Man-made Disaster: In-hospital Management
November 1, 2015
Reprints
Authors
Robert E. Falcone, MD, FACS, Vice President Population Health, Ohio Hospital Association, Clinical Professor of Surgery, The Ohio State University, Columbus.
Andrew Detty, BA, Quality and Population Health Analyst, Ohio Hospital Association, Columbus.
Peer Reviewer
James J. Augustine, MD, Clinical Professor, Department of Emergency Medicine, Wright State University, Dayton, OH; Director of Clinical Operations, EMP Management, Canton, OH; Medical Director for Fire EMS Services in Ohio, and Atlanta, GA.
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Executive Editor Ms. Mark’s spouse works for a company that creates advertising for Uroplasty. Dr. Dietrich (editor in chief), Dr. Falcone (author), Mr. Detty (author), Dr. Augustine (peer reviewer), Ms. Behrens (nurse reviewer), and Mr. Landenberger (continuing education and editorial director) report no relationships with companies related to this field of study.
Executive Summary
- Blast injury is generally divided into four categories based on the mechanism of injury: primary, secondary, tertiary, and quaternary. Many of the injured are exposed to more than one mechanism, and the outcome is determined by a number of factors, including the size of the detonation, the distance from the explosion, the surrounding environment (open air vs. enclosed space), and the presence of fire, toxic gases, projectiles, and biologic agents.
- A ruptured tympanic membrane (TM) once was considered pathognomonic of a potential primary blast injury (lung or gastrointestinal tract), but the recent literature does not support this analysis.
- The victims of mass public shootings with serious injury are largely subject to penetrating injury, and the number one cause of preventable death in this population is hemorrhage. The Hartford Consensus (of experts) recommends five critical actions contained in the acronym THREAT: 1. Threat suppression; 2. Hemorrhage control; 3. Rapid extraction to safety; 4. Assessment by medical providers; 5. Transport to definitive care.
- The time of onset of vomiting from exposure provides a rough guide to the severity of radiation exposure.
- External dosimetry of the body and wounds, and dosimetry of the excreta, can predict the level of contamination and direct further decontamination or debridement.
The human capacity for misadventure, both accidental and intentional, is boundless and legendary. Our past and recent history are filled with mass casualty situations directly related to human action. There are also many examples of natural calamities, which have become man-made disasters as a result of inaction, incompetence, a lack of resources, or a combination thereof. Natural calamities and their management (most notably the federal response to hurricane Katrina1) are beyond the scope of this paper.
Man-made disaster directly impacts the emergency department (ED) and hospital when a mass casualty situation ensues, and is the focus of this review article. Using contemporary examples and the current literature, what follows is a primer on the causes, injury patterns, resource utilization, triage, and preparation for man-made mass casualty events. These include explosions, fires, crush events, and public mass shootings, as well as vehicular, chemical, biological, and radiation events.
— The Editor
Mass Casualty Events
Explosion. Accidental explosions are relatively common and, fortunately, rarely lead to mass casualty events. One notable exception occurred on August 12, 2015, in China, where a series of explosions devastated a container storage station at the Port of Tianjin. The first two explosions, which occurred within seconds of each other, were from hazardous materials in shipping containers at a plant warehouse located in the Binhai New Area of Tianjin. Several other explosions followed three days later as the result of massive fires.2 As of August 2015, there were 123 dead, 50 missing (mostly firefighters), and, according to the Tianjin government, more than 700 injured by blast and subsequent fire.3 In the United States, the explosion event of note occurred in 2013 in West, TX. Fifteen people were killed, approximately 200 were injured, and close to 200 buildings were damaged. Ammonium nitrate was the agent.4
Intentional explosion, a tool well-known to terrorists, results in blast injury, which can be a dramatic cause of mass casualty situations. There have been more than 50 local wars and conflicts in the first decade of this century, and significant terrorist activity in Afghanistan, Britain, India, Iraq, Pakistan, and Spain.5 Major trends in terrorism in 2014 have largely involved the Islamic State in Iraq and the Levant’s (ISIS) activity in Iraq, Syria, Yemen, Libya, and Nigeria.6
It would be tempting to consider terrorist activity an overseas problem; however, it is much too common on U.S. soil. In point of fact, in the two decades between 1983 and 2002, more than 36,100 criminal bombing incidents occurred on American soil, and a number of high-profile terrorist bombings leading to mass casualty situations have occurred in the United States during the past two decades. (See Table 1.)
Table 1. Civilian Blast Event Severity of Injury
Event and Year |
Casualties |
Dead |
Treated |
Explosive |
|
Hospitalized |
Released |
||||
|
Adapted from Falcone R. Civilian blast injury. Trauma Reports 2013;14(5):1–11. |
|||||
|
Oklahoma City 1995 |
759 |
168 (22%) |
83 (14%) |
508 (86%) |
Fertilizer and fuel oil |
|
Atlanta Olympics 1996 |
111 |
1 (< 1%) |
24 (22%) |
87 (78%) |
Pipe bomb and shrapnel |
|
World Trade Center 2001 |
3922 |
2819 (72%) |
181 (17%) |
810 (73%) |
Jet fuel |
|
Madrid 2004 |
2000 |
191 (10%) |
91 (29%) |
221 (71%) |
Military explosives and shrapnel |
|
London 2005 |
775 |
56 (7%) |
27 (14%) |
167 (86%) |
Military explosives and shrapnel |
|
Boston Marathon 2013 |
267 |
3 (1%) |
20 (8%) |
244 (92%) |
Black powder and shrapnel |
Blast injury is generally divided into four categories based on the mechanism of injury: primary, secondary, tertiary, and quaternary. (See Table 2.) Many of the injured are exposed to more than one mechanism, and the outcome is determined by a number of factors, including the size of the detonation, the distance from the explosion, the surrounding environment (open air vs. enclosed space), and the presence of fire, toxic gases, projectiles, and biologic agents. Table 3 summarizes common blast-related injuries.
Table 2. Classification of Blast Injuries
Classification |
Type |
Mechanism |
Typical Injuries |
|
Adapted from: Falcone R. Civilian blast injury. Trauma Reports 2013;14(5):1–11. |
|||
|
Primary |
Blast wave |
||
|
Implosion |
Air-filled structures rupture from over-pressurization |
Tympanic membrane rupture, blast lung, gastrointestinal rupture |
|
|
Spalling |
Explosive energy transfer in tissue interfaces of differing density |
Lung, liver, brain contusion |
|
|
Inertia |
Acceleration and deceleration forces lead to shearing injury |
Mesenteric tears, axonal injury |
|
|
Secondary |
Blast wind |
Bomb fragments, displaced foreign bodies |
Penetrating or blunt multi-system injury |
|
Tertiary |
Blast wave and wind |
Individual or structure thrown or crushed |
Penetrating or blunt multi-system injury |
|
Quaternary |
By-products of explosion |
Fireball and toxic agents |
Burns and inhalation injuries |
Table 3. Overview of Explosion-related Injuries
System |
Injury or Condition |
|
Adapted from Falcone R. Civilian blast injury. Trauma Reports 2013;14(5):1–11. |
|
|
Auditory system |
Tympanic membrane rupture, ossicular disruption, cochlear damage, foreign body |
|
Cardiovascular |
Cardiac contusion, myocardial infarction from air embolism, shock, vasovagal hypotension, peripheral vascular injury, air embolism-induced injury |
|
Extremity injuries |
Traumatic amputations, fractures, crush injuries, compartment syndrome, burns, cuts, lacerations, acute arterial occlusion, air embolism-induced injury |
|
Gastrointestinal |
Bowel perforation, hemorrhage, ruptured liver or spleen, sepsis, mesenteric ischemia from air embolism |
|
Neurologic system |
Concussion, closed and open brain injury, stroke, spinal cord injury, air embolism-induced injury |
|
Ocular injury |
Perforated globe, foreign body, air embolism, fracture |
|
Renal injury |
Renal contusion, laceration, acute renal failure due to rhabdomyolysis, hypotension, and hypovolemia |
|
Respiratory system |
Blast lung, hemothorax, pneumothorax, pulmonary contusion and hemorrhage, arteriovenous fistulas (source of air embolism), airway epithelial damage, aspiration pneumonitis, sepsis |
Because blast injury often involves multiple simultaneous mechanisms, these patients are typically more seriously injured than a multiple trauma cohort, and subsequently sustain a higher morbidity and mortality.5 Primary, secondary, tertiary, and quaternary mechanisms may all impact the victim simultaneously, making the chance of missed injury higher and time to treatment critical. “Delayed” injury, which is often a blast-associated injury to hollow viscus, should be carefully anticipated.
Unfortunately, in the absence of obvious injury, there is no accurate harbinger of occult or delayed primary blast injury. The common wisdom has been that a ruptured tympanic membrane (TM) was pathognomonic of a potential primary blast injury (lung or gastrointestinal tract), but the recent literature does not support this analysis.7,8,9 For example, in the London train bombings in 2005, TM injury as a marker of more serious injury had a low positive predictive value and a sensitivity and specificity no better than random chance.8 Evidence of significant external injury may be more predictive.5
Fortunately, the majority of survivors are not severely injured. (See Table 1.) The scenes of injury, however, are often initially chaotic: Communication with the field is difficult, if not dysfunctional, and transportation hectic. The result is that the nearest facility is often inundated with patients, many of whom are “walking wounded.” Triage, rapid mobilization of available resources, and regional coordination of hospital and trauma center resources are essential. A recent review of civilian blast injury provides a good primer on this subject.5
Fire. Although a mass casualty fire event is not common, the results can be devastating.10 There are multiple victims, often with extensive burns and concomitant injuries, which are resource-intensive. Burns as a result of terrorist attacks are usually the result of explosions, and the burn injuries are often moderate.11 However, burn injuries as a result of human misadventure can be devastating, as described in the case of the Tianjin explosions and fire described above.
One recent event is particularly illustrative. On February 20, 2003, a nightclub fire in Rhode Island caused a mass casualty situation. Four hundred thirty-nine people were in the club at the time: 96 died at the scene, four subsequently died in hospital, and 215 were transported to 16 local hospitals. Sixty-four patients were transferred to the Rhode Island Hospital (RIH), the state’s only trauma center. Forty-seven (73%) were admitted, 17 were treated and released, eight were transferred to other trauma centers, and 32 were admitted to other hospitals.
The RIH experience points to the enormous resource utilization a mass casualty burn event might require. Sixty percent of the admitted patients were intubated, and 30% had greater than 20% total body surface burn. Emergent surgical procedures included one cricothyroidotomy and 12 escharotomies. A total of 32 patients required 184 bronchoscopies. The average length of stay was 21.5 days (range 1–77).12
In fire events, proper use of limited burn resources and knowledge of regional resources are necessary. For example, in the Savannah sugar refinery explosion and fire event in 2008, a burn team from the Joseph M. Still Burn Center in Augusta, GA, was flown to Savannah to assist in triage of burn resources and management of victims at the local trauma center.13 The Las Vegas casino fires, the last in 1980, are further examples of mass casualty incidents involving the use of a community’s entire health system.14
Crush Events. These incidents involve the movement of people in a congested space, in a manner that results in severe injury and loss of life. These occur in large public events and entertainment venues, and can occur when someone raises a concern about fire, terrorism, or active weapons. Crush conditions in exit doorways were a factor in the Rhode Island nightclub fire referenced above, preventing the egress of nightclub patrons.15 In the crush event in Cincinnati at a Who rock concert in 1979, 11 people died and at least 26 were injured.16 In Chicago in 2003, a stampede occurred when pepper spray was released in a nightclub, and 21 people died and more than 50 were injured.17 Crush injuries can occur from rapid and uncontrolled crowd movement due to real or perceived threats.
Public Mass Shooting. The Congressional Research Service (CRS) defines a public mass shooting as one that occurs in a relatively public place and involves four or more deaths, not including the shooter(s). From 2000 to 2013, a total of 160 public mass shootings resulted in 486 deaths and 557 wounded.18 Figure 1 illustrates a disturbing trend in increasing incidence. Three recent public mass shootings are illustrative: Newtown, CT; Aurora, CO; and Fort Hood, TX.
Figure 1. Annual Casualty Totals in 160 Active Shooter Incidents, United States, 2000-2013
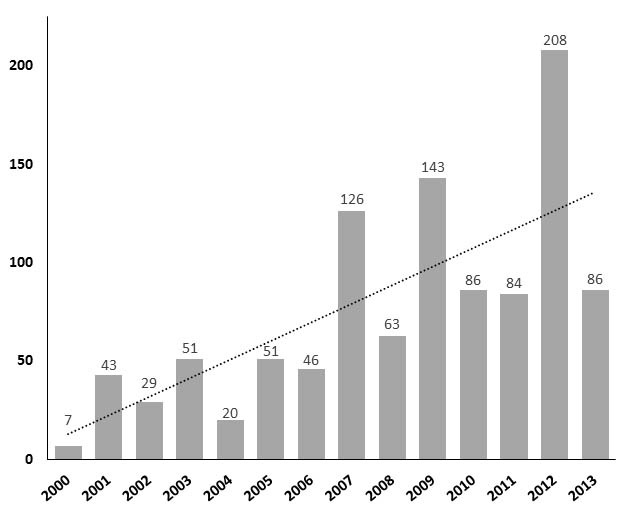
Source: Blair JP, Schweit KW. A study of active shooter incidents in the United States between 2000 and 2013. Washington, DC: Texas State University and Federal Bureau of Investigation, U.S. Department of Justice; 2014. Retrieved from https://www.fbi.gov/news/stories/2014/september/fbi-releases-study-on-active-shooter-incidents/pdfs/a-study-of-active-shooter-incidents-in-the-u.s.-between-2000-and-2013.
Newtown, CT. On December 14, 2012, Adam Lanza fatally shot his mother with a .22 caliber Savage MK II-F bolt action rifle. Then, armed with his mother’s Bushmaster XM15-E2S semiautomatic rifle and Glock 20 10 mm and Sig Sauer P226 semiautomatic handguns, he went on to methodically shoot and kill 20 children and six adults at the Sandy Hook Elementary School in Newtown, CT. Eighteen children and 6 adults were pronounced dead at the scene, and two children and two adults were transported to local hospitals. The children were pronounced dead in the ED, and the two adults were treated and survived.19 In this setting, hospital resources were not stretched, but community resources to respond to shock and grief were.
Aurora, CO. On July 20, 2012, James Egan Holmes, armed with two tear gas grenades, a Smith & Wesson rifle, a tactical shotgun, and a Glock 22 handgun,20 opened fire in a theater full of people and methodically began to shoot his victims. There were 12 deaths and 70 injuries (58 gunshot or shotgun wounds, four tear gas injuries, and eight blunt injuries from fleeing the scene). Ten fatalities were pronounced at the scene, one victim was dead on arrival to the ED, and another was pronounced dead after a short resuscitation.21
Most of the patients were transported to The Medical Center of Aurora (a Level II Trauma Center), the University of Colorado Hospital (UCH), the Children’s Hospital of Colorado (a Level I Pediatric Trauma Center), which took several adult victims, and several other surrounding hospitals.22
The UCH experience is particularly illustrative of the chaos that frequently follows a mass casualty shooting. The first patients, a mother and infant, arrived by private vehicle, and within minutes, nine police vehicles brought one to three patients each to the UCH ED. Three patients subsequently arrived by ambulance, and another arrived on foot. In total, UCH received 23 patients within minutes of the event. Frequent preparedness activities and drills were credited with an amazing response to a zero-notification event.23
Fort Hood, TX. On April 2, 2014, Fort Hood experienced its second public mass shooting in five years. The first occurred in 2009 and resulted in 13 deaths and 30 wounded; the second, in 2014, resulted in four deaths and 14 wounded. The shooter, 34-year-old Army Specialist Ivan Lopez, used a .45 caliber Smith & Wesson MP handgun and died of a self-inflicted gunshot wound. The victims were initially transported to a single Level III Trauma Center located on the base (Carl R. Darnall Army Medical Center). It should be noted that one victim with an arm wound and an abdominal injury unnoticed on initial triage was quickly identified on subsequent secondary triage.24
The victims of mass public shootings with serious injury are largely subject to penetrating injury, which is surgically intensive in resource utilization. Unlike victims of blast injury, many shooting survivors are critically injured and often require urgent or emergent multidisciplinary operative intervention. The number one cause of preventable death in this population is hemorrhage. The Hartford Consensus (of experts)25 recommends five critical actions contained in the acronym THREAT:
- Threat suppression;
- Hemorrhage control;
- Rapid extraction to safety;
- Assessment by medical providers;
- Transport to definitive care.
Prehospital providers, including law enforcement, should clearly understand hemorrhage control. Extremity hemorrhage may require control with tourniquet use,25,26 and torso and head hemorrhage may not be amenable to field treatment and may require rapid transport for management in a hospital setting.27 Transfer to definitive care is often chaotic, but, when possible, should be to the facility or facilities most capable of handling penetrating injury. However, any facility proximate to the disaster may be tasked with initial triage, resuscitation, and initial definitive care.
In the setting of mass casualties, damage control surgery is an appropriate option.27 A discussion of damage control is beyond the scope of this review, but put simply, it includes stopping bleeding, controlling contamination, reestablishing critical vascular flow (usually with temporary shunts), and delaying definitive repair until resuscitation is complete or resources are available.
Vehicle. Car/Truck. In the first half of this decade, there have been more than 18 documented chain-reaction motor vehicle collisions in the United States, involving 1390 vehicles and leading to 346 injuries and 34 deaths. The average number of dead and injured per incident is two deaths and 30 injuries (median: one death and 24 injuries). The weather that causes these crashes often delays emergency response, and transport may be delayed significantly. Triage may be limited in inclement weather conditions.
Train. There have been seven major U.S. mass casualty train disasters in the past 10 years, resulting in 693 injuries and 69 deaths. (See Table 4.) The injuries are typically blunt, although foreign body penetration, burns, and smoke inhalation are not uncommon. Unlike victims of motor vehicle collisions, who are in an enclosed space and often protected by seatbelts and airbags, victims in train collisions frequently become projectiles, leading to a disproportionate number of head, spine, and extremity injuries.28
Table 4. Mass Casualty Railroad Accidents, United States, 2002-2015
Date |
Location |
# Killed |
# Injured |
|
Source: Center for Justice & Democracy. (June 17, 2015). Fact Sheet: Mass-Casualty Railroad Accidents and Liability Caps. Retrieved from http://centerjd.org/content/fact-sheet-mass-casualty-railroad-accidents-and-liability-caps. |
|||
|
April 18, 2002 |
Crescent City, FL |
4 |
142 |
|
Sept. 25, 2005 |
Glendale, CA |
11 |
180 |
|
Sept. 12, 2008 |
Chatsworth, CA |
25 |
135 |
|
June 22, 2009 |
Washington, DC |
9 |
80 |
|
June 24, 2011 |
Churchill County, NV |
6 |
16 |
|
Dec. 1, 2013 |
Bronx, NY |
4 |
≥ 70 |
|
Feb. 3, 2015 |
Valhalla, NY |
6 |
≥ 12 |
|
May 12, 2015 |
Philadelphia, PA |
8 |
≥ 200 |
Temple University Hospital’s experience with the 2015 Amtrak regional train derailment in Philadelphia is illustrative. This derailment led to eight deaths and more than 200 injuries. Temple University Hospital (a Level I Trauma Center) received the greatest proportion of casualties, seeing 54 patients and admitting 24. One of these patients died with five fatal injuries noted on autopsy. Many of the injured had chest and extremity injuries, but perhaps not surprisingly for a largely blunt mechanism, only three of the 24 patients admitted as inpatients went to the operating room that night.28 The remainder of the injured went to nine area hospitals. Notably, several patients of the 28 treated at Hahnemann University Hospital had spinal cord injuries.28
Airplane. Air disasters are unusual and quite rare on U.S. soil, with only 12 mass casualty incidents in the past 50 years. Although mass casualty events involving hospital care can occur, the overwhelming majority of victims die at the scene. (See Table 5.)
Table 5. Ten Air Crashes on US Soil with the Greatest Number of Fatalities, 2000-Present
Date |
Onboard Fatalities |
Total # Onboard |
Location |
Aircraft Type |
Source |
|
Feb. 12, 2009 |
49 |
49 |
Buffalo, NY |
Bombardier Dash-8 Q400 |
Wald ML, Robbins L. (2009, February 13). 50 Killed as Plane Hits House Near Buffalo. The New York Times. Retrieved from http://www.nytimes.com |
|
Aug. 27, 2006 |
49 |
50 |
Lexington, KY |
Bombardier CL-600-2B19 |
National Transportation Safety Board. (2007). Attempted Takeoff From Wrong Runway, Comair Flight 5191, Bombardier CL-600-2B19, N431CA, Lexington, Kentucky, August 27, 2006. Washington, DC: National Transportation Safety Board. Retrieved from http://www.ntsb.gov |
|
Jan. 8, 2003 |
21 |
21 |
Charlotte, NC |
Beechcraft 1900D |
National Transportation Safety Board. (2004). Loss of Pitch Control During Takeoff Air Midwest Flight 5481 Raytheon (Beechcraft) 1900D, N233YV Charlotte, North Carolina January 8, 2003. Washington, DC: National Transportation Safety Board. Retrieved from http://www.ntsb.gov |
|
Nov. 12, 2001 |
260 |
260 |
New York, NY |
Airbus A300-605R |
National Transportation Safety Board. (2004). In-Flight Separation of Vertical Stabilizer American Airlines Flight 587 Airbus Industrie A300-605R, N14053 Belle Harbor, New York November 12, 2001. Washington, DC: National Transportation Safety Board. Retrieved from http://www.ntsb.gov |
|
Sept. 11, 2001 |
92 |
92 |
New York, NY |
Boeing 767 |
National Commission on Terrorist Attacks Upon the United States. (2004). The 9/11 Commission Report: Final Report of the National Commission on Terrorist Attacks Upon the United States (9/11 Report). Washington, DC: Government Printing Office. Retrieved from http://www.gpo.gov |
|
Sept. 11, 2001 |
65 |
65 |
New York, NY |
Boeing 767 |
9/11 Report |
|
Sept. 11, 2001 |
64 |
64 |
Washington, DC |
Boeing 757 |
9/11 Report |
|
Sept. 11, 2001 |
44 |
44 |
Harrisburg, PA |
Boeing 757 |
9/11 Report |
|
March 3, 2001 |
21 |
21 |
Unadilla, GA |
Short 330 |
CNN. (2001, March 3). 21 dead in National Guard plane crash in Georgia. CNN.com. Retrieved from http://www.cnn.com |
|
Jan. 31, 2000 |
88 |
88 |
Los Angeles, CA |
McDonnell Douglas MD-83 |
National Transportation Safety Board. (2003). Aircraft Accident Report: Loss of Control and Impact with Pacific Ocean Alaska Airlines Flight 261 McDonnell Douglas MD-83, N963AS About 2.7 Miles North of Anacapa Island, California January 31, 2000. Washington, DC: National Transportation Safety Board. Retrieved from http://www.ntsb.gov |
In the case of Asiana Airlines Flight 214, which crashed at San Francisco International Airport on July 6, 2013, two of the 307 individuals aboard the plane died, and more than 180 were injured, one of whom died 6 days later. In addition to improved plane design, speedy evacuation, rapid fire extinguishment, and effective rescue efforts, observers attributed the relatively low death rate in part to the use of established protocols for triage and re-triage at the crash scene.29
US Airways Flight 1549, piloted by Chesley Sullenberger on January 15, 2009, is another notable illustration of a survivable air crash with injuries. Multiple bird strikes caused both engines to fail on takeoff, and the pilots were forced to make an unpowered emergency landing on the Hudson River. Rescue efforts were largely by untrained good Samaritans on nearby watercraft.
There were 155 occupants and no fatalities. Seventy-eight people were treated for injuries, which were mostly minor, in the prehospital setting. Twenty-four passengers and two rescue workers were transported to four local hospitals. Eight patients were seen at Saint Vincent’s Catholic Medical Center, 10 at St. Luke’s Roosevelt Hospital Center, three at New York Downtown Hospital, and five at Palisades Medical Center in North Bergen, NJ. Injuries included bumps, bruises, lacerations, and hypothermia. Only two of the 26 patients who received hospital care required an overnight stay.30 Excellent scene triage meant that no individual hospital was overwhelmed with patients.
Vehicular mass casualty events may initially stretch local resources; however, good scene triage, appropriate patient distribution, and a typically low acuity load mitigate the overwhelming of hospital resources. Because the injuries are usually blunt, careful triage and re-triage are essential to assure the appropriate use of limited resources such as ED bays, critical care beds, and computerized axial tomography (CAT) scanners.
Chemical. The documented use of chemical agents as weapons of war and terror dates to the Peloponnesian War (431 BCE) when Thrace and Sparta used burning coal, sulfur, and pitch to insufflate fumes into a fort during a siege.31 There are multiple examples of other forms of chemical and biologic warfare; however, modern chemical warfare was ushered in by the use of chlorine gas during World War I (WWI). International treaties ban the current use of chemical weapons in war, although there is strong evidence that chemical weapons were used recently in the Syrian civil war.32
There are four major classes of chemical weapons: cyanide, pulmonary agents, vesicants, and nerve agents. In addition, there are several common riot control agents used to disperse crowds or incapacitate an individual. (See Table 6.)
Table 6. Nerve Agents and Riot Control Agents
Common Name |
NATO Name |
|
Sources: • Adapted from Schecter WP, Fry DE. The surgeon and acts of civilian terrorism: Chemical agents. J Am Coll Surgeons 2005;200:128–135. • Borden Institute, US Army Medical Research Institute of Chemical Defense, & Office of The Surgeon General, United States Army. Medical Management of Chemical Casualties Handbook, 5th ed. Fort Sam Houston: Office of the Surgeon General; 2014. Retrieved from http://www.cs.amedd.army.mil/borden/Portlet.aspx?ID=a0968070-71b0-46c0-a139-9362d1b13265. |
|
|
Nerve Agents |
|
|
Tabun |
GA |
|
Sarin |
GB |
|
Soman |
GD |
|
GF |
GF |
|
VX |
VX |
|
Riot Control Agents |
|
|
O-chlorobenzylidene malononitrile |
CS |
|
Bromobenzylcyanide |
CA |
|
Chloroacetophenone (Mace) |
CN |
|
CR |
CR |
|
Diphenylaminearsine |
DM |
|
Capsaicin (pepper spray) |
OC |
Cyanide is a naturally occurring plant substance. Hydrogen cyanide and cyanogen chloride both exist as volatile liquids or gases. Because of this volatility, cyanide is most effective in closed spaces (e.g., in the Nazi German death camps).31
The chemical can be absorbed by ingestion, percutaneous absorption, or inhalation. The cyanide ion forms a strong but reversible bond in the mitochondrial cytochrome system. Untreated poisoning leads to rapid loss of consciousness, apnea, and death. The treatment choices for cyanide poisoning are the use of a binding agent like hydroxocobalamin, or the sequential use of agents to oxidize cyanohemoglobin to methemoglobin using amyl nitrite, and shortly thereafter use of thiosulfate to break down the resulting methemoglobin.31
Pulmonary Agents. Chlorine used during WWI was quickly replaced with the more effective phosgene gas. The effects are a progressive respiratory distress and eventual pulmonary edema from small airway injury.31 In 1984, a Union Carbide plant in Bhopal, India, inadvertently vented methyl isocyanate gas (a precursor to phosgene) into the surrounding air, killing 3800 victims and permanently disabling an additional 2700 people.33 A 2005 rail crash in Graniteville, SC, involving a major chlorine release resulted in nine deaths.34 These events provide good examples of the lethality of this class of chemicals. A specific treatment beyond respiratory care with mechanical ventilation and critical care support (if needed) is not available.31 Attempts by insurgents in Iraq to add chlorine canisters to improvised explosive devices exemplify the potential to use these agents to produce human and environmental catastrophes.35
Vesicants. Nitrogen mustard is an effective chemical weapon used in the 1980s in the Iraq-Iran war with an estimated 40,000 Iranian casualties. Mustard is generally a liquid and is often absorbed transcutaneously. The effects are dependent on the extent and duration of exposure. The topical effect is typical of a partial thickness burn; the systemic effect is bone marrow suppression. The injuries are often delayed by hours, making this a particularly insidious weapon.31
Nerve Agents. Nerve agents are cholinesterase inhibitors that result in a cholinergic crisis. These organophosphates were originally introduced as insecticides, but have subsequently been developed as weapons of war and terror. Fortunately, their use is outlawed by international treaty;36 unfortunately, known (and unknown) stockpiles still exist.37
There are five contemporary agents: tabun (GA), sarin (GB), soman (GD), GF, and VX. Each has its own toxic profile and nuance. The effects are muscarinic (visceral) and nicotinic (muscular). Treatment starts with decontamination in the field, followed by secondary decontamination outside the ED. Responders providing emergency resuscitation must wear protective garb. Specific treatment is with atropine and pralidoxime chloride (PAM).
Riot Control Agents. Riot control agents are used to control individuals or disperse crowds. They have a relatively low toxicity and are meant to irritate skin and mucous membranes. Tearing, sneezing, vomiting, and skin irritation are the common effects. Common agents include o-chlorobenzylidene malononitrite (CS), bromobenzylcyanide (CA), diphenylaminearsine (DM), and capsaicin (pepper-spray). Pepper spray is already aerosolized and marketed as a self-defense agent. High concentrations of the agent are present in canisters intended for use as a bear repellent. The others are solids that are generally aerosolized by detonation.31 Fresh air and water irrigation usually suffice as treatment. More serious injury may result from the canister projectile, the fragments of detonation, or exacerbation of underlying chronic pulmonary disease.
Two terrorist incidents from the late 20th century illustrate the devastating effect of chemical weapons on a civilian population. In 1994, Aum Shinrikyo terrorists released sarin gas in Matsumoto, Japan, killing eight and injuring 200 people.31 One year later, this same terrorist bloc released sarin gas in a crowded Tokyo subway, resulting in 12 deaths and 1038 poisonings. Most pertinent to our discussion of mass casualty events, 4460 walking well presented to Tokyo hospitals, overwhelming the health care system.38
Fortunately, we have not had a major chemical event in the United States since 1968, when 320 gallons of VX were accidentally released at the Dugway Proving Ground in Utah, drifting 45 miles and killing thousands of sheep.39
Still, preparation for accidental or intentional chemical release is essential to disaster preparedness. Scene decontamination with fresh air, clothing removal, and water is essential and should be continued in the hospital setting.31 Although all hospital responders should have a working knowledge of chemical poisoning, the primary responsibility for management usually falls on the ED clinicians. Schecter and Fry recommend modifying the Advanced Trauma Life Support (ATLS) paradigm to ABCDDDE (Airway, Breathing, Circulation, Decontamination, Drugs, Disability, and Exposure) to remind the resuscitation team of the basics of chemical injury management.31 Good reference material is available in the literature,31 and the reader is encouraged to pursue a deeper understanding.
Biologic. These agents can be either disease-producing bacteria or viruses (pathogens), or poisons of bacterial origin (toxins).31,33 Typical pathogens include anthrax, tularemia, and smallpox. Typical toxins include botulinum, ricin, and mycotoxin.
In the 1950s and 1960s, Fort Detrick, MD, was the Army’s biological warfare center. The army conducted a number of open-air tests during this period to evaluate dispersal and effect of “harmless agents.” One such test occurred in 1950, when the army sprayed the San Francisco Bay with Serratia marcescens, thought to be a harmless bacterium. The result was the hospitalization of 11 patients with the never-before-seen pathogen (Serratia) and one death.40
Anthrax was a particular concern during the first Gulf War and the 2003 invasion of Iraq, leading to a number of protective measures for the troops, including vaccination. Anthrax was also used as a weapon of terror in September and October 2001, when the U.S. Postal Service inadvertently delivered at least five letters containing weaponized anthrax to two senatorial offices and media organizations in New York City and Boca Raton, FL. Five people died as a result of inhalational exposure, and another 17 were injured as a result of cutaneous exposure. Ten thousand people potentially exposed during these incidents received prophylactic antibiotics and careful monitoring.41
Additionally, more than 750 copycat events occurred in October and November that same year, with resulting chaos for the victims, communities, and health care workers involved.40 One example of a copycat event occurred in Columbus, OH, in September 2001, when a worker in a state office building inadvertently exposed a number of coworkers to a brown powder sent through the mail. Several patients were taken to Grant Medical Center, the Level I Trauma Center most proximate to the event. There they underwent decontamination outside the ED in makeshift outdoor showers, and were subsequently evaluated and treated with antibiotic prophylaxis prior to the confirmation that the substance was not toxic. This scenario, which played out in multiple cities, caused significant disruption during the months that followed the September 11, 2001, World Trade Center attack.42
Another particularly illustrative event occurred in central Ohio in 2015, when a church group inadvertently ingested home-canned potato products contaminated with botulinum toxin. The result was the largest botulism outbreak in the United States since 1994. In all, 77 people attended the event where the products were served. Two patients presented to the local ED with stroke-like symptoms. The staff rapidly made the diagnosis, called for antitoxin from the Centers for Disease Control and Prevention (CDC), and involved the Ohio Department of Health and the Central Ohio Trauma System (a regional trauma and disaster resource). The local ED saw more than 50 patients. There were 25 confirmed and four probable cases. In the end, because of a rapid and coordinated response, only one person died. Twenty-nine others, however, were hospitalized in several surrounding tertiary facilities, and many required prolonged critical care. Other “worried well” flooded local EDs to assure they were not contaminated with the toxin.43
The treatment of biologics varies by the agent: Pathogens are generally treatable with antibiotics, antivirals, or antifungals; botulism is responsive to antitoxin; and anthrax may be prevented with immunization. The viral agents are generally contagious; the others are not (although the inciting contaminant may be). There are a number of excellent resources on biologic agents from the American College of Surgeons.44
Radiation. Despite the ubiquitous use of radioactive material in health care, research, manufacturing, energy, and defense, nuclear accidents involving serious injury are rare. Between 1944 and 2000, 243 nuclear accidents on U.S. soil have led to 1342 persons exposed (790, or 59% seriously exposed) and 30 deaths, for an overall mortality of 2.2%.45 (See Table 7.)
Table 7. U.S. Radiation Accidents Resulting in Deaths (1944-December 1999)
State |
Number of Deaths |
Accident Circumstances |
|
Adapted from: Ricks RC, Berger ME, Holloway EC, et al. REAC/TS Radiation Accident Registry: Update of Accidents in the United States. Oak Ridge: Oak Ridge Institute for Science and Education; 2000. Retrieved from http://www.irpa.net/irpa10/cdrom/00325.pdf. |
||
|
Idaho |
3 |
Trauma/reactor criticality (non-radiation death) |
|
New Mexico |
3 |
2 – Research with critical assembly 1 – Chemical operations/criticality |
|
Ohio |
10 |
Radiation therapy |
|
Oklahoma |
1 |
Self-inflicted injury (probable) |
|
Pennsylvania |
1 |
Radiation therapy (brachytherapy) |
|
Rhode Island |
1 |
Chemical operations/criticality |
|
Texas |
9 |
7 – Nuclear medicine therapy 2 – Radiation therapy/computer programming |
|
Washington |
1 |
Radiation therapy (non-radiation death) |
|
Wisconsin |
1 |
Nuclear medicine therapy |
There have been 10 nuclear disasters worldwide graded International Nuclear Event Scale (INES) Level 4 to Level 7 since 1957.46 Three of these events are notable for their severity: Three Mile Island, PA, 1979, Level 5; Chernobyl, Ukraine, 1986, Level 7; and Fukushima, Japan, 2011, Level 7.46 There were no deaths nor radiation casualties reported for the Three Mile Island and Fukushima events; the Chernobyl event resulted in 30 deaths and, according to the United Nations Scientific Committee on the Effects of Atomic Radiation (UNSCEAR), apart from an increased incidence of thyroid cancer, “there is no evidence of a major public health impact attributable to radiation exposure 20 years after the accident.”47 The latter two of these events produced significant and ongoing environmental damage.
The threat, of course, remains one of nuclear terrorism. With the relative availability of nuclear material from medicine, science, industry, and defense, the opportunity to spread nuclear material (and panic) with “dirty bombs,” poisoned environmental resources, or crude nuclear weapons is an ongoing threat. Terrorist groups, including al-Qaida, Chechen separatists, Lashkar-e-Taiba, and Aum Shinrikyo, have all professed an interest in obtaining a nuclear weapon,48,49 making the threat more proximate.
Conceding that radiation exposure, either accidental or intentional, is an unlikely cause of a mass casualty situation, the potential for disaster and panic mandate a basic understanding of the assessment and management of this potential threat.50 The potential for devastation is real. For example, it has been estimated that a relatively small (1 megaton) nuclear detonation in Chicago would result in an immediate loss of one-third of the hospitals, disruption to emergency medical services (EMS), an influx of walking wounded with varying degrees of radiation sickness, untold numbers of serious burns and injuries, and devastating mortality.51 The immediate morbidity and mortality of the 1944 nuclear detonation (16 kilotons) in Hiroshima, an industrial Japanese city, resulted in an estimated 135,000 casualties (half the population), and 66,000 deaths. Sixty percent of the deaths were from burn injuries.52
Potential victims could be irradiated, contaminated with radioactive material, or injured by heat or explosion.50 Exposure to penetrating radiation leads to potential irradiation injury, which is often local (e.g., limited to the hand), or systemic (when a majority of the body is exposed). Contamination can be external (when radioactive material penetrates the body surface) or internal (when radioactive material is inhaled or ingested).
In all cases, the dose or radiation exposure is determined by the distance from the event, duration of exposure, and mitigation by interspersed shielding. (See Table 8 for a basic summary of commonly used radiation exposure equivalents.) Humans are all exposed to very small quantities of environmental radiation, and many individuals are exposed to small quantities of radiation from industry, health care, research, and defense. Serious exposure, however, can lead to a constellation of injuries which, if not immediately fatal, can lead to a protracted course of illness.
Table 8. Radiation Measurements and Conversions
Radioactivity |
Absorbed Dose |
Dose Equivalent |
Exposure |
|
|
Source: Radiation Emergency Assistance Center/Training Site (REAC/TS). (n.d.). Guidance for Radiation Accident Management: Measurement. Retrieved from http://orise.orau.gov/reacts/guide/measure.htm. |
||||
|
Common Units |
Curie (Ci) |
Rad |
Rem |
Roentgen (R) |
|
SI Units |
Becquerel (Bq) |
Gray (Gy) |
Sievert (Sv) |
Coulomb/kilogram (C/kg) |
|
Conversion Equivalence |
1 Bq = 1 distintegration/sec 1 Ci = 3.7 x 1010 Bq |
1 Gy = 100 rad |
1 Sv = 100 rem |
1 C/kg = 3880 R |
Fifty percent of individuals exposed to 4.5 Gy (4.5 Sv or 4500 rad) to the majority of their body surface will die.50 Those exposed to lower doses will develop various manifestations of radiation sickness, which include hematologic and gastrointestinal syndromes. Gastrointestinal distress is often followed by a latent period with subsequent immune compromise and hemorrhage. Neurovascular symptoms are the result of massive radiation (15-30 Gy), and lead to immediate central nervous system dysfunction and rapid deterioration to coma and death. Local exposure can lead to radiation burns, which are often delayed in their onset and indolent.50
The time of onset of vomiting from exposure provides a rough guide to the severity of radiation exposure. (See Table 9.) External dosimetry of the body and wounds, and dosimetry of the excreta, can predict the level of contamination and direct further decontamination or debridement.
Table 9. Estimation of Radiation Dose Related to Onset of Vomiting
Time to Onset of Vomiting |
Estimated Dose |
|
Notes: Estimates are for a single, acute exposure. The timeframe for symptom onset may vary if dose rate was low. Source: Adapted from Berger ME, Leonard RB, Ricks RC, et al. Hospital Triage in the First 24 Hours after a Nuclear or Radiological Disaster. Oak Ridge: Radiation Emergency Assistance Center/Training Site; 2004. Retrieved from https://orise.orau.gov/files/reacts/triage.pdf. |
|
|
Less than 10 minutes |
> 8 Gy |
|
10-30 minutes |
6-8 Gy |
|
Less than 1 hour |
4-6 Gy |
|
1-2 hours |
2-4 Gy |
|
More than 2 hours after |
< 2 Gy |
The specific management of radiation injury is complex and beyond the scope of this paper. Fortunately, the emergent management is quite basic: decontamination, both external and internal; debridement of radioactive material; and the management of concomitant emergent injuries. Unless there is imbedded, ingested, or inhaled radioactive material, simply removing the victim’s clothing and washing with soap and water will remove 90% of the contamination.33
In the absence of life-threatening injury, patient management should follow decontamination. Uninjured patients without gastrointestinal symptoms (indicating significant exposure) can be managed initially in the ambulatory setting.53 Internal decontamination may be accomplished with gastrointestinal or bronchial lavage, laxatives, and/or debridement. Personal protective equipment (PPE) and personal dosimetry are essential for the provider, although extensive contamination of the medical staff is unlikely. In the Chernobyl incident, for example, medical personnel sustained minimal radiation exposure and no morbidity.54
Decontamination
As with all emergency response, the responder must be appropriately attired in PPE to prevent exposure or injury. The level of PPE is commensurate with the type and risk of exposure. Potential radiation contamination mandates the routine use of personal dosimeters for those providers who care for the patients, clean the rooms, or manage the waste.
Although most contemporary EDs are fitted with decontamination rooms with an isolated entrance and controlled exit to treatment rooms, a mass casualty decontamination is best accomplished outside the ED. Portable trailers, temporary sheds, and outdoor showers can be assembled quickly for use. In central Ohio, local facilities have immediate access to portable decontamination supplies and facilities available on trailers shared by the region.
The University Hospitals of Cleveland have an outdoor decontamination space. The hospital outfitted the parking garage nearest the ED with overhead shower nozzles to allow rapid decontamination en masse in the open air of a controlled space. (See Figures 2A-B.)
Figure 2A. Parking Garage Outfitted with Overhead Grid Containing Shower Heads and Exterior Heaters for Mass Decontamination (University Hospital, Cleveland, OH)

Figure 2B. Detail: Parking Garage Outfitted with Overhead Shower Heads for Mass Decontamination (University Hospital, Cleveland, OH)

Clothing removal and copious water irrigation are usually sufficient for most contaminants. Toxic materials that are ingested or inhaled, such as toxins, radioactive material, and noxious chemicals, may require “internal” decontamination such as lavage, the use of adsorbents or purgatives, or debridement.
Triage
Effective triage is the first step in preventing unnecessary death or disability. Most American fire and EMS agencies utilize the Incident Management System to develop an action plan and establish scene control. A large number of casualties that present in certain incidents will mandate an effective use of limited resources at the scene and in hospital.55-58
The five standard triage categories are usually listed as: immediate, delayed, minimal, expectant, and dead. The immediate category of patients requires immediate but sometimes simple lifesaving measures. The ATLS ABCDE paradigm of trauma evaluation typically applies to this group. They usually get first access to procedures, operating rooms, and critical care units.
The delayed group of patients has emergent injuries, which can wait. Examples of such injuries include closed head injuries with an adequate airway, extremity fractures, soft-tissue injuries, and penetrating torso injuries in a hemodynamically stable patient.
Minimal (also often called “walking wounded” or “walking well”) patients often reach the hospital first because they are not transported by EMS. These patients are not scene triaged, and can quickly use up valuable ED and hospital resources if their care is provided as it might be in a non-mass casualty situation.
The expectant are alive, but not for long. These are the patients with severe head injuries, total body burns, penetrating injuries to the torso with imminent or recent cardiac arrest, and massive radiation exposure. The dead category is self-explanatory. These last two categories require the greatest adjustment from routine care, because they should be given minimal treatment (comfort care) or quickly pronounced dead. Resurgence in ED thoracotomy for penetrating injury59 might tempt the practitioner to go “all-out” on an expectant or recently dead patient, when those resources could be more appropriately expended on a salvageable patient.
Over- and under-triage should be minimized. Typically, over-triage is the problem. The walking wounded are especially problematic in dramatic events. This group can rapidly overwhelm a facility. The most pressing example is the Aum Shinrikyo terrorist release of sarin gas in a crowded Tokyo subway, after which 4460 walking well presented to Tokyo hospitals, overwhelming the health care system.33
The relatively small, but locally overwhelming mass casualty event at Fort Hood in 2014 involved four deaths and 14 wounded. The victims were initially transported to a single Level III Trauma Center located on the base, and triage was simplified to immediate or delayed. One patient with an arm wound and an abdominal injury was inappropriately triaged as delayed (for the arm) when the abdominal injury was overlooked, and subsequently correctly moved to immediate on secondary triage.24
It is not unusual for a facility to receive inaccurate information from the scene or no information at all. This lack of communication is often singled out as a weakness in multiple after action reports. However, it should be anticipated and controlled for with effective hospital triage. The University of Colorado Hospital experience with the 2012 Aurora shooting discussed above is illustrative.
Triage in the hospital setting should be provided by the most experienced clinicians available. Initial interventions after triage should include only lifesaving procedures, and the victims should be moved in one direction to successive hierarchies of care.56 Secondary triage along the line of patient flow is essential, as exemplified in the 2014 Fort Hood shooting. Surgical procedures should be prioritized by urgency and not by indication. The walking wounded may be segregated to a space away from the ED and carefully re-triaged and reassured.
The triage officer(s) should not only understand the clinical consequences of injury, but also the facility’s and region’s resources. This is exemplified by the RIH fire mass casualty response and the Savannah sugar refinery explosion. The ED full of existing patients needs to be triaged and cleared, elective surgery delayed or cancelled, elective admissions delayed or cancelled, intensive care units (ICUs) cleared, and secondary critical care units established. These require the cooperation and participation of a wide range of hospital medical staff and clinicians, and consideration of methods to move stable patients rapidly to facilities that are not directly involved in the major event. This practice is usually undertaken in natural events like tornadoes or hurricanes, but may be necessary in overwhelming man‐made events.
Once the mass casualty event is identified in the community or by the media, volunteer staff begin to arrive to assist with rescue and medical duties. Establishing a staging area to vet these volunteers and assign them to appropriate tasks may be beneficial.
All the surgical and medical specialties may eventually be needed, depending on the type of disaster. Essential emergent clinician resources include Emergency Medicine, General (Trauma) Surgery, and Anesthesia. Even in surgery-heavy disasters (explosions, fire, and mass casualty shooting events), emergency surgery is not common. Critical senior surgical resources should be used for triage and not saved for a potential influx of victims who might require urgent surgery.12
Sub-specialist need varies. For example, in the Oklahoma City bombing, operative resources (in decreasing order of need) included: General Surgery, Ophthalmology, Neurosurgery, and Vascular Surgery.5 Of these, the need for Ophthalmology may not be initially intuitive. However, in the 2001 World Trade Center attack, ocular injury (26%) was the second most common injury in survivors.5 Chemical, biologic, and nuclear attacks rely heavily on the medical specialties. Understanding potential gaps in the facility, medical staff, and other clinical resources is essential to local and regional preparedness.
Preparation
Although it is human nature to ignore the infrequent and unlikely, the multiple examples above and in the literature point to the need of any health care facility to be prepared for a disaster. Multiple published after action reports credit education, planning, training, and drilling with preventing unnecessary morbidity and mortality.58 Preparation should include the elements mandated under the National Incident Management System (NIMS). These include the preparation of Hazardous Vulnerability Analysis (HVA) plans; an Incident Management System (IMS); a Hospital Emergency Incident Command System (HEICS); a clear understanding of local, regional, state, and national resources; education; and simulation training.58
ICS. The Incident Command System was developed as a regional resource in 1970 following devastating wildfires in Southern California, and subsequently developed and distributed as the National Interagency ICS Management System.58 ICS provides a standardized hierarchy, process scaffold, essential operational units, and job assignments necessary to manage a disaster. ICS methodology should be part of any regional disaster plan.
HEICS. The Hospital Emergency Incident Command System, developed in California in 1991,58 translates ICS methodology for hospital response to a disaster. The coordination of terminology and infrastructure between ICS and HEICS allows for a more seamless hospital response and system-wide response. This becomes evident in regional disaster drills and proves essential in a mass casualty disaster.
Resources. Although man-made disasters often stress local facilities, they generally do not exceed regional capacity.5 In the 2001 World Trade Center attack, two affiliated New York City hospitals managed 911 patients. Of those patients, 776 (85%) were walking wounded with mild ocular and inhalational injury, 135 (15%) were admitted, and 18 required surgery.60
Propper and colleagues61 evaluated surge response for three mass casualty situations (civilian blast injuries) in a U.S. military hospital in Iraq. Using their experience, they developed a useful model predicting critical resource utilization. (See Table 10.) In one interesting approach, Hirshberg and colleagues, using computer simulation of casualty load and surge capacity, found that over-triage significantly decreased the ability to effectively care for multiple seriously injured patients.62
Table 10. Guidelines for Requirements in the Areas of Transfusion, Surgical Requirements, and Intensive Care Needs Following Single Explosive Event
Resource |
Guideline |
|
Source: Adapted from: Propper BW, Rasmussen TE, Davidson SB, et al. Surgical response to multiple casualty incidents following single explosive events. Ann Surg 2009;250:311–315. |
|
|
Blood and plasma |
3.5 units of pRBC and plasma per admitted casualty |
|
Operations |
0.75 operations per admitted casualty 3.5 procedures per admitted casualty |
|
Intensive care beds |
0.5 ICU bed per admitted casualty |
|
Mechanical ventilator |
0.5 mechanical ventilator per admitted casualty |
Mass casualty events that do not generally require surgical management, such as chemical, biological, and radiation events, may require resources and expertise exceeding local capability. In this setting, Poison Control Centers, state and local health departments, and federal agencies (CDC) can often provide rapid response (see the discussion of botulism above for an example). Identifying important contacts and resource availability should be part of any hospital disaster plan.
The Radiation Emergency Assistance Center/Training Site (REAC/TS; https://orise.orau.gov/reacts/) in Oak Ridge, TN, can provide guidance, education, and training opportunities. The REAC/TS staff emergency number is 865.576.1005 (ask for REAC/TS).
Education. Disaster management requires training and skills that exceed routine medical care; failure to obtain this training may result in suboptimal outcomes.63 The International Society of Disaster Medicine defines an ideal curriculum.58 There are a number of courses available in the United States: the National Disaster Life Support (NLDS) course from the National Disaster Life Support Foundation (http://www.ndlsf.org/); EMS and Disaster Preparedness from the American College of Emergency Physicians (http://www.acep.org/Content.aspx?id=30194); Disaster Management and Emergency Preparedness (DMEP) course from the American College of Surgeons (https://www.facs.org/quality%20programs/trauma/education/dmep); and a number of postgraduate degree courses on disaster management at universities throughout the United States. International courses are also available from the Red Cross and Red Crescent (https://www.ifrc.org/Global/Documents/Secretariat/201501/DM%20Course%20Brochure.pdf), the World Health Organization (WHO International Diploma Course in Vulnerability Reduction and Emergency Preparedness),64 and the United Nations Office for Disaster Risk Reduction (an Online Certificate Course in Disaster Management, http://www.unisdr.org/we/inform/events/45458).
Simulation Drills. “We fight as we train” is a U.S naval mantra that seems appropriate. The Boston Brigham and Women’s Hospital (BWH) treated 39 survivors of the Boston Marathon bombing. Nine patients required emergent operation for open fractures, devascularized limbs, burns, debridement, and amputation.65 Goralnick and Gates credit simulation and experience for an effective lifesaving response. BWH activated its emergency response team 78 times during the eight years preceding the mass casualty event for both real and simulated disasters.65
A number of other authors have supported the belief that simulation training may be lifesaving. For example, Feliciano and colleagues attributed some of the excellent outcomes of the 1996 Centennial Olympic Park bombing in Atlanta to preparedness.58,66 Mahoney and colleagues thought that disaster drills were invaluable in preparation for the RIH response to an unexpected Rhode Island nightclub fire and subsequent mass casualty situation.12
Lessons Learned
- Scene triage is often hectic, despite careful planning, multiple protocols, and frequent disaster drills. The enormity of these events and the multitude of different responders often lead to confusion early on.
- Notification is unusual. The often chaotic scene leads to infrequent communication with the receiving facilities; coupled with perceived urgency at the scene, this often leads to zero-notice events.
- Transportation is often by non-traditional means. The seriously injured may be simply scooped and transported by local police, and the “walking wounded” will often find their own way to the hospital ED.
- The type of disaster will help to define mechanisms of injury. Understanding the common patterns of injury based on the incident can help a facility allocate resources early in the process.
- Competent hospital triage is essential.
- Resource utilization usually does not exceed local capacity. Despite scene chaos, multiple casualties, and zero notification, most disaster response after action evaluations do not identify resource utilization as a constraint. One exception is the event typified by the Tokyo sarin attack, in which the “worried well” initially overwhelmed hospital resources.
- Preparation helps. A number of after action reports have credited disaster planning and drills with saving lives. These are essential components for any hospital or ED. In an emergency, the nearest facility will receive patients regardless of the available resources.
REFERENCES
- United States. Executive Office of the President. (2006). The Federal Response to Hurricane Katrina: Lessons Learned. Washington, DC: Government Printing Office. Retrieved from http://permanent.access.gpo.gov/lps67263/katrina-lessons-learned.pdf.
- BBC News. (Aug. 13, 2015). China blasts: Tianjin port city rocked by explosions. BBC News. Retrieved from http://www.bbc.com/news/world-asia-china-33896292.
- 2015 Tianjin explosions. (Sept. 2, 2015). In Wikipedia. Retrieved from https://en.wikipedia.org/w/index.php?title=2015_Tianjin_explosions.
- Durso F. In West’s Wake. NFPA Journal March-April 2014. Retrieved from http://www.nfpa.org/newsandpublications/nfpa-journal/2014/march-april-2014/features/nfpa-400.
- Falcone RE. Civilian blast injury. Trauma Reports 2013;14(5):1–11.
- United States Department of State, Bureau of Counterterrorism. Country Reports on Terrorism 2014. Washington, DC: United States Department of State. Retrieved from http://www.state.gov/documents/organization/239631.pdf.
- Okpala N. Management of blast ear injuries in mass casualty environments. Mil Med 2011;176:1306–1310.
- Radford P, Patel HDL, Hamilton N, et al. Tympanic membrane rupture in the survivors of the July 7, 2005, London bombings. Otolaryngol Head Neck Surg 2011;145:806–812.
- Peters P. Primary blast injury: An intact tympanic membrane does not indicate the lack of a pulmonary blast injury. Mil Med 2011;176:110–114.
- Masellis M, Ferrara MM, Gunn SWA. Fire disaster and burn disaster: Planning and management. Ann Burns Fire Disasters 1999;12:67-76.
- Rosenberg B, Sternberg N, Zagher U, et al. Burns due to terroristic attacks on civilian populations from 1975 to 1979. Burns 1982;9:21–23.
- Mahoney EJ, Harrington DT, Biffl WL, et al. Lessons learned from a nightclub fire: Institutional disaster preparedness. em>J Trauma-Injury Infection 2005;58:487–491.
- Joseph M. Still Burn Center. Battling Big Burns: The Imperial Sugar Company Fire. Burn Care Commentary 4 (Summer 2008). Retrieved from http://doctors-hospital.net/util/documents/commentarysummer08.pdf.
- Buerk CA, Batdorf JW, Cammack KV, et al. The MGM Grand Hotel Fire: Lessons learned from a major disaster. Arch Surg 1982;117:641–644.
- Harding PJ, Amos M, Gwynne S. (2010). Prediction and mitigation of crush conditions in emergency evacuations. In: Klingsch WWF, Rogsch C, Schadschneider A, et al, eds. Pedestrian and Evacuation Dynamics. Springer Berlin Heidelberg; 2008:233-246. Retrieved from http://link.springer.com/chapter/10.1007/978-3-642-04504-2_18.
- Bittenbender S. Cincinnati marks 35th anniversary of Who concert tragedy. Reuters. Dec. 4, 2014. Retrieved from http://www.reuters.com/article/2014/12/04/us-usa-ohio-thewho-idUSKCN0JI0AS20141204.
- Wilgoren J. (Feb. 18, 2003). 21 die in stampede of 1,500 at Chicago nightclub. The New York Times. Feb. 18, 2003. Retrieved from http://www.nytimes.com/2003/02/18/us/21-die-in-stampede-of-1500-at-chicago-nightclub.html.
- Bjelopera JP, Bagalman E, Caldwell SW, et al. Public Mass Shootings in the United States: Selected Implications for Federal Public Health and Safety Policy (No. R43004). Washington, DC: Library of Congress Congressional Research Service. March 18, 2013. Retrieved from http://journalistsresource.org/wp-content/uploads/2013/03/MassShootings_CongResServ.pdf.
- Sedensky SJ. Report of the State’s Attorney for the Judicial District of Danbury on the Shootings at Sandy Hook Elementary School and 36 Yogananda Street, Newtown, Connecticut on December 14, 2012. Rocky Hill: State of Connecticut Division of Criminal Justice. Retrieved from http://www.ct.gov/csao/lib/csao/Sandy_Hook_Final_Report.pdf.
- 2012 Aurora shooting. In: Wikipedia. Retrieved from https://en.wikipedia.org/w/index.php?title=2012_Aurora_shooting. Accessed Aug. 30, 2015.
- Amended Complaint. Phillips v. Lucky Gunner, No. 2014CV031946 (District Court, Arapahoe County, Colorado Sept. 16, 2014). Retrieved from http://media.thedenverchannel.com/documents/brady%20center%20ammo%20seller%20lawsuit.pdf.
- TriData Division, System Planning Corporation. Aurora Century 16 Theater Shooting: After Action Report for the City of Aurora. Arlington: TriData Division, System Planning Corporation. 2014. Retrieved from https://www.courts.state.co.us/Media/Opinion_Docs/14CV31595%20After%20Action%20Review%20Report%20Redacted.pdf.
- Pittman E. One hospital’s incredible response to the Aurora, Colo., shooting. Emergency Management. Sept. 21, 2012. Retrieved from http://www.emergencymgmt.com/safety/One-Hospitals-Incredible-Response-to-the-Aurora-Colo-Mass-Shooting.html.
- Strommen JJ, Waterman SM, Mitchell CA, et al. 2014 Fort Hood, Texas, mass casualty incident: Reviews and perspectives. Curr Rev Musculoskel Med 2015;8:298–303.
- Jacobs LM, McSwain NE, Rotondo MF, et al. Improving survival from active shooter events: The Hartford Consensus. J Trauma Acute Care Surg 2013;74:1399–1400.
- Schroll R, Smith A, McSwain NE, et al. A multi-institutional analysis of prehospital tourniquet use. J Trauma Acute Care Surg 2015;79:10–14.
- Holcomb JB, Helling TS, Hirshberg A. Military, civilian, and rural application of the damage control philosophy. Mil Med 2001;166:490–493.
- Stanton T. Trained for trauma: Philadelphia hospitals were well prepared for the mass casualties of an Amtrak crash. AAOS Now. Retrieved from http://aaos.org/news/aaosnow/jul15/youraaos2.asp. July 2015.
- Hampton T. Disaster training, capacity for quality trauma care key to aiding injured in Asiana Airlines crash. JAMA 2013;310:467–467.
- US Airways Flight 1549. (2015, August 31). In Wikipedia. Retrieved from https://en.wikipedia.org/w/index.php?title=US_Airways_Flight_1549.
- Schecter WP, Fry DE. The surgeon and acts of civilian terrorism: Chemical agents. J Am Coll Surgeons 2005;200:128–135.
- Abdelaziz S, Gorani H, Bickford A. U.N. confirms use of chemical weapons in Syria. CNN. Dec. 12, 2013. Retrieved from http://www.cnn.com/2013/12/12/world/meast/syria-civil-war/index.html.
- Ciraulo DL, Barie PS, Briggs SM, et al. An update on the surgeons scope and depth of practice to all hazards emergency response. J Trauma 2006;60:1267–1274.
- Buckley RL, Hunter CH, Addis RP, et al. Modeling dispersion from toxic gas released after a train collision in Graniteville, SC. J Air & Waste Management Assoc 2007;57:268–278.
- Cave D, Fadam A. Iraq insurgents employ chlorine in bomb attacks. The New York Times. Feb. 22, 2007. Retrieved from http://www.nytimes.com/2007/02/22/world/middleeast/22iraq.html.
- Organisation for the Prohibition of Chemical Weapons. Convention on the Prohibition of the Development, Production, Stockpiling, and Use of Chemical Weapons and on Their Destruction. Organisation for the Prohibition of Chemical Weapons. July 29, 2005. Retrieved from https://www.opcw.org/fileadmin/OPCW/CWC/CWC_en.pdf.
- Arms Control Association. Chemical and Biological Weapons Status at a Glance. Washington, DC: Arms Control Association. 2014. Retrieved from https://www.armscontrol.org/printpdf/2473.
- Suzuki T, Morita H, Ono K, et al. Sarin poisoning in Tokyo subway. Lancet 1995;345:980–981.
- Woolf J. Feds finally admit that nerve agent was found near 1968 sheep kill. Salt Lake Tribune. Jan. 2, 1998. Retrieved from http://pages.suddenlink.net/anomalousimages/images/news/news154.html.
- Cole LA. Clouds of Secrecy: The Army’s Germ Warfare Tests Over Populated Areas. Lanham: Rowman & Littlefield Publishers; 1988.
- United States Department of Justice. (2010). Amerithrax Investigative Summary: Released Pursuant to the Freedom of Information Act. Washington, DC: United States Department of Justice. Retrieved from http://www.justice.gov/archive/amerithrax/docs/amx-investigative-summary.pdf.
- Snyder L, Pate J. Research Story of the Week: Tracking Anthrax Hoaxes and Attacks. May 20, 2002. Retrieved from http://cns.miis.edu/stories/020520.htm.
- Ohio Department of Health. Homeland Security Exercise and Evaluation Program (HSEEP): 2015 Botulism Outbreak Response. Received via personal communication.
- Fry DE, Schecter WP, Parker JS, et al. (2005). The surgeon and acts of civilian terrorism: Biologic agents. J Am Coll Surgeons 2005;200:291–302.
- Ricks RC, Berger ME, Holloway EC, et al. REAC/TS Radiation Accident Registry: Update of Accidents in the United States. Oak Ridge: Oak Ridge Institute for Science and Education. 2000. Retrieved from http://www.irpa.net/irpa10/cdrom/00325.pdf.
- Wall A. (n.d.). Top 10 Nuclear Disasters. Retrieved from http://www.processindustryforum.com/hottopics/nucleardisasters.
- United Nations Scientific Committee on the Effects of Atomic Radiation. The Chernobyl accident: UNSCEAR’s assessments of the radiation effects. July 16, 2012. Retrieved from http://www.unscear.org/unscear/en/chernobyl.html.
- Graham A. Nuclear Terrorism Fact Sheet (Policy Memo). Cambridge: Belfer Center for Science and International Affairs, Harvard Kennedy School. 2010. Retrieved from http://belfercenter.ksg.harvard.edu/files/Nuclear-Security-Fact-Sheet.pdf.
- Tobey WH, Zolotarev P. (2014, January). The Nuclear Terrorism Threat. Presented at the Meeting of the 2014 Nuclear Security Summit Sherpas, Hosted by the Thai Ministry of Foreign Affairs, Pattaya, Thailand. Retrieved from http://belfercenter.ksg.harvard.edu/files/nuclearterrorismthreatthailand2014.pdf.
- Chambers JA, Purdue GF. Radiation injury and the surgeon. J Am Coll Surgeons 2007;204:128–139.
- Henken RE, Wagner RH. (n.d.). Physician and Hospital Responses to Radiological Incidents. Loyola University, Section on Nuclear Medicine/Department of Radiology, Maywood, Illinois. Retrieved from http://www.meddean.luc.edu/lumen/MedEd/Radio/curriculum/IPM/LUM%20RAD%20Accident.ppt.
- AJ Software & Multimedia. (n.d.). The Atomic Bombings of Hiroshima and Nagasaki: Total Casualties. Retrieved from http://www.atomicarchive.com/Docs/MED/med_chp10.shtml.
- Berger ME, Leonard RB, Ricks RC, et al. Hospital Triage in the First 24 Hours after a Nuclear or Radiological Disaster. Oak Ridge: Radiation Emergency Assistance Center/Training Site. 2004. Retrieved from https://orise.orau.gov/files/reacts/triage.pdf.
- Mettler FA, Voelz GL. Major radiation exposure — What to expect and how to respond. N Engl J Med 2002;346:1554–1561.
- Frykberg ER. Principles of mass casualty management following terrorist disasters. Ann Surgery 2004;239:319–321.
- Frykberg ER. Triage: Principles and practice. Scand J Surg 2005;94:272–278.
- Einav S, Spira RM, Hersch M, et al. (Surgeon and hospital leadership during terrorist-related multiple-casualty events: A coup d’état. Arch Surg 2006;141: 815–822.
- O’Neill PA. The ABCs of disaster response. Scand J Surg 2005;94:259–266.
- Seamon MJ, Haut ER, Van Arendonk K, et al. An evidence-based approach to patient selection for emergency department thoracotomy: A practice management guideline from the Eastern Association for the Surgery of Trauma. J Trauma Acute Care Surg 2015;79:159–173.
- Cushman JG, Pachter HL, Beaton HL. Two New York City hospitals’ surgical response to the September 11, 2001, terrorist attack in New York City. J Trauma: Injury, Infection, Crit Care 2003;54:147–155.
- Propper BW, Rasmussen TE, Davidson SB, et al. Surgical response to multiple casualty incidents following single explosive events. Ann Surg 2009;250:311–315.
- Hirshberg A, Scott BG, Granchi T, et al. How does casualty load affect trauma care in urban bombing incidents? A quantitative analysis. J Trauma: Injury, Infection, Crit Care 2005;58:686–695.
- Lennquist S. Education and training in disaster medicine. Scand J Surg 2005;94:300–310.
- Dubouloz M. WHO International Diploma Course in Vulnerability Reduction and Emergency Preparedness. Int J Disaster Med 2003;1:21–24.
- Goralnick E, Gates J. We fight like we train. N Engl J Med 2013;368:1960–1961.
- Feliciano D, Anderson Jr. G, Rozycki G, et al. Management of casualties from the bombing at the Centennial Olympics. Am J Surg 1998;176:538–543.
Man-made disaster directly impacts the emergency department and hospital when a mass casualty situation ensues, and is the focus of this review article. Using contemporary examples and the current literature, what follows is a primer on the causes, injury patterns, resource utilization, triage, and preparation for man-made mass casualty events.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
