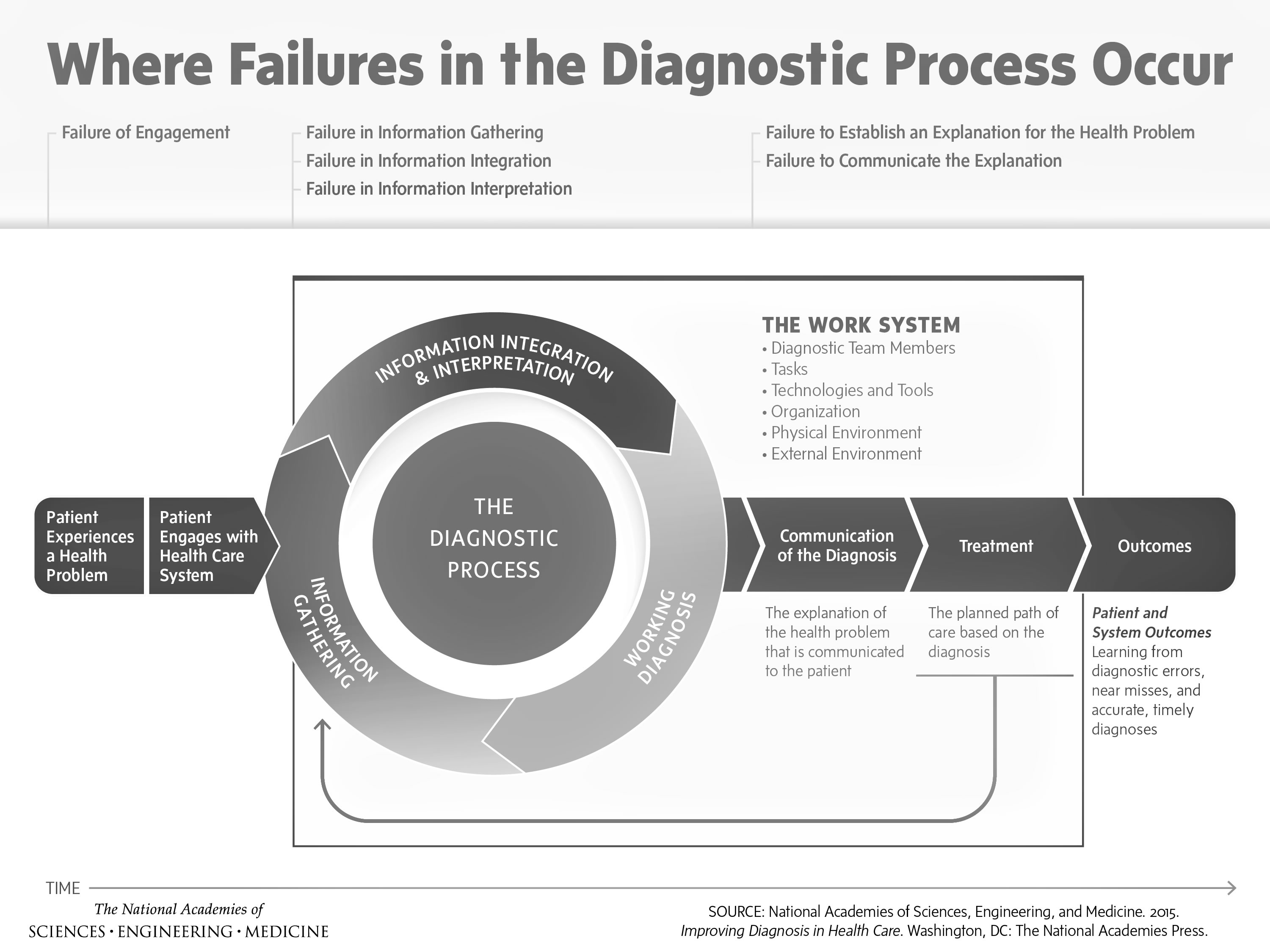
This is an excerpt from the Institute of Medicine’s Report of the Committee on Diagnostic Error in Health Care:
The delivery of healthcare has proceeded for decades with a blind spot: Diagnostic errors—inaccurate or delayed diagnoses—persist throughout all settings of care and continue to harm an unacceptable number of patients. For example:
- A conservative estimate found that 5% of U.S. adults who seek outpatient care each year experience a diagnostic error.
- Postmortem examination research spanning decades has shown that diagnostic errors contribute to approximately 10% of patient deaths.
- Medical record reviews suggest that diagnostic errors account for six to 17% of hospital adverse events.
- Diagnostic errors are the leading type of paid medical malpractice claims, are almost twice as likely to have resulted in the patient’s death compared to other claims, and represent the highest proportion of total payments.
In reviewing the evidence, the committee concluded that most people will experience at least one diagnostic error in their lifetime, sometimes with devastating consequences. Despite the pervasiveness of diagnostic errors and the risk for serious patient harm, diagnostic errors have been largely unappreciated within the quality and patient safety movements in healthcare. Without a dedicated focus on improving diagnosis, these errors will likely worsen as the delivery of healthcare and the diagnostic process continue to increase in complexity.
Getting the right diagnosis is a key aspect of healthcare — it provides an explanation of a patient’s health problem and informs subsequent healthcare decisions. Diagnostic errors stem from a wide variety of causes, including: inadequate collaboration and communication among clinicians, patients, and their families;1 a healthcare work system that is not well designed to support the diagnostic process; limited feedback to clinicians about diagnostic performance; and a culture that discourages transparency and disclosure of diagnostic errors — impeding attempts to learn from these events and improve diagnosis. Diagnostic errors may result in different outcomes, and as evidence accrues, these outcomes will be better characterized. For example, if there is a diagnostic error, a patient may or may not experience harm. Errors can be harmful because they can prevent or delay appropriate treatment, lead to unnecessary or harmful treatment, or result in psychological or financial repercussions. Harm may not result, for example, if a patient’s symptoms resolve even with an incorrect diagnosis.
Improving the diagnostic process is not only possible, but it also represents a moral, professional, and public health imperative. Achieving that goal will require a significant re-envisioning of the diagnostic process and a widespread commitment to change among healthcare professionals, healthcare organizations, patients and their families, researchers, and policymakers.