentrate is also effective at reversing the effects of warfarin. Antiplatelet medications clopidogrel, aspirin, or Aggrenox do not have such an easy reversal agent. Simple administration of platelets provides a benefit; however, there is limited literature to recommend its use in patients who are otherwise healthy.57
Early surgical management is the core of trauma resuscitation and should never be delayed. The emergency medicine physician’s role in trauma resuscitation is to control hemorrhage to the extent possible, delay irreversible shock, optimize physiologic parameters, manage the airway, and provide appropriate oxygenation and ventilation.
The Risks
While damage control resuscitation has been shown to improve outcomes when applied in the appropriate situation, it should be used carefully, as this therapy can also cause significant harm to the patient.57 Adverse effects range from benign to fatal, including infectious blood-borne pathogens, sepsis, as well as non-infectious, including acute hemolysis, allergic reaction/anaphylaxis, transfusion-related acute lung injury (TRALI), and transfusion associated circulatory overload (TACO).
TRALI is the development of a non-cardiac pulmonary edema through the activation of the patient’s immune system resulting in acute hypoxemia within six hours of initial transfusion. It has been reported to occur in 0.08% to 8% of transfused patients in the recent literature.60 TRALI is difficult to detect in the early stages of neutrophil activation; however, it appears to be associated with resuscitation protocols containing large amounts of plasma. Signs include acute respiratory distress, hypoxemia (PaO2/FiO2 ? 300 or SPO2 < 90% on room air or other clinical evidence of hypoxemia), bilateral infiltrates, and absence of left atrial hypertension, all within 6 hours of transfusion. Management includes immediate discontinuation of the transfusion and initiation of supportive therapies including positive pressure ventilation (CPAP, BiPAP, or intubation) with maintenance of hemodynamic support, including fluids and vasopressors as needed.
TACO, on the other hand, is the result of a rapid transfusion of a blood volume that is more than the total capacity of the patient’s circulatory system, occurring in 1-8% of transfusions. Unlike TRALI, it is not related to an immune system activation, and is most common in patients with underlying diseases such as a history of congestive heart failure, renal failure, chronic anemia, cardiopulmonary compromise, and extremes of age.61 Prevention includes limiting the total amount of plasma administered and reducing the rate of infusion in those patients with significant risk factors for overloading with recommended rates of 42 mL/hr to 120 mL/hr, depending on risk factors.62 Potential harm not only results from the adverse events that may be associated with the administration of blood products; it should be noted that blood products are precious resources that should be carefully conserved and utilized only as needed.63
Controlled Hypotension
Given the significant risk of aggressive resuscitation, the idea of controlled hypotension (allowing the SBP to range between 70 and 90 during the initial resuscitative efforts) has been explored and is beginning to take hold in the setting of extensive hemorrhage, including those cases of penetrating trauma.33,57,64 Some studies have even used the patient’s mental status as the barometer to regulate the ultimate “safe” limit of this controlled hypotension.65 Despite a lack of established, randomized data touting its benefits, initial studies have demonstrated improved 24-hour mortality as well as no statistically significant differences with regard to 30-day mortality.35,66 Patients who were allowed to remain slightly hypotensive required significantly fewer blood product transfusions and yet experienced no significant differences in the incidence or severity of coagulopathy, thrombocytopenia, or anemia.
Patients presenting in hemorrhagic shock due to stab/penetrating wounds, especially those in the torso, secondary to gunshot wounds, cases of blunt injury, and especially those with obvious or even suspected brain injury or other intracranial process, should be resuscitated to goal blood pressures (SBP > 90 mmHg, MAP > 65 mmHg) due to concerns of under-perfusing tissue. Secondary brain injury is driven by a combination of systemic derangements (hypoxia, hypotension, hypercarbia, hypocarbia, hyperglycemia, and hypoglycemia) following the initial traumatic insult. Hypotension (SBP < 90 mmHg) has been identified as an independent risk factor for increased mortality/morbidity in cases of traumatic brain injury, including multi-system diseases such as neurogenic pulmonary edema.31,67-70
Progressing Technology
The goal of damage control resuscitation is to replace what the patient has lost given their specific mechanism of injury and pertinent comorbidities. The ideal situation would be to tailor replacement to a patient’s specific needs versus algorithm-based therapies. This would reduce waste of blood product resources, limit risks to the patient, and make replacement more effective by ensuring the patient is getting the product that he or she needs. In order to achieve this goal, we need point-of-care testing that is reliable, fast, and gives us information on the whole spectrum of the coagulation cascade. Two commercially available technologies include Thromboelastography (TEG) and Rotational Thromboelastometry (ROTEM). These tests have been widely adopted in Europe and the military, and are quickly becoming the standard of care in the United States. Both of these tests are available as point-of-care testing and are able to give a dynamic assessment of the coagulation cascade, including initiation, progression, final clot stability, and lysis of clot. The information gathered allows for guided coagulation specific transfusions. One study demonstrated that 30% of patients with resuscitation guided by ROTEM received only fibrinogen and prothrombin complex concentrate with no need for platelet transfusion.11 Another retrospective analysis showed improved observed mortality over predicted using mainly coagulation factor concentrates guided by ROTEM.71 Current research in this area is aimed at better realizing the clinical applications of the information derived from these coagulation tests.
New strategies for resuscitation are also being explored, including algorithms that place emphasis on the plasma first, as studies have shown that early replacement of plasma has prevented patients from needing massive transfusion.72 Some have suggested that there will be a benefit to bringing this component of the resuscitation forward into the field, although more research is needed to establish this as a practice.73
Freeze dried plasma was developed to address the complications of storage and management of plasma and make it available in more austere environments. The French army has been using this since 1994, and recent studies have shown it to be both effective and safe in resuscitation.74 Resuscitative endovascular balloon occlusion of the aorta (REBOA) is another technology being explored for hemorrhage control. REBOA aims at gaining proximal hemorrhage control similar to thoracotomy with aortic cross clamping; however, it utilizes arterial access at the femoral artery with sheath and catheter setup that is advanced to the desired level and balloon tip inflated. While not conceptually new, there is renewed interest in understanding which patients would benefit from this application and streamlining the process for vascular access and balloon deployment at the desired level.75
Summary
In summation, damage control resuscitation is the pathway for optimal care of patients who present with massive hemorrhage. The core principles are to stop the source of blood loss, replace fluids, and control the lethal triad of acidosis, hypothermia, and coagulopathy. It is important to keep in mind that while it is commonly implemented in the trauma setting, any patient with massive hemorrhage such as a GI bleed or ruptured AAA would benefit from implementing this strategy. Damage control resuscitation is a concept and plan of action critical across the trauma system, from the rural care setting to the level 1 trauma center. Damage control resuscitation may be necessary in a patient while awaiting surgical management or during transfer to a trauma center. This resuscitation relies on a system-ready approach that involves a protocol so that resources can be made available and staff ready to implement them. Damage control resuscitation continues to be an active area of research and its management principles continue to be refined to offer patients the optimal therapy.
References
- Gruen RL, Brohi K, Schreiber M, et al. Haemorrhage control in severely injured patients. Lancet 2012:1099-1108.
- Palm K, Apodaca A, Spencer D, et al. Evaluation of military trauma system practices related to damage-control resuscitation. J Trauma Acute Care Surg 2012;6(Suppl 5):S459-464.
- Schöchl H, Grassetto A, Schlimp CJ. Management of hemorrhage in trauma. Journal of Cardiothoracic and Vascular Anesthesia 2013;4(Suppl 1):S35-43.
- Khan S, Allard S, Weaver A, Barber C, Davenport R, Brohi K. A major haemorrhage protocol improves the delivery of blood component therapy and reduces waste in trauma massive transfusion. Injury 2012:587-592.
- Cohen MJ. Towards hemostatic resuscitation: The changing understanding of acute traumatic biology, massive bleeding, and damage-control resuscitation. Surg Clin North Am 2012;92(4):877-891.
- Stanworth S, Morris T, Gaarder C, Goslings J, Maegele M, Cohen M, et al. Reappraising the concept of massive transfusion in trauma. Crit Care 2010;14:R239.
- Curry N, Davis P. What’s new in resuscitation strategies for the patient with multiple trauma? Injury 2012;43(7):1021-1028.
- Alarcon LH PJPA. Chapter 12. Management of Shock. In: Mattox KL MEFD, ed. Trauma. 7th ed. New York, NY: McGraw-Hill; 2013.
- American College of Surgeons Committee on Trauma. Chapter 3: Shock. ATLS Student Course Manual. 9th ed. Chicago, IL: American College of Surgeons; 2012.
- Jenkins DH, Rappold JF, Badloe JF, Berseus O, Blackbourne L. Trauma hemostasis and oxygenation research position paper on remote damage control resuscitation: Definitions, current practice, and knowledge gaps. Shock 2014;41(Suppl 1):3-12.
- Davenport R. Pathogenesis of acute traumatic coagulopathy. Transfusion 2013;53(Suppl 1):23-27.
- Frischknecht A, Lustenberger T, Bukur M, Turina M, Billeter A, Mica L, et al. Damage control in severely injured trauma patients — A ten-year experience. J Emerg Trauma Shock 2011;4:450-454.
- Darlington DN, Kheirabadi BS, Delgado AV, Scherer MR, Martin WZ, Dubick MA. Coagulation changes to systemic acidosis and bicarbonate correction in swine. J Trauma 2011;71(5):1271-1277.
- Cotton BA, Reddy N, Hatch QM, LeFebvre E. Damage control resuscitation is associated with a reduction in resuscitation volumes and improvement in survival in 390 damage control laparotomy patients. Ann Surg 2011;254(4):298-605.
- Franco M, Otten E, Ditzer TF, Compton S, Hastings PR. Combat and Casualty Care. In: Auerbach PS, ed. Wilderness Medicine. 6th ed: Mosby; 2012.
- NAEMT A. Chapter 7: Shock. PHTLS Prehospital Trauma Life Support: Military Edition. 7th ed. St Louis, MO: Mosby Elsevier; 2014.
- Kragh JF, Littrel ML, Jones JA, et al. Battle casualty survival with emergency tourniquet use to stop limb bleeding. J Emerg Med 2011;41:590-597.
- Gerhardt R, Strandenes G, Cap A, et al. Remote damage control resuscitation and the Solstrand Conference: Defining the need, the language, and a way forward. Transfusion 2013;53(Suppl 1):9s-16s.
- Schreiber MA. The beginning of the end for damage control surgery. Br J Surgery 2012;99(Suppl 1):10-11.
- Butler F. Tactical combat casualty care: Update 2009. J Trauma 2010;69(Suppl 1):S10-13.
- Snyder D, TASK. Efficacy of prehospital application of tourniquets and hemostatic dressings to control traumatic external hemorrhage. DOT HS 811 999b. Washington, DC: National Highway Traffic Safety Administration; 2014.
- Politi L, Aprile A, Paganelli C. Randomized clinical trial on short-time compression with kaolin-filled pad: A new strategy to avoid early bleeding and subacute radial artery occlusion after percutaneous coronary intervention. J Interven Cardiol 2011;24:65-72.
- Kheirabadi B. Evaluation of topical hemostatic agents for combat wound treatment. US Army Med Dep J 2011 Apr-Jun:25-37.
- Smith A, Laird C, Porter K, Bloch M. Haemostatic dressings in prehospital care. Emerg Med J 2013;30(10):784-789.
- Bennett BL, Littlejohn LF, Kheirabadi BS, et al. Management of external hemorrhage in tactical combat casualty care: Chitosan-based hemostatic gauze dressings — TCCC Guidelines-Change 13-05. J Spec Oper Med 2014;14:40-57.
- Gabbe B, Simpson P, Sutherland A, et al. Improved functional outcomes for major trauma patients in a regionalized, inclusive trauma system. Ann Surgery 2012;255(6):1009-1015.
- Gerhardt R, Berry J, Blackbourne L. Analysis of life-saving interventions performed by out-of-hospital combat medical personnel. J Trauma 2011;71(Suppl 1):S109-113.
- Spinella P, Strandenes G. The Trauma Hemostasis and Oxygenation Research Network’s Remote Damage Control Resuscitation Symposium. Shock 2014;41(Suppl 1):1-2.
- Strandenes G, Spinella PC. The Solstrand Remote Damage Control Resuscitation Symposium. Transfusion 2013;53(Suppl 1):6-8.
- Hervig T, Doughty H, Ness P. Prehospital use of plasma: The blood bankers’ perspective. Shock 2014;41(Suppl 1):39-43.
- Dutton R. Resuscitative strategies to maintain homeostasis during damage control surgery. Br J Surg 2012;99(Suppl 1):21-28.
-
Dutton R, Mackenzie C, Scalea T. Hypotensive resuscitation during active hemorrhage: Impact on in-hospital mortality. J Trauma 2002;52(6):
1141-1146. - Bickell W, Wall MJ, Pepe P, et al. Immediate versus delayed fluid resuscitation for hypotensive patients with penetrating torso injuries. N Engl J Med 1994;331(17):1105-1109.
- Duke M, Guidry C, Guice J, et al. Restrictive fluid resuscitation in combination with damage control resuscitation: Time for adaptation. J Trauma Acute Care 2012;73(3):674-678.
- Morrison C, Carrick M, Norman M, et al. Hypotensive resuscitation strategy reduces transfusion requirements and severe postoperative coagulopathy in trauma patients with hemorrhagic shock: Preliminary results of a randomized controlled trial. J Trauma 2011;70(3):652-653.
- Ley E, Clond M, Srour M, et al. Emergency department crystalloid resuscitation of 1.5 L or more is associated with increased mortality in elderly and nonelderly trauma patients. J Trauma 2011;70(2):398-400.
- Kasotakis G, Sideris A, Yang Y, et al. Aggressive early crystalloid resuscitation adversely affects outcomes in adult blunt trauma patients: An analysis of the Glue Grant database. J Trauma Acute Care Surg 2013;74(5):1215-1221.
- Neal M, Hoffman M, Cuschieri J, et al. Crystalloid to packed red blood cell transfusion ratio in the massively transfused patient: When a little goes a long way. J Trauma Acute Care Surg 2012;72(4):892-898.
- Medby C. Is there a place for crystalloids and colloids in remote damage control resuscitation? Shock 2012;41(Suppl 1):47-50.
- Diluting the benefits of hemostatic resuscitation: A multi-institutional analysis. J Trauma Acute Care Surg 2013;75(1):76-82.
- Young J, Utter G, Schermer C, et al. Saline versus Plasma-Lyte A in initial resuscitation of trauma patients: A randomized trial. Ann Surgery 2014;259(2):255-262.
- Guidry C, Gleeson E, Meade P, Stuke ER, McSwain NE. Initial assessment on the impact of crystalloids versus colloids during damage control resuscitation. J Surg Res 2013;185(1):294-299.
- Bhananker S, Ramaiah R. Trends in trauma transfusion. Int J Crit Illn Inj Sci 2011;1(1):51-56.
- Carlino W. Damage control resuscitation from major haemorrhage in polytrauma. Eur J Orthop Surg Traumatol 2014;24(2):137-141.
- Chovanes J, Cannon J, Nunez T. The evolution of damage control surgery. Surg Clin North Am 2012;92(4):859-875.
- Ordonez CA, Badiel M, Pino LF, Salamea JC. Damage control resuscitation: Early decision strategies in abdominal gunshot wounds using an easy ‘‘ABCD’’ mnemonic. J Trauma Acute Care Surg 2012;73(5):1074-1078.
- Davis DT, Johannigman JA, Pritts TA. New strategies for massive transfusion in the bleeding trauma patient. J Trauma Nurs 2012;19(2):69-75.
- Johansson PI, Oliveri RS, Ostrowski SR. Hemostatic resuscitation with plasma and platelets in trauma. J Emerg Trauma Shock 2012;5(2):120-125.
- Dua A, Patel B, Kragh J, Holcomb J, Fox C. Long-term follow-up and amputation-free survival in 497 casualties with combat-related vascular injuries and damage-control resuscitation. J Trauma Acute Care Surg 2012;73(6):1517-1524.
- Shakur H, Roberts I, Bautista R, CRASH-2 Trial Collaborators. Effects of tranexamic acid on death, vascular occlusive events, and blood transfusion in trauma patients with significant haemorrhage (CRASH-2): A randomised, placebo-controlled trial. Lancet 2010;376:23-32.
- Tarmey NT, Woolley T, Jansen JO, et al. Evolution of coagulopathy monitoring in military damage-control resuscitation. J Trauma Acute Care Surg 2012;6(Suppl 5):417-422.
- Hauser C, Boffard K, Dutton R, et al. Results of the CONTROL trial: Efficacy and safety of recombinant activated Factor VII in the management of refractory traumatic hemorrhage. J Trauma 2010;69(3):489-500.
- 53.Lier H, Krep H, Schroeder S, Stuber F. Preconditions of hemostasis in trauma: A review. The influence of acidosis, hypocalcemia, anemia, and hypothermia on functional hemostasis in trauma. J Trauma 2008;65(4):951-960.
- Holcomb JB, Fox EE, Zhang X, White N, Wade CE. Cryoprecipitate use in the PROMMTT study. J Trauma Acute Care Surg 2013;75(Suppl 1):31-39.
- Dutton R. Haemostatic resuscitation. Br J Anaesth 2012;109(Suppl 1):i39-i46.
- Gorgas DL, Kaide G. Transfusion Therapy. In: Roberts JR, ed. Roberts and Hedges’ Clinical Procedures in Emergency Medicine. 6th ed. Philadelphia, PA: Saunders; 2014.
- Spahn D, Bouillon B, Cerny V, et al. Management of bleeding and coagulopathy following major trauma: An updated European guideline. Crit Care 2013;17(2):R76.
- Tobin J, Varon A. Review article: Update in trauma anesthesiology: Perioperative resuscitation management. Anesthesia and Analgesia 2012;115(6):1326-1333.
- Kaafarani H, Velmahos G. Damage control resuscitation in trauma. Scandinavian Journal of Surgery 2014;103(2):81-88.
- Vlaar A, Binnekade J, Prins D, et al. Risk factors and outcome of transfusion-related acute lung injury in the critically ill: A nested case–control study. Crit Care Med 2010;38(3):771-778.
- Li G, Rachmale S, Kojicic M, et al. Incidence and transfusion risk factors for transfusion-associated circulatory overload among medical intensive care unit patients. Transfusion 2011;51(2):338-343.
- Andrzejeweski C, Casey M, Popovasky M. How we view and approach transfusion-associated circulatory overload: Pathogenesis, diagnosis, management, mitigation, and prevention. Transfusion 2013;53(12):3037-3047.
- Hemostatic effects of fresh frozen plasma may be maximal at red cell ratios of 1:2. J Trauma 2011;70(1):90-96.
- Bougle A, Harrois A, Diranteau J. Resuscitative strategies in traumatic hemorrhagic shock. Ann Intensive Care 2013;3:1.
- Bonanno FG. Hemorrhagic shock: The “physiology approach.” J Emerg Trauma Shock 2012;5(4):285-295.
- Zhang YM, Gao B, Wang Jj, Sun Xd, Liu Xw. Effect of hypotensive resuscitation with a novel combination of fluids in a rabbit model of uncontrolled hemorrhagic shock. PLoS One 2013;8(6):e66916.
- Martini RP, Deem S, Treggiari MM. Targeting brain tissue oxygenation in traumatic brain injury. Respiratory Care 2013;58(1):167-172.
- Rosenfeld J, Maas A, Bragge P, Morganti O, Kossmann C, Manley G, Gruen R. Early management of severe traumatic brain injury. Lancet 2012;380(9847):1088-1098.
- Wiles MD. Evidence for damage control resuscitation is lacking. BMJ 2012;345:e7205.
- Curry P, Viernes D, Sharma D. Perioperative management of traumatic brain injury. Int J Crit Illn Inj Sci 2011;1(1):27-35.
- Schöchl H, Nienaber U, Hofer G, et al. Goal-directed coagulation management of major trauma patients using thromboelastometry (ROTEM)-guided administration of fibrinogen concentrate and prothrombin complex concentrate. J Crit Care 2010;14(2):R55.
- deBiasi A, Stansbury L, Dutton R, Stein D, Scalea T, Hess J. Blood product use in trauma resuscitation: Plasma deficit versus plasma ratio as predictors of mortality in trauma. Transfusion 2011;51(9):1925-1932.
- Moore E, Chin T, Chapman M, et al. Plasma first in the field for postinjury hemorrhagic shock. Shock 2014;41(S1):35-38.
- Martinaud C, Ausset S, Deshayes A, Cauet A, Demazeau N, Sailliol A. Use of freeze-dried plasma in French intensive care unit in Afghanistan. J Trauma 2011;71(6):1761-1764.
- Brenner M, Moore L, DuBose J, et al. A clinical series of resuscitative endovascular balloon occlusion of the aorta for hemorrhage control and resuscitation. J Trauma Acute Care Surg 2013;75(3):506-511.
MONOGRAPH: Exsanguinating hemorrhage is one of (if not the) most common preventable cause of death after trauma.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.