The Vomiting Patient in the ED: Evaluation and Management
The Vomiting Patient in the ED: Evaluation and Management
Authors: Michael C. Plewa, MD, Research Director, Saint Vincent Mercy Medical Center, Emergency Medicine Residency, Toledo, OH; Robert Young, DO, Resident, St. Vincent Mercy Medical Center, Emergency Medicine Residency, Toledo, OH; and Joseph Perkins, DO, Resident, St. Vincent Mercy Medical Center, Emergency Medicine Residency, Toledo, OH.
Peer Reviewer: Bryce Yerman, MD, Department of Emergency Medicine, University of Rochester, NY.
Note: *All medication uses discussed in this paper are considered off-label by the FDA except: prochlorperazine and perphenazine for severe nausea and vomiting; thiethylperazine and chlorpromazine for nausea and vomiting; trimethobenzamide for nausea with gastroenteritis; promethazine, scopolamine, cyclizine, dimenhydrinate, diphenhydramine, and meclizine for motion sickness; lidocaine for topical anesthesia of mucous membranes.
It's always the little things, right? What do patients remember when discharged from the emergency department? It's the little things, like did the gurney have a pillow, was the bedrail clean, did the nurse who drew my blood leave a bruise? Often, it's not the big things, like was the right diagnosis made, and was the correct treatment provided. For patients who come to the emergency department miserable from vomiting, it is did we take away the symptoms and make them feel better? Because of the frequency of this symptom in emergency department patients, you would expect there to be an evidence-based approach to assessment and management. Unfortunately, the diagnostic possibilities for vomiting are so vast, it is difficult to develop a consensus approach that incorporates all the aspects that an experienced clinician considers when evaluating and treating a specific patient. Likewise, it is impossible to cover all aspects in a review article. Purposefully, this article was designed to highlight important aspects of treatment, especially the benefits and risk of antiemetic use. I hope you find new and useful ideas here that you can incorporate into your practice.
J. Stephan Stapczynski, MD, Editor
Introduction
Few sounds or smells in the emergency department (ED) get our attention as easily as vomiting. In response, we might reflexively order our "one-size-fits-all" standard antiemetic and begin by assuming that this is probably just another case of "gastroenteritis." There are, however, several antiemetics to choose from, each with its own advantages and disadvantages, as well as a myriad of diagnostic possibilities to consider. (See Table 1.) In evaluating and treating the vomiting patient, the emergency physician should discern the correct diagnosis from the multitude of potential causes, exclude the serious and potentially life-threatening conditions (see Table 2), identify potential complications of persistent or severe vomiting, assess and treat dehydration, and carefully consider therapeutic options of nasogastric (NG) suctioning, intravenous (IV) hydration, and antiemetic medication.
 |
 |
Pathophysiology
There are three basic phases of vomiting. Nausea is the unpleasant sensation that immediately precedes vomiting, and is typically associated with hypersalivation and tachycardia. Retching, the second phase, occurs when the pylorus contracts while the fundus relaxes, allowing contents to move toward the gastric cardia. Finally, emesis occurs with the forceful contraction of the abdominal muscles and relaxation of the lower esophageal sphincter, causing retrograde movement of the gastric contents from the stomach out the mouth. In contrast, regurgitation is the involuntary return of esophageal contents to the hypopharynx without preceding nausea and little abdominal muscular effort.
The numerous signals necessary to coordinate the act of vomiting are processed by several brainstem nuclei in the reticular formation of the medulla and pons, together called the emesis center, which receives input from the chemoreceptor trigger zone (CTZ) of the area postrema of the fourth ventricle, the autonomic afferent nerves (especially the vagus) from the gastrointestinal tract, the labyrinthine system, and the cerebral cortex (vision, smell, taste).
Vomiting is a potentially protective mechanism, emptying the stomach to eliminate toxins, and decrease volume and minimize luminal pressures in obstructions. When persistent or severe, however, vomiting can become more than a nuisance and can lead to various complications. (See Table 3.)
 |
Clinical Approach to the Vomiting Patient
History. There are five aspects to the history that help narrow the differential from the long list of causes (see Table 1): age, duration, frequency and timing, characteristics of the vomitus, and associated symptoms.
Bilious vomiting in a neonate is an ominous sign and should prompt an evaluation with contrast (barium) swallow radiographs to evaluate for malrotation with or without volvulus, intestinal atresia or intestinal stenosis. Nonbilious vomiting in a neonate could indicate hypertrophic pyloric stenosis (HPS), intestinal atresia, or an obstructing lesion (web, band) proximal to the ampulla of Vater. In early infancy, inborn errors of metabolism can manifest with vomiting, seizures, hypotonia or hypertonia, and lethargy or coma. Metabolic acidosis, ketosis, elevated ammonia or hypoglycemia may be clues to these disorders of carbohydrate metabolism (such as glycogen storage), amino acid or organic acid defects (such as phenylketonuria), lysosomal storage, peroxisomes, or fatty acid oxidation. Food sensitivity is common, affecting up to 3-5% of bottle-fed infants.1 Infants and small children are most likely to have simple gastroenteritis, otitis, urinary tract infection or pharyngitis, but are also at risk for intussusception. Adolescents with vomiting might have appendicitis, and young women should be suspected of pregnancy or pyelonephritis. In contrast, the elderly are more likely to have mesenteric infarction, cancer, volvulus, Addison's disease, Ménière's disease, glaucoma, subdural hematoma, or uremia.
Symptom duration is helpful because the differential diagnoses differ significantly for acute and chronic symptoms. Acute vomiting (less than one month in duration) tends to be more worrisome and is more frequently seen in the ED. Chronic vomiting occurs over a period greater than one month and is usually less common. Rapidity of symptom onset is also helpful. An abrupt onset of nausea and vomiting might suggest gastroenteritis, pancreatitis, cholecystitis, food poisoning, or a drug-related side-effect. A more insidious onset is suggestive of reflux, gastroparesis, medications, metabolic disorders, or pregnancy.
Timing and frequency is also of particular importance. The vomiting may be directly associated with meals or may occur continuously, either irregularly or at predictable times. Think of an ingested bacterial toxin for acute vomiting 2-6 hours after eating, as seen with Staphylococcus aureus or Bacillus cereus. Vomiting that is precipitated by meals suggests psychogenic vomiting, pyloric channel ulcer, gastritis, biliary disease, or pancreatitis. Chronic vomiting within one hour of ingestion is consistent with gastric or proximal small bowel obstruction, which can include peptic ulcer, neoplasm, and, less commonly, superior mesenteric artery syndrome or gastric volvulus. If the onset is delayed greater than one hour after eating, gastroparesis and distal bowel obstruction should be of concern. Vomiting that occurs in the early morning upon awakening points toward alcoholic binge, early pregnancy, increased intracranial pressure (ICP), or metabolic disturbances such as uremia or Addison's disease. If a psychological reason is suspected, conversion disorders tend to present with continuous vomiting, while vomiting associated with major depression tend to present with either habitual postprandial or irregular vomiting. A psychological etiology should be a diagnosis of exclusion in the patient with chronic unexplained vomiting only after thorough work-up, and usually is not made by the emergency physician.
The character of the vomitus is the fourth key portion of the history. Is the vomitus bloody, bilious, nonbilious, feculant, or projectile? Hematemesis or coffee ground emesis is suggestive of peptic ulcer disease, Mallory-Weiss tear, esophageal varices, or malignancy. Regurgitation of undigested food is suggestive of esophageal disorders such as achalasia, esophageal stricture, bolus impaction, hiatal hernia, or Zenker's diverticulum. Non-bilious emesis and partially digested food signifies gastritis, gastroparesis, or gastric outlet obstruction as seen in patients with pyloric strictures secondary to peptic ulcer disease (PUD) and infants with HPS. Bilious vomiting, on the other hand, excludes gastric outlet obstruction and can signify small bowel obstruction. Feculant vomiting reflects bacterial degradation of stagnant intestinal contents and is associated with distal small or large bowel obstruction. This can also be seen with blind-loop syndrome. Projectile vomiting is associated with disorders that increase ICP such as malignancy, hemorrhage, meningitis, or hydrocephalus.
Finally, ask about associated symptoms. Essential historical points include associated fever, abdominal pain, jaundice, weight loss, prior surgery, diabetes, chest pain, and neurological symptoms. Fever is suggestive of an infectious etiology. In febrile infants, the presence of vomiting is a nonspecific finding and may be associated with sepsis, meningitis, pneumonia, pharyngitis, otitis media, urinary tract infection, or appendicitis. Associated diarrhea, crampy abdominal pain, and fever suggest gastroenteritis. Vomiting with pain is more likely to be an organic cause. Although there is a large overlap in pain syndromes, a precise description of associated pain may help localize the underlying process. Severe abdominal pain that is colicky in nature and temporarily improves after vomiting points toward small bowel obstruction, while pain associated with cholecystitis (in the right upper quadrant, colicky, radiating to the right flank) and pancreatitis (constant burning epigastric pain radiating into the back) is unaffected by vomiting. Pelvic or groin pain might suggest ovarian torsion, testicular torsion, incarcerated hernia, or ureterolithiasis. Early satiety and postprandial bloating with epigastric pain are associated with gastroparesis and gastritis. Abdominal distention is suggestive of bowel obstruction or volvulus.
The presence of neurological symptoms such as headache, vertigo, stiff neck, or focal neurological deficits suggests a central or intracranial cause of vomiting. Brainstem tumors are frequently associated with vomiting and are usually accompanied by cranial neuropathies. If vertigo (the illusion of movement) is the only associated neurological symptom, suspect a labyrinthine cause; however, be sure to consider more serious intracranial lesions or cerebellar stroke. If headache is the only associated symptom, migraine may be the most likely cause, but think also of subarachnoid hemorrhage, meningitis, cyclic vomiting syndrome, and causes of increased ICP. Focal neurologic deficits suggest central nervous system (CNS) tumors, stroke, hydrocephalus, and brain abscess.
Chest pain with vomiting is classic for acute coronary syndrome or myocardial infarction. When vomiting after fish ingestion is coupled with itching, hives, or wheezing, think of Scombroid poisoning, and with paresthesias and hot-cold reversal think of Cigateura poisoning. In the pregnant woman with hyperemesis, consider molar or twin gestation, hyperthyroidism, pyelonephritis, as well as intra-abdominal disorders.
Physical Examination. The physical examination in patients with vomiting initially should focus on signs of dehydration such as poor skin turgor, dry mucous membranes, tachycardia, orthostasis, and hypotension. The general examination should assess vital signs, mental status, presence of jaundice or lymphadenopathy, and features of thyrotoxicosis. Check stool for occult blood, which suggests mucosal injury from ulcer, ischemia, inflammatory process, or malignancy. Auscultate the lungs for signs of aspiration. Examine the hands for dorsal calluses suggestive of self-induced vomiting. Other findings consistent with bulimia include lanugo, parotid enlargement, and loss of tooth enamel. Bronze skin, loss of axillary hair, and diminished temperature, pulse, and blood pressure are suggestive of Addison's disease.
Inspect the abdomen for distention, visible peristalsis (a rare if virtually diagnostic finding of bowel obstruction), hernias, and scars from previous surgeries. Palpate the abdomen to localize tenderness, identify masses (such as the firm, ovoid epigastic "olive" of HPS) and hernias. Tenderness in the right upper quadrant suggests biliary or hepatic disease; in the midepigastrium, pancreatitis or peptic ulcer; and in the right lower quadrant, appendicitis. Costoverterbral angle tenderness should point toward a primary renal source such as pyelonephritis or stone. Auscultate the abdomen for increased or high-pitched bowel sounds in obstruction, absent bowel sounds in an ileus, and a succession splash over the epigastrium upon abrupt lateral movement or palpation in gastroparesis or pyloric obstruction.
Finally, a neurological examination should be done to exclude CNS etiologies. Observe speech, cranial nerves, balance, gait, coordination, and strength. Look for nystagmus and consider the Dix-Hallpyke test when evaluating vertigo. Check for neck stiffness to rule out meningitis and inspect the fundi for papilledema suggestive of increased ICP.
Diagnostic Testing. There are evidence-based consensus guidelines for the prevention and management of postoperative and chemotherapy-induced nausea and vomiting, but there is no similar guideline for the undifferentiated patient presenting to the emergency department with nausea and vomiting. Thus, recommendations for the use of laboratory studies and further testing cannot be firm and should be guided by history, physical examination, and clinical experience. Although electrolytes are usually unnecessary for the majority of cases, prolonged or severe vomiting can produce hypernatremia and/or hypochloremic metabolic alkalosis. In addition, severe diarrhea can produce a metabolic acidosis with low serum bicarbonate. Consider measuring serum calcium in patients with known cancer or weakness, especially in the elderly. Measure glucose to exclude hypoglycemia in lethargic cases, especially children and the elderly. Low glucose and sodium with elevated potassium might indicate Addison's crisis. An elevated blood urea nitrogen (BUN) to creatinine ratio is suggestive of dehydration, but can also be a clue to occult gastrointestinal bleeding. A complete blood count is not always necessary, yet might reveal anemia in those with bleeding or leukocytosis with an infectious process. Consider serum liver enzyme and lipase measurement in cases with upper abdominal pain and tenderness, or possible acetaminophen or mushroom ingestion, and serum ammonia in suspected hepatic failure or end-stage Reye's syndrome. Urinalysis is useful to screen for blood, white cells, bacteria, ketones, and elevated specific gravity. Serum may be better than urine pregnancy testing when considering ectopic pregnancy or radiographic imaging. Other laboratory tests to consider include blood alcohol, urine drug screen, serum levels of digoxin, theophylline or acetaminophen in overdose situations, and thyroid stimulating hormone in suspected thyrotoxicosis.
Stool cultures should be obtained for cases of possible dysentery, presenting with fever, diarrhea, and blood in stool, and consider ova and parasite testing looking for Giardia in children attending daycare.
An electrocardiogram (ECG) is essential in vomiting patients with chest pain, and even those without chest pain but risk factors for acute coronary syndrome, as well as a screen for QT prolongation if certain antiemetics are to be used (see below).
Bedside ultrasound can be useful in identifying ascites, gallstones, cholecystitis (with gallbladder wall thickening, pericholecystic fluid, and dilation of the common bile duct), and hydronephrosis.
Acute abdominal series radiographs can identify perforation and obstruction, although a significant number of cases will not have diagnotic findings on initial films if the perforation is small or the obstruction is early in its time course. Abdominal computerized tomography (CT) is especially useful in evaluation of vomiting with abdominal pain in the elderly, appendicitis, possible necrotizing pancreatitis, mesenteric infarction and small bowel obstruction and should be considered in cases with persistent abdominal pain or tenderness of uncertain etiology.
Head CT is indicated in vomiting patients with history of ventriculoperitoneal shunt or head injury, especially in the elderly, alcoholics and those anticoagulated, and those suspected of subarachnoid hemorrhage, intracranial hypertension, or mass. One bedside test for increased ICP is the use of the bedside vascular ultrasound probe placed over the eye to identify swelling of the optic nerve sheath. An optic nerve sheath diameter greater than 5 mm, measured 3 mm behind the globe, correlates with an ICP > 20 cm water.2
When evaluating an infant for possible HPS, consider insertion of an 8 F feeding tube to measure gastric aspirate volume. In one study, the aspiration of greater than 5 mL of fluid had a 91% sensitivity (95% CI 70 to 98%) and an 88% specificity (95% CI 77 to 94%) for HPS.3 These authors calculated the most cost- and time-effective algorithm for HPS evaluation was to perform ultrasound in infants with NG aspirates greater than or equal to 5 mL and upper gastrointestinal series (UGI) in those with less than 5 mL.3 Ultrasound diagnostic criteria for HPS include muscle wall thickness of at least 4 mm, a diameter of at least 13 mm, and/or a pyloric length of at least 17 mm.
When considering possible intussusception, accurate diagnosis (and treatment) involves an air or barium enema following IV hydration and sedation. Ultrasonography is also diagnostic, and less expensive than air or barium enema, though not therapeutic. Few cases require surgical decompression when air enema is ineffective.
Complications of Vomiting
Dehydration. Dehydration can vary from mild to life-threatening, and is more prevalent in the very young and very old, especially with concomitant diarrhea. An adult with dehydration may present with weakness, fatigue, dizziness, altered mentation, or falling. For children, mild dehydration (< 3%) can occur without overt physical findings, and easily may be missed, whereas moderate dehydration (3-9%) is easily overestimated, but can manifest with tachycardia, diminished tears, dry mouth, delayed skin fold recoil (but < 2 seconds), slight delay in capillary refill, cool extremities, and decreased urine output.4 Altered mental status (lethargy, apathy, or unconsciousness), marked tachycardia (or even bradycardia when severe), thready pulses, sunken eyes, absent tears, delayed skin fold recoil (> 2 seconds), skin changes (such as minimal capillary refill, cool, mottled, or cyanotic extremities), and minimal urine output4 suggest severe dehydration (> 9%) and can lead to circulatory collapse when > 15%. The presumably most accurate method of assessing level of dehydration is by comparing the present to previous weight on the same scale, although this information is rarely available.
Boerhaave's Syndrome. Boerhaave's syndrome is a spontaneous full-thickness rupture of the esophagus classically described as a sudden onset of severe chest, upper abdominal, or back pain following forceful or repetitive vomiting, but may also occur prior to vomiting in 14% of cases or without vomiting (but with coughing, straining) in another 14%.5 The Meckler's triad of pain, vomiting, and subcutaneous emphysema is seen in about half of cases, and Hamman's crunch may be present in 20%. Chest radiography is abnormal in 70-90% with widened mediastinum, pneumomediastinum, atelectasis, or infiltrate and pleural effusion, and occasionally pneumoperitoneum. Water soluble (Gastrografin) swallowing studies (esophogram or CT scan) are diagnostic. Endoscopy may be falsely negative. Complications can include mediastinitis, sepsis, pneumonia, empyema, persistent esophageal leak, and death. The mortality rate of 50% is related to delayed diagnosis.
Mallory Weiss Syndrome. Upper gastrointestinal bleeding associated with vomiting may be related to the Mallory-Weiss lesion, a linear tear in the mucosa of the esophagogastric junction. Although this lesion classically follows an episode of forceful vomiting, the lesion may be unrelated to vomiting and associated with regurgitation, increased abdominal pressure, or Valsalva maneuver, and is associated with alcohol consumption and portal hypertension. Although considered benign and self-limited, this syndrome may result in recurrent bleeding in 10%, necessitate transfusion in 25%, require therapeutic endoscopy or surgery in 10%, and result in death in 10% of cases.6 Because of the possibility of morbidity and mortality, gastroenterologist consultation is recommended.
Treatment of Vomiting
Enteral Rehydration. Consider oral rehydration with clear liquids containing sugar and electrolytes as the first option in most cases of vomiting that are mild, early, or resolving. In children with gastroenteritis with mild to moderate dehydration, consider oral rehydration when bowel sounds are present and there are no signs of obstruction, protracted vomiting, or other need for IV placement. Enteral hydration is safer and less expensive than IV hydration.7 Because of thirst, patients may attempt drinking large volumes of fluids, which can precipitate further vomiting. Drinking small amounts at a time may minimize this effect, such as starting with 5 mL of electrolyte solution (such as Pedialyte) every 5 minutes if younger than 4 years of age or 10 mL every 5 minutes if older. After one hour, increase the rate to 10 mL and 20 mL, respectively, every 5 minutes. If vomiting recurs, discontinue oral fluids for 30 minutes, then resume at the initial (lower) rate. If there are 3 or more episodes of vomiting, start IV therapy. Atherly-John, et al.8 found this method of oral hydration superior to IV hydration with regard to length of stay, nursing staff time, and parental satisfaction, without differences in hospitalization or relapse rates.
Numerous oral electrolyte solutions are commercially available, and they typically contain 45-90 mEq/L sodium, 20-25 mEq/L potassium, 35-80 mEq/L chloride, 30 mEq/L of bicarbonate or citrate, and 2-2.5% glucose. Although oral rehydration solutions can be expensive, especially the premixed brands rather than powders, they are less expensive than IV therapy.
The amount of fluids that should be replaced is calculated by combining an estimate of fluid loss plus the typical daily maintenance of about 150 mL/kg/days. Fluid loss from visible vomiting or diarrhea can be estimated by the following tips: one tablespoon will make a spot 4 inches in diameter on cloth, 2 oz. will make a spot 8 inches in diameter, and 8 oz. will saturate a 9x12-inch diaper.
Another option to consider in patients reluctant to drink is insertion of an NG tube for enteral rehydration. Nager, et al.9 found rapid NG hydration with Pedialyte at a rate of 50 mL/kg over 3 hours to be similar in efficacy and labor intensity, yet with fewer complications and lower cost than rapid IV hydration with normal saline at a similar rate.
Intravenous Hydration. Intravenous fluids are indicated in those patients with shock, severe dehydration, moderate dehydration with inability to tolerate oral fluids, gastrointestinal bleeding, ileus or obstruction, and severe or persistent gastrointestinal disorder (pancreatitis, cholecystitis). Consider IV fluids in those with elevated BUN, electrolyte abnormalities (such as hypernatremia, metabolic alkalosis), or other need for an IV catheter placement. Initially, isotonic fluids such as normal saline or lactated Ringer's are bolused in amounts of 20 mL/kg until vital signs and mental status are normalized. If large volumes are used (e.g., > 80 mL/kg), lactated Ringer's may be preferable over normal saline, which can lead to a hyperchloremic metabolic acidosis, although the effect is of uncertain clinical consequence. Be cautious to avoid over-aggressive fluid resuscitation in patients with congestive heart failure or possible cerebral edema (e.g., Reye's syndrome). Although previous recommendations advocated cautious rehydration over 24-48 hours, rapid IV rehydration of children at a rate of 10 mL/kg/hr over three hours may be safe and avoid requirement for admission.10
Glucose-containing solutions have traditionally been avoided during intravenous rehydration. However, in children, glucose may have benefit. Levy, et al., found that a glucose-containing solution in a dose of D5NS at 20 mL/kg bolus, can reverse ketosis and hasten resolution of nausea, and decrease the chance of admission in children 6 months to 6 years of age.11 After the initial isotonic bolus, D5 with 0.45 saline if age older than 2 years or D5 with 0.33 saline if age younger than 2 years, with supplements of potassium chloride, can be given at 1.5 times maintenance amounts.
Antiemetic Agents. Antiemetics are indicated when vomiting is persistent, likely to cause harm, and when not contraindicated. There are several classes of antiemetic medications available for use (see Table 4) including the anticholinergics, antihistamines, phenothiazines, butyrophenones, dopamine antagonists, and serotonin antagonists. The newest classes of antiemetics are the cannabinoids (dronabinol) and substance P antagonists (aprepitant), and have been effective in chemotherapy-induced nausea and vomiting (CINV) and post-operative nausea and vomiting (PONV), yet are not typically used in the ED.
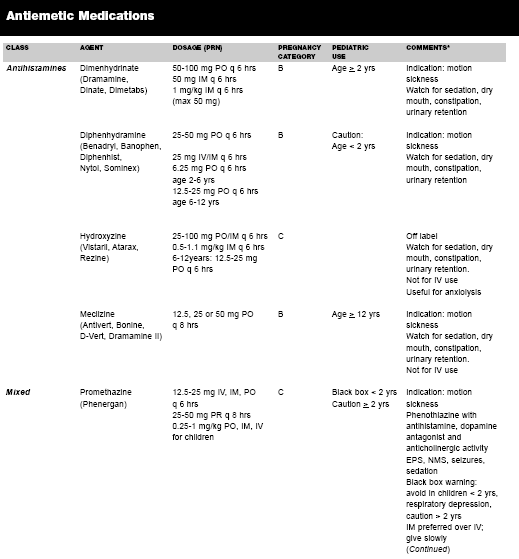 |
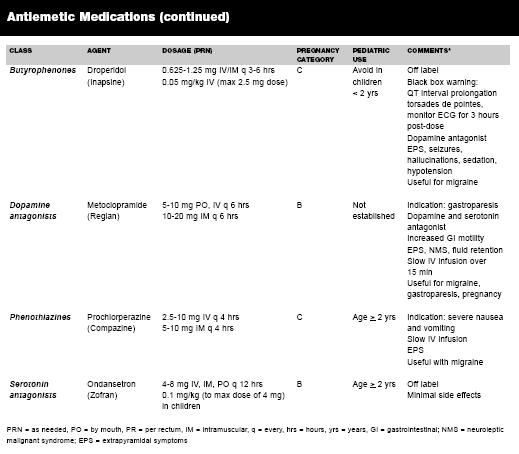 |
There are few clinical trials comparing antiemetics in general ED populations with nausea or vomiting. In one double-blind, randomized, controlled trial (RCT) of IV metoclopramide (Reglan) 10 mg, droperidol (Inapsine) 1.25 mg, and prochlorperazine (Compazine) 10 mg vs. placebo in 97 adults with nausea, droperidol was most effective at reducing nausea as measured by the visual analog scale, whereas metoclopramide and prochlorperazine were not different than placebo.12 By contrast, another double-blind, RCT of IV prochlorperazine 10 mg vs. promethazine 25 mg IV in adults with gastritis/gastroenteritis found better relief with prochlorperazine, shorter time to complete relief, fewer treatment failures (9.5% vs 31%), fewer complaints of sleepiness (38% vs 71%), and similar rate of extrapyramidal reaction.13 In a small, underpowered, non-ED RCT comparing IV promethazine 6.25 or 12.5 mg with IV ondansetron 4 mg for non-pregnancy, non-chemotherapy related vomiting in 46 adults, nausea and sedation scores were similar between groups.14 A recent RCT found similar efficacy between IV promethazine 25 mg and ondansetron 4 mg in undifferentiated nausea and vomiting in adult ED patients,15 although this dose of promethazine resulted in greater sedation. Because of the lack of clinical trials, the following general guidelines are suggested for the choice of antiemetic.
Choose the Antiemetic Agent with the Least Side Effects.
- The anticholinergic (scopolamine) as well as antihistamine agents (cyclizine, dimenhydrinate, diphenhydramine, hydroxyzine, meclizine) can result in sedation, insomnia, dizziness, dry mouth, blurred vision, tachycardia, and urinary retention and should be avoided in cases of angle-closure glaucoma or prostatic hypertrophy. The antihistamines generally are sedating and can result in dizziness, fatigue, and confusion, especially the elderly.
- The dopamine antagonists (metoclopramide, haloperidol, droperidol, promethazine, and phenothiazines) can result in extrapyramidal symptoms, QT interval prolongation, sedation, seizures, and rarely blood dyscrasias and agranulocytosis. Extrapyramidal symptoms (EPS) can be common with symptoms such as akathisia or dystonia, or rare, with syndromes of tardive dyskinesia (involuntary facial movements or tics such as lip smacking), parkinsonism (bradykinesia, tremor, rigidity), or neuroleptic malignant syndrome (fever, rigidity, tremor, autonomic disturbances, labile blood pressure). Dystonia can involve the neck (torticollis), jaw (trismus), back (opisthotonus), eyes (oculogyric crisis), and larynx (stridor). Akathisia is described as inner tension, restlessness, and inability to remain still, which can be so troubling as to lead to suicide attempts. The incidence with prochlorperazine has been reported at 16% to 44%,16,17 as much as 72% with droperidol,12 and 3% with promethazine.15 Slow infusion of prochlorperazine18 and metoclopramide19 over 15 minutes may minimize the risk of akathisia. In general, EPS are more common in children and usually occur with repeated use. EPS, especially akathisia and dystonia, can be treated with benzodiazepines, such as midazolam,20 or anticholinergic agents (diphenhydramine, benztropine, biperiden, or trihexyphenidyl), and treatment for 2-3 days may be necessary in severe reactions.* Beta-blockers, clonidine, amantadine, serotonin antagonists (cyproheptadine, remeron), and vitamin B6 (pyridoxine) may also be effective.*
- Avoid dopamine antagonists in young children, and those with seizures and prior EPS.
- Side effects for 5HT3 serotonin antagonists (ondansetron) are few and uncommon, and can include hypersensitivity, mild sedation, headache, dizziness and anxiety, warmth, flushing, diarrhea, and rapid infusion can cause transient blurred vision. Ondansetron (Zofran) has recently become generic and is becoming more cost-effective, whereas the other serotonin (5HT3) antagonists, granisetron (Kytril) and dolasetron (Anzemet), have been studied in CINV and PONV, yet are rarely used in ED patients with vomiting because of their cost.
- Promethazine (Phenergan) has a black box warning by the FDA recommending avoiding use in children younger than 2 years due to fatal respiratory depression, exercising caution with use in children older than 2 years, and avoiding promethazine with other medications that can also have respiratory depressant effects.
- Droperidol (Inapsine) has a black box warning by the FDA because of the risk of QT interval prolongation and arrhythmias (torsades de pointes), even in low doses, and although risk is low, there are strong opinions on both sides of this warning.21,22 At this time, it is prudent to consider other agents first. If droperidol is to be used, obtain a baseline 12-lead ECG and avoid using droperidol if the baseline QTc is > 440 msec. Continuous ECG monitoring should continue until 2-3 hours after droperidol administration.
- Because of its effects on GI motility, metoclopramide is contraindicated in bowel obstruction, perforation, and GI hemorrhage.
Choose an Agent Based on Familiarity, Availability, and Clinical Experience.
- Promethazine is probably still the most commonly used antiemetic in the ED,23 although ondansetron may be gaining in popularity as generic forms become available. Several agents not listed in Table 4, such as scopolamine, cyclizine, trimethobenzamide, chlorpromazine, perphenazine, thiethylperazine, and haloperidol are rarely used in the ED for vomiting.
Choose the Antiemetic Agent Based on Coexisting Conditions.
- In vertigo, choose anticholinergics or antihistamines, since these are traditionally considered more effective than others. Dimenhydrinate, a salt of diphenhydramine (58% by volume) and 8-chlorotheophylline, can be given orally or parenterally and is more effective and less sedating than lorazepam24 and equally as effective as droperidol 2.5 mg.25 Meclezine (Antivert), also available over-the-counter as Bonine and Dramamine II, is less sedating than dimenhydrinate (Dramamine), but is only given orally. Lorazepam (Ativan) or diazepam (Valium) may be effective both for the illusion of movement as well as the anxiety associated with vertigo, although supporting RCTs are few. *
- Gastroenteritis typically involves the D1 dopamine and 5HT3 serotonin receptors of the visceral nervous system. For children with simple gastroenteritis, the American Academy of Pediatrics suggests avoiding antiemetics26 since the disease is self-limited, and antiemetics are often ineffective and cause frequent side-effects. Despite this, as many as 44-52% of pediatricians, 18-55% pediatric emerency physicians, and 44-79% of emergency physicians use phenothiazines in children.27,28 Prior to ondansetron, the phenothiazines promethazine, trimethobenzamide, and prochlorperazine were most commonly prescribed.27-29 Recent studies support the safety and efficacy of oral or IV ondansetron in children with gastroenteritis.30-32*
- In vomiting associated with migraine, choose agents such as droperidol, prochlorperazine, metoclopramide, or chlorpromazine, which have demonstrated efficacy for both the headache and nausea.* Consider co-administering diphenhydramine 25 mg IV, in addition to a slow infusion of these agents over 15 minutes, since they each have a high likelihood of akathisia.
- In head injury, suspected elevation of ICP, or altered mental status, avoid antiemetics, which can lead to sedation or seizures. Ondansetron, which is nonsedating, may be a good choice in this setting. When sedating antiemetics are necessary, use the lowest dose possible.
- In overdose situations, especially theophylline or use of oral N-acetylcysteine, ondansetron may be especially effective.
- In early pregnancy, especially the first 10 weeks during organogenesis when medication use is discouraged, pyridoxine (vitamin B6)* at doses of 25 mg every 8 hours is considered safe and can prevent vomiting. For persistent nausea or vomiting, the antihistamines dimenhydrinate and diphenhydramine, or ginger (see below), are considered safe, and may be recommended for occasional outpatient use. Ginger may be more effective than pyridoxine or diphenhydramine.33 In cases of hyperemesis gravidarum, defined as intractable vomiting with dehydration, starvation ketosis, and weight loss requiring recurrent outpatient IV hydration, the use of metoclopramide, promethazine, ondansetron, prochlorperazine, or trimethobenzamide are acceptable. Ondansetron has become popular because of its low incidence of adverse effects, and has efficacy similar to promethazine. Avoid meclizine, cyclizine, thiethylperazine, and chlorpromazine during pregnancy. Small studies have reported that high-dose glucocorticoid therapy (dexamethasone or prednisone)* is either effective34 or not effective35 for pregnant patients with refractory or persistent symptoms and requirement for IV medications. Enteral and parenteral nutrition have been used in refractory cases of hyperemesis gravidarum.
- Anxiety frequently worsens nausea and vomiting, especially in anticipatory nausea of CINV. Sedating antiemetics may be advantageous in cases with anxiety such as ACS or obstruction, but should be avoided in patients with head injuries, baseline altered mental status, or those who might drive home. In some patients with persistent or refractory nausea or vomiting, treatment of anxiety with a benzodiazepine may be useful, in addition to an antiemetic. Midazolam, a short-acting benzodiazepine, has been found to decrease the risk of PONV,36* perhaps more effectively than ondansetron,37 but has not been studied in ED vomiting patients.
- In the setting of gastroparesis, treatment is with motility agents such as metoclopramide 10 mg IV or erythromycin 3 mg/kg IV (which acts directly on the motilin receptor for smooth muscles increasing antral contractions). In addition, patients should modify their diet to include more fluids than solids, avoidance of high-residue (fiber) and high-fat foods, as well as tighter control of blood glucose if diabetic. Patients with severe, grade 3 gastroparesis (termed gastric failure) refractory to medications resulting in malnutrition, dehydration, and frequent ED visits, may benefit from enteral (jejunostomy tube feedings) or parenteral nutrition, endoscopic therapy, or implantation of a gastric electrical stimulator.
In refractory nausea or vomiting, rather than repeating another or higher dose of the same agent, consider medications that work on different receptors to avoid exaggerating adverse events. Although steroids such as IV dexamethasone 8-10 mg have been used for PONV and CINV,38* use in persistent, refractory vomiting in ED patients has been limited.
Alternative Methods. Nonpharmacological methods of treating nausea and vomiting include acupuncture, acupressure, herbal therapy (ginger), massage, hypnosis, and biofeedback. Acupuncture at the P6 (Neiguan point) may have similar efficacy as traditional antiemetic medications.39 P6 is located two Chinese inches (the width across the thumb interphalangeal joint) below the wrist crease between the flexor carpi radialis and palmaris longus tendons at a depth of 1 cm. Acupressure at P6 (Sea-Band) may be slightly useful for motion sickness as well as during pregnancy40 and can be purchased from boating stores, travel agencies, and some drug stores.
Ginger has a weak 5-HT3 antagonistic effect, and may help cases of motion sickness,41 vomiting in pregnancy,33,42 and post-operative vomiting. Dosages of 250 mg PO four times daily to 500 mg PO three times daily are typical.
Nasogastric Suctioning. The primary indication for gastric decompression with a nasogastric (NG) tube in the vomiting patient is to prevent esophageal, gastric, or bowel perforation, as when the obstruction is severe and increased intraluminal pressures are associated with wall ischemia, or in patients with suspected perforations (such as Boerhaave's syndrome). NG suction is not considered efficacious for pancreatitis or large bowel obstruction (with competent ileocecal valve).43 Because NG intubation has many potential complications, including pain, bleeding, perforation, and induced vomiting, the potential benefits do not outweigh the risks in those with mild obstruction or paralytic ileus. Conversely, do consider NG suction in patients with persistent abdominal pain, distention, and vomiting refractory to medications. NG intubation is relatively contraindicated in patients with recent nasal surgery or midface trauma, coagulopathy, esophageal varices (including recent banding or cautery), esophageal stricture, or inability to protect the airway (such as coma or loss of gag reflex). Avoid blind NG insertion in patients who have undergone gastric bypass procedures unless approved by their bariatric surgeon, since NG insertion could be difficult or result in perforation of the anastomosis. Patients consider NG intubation a painful procedure, perhaps worse than abscess drainage, fracture reduction, or urethral catheterization.44 In addition to discomfort and bleeding (which can be minimized by use of vasoconstrictive agent), NG insertion can result in tracheal or bronchial misplacement, perforation of the pharynx or esophagus, and pneumothorax. The discomfort of NG insertion can be minimized by local anesthesia with nasal viscous 2% or atomized lidocaine, nebulized lidocaine solution (1%, 2%, or 4%, not to exceed 4 mg/kg) via facemask, or nasal spray containing benzocaine or tetracaine-benzocaine-butyl aminobenzoate (Cetacaine). IV metoclopramide 10 mg prior to NG insertion may diminish both the nausea as well as the discomfort associated with NG tube placement.45
Conclusion
Because of the broad range of potential etiologies of nausea and vomiting, an ordered approach to evaluation is necessary to maintain cost effectiveness and avoid misdiagnosis. In the ED, it is imperative to decide whether there is potential for an acute life-threatening emergency (see Table 2) and beware of the potential medicolegal pitfall of mislabeling appendicitis, meningitis, or sepsis as "gastroenteritis." Patients with severe, refractory symptoms, significant metabolic abnormalities, or evidence of an acute emergency require hospitalization for expedited evaluation and treatment. The emergency physician must also decide what diagnostic tests are indicated in the ED and which are appropriate for the outpatient setting. Not all vomiting requires IV hydration; oral hydration is often safer, cheaper, and as effective. Not all nausea or vomiting cases require antiemetic use; many patients have self-limited conditions Remember that all antiemetics have side effects, and the emergency physician needs to be prepared to treat serious medication side effects.
References
1. Bhatia J, Greer F, American Academy of Pediatrics Committee on Nutrition. Use of soy protein-based formuals in infant feeding. Pediatrics 2008;121: 1062-1068.
2. Kimberly HH, Shah S, Marill K, et al. Correlation of optic nerve sheath diameter with direct measurement of intracranial pressure. Acad Emerg Med 2008; 15:201-204.
3. Mandell GA, Wolfson PJ, Adkins ES, et al. Cost-effective imaging approach to the nonbilious vomiting infant. Pediatrics 1999;103:1198-1202.
4. King CK, Glass R, Bresee JS, et al. Managing acute gastroenteritis among children, oral rehydration, maintenance, and nutritional therapy. MMWR Morb Mortal Wkly Rep 2003;52:1-16.
5. Walker WS, Cameron EW, Walbaum PR. Diagnosis and management of spontaneous transmural rupture of the esophagus (Boerhaave's syndrome). Br J Surg 1985;72: 204-207.
6. Harris JM, DiPalma JA. Clinical significance of Mallory-Weiss tears. Am J Gastroenter 1993;88: 2056-8.
7. Fonseca BK, Holdgate A, Craig JC. Enteral vs intravenous rehydration therapy for children with gastroenteritis: A meta-analysis of randomized controlled trials. Arch Pediatr Adolesc Med 2004;158:483-490.
8. Atherly-John YC, Cunningham SJ, Crain EF. A randomized trial of oral vs intravenous rehydration in a pediatric emergency department. Arch Pediatr Adolesc Med 2002;156:1240-1243.
9. Nager AL, Wang VJ. Comparison of nasogastric and intravenous methods of rehydration in pediatric patients with acute dehydration. Pediatrics 2002;109:566-572.
10. Moineau G, Newman J. Rapid intravenous rehydration in the pediatric emergency department. Ped Emerg Care 1990;6:186-188.
11. Levy JA, Bachur RG. Intravenous dextrose during outpatient rehydration in pediatric gastroenteritis. Acad Emerg Med 2007;14:324-331.
12. Braude D, Soliz T, Crandall C, et al. Antiemetics in the ED: A randomized controlled trial comparing 3 common agents. Am J Emerg Med 2006;24: 177-182.
13. Ernst AA, Takakuwa KM, Weiss SJ, et al. Prochlorperazine versus promethazine for gastritis/gastroenteritis: A randomized clinical trial. Acad Emerg Med 2000;7:445-446.
14. Moser JD, Caldwell JB, Rhule FJ. No more than necessary: Safety and efficacy of low-dose promethazine. Ann Pharmacother 2006;40:45-48.
15. Braude D, Crandall C. Ondansetron versus promethazine to treat acute undifferentiated nausea in the emergency department: A randomized, double-blind, noninferiority trial. Acad Emerg Med 2008;15:209-215.
16. Drotts DL, Vinson DR. Prochlorperazine induces akathisia in emergency patients. Ann Emerg Med 1999;34:469-475.
17. Olsen JC, Keng JA, Clark JA. Frequency of adverse reactions to prochlorperazine in the ED. Am J Emerg Med 2000;18:609-611.
18. Vinson DR, Migala AF, Quesenberry CP, Jr. Slow infusion for the reduction of akathisia induced by prochlorperazine: A randomized controlled trial. J Emerg Med 2001;20:113-119.
19. Parlak I, Atilla R, Cicek M, et al. Rate of metoclopramide infusion affects the severity and incidence of akathisia. Emerg Med J 2005;22:621-624.
20. Parlak I, Erdur B, Parlak M, et al. Midazolam vs. diphenydramine for the treatment of metoclopramide-induced akathisia: A randomized controlled trial. Acad Emerg Med 2007;14:715-721
21. Jackson CW, Sheehan AH, Reedan JG. Evidence-based review of the black-box warning for droperidol. Am J Health Syst Pharm 2007;64:1174-1186.
22. Gan TJ. Black box warning on droperidol: A report of the FDA convened expert panel. Anesth Analg 2004;98:1809.
23. LaValley J, Crandall CS, Braude DA. Nausea and vomiting management in US emergency departments [abstract]. Acad Emerg Med 2003;10:461.
24. Marill KA, Walsh MJ, Nelson BK, et al. Intravenous lorazepam versus dimenhydrinate for treatment of vertigo in the emergency department: A randomized clinical trial. Ann Emerg Med 2000;36:310-319.
25. Irving C, Richman PB, Kaiafas C, et al. Intramuscular droperidol versus intramuscular dimenhydrinate for the treatment of acute peripheral vertigo in the emergency department: A randomized, clinical trial. Acad Emerg Med 2002;9:650-653.
26. Practice parameter: The management of acute gastroenteritis in young children. American Academy of Pediatrics, Provisional Committee on Quality Improvement, Subcommittee on Acute Gastroenteritis. Pediatrics 1996;97: 424-435.
27. Forstater AT, Labor J, Kost SI, et al. Phenothiazine use for vomiting in children with gastroenteritis: A survey. Ann Emerg Med 2000;36:S29.
28. Kwon KT, Rudkin SE, Langdorf MI. Antiemetic use in pediatric gastroenteritis: A national survey of emergency physicians, pediatricians, and pediatric emergency physicians. Clin Pediatr 2002;41:641-652.
29. Freedman SB, Fuchs S. Antiemetic therapy in pediatric emergency departments. Pediatr Emerg Care 2004;20:625-633.
30. Ramsook C, Sahagun-Carreon I, Kozinetz CA, et al. A randomized clinical trial comparing oral ondansetron with placebo in children with vomiting from acute gastroenteritis. Ann Emerg Med 2002;39:397-403.
31. Freedman SB, Adler M, Seshadri R, et al. Oral ondansetron for gastroenteritis in a pediatric emergency department. N Engl J Med 2006;354:1698-1705.
32. Stork CM, Brown KM, Reilly TH, et al. Emergency department treatment of viral gastritis using intravenous ondansetron or dexamethasone in children. Acad Emerg Med 2006;13:1027-1033.
33. Vutyavanich T, Kraisarin T, Ruangsri R. Ginger for nausea and vomiting in pregnancy: Randomized, double-masked, placebo-controlled trial. Obstet Gynecol 2001;97:577-582.
34. Bondok RS, El Sharnouby NM, Eid HE, et al. Pulse steroid therapy is an effective treatment for intractable hyperemesis gravidarum. Crit Care Med 2006;34:2781-2783.
35. Yost NP, McIntire DD, Wians FH, et al. A randomized, placebo-controlled trial of corticosteroids for hyperemesis due to pregnancy. Obstet Gynecol 2003;102:1250-1254.
36. Bauer KP, Dom PM, Ramirez AM, et al. Preoperative intravenous midazolam: Benefits beyond anxiolysis. J Clin Anesth 2004;16:177-183.
37. Sanjay OP, Tauro DI. Midazolam: An effective antiemetic after cardiac surgerya clinical trial. Anesth Analg 2004;99:339-343.
38. Henzi I, Walker B, Tramer MR. Dexamethasone for the prevention of postoperative nausea and vomiting: A quantitative systematic review. Anesth Analg 2000;90:186-194.
39. Ezzo J, Streitberger K, Schneider A. Cochrane systematic reviews examine P6 acupuncture-point stimulation for nausea and vomiting. J Altern Complement Med 2006;12:489-495.
40. Helmreich RJ, Shiao SY, Dune LS. Meta-analysis of acustimulation effects on nausea and vomiting in pregnant women. Explore (NY) 2006;2:412-421.
41. Schmid R, Schick T, Steffen R, et al. Comparison of seven commonly used agents for prophylaxis of seasickness. J Trav Med 1994;1:203-206.
42. Fischer-Rasmussen W, Kjaer S, Dahl C, et al. Ginger treatment of hyperemesis gravidarum. Eur J Obstet Gynecol Reprod Biol 1990;38:19-24.
43. Witting MD. "You wanna do what?!" Modern indications for nasogastric intubation. J Emerg Med 2007;33:61-64.
44. Singer AJ, Richman PB, Kowalska A, et al. Comparison of patient and practitioner assessments of pain from commonly performed emergency department procedures. Ann Emerg Med 1999;33:652-658.
45. Ozucelik DN, Karaca MA, Sivri B. Effectiveness of pre-emptive metoclopramide infusion in alleviating pain, discomfort and nausea associated with nasogastric tube insertion: A randomized, double-blind, placebo-controlled trial. Int J Clin Pract 2005;59:1422-1427.
Few sounds or smells in the emergency department (ED) get our attention as easily as vomiting. In response, we might reflexively order our "one-size-fits-all" standard antiemetic and begin by assuming that this is probably just another case of "gastroenteritis." There are, however, several antiemetics to choose from, each with its own advantages and disadvantages, as well as a myriad of diagnostic possibilities to consider.Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
